Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (23): 3688-3693.doi: 10.3969/j.issn.2095-4344.2017.23.014
Previous Articles Next Articles
Pedicle screw fixation combined with posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis in the elderly
Chen Kang-wu, Zhang Kai, Chen Hao, Wang Gen-lin, Zhu Xiao-yu, Qian Zhong-lai, Yang Hui-lin
- Department of Orthopedics, the Affiliated Hospital of Soochow University, Suzhou 215006, Jiangsu Province, China
-
Online:2017-08-18Published:2017-09-01 -
Contact:Yang Hui-lin, Professor, Chief physician, Doctoral supervisor, Department of Orthopedics, the Affiliated Hospital of Soochow University, Suzhou 215006, Jiangsu Province, China -
About author:Chen Kang-wu, Master, Attending physician, Department of Orthopedics, the First Affiliated Hospital of Soochow University, Suzhou 215006, Jiangsu Province, China -
Supported by:the General Project of the Jiangsu Provincial Natural Science Foundation of the Universities, No. 16KJD320004; the Suzhou Young Science and Technology Project, No. kjxw2014009
CLC Number:
Cite this article
Chen Kang-wu, Zhang Kai, Chen Hao, Wang Gen-lin, Zhu Xiao-yu, Qian Zhong-lai, Yang Hui-lin. Pedicle screw fixation combined with posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis in the elderly[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(23): 3688-3693.
share this article
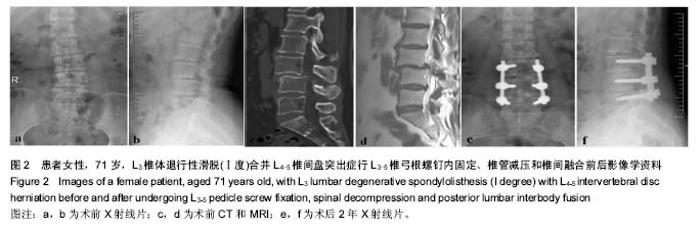
2.3 内固定效果分析 30例高龄退行性腰椎滑脱症患者均顺利完成手术。平均住院时间为(16.6±2.9) d(9-41) d,术前平均住院时间为(4.9±1.2) d(2-18 d)。平均手术时间(225.6±23.4) min,平均术中出血量(470±45.5) mL。手术固定范围:L4-L5 18例、L3-L5 5例、L4-S1 3例、L2-L5 2例、L3-S1 2例;融合节段:1节段24例(L4-5 23例、L5-S1 1例)、2节段3例(L3-L5 2例、L4-S1 1例)、3节段3例(L2-L5 2例、L3-S1 1例)。其中有1例患者诊断为L3椎体退行性滑脱(Ⅰ度)合并L4-5椎间盘突出症,予以L3-5椎弓根螺钉内固定、椎管减压和椎间融合术,手术疗效满意(图2)。"
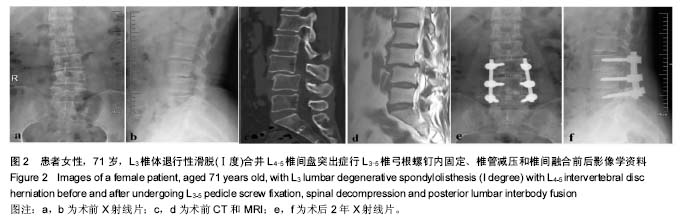
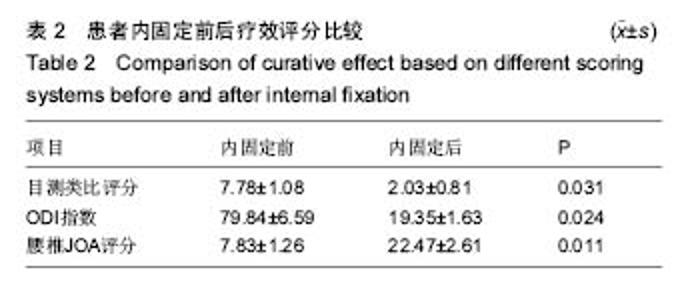
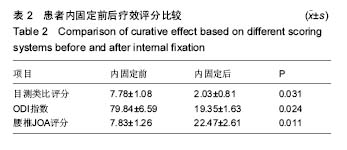
2.4 疗效评价 内固定后目测类比评分为显著优于内固定前,差异均有显著性意义(P < 0.05); 内固定后后ODI指数与腰椎JOA评分较内固定前前有明显改善(P < 0.05),见表2。 腰椎JOA评分改善率情况:治愈3例,显著有效24例,有效3例,无效0例。 根据椎间融合判定标准,所有患者均达到骨性融合,平均融合时间为4-8(5.13±0.65)个月。 2.5 不良反应 围手术期无全身伴发疾病相关并发症发生,有6例(20%)患者出现手术相关并发症。其中1例硬膜囊撕裂,术后发生脑脊液漏,予以头低足高位,术后3 d拔除引流管,紧密缝合引流口,2周后切口愈合良好;2例麻痹性肠梗阻,经胃管减压、灌肠等保守治疗后缓解。3例患者出现一过性神经症状加重,经用脱水、小剂量激素、营养神经等治疗后缓解。随访期间无椎间融合器移位、椎弓根螺钉松动或断裂等并发症发生。 "
| [1] Kalichman L, Hunter DJ.Diagnosis and conservative management of degenerative lumbar spondylolisthesis. Eur Spine J.2008;17(3):327-335. [2] Alfieri A, Gazzeri R, Prell J, et al. The current management of lumbar spondylolisthesis. J Neurosurg Sci.2013; 57(2): 103-113.[3] Xu H, Tang H, Li Z. Surgical treatment of adult degenerative spondylolisthesis by instrumented transforaminal lumbar interbody fusion in the Han nationality. J Neurosurg Spine 2009;10(5):496-499.[4] Ishimoto Y, Yoshimura N, Muraki S, et al. Association of Lumbar Spondylolisthesis With Low Back Pain and Symptomatic Lumbar Spinal Stenosis in a Population-based Cohort: The Wakayama Spine Study. Spine (Phila Pa 1976). 2017;42(11):E666-E671. [5] Carreon LY, Puno RM, Dimar JR, et al. Perioperative complications of posterior lumbar decompression and arthrodesis in older adults. J Bone Joint Surg Am. 2003; 85(11):2089-2092.[6] Okuda S, Oda T, Miyauchi A, et al. Surgical outcomes of posterior lumbar interbody fusion in elderly patients. J Bone Joint Surg Am. 2006; 88(12):2714-2720.[7] Vibert BT, Sliva CD, Herkowitz HN. Treatment of instability and spondylolisthesis: surgical versus nonsurgical treatment. Clin Orthop Relat Res. 2006; 443:222-227.[8] Ghogawala Z,Dziura J,Butler WE,et al. Laminectomy plus Fusion versus Laminectomy Alone for Lumbar Spondylolisthesis. N Engl J Med. 2016; 374(15):1424-1434.[9] 陈德龙,陈小强,叶永松. 后路腰椎椎体间融合术治疗腰椎滑脱的临床疗效[J]. 脊柱外科杂志,2014. 12(4):245-247.[10] Meyerding HW. Spondylolisthesis. J Bone Joint Surg Am. 1932; 13(1):39-48.[11] Sun Y, Wang H, Yang D, et al. Characterization of radiographic features of consecutive lumbar spondylolisthesis. Medicine (Baltimore). 2016; 95(46):e5323.[12] Lieber BA, Chiang V, Prabhu AV, et al. Postoperative Complications for Elderly Patients After Single-Level Lumbar Fusions for Spondylolisthesis. World Neurosurg. 2016; 91: 149-153.[13] Matz PG, Meagher RJ, Lamer T, et al. Guideline summary review: An evidence-based clinical guideline for the diagnosis and treatment of degenerative lumbar spondylolisthesis. Spine J. 2016;16(3):439-448.[14] Gandhoke GS, Kasliwal MK, Smith JS, et al. Multicenter Evaluation of Clinical and Radiographic Outcomes Following High-gradeSpondylolisthesis Reduction and Fusion. Clin Spine Surg. 2017; 30(4):E363-E369.[15] Sakaura H, Miwa T, Yamashita T, et al. Posterior lumbar interbody fusion with cortical bone trajectory screw fixation versus posteriorlumbar interbody fusion using traditional pedicle screw fixation for degenerative lumbar spondylolisthesis: a comparative study. J Neurosurg Spine. 2016; 25(5):591-595.[16] Joaquim AF, Milano JB, Ghizoni E, et al. Is There a Role for Decompression Alone for Treating Symptomatic Degenerative Lumbar Spondylolisthesis?: A Systematic Review. Clin Spine Surg. 2016; 29(5):191-202.[17] Tay KS, Bassi A, Yeo W, et al. Intraoperative reduction does not result in better outcomes in low-grade lumbar spondylolisthesis with neurogenic symptoms after minimally invasive transforaminal lumbar interbody fusion-a 5-year follow-up study. Spine J. 2016; 16(2):182-190.[18] Audat ZM, Darwish FT, Al Barbarawi MM, et al. Surgical management of low grade isthmic spondylolisthesis; a randomized controlled study of the surgical fixation with and without reduction. Scoliosis. 2011; 6(1):14. [19] Lian XF, Hou TS, Xu JG, et al. Posterior lumbar interbody fusion for aged patients with degenerative spondylolisthesis: is intentional surgical reduction essential? Spine J. 2013; 13(10):1183-1189.[20] Bai X, Chen J, Liu L, et al. Is reduction better than arthrodesis in situ in surgical management of low-gradespondylolisthesis? A system review and meta analysis. Eur Spine J. 2017; 26(3): 606-618.[21] 张林林,孟斌,杨惠林. 成人平衡型L5-S1 Ⅲ度峡部裂型腰椎滑脱后路复位对骨盆平衡的影响[J]. 中华医学杂志, 2016. 96(23): 1811-1814.[22] Sears W. Posterior lumbar interbody fusion for degenerative spondylolisthesis: restoration of sagittal balance using insert-and-rotate interbody spacers. Spine J. 2005; 5(2): 170-179.[23] Ghogawala Z, Resnick DK, Glassman SD, et al. Randomized controlled trials for degenerative lumbar spondylolisthesis: which patients benefit from lumbar fusion? J Neurosurg Spine. 2017; 26(2):260-266[24] Jalalpour K, Neumann P, Johansson C, et al. A Randomized Controlled Trial Comparing Transforaminal Lumbar Interbody Fusion and Uninstrumented Posterolateral Fusion in the Degenerative Lumbar Spine. Global Spine J. 2015; 5(4): 322-328.[25] Ohtori S, Koshi T, Yamashita M, et al. Single-level instrumented posterolateral fusion versus non-instrumented anterior interbody fusion for lumbar spondylolisthesis: a prospective study with a 2-year follow-up. J Orthop Sci. 2011; 16(4):352-358.[26] Chandra VV, Prasad BC, Jagadeesh MA, et al. Segmental polymethylmethacrylate-augmented fenestrated pedicle screw fixation for lumbar spondylolisthesis in patients with osteoporosis - A case series and review of literature. Neurol India. 2017; 65(1):89-95.[27] Chang MC, Kao HC, Ying SH, et al. Polymethylmethacrylate augmentation of cannulated pedicle screws for fixation in osteoporotic spines and comparison of its clinical results and biomechanical characteristics with the needle injection method. J Spinal Disord Tech. 2013; 26(6):305-315.[28] Kuraishi S, Takahashi J, Mukaiyama K, et al. Comparison of clinical and radiological results of posterolateral fusion and posterior lumbar interbody fusion in the treatment of L4 degenerative lumbar spondylolisthesis. Asian Spine J. 2016; 10(1):143-152.[29] Pawar AY, Hughes AP, Sama AA, et al. A comparative study of lateral lumbar interbody fusion and posterior lumbar interbody fusion in degenerative lumbar spondylolisthesis. Asian Spine J. 2015; 9(5):668-674. [30] Liu J, Deng H, Long X, et al. A comparative study of perioperative complications between transforaminal versus posterior lumbar interbody fusion in degenerative lumbar spondylolisthesis. Eur Spine J. 2016; 25(5):1575-1580.[31] 田海军,陈德玉,卢旭华,等. 两种融合手术治疗腰椎滑脱症的影像学及临床疗效比较[J]. 中华骨科杂志, 2009. 29(5):445-449.[32] 陈涛,贾世青,陈武,等. 椎体间融合内固定治疗腰椎滑脱症:脊柱-骨盆参数的变化[J].中国组织工程研究, 2013,17(4):576-581.[33] Macki M, Bydon M, Weingart R, et al. Posterolateral fusion with interbody for lumbar spondylolisthesis is associated with less repeat surgery than posterolateral fusion alone. Clin Neurol Neurosurg. 2015; 138(8):117-123.[34] Atabey C, Gocmen S, Simsek H, et al. Surgical results of degenerative spondylolisthesis patients over 70 years old: a single-center experience and clinical outcomes. Turk Neurosurg, 2012, 22(5):534-539. [35] 杨二柱,徐建广,连小峰. 提拉复位治疗老年腰椎退变性滑脱[J]. 中国矫形外科杂志, 2012. 20(15):1377-1379.[36] Benz RJ, Ibrahim ZG, Afshar P, et al. Predicting complications in elderly patients undergoing lumbar decompression. Clin Orthop Relat Res. 2001; 384(4):116-121.[37] Cassinelli EH, Eubanks J, Vogt M, et al. Risk factors for the development of perioperative complications in elderly patients undergoing lumbar decompression and arthrodesis for spinal stenosis: an analysis of 166 patients. Spine. 2007; 32(2): 230-235.[38] Okuda S, Oda T, Miyauchi A, et al. Surgical outcomes of posterior lumbar interbody fusion in elderly patients. Surgical technique. J Bone Joint Surg Am. 2007; 89(2):310-320. |
| [1] | Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao. Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 796-802. |
| [2] | Annikaer•Aniwaer, Palidaimu•Tuerti, Adili•Maimutimin, Zhang Fan, Niruti•Tuerxun. Three-dimensional finite element analysis of different implant prostheses in maxillary anterior teeth region under different occlusal relationships [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(16): 2531-2536. |
| [3] | Fu Jiaxin, Xiao Lianping, Wang Shusen, Li Xiaodong, Han Liqiang, Wang Tonghao. Therapeutic effects of paraspinal approach combined with internal fixation through pedicle of fractured vertebra versus traditional AF screw-rod system for thoracolumbar fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1177-1181. |
| [4] | Qiu Zhongpeng, Li Ke, Li Gang, Liu Keyu, Du Xinhui, Meng Defeng, Shi Chenhui, Wang Weishan. Different treatments for two-part and three-part proximal humeral fractures by Neer classification: follow-up results analyzed using clinical economics [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1188-1195. |
| [5] | Ke Wei, Li Ke, Wang Sibo, Du Xinhui, Qiu Zhongpeng, Kang Zhilin, Wang Weishan, Li Gang . Open reduction and plate fixation versus closed reduction and external fixation for distal radius fractures: scores and linear regression analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1196-1202. |
| [6] | Fan Zhirong, Peng Jiajie, Zhong Degui, Zhou Lin, Su Haitao, Huang Yongquan, Wu Jianglin, Liang Yihao. Suture anchor combined with open reduction and internal fixation versus open reduction and internal fixation for ankle fracture combined with deltoid ligament injury: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1307-1312. |
| [7] | Zhou Yu, Liu Yuehong, Liu Shuping, Chen Xi, Qin Wei, Li Qifeng. Spinal stability of intervertebral grafting reinforced by five or six augmenting screws versus transvertebral grafting reinforced by four augmenting screws for thoracolumbar vertebral fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 505-511. |
| [8] | Li Xianzhou, Wang Qian, Zhang Cunxin . Lumbar spondylolisthesis: status and prospects of implant treatment [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 621-627. |
| [9] | Yin Hao, Zhou Enchang, Pan Zhengjun, Chen Guang, Jiang Hua. Finite element analysis of the four and three cannulated screws combined with buttress plate fixation for the treatment of Pauwels III femoral neck fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(32): 5133-5137. |
| [10] |
Wang Lei, Li Zilong, Yuan Binbin, Wu Qingwei, Tang Fengming.
Clinical effect of locking plate versus anterograde intramedullary nail in the treatment of adult humeral shaft fractures: a meta-analysis
[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(24): 3924-3930.
|
| [11] | Hao Liang, Zhang Zhonglin, Wang Baodong, Bi Zhenggang. Intertrochanteric fracture of the femur: improvement of internal fixation device, surgical changes and related disputes [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(18): 2927-2935. |
| [12] | Yao Liquan, Ling Qinjie, Li Jiaying, Zhong Letian, Zhou Xingping, Liu Jintao, He Erxing, Yin Zhixun. Antibiotic artificial bone implantation for treating pyogenic spondylodiscitis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2133-2139. |
| [13] | Gong Zhibing, Wu Zhaoke, Zhang Huantang, Xu Zhiqing, Zhuang Zhikun, Zhang Qianjin. Allogeneic cortical bone plate combined with locking plate for Vancouver type B1 and C osteoporotic periprosthetic femoral fractures after hip arthroplasty in older adults [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1812-1817. |
| [14] | Li Xiaofeng, Xie Furong, Zhan Long, Yang Yuan. Design of locking compression plate through transoral approach [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1824-1828. |
| [15] | Tian Youyong, Wang Zhiyong. Short-term follow-up of dynamic hip screw versus proximal femoral nail anti-rotation for type AO/OTA A1 intertrochanteric femoral fracture in older adults [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1834-1839. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||