Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (32): 5158-5163.doi: 10.3969/j.issn.2095-4344.1982
Previous Articles Next Articles
Application of three-dimensional digital operation planning to individualized adolescent idiopathic scoliosis surgery
-
Online:2019-11-18Published:2019-11-18 -
Contact:Li Xiaohe, MD, Professor, Master’s supervisor, Department of Human Anatomy, Basic Medical School, Inner Mongolia Medical University, Huhhot 010010, Inner Mongolia Autonomous Region, China Li Zhijun, Master, Professor, Master’s supervisor, Department of Human Anatomy, Basic Medical School, Inner Mongolia Medical University, Huhhot 010010, Inner Mongolia Autonomous Region, China -
About author:Fu Yu, MD, Chief physician, Department of Spine, the Second Affiliated Hospital of Inner Mongolia Medical University, Huhhot 010010, Inner Mongolia Autonomous Region, China Zhang Yunfeng, Master, Associate chief physician, Department of CT Center, the Second Affiliated Hospital of Inner Mongolia Medical University, Huhhot 010010, Inner Mongolia Autonomous Region, China Fu Yu and Zhang Yunfeng contributed equally to this work. -
Supported by:the National Natural Science Foundation of China, No. 81560348, 81260269, 81550042 (to LZJ), No. 81460330 (to LXH)| the Youth Elite of Science and technology of Inner Mongolia Autonomous Region Colleges and Universities “Young Science and Technology Talents Program”, No. NJYT-15-B05 (to LXH)| the Inner Mongolia Autonomous Region Science and Technology Plan Project (2016) (to LXH)| the Natural Science Foundation of Inner Mongolia Autonomous Region, No. 2016MS08131 (to LXH)| the Science and Technology Innovation Leading Project of Inner Mongolia Autonomous Region (2017) (to LXH)| the Fund for Returnees from the Department of Human Resources and Social Security of Inner Mongolia Autonomous Region (to LXH)
CLC Number:
Cite this article
Fu Yu, Zhang Yunfeng, Su Baoke, Zhao Yan, Xin Daqi, Wang Haiyan, Xu Yangyang, Zhang Cong, Wang Yidan, Wang Xing, Gao Shang, En He, Cai Yongqiang, Wang Jianzhong, Wang Zhiqiang, Gao Mingjie, Li Zhijun, Ma Jierong, Li Xiaohe. Application of three-dimensional digital operation planning to individualized adolescent idiopathic scoliosis surgery[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(32): 5158-5163.
share this article
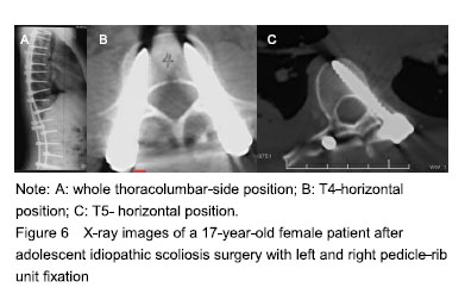
Digital virtual visual reconstruction for AIS The spine of the AIS patient could be reconstructed using the preoperative thoracolumbar thin-section CT scan data and 3D reconstruction software. The 3D morphology of the spine was clearly displayed, and could be observed from any angle as needed. The internal structure and boundaries of the bone were also clearly displayed after transparency processing (Figure 2). Digital virtual visual planning for AIS A screw placement plan was developed from three angles using the 3D rotation and transparency processing functions in the reverse engineering module of the 3D digital reconstruction software. Comprehensive virtual operation planning was achieved in the software (screw diameter, lateral angle, upward (downward) angle, and screw insertion length (screw path length) (Figure 6). Postoperation follow-up The success rate of screw placement in AIS patients was significantly improved with the development of the digital virtual operation planning system. Of the 24 thoracic pedicle screws placed according to the preoperative digital screw placement plan, 16 were grade I, and 6 were grade II and penetrated the lateral wall. No screws were grade III or IV. All screws met the placement requirements. No surrounding soft tissues and vital structures were damaged. The 6 screws that penetrated the lateral wall were all placed in accordance with the pedicle fixation method, and all penetrated the pedicle wall by less than 2 mm. The patient was followed up for 16 to 24 months. No screw loosening occurred, rendering a 100% success rate of screws placement (Figure 6). Biocompatibility analysis Since the use of screws was an existing long-term clinically used production-licensed product, its adverse reactions and biocompatibility were in line with clinical studies, and no related adverse reactions had been reported. "
| [1]Choo QQ, Chiu CK, Lisitha KA,et al. Quantitative analysis of local bone graft harvested from the posterior elements during posterior spinal fusion in adolescent idiopathic scoliosis patients. J Orthop. 2019;16(1):74-79.[2]Demura S, Yaszay B, Bastrom TP, et al. Is decompensation preoperatively a risk in Lenke 1C curves? Spine. 2013;38(11):E649-E655.[3]Aya KL, Yngve D, Charls RM. Acute appendicitis after spine fusion for adolescent idiopathic scoliosis: a case report. Cureus. 2018;10(10):e3522.[4]Xia C, Xu L, Xue B, et al. Rare variant of HSPG2 is not involved in the development of adolescent idiopathic scoliosis: evidence from a large-scale replication study. 2019;20(1):24.[5]Ghayem-Hasankhani E, Omidi-Kashani F. Generalized ligamentous laxity; a parameter should not to be forgotten in preoperative planning of adolescent idiopathic scoliosis. Iran Red Crescent Med J. 2012;14(11):702-704.[6]Bastrom TP, Yaszay B, Shah SA, et al. Major complications at two years after surgery impact srs scores for adolescent idiopathic scoliosis patients. Spine deform. 2019;7(1):93-99.[7]Blanco JS, Perlman SL, Cha HS et al. Multimodal pain management after spinal surgery for adolescent idiopathic scoliosis. Orthopedics. 2013;36:33-35.[8]Lonner BS, Ren Y, Bess S, et al. Surgery for the adolescent idiopathic scoliosis patients after skeletal maturity: early versus late surgery. Spine deform. 2019;7(1):84-92.[9]Pasha S, Sankar WN, Castelein RM. The Link between the 3D spino-pelvic alignment and vertebral body morphology in adolescent idiopathic scoliosis. Spine deform. 2019;7(1):53-59.[10]Moon ES, Kim HS, Sharma V, et al. Analysis of single nucleotide polymorphism in adolescent idiopathic scoliosis in Korea: for personalized treatment. Yonsei Med J. 2013;54(2):500-509.[11]Etemadifar MR, Andalib A, Rahimian A, et al. Cobalt chromium-Titanium rods versus Titanium-Titanium rods for treatment of adolescent idiopathic scoliosis; which type of rod has better postoperative outcomes? Rev Assoc Med Bras (1992). 2018;64(12):1085-1090.[12]Mao S, Xu L, Zhu Z, et al. Association between genetic determinants of peak height velocity during puberty and predisposition to adolescent idiopathic scoliosis. Spine. 2013;38(12):1034-1039.[13]Acar B, Us AK. Results of a new correction technique in surgical treatment of idiopathic scoliosis: mid-term clinical and radiological outcomes. Cureus. 2018;10(10):e3454.[14]Illés T, Somoskeöy S. Comparison of scoliosis measurements based on three-dimensional vertebra vectors and conventional two-dimensional measurements: advantages in evaluation of prognosis and surgical results. Eur Spine J. 2013;22(6):1255-1263.[15]Benke B, Marada G, Tunyogi Csapó M, et al. Comparing the function of the temporomandibular joint before and after surgical treatment in a young patient with idiopathic scoliosis. Case presentation. Orv Hetil. 2018;159(50):2144-2149.[16]Trobisch PD, Samdani AF, Betz R, et al. Sagittal balance and compensatory mechanism after segmental instrumentation for adolescent idiopathic scoliosis. Z Orthop Unfall. 2012;150(6):583-587.[17]Zhang M, Li F, He Y, et al. Registration of brainstem surfaces in adolescent idiopathic scoliosis using discrete Ricci flow. Medical image computing and computer-assisted intervention: MICCAI International Conference on Medical Image Computing and Computer-Assisted Intervention. 2012;15(Pt 2):146-154.[18]Fan Q, Xie H, Ma Z, et al. Perioperative predictors of moderate and severe postoperative pain in idiopathic scoliosis patients following spinal correction and fusion operations. Medicine. 2018;97(46):e13215.[19]Snowden RD, Prusick VW, Oeffinger DJ, et al. Increased acute postoperative wound problems following spinal fusion in overweight patients with adolescent idiopathic scoliosis. J Pediatr Orthop B. 2019;28(4):374-379.[20]Choi DE, Vives MJ, Shah H, et al. Do postoperative drain volumes correlate with intraoperative blood loss and postoperative transfusion requirements in posterior spinal fusion for adolescent idiopathic scoliosis? J Pediatr Orthop B. 2019;28(4):368-373.[21]Ck C, Kj L, Wh C, et al. Does the severity of the curve in lenke 1 and 2 adolescent idiopathic scoliosis patients affect the distance and position of the aorta from vertebra? Spine. 2019;44(11):785-792.[22]Malik AT, Kim J, Yu E, et al. Predictors of a non-home discharge destination following spinal fusion for adolescent idiopathic scoliosis (AIS). Spine. 2019; 44(8):558-562.[23]Ovadia D, Drexler M, Kramer M, et al. Closed wound subfascial suction drainage in posterior fusion surgery for adolescent idiopathic scoliosis: a prospective randomized control study. Spine. 2019;44(6):377-383.[24]Chan CYW, Mohamad SM, Tan SH, et al. Do overweight adolescent idiopathic scoliosis (ais) patients have an increased perioperative risk for posterior spinal fusion (PSF) surgery? A propensity score matching analysis of 374 AIS patients. Spine. 2019;44(6):389-396.[25]Kwan MK, Chiu CK, Hasan MS, et al. Perioperative outcome of single stage posterior spinal fusion for severe adolescent idiopathic scoliosis (AIS) (Cobb Angle ≥90°): the role of a dual attending Surgeon strategy. Spine. 2019;44(6):E348-E356.[26]Uehara M, Takahashi J, Ikegami S, et al. Prediction of spontaneous lumbar curve correction after posterior spinal fusion for adolescent idiopathic scoliosis lenke type 1 curves. Clin Spine Surg. 2019;32(2):E112-E116.[27]Abousamra O, Sponseller P D, Lonner BS, et al. Thoracic lordosis, especially in males, increases blood loss in adolescent idiopathic scoliosis. J Pediatr Orthop. 2019;39(3):e201-e204.[28]Kakar RS, Li Y, Brown CN, et al. Spine and lower extremity kinematics exhibited during running by adolescent idiopathic scoliosis patients with spinal fusion. Spine Deform. 2019;7(2):254-261.[29]Holewijn RM, De Kleuver M, Kingma I, et al. A prospective analysis of motion and deformity at the shoulder level in surgically treated adolescent idiopathic scoliosis. Gait Posture. 2019;69:150-155.[30]Rapp Van Roden EA, Richardson RT, Russo SA, et al. Analysis of shoulder complex function after posterior spinal fusion in adolescents with idiopathic scoliosis. J Pediatr Orthop. 2019;39(1):e32-e38. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Lu Dezhi, Mei Zhao, Li Xianglei, Wang Caiping, Sun Xin, Wang Xiaowen, Wang Jinwu. Digital design and effect evaluation of three-dimensional printing scoliosis orthosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1329-1334. |
| [3] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [4] | Liu Zhengpeng, Wang Yahui, Zhang Yilong, Ming Ying, Sun Zhijie, Sun He. Application of 3D printed interbody fusion cage for cervical spondylosis of spinal cord type: half-year follow-up of recovery of cervical curvature and intervertebral height [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 849-853. |
| [5] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [6] | Xu Junma, Yu Yuechao, Liu Zhi, Liu Yu, Wang Feitong. Application of 3D-printed coplanar template combined with fixed needle technique in percutaneous accurate biopsy of small pulmonary nodules [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 761-764. |
| [7] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [8] | Huang Youyi, Yuan Wei. Application of 3D printing technology in fracture and deformity of foot and ankle [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 438-442. |
| [9] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [10] | Wu Xuehai, Wang Xing, Zhang Shaojie, Xu Xuebin, Shi Jun, Wang Tieying, Li Zhijun. Establishment and validation of a finite element model of sacral lumbarization in adolescents [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(27): 4283-4288. |
| [11] | Meng Lingjie, Qian Hui, Sheng Xiaolei, Lu Jianfeng, Huang Jianping, Qi Liangang, Liu Zongbao. Application of three-dimensional printing technology combined with bone cement in minimally invasive treatment of the collapsed Sanders III type of calcaneal fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3784-3789. |
| [12] | Hu Jing, Xiang Yang, Ye Chuan, Han Ziji. Three-dimensional printing assisted screw placement and freehand pedicle screw fixation in the treatment of thoracolumbar fractures: 1-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3804-3809. |
| [13] | Shu Qihang, Liao Yijia, Xue Jingbo, Yan Yiguo, Wang Cheng. Three-dimensional finite element analysis of a new three-dimensional printed porous fusion cage for cervical vertebra [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3810-3815. |
| [14] | Sun Maji, Wang Qiuan, Zhang Xingchen, Guo Chong, Yuan Feng, Guo Kaijin. Development and biomechanical analysis of a new anterior cervical pedicle screw fixation system [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3821-3825. |
| [15] | Zou Shouping, Lu Daoyun, Ye Li. Minimally invasive percutaneous pedicle screw technique for thoracolumbar fractures: biomechanical changes of the spine during 6-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3865-3869. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||