Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (20): 3707-3714.doi: 10.3969/j.issn.2095-4344.2013.20.014
Previous Articles Next Articles
Pigment epithelium-derived factor inhibits corneal neovascularization after corneal alkali burn
Zhu Dan, Lu Xiao-he, Fu Yue
- Department of Ophthalmology, Zhujiang Hospital of Southern Medical University, Guangzhou 510282, Guangdong Province, China
-
Received:2012-11-17Revised:2013-01-21Online:2013-05-14Published:2013-05-14 -
Contact:Lu Xiao-he, Professor, Doctoral supervisor, Department of Ophthalmology, Zhujiang Hospital of Southern Medical University, Guangzhou 510282, Guangdong Province, China luxh63@ 163.com -
About author:Zhu Dan★, Studying for master’s degree, Department of Ophthalmology, Zhujiang Hospital of Southern Medical University, Guangzhou 510282, Guangdong Province, China 164028927@qq.com
CLC Number:
Cite this article
Zhu Dan, Lu Xiao-he, Fu Yue. Pigment epithelium-derived factor inhibits corneal neovascularization after corneal alkali burn [J]. Chinese Journal of Tissue Engineering Research, 2013, 17(20): 3707-3714.
share this article

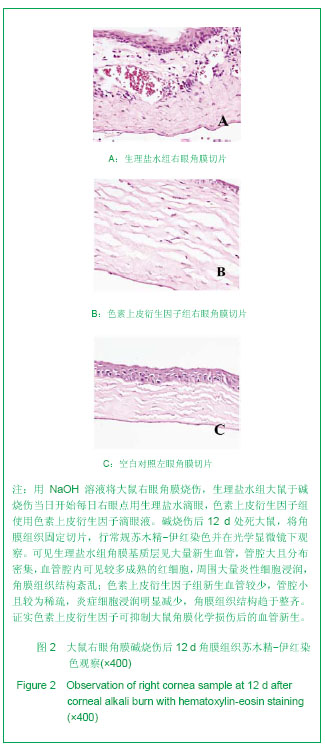
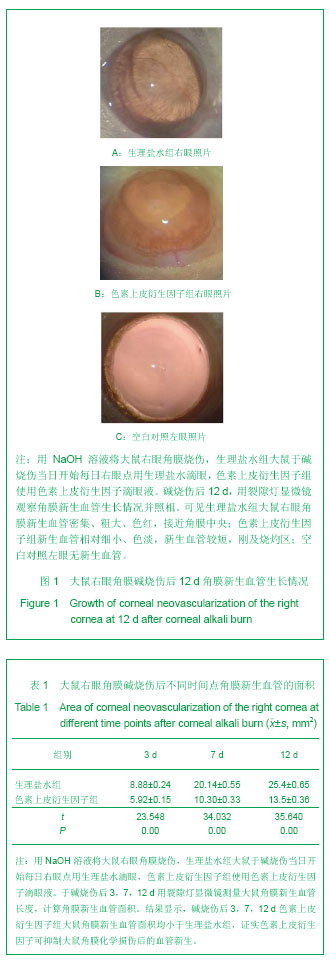
2.1 角膜新生血管的观察及宏观测量 大鼠右眼角膜碱烧伤后24 h,角膜缘血管网充盈,角膜中央浑浊水肿。3 d时,生理盐水组大鼠右眼角膜新生血管芽深入角膜缘,新生血管密集,在角膜上方呈刷状迅速生长;色素上皮衍生因子组角膜新生血管相对稀疏,长势较缓。7 d时,生理盐水组大鼠右眼角膜新生血管深入烧灼区,色素上皮衍生因子组未达烧灼区。12 d时,生理盐水组大鼠右眼角膜新生血管密集、粗大、色红,接近角膜中央;色素上皮衍生因子组角膜新生血管相对细小、色淡,新生血管较短,刚及烧灼区,见图1。各时间点角膜新生血管面积见表1。大鼠右眼角膜碱烧伤后3,7,12 d色素上皮衍生因子组大鼠角膜新生血管面积均小于生理盐水组,差异有显著性意义(P < 0.05)。"
| [1] Chang JH, Gabison EE, Kato T, et al. Corneal neovascularization. Curr Opin Ophthalmol. 2001;12(4): 242-249.[2] Peyman GA, Kivilcim M, Morales AM, et al. Inhibition of corneal angiogenesis by ascorbic acid in the rat model. Graefes Arch Clin Exp Ophthalmol. 2007;245:1461-1467.[3] Miller JW. Vascular endothelial growth factor and ocular neovascularization. Am J Pathol. 1997;151(1):13-23.[4] Dawson DW, Volpert OV, Gillis P, et al. Pigment epithelium-derived factor: a potent inhibitor of angiogenesis. Science. 1999;285(5425):245-248.[5] Kvanta A. Ocular angiogenesis: the role of growth factors. Acta Ophthalmol Scand. 2006;84:282-288.[6] Dorrell M, Usitalo-Jarvinen H, Aguilar E, et al. Ocular neovascularization: basic mechanisms and therapeutic advances. Surv Ophthalmol. 2007;52(Suppl):S3-S19.[7] Jimenez B, Volpert OV. Mechanistic insights on the inhibition of tumor angiogenesis. J Mol Med. 2001;78: 663-672.[8] Ambati BK, Nozaki M, Singh N, et al. Corneal avascularity is due to soluble VEGF receptor-1. Nature. 2006;443:993-997.[9] Spranger J, Osterhoff M, Reimann M, et al. Loss of the antiangiogenic PEDF in patients with angiogenic eye disease. Diabetes. 2001;50:2641-2645.[10] Gao G, Li Y, Zhang D, et al. Unbalanced expression of VEGF and PEDF in ischemia-induced retinal neovascularization. FEBS Lett. 2001;489(2-3):270-276.[11] Gao G, Ma J. Tipping the balance for angiogenic disorders. Drug Discov Today. 2002;7(3):171-172.[12] Amano S, Rohan R, Kuroki M, et al. Requirement for vascular endothelial growth factor in wound- and inflammation-related corneal neovascularization. Invest Ophthalmol Vis Sci. 1998; 39(1):18-22.[13] Tombran-Tink J, Johnson LV. Collagen-induced alterations in intercellular adhesion and antigen expression in retinoblastoma cells. Exp Eye Res. 1989;48(4):549-559.[14] Elahy M, Baindur-Hudson S, Dass CR. The emerging role of PEDF in stem cell biology. J Biomed Biotechnol. 2012;2012: 239091.[15] Yabe T, Sanagi T, Yamada H. The neuroprotective role of PEDF: implication for the therapy of neurological disorders. Curr Mol Med. 2010;10(3):259-266.[16] Tombran-Tink J. PEDF in angiogenic eye diseases. Curr Mol Med. 2010;10(3):267-278.[17] Kawaguchi T, Yamagishi SI, Sata M. Structure-function relationships of PEDF. Curr Mol Med. 2010;10(3):302-311.[18] Broadhead ML, Dass CR, Choong PF. In vitro and in vivo biological activity of PEDF against a range of tumors. Expert Opin Ther Targets. 2009;13(12):1429-1438.[19] Filleur S, Nelius T, de Riese W, et al. Characterization of PEDF: a multi-functional serpin family protein. J Cell Biochem. 2009;106(5):769-775.[20] Zhang SX, Ma JX. Ocular neovascularization: Implication of endogenous angiogenic inhibitors and potential therapy. Prog Retin Eye Res. 2007;26(1):1-37.[21] Duh EJ, Yang HS, Suzuma I, et al. Pigment epithelium-derived factor suppresses ischemia-induced retinal neovascularization and VEGF-induced migration and growth. Invest Ophthalmol Vis Sci. 2002;43(3):821-829.[22] Ueda S, Yamagishi SI, Okuda S. Anti-vasopermeability effects of PEDF in retinal-renal disorders. Curr Mol Med. 2010;10(3):279-283.[23] Jin J, Ma JX, Guan M, et al. Inhibition of chemical cautery-induced corneal neovascularization by topical pigment epithelium-derived factor eyedrops. Cornea. 2010; 29(9):1055-1061.[24] Stellmach V, Crawford SE, Zhou W, et al. Prevention of ischemia-induced retinopathy by the natural ocular antiangiogenic agent pigment epithelium-derived factor. Proc Natl Acad Sci USA. 2001;98(5):2593-2597.[25] Zhang SX, Wang JJ, Gao G, et al. Pigment epithelium-derived factor (PEDF) is an endogenous antiinflammatory factor. FASEB J. 2006;20(2):323-325.[26] Shi H, Yu HJ, Wang HY, et al. Topical administration of peroxiredoxin-6 on the cornea suppresses inflammation and neovascularization induced by ultraviolet radiation. nvest Ophthalmol Vis Sci. 2012;53(13):8016-8028.[27] Shin YJ, Nam WH, Park SE, et al. Aqueous humor concentrations of vascular endothelial growth factor and pigment epithelium-derived factor in high myopic patients. Mol Vis. 2012;18:2265-2270.[28] Chen HC, Yeh LK, Tsai YJ, et al. Expression of angiogenesis-related factors in human corneas after cultivated oral mucosal epithelial transplantation. Invest Ophthalmol Vis Sci. 2012;53(9):5615-5623. [29] Han Y, Shao Y, Lin Z, et al. Netrin-1 simultaneously suppresses corneal inflammation and neovascularization. Invest Ophthalmol Vis Sci. 2012;53(3):1285-1295.[30] Zhou Q, Yang L, Qu M, et al. Role of senescent fibroblasts on alkali-induced corneal neovascularization. J Cell Physiol. 2012; 227(3):1148-1156. [31] Jia C, Zhu W, Ren S, et al. Comparison of genome-wide gene expression in suture- and alkali burn-induced murine corneal neovascularization. Mol Vis. 2011;17:2386-2399. [32] Jin J, Ma JX, Guan M, et al. Inhibition of chemical cautery-induced corneal neovascularization by topical pigment epithelium-derived factor eyedrops. Cornea. 2010; 29(9):1055-1061.[33] Kuo CN, Yang LC, Yang CT, et al. Inhibition of corneal neovascularization with plasmid pigment epithelium-derived factor (p-PEDF) delivered by synthetic amphiphile INTeraction-18 (SAINT-18) vector in an experimental model of rat corneal angiogenesis. Exp Eye Res. 2009;89(5):678-685. [34] Feher J, Kovacs I, Pacella E, et al. Pigment epithelium-derived factor (PEDF) attenuated capsaicin-induced neurotrophic keratouveitis. Invest Ophthalmol Vis Sci. 2009;50(11):5173-5180.[35] Abdiu O, Van Setten G. Antiangiogenic activity in tears: presence of pigment-epithelium-derived factor. New insights and preliminary results. Ophthalmic Res. 2008;40(1):16-18.[36] Bock F, König Y, Kruse F, et al. Bevacizumab (Avastin) eye drops inhibit corneal neovascularization. Graefes Arch Clin Exp Ophthalmol. 2008;246:281-284.[37] Brown LF, Detmar M, Claffey K, et al. Vascular permeability factor/vascular endothelial growth factor: a multifunctional angiogenic cytokine. EXS. 1997;79:233-269.[38] Ferrara N, Gerber HP, LeCouter J. The biology of VEGF and its receptors. Nat Med. 2003;9:669-676.[39] Takahashi T, Ueno H, Shibuya M. VEGF activates protein kinase C-dependent, but Ras-independent Raf-MEK-MAP kinase pathway for DNA synthesis in primary endothelial cells. Oncogene. 1999;18:2221-2223.[40] Zwick E, Bange J, Ullrich A. Receptor tyrosine kinase signalling as a target for cancer intervention strategies. Endocr Relat Cancer. 2001;8:161-173.[41] Middleton J, Americh L, Gayon R, et al. A comparative study of endothelial cell markers expressed in chronically inflamed human tissues:MECA-79, Duffy antigen receptor for chemokines, von Willebrand factor,CD31, CD34, CD105 and CD146. J Pathol. 2005;206:260-268.[42] Apte RS, Barreiro RA, Duh E, et al. Stimulation of neovascularization by the anti-angiogenic factor PEDF. Invest Ophthalmol Vis Sci. 2004;45(12):4491-4497.[43] Takenaka K, Yamagishi S, Jinnouchi Y, et al. Pigment epithelium-derived factor (PEDF)-induced apoptosis and inhibition of vascular endothelial growth factor (VEGF) expression in MG63 human osteosarcoma cells. Life Sci. 2005;77(25):3231-3241.[44] Noel A, Jost M, Lambert V, et al. Anti-angiogenic therapy of exudative age-related macular degeneration: current progress and emerging concepts. Trends Mol Med. 2007; 13(8):345-352. [45] Zhang J, Huang C, Feng Y, et al. Comparison of beneficial factors for corneal wound-healing of rat mesenchymal stem cells and corneal limbal stem cells on the xenogeneic acellular corneal matrix in vitro. Mol Vis. 2012;18:161-173.[46] Venturi G, Gandini A, Monti E, et al. Lack of expression of SERPINF1, the gene coding for pigment epithelium-derived factor, causes progressively deforming osteogenesis imperfecta with normal type I collagen. J Bone Miner Res. 2012;27(3):723-728. |
| [1] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [2] | Yang Xin, Jin Zhe, Feng Xu, Lu Bing. The current situation of knowledge and attitudes towards organ, eye tissue, body donation of residents in Shenyang [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 779-784. |
| [3] | Cao Guolong, Tian Faming, Liu Jiayin. Lovastatin combined with insulin effects on fracture healing in rat models of bilateral ovariectomized type 2 diabetic mellitus [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 673-681. |
| [4] | Li Wenbo, Shi Jie, Shi Peisheng, Xue Yun, Huang Qiang, Li Chuangbing, Gao Qiuming. L-arginine promotes the survival of extended dorsal perforator skin flap through activating L-arginine-nitric oxide pathway [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(29): 4632-4637. |
| [5] | Liu Guoming, Wang Qinfen, Lin Kefeng, Zhou Shiguo, Chen Zuxing, Lin Shishui. Whole body application of nerve growth factor promotes early healing of tibial shaft fracture and improves expression of bone morphogenetic protein-2 and vascular endothelial growth factor in rats [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(29): 4680-4685. |
| [6] |
Geng Kang, Ding Xiaobin, Tian Xinli, Wang Xue, Yang Yuting, Yan Hong.
Electrical stimulation promotes wound healing and angiogenesis in diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4152-4156. |
| [7] | Xu Zhongzhong, Yu Xiaofei, Wang Liya. In vitro culture of human corneal epithelial stem cells using modified explant culture [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(25): 4012-4017. |
| [8] | Zhang Yuan, Zeng Min, Zhai Bo. Vitrification-based cryopreservation of tissues: strengths and existing problems [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(23): 3751-3755. |
| [9] | Zhao Jianfeng, Geng Yu, Chen Qianbo, Yang Jinghui, Li Yan. Changes in insulin resistance and inflammatory factors in cataract patients with glaucoma after phacoemulsification and trabeculectomy: a self-controlled trial [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(11): 1750-1755. |
| [10] | Liu Zhiling, Gao Minghong, Chen Yingxin. Bio-engineering cornea versus human donor cornea in the treatment of fungal corneal ulcer [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(10): 1563-1569. |
| [11] | Sun An, Bi Xiangyu, Han Xiangzhen, Zhou Qiqi, He Huiyu. Effects of vascular endothelial growth factor combined with platelet-derived growth factor-BB on the angiogenic and proliferative abilities of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(1): 1-6. |
| [12] | Zhang Jingyi, Hai Guodong, Yang Haofei, Fan Congliang, Yan Lei, Zhang Chunlei, Dou Junfeng, Ma Hailong. Changes in serum levels of fibroblast growth factor-2, hypoxia-inducible factor-1alpha and vascular endothelial growth factor in patients with avascular necrosis of femoral head treated by enriched autologous bone marrow stem cell transplantation combined with core decompression [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(1): 14-14. |
| [13] | Yang Xiongfeng, Jiang Huijiao, Wang Xiaoyi, Guo Lijiao, Zhou Qing, Han Huanhuan, Li Linlin, Liao Zhenyu, Lei Zhen, Chen Xueling, Zhang Hongwei, Wu Xiangwei. An increase in proliferation of rat bone mesenchymal stem cells and secretion of vascular endothelial growth factor under negative pressure in vitro [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(1): 33-39. |
| [14] | Wang Yifei, Song Yang, Guan Yongge, Xu Chunyan. Bone marrow mesenchymal stem cell transplantation in a rat model of thin endometrium based on HOXA10 regulatory network [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(9): 1397-1402. |
| [15] | Gao Kun1, Zhu Wenxiu2, Li Heng1, Liu Weidong1, Li Quan1, Yu Weiji1, Wang Lixin1, Cao Yafei1. Exosomes in serum of ovariectomized rats promote primary osteoblast proliferation [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(7): 958-989. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||