Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (21): 3316-3322.doi: 10.3969/j.issn.2095-4344.1749
Previous Articles Next Articles
Bone marrow mesenchymal stem cell exosomes alleviate oxygen-glucose deprivation/reperfusion injury in hippocampal neurons
Shi Jiang, Gao Shilun, Liu Jinduo, Gu Tianxiang, Shi Enyi
- Department of Cardiac Surgery, First Affiliated Hospital of China Medical University, Shenyang 110000, Liaoning Province, China
-
Revised:2019-02-11Online:2019-07-28Published:2019-07-28 -
Contact:Shi Enyi, Doctoral supervisor, Professor, Chief physician, Department of Cardiac Surgery, First Affiliated Hospital of China Medical University, Shenyang 110000, Liaoning Province, China -
About author:Shi Jiang, Master, Department of Cardiac Surgery, First Affiliated Hospital of China Medical University, Shenyang 110000, Liaoning Province, China -
Supported by:the National Natural Science Foundation of China, No. 81471267 (to SEY)
CLC Number:
Cite this article
Shi Jiang, Gao Shilun, Liu Jinduo, Gu Tianxiang, Shi Enyi. Bone marrow mesenchymal stem cell exosomes alleviate oxygen-glucose deprivation/reperfusion injury in hippocampal neurons[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(21): 3316-3322.
share this article
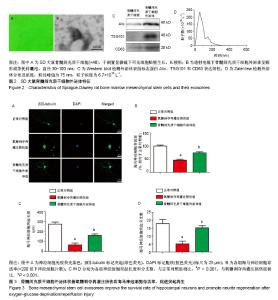
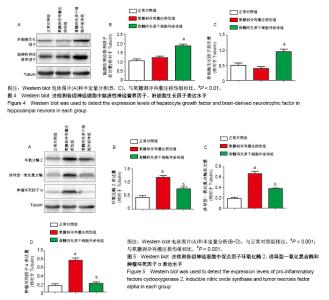
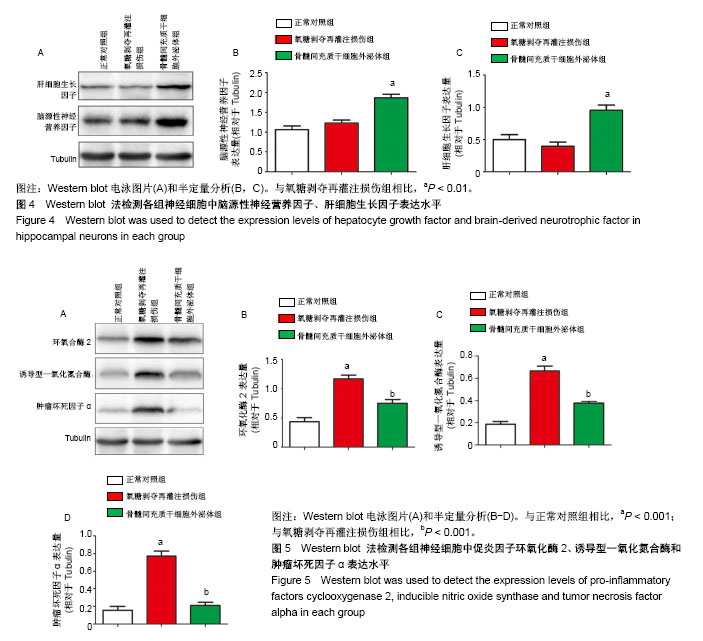
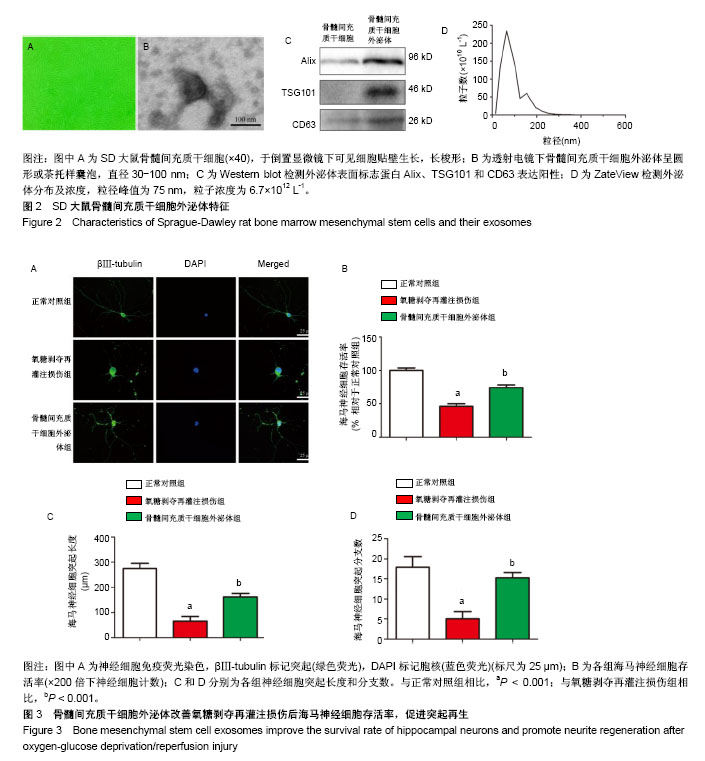
2.1 骨髓间充质干细胞外泌体形态及特点 倒置显微镜下可见SD大鼠骨髓间充质干细胞贴壁生长,长梭形,见图2A。通过超高速离心法从骨髓间充质干细胞条件培养基中提取外泌体。在透射电镜下观察,其外泌体为圆形或茶托样膜性囊泡,直径为30-100 nm,见图2B。Western blot显示骨髓间充质干细胞外泌体蛋白标志物Alix、TSG101和CD63表达阳性,见图2C。ZateView检测外泌体的粒径峰值为75 nm,粒子浓度为6.7×1012 L-1,见图2D。 2.2 骨髓间充质干细胞外泌体增加氧糖剥夺再灌注损伤后海马神经细胞的存活率,促进海马神经细胞突起再生 免疫荧光染色用于观察海马神经细胞突起生长情况,与正常对照组海马神经细胞突起长度(275.27±19.87) μm和分支数(17.89±2.67)比较,氧糖剥夺再灌注损伤组明显降低海马神经细胞突起长度(65.14±18.14) μm和分支数(5.00±1.87) (P < 0.001);与氧糖剥夺再灌注损伤组比较,骨髓间充质干细胞外泌体组增加突起长度(162.22±13.43) μm及分支数(15.22±1.39)(P < 0.001),见图3。海马神经细胞存活率通过神经细胞计数评估,氧糖剥夺再灌注损伤组显著降低神经细胞存活率(46.07±3.78)%(相对于正常对照组,P < 0.001),见图3。与氧糖剥夺再灌注损伤组比较,骨髓间充质干细胞外泌体组显著提高神经细胞生存率(74.14±4.20)%(P < 0.001)。 2.3 骨髓间充质干细胞外泌体增加氧糖剥夺再灌注损伤后海马神经细胞内的神经营养因子表达水平 为了进一步探究骨髓间充质干细胞外泌体对海马神经细胞氧糖剥夺再灌注损伤后的保护作用机制,通过Western blot检测脑源性神经营养因子、肝细胞生长因子表达水平,见图4A。与正常对照组比较,氧糖剥夺再灌注损伤组轻微提升脑源性神经营养因子表达量及下调肝细胞生长因子的表达量,但差异无显著性意义(P > 0.05)。与氧糖剥夺再灌注损伤组比较,骨髓间充质干细胞外泌体组显著增加海马神经细胞内的脑源性神经营养因子和肝细胞生长因子表达水平(P < 0.01),见图4B,C。 2.4 骨髓间充质干细胞外泌体抑制氧糖剥夺再灌注损伤后海马神经细胞的促炎因子表达 炎症反应在海马神经细胞损伤中发挥着重要作用。实验通过Western blot检测促炎因子环氧化酶2、诱导型一氧化氮合酶和肿瘤坏死因子α表达水平,见图5A。与正常对照组比较,氧糖剥夺再灌注损伤组显著提高环氧化酶2、诱导型一氧化氮合酶和肿瘤坏死因子α的表达水平(P < 0.001)。与氧糖剥夺再灌注损伤组比较,骨髓间充质干细胞外泌体组显著抑制环氧化酶2、诱导型一氧化氮合酶和肿瘤坏死因子α的表达(P < 0.001),见图5B-D。"
| [1] Gega A, Rizzo JA, Johnson MH, et al. Straight deep hypothermic arrest: experience in 394 patients supports its effectiveness as a sole means of brain preservation. Ann Thorac Surg. 2007;84(3):759-766.[2] Wang Y, Gu T, Shi E, et al. Inhibition of microRNA-29c protects the brain in a rat model of prolonged hypothermic circulatory arrest. J Thorac Cardiovasc Surg. 2015;150(3):675-684.[3] Jiang X, Gu T, Liu Y, et al. Protection of the rat brain from hypothermic circulatory arrest injury by a chipmunk protein. J Thorac Cardiovasc Surg. 2018;156(2):525-536.[4] György B, Hung ME, Breakefield XO, et al. Therapeutic applications of extracellular vesicles: clinical promise and open questions. Annu Rev Pharmacol Toxicol. 2015;55:439-464.[5] Xin H, Li Y, Liu Z, et al. MiR-133b promotes neural plasticity and functional recovery after treatment of stroke with multipotent mesenchymal stromal cells in rats via transfer of exosome-enriched extracellular particles. Stem Cells. 2013;31(12):2737-2746.[6] Xin H, Li Y, Cui Y, et al. Systemic administration of exosomes released from mesenchymal stromal cells promote functional recovery and neurovascular plasticity after stroke in rats.J Cereb Blood Flow Metab. 2013;33(11):1711-1715.[7] Zhang Y, Chopp M, Meng Y, et al. Effect of exosomes derived from multipluripotent mesenchymal stromal cells on functional recovery and neurovascular plasticity in rats after traumatic brain injury. J Neurosurg. 2015;122(4):856-867. [8] Yu B, Zhang X, Li X. Exosomes derived from mesenchymal stem cells. Int J Mol Sci. 2014;15(3):4142-4157.[9] Seibenhener ML, Wooten MW. Isolation and culture of hippocampal neurons from prenatal mice. J Vis Exp. 2012;(65): 3634.[10] Zhao L, Jiang X, Shi J, et al. Exosomes derived from bone marrow mesenchymal stem cells overexpressing microRNA-25 protect spinal cords against transient ischemia. J Thorac Cardiovasc Surg. 2019; 157(2):508-517.[11] Bellinger DC, Jonas RA, Rappaport LA, et al. Developmental and neurologic status of children after heart surgery with hypothermic circulatory arrest or low-flow cardiopulmonary bypass. N Engl J Med. 1995;332(9):549-555.[12] Wang X, Chu W, Zhuang Y, et al. Bone Mesenchymal Stem Cell-Enriched β-Tricalcium Phosphate Scaffold Processed by the Screen-Enrich-Combine Circulating System Promotes Regeneration of Diaphyseal Bone Non-Union. Cell Transplant. 2019;28(2):212-223. [13] Li B. MicroRNA Regulation in Osteogenic and Adipogenic Differentiation of Bone Mesenchymal Stem Cells and its Application in Bone Regeneration. Curr Stem Cell Res Ther. 2018;13(1):26-30.[14] Zhu T, Yu D, Feng J, et al. GDNF and NT-3 induce progenitor bone mesenchymal stem cell differentiation into neurons in fetal gut culture medium. Cell Mol Neurobiol. 2015;35(2):255-264.[15] Ueno Y, Chopp M, Zhang L, et al. Axonal outgrowth and dendritic plasticity in the cortical peri-infarct area after experimental stroke. Stroke. 2012;43(8):2221-2228.[16] Gutiérrez-Fernández M, Rodríguez-Frutos B, Ramos-Cejudo J, et al. Effects of intravenous administration of allogenic bone marrow- and adipose tissue-derived mesenchymal stem cells on functional recovery and brain repair markers in experimental ischemic stroke. Stem Cell Res Ther. 2013;4(1):11.[17] Egashira Y, Sugitani S, Suzuki Y, et al. The conditioned medium of murine and human adipose-derived stem cells exerts neuroprotective effects against experimental stroke model. Brain Res. 2012;1461: 87-95.[18] Tsai MJ, Tsai SK, Hu BR, et al. Recovery of neurological function of ischemic stroke by application of conditioned medium of bone marrow mesenchymal stem cells derived from normal and cerebral ischemia rats. J Biomed Sci. 2014;21:5.[19] Zhang ZG, Chopp M. Exosomes in stroke pathogenesis and therapy. J Clin Invest. 2016;126(4):1190-1197.[20] Long Q, Upadhya D, Hattiangady B, et al. Intranasal MSC-derived A1-exosomes ease inflammation, and prevent abnormal neurogenesis and memory dysfunction after status epilepticus. Proc Natl Acad Sci U S A. 2017;114(17):E3536-E3545. [21] Tian T, Zhang HX, He CP, et al. Surface functionalized exosomes as targeted drug delivery vehicles for cerebral ischemia therapy. Biomaterials. 2018;150:137-149.[22] Xin H, Li Y, Buller B, et al. Exosome-mediated transfer of miR-133b from multipotent mesenchymal stromal cells to neural cells contributes to neurite outgrowth. Stem Cells. 2012;30(7):1556-1564.[23] Zhang Y, Chopp M, Liu XS, et al. Exosomes Derived from Mesenchymal Stromal Cells Promote Axonal Growth of Cortical Neurons. Mol Neurobiol. 2017;54(4):2659-2673.[24] Shang J, Deguchi K, Ohta Y, et al. Strong neurogenesis, angiogenesis, synaptogenesis, and antifibrosis of hepatocyte growth factor in rats brain after transient middle cerebral artery occlusion. J Neurosci Res. 2011;89(1):86-95. [25] Zeng W, Ju R, Mao M. Therapeutic potential of hepatocyte growth factor against cerebral ischemia (Review). Exp Ther Med. 2015;9(2): 283-288.[26] Liu XS, Li JF, Wang SS, et al. Human umbilical cord mesenchymal stem cells infected with adenovirus expressing HGF promote regeneration of damaged neuron cells in a Parkinson's disease model. Biomed Res Int. 2014;2014:909657.[27] Pollock K, Dahlenburg H, Nelson H, et al. Human Mesenchymal Stem Cells Genetically Engineered to Overexpress Brain-derived Neurotrophic Factor Improve Outcomes in Huntington's Disease Mouse Models. Mol Ther. 2016;24(5):965-977.[28] Kim D, Chung S, Lee SH, et al. Decreased hippocampal brain-derived neurotrophic factor and impaired cognitive function by hypoglossal nerve transection in rats. J Cell Mol Med. 2017;21(12):3752-3760.[29] Lee J, Duan W, Mattson MP. Evidence that brain-derived neurotrophic factor is required for basal neurogenesis and mediates, in part, the enhancement of neurogenesis by dietary restriction in the hippocampus of adult mice. J Neurochem. 2002;82(6):1367-1375.[30] Reichardt LF. Neurotrophin-regulated signalling pathways. Philos Trans R Soc Lond B Biol Sci. 2006;361(1473):1545-1564.[31] Jin JL, Liu Z, Lu ZJ, et al. Safety and efficacy of umbilical cord mesenchymal stem cell therapy in hereditary spinocerebellar ataxia. Curr Neurovasc Res. 2013;10(1):11-20.[32] Liu S, Sandner B, Schackel T, et al. Regulated viral BDNF delivery in combination with Schwann cells promotes axonal regeneration through capillary alginate hydrogels after spinal cord injury. Acta Biomater. 2017;60:167-180.[33] Wong WK, Cheung AW, Yu SW, et al. Hepatocyte growth factor promotes long-term survival and axonal regeneration of retinal ganglion cells after optic nerve injury: comparison with CNTF and BDNF. CNS Neurosci Ther. 2014;20(10):916-929.[34] Dantzer R, O'Connor JC, Freund GG, et al. From inflammation to sickness and depression: when the immune system subjugates the brain. Nat Rev Neurosci. 2008;9(1):46-56.[35] Trounson A. New perspectives in human stem cell therapeutic research. BMC Med. 2009;7:29.[36] Hurn PD, Subramanian S, Parker SM, et al. T- and B-cell-deficient mice with experimental stroke have reduced lesion size and inflammation. J Cereb Blood Flow Metab. 2007;27(11):1798-1805.[37] Kim DK, Nishida H, An SY, et al. Chromatographically isolated CD63+CD81+ extracellular vesicles from mesenchymal stromal cells rescue cognitive impairments after TBI. Proc Natl Acad Sci U S A. 2016;113(1):170-175. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Hou Jingying, Yu Menglei, Guo Tianzhu, Long Huibao, Wu Hao. Hypoxia preconditioning promotes bone marrow mesenchymal stem cells survival and vascularization through the activation of HIF-1α/MALAT1/VEGFA pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 985-990. |
| [3] | Liang Xueqi, Guo Lijiao, Chen Hejie, Wu Jie, Sun Yaqi, Xing Zhikun, Zou Hailiang, Chen Xueling, Wu Xiangwei. Alveolar echinococcosis protoscolices inhibits the differentiation of bone marrow mesenchymal stem cells into fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 996-1001. |
| [4] | Geng Yao, Yin Zhiliang, Li Xingping, Xiao Dongqin, Hou Weiguang. Role of hsa-miRNA-223-3p in regulating osteogenic differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1008-1013. |
| [5] | Lun Zhigang, Jin Jing, Wang Tianyan, Li Aimin. Effect of peroxiredoxin 6 on proliferation and differentiation of bone marrow mesenchymal stem cells into neural lineage in vitro [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1014-1018. |
| [6] | Zhu Xuefen, Huang Cheng, Ding Jian, Dai Yongping, Liu Yuanbing, Le Lixiang, Wang Liangliang, Yang Jiandong. Mechanism of bone marrow mesenchymal stem cells differentiation into functional neurons induced by glial cell line derived neurotrophic factor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1019-1025. |
| [7] | Pei Lili, Sun Guicai, Wang Di. Salvianolic acid B inhibits oxidative damage of bone marrow mesenchymal stem cells and promotes differentiation into cardiomyocytes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1032-1036. |
| [8] | Zhao Min, Feng Liuxiang, Chen Yao, Gu Xia, Wang Pingyi, Li Yimei, Li Wenhua. Exosomes as a disease marker under hypoxic conditions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1104-1108. |
| [9] | Wang Shiqi, Zhang Jinsheng. Effects of Chinese medicine on proliferation, differentiation and aging of bone marrow mesenchymal stem cells regulating ischemia-hypoxia microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1129-1134. |
| [10] | Chen Junyi, Wang Ning, Peng Chengfei, Zhu Lunjing, Duan Jiangtao, Wang Ye, Bei Chaoyong. Decalcified bone matrix and lentivirus-mediated silencing of P75 neurotrophin receptor transfected bone marrow mesenchymal stem cells to construct tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 510-515. |
| [11] | Chen Ziyang, Pu Rui, Deng Shuang, Yuan Lingyan. Regulatory effect of exosomes on exercise-mediated insulin resistance diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 4089-4094. |
| [12] | Jiang Tao, Ma Lei, Li Zhiqiang, Shou Xi, Duan Mingjun, Wu Shuo, Ma Chuang, Wei Qin. Platelet-derived growth factor BB induces bone marrow mesenchymal stem cells to differentiate into vascular endothelial cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3937-3942. |
| [13] | Sun Jianwei, Yang Xinming, Zhang Ying. Effect of montelukast combined with bone marrow mesenchymal stem cell transplantation on spinal cord injury in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3962-3969. |
| [14] | Zhang Lishu, Liu Anqi, He Xiaoning, Jin Yan, Li Bei, Jin Fang. Alpl gene affects the therapeutic effect of bone marrow mesenchymal stem cells on ulcerative colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3970-3975. |
| [15] | Hao Xiaona, Zhang Yingjie, Li Yuyun, Xu Tao. Bone marrow mesenchymal stem cells overexpressing prolyl oligopeptidase on the repair of liver fibrosis in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3988-3993. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||