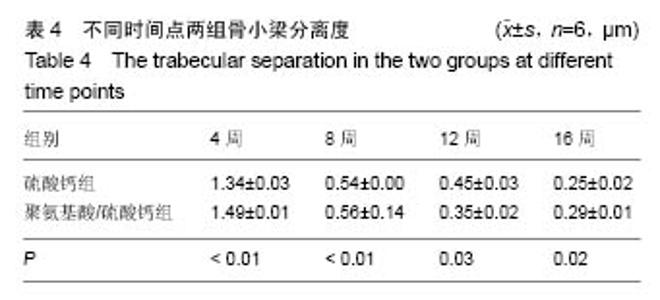
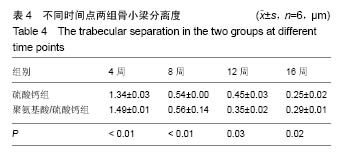
Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (6): 829-835.doi: 10.3969/j.issn.2095-4344.2017.06.002
Previous Articles Next Articles
Calcium sulfate bone cement with or without injectable polyamino acid for goat vertebral defects: a comparative experiment
- Department of Orthopaedics, West China Hospital of Sichuan University, Chengdu 610041, Sichuan Province, China
-
Received:2016-12-02Online:2017-02-28Published:2017-03-16 -
Contact:Zeng Jian-cheng, Associate professor, Department of Orthopaedics, West China Hospital of Sichuan University, Chengdu 610041, Sichuan Province, China -
About author:Wang Xian-di, Master, Physician, Department of Orthopaedics, West China Hospital of Sichuan University, Chengdu 610041, Sichuan Province, China -
Supported by:the Science and Technology Program of the Science & Technology Department of Sichuan Province, No. 2012SZ0128
CLC Number:
Cite this article
Wang Xian-di, Chen Guo, Li Zhu-hai, Jiang Hu-shan, Nie Hong-fei, Xie Tian-hang, Huang Hong-jie, Pei Fu-xing, Song Yue-ming, Zeng Jian-cheng. Calcium sulfate bone cement with or without injectable polyamino acid for goat vertebral defects: a comparative experiment[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(6): 829-835.
share this article
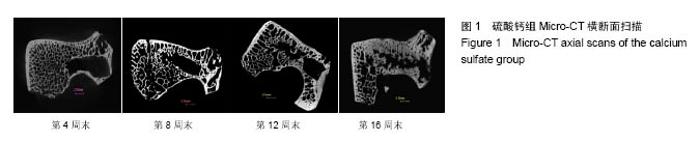
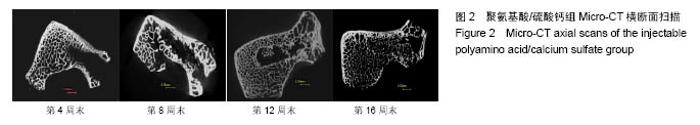
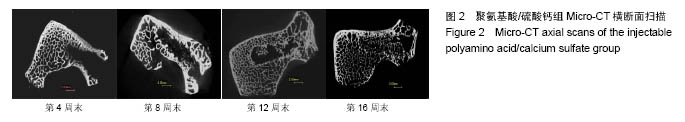
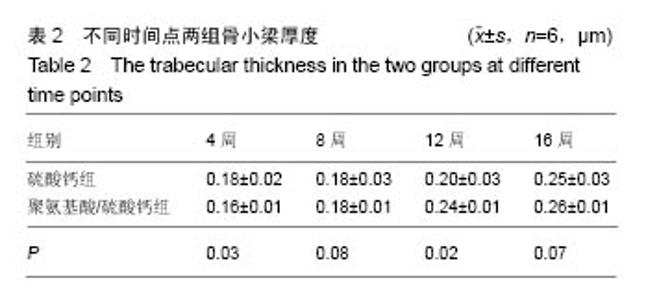
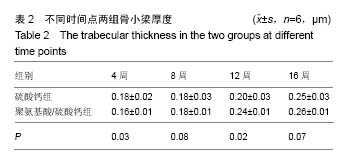
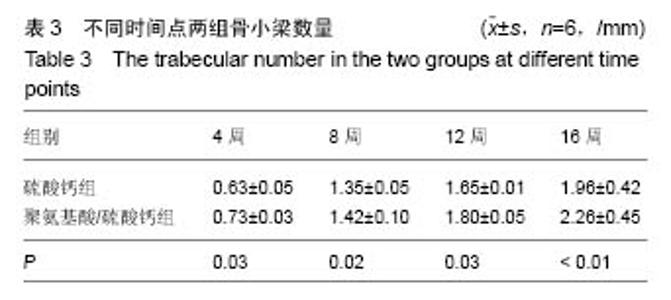
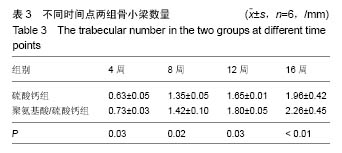
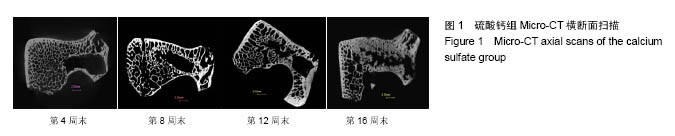
2.1 一般情况 所有实验动物均进入结果分析。切口均Ⅰ/甲愈合,无感染、无神经脊髓损伤。取材时见外口骨蜡存在,骨蜡覆盖处有不同量新骨形成。 2.2 Mirco-CT横断面观察 两组在4个不同时间点的Micro-CT二维扫描图像见图1,2。 4周末时,两组骨缺损内均未见填充材料。在骨缺损边缘均有少量骨小梁生成,PAA/CS组底部生成的骨小梁较硫酸钙组多。 8周末时,两组骨缺损有缩小趋势,硫酸钙组骨缺损底部有一定新骨生成。PAA/CS组除在底部有新骨生成外,在骨缺损的外口部也有少量的新骨生成,骨缺损已变得不规则。新生骨小梁密度稍高于周围正常骨小梁,排列结构欠清晰。 12周末时,硫酸钙组新生骨较多,骨缺损已变得不规则,底部和中部新生骨小梁已有少部分相互链接。PAA/CS组新生骨小梁明显,在骨缺损外口处和中间部相连,将其分隔。 16周末时,硫酸钙组骨缺损尚剩余不规则腔隙,新生骨小梁密度较高,排列欠规则。PAA/CS组新生骨小梁几乎将骨缺损完全充填,骨小梁结构清晰,连接良好。在Micro-CT二维横断面上显示骨缺损残留硫酸钙组多于PAA/CS组。"
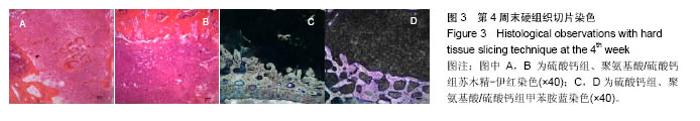
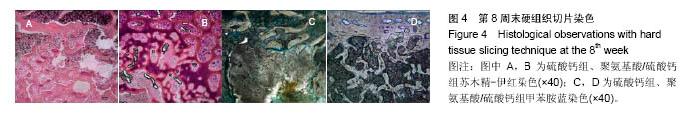
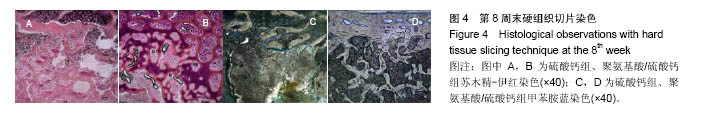
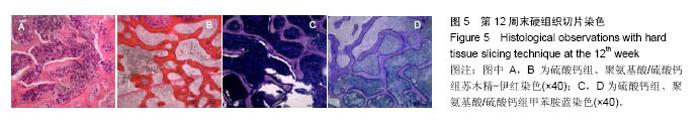
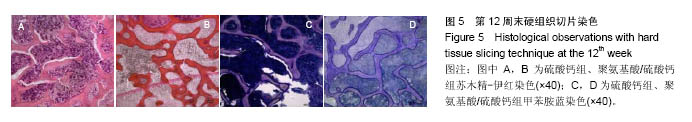
2.4 硬组织切片观察结果 术后4周(图3):两组标本内可见到清晰的骨缺损,内填充成纤维细胞,有淋巴细胞灶状浸润。骨缺损内有较多胶原纤维生成,周边部可见到有少量新生骨小梁,有成骨细胞整齐排列于表面,可见较多炎性细胞浸润,炎性细胞在PAA/CS组标本中明显少于硫酸钙组。 术后8周(图4):两组标本骨缺损中的新生骨小梁数目均有增多,可见排列整齐的成骨细胞围绕新生骨小梁排列。硫酸钙组新生骨小梁主要集中在骨缺损底部,PAA/CS组标本在底部及中间部均有新生骨小梁生成。PAA/CS组骨缺损中心部位仍可见淋巴细胞浸润。 术后12周(图5):两组骨小梁数目继续增多、增粗、密度增高。周边部分编织骨已开始转化为板层骨,具有正常骨小梁的形态,靠近缺损中心的骨小梁周围仍然可见成骨细胞规则排列在骨缺损底部,骨小梁形成于中间部分。PAA/CS组中间部分骨小梁形成多于硫酸钙组。 术后16周(图6):两组均有大量骨小梁生成,部分连接,大部分新生骨小梁已具有正常骨小梁结构。"
| [1]Younger EM, Chapman MW Morbidity at bone graft donor sites. J Orthop Trauma. 1989;3(3):192-195.[2]Pryor LS, Gage E, Langevin CJ, et al. Review of bone substitutes. Craniomaxillofac Trauma Reconstr. 2009;2(3): 151-160.[3]Perry A, Mahar A, Massie J, et al. Biomechanical evaluation of kyphoplasty with calcium sulfate cement in a cadaveric osteoporotic vertebral compression fracture model. Spine J. 2005;5(5):489-493.[4]Stubbs D, Deakin M, Chapman-Sheath P, et al. In vivo evaluation of resorbable bone graft substitutes in a rabbit tibial defect model. Biomaterials. 2004;25(20):5037-5044.[5]Goodrich JT, Sandler AL, Tepper O. A review of reconstructive materials for use in craniofacial surgery bone fixation materials, bone substitutes, and distractors. Childs Nerv Syst. 2012;28(9):1577-1588.[6]Magnan B, Bondi M, Maluta T, et al. Acrylic bone cement: current concept review. Musculoskelet Surg. 2013;97(2):93-100.[7]Wu XT, Jiang XJ, Zhang SD, et al. Biomechanical evaluation of vertebroplasty using calcium sulfate cement for thoracolumbar burst fractures. Chin J Traumatol. 2007;10(6): 327-333.[8]Taylor RS, Fritzell P, Taylor RJ. Balloon kyphoplasty in the management of vertebral compression fractures: an updated systematic review and meta-analysis. Eur Spine J. 2007;16(8): 1085-1100.[9]Heini PF, Berlemann U. Bone substitutes in vertebroplasty. Eur Spine J. 2001;10 Suppl 2:S205-213.[10]Xie P, Zhao Y, Li G. Efficacy of percutaneous vertebroplasty in patients with painful vertebral metastases: A retrospective study in 47 cases. Clin Neurol Neurosurg. 2015;138:157-161.[11]Dressmann H. Ueber Knochenplombierung bei Hohlenformigen Defekten des Knochens. Beitr Klin Chir. 1892; 9: 804-810.[12]Turner TM, Urban RM, Gitelis S, et al. Resorption evaluation of a large bolus of calcium sulfate in a canine medullary defect. Orthopedics. 2003;26(5 Suppl):s577-579.[13]Zhang J, He F, Zhang W, et al. Mechanical force enhanced bony formation in defect implanted with calcium sulphate cement. Bone Res. 2015;3:14048.[14]Zampelis V, Tägil M, Lidgren L, et al. The effect of a biphasic injectable bone substitute on the interface strength in a rabbit knee prosthesis model. J Orthop Surg Res. 2013;8:25.[15]Liu W, Wu C, Liu W, et al. The effect of plaster (CaSO4 •1/2H2O) on the compressive strength, self-setting property, and in vitro bioactivity of silicate-based bone cement.J Biomed Mater Res B Appl Biomater. 2013;101(2):279-286.[16]崔文岗,石岩,肖德明.硫酸钙人工骨修复骨缺损的应用研究进展[J]. 生物骨科材料与临床研究, 2013, 10(5): 21-23.[17]Ryu KS, Shim JH, Heo HY, et al. Therapeutic efficacy of injectable calcium phosphate cement in osteoporotic vertebral compression fractures: prospective nonrandomized controlled study at 6-month follow-up. World Neurosurg. 2010;73(4): 408-411.[18]Cardoso DA, van den Beucken JJ, Both LL, et al. Gelation and biocompatibility of injectable alginate-calcium phosphate gels for bone regeneration. J Biomed Mater Res A. 2014; 102(3):808-817.[19]Evaniew N, Tan V, Parasu N, et al. Use of a calcium sulfate-calcium phosphate synthetic bone graft composite in the surgical management of primary bone tumors. Orthopedics. 2013;36(2):e216-222.[20]黄强,李程,周宗科,等.掺锶硫酸钙复合骨修复材料的制备及体外特性研究[J].生物医学工程学杂志,2009,26(3):575-579.[21]张民,王建生,卫小春,等.注射性硫酸钙/羟基磷灰石骨替代材料的性能研究[J].中国康复,2006,21(1): 16-17.[22]陈华,田学忠,张伯勋,等.硫酸钙骨内植入修复兔包容性骨缺损的力学分析[J].中国矫形外科杂志, 2008, 16(5): 373-375.[23]赵增辉,蒋电明,权正学,等. 灭菌对聚氨基酸/硫酸钙复合材料理化性能的影响[J].第三军医大学学报, 2011, 33(2): 119-123.[24]严永刚,李鸿,吕国玉,等.氨基酸共聚物-硫酸钙复合材料及制备方法:中国, CN101560326B [P].2011-01-19.[25]周春光,宋跃明,屠重棋,等. 多元氨基酸共聚物/磷酸钙复合材料椎间融合器的设计制备及压缩强度测试[J]. 生物医学工程学杂志, 2011, 28(6): 1136-1140.[26]Bell WH. Resorption Characteristics of Bone and Bone Substitutes. Oral Surg Oral Med Oral Pathol. 1964;17: 650-657.[27]姜星杰,吴小涛,张绍东,等. 硫酸钙骨水泥降解成骨性能的实验研究[J].中华创伤骨科杂志,2007, 9(8): 717-720.[28]普有登,汤逊. 硫酸钙骨移植替代材料的研究及应用进展[J].中国矫形外科杂志,2011,19(11): 931-933.[29]Carinci F, Piattelli A, Stabellini G, et al. Calcium sulfate: analysis of MG63 osteoblast-like cell response by means of a microarray technology. J Biomed Mater Res B Appl Biomater. 2004;71(2):260-267.[30]Sidqui M, Collin P, Vitte C, et al. Osteoblast adherence and resorption activity of isolated osteoclasts on calcium sulphate hemihydrate. Biomaterials. 1995;16(17):1327-1332.[31]Ricci JL,Weiner MJ,Iorio DD,et al. Evaluation of Timed Release Calcium Sulfate (CS-TR) Bone Graft Substitutes. Microscopy & Microanalysis. 2005; 11(11):1256-1257.[32]Palmieri A, Pezzetti F, Brunelli G, et al. Calcium sulfate acts on the miRNA of MG63E osteoblast-like cells. J Biomed Mater Res B Appl Biomater. 2008;84(2):369-374.[33]Walsh WR, Morberg P, Yu Y, et al. Response of a calcium sulfate bone graft substitute in a confined cancellous defect. Clin Orthop Relat Res. 2003;(406):228-236.[34]Lazáry A, Speer G, Varga PP, et al. Effect of vertebroplasty filler materials on viability and gene expression of human nucleus pulposus cells. J Orthop Res. 2008;26(5):601-607.[35]Dasmah A, Sennerby L, Rasmusson L, et al. Intramembraneous bone tissue responses to calcium sulfate: an experimental study in the rabbit maxilla. Clin Oral Implants Res. 2011;22(12):1404-1408.[36]Rauschmann MA, Wichelhaus TA, Stirnal V, et al. Nanocrystalline hydroxyapatite and calcium sulphate as biodegradable composite carrier material for local delivery of antibiotics in bone infections. Biomaterials. 2005;26(15): 2677-2684.[37]Mazurkiewicz T, Matuszewski L, Matuszewska A, et al. Implanted bisphosphonates in bone cement affect bone markers in rat serum. Int Orthop. 2013;37(5):969-974. |
| [1] | Yao Xiaoling, Peng Jiancheng, Xu Yuerong, Yang Zhidong, Zhang Shuncong. Variable-angle zero-notch anterior interbody fusion system in the treatment of cervical spondylotic myelopathy: 30-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1377-1382. |
| [2] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [3] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [4] | He Yunying, Li Lingjie, Zhang Shuqi, Li Yuzhou, Yang Sheng, Ji Ping. Method of constructing cell spheroids based on agarose and polyacrylic molds [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 553-559. |
| [5] | He Guanyu, Xu Baoshan, Du Lilong, Zhang Tongxing, Huo Zhenxin, Shen Li. Biomimetic orientated microchannel annulus fibrosus scaffold constructed by silk fibroin [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 560-566. |
| [6] | Chen Xiaoxu, Luo Yaxin, Bi Haoran, Yang Kun. Preparation and application of acellular scaffold in tissue engineering and regenerative medicine [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 591-596. |
| [7] | Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603. |
| [8] | Shen Jiahua, Fu Yong. Application of graphene-based nanomaterials in stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 604-609. |
| [9] | Zhang Tong, Cai Jinchi, Yuan Zhifa, Zhao Haiyan, Han Xingwen, Wang Wenji. Hyaluronic acid-based composite hydrogel in cartilage injury caused by osteoarthritis: application and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 617-625. |
| [10] | Li Hui, Chen Lianglong. Application and characteristics of bone graft materials in the treatment of spinal tuberculosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 626-630. |
| [11] | Gao Cangjian, Yang Zhen, Liu Shuyun, Li Hao, Fu Liwei, Zhao Tianyuan, Chen Wei, Liao Zhiyao, Li Pinxue, Sui Xiang, Guo Quanyi. Electrospinning for rotator cuff repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 637-642. |
| [12] | Chen Jinmin, Chen Suisheng, Ding Jing, Xia Baoquan, Luo Xiaojia, Lu Chenghai. Stability of balloon dilation with injectable calcium sulfate cement for tibial plateau fractures [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 414-418. |
| [13] | Guan Jian, Jia Yanfei, Zhang Baoxin , Zhao Guozhong. Application of 4D bioprinting in tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 446-455. |
| [14] | Huang Bo, Chen Mingxue, Peng Liqing, Luo Xujiang, Li Huo, Wang Hao, Tian Qinyu, Lu Xiaobo, Liu Shuyun, Guo Quanyi . Fabrication and biocompatibility of injectable gelatin-methacryloyl/cartilage-derived matrix particles composite hydrogel scaffold [J]. Chinese Journal of Tissue Engineering Research, 2022, 10(16): 2600-2606. |
| [15] | Liu Jiali, Suo Hairui, Yang Han, Wang Ling, Xu Mingen. Influence of lay-down angles on mechanical properties of three-dimensional printed polycaprolactone scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2022, 10(16): 2612-2617. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||