Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (7): 1180-1184.doi: 10.3969/j.issn.2095-4344.2013.07.008
Previous Articles Next Articles
Tensile and compressive mechanical property of human bone tissue
Wang Shang-cheng1, Wang Dong-mei1, Wang Fang2, Wang Qiu-gen2, Wang Chun-hui3, Chen Shan-guang3
- 1 School of Mechanical Engineering, Shanghai Jiao Tong University, Shanghai 200240, China
2 The First Affiliated People’s Hospital, Shanghai Jiao Tong University, Shanghai 200240, China
3 China Astronaut Training Center, Beijing 100094, China
-
Received:2012-10-18Revised:2012-10-20Online:2013-02-12Published:2013-02-12 -
About author:Wang Shang-cheng★, Studying for master’s degree, School of Mechanical Engineering, Shanghai Jiao Tong University, Shanghai 200240, China boyang@sjtu.edu.cn Wang Dong-mei☆, Doctor, Associate professor, School of Mechanical Engineering, Shanghai Jiao Tong University, Shanghai 200240, China dmwang@sjtu.edu.cn Wang Shang-cheng and Wang Dong-mei contributed equally to this paper.
CLC Number:
Cite this article
Wang Shang-cheng, Wang Dong-mei, Wang Fang, Wang Qiu-gen, Wang Chun-hui, Chen Shan-guang. Tensile and compressive mechanical property of human bone tissue[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(7): 1180-1184.
share this article
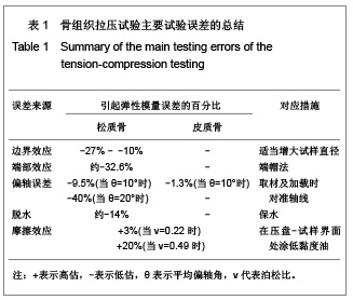
1 试样制备 1.1 骨试样的取材方向 旧规范对取材方向不重视。实际上骨表现为各向异性,测试轴线应与材料主方向重合,以形成在轴加载,否则将出现偏轴效应[1,10]。松质骨的力学各向异性方向和结构主方向几乎重合,因此松质骨组织根据骨小梁的结构主方向来确定试样轴向,皮质骨则根据哈弗氏系统的结构方向来确定,偏轴角需减小到10°以下[11-12]。 1.2 试样尺寸 1.2.1 符合连续体假设 骨组织的宏观力学性能测试基于连续性和均匀假设。皮质骨试样尺寸至少应含有几个基本的加强单元和定向结构即哈弗氏系统[2]。松质骨是骨小梁相互交织组成的网状固体,试样则须包含至少5个骨小梁及其间距时才符合连续体假设。 1.2.2 试样尺寸的选择 立方块或长方块骨试样适合测量骨的单轴或多轴压缩模量及各向异性,且易加工,但只能用压盘方法压缩。压盘法所用试样几何尺寸的不同,带来的端部效应和摩擦误差就不同,因此实验结果是依赖于尺寸的[14-16]。 圆柱试样适用端帽法压缩和拉伸,端帽法下的摩擦和端部效应已经锐减,Lievers等[17]的研究表明试验结果已独立于纵横比,但由于边界效应的影响,结果仍受直径影响,且大直径带来误差较小[18]。考虑到骨实际尺寸,推荐直径为5-10 mm、测试长度-直径比为2∶1(不应小于1∶1)并且测试长度最小为10 mm的规格[1,17]。 哑铃状试样也叫狗骨头状试样,是理想的拉伸试样形状,但往往只能在大骨头上获得[19-20],中段截面积减小即为缩颈,横截面可为圆形或长方形。缩颈设计使标距端的应力大于其他节段,有利于保证断裂优先发生在标距段而不是端部。圆弧式缩颈较斜线式缩颈更能减小夹持区附近的应力集中,防止在过渡处发生断裂[19]。 1.3 试样加工 在选定取材方向和设计好试样最终尺寸后,即可规划试样加工流程。对于哑铃试样,宜用切片机切出皮质骨平片,平整后再用端铣刀铣出圆弧或斜线缩颈。对圆柱试样,用钻床上的空心钻刀即可钻取松质骨芯。加工骨头时用金刚石涂层的刀具,采用低切削速率和不断的液体冷却来防止骨过热。失败的加工包括试样瘢痕、过热烧灼或者取材的过度偏轴。 1.4 骨髓的处理与否 骨髓在孔隙内的黏性流动会对骨力学性能的测量产生影响。当应变率低于1应变每秒时,骨髓的流动不会显著影响骨的刚度和强度[21]。准静态测试是以低应变率加载试样,所取试样中的骨髓不必去除,但高速测试则需考虑髓脂的影响。 1.5 冰冻保存 骨组织离体后就开始发生组织自溶,对其力学性能产生不可逆转的破坏。在-20 ℃下冰冻保存并且确保骨内水分的情况下,骨组织的力学性能没有较明显变化[22]。冰冻过的试样在拉压测试前在磷酸化生理盐水中常温解冻数小时以重新水合。 2 拉压测试 2.1 测试温度和保水 一般认为温度和水合将影响骨的力学性能。理论上骨试样温度维持在37 ℃。实际上将温度设定在24 ℃左右,此时弹性模量只比在37 ℃时高出2%-4%[23],可见误差是非常小的。然而室温下脱水将使松质骨的表观弹性模量下降约14%[24],故需采取措施减缓骨组织的脱水,如包裹湿纱布等。 2.2 试样装夹 试样尺寸的设计决定了采用何种装夹方式,如长方块试样采用压盘法压缩,圆柱试样可采用端帽法拉压或压盘法,哑铃试样则直接夹具夹持端部以拉压。 传统压缩测试多采用压盘方法,即把试样直接置于两个平行压盘之间压缩[6]。这种方法简单易行,对长方块试样很实用。但端部效应及摩擦会带来20%-40%的误差。因此尽量不用压盘法压缩,或者采取措施减少误差,见表1。"
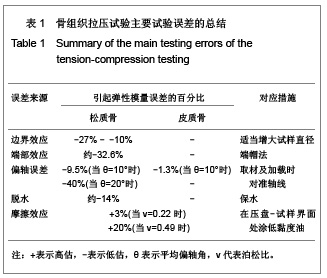

针对压盘方法的不足,Keaveny等[5]设计出端帽法。端帽法是把端部粘到预先对准的铜端帽里或者做端帽状包埋来约束端部,从而提供可靠的装夹面。铜端帽通过特殊胶和试样黏合,然后夹到试验机V形装夹口中以拉压。 2.3 加载控制 试样装夹好后需进行预调,可使骨组织达到黏弹性稳定状态。由于骨组织的黏弹性,卸载后有残余应变,一般通过5-15个循环后即可稳定[6]。预调时应变不应超过屈服应变[25-26],以免黏弹性稳定前试样就发生塑形破坏。加载和卸载速率根据研究目的确定,可用位移控制或力控制。试验过程中试验机自动记录载荷信息,同时位移采集设备采集位移。 2.4 应变测量 由于端部效应和摩擦的存在,试样变形直接用测试机框架的移动来替代会带来较大误差,宜采用电子引伸计或者数字散斑相关技术等来测量。引伸计由夹在试样表面的两夹头直接感知试样的变形[5,24]。数字散斑技术对板状拉伸试样尤其适用,其原理是通过数字相关算法处理图像序列,确定试样变形前后对应的几何点,从而确定位移及应变[27]。"


3 数据处理获得力学参数 3.1 应力-应变曲线 完成实验后,取骨黏弹性稳定后的试验数据来构建载荷-位移曲线或者应力-应变曲线,从而得出骨的力学性能参数。载荷-位移曲线与应力-应变曲线相似,但应力-应变曲线独立于试样尺寸,很好反映了材料的内在性能。应力-应变曲线的初始阶段在误差少时为线性,应力-应变成比例变化,满足虎克定律;越过屈服点进入塑性变形阶段,最终试样达到最大应力就开始发生断裂。 3.2 屈服强度和弹性模量的确定 由应力-应变曲线可得到弹性模量、屈服强度和屈服应变、极限应力和韧性等[28],这些量在相关书中都有定义,数据处理方法也基本相同,但屈服应力和弹性模量则需要特别处理。 屈服应力:屈服是指应力不增加,而应变却显著增加,材料好像不能抵抗变形的现象。骨组织拉压时不呈现明显的屈服,屈服点推荐按工程常用方法来定义,即在0.2%应变点处作一条平行与弹性模量定义线的斜线[29],斜线与曲线的交点即为屈服点。 弹性模量:通常弹性模量定义为曲线初始线性段的斜率,用线性拟合得出。但当初始段的非线性较强时,弹性模量定义的误差能放大传递到屈服强度的定义中去;为使定义屈服点的误差最小,宜用二次方程来拟合应力-应变曲线的0-0.2%应变部分并取原点处的切线斜率为弹性模量[29]。"


5 总结 骨组织的拉压测试看似简单和直接,却很容易受试样制备、测试方法、环境条件和数据处理的影响。如果按标准操作,不同研究之间便易对比,或许模量-密度关系能得到更准确的反映,而不是非常离散地分布。 本文回答了骨组织的拉压试验准备与执行、数据处理和误差评估等关键问题,对误差来源和误差减少技术进行了重点介绍。以往骨组织力学性能测试的研究较多是简单地照抄材料力学中的典型方法,殊不知旧方法存在很大缺陷和系统误差,急需整理和解决争议,在减少误差的宗旨下尝试解决骨力学性能测试的标准问题[33]。本文潜在的误差来源和误差大小。要知道当要求高精度分析(如材料敏感性分析)和研究对比时,试验误差的减小和规范就变得格外重要[34-35]。因此,本文论述了骨组织拉压测试的最新进展,对少误差的方法做了重点介绍,有助于此类试验的正确开展。 致谢:感谢上海市第一人民医院骨科刘锐和王倞对试验标准问题和作者的讨论。 基金资助:国家重点基础研究发展计划(973计划)(2011CB711000);国家自然科学基金资助项目(81071234);上海市松江区卫生局经费资助项目(2011LX14)。 作者贡献:第一作者构思并设计文章,同时分析并解析相关数据,经导师王冬梅副教授修改,所有作者共同起草,第一作者对本文负责。 利益冲突:课题未涉及任何厂家及相关雇主货其他经济组织直接或间接的经济或利益的赞助。 伦理要求:无涉及伦理冲突的内容。 作者声明:文章为原创作品,数据准确,内容不涉及泄密,无一稿两投,无抄袭,无内容剽窃,无作者署名争议,无与他人课题以及专利技术的争执,内容真实,文责自负。"

| [1] Keaveny TM, Morgan EF, Niebur GL, et al. Biomechanics of trabecular bone. Annu Rev Biomed Eng. 2001;3:307-333.[2] Reilly DT, Burstein AH. The Mechanical properties of cortical bone. J Bone Joint Surg Am. 1974;56:1001-1022.[3] Ozcivici E, Ferreri S, Qin YX, et al. Determination of bone’s mechanical matrix properties by nanoindentatio. Methods Mol Biol. 2008;455:323-334.[4] Helgason B, Perilli E, Schileo E, et al. Mathematical relationships between bone density and mechanical properties: A literature review. Clin Biomech. 2008;23:135-146.[5] Keaveny TM, Pinilla TP, Crawford RP, et al. Systematic and random errors in compression testing of trabecular bone. J Orthop Res. 1997;15:101-110.[6] Linde F, Gøthgen CB, Hvid I, et al. Mechanical properties of trabecular bone by a non-destructive compression testing approach. Eng Med. 1988;17(1):23-29.[7] Turner CH, Burr DB. Basic biomechanical measurements of bone: a tutorial. Bone. 1993;14(4):595-608.[8] Aspden RM. Mechanical testing of bone ex vivo. Methods Mol Med. 2003;80:369-379.[9] Beaupied H, Lespessailles E, Benhamou CL. Evaluation of macrostructural bone biomechanics. Joint Bone Spine. 2007; 74:233-239.[10] Chen XM, Zhao YF. Huaxi Yike Daxue Xuebao. 1991; 22(2): 171-174. 陈新民,赵云凤.人体下颌骨的偏轴应力-应变关系研究[J].华西医科大学学报,1991,22(2):171-174.[11] Wirtz DC, Schiffers N, Pandorf T, et al. Critical evaluation of known bone material properties to realize anisotropic FE-simulation of the proximal femur. J Biomech. 2000;33 (10):1325-1330.[12] Ohman C, Baleani M, Perilli E, et al. Mechanical testing of cancellous bone from the femoral head:experimental errors due to off-axis measurements. J Biomech. 2007;40(11): 2426-2433.[13] Harrigan TP,Jasty M,Mann RW,et al. Limitations of the continuum assumption in cancellous bone. J Biomech. 1988; 21:269-275.[14] Linde F,Hvid I,Madsen F. The effect of specimen geometry on the mechanical behaviour of trabecular bone specimens. J Biomech. 1992;25:359-368.[15] Keaveny TM,Borchers RE,Gibson LJ,et al. Theoretical analysis of the experimental artifact in trabecular bone compressive modulus. J Biomech. 1993;26(9):599-607.[16] Keaveny TM, Borchers RE, Gibson LJ, et al. Trabecular bone modulus and strength can depend on specimen geometry. J Biomech. 1993;26(8):991-995.[17] Lievers WB, Waldman SD, Pilkey AK. Minimizing specimen length in elastic testing of end-constrained cancellous bone. J Mech Behav Biomed Mater. 2010;3(1):22-30.[18] Lievers WB, Petryshyn AC, Poljsak AS, et al. Specimen diameter and “side artifacts” in cancellous bone evaluated using end-constrained elastic tension. Bone. 2010;47: 371-377.[19] Feng L, Jasiuk I. Effect of specimen geometry on tensile strength of cortical bone. J Biomed Mater Res Part A. 2010; 95A(20):580-587.[20] Carter DR, Caler WE, Spengler DM, et al. Fatigue behavior of adult cortical bone: the influence of mean strain and strain range. Acta Orthop Scand.1981;52:481-490.[21] Carter DR, Hayes WC. The compressive behavior of bone as a two-phase porous structure. J Bone Joint Surg Am. 1977; 59:954-962.[22] Martin RB, Sharkey NA. Mechanical effects of postmortem changes, preservation, and allograft bone treatments. In: Bone Mechanics Handbook, Cowin, S. C. (Ed.). CRC Press, Florida. 2001:(20-1)-(20-24).[23] An YH, Bensen CV. General considerations of mechanical testing, In: Mechanical Testing of Bone and the Bone-Implant Interface, Yuehuei H. An,Robert A. Draughn. CRC Press. Florida.2000:119-131.[24] Lievers WB, Poljsak AS, Waldman SD, et al. Effects of dehydration-induced structural and material changes on the apparent modulus of cancellous bone. Med Eng Phys. 2010; 32(8):921-925.[25] Morgan EF, Keaveny TM. Dependence of yield strain of human trabecular bone on anatomic site. J Biomech. 2001; 34:569-577.[26] Bayraktar HH, Morgan EF, Niebur GL,et al. Comparison of the elastic and yield properties of human femoral trabecular and cortical bone tissue. Journal Biomech. 2004;37:27-35.[27] Pan B, Qian K, Xie HM,et al. Two-dimensional digital image correlation for in-plane displacement and strain measurement: a review. Meas Sci Technol. 2009;20:062001.[28] Kalouche I, Crépin J, Abdelmoumen S, et al. Mechanical properties of glenoid cancellous bone. Clin Biomech (Bristol, Avon). 2010;25(4):292-298.[29] Morgan EF, Yeh OC, Chang WC, et al. Nonlinear behavior of trabecular bone at small strains. J Biomech Eng. 2001;123 (1):1-9.[30] Bevill G, Easley SK, Keaveny TM. Side-artifact errors in yield strength and elastic modulus for human trabecular bone and their dependence on bone volume fraction and anatomic site. J Biomech. 2007;40(15): 3381-3388.[31] Odgaard A, Linde F. The underestimation of Young's modulus in compressive testing of cancellous bone specimen. J Biomech.1991;24(8):691-698.[32] Turner CH,Cowin SC.Errors induced by off-axis measurement of the elastic properties of bone. J Biomech. 1988;110:213-215.[33] Wu SQ. Zhongbei Daxue Xuebao: Ziran Kexueban. 2012; 33(2):216-220. 吴淑琴. 股骨皮质骨生物力学特性研究[J].中北大学学报:自然科学版,2012,33(2):216-220.[34] Ruan WD, Xue Y. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchang Kangfu. 2010; 14(43):8113-8116. 阮文东,雪原.股骨头的力学测定:实验与方法[J].中国组织工程研究与临床康复, 2010, 14(43):8113-8116.[35] Cristofolini L, Schileo E, Juszczyk M, et al. Mechanical testing of bones: the positive synergy of finite-element models and in vitro experiments. Philos Transact A Math Phys Eng Sci. 2010; 368(1920):2725-2763. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [3] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [4] | Luo Lin, Song Naiqing, Huang Jin, Zou Xiaodong. Review and prospect of international research on preschool children’s movement development assessment: a CiteSpace-based visual analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1270-1276. |
| [5] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [6] | Cai Qunbin, Zou Xia, Hu Jiantao, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei. Relationship between tip-apex distance and stability of intertrochanteric femoral fractures with proximal femoral anti-rotation nail: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 831-836. |
| [7] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [8] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [9] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Comparison of the advantages and disadvantages of multiple implants in treatment of traumatic dislocation of sternoclavicular joint [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 443-448. |
| [10] | Nie Shaobo, Li Jiantao, Sun Jien, Zhao Zhe, Zhao Yanpeng, Zhang Licheng, Tang Peifu. Mechanical stability of medial support nail in treatment of severe osteoporotic intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 329-333. |
| [11] | Tan Jiachang, Yuan Zhenchao, Wu Zhenjie, Liu Bin, Zhao Jinmin. Biomechanical analysis of elastic nail combined with end caps and wire fixation for long oblique femoral shaft fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 334-338. |
| [12] | Chen Lu, Zhang Jianguang, Deng Changgong, Yan Caiping, Zhang Wei, Zhang Yuan. Finite element analysis of locking screw assisted acetabular cup fixation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 356-361. |
| [13] | Liu Yulin, Li Guotai. Combined effects of hyperbaric oxygen, vibration training and astaxanthin on bone mineral density, glucose metabolism and oxidative stress in diabetic osteoporosis rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3117-3124. |
| [14] | Li Yuanyuan, Lu Yingjuan, Ye Yushan, Mustafa M.M Weldali, Chang Shaohai. Constructing finite element models of three maxillary arch forms [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3125-3129. |
| [15] | Liu Jiahui, Zhang Zhongjiu, Jia Dianxiang, Zhai Aoqing, Niu Guangyun, Jiang Haibo. Research status and clinical application of artificial knee joint testing machine [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2895-2901. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

