Chinese Journal of Tissue Engineering Research
Previous Articles Next Articles
Polyetheretherketone cage for treating type II and type IIa Hangman’s fractures: 6-month follow-up
Huang Yang-liang1, Zhong Yi2, Liu Shao-yu1
- 1Department of Spine Surgery, the First Affiliated Hospital of Sun Yat-sen University, Guangzhou 510700, Guangdong Province, China
2Department of Physiology, Guangzhou Medical University, Guangzhou 510000, Guangdong Province, China
-
Online:2015-09-24Published:2015-09-24 -
Contact:Huang Yang-liang, Department of Spine Surgery, the First Affiliated Hospital of Sun Yat-sen University, Guangzhou 510700, Guangdong Province, China -
About author:Huang Yang-liang, Master, Attending physician, Department of Spine Surgery, the First Affiliated Hospital of Sun Yat-sen University, Guangzhou 510700, Guangdong Province, China
CLC Number:
Cite this article
Huang Yang-liang, Zhong Yi, Liu Shao-yu. Polyetheretherketone cage for treating type II and type IIa Hangman’s fractures: 6-month follow-up[J]. Chinese Journal of Tissue Engineering Research, doi: 10.3969/j.issn.2095-4344.2015.39.013.
share this article
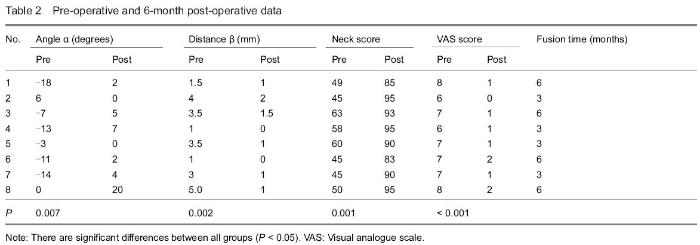
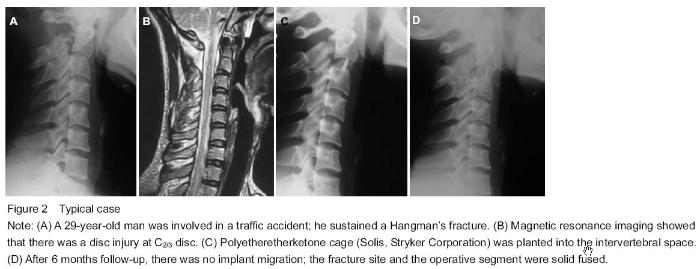
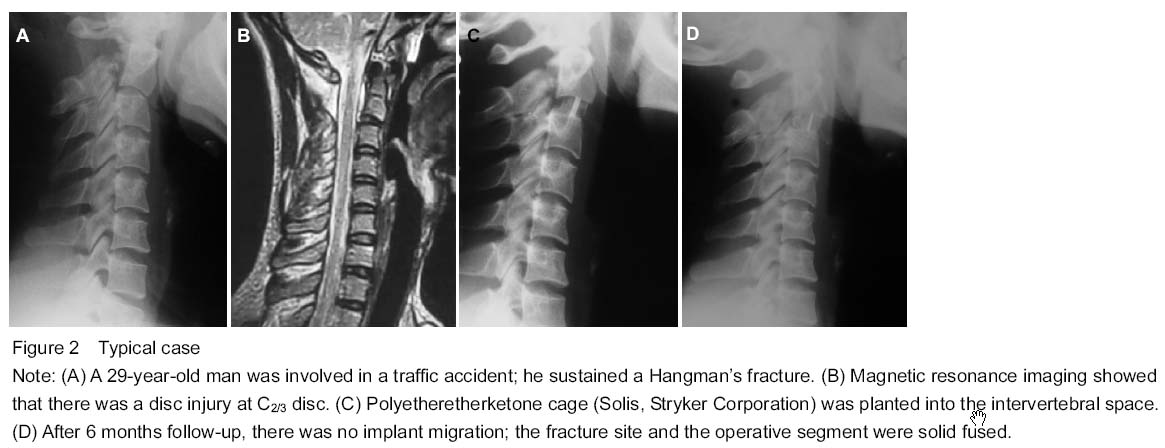
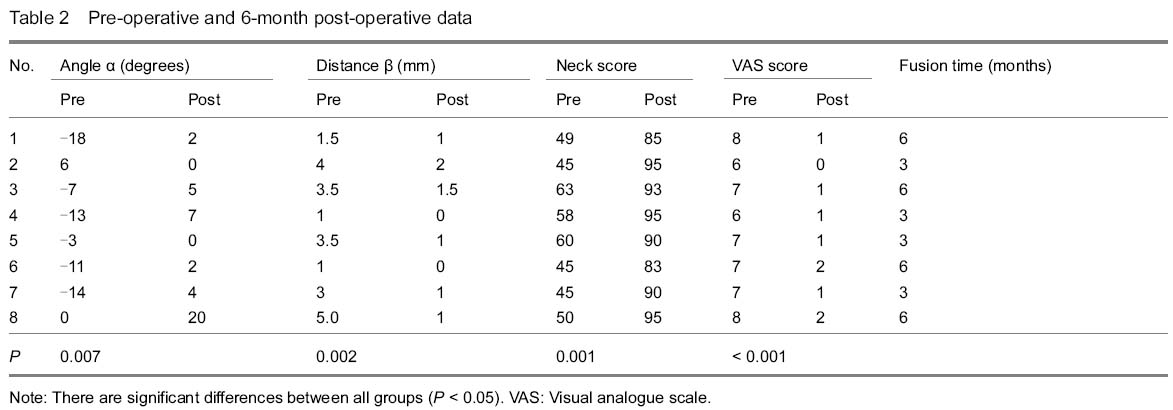
Quantitative analysis of participants Eight patients were collected at the beginning, and they were all successfully follow-up for 6 months or longer. None of them was lost, so their data were put into final statistical analysis. Clinical results The mean operative time was 97.0±21.4 minutes (range 70-135) and the mean hemorrhage amount was 31±10.5 mL (range 20-50). We did not observe transient or permanent hoarseness, dysphagia and dysphonia. By Smith and Robinson approach, lower part of axis body could be exposed without difficulty in all of our patients. There were no further operations. Of the total 8 consecutive patients, follow-up evaluation data of 6 months or longer were available for all patients at a mean clinical follow-up of 13.0±6.21 months (range 6-26). The Clinical Post-Traumatic Neck Score (Mayo) was 51.88±7.38 (range 45-63) pre-operatively and 90.75±4.68 (range 83-95) at 6-month follow-up. There was a significant improvement (P=0.001). The pre-operative VAS scale score was 7.00±0.76 (range 6-8) and 6-month post-operative score was 1.13±0.64 (range 0-2). There was a significant difference between pre and post-operative results (P < 0.001) (Table 2). In our 6-month post-operative questionnaires of Neck Score, no patients complained of cervical movement limitation that disturbed daily activities; and cervical pain was relieved, no further oral analgesics were needed. On last follow-up, there was no cervical pain recorded either. Radiographic results Cervical radiograph examinations performed at the last follow-up visits showed no subsidence, collapse, breaking, or pseudarthrosis at the level of the implants. There was no bone material absorption or necrosis at the contiguous vertebral bodies, and no noticeable inflammatory reaction. There were no lucency gaps between fracture lines. Fusion was observed after 3 or 6 months in all of our patients. The mean of angle deformity (α) pre-operatively was -7.50±8.05, and 6-month post-operatively was 5.00±6.52; the difference was significant (P=0.007). The mean of displacement distance (β) pre-operatively was 2.81±1.49, and 6-month post-operatively was 0.94±0.68, which was significant either (P=0.002) (Table 2)."
| [1] Müller EJ, Wick M, Muhr G. Traumatic spondylolisthesis of the axis: treatment rationale based on the stability of the different fracture types. Eur Spine J. 2000;9(5):123-128. [2] Ferro FP, Borgo GD, Letaif OB, et al. Traumatic spondylilisthesis of axis: epidemiology, management and outcome. Acta Ortop Bras. 2012;20(2):84-87. [3] Bransford RJ, Alton TB, Patel AR, et al. Upper cervical spine trauma. J Am Acad Orthop Surg. 2014;22(11):718-729. [4] Marcon RM, Cristante AF, Teixeira WJ, et al. Fractures of the cervical spine. Clinics (Sao Paulo). 2013;68(11):1455-1461. [5] Effendi B, Roy D, Cornish B, et al. Fractures of the ring of the axis: A classification based on the analysis of 131 cases. J Bone Joint Surg Br. 1981;63B(5):319-327. [6] Dalbayrak S, Yaman O. A coinsidence, a chance or a misfortune? Hangman's fracture. Neurol Neurochir Pol. 2014;48(4):305-307. [7] Levine AM, Edwards CC. The management of traumatic spondylolisthesis of the axis. J Bone Joint Surg Am. 1985;67(7):217-226. [8] Verheggen R, Jansen J. Hangman's Fracture: arguments in favor of surgical therapy for Type Ⅱand Ⅲ according to Edwards and Levine. Surg Neurol. 1998;49(5):253-262. [9] White AA, Panjabi MM. Clinical biomechanics of the spine. Lippincott, Philadephia, USA. 1978. [10] Li Z, Li F, Hou S, et al. Anterior discectomy/corpectomy and fusion with internal fixation for the treatment of unstable hangman's fractures: a retrospective study of 38 cases. J Neurosurg Spine. 2015;22(4):389-393. [11] Singh PK, Garg K, Sawarkar D, et al. Computed tomography-guided C2 pedicle screw placement for treatment of unstable hangman fractures. Spine (Phila Pa 1976). 2014;39(18):E1058-E1065. [12] Chowdhury FH, Haque MR. C1-C3 Lateral Mass Screw-Rod Fixation and Fusion for C2 Pathologies and Hangman's Fractures. Asian Spine J. 2014;8(6):735-746. [13] Jeong DH, You NK, Lee CK, et al. Posterior C2-C3 Fixation for Unstable Hangman's Fracture. Korean J Spine. 2013; 10(3): 165-169. [14] McAfee PC, Bohlman HH, Riley LH, et al. The anterior retropharyngeal approach to the upper part of the cervical spine. J Bone Joint Surg. 1987;69(6):1371-1383. [15] Park SH, Sung JK, Lee SH, et al. High anterior cervical approach to the upper cervical spine. Surg Neurol. 2007; 68(1):519-524. [16] Hur H, Lee JK, Jang JW, et al. Is it feasible to treat unstable hangman's fracture via the primary standard anterior retropharyngeal approach? Eur Spine J. 2014;23(8): 1641-1647. [17] Wison AJ, Marshall RW, Ewart M. Transoral fusion with internal fixation in a displaced hangman’s fracture. Spine. 1999;24(4):295-298. [18] Lin CN, Wu YC, Wang NP, et al. Preliminary experience with anterior interbody titanium cage fusion for treatment of cervical disc disease. Kaohsiung J Med Sci. 2003;19(4): 208-216. [19] McGrory BJ, Klassen RA. Arthrodesis of the cervical spine for fractures and dislocations in children and adolescents. A long-term follow-up study. J Bone Joint Surg Am. 1994; 76(10):1606-1616. [20] Truumees E, Demetropoulos CK, Yang KH, et al. Effects of disc height and distractive forces on graft compression in an anterior cervical discectomy model. Spine. 2002;33(9): 2441-2445. [21] Mastronardi L, Ducati A, Ferrante L. Anterior cervical fusion with polyetheretherketone (PEEK) cages in the treatment of degenerative disc disease, Preliminary observations in 36 consecutive cases with a minimum 12-month follow-up. Acta Neurochir (Wien). 2006.148(9):307-312. [22] Junaid M, Kalsoom A, Khalid M, et al. Cervical disc replacement with polyetheretherketone cages: clinical experience with 151 cases. J Ayub Med Coll Abbottabad. 2014;26(4):444-447. [23] Cho DY, Liau WR, Lee WY, et al. Preliminary experience using a polyetheretherketone (PEEK) cage in the treatment of cervical disc disease. Neurosurgery. 2002;51(3): 1343-1350. [24] Kim CH, Chung CK, Jahng TA, et al. Segmental kyphosis after cervical interbody fusion with stand-alone polyetheretherketone (PEEK) cages: a comparative study on 2 different PEEK cages. J Spinal Disord Tech. 2015; 28(1):E17-E24. [25] Li XF, Dai LY, Lu H, et al. A systematic review of the management of hangman’s fracture. Eur Spine J. 2006; 15(2):257-269. [26] Shin JJ, Kim SH, Cho YE, et al. Primary surgical management by reduction and fixation of unstable hangman's fractures with discoligamentous instability or combined fractures: clinical article. J Neurosurg Spine. 2013;19(5):569-575. [27] Watanabe M, Nomura T, Toh E, et al. Residual neck pain after traumatic spondylolisthesis of the axis. J Spinal Disord Tech. 2005;18(6):148-151. [28] Schofferman J, Garges K,Goldthwaite N, et al. Upper cervical anterior diskectomy and fusion improves discogenic cervical headaches. Spine. 2002;27(4): 2240-2244. [29] Heiko K, Anton K. Letter to the Editor concerning: A systematic review of the management of hangman’s fracture. Eur Spine J. 2006;15(2):1415-1418. [30] Lewkonia P, Dipaola C, Schouten R, et al. An evidence-based medicine process to determine outcomes after cervical spine trauma: what surgeons should be telling their patients. Spine (Phila Pa 1976). 2012;37(18):E1140- E1147. [31] Muthukumar N. C1-C3 lateral mass fusion for type Ⅱa and typeⅡI Hangman's fracture. J Craniovertebr Junction Spine. 2012;3(2):62-66. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Lu Dezhi, Mei Zhao, Li Xianglei, Wang Caiping, Sun Xin, Wang Xiaowen, Wang Jinwu. Digital design and effect evaluation of three-dimensional printing scoliosis orthosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1329-1334. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Yao Rubin, Wang Shiyong, Yang Kaishun. Minimally invasive transforaminal lumbar interbody fusion for treatment of single-segment lumbar spinal stenosis improves lumbar-pelvic balance [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1387-1392. |
| [5] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [6] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [7] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [8] | Zhang Wei, Hu Jiang, Tang Liuyi, Wan Lun, Yu Yang, Lin Shu, Tang Zhi, Wang Fei. Advantages of robot assisted percutaneous biopsy in the diagnosis of spinal lesions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 844-848. |
| [9] | He Li, Tian Wei, Xu Song, Zhao Xiaoyu, Miao Jun, Jia Jian. Factors influencing the efficacy of lumbopelvic internal fixation in the treatment of traumatic spinopelvic dissociation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 884-889. |
| [10] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [11] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [12] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [13] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [14] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [15] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||