Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (18): 3405-3412.doi: 10.3969/j.issn.2095-4344.2013.18.024
Previous Articles Next Articles
Autologous muscle transplantation for reconstruction of artificial anal sphincter
Zhang Qin-liang
- Fengtian Hospital Affiliated to Shenyang Medical College, Shenyang 110024, Liaoning Province, China
-
Received:2012-10-18Revised:2013-02-27Online:2013-04-30Published:2013-04-30 -
About author:Zhang Qin-liang★, Master, Associate chief physician, Fengtian Hospital Affiliated to Shenyang Medical College, Shenyang 110024, Liaoning Province, China zql_168@163.com
CLC Number:
Cite this article
Zhang Qin-liang. Autologous muscle transplantation for reconstruction of artificial anal sphincter[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(18): 3405-3412.
share this article

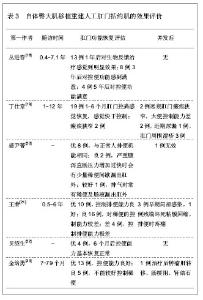
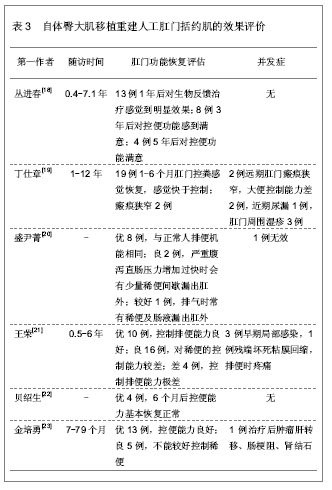
2.1 自体臀大肌移植重建人工肛门括约肌 2.1.1 自体臀大肌移植重建人工肛门括约肌的解剖学基础 臀大肌为臀肌中最表浅的肌肉组织,轮廓宽厚,具有广泛的起止点,起于髂后上棘,臀后线和髂棘之间的一部分髂骨及腰背筋膜,骶结节韧带的背面,骶骨、尾骨外侧线和骶部韧带,肌纤维斜向外下,有相互平行的2个缘,臀大肌的下1/4附着于股骨臀肌转子,臀大肌滑囊将肌腱于股骨大转子分开,其余3/4呈带状腱膜,与阔筋膜张肌的带状腱膜联合,形成髂胫束下行,最后附着于胫骨外髁[11-14]。臀大肌上缘长约10.9 cm,上缘中点肌层厚约1.2 cm,下缘长约12.6 cm,下缘中点肌层厚约2.4 cm,起、止点宽约11.0 cm[15]。臀大肌的作用是参与髋关节伸与旋外,下肢固定时,能伸直躯干,固定骨盆,防止躯干前倾,对于维持人体直立姿势和肢体运动具有重要的作用[16]。 臀大肌的血液供应相当丰富,有从髂内动脉分出的臀上动脉,从梨状肌上缘传出后分成深、浅两支,浅支在臀大肌深面入臀大肌,供应臀大肌和臀上部皮肤及皮下脂肪组织,深支在臀中肌深面走行,供应臀中肌。臀下动脉也是髂内动脉的分支,在骶结节韧带的外侧,从梨状肌下缘出来,穿过臀大肌深面到其止点,主要分布于臀大肌下部及股后部。此外,臀大肌远侧部分尚有来自旋股外侧动脉的第一穿动脉,旋股内侧动脉横支及旋股外返动脉横支的吻合支供养。臀上、臀下动脉均有相应的静脉和神经伴行[17]。 臀大肌血管分布类型中,Ⅰ型占67%,臀大肌上份由臀上动脉供给,下份由臀下动脉供给,中份由臀上、下动脉共同供给;Ⅱ型占18%,臀大肌上份和中份由臀上动脉供给,下份由臀下动脉供给;Ⅲ型占9%,臀上动脉供给臀大肌上份,臀下动脉供给臀大肌中、下份;Ⅳ型占4%,臀下动脉缺如,臀大肌全部由臀上动脉供给;Ⅴ型占2%,臀上动脉供给臀大肌上、中、下份,臀下动脉与阴部内动脉共干的细支供给臀大肌下份。 根据臀大肌在体表的投影轮廓选取移植肌肉组织,臀大肌上内方的臀肌与骶骨交界,内下方的臀下皱襞形成,下外侧臀部与大腿交界,中外侧臀部与髋部交界。内下方为臀下皱襞,上端起源于臀间沟,为臀部开始从中线分离的起始处,为臀肌的2/3或3/4处,此分离线呈45°偏离中线,终止于臀部中线或略外侧。下外侧臀部与大腿过渡,中外侧臀部与髋部移行自然,部分伴有外侧凹陷。 2.1.2 自体臀大肌移植重建人工肛门括约肌的临床应用 从臀大肌肌瓣的解剖学基础可以看出,其下部肌瓣解剖位置与肛提肌邻近,可以分离出足够大小和厚度的带蒂肌瓣供重建肛门括约肌应用,游离后的肌瓣仍能保存完整的血管和神经纤维,并具有良好的收缩功能。因此,应用臀大肌下部肌瓣移植重建肛门括约肌具有解剖学基础和依据,利用带蒂的臀大肌瓣代替肛门括约肌,具有移植操作简单、移植组织容易获得、安全、创伤小等优点,不但能保证移植肌瓣的血液供应和神经支配,而且还具有肛括约肌的功能。文章对自体臀大肌移植重建人工肛门括约肌的患者进行随访观察,大部分为直肠癌患者,也有肛瘘或其它原因导致肛门失禁患者以及肛门失禁经过治疗后仍不能较好的控制排便或引起肛门狭窄导致肛门括约肌控排便功能障碍患者,其中直肠癌患者给予肿瘤切除联合肛门括约肌重建治疗,而其它原因导致肛门失禁者给予臀大肌移植重建肛门括约肌治疗,移植后可给予加强肛周肌肉力量的反馈训练,以及改善肛门括约肌控排便的协调性反馈训练等干预措施,以利于肛门括约肌控排便功能的早期恢复,具体分析见表1-3。"
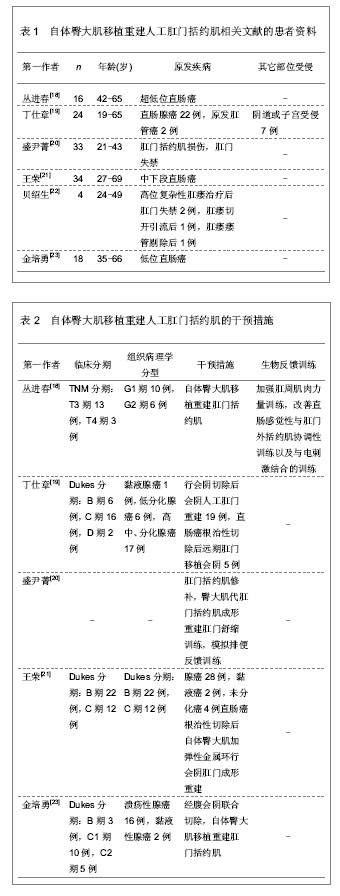
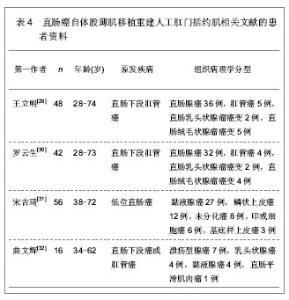
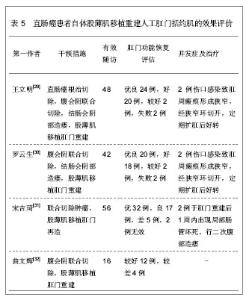
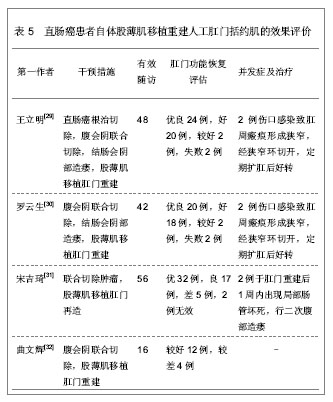
2.2 自体股薄肌移植重建人工肛门括约肌 2.2.1 自体股薄肌移植重建人工肛门括约肌的解剖学基础 股薄肌是位于大腿内侧扁薄的带状肌,以腱膜起自耻骨下支,向下于耻骨内上髁平面移行为条索状肌腱,最后以扇形放散,止于胫骨转子内侧[24]。股薄肌全长(42.0±0.6) cm,肌腹长(31.0±3.8) cm,肌腱长(10.9±0.9) cm[25]。股薄肌位于大腿内侧,位置表浅,部位隐蔽,有众多协同肌,切取后对大腿的内收功能影响不大,肌瓣具有正常肌的抗拉力和张力,血管神经蒂长,获取操作简便易行,是理想的供肌[26]。 股薄肌血供丰富,为多源性,有股深动脉的股薄肌支、旋股内侧动脉、闭孔动脉和膝降动脉等。供血于股薄肌中、上部的动脉,以来自股深动脉股薄肌支占绝大多数,约为96%,多数从股深动脉内侧壁和前壁发出,发出后恒定向下斜行于长收肌的深面,在股薄肌中上1/3交界点外侧2.0-3.0 cm处,由其主干发出3、4个分支,分布于股薄肌。与之伴行的静脉多数为双支少数为单支。供血于股薄肌下部的血管绝大多数来自膝降动脉。股薄肌上、中、下段之间的动脉吻合丰富,结扎切断该肌的中、下端来源动脉,肌瓣血供可通过血管吻合沟通。 支配股薄肌的神经均来自闭孔神经前支的分支,该神经进入大腿后,在长收肌与短收肌之间向内下斜行,逐渐与股薄肌的主要血管伴行,形成血管神经束,在股薄肌中上1/3交界处前缘深部进入肌肉[27-28]。 2.2.2 自体股薄肌移植重建人工肛门括约肌的临床应用 股薄肌和肛门外括约肌都是横纹肌,但股薄肌没有持续耐疲劳的能力,而来自肛门外括约肌的神经供应可以使股薄肌的酶和代谢发生改变,具有耐疲劳的能力,经过神经压榨的去肌膜股薄肌既可以达到暂时去神经的状态,接受外来神经的再生和支配,建立双重神经支配,又可以避免失去神经的肌肉出现萎缩、纤维化。此外,移植的肌肉可以和平滑肌直接接触,肌电活动相互影响,从而使移植的肌肉更容易达到较好的肛门外括约肌功能。 文章对自体股薄肌移植重建人工肛门括约肌的直肠癌患者进行随访观察,患者多为直肠下段肛管癌,肿瘤组织病理学分型中以直肠腺癌占大多数,鳞状上皮癌和未分化癌等患者较少,经过肿瘤根治性切除联合自体股薄肌移植重建人工肛门括约肌治疗后,肛门括约肌控排便功能恢复较好,大部分患者可恢复肛门括约肌控排便功能,较少患者出现肛门狭窄以及肛周感染的并发症,经过相应对症处理后均可好转,能够恢复人工肛门括约肌的控排便功能,具体分析见表4、5。"
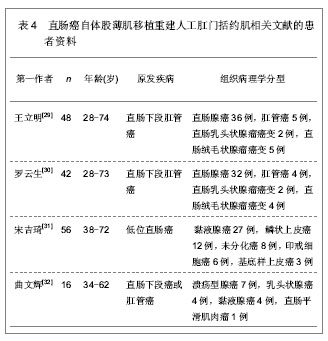
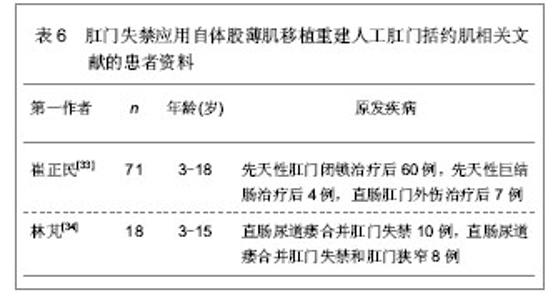
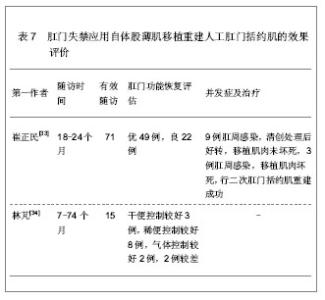
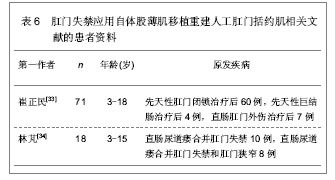
文章研究显示直肠癌患者在肿瘤切除时联合自体股薄肌移植重建人工肛门括约肌能够获得较好的肛门排控便功能,是理想的人工肛门重建自体移植肌肉组织。而对于其它原因导致的肛门失禁以及肛门闭锁、肛门狭窄等,应用自体股薄肌移植重建人工肛门括约肌同样能够恢复较好的肛门排控便功能,获得满意的移植效果。崔正民等[33]和林芃等[34]分别对先天性肛门闭锁、先天性巨结肠治疗后肛门失禁、外伤性肛门失禁以及直肠尿道瘘合并肛门失禁的儿童患者进行自体股薄肌移植重建人工肛门括约肌的治疗随访,患者年龄3-18岁,经自体股薄肌移植重建人工肛门括约肌治疗后,可恢复较好的控排便功能,移植后可能发生肛周感染引起移植肌肉组织坏死等并发症,从而导致肛门括约肌重建失败,因此,在移植治疗后因密切观察肛周的感染情况,一旦发生肛周感染,应立即给予相应处理,避免感染加重导致移植肌肉组织坏死,减轻患者的痛苦,具体结果见表6、7。"
| [1] 艾中立,袁玉峰.肛门括约肌损伤的诊治[J].临床外科杂志, 2007, 15(2):82-83.[2] Foley F. An artificial sphincter; a new device and operation for control of enuresis and urinary incontinence. J Urol. 1947; 58(4):250-259.[3] Scott FB, Bradley WE, Timm GW. Treatment of urinary incontinence by an implantable prosthetic urinary sphincter. 1974. J Urol. 2002;167(2 Pt 2):1125-1129; discussion 1130.[4] Heiblum M, Cordoba A. An artificial sphincter: a preliminary report. Dis Colon Rectum. 1978;21(8):562-566. [5] Christiansen J, Lorentzen M. Implantation of artificial sphincter for anal incontinence. Report of five cases. Dis Colon Rectum. 1989;32(5):432-436.[6] Christiansen J, Sparsø B. Treatment of anal incontinence by an implantable prosthetic anal sphincter. Ann Surg. 1992;215 (4):383-386.[7] Banik RK, Subieta AR, Wu C, et al. Increased nerve growth factor after rat plantar incision contributes to guarding behavior and heat hyperalgesia. Pain. 2005;117(1-2):68-76.[8] 刘利兵.人工肛门括约肌的材料学特征及其临床应用[J].中国组织工程研究与临床康复,2010,14(29):5427-5430. [9] 中国知网.中国学术期刊总库[DB/OL].2013-1-10. https://www.cnki.net[10] 万方数据库.万方数据知识服务平台[DB/OL].2013-1-10. http://www.wanfangdata.com.cn/ [11] 汪良能,高学书.整形外科学[M].北京:人民卫生出版社,1989: 191-192.[12] 王启华,孙博.临床解剖学丛书四肢分册[M].北京:人民卫生出版社, 1996:236-246.[13] 武勇进,刘立刚.臀大肌肌皮瓣的基础研究与临床应用[J].中国实用美容整形外科杂志,2005,16(2):112-114.[14] 张春雷,张建平,蒋纯志.臀大肌肌皮瓣的解剖学特点及临床应用[J].医学综述,2011,17(12):1821-1823.[15] 许家洲,薛黔.臀大肌的肌构筑学研究[J].四川解剖学杂志,2009, 17(1):25-26.[16] 吴先国.人体解剖学[M].北京:人民卫生出版社,2004:83.[17] 洪志坚.臀部美学和应用解剖[J].中国美容医学,2009,18(6): 879-881.[18] 丛进春,陈春生,张宏,等.超低位直肠癌行臀大肌替代部分括约肌重建肛门[J].中国肿瘤临床,2007,34(14):807-810.[19] 丁仕章.肛门括约肌复合重建术在直肠肛管癌治疗中的应用[J].陕西肿瘤医学,2002,10(1):46-47.[20] 盛尹菁.肛门失禁综合手术治疗12例体会[J].中国实用医药, 2010, 5(1):167.[21] 王荣,王红军.臀大肌瓣加弹性金属环行肛门成形术[J].中国普外基础与临床杂志,2003,10(6):605-606.[22] 贝绍生,丁克,王建新.臀大肌转移修补治疗肛瘘术后肛门括约肌缺损[J].中华外科杂志,2010,48(11):872-873.[23] 金培勇,王亚力,韩国新,等.直肠下段癌根治术后一侧臀大肌代肛管括约肌的治疗体会[J].泰山医学院学报,2002,23(2):163.[24] 吴樾,田奉宸,刘庚辰,等.带血管蒂股薄肌瓣的应用解剖[J].解剖学杂志,2005,28(3):328.[25] 马大军,谭宏,刘亚国,等.带血管神经蒂股薄肌瓣重建尿道括约肌的应用解剖[J].中国临床解剖学杂志,2001,19(2):131-133.[26] 舒先涛,许本柯,周文明,等.股薄肌神经血管门的应用解剖[J].解剖与临床,2005,10(1):28-29.[27] 史松,刘浩.股薄肌应用解剖学特点及在重建外科中的临床应用[J].实用医学杂志,2006,22(24):2937-2938.[28] 毛增荣,黄瀛,施思娟,等.股薄肌及其血管神经的显微外科解剖[J].第二军医大学学报,1980,1(1):18-23.[29] 王立明,罗云生,刘作金,等.二期股薄肌移植肛门成形术48例分析[J].重庆医学,2001,30(4):348-349.[30] 罗云生,单治堂.二期股薄肌移植肛门成形术体会[J].第三军医大学学报,2001,23(2):223,226.[31] 宋吉琦,孙广增.双侧股薄肌代括约肌原位肛门再造术的疗效分析[J].河南外科学杂志,2001,7(2):143-144.[32] 曲文辉.直肠癌腹会阴切除股薄肌肛门成形术[J].中外健康文摘, 2011,8(3):115-116.[33] 崔正民,陈维秀,陈雨历,等.股薄肌转移代肛门外括约肌重建术治疗大便失禁[J].临床小儿外科杂志,2005,4(6):414-416.[34] 林芃,陈雨历,谢义德.小儿直肠尿道瘘的修补与肛门括约肌重建术[J].中华整形外科杂志,2001,17(4):225-226.[35] 张在东,曾升明,邓小明,等.股薄肌代肛门括约肌治疗外伤性大便失禁一例[J].中国修复重建外科杂志,2001,15(6):337.[36] 潘斯俭,伍尚敏,李允怡,等.股薄肌代肛门括约肌治疗先天性巨结肠术后大便失禁1例[J].昆明医学院学报,2005,26(1):137-138.[37] Altomare DF, Dodi G, La Torre F, et al. Multicentre retrospective analysis of the outcome of artificial anal sphincter implantation for severe faecal incontinence. Br J Surg. 2001;88(11):1481-1486.[38] Benoist S, Panis Y, Michot F, et al. Artificial sphincter with colonic reservoir for severe anal incontinence because of imperforate anus and short-bowel syndrome: report of a case. Dis Colon Rectum. 2005;48(10):1978-1982.[39] Conzo G, Brancaccio U, Esposito MG, et al. Surgical treatment of fecal incontinence secondary to obstetric trauma. Ann Ital Chir. 2006;77(3):241-246; discussion 246.[40] Parker SC, Spencer MP, Madoff RD, et al. Artificial bowel sphincter: long-term experience at a single institution. Dis Colon Rectum. 2003;46(6):722-729.[41] Luo Y, Higa M, Amae S, et al. Preclinical development of SMA artificial anal sphincters. Minim Invasive Ther Allied Technol. 2006;15(4):241-245.[42] Schrag HJ, Ruthmann O, Doll A, et al. Development of a novel, remote-controlled artificial bowel sphincter through microsystems technology. Artif Organs. 2006;30(11):855-862.[43] 黄成良,李明月,郑均.结肠套叠臀大肌原位肛门重建50例报告[J].咸宁学院学报(医学版),2003,17(3):193-194.[44] 吴仕光,李殿波,吕军吉,等.带蒂臀大肌束环绕下拉结肠重建肛门外括约肌功能的应用[J].癌症,1999,18(S1):117.[45] Kiene S. Reconstructive gluteus maximus muscle pedicled flaps in the treatment of resistant fistulae of the pelvic organs. Rozhl Chir. 2000;79(12):636-639.[46] Pak-Art R, Silapunt P, Bunaprasert T, et al. Prospective, randomized, controlled trial of proximally based vs. distally based gluteus maximus flap for anal incontinence in cadavers. Dis Colon Rectum. 2002;45(8):1100-1103.[47] Rasmussen OØ. Fecal incontinence. Studies on physiology, pathophysiology and surgical treatment. Dan Med Bull. 2003; 50(3):262-282.[48] da Silva GM, Jorge JM, Belin B, et al. New surgical options for fecal incontinence in patients with imperforate anus. Dis Colon Rectum. 2004;47(2):204-209.[49] 秦荣,罗云生,单治堂.直肠癌根治会阴部造口术后二期股薄肌移植肛门成形[J].消化外科,2005,4(2):84-86. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Liang Yan, Zhao Yongfei, Xu Shuai, Zhu Zhenqi, Wang Kaifeng, Liu Haiying, Mao Keya. Imaging evaluation of short-segment fixation and fusion for degenerative lumbar scoliosis assisted by highly selective nerve root block [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1423-1427. |
| [3] | Yuan Jiawei, Zhang Haitao, Jie Ke, Cao Houran, Zeng Yirong. Underlying targets and mechanism of Taohong Siwu Decoction in prosthetic joint infection on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1428-1433. |
| [4] | Wan Ran, Shi Xu, Liu Jingsong, Wang Yansong. Research progress in the treatment of spinal cord injury with mesenchymal stem cell secretome [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1088-1095. |
| [5] | Li Shanshan, Guo Xiaoxiao, You Ran, Yang Xiufen, Zhao Lu, Chen Xi, Wang Yanling. Photoreceptor cell replacement therapy for retinal degeneration diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1116-1121. |
| [6] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [7] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [8] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [9] | Zhang Nianjun, Chen Ru. Analgesic effect of cocktail therapy combined with femoral nerve block on total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 866-872. |
| [10] | Luo Xuanxiang, Jing Li, Pan Bin, Feng Hu. Effect of mecobalamine combined with mouse nerve growth factor on nerve function recovery after cervical spondylotic myelopathy surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 719-722. |
| [11] | Yang Xin, Jin Zhe, Feng Xu, Lu Bing. The current situation of knowledge and attitudes towards organ, eye tissue, body donation of residents in Shenyang [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 779-784. |
| [12] | Li Chenjie, Lü Linwei, Song Yang, Liu Jingna, Zhang Chunqiu. Measurement and statistical analysis of trabecular morphological parameters of titanium alloy peri-prosthesis under preload [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 516-520. |
| [13] | Zhou Jihui, Yao Meng, Wang Yansong, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Influence of novel nanoscaffolds on biological behaviors of neural stem cells and the related gene expression [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 532-536. |
| [14] | Li Quanxi, Shen Yu, Wan Wei, Sun Shanzhi. Changes of abdominal wall mechanics and pain after tension-free inguinal hernia repair with polypropylene mesh [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 548-552. |
| [15] | Song Kaikai, Zhang Kai, Jia Long. Microenvironment and repair methods of peripheral nervous system injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 651-656. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||