Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (7): 1101-1106.doi: 10.3969/j.issn.2095-4344.1849
Previous Articles Next Articles
Three-dimensional hanging-drop culture of mesenchymal stem cells in the treatment of tissue injury
Deng Junhao1, 2, Li Miao2, Zhang Licheng1, Tang Peifu1
- 1Department of Orthopedics, PLA General Hospital, Beijing 100853, China; 2Peking University Shenzhen Graduate School, Shenzhen 518055, Guangdong Province, China
-
Received:2019-05-05Revised:2019-05-21Accepted:2019-07-05Online:2020-03-08Published:2020-01-20 -
Contact:Tang Peifu, MD, Chief physician, Professor, Department of Orthopedics, PLA General Hospital, Beijing 100853, China -
About author:Deng Junhao, Master, Physician, Department of Orthopedics, PLA General Hospital, Beijing 100853, China; Peking University Shenzhen Graduate School, Shenzhen 518055, Guangdong Province, China -
Supported by:the National Natural Science Foundation of China, No. 81520108017
CLC Number:
Cite this article
Deng Junhao, Li Miao, Zhang Licheng, Tang Peifu. Three-dimensional hanging-drop culture of mesenchymal stem cells in the treatment of tissue injury [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(7): 1101-1106.
share this article
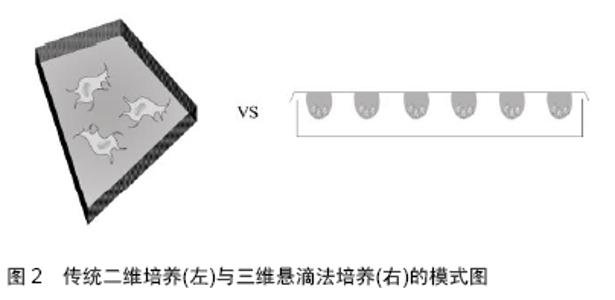
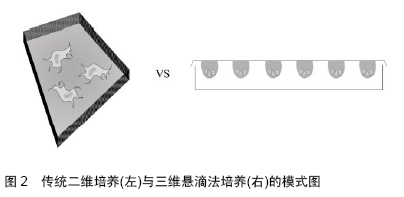
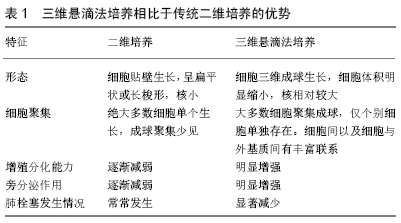
2.1 间充质干细胞概述 2.1.1 间充质干细胞的生物学特征 间充质干细胞是一类来源于中胚层、具备高度可塑性的多能干细胞[13-14]。在20世纪70年代,FRIEDENSTEIN等首次从骨髓中分离得到了间充质干细胞,因其易于分离培养、具备高度自我增殖和多向分化潜能以及强大的免疫调控作用等优点,其治疗各类疾病的研究逐步深入开展,被认为是组织工程和损伤修复中理想的种子细胞。然而,目前对于间充质干细胞的定义仍存在较大的争议。直至今日,依然没有找到间充质干细胞特定的表面标志。国际上目前倾向于以下标准:①在标准细胞培养条件下,细胞贴壁生长,形似梭形或纤维样细胞;②高表达某些基质细胞抗原,如CD73、CD90和CD105,同时不表达或低表达以下表面抗原,包括CD34、CD45、CD11、CD14、CD79、HLA-DR等;③在特定的条件下,具备向以下细胞分化的能力,包括脂肪细胞、成骨细胞和软骨细胞 等[15-16]。根据这一定义,间充质干细胞来源十分广泛,可以从多种组织诸如骨髓、外周血、脂肪、脐带、胎盘、羊水、牙髓等分离得到[15,17]。不同来源间充质干细胞的生物学特征有一定的差异,例如在增殖能力上,胎盘和脐带来源间充质干细胞要强于脂肪及骨髓来源间充质干细胞;在分化潜能方面,胎盘来源和骨髓来源间充质干细胞在向血管内皮及成骨分化上要强于脂肪和脐带来源间充质干细胞[17-19]。 2.1.2 间充质干细胞修复损伤的潜在机制 目前,关于间充质干细胞发挥组织损伤修复的确切机制尚未明了,有两大主要观点:其一是间充质干细胞通过自身强大的旁分泌作用,营造适宜的修复微环境,从而保护残存的组织及促进损伤修复。移植后的间充质干细胞能够分泌多种细胞营养因子,促进损伤局部的特定组织细胞的增生分化,同时间充质干细胞分泌血管内皮生长因子、成纤维细胞生长因子等,能够有效促进周围新生小血管的形成,从而对损伤局部进行组织修复。此外,间充质干细胞有强大的免疫调控作用,能上调特定的抗炎因子如白细胞介素10、白细胞介素13等,也能下调某些促炎因子如白细胞介素4等,参与损伤局部的炎症调节[20-21],从而间接调节局部组织的损伤修复。MAUMAS等[22]通过全面总结间充质干细胞的分泌谱,指出间充质干细胞参与组织损伤修复的主要机制是通过产生多种营养因子实现的。多个研究发现间充质干细胞能通过不同的细胞因子发挥多种功能,如分泌的血管生长因子多肽、血小板衍生生长因子等参与血管新生[23];分泌的转化生长因子β能够有效防止细胞凋亡;分泌的肝细胞生长因子及碱性成纤维细胞生长因子等参与组织纤维化的调节;分泌的多种抗炎因子如白细胞介素6、前列腺素E2等能有效调节局部的炎症反应[24]。此外,间充质干细胞还能分泌部分抗氧化物质如血红素加氧酶和红细胞生成素等[25];其二是间充质干细胞通过增殖分化、替代坏死凋亡的组织细胞,从而促使组织损伤修复。移植后的间充质干细胞具有较强的病灶迁移能力,在周围微环境的作用下能够向特定类型的细胞分化,补充坏死凋亡的细胞。MILADPOUR等[26]在体外特异性诱导间充质干细胞向胰腺β细胞分化,胰岛素表达明显增加;MEYER等[27]指出在不同的条件下可以按照人们主观意愿调控间充质干细胞的分化方向,从而特异性补充特定的细胞;GUO等[28]将细胞移入到脑组织损伤局部后,能观察到间充质干细胞特异性表达神经元类标志物如胶质纤维酸性蛋白、微管相关蛋白2等。 通常情况下,间充质干细胞既能特定向局部损伤的细胞分化,也能通过营造局部的适宜微环境动员内源性细胞增殖分化从而补充坏死凋亡的细胞。在不同的组织损伤中,二者所起作用略有不同。ZHOU等[29]研究发现,在脊髓损伤修复中主要是后者发挥修复作用,因为移植后的间充质干细胞存活率不高,难以通过外源性补充特定细胞而发挥修复作用;HO等[30]研究发现,间充质干细胞能够补充坏死凋亡的细胞,同时分泌多种营养因子,共同促进骨缺损的修复。 2.1.3 间充质干细胞二维培养的缺陷 间充质干细胞虽然来源广泛,但各组织所含细胞总量并不充足。众所周知,间充质干细胞在进行实际应用之前,必须进行相当程度的体外扩增。目前,间充质干细胞的体外培养绝大多数依然是应用培养皿进行传统的细胞贴壁培养。这种“金标准”方法是由FRIEDENSTEIN首创,即差异贴壁培养法,其突出优势是操作简便,耗费较低,能够在较短时间内扩增获得相当数量的细胞,但是这种方法忽视了细胞微环境的重要性,导致细胞在扩增数代后,虽然得到足够数量的干细胞,但细胞性状发生了明显改变。这是因为传统的贴壁培养方式,迫使间充质干细胞向二维平面伸展,细胞原有的三维结构和形态遭到破坏,细胞间的相互作用明显减少,从而使得间充质干细胞的性状难以保持,增殖分化潜能受损,最终影响细胞移植的疗效[31],见图2。 "
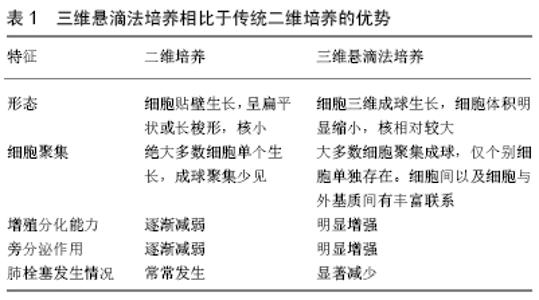

2.1.4 间充质干细胞的三维培养 在生理情况下,体内的细胞均存在于立体环境下,因此三维培养的细胞理论上更能接近体内的真实环境。以三维形式培养的细胞,具备以下几点优势:①三维微环境更能保留细胞的生理表型;②细胞与细胞之间能更好地接触作用,相互影响;③三维环境下分泌的细胞外基质充斥在细胞周围,有利于细胞在局部的停留;④核心部分相对低氧的环境有利于细胞营养因子的分泌[32]。目前对于三维细胞培养,主要可分为无材料依赖型和材料依赖型培养两种方式,后者依赖各种材料搭载三维空间后再种植间充质干细胞,间接模拟细胞的三维状态,这种方式可以搭载多种生物活性材料,如水凝胶、壳聚糖等,能增强和延迟间充质干细胞的功能活性,进一步促进组织的损伤修复。然而,这种可依附的生物材料必须满足特定的生物相容性,并且需要具备可降解的能力,因此对所选材料的要求较高。另外,在进行细胞移植时需同时移植活性材料,不仅会在生物体内占据相当的空间,而且许多材料本质上仍是异物,且常常难以降解,加大病灶损害,不利于干细胞的移植治疗。 无材料依赖型的三维成球培养,目前主要有悬滴法和悬浮培养两种。它们都具备悬浮状态下自发成球的特点,避免了其他因素的干扰。但在悬浮培养中,细胞聚集成球的大小差异较大,过大的细胞球会影响细胞球体内的物质交换,影响细胞的活性。不同于悬浮培养,以悬滴法构建的三维培养体系则显示出明显的优势:①悬滴法构建的细胞悬滴,所含细胞数相同,球体大小一致;②无需借助额外装置,自发实现细胞成球,有利于控制无关变量;③悬滴法的成球是一个连续的生物过程,更接近体内的细胞聚集方式;④原理简单,容易进行学习和操作。由于上述优点,越来越多的研究聚焦到悬滴法上,如SALEH等[33]发现三维悬滴法培养明显增强了间充质干细胞的成脂、成骨等分化能力;DROMAND等[34-35]指出营养因子分泌能力明显加强。综上所述,相比于二维培养的间充质干细胞,悬滴法培养的三维间充质干细胞更易于保持干细胞的原始性状,如增殖分化潜能增强、相关营养因子的分泌增多等,见表1。 "


2.2.1 三维间充质干细胞与脑卒中 脑卒中是一类常见的致死致残性疾病,可分为出血性脑卒中和缺血性脑卒中。由于其狭窄的治疗时间窗,相当数量的脑卒中患者不可避免地发展为瘫痪状态,治疗效果极其有限。脑卒中发生后,局部组织会出现神经元、星形胶质细胞等急剧减少,相应突触结构遭到破坏,从而导致神经功能丧失。目前多项研究表明,三维成球培养的间充质干细胞能够有效减少脑梗死病灶大小并促进功能恢复。研究发现,三维间充质干细胞明显高表达血管内皮生长因子、肝细胞生长因子、成纤维细胞生长因子等血管生成因子,有效增加梗死局部组织的血流供应[36-37]。BARTOSH等[38]发现三维间充质干细胞移植到局部组织后,抗炎因子如白细胞介素10、白细胞介素13、肿瘤坏死因子诱导蛋白6等分泌明显增加,从而调节损伤后局部过强的炎症反应。GUO等[28]研究表明,三维间充质干细胞的增殖分化能力明显强于二维间充质干细胞,神经细胞表面标志物的表达如巢蛋白、胶质纤维酸性蛋白、微管相关蛋白2等明显上升。此外,三维间充质干细胞因细胞直径小而更不容易发生血管堵塞,能让更多的间充质干细胞迁移到病灶周围发挥作用;最后,他们分别采用改良大鼠神经功能缺损评分和Adhesive-removal实验评估了大鼠的功能学恢复,发现三维间充质干细胞移植后能够明显改善大鼠的功能活动。 2.2.2 三维间充质干细胞与脊髓损伤 脊髓损伤也是一类严重的、能高度致残的中枢神经系统损伤性疾病。由于其结构和功能的特殊性以及复杂的病理生理过程,使得当前的脊髓损伤治疗极其困难[39]。目前尚未有三维悬滴法培养的间充质干细胞在脊髓损伤中的应用研究。作者将三维间充质干细胞移植到脊髓损伤小鼠体内,能够明显抑制局部的炎性渗出和胶质瘢痕形成,借助双光子显微镜活体观察到损伤轴突的退变速度及距离明显缩短,但未见到间充质干细胞向神经细胞方向分化(数据未发表)。因此,作者推测在脊髓损伤中主要是三维间充质干细胞的旁分泌因子而非细胞替代发挥了主要的治疗作用。这与二维间充质干细胞在移植到脊髓损伤局部后的命运相似[40],但未来仍需更多三维间充质干细胞治疗脊髓损伤实验研究支持。 2.2.3 三维间充质干细胞与心肌损伤修复 心血管疾病,特别是冠心病,仍是当今导致患者死亡的“头号杀手”。冠心病的发生通常是由于冠状动脉狭窄、局部供血不足而引起的心肌功能障碍或器质性病变。冠心病发作后,易导致相应部位的心肌梗死及心肌细胞的溶解死亡,出现进行性心肌壁变薄弱,纤维环及心腔进行性扩大。此外,由于心肌的再生能力相当有限,常导致心肌损伤后难以进行自我修复。当前,三维间充质干细胞在心肌损伤修复中的研究已有不少,JOSHI等[41]联合三维间充质干细胞和静电纺丝纳米纤维进行体外实验,三维间充质干细胞能够分化为心肌类细胞并长期表达心肌细胞表面标志。LEE等[42]和KIM等[43]进一步将三维间充质干细胞移植到心肌损伤局部,结果发现,相比于二维间充质干细胞,三维成球的细胞更容易聚集和停留在损伤局部。移植后的三维间充质干细胞在病灶周围聚集,其抗炎因子的表达明显提高,更好地调整局部过强的炎症反应[44]。 2.2.4 三维间充质干细胞与骨骼肌肉损伤 细胞移植在骨骼肌肉损伤中的应用并不少见,但常常由于移植细胞难以在损伤局部停留及细胞存活率较低,导致损伤修复效果不佳。三维悬滴法培养的间充质干细胞,因低氧环境的刺激可明显提高细胞的存活力,而细胞的聚集成球则增加了局部营养因子的分泌,这些均为三维间充质干细胞在骨骼肌肉疾病中的应用打下基础。LEE等[45]将三维间充质干细胞移植到兔骨软骨缺损区域,相比于传统培养的间充质干细胞移植,局部骨软骨的修复明显加快,软骨缺损面积显著减小,他们认为最主要的原因是三维间充质干细胞分泌的营养因子增多和免疫抑制作用增强。MURPHY等[46]发现三维间充质干细胞通过调节α2β1信号通路,增强自身成骨特性,能更好参与骨组织损伤的修复。 2.2.5 三维间充质干细胞与其他损伤修复 除上述疾病外,三维间充质干细胞也在其他多种损伤中有相关应用的报道。在皮肤损伤修复上,SANTOS等[47]通过皮下注射将三维间充质干细胞移植到损伤局部,发现血管内皮生长因子等营养因子表达明显增加,皮肤伤口愈合速度明显加快。在急性肾损伤中,三维间充质干细胞能够在损伤局部高表达诸如前列腺素E2、肿瘤坏死因子诱导蛋白6等炎症调节因子以及血管内皮生长因子、肝细胞生长因子等营养因子,营造适宜的微环境,增加局部血流供应,有利于肾损伤的修复[48-49]。在肝损伤方面,三维间充质干细胞移植到损伤局部后,通过旁分泌作用能够有效抑制肝组织的纤维化,减少肝细胞凋亡坏死[50-51]。 简而言之,三维间充质干细胞在多种损伤中均有较强的促修复作用,大多通过其增强的旁分泌作用进而抑制局部过强的炎症反应和促进组织再生,少部分能直接分化为特定的细胞,替代相应坏死的细胞,从而促进组织的再生。 "

| [1] WALKER PA, SHAH SK, HARTING MT, et al. Progenitor cell therapies for traumatic brain injury: barriers and opportunities in translation. Dis Model Mech. 2009;2(1-2):23-38. [2] HO AD, WAGNER W, FRANKE W. Heterogeneity of mesenchymal stromal cell preparations. Cytotherapy. 2008;10(4):320-330. [3] UCCELLI A, MORETTA L, PISTOIA V. Mesenchymal stem cells in health and disease. Nat Rev Immunol. 2008;8(9):726-736. [4] FRIEDENSTEIN AJ, PETRAKOVA KV, KUROLESOVA AI, et al. Heterotopic of bone marrow. Analysis of precursor cells for osteogenic and hematopoietic tissues. Transplantation.1968;6(2):230-247. [5] LUGER D, LIPINSKI MJ, WESTMAN PC, et al. Intravenously Delivered Mesenchymal Stem Cells: Systemic Anti-Inflammatory Effects Improve Left Ventricular Dysfunction in Acute Myocardial Infarction and Ischemic Cardiomyopathy. Circ Res. 2017;120(10):1598-1613. [6] CHEN Y, ZHAO Y, CHEN W, et al. MicroRNA-133 overexpression promotes the therapeutic efficacy of mesenchymal stem cells on acute myocardial infarction. Stem Cell Res Ther. 2017;8(1):268. [7] ZHOU P, LIU Z, LI X, et al. Migration ability and Toll-like receptor expression of human mesenchymal stem cells improves significantly after three-dimensional culture. Biochem Biophys Res Commun. 2017; 491(2):323-328. [8] LIANG L, LI Z, MA T, et al. Transplantation of Human Placenta-Derived Mesenchymal Stem Cells Alleviates Critical Limb Ischemia in Diabetic Nude Rats. Cell Transplant. 2017;26(1):45-61. [9] ISHIZAKA S, HORIE N, SATOH K, et al. Intra-arterial cell transplantation provides timing-dependent cell distribution and functional recovery after stroke. Stroke. 2013;44(3):720-726. [10] GHAZAVI H, HOSEINI SJ, EBRAHIMZADEH-BIDESKAN A, et al. Fibroblast Growth Factor Type 1 (FGF1)-Overexpressed Adipose- Derived Mesenchaymal Stem Cells (AD-MSCFGF1) Induce Neuroprotection and Functional Recovery in a Rat Stroke Model. Stem Cell Rev. 2017;13(5):670-685. [11] OH SK, CHOI KH, YOO JY, et al. A Phase III Clinical Trial Showing Limited Efficacy of Autologous Mesenchymal Stem Cell Therapy for Spinal Cord Injury. Neurosurgery. 2016;78(3):436-447. [12] KIM HS, LEE JH, ROH KH, et al. Clinical Trial of Human Umbilical Cord Blood-Derived Stem Cells for the Treatment of Moderate-to-Severe Atopic Dermatitis: Phase I/IIa Studies. Stem Cells. 2017;35(1):248-255. [13] WONG SP, ROWLEY JE, REDPATH AN, et al. Pericytes, mesenchymal stem cells and their contributions to tissue repair. Pharmacol Ther. 2015; 151:107-120. [14] ANKRUM JA, ONG JF, KARP JM. Mesenchymal stem cells: immune evasive, not immune privileged. Nat Biotechnol. 2014;32(3):252-260. [15] CUNNINGHAM CJ, REDONDO-CASTRO E, ALLAN SM. The therapeutic potential of the mesenchymal stem cell secretome in ischaemic stroke. J Cereb Blood Flow Metab. 2018;38(8):1276-1292.d [16] DOMINICI M, LE BLANC K, MUELLER I, et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy. 2006; 8(4):315-317. [17] XU L, LIU Y, SUN Y, et al. Tissue source determines the differentiation potentials of mesenchymal stem cells: a comparative study of human mesenchymal stem cells from bone marrow and adipose tissue. Stem Cell Res Ther. 2017;8(1):275. [18] COOPER GM, DURHAM EL, CRAY JJ JR, et al. Direct comparison of progenitor cells derived from adipose, muscle, and bone marrow from wild-type or craniosynostotic rabbits. Plast Reconstr Surg. 2011;127(1): 88-97. [19] PERS YM, MAUMUS M, BONY C, et al. Contribution of microRNAs to the immunosuppressive function of mesenchymal stem cells. Biochimie. 2018;155:109-118. [20] ZHU Y, ZHANG K, ZHAO R, et al. Bone regeneration with micro/nano hybrid-structured biphasic calcium phosphate bioceramics at segmental bone defect and the induced immunoregulation of MSCs. Biomaterials. 2017;147:133-144. [21] UCHIDA S, HAYAKAWA K, OGATA T, et al. Treatment of spinal cord injury by an advanced cell transplantation technology using brain-derived neurotrophic factor-transfected mesenchymal stem cell spheroids. Biomaterials. 2016;109:1-11. [22] MAUMUS M, JORGENSEN C, NOËL D. Mesenchymal stem cells in regenerative medicine applied to rheumatic diseases: role of secretome and exosomes. Biochimie. 2013;95(12):2229-2234. [23] MEIRELLES LDA S, FONTES AM, COVAS DT, et al. Mechanisms involved in the therapeutic properties of mesenchymal stem cells. Cytokine Growth Factor Rev. 2009;20(5-6):419-427. [24] GHANNAM S, BOUFFI C, DJOUAD F, et al. Immunosuppression by mesenchymal stem cells: mechanisms and clinical applications. Stem Cell Res Ther. 2010;1(1):2. [25] DE ALMEIDA DC, DONIZETTI-OLIVEIRA C, BARBOSA-COSTA P, et al. In search of mechanisms associated with mesenchymal stem cell-based therapies for acute kidney injury. Clin Biochem Rev. 2013;34(3):131-144. [26] MILADPOUR B, RASTI M, OWJI AA, et al. Quercetin potentiates transdifferentiation of bone marrow mesenchymal stem cells into the beta cells in vitro. J Endocrinol Invest. 2017;40(5):513-521. [27] MEYER MB, BENKUSKY NA, SEN B, et al. Epigenetic Plasticity Drives Adipogenic and Osteogenic Differentiation of Marrow-derived Mesenchymal Stem Cells. J Biol Chem. 2016;291(34):17829-17847. [28] GUO L, GE J, ZHOU Y, et al. Three-dimensional spheroid-cultured mesenchymal stem cells devoid of embolism attenuate brain stroke injury after intra-arterial injection. Stem Cells Dev. 2014;23(9):978-989. [29] ZHOU Z, CHEN Y, ZHANG H, et al. Comparison of mesenchymal stromal cells from human bone marrow and adipose tissue for the treatment of spinal cord injury. Cytotherapy. 2013;15(4):434-448. [30] HO SS, HUNG BP, HEYRANI N, et al. Hypoxic Preconditioning of Mesenchymal Stem Cells with Subsequent Spheroid Formation Accelerates Repair of Segmental Bone Defects. Stem Cells. 2018;36(9): 1393-1403. [31] HUANG GS, DAI LG, YEN BL, et al. Spheroid formation of mesenchymal stem cells on chitosan and chitosan-hyaluronan membranes. Biomaterials. 2011;32(29):6929-6945. [32] GÜNTER J, WOLINT P, BOPP A, et al. Microtissues in Cardiovascular Medicine: Regenerative Potential Based on a 3D Microenvironment. Stem Cells Int. 2016;2016:9098523. [33] SALEH FA, WHYTE M, GENEVER PG. Effects of endothelial cells on human mesenchymal stem cell activity in a three-dimensional in vitro model. Eur Cell Mater. 2011;22:242-257. [34] DROMARD C, BOURIN P, ANDRÉ M, et al. Human adipose derived stroma/stem cells grow in serum-free medium as floating spheres. Exp Cell Res. 2011;317(6):770-780. [35] KAPUR SK, WANG X, SHANG H, et al. Human adipose stem cells maintain proliferative, synthetic and multipotential properties when suspension cultured as self-assembling spheroids. Biofabrication. 2012;4(2):025004. [36] CESARZ Z, TAMAMA K. Spheroid Culture of Mesenchymal Stem Cells. Stem Cells Int. 2016;2016:9176357. [37] LARANJEIRA P, PEDROSA M, PEDREIRO S, et al. Effect of human bone marrow mesenchymal stromal cells on cytokine production by peripheral blood naive, memory, and effector T cells. Stem Cell Res Ther. 2015;6:3. [38] BARTOSH TJ, YLÖSTALO JH, MOHAMMADIPOOR A, et al. Aggregation of human mesenchymal stromal cells (MSCs) into 3D spheroids enhances their antiinflammatory properties. Proc Natl Acad Sci U S A. 2010;107(31): 13724-13729. [39] NAKAMURA M, OKANO H. Cell transplantation therapies for spinal cord injury focusing on induced pluripotent stem cells. Cell Res. 2013;23(1): 70-80. [40] MADRIGAL M, RAO KS, RIORDAN NH. A review of therapeutic effects of mesenchymal stem cell secretions and induction of secretory modification by different culture methods. J Transl Med. 2014;12:260. [41] JOSHI J, BRENNAN D, BEACHLEY V, et al. Cardiomyogenic differentiation of human bone marrow-derived mesenchymal stem cell spheroids within electrospun collagen nanofiber mats. J Biomed Mater Res A. 2018;106(12):3303-3312. [42] LEE WY, CHANG YH, YEH YC, et al. The use of injectable spherically symmetric cell aggregates self-assembled in a thermo-responsive hydrogel for enhanced cell transplantation.Biomaterials. 2009;30(29): 5505-5513. [43] KIM JH, PARK IS, PARK Y, et al. Therapeutic angiogenesis of three-dimensionally cultured adipose-derived stem cells in rat infarcted hearts. Cytotherapy. 2013;15(5):542-556. [44] BARTOSH TJ, YLÖSTALO JH, MOHAMMADIPOOR A, et al. Aggregation of human mesenchymal stromal cells (MSCs) into 3D spheroids enhances their antiinflammatory properties. Proc Natl Acad Sci U S A. 2010;107(31):13724-13729. [45] LEE BH, PARK JN, LEE EJ, et al. Therapeutic Efficacy of Spherical Aggregated Human Bone Marrow-Derived Mesenchymal Stem Cells Cultured for Osteochondral Defects of Rabbit Knee Joints. Am J Sports Med. 2018;46(9):2242-2252. [46] MURPHY KC, HOCH AI, HARVESTINE JN, et al. Mesenchymal Stem Cell Spheroids Retain Osteogenic Phenotype Through α2β1 Signaling. Stem Cells Transl Med. 2016;5(9):1229-1237. [47] SANTOS JM, CAMÕES SP, FILIPE E, et al. Three-dimensional spheroid cell culture of umbilical cord tissue-derived mesenchymal stromal cells leads to enhanced paracrine induction of wound healing. Stem Cell Res Ther. 2015;6:90. [48] BORGES FT, SCHOR N. Regenerative medicine in kidney disease: where we stand and where to go. Pediatr Nephrol. 2018;33(9):1457-1465. [49] XU Y, SHI T, XU A, et al. 3D spheroid culture enhances survival and therapeutic capacities of MSCs injected into ischemic kidney. J Cell Mol Med. 2016;20(7):1203-1213. [50] SUN Y, WANG Y, ZHOU L, et al. Spheroid-cultured human umbilical cord-derived mesenchymal stem cells attenuate hepatic ischemia- reperfusion injury in rats. Sci Rep. 2018;8(1):2518. [51] ZHANG X, HU MG, PAN K, et al. 3D Spheroid Culture Enhances the Expression of Antifibrotic Factors in Human Adipose-Derived MSCs and Improves Their Therapeutic Effects on Hepatic Fibrosis. Stem Cells Int. 2016;2016:4626073. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Lin Qingfan, Xie Yixin, Chen Wanqing, Ye Zhenzhong, Chen Youfang. Human placenta-derived mesenchymal stem cell conditioned medium can upregulate BeWo cell viability and zonula occludens expression under hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 4970-4975. |
| [3] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [4] | Shi Yangyang, Qin Yingfei, Wu Fuling, He Xiao, Zhang Xuejing. Pretreatment of placental mesenchymal stem cells to prevent bronchiolitis in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 991-995. |
| [5] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [6] | Fan Quanbao, Luo Huina, Wang Bingyun, Chen Shengfeng, Cui Lianxu, Jiang Wenkang, Zhao Mingming, Wang Jingjing, Luo Dongzhang, Chen Zhisheng, Bai Yinshan, Liu Canying, Zhang Hui. Biological characteristics of canine adipose-derived mesenchymal stem cells cultured in hypoxia [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1002-1007. |
| [7] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [8] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [9] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [10] | Duan Liyun, Cao Xiaocang. Human placenta mesenchymal stem cells-derived extracellular vesicles regulate collagen deposition in intestinal mucosa of mice with colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1026-1031. |
| [11] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [12] | Wang Xianyao, Guan Yalin, Liu Zhongshan. Strategies for improving the therapeutic efficacy of mesenchymal stem cells in the treatment of nonhealing wounds [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1081-1087. |
| [13] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [14] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [15] | Chen Junyi, Wang Ning, Peng Chengfei, Zhu Lunjing, Duan Jiangtao, Wang Ye, Bei Chaoyong. Decalcified bone matrix and lentivirus-mediated silencing of P75 neurotrophin receptor transfected bone marrow mesenchymal stem cells to construct tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 510-515. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

