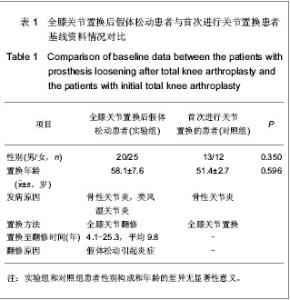
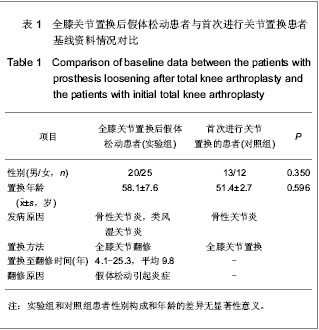
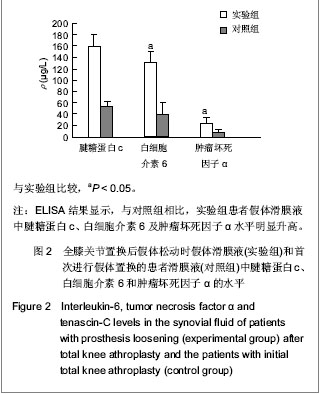
Chinese Journal of Tissue Engineering Research
Previous Articles Next Articles
Diagnostic markers in synovial fluid during prosthetic loosening after total knee arthroplasty
Zhao Xu-hong, Wu Ji, Li Song-lin, Chu Dong
- Department of the Orthopedics, General Hospital of Air Force of PLA, Beijing 100142, China
-
Received:2012-12-22Revised:2013-01-16Online:2013-06-25Published:2013-06-25 -
Contact:Wu Ji, M.D., Professor, Chief physician, Department of the Orthopedics, General Hospital of Air Force of PLA, Beijing 100142, China bjwuji@gmail.com -
About author:Zhao Xu-hong, Attending physician, Department of the Orthopedics, General Hospital of Air Force of PLA, Beijing 100142, China zhaoxuhong30@gmail.com
CLC Number:
Cite this article
Zhao Xu-hong, Wu Ji, Li Song-lin, Chu Dong. Diagnostic markers in synovial fluid during prosthetic loosening after total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, doi: 10.3969/j.issn.2095-4344.2013.26.005.
share this article

2.3 假体松动后假体滑膜液中腱糖蛋白c表达水平的变化 通过Western blot检测,发现全膝关节置换后假体松动时滑膜液中存在大的腱糖蛋白c可变体(包含FNIIIC结构域,相对分子质量为350 000),有比较明显的条带。 4F10TT抗体能够特异性的结合表皮生长因子样结构域,可检测到假体滑膜液中相对分子质量在所有210 000-350 000的所有腱糖蛋白c可变体[12]。最大的腱糖蛋白c可变体(L)相对分子质量为350 000。而最小的可变区(S),缺乏可选择性剪接FNIII重复结构域,相对分子质量为210 000[12],在实验中标记的效果很差。19C4MS能够特异性的结合较大的腱糖蛋白c可变,可检测到相对分子质量在350 000-240 000之间和 200 000之下的蛋白[12]。没有检测到19C4MS标记相对分子质量在210 000的腱糖蛋白c可变体,见图1。"
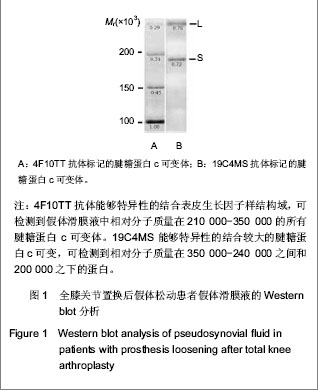

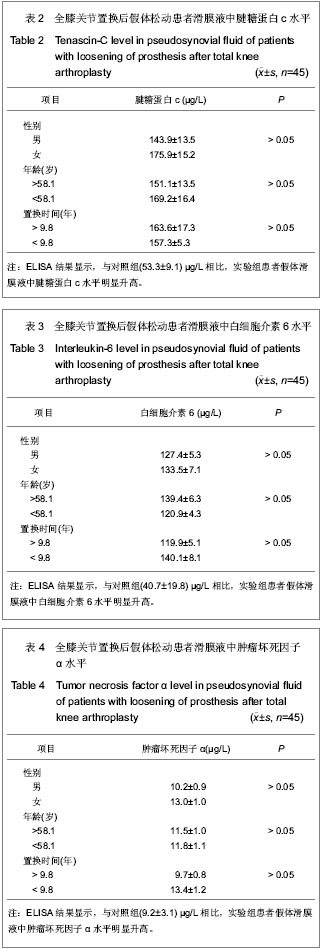
这些结果显示,由于假体松动导致翻修手术的患者,假体滑膜液中大的腱糖蛋白c可变体的表达水平明显升高。 2.4 假体松动后假体滑膜液中腱糖蛋白c、白细胞介素6和肿瘤坏死因子α表达水平的变化 ELISA定量检测患者全膝关节置换后假体松动时假体滑膜液中腱糖蛋白c的水平为(160.8±20.5) μg/L,大约是全膝关节置换后对照组的3倍,为(53.3±9.1) μg/L(P=0.036);假体滑膜液中白细胞介素6的水平为(130.1±19.6) ng/L,也是对照组的3倍(40.7±19.8) ng/L,(P=0.000 1);假体滑膜液中肿瘤坏死因子a的水平为(23.1±11.3) μg/L,大约为对照组的2.5倍(9.2±3.1) μg/L(P=0.000 3)。 在松动的人工关节的假体滑膜液中,腱糖蛋白c、白细胞介素6和肿瘤坏死因子α质量浓度见表2-4,这些因子的水平不受患者性别,年龄以及从首次置换手术至翻修手术时间的影响。"
| [1] Ingham E, Fisher J. The role of macrophages in osteolysis of total joint replacement. Biomaterials. 2005;26(11):1271-1286.[2] Wang CJ, Shi JF, Morgan C, et al. Design and simulation of a femoral component peg in total knee replacement. Key Eng Mater. 2011(450):111-114.[3] Harris WH. Wear and periprosthetic osteolysis: the problem. Clin Orthop Relat Res. 2001;(393):66-70.[4] Cobelli N, Scharf B, Crisi GM, et al. Mediators of the inflammatory response to joint replacement devices. Nat Rev Rheumatol. 2011;7(10):600-608. [5] Bottner F, Wegner A, Winkelmann W, et al. Interleukin-6, procalcitonin and TNF-alpha: markers of peri-prosthetic infection following total joint replacement. J Bone Joint Surg Br. 2007;89(1):94-99.[6] Konttinen YT, Li TF, Xu JW, et al. Expression of laminins and their integrin receptors in different conditions of synovial membrane and synovial membrane-like interface tissue. Ann Rheum Dis. 1999;58(11):683-690.[7] Li TF, Xu JW, Santavirta S, et al. Expression of vitronectin and its integrin receptors in the synovial membrane-like interface tissue from aseptic loosening of total hip replacement. J Rheumatol. 2000;27(3):727-734.[8] Konttinen YT, Li TF, Michelsson O, et al. Expression of tenascin-C in aseptic loosening of total hip replacement. Ann Rheum Dis. 1998;57(10):619-623.[9] Westacott CI, Sharif M. Cytokines in osteoarthritis: mediators or markers of joint destruction? Semin Arthritis Rheum. 1996; 25(4):254-272.[10] Shao JJ, Jiang Y, Zhang XL, et al. Shanghai Yixue. 2002;25 (S1): 30-32.邵俊杰,蒋垚,张先龙,等.白介素-6和转化生长因子-β1在膝骨关节炎发病中的作用[J].上海医学,2002,25(S1):30-32.[11] Botha-Scheepers S, Watt I, Slagboom E, et al. Innate production of tumour necrosis factor alpha and interleukin 10 is associated with radiological progression of knee osteoarthritis. Ann Rheum Dis. 2008;67(8):1165-1169.[12] Hasegawa M, Sudo A, Nagakura T, et al. Tenascin-C levels in pseudosynovial fluid of loose hip prostheses. Scand J Rheumatol. 200534(6):464-468.[13] Venn G, Nietfeld JJ, Duits AJ, et al. Elevated synovial fluid levels of interleukin-6 and tumor necrosis factor associated with early experimental canine osteoarthritis. Arthritis Rheum. 1993;36(6):819-826.[14] Li NH, Xue QY, Zhang Y, et al. ZHongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2008;12(33):6546-6549.李宁华,薛庆云,张毅,等.中国6个城市4577名中老年人手骨关节炎流行病学调查[J].中国组织工程研究与临床康复,2008, 12(33): 6546-6549.[15] Hasegawa M, Hirata H, Sudo A, et al. Tenascin-C concentration in synovial fluid correlates with radiographic progression of knee osteoarthritis. J Rheumatol. 2004;31(10): 2021-6.[16] Schmalzried TP, Jasty M, Harris WH. Periprosthetic bone loss in total hip arthroplasty. Polyethylene wear debris and the concept of the effective joint space. J Bone Joint Surg Am. 1992;74(6):849-863.[17] Grassmé H, Kirschnek S, Riethmueller J, et al. CD95/CD95 ligand interactions on epithelial cells in host defense to Pseudomonas aeruginosa. Science. 2000;290(5491): 527-530.[18] Zhao JN, Mei XL, Guo T, et al. Zhonghua Chuangshang Guke Zazhi. 2011;13(1):21-24.赵建宁,梅晓亮,郭亭,等.全髋关节置换术后血清白细胞介素6、10与纤维蛋白原表达的特点分析[J].中华创伤骨科杂志, 2011, 13(1):21-24.[19] Rettig WJ, Erickson HP, Albino AP, et al. Induction of human tenascin (neuronectin) by growth factors and cytokines: cell type-specific signals and signalling pathways. J Cell Sci. 1994; 107 ( Pt 2):487-497.[20] Imanaka-Yoshida K, Hiroe M, Yoshida T. Interaction between cell and extracellular matrix in heart disease: multiple roles of tenascin-C in tissue remodeling. Histol Histopathol. 2004; 19(2):517-525.[21] Järvinen TA, Jozsa L, Kannus P, et al. Mechanical loading regulates tenascin-C expression in the osteotendinous junction. J Cell Sci. 1999;112 Pt 18:3157-3166.[22] Chiquet M, Sarasa-Renedo A, Tunç-Civelek V. Induction of tenascin-C by cyclic tensile strain versus growth factors: distinct contributions by Rho/ROCK and MAPK signaling pathways. Biochim Biophys Acta. 2004;1693(3):193-204.[23] Imai S, Konttinen YT, Jumppanen M, et al. High levels of expression of collagenase-3 (MMP-13) in pathological conditions associated with a foreign-body reaction. J Bone Joint Surg Br. 1998;80(4):701-710.[24] Takei I, Takagi M, Santavirta S, et al. Matrix metalloproteinases and tissue inhibitors of metalloproteinases in joint fluid of the patients with loose artificial hip joints. J Biomed Mater Res. 1999;45(3):175-183.[25] Syggelos SA, Eleftheriou SC, Giannopoulou E, et al. Gelatinolytic and collagenolytic activity in periprosthetic tissues from loose hip endoprostheses. J Rheumatol. 2001; 28(6):1319-1329.[26] Siri A, Knäuper V, Veirana N, et al. Different susceptibility of small and large human tenascin-C isoforms to degradation by matrix metalloproteinases. J Biol Chem. 1995;270(15): 8650-8654.[27] Spring J, Beck K, Chiquet-Ehrismann R. Two contrary functions of tenascin: dissection of the active sites by recombinant tenascin fragments. Cell. 1989;59(2):325-334.[28] Weber P, Zimmermann DR, Winterhalter KH, et al. Tenascin-C binds heparin by its fibronectin type III domain five. J Biol Chem. 1995;270(9):4619-4623.[29] Day JM, Olin AI, Murdoch AD, et al. Alternative splicing in the aggrecan G3 domain influences binding interactions with tenascin-C and other extracellular matrix proteins. J Biol Chem. 2004;279(13):12511-12518. [30] Okamura N, Hasegawa M, Nakoshi Y, et al. Deficiency of tenascin-C delays articular cartilage repair in mice. Osteoarthritis Cartilage. 2010;18(6):839-848. [31] Nakoshi Y, Hasegawa M, Akeda K, et al. Distribution and role of tenascin-C in human osteoarthritic cartilage. J Orthop Sci. 2010;15(5):666-673. [32] Sofat N, Robertson SD, Hermansson M, et al. Tenascin-C fragments are endogenous inducers of cartilage matrix degradation. Rheumatol Int. 2012;32(9):2809-2817. |
| [1] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [2] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [3] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [4] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [5] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [6] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [7] | Yuan Mei, Zhang Xinxin, Guo Yisha, Bi Xia. Diagnostic potential of circulating microRNA in vascular cognitive impairment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1299-1304. |
| [8] | Liao Chengcheng, An Jiaxing, Tan Zhangxue, Wang Qian, Liu Jianguo. Therapeutic target and application prospects of oral squamous cell carcinoma stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1096-1103. |
| [9] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [10] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [11] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [12] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| [13] | Zhang Nianjun, Chen Ru. Analgesic effect of cocktail therapy combined with femoral nerve block on total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 866-872. |
| [14] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [15] | Yang Yang, Yao Yu, Shen Xiaotian, Liu Jiajia, Xue Jianhua. Expression and significance of interleukin-21 in intervertebral disc degeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 690-694. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||