Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (27): 4342-4347.doi: 10.3969/j.issn.2095-4344.0350
Previous Articles Next Articles
Predictive factors of refractures located in adjacent vertebrae after bone cement augmentation
Huang Tian-ji, Zhang Shi-yang, Lu Chao
- Department of Orthopedics, the First Affiliated Hospital of Chongqing Medical University, Chongqing 400016, China
-
Online:2018-09-28Published:2018-09-28 -
Contact:Lu Chao, M.D., Attending physician, Department of Orthopedics, the First Affiliated Hospital of Chongqing Medical University, Chongqing 400016, China -
About author:Huang Tian-ji, M.D., Physician, Department of Orthopedics, the First Affiliated Hospital of Chongqing Medical University, Chongqing 400016, China
CLC Number:
Cite this article
Huang Tian-ji, Zhang Shi-yang, Lu Chao . Predictive factors of refractures located in adjacent vertebrae after bone cement augmentation[J]. Chinese Journal of Tissue Engineering Research, 2018, 22(27): 4342-4347.
share this article
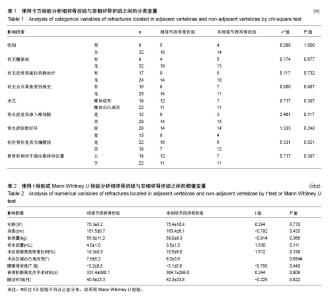
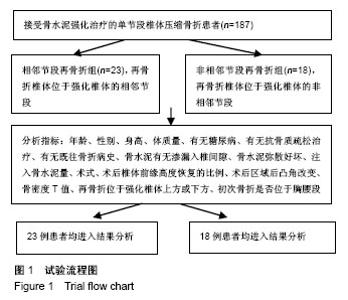
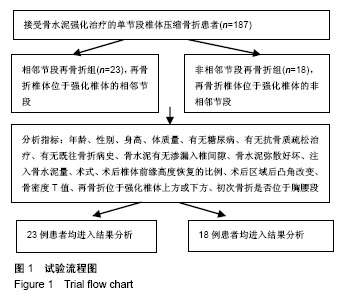
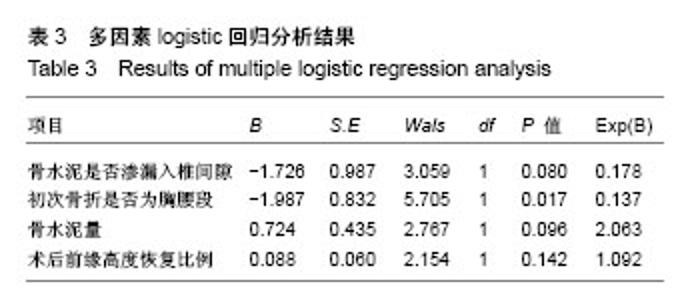
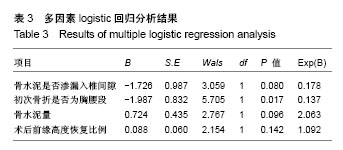
2.3 再骨折发生情况 187例患者中,共41例患者发生其他节段的再次骨折,再骨折发生率为21.9%(41/187),其中相邻椎体再骨折23例,占56.1%(23/41);非相邻椎体再骨折18例,占43.9%(18/41)。 41例再发骨折患者首次压缩骨折节段分布为:胸段(T10及以上)10例,占24.4%(10/41);胸腰段(T11至L2)22例,占53.7%(22/41);腰段(L3及以下)9例,占22.0%(9/41)。对于多次再骨折患者,仅统计首次再骨折的节段,以便进行统计学分析。 41例再骨折节段分布为:胸段(T10及以上)8例,占19.5%(8/41);胸腰段(T11-L2)25例,占61.0% (25/41);腰段(L3及以下)8例,占19.5%(8/41)。 再骨折距离首次椎体强化时间最短为7 d,最长为 1 580 d;3个月内再骨折15例,占36.6%(15/41);1年内再骨折28例,占68.3%(28/41);再骨折椎体位于强化椎体上方19例,位于强化椎体下方22例。 2.4 统计学分析 使用卡方检验、独立样本t 检验、Mann Whitney U 检验进行单因素分析,将P < 0.2的变量,即骨水泥是否渗入椎间隙、初始骨折是否为胸腰段、骨水泥用量、术后椎体前缘高度恢复比例纳入多因素logistic回归分析,结果显示:初次骨折为胸腰段骨折是再骨折发生于强化椎体相邻节段的独立预测因素(P=0.017),年龄、性别、身高、体质量、有无糖尿病、有无抗骨质疏松治疗、有无既往骨折病史、有无骨水泥渗入椎间隙、骨水泥弥散好坏、注入骨水泥量、术式为椎体成形或椎体后凸成形、术后椎体前缘高度恢复的比例、术后区域后凸角改变、骨密度T值、再骨折位于强化椎体上方或下方均不能预测再骨折发生在强化椎体的相邻节段或非相邻节段,见表1-3。"
| [1] 董平,麻春杰,李舒扬,等.高龄老人骨质疏松骨折的中医保守疗法及护理[J].世界最新医学信息文摘, 2018,18(28):181-182,185.[2] 才久波.口服金天格胶囊联合可塑形胸腰支具治疗老年骨质疏松椎体压缩骨折的临床研究[J].中国医药指南, 2017,15(26): 196-197.[3] 仝尊,张晓刚,赵永利,等.手法复位治疗老年骨质疏松性椎体压缩骨折研究进展[J].亚太传统医药,2017,13(14):71-73.[4] 于前进,唐家广,杨枭雄,等.3种方法治疗老年骨质疏松性椎体压缩骨折的效果对比[J].中国老年学杂志, 2018,38(7): 1633-1636.[5] 于江涛,杨鸫祥.保守治疗老年骨质疏松椎体压缩性骨折研究进展[J].辽宁中医药大学学报,2017,19(10):103-105.[6] 姚松.中医综合保守治疗单纯性胸腰椎压缩骨折的疗效[J].内蒙古中医药,2016,35(15):68.[7] Yu W,Xu W,Jiang X,et al.Risk Factors for Recollapse of the Augmented Vertebrae After Percutaneous Vertebral Augmentation:A Systematic Review and Meta-Analysis.World Neurosurg.2018;111:119-129.[8] Muratore M,Ferrera A,Masse A,et al.Osteoporotic vertebral fractures:predictive factores for conservative treatment failure. A systematic review.Eur Spine J.2017. doi: 10.1007/s00586-017-5340-z.[Epub ahead of print][9] Zhang H,Xu C,Zhang T,et al.DoesPercutaneous Vertebroplasty or Balloon Kyphoplasty for Osteoporotic VertebralCompression Fractures Increase the Incidence of New Vertebral Fractures? A Meta-Analysis.Pain Physician. 2017;20(1):E13-E18.[10] Schousboe JT.Epidemiology of vertebral fracutures.J Clin Densitom.2016;19(1):8-22.[11] Sebaaly A,Nabhane L,Issa EI,et al.Vertebral augmentation: state of the art.Asian Spine J. 2016;10(2):370-376.[12] Petersen A,Hartwig E,Koch EM,et al.Clinical comparison of postoperative results of balloon kyphoplasty(BKP) versus radiofrequency-targeted vertebral augementation(RF-TVA): a prospective clinical study.Eur J Orthop Surg Traumatol.2016; 26(1):67-75.[13] Chen X,Ren J,Zhang J,et al.Impact of cement placement and leakage in osteoporotic vertebral compression fractures followed by percutaneous vertebroplasty.Clin Spine Surg. 2016;29(7):E365-370.[14] Karlsson MK,Kherad M,Hasserius R,et al.Characteristics of prevalent vertebral fractures predict new fractures in elderly men.J Bone Joint Surg Am.2016;98(5):379-385.[15] Kim HS,Ju CI.Spinal instability predictive scoring system for subsequent fracture after bone cement augmentation in patients with osteoporotic vertebral compression fracture. World Neurosug. 2017;106:736-745.[16] Deibert CP,Gandhoke GS,Paschel EE,et al.A longitudinal cohort investigation of the development of symptomatic adjacent level compression fractures following balloon-assisted kyphoplasty in a series of 726 patients.Pain Physician.2016;19(8):E1167-E1172.[17] 黄天霁,寇玉辉,殷晓峰,等.椎体强化术后再发椎体骨折的临床特点和危险因素[J].北京大学学报(医学版),2015,47(2):237-241.[18] Li YA,Lin CL,Chang MC,et al.Subsequent vertebral fracture after vertebroplasty. Spine (Phila Pa 1976). 2012;7(3): 179-183.[19] Rho YJ,Choe WJ,Chun Y.Risk factors predicting the new symptomatic vertebral compression fractures after percutaneous vertebroplasty or kyphoplasty.Eur Spine J. 2012;21(5):905-911.[20] Lin WC,Cheng TT,Lee YC,et al.New vertebral osteoporotic compression fractures after percutaneous vertebroplasty: retrospective analysis of risk factors.J Vasc Interv Radiol. 2008;19(2 Pt 1):225-231.[21] Kim SH,Kang HS,Choi JA,et al.Risk factors of new compression fractures in adjacent vertebrae after percutaneous vertebroplasty.Acta Radiol.2004;45(4):440-445.[22] Chen YC, Lin WC. Can anti-osteoporotic therapy reduce adjacent fracture in magnetic resonance imagine-proven acute osteoporotic vertebral fractures? BMC Musculoskelet Discord.2016;6(17):151.[23] Bae JS,Park JH,Kim KJ,et al.Analysis of risk factors for secondary new vertebral compression fracture following percutaneous vertebroplasty in patients with osteoporosis. World Neurosurg. 2017;99:387-394.[24] Jacobson RE,Palea O,Granville M.Progression of vertebral compression fractures after previous vertebral augmentation: technical reasons for recurrent fractures in a previously treated vertebra.Cureus.2017;9(10):e1776[25] 王吉博.有限元法评估经皮椎体成形和后凸成形治疗脊柱三明治骨折的生物力学变化[J].中国组织工程研究, 2017,21(35): 5703-5708.[26] 李贵星.骨水泥椎体强化术后再发邻椎骨折的综合治疗[J].颈腰痛杂志,2017,38(5):424-427.[27] 罗琦,刘凯.胸腰段骨质疏松性压缩骨折再次骨折的相关因素分析[J].陕西医学杂志,2017,46(9):1215-1216.[28] 唐勇涛,魏思奇,吴长军,等.PKP不同增强方式对相邻椎体结构生物力学影响的有限元分析[J].中国骨科临床与基础研究杂志, 2017,9(3):167-174.[29] 王化明.经皮椎体成形术后椎体压缩性骨折患者再骨折的危险因素分析[J].中国矫形外科杂志,2016,24(4):300-303.[30] Movrin l,Vengust R,Komadina R.Adjacent vertebral fractures after percutaneous vertebral augmentation of osteoporotic vertebral compression farcture : a comparison of balloon kyphoplasty and vertebroplasty.Arch Orthop Trauma Surg. 2010;130(9):1157-1166.[31] Frankel BM,Monroe T,Wang C.Percutaneous vertebral augmentation : an elevation in adjacent-level fracture risk in kyphoplasty as compared with vertebroplasty.Spine J. 2007; 7(5):575-582.[32] 张湛金,王煜巍,陈浩,等.经皮椎体成形术与经皮椎体后凸成形术术后手术椎体再发骨折比较[J].中华骨质疏松和骨矿盐疾病杂志,2017,10(1):20-26.[33] Ahn Y,Lee JH,Lee HY,et al.Predictive factors for subsequent vertebral fracture after percutaneous vertebroplasty.J Neurosurg Spine.2008;9(2):129-136.[34] Lee KA,Hong SJ,Lee S,et al.Analysis of adjacent frature after percutaneous vertebroplasty: does intradiscal cement leakage really increase the risk of adjacent vertebral fracture.Skeletal Radiol.2011;40(12):1537-1542.[35] Wang YT,Wu XT,Chen H,et al.Adjacent-level symptomatic fracture after percutaneous vertebral augmentation of osteoporotic vertebral compression fracture : a retrospective analysis.J Orthop Sci.2014;19(6):868-876.[36] Zhang Z,Fan J,Ding Q,et al.Risk factors for new osteoporotic vertebral compression fractures after vertebroplasty: a systematic review and meta-analysis.J Spinal Disord Tech. 2013;26(4):E150-157.[37] Yoo CM,Park KB,Hwang SH,et al.The analysis of patterns and risk factors of newly developed vertebral compression fractures after percutaneous vertebroplasty.J Korean Neurosurg Soc. 2012;52(4):339-345.[38] Han SL,Wan SL,Li QT,et al.Is vertebroplasty a risk factor for subsequent vertebral fracture,meta-analysis of published evidence?Osteoporos Int.2015;26(1):113-122.[39] Villarraga ML,Bellezza AJ,Harrigan TP,et al.The biomechanical effects of kyphoplasty on treated and adjacent nontreated vertebral bodies.J Spinal Disord Tech. 2005;18(1): 84-91.[40] Fan B,Wei Z,Zhou X,et al.Does vertebral augmentation lead to an increasing incidence of adjacent vertebral failure ? A systematic review and meta-analysis.Int J Surg.2016;36(Pt A):369-376.[41] 王强.椎体强化治疗骨质疏松椎体压缩骨折[J].中国组织工程研究,2015,19(53):8661.[42] 罗晓彬.胸腰段骨折经皮骨水泥强化复位疗效分析[J].湖南师范大学学报(医学版),2018,15(1):181-183.[43] 梁得华,鲁世保.有限元分析法在胸腰段脊柱骨折的应用进展[J].北京医学,2016,38(7):706-708.[44] 程真,陈贵月,郭家斌,等.唑来膦酸对骨质疏松性压缩骨折患者经皮椎体成形术术后骨密度及临床症状的影响[J].山西医药杂志, 2017,46(2):167-170.[45] Yokoyama K,Kawanishi M,Yamada M,et al.Safety and therapeutic efficacy of the second treatment for new fractures developed after initial vertebroplasty performed for painful vertebral compression fractures.Neurol Res. 2013;35(6): 608-613. |
| [1] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [2] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [3] | Liu Lihua, Sun Wei, Wang Yunting, Gao Fuqiang, Cheng Liming, Li Zirong, Wang Jiangning. Type L1 steroid-induced osteonecrosis of the femoral head through femoral head and neck junction decompression by fenestration: a single-center prospective clinical study [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 906-911. |
| [4] | Xu Dongzi, Zhang Ting, Ouyang Zhaolian. The global competitive situation of cardiac tissue engineering based on patent analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 807-812. |
| [5] | Wu Zijian, Hu Zhaoduan, Xie Youqiong, Wang Feng, Li Jia, Li Bocun, Cai Guowei, Peng Rui. Three-dimensional printing technology and bone tissue engineering research: literature metrology and visual analysis of research hotspots [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 564-569. |
| [6] | Chang Wenliao, Zhao Jie, Sun Xiaoliang, Wang Kun, Wu Guofeng, Zhou Jian, Li Shuxiang, Sun Han. Material selection, theoretical design and biomimetic function of artificial periosteum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 600-606. |
| [7] | Liu Fei, Cui Yutao, Liu He. Advantages and problems of local antibiotic delivery system in the treatment of osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 614-620. |
| [8] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [9] | Zhang Zhenkun, Li Zhe, Li Ya, Wang Yingying, Wang Yaping, Zhou Xinkui, Ma Shanshan, Guan Fangxia. Application of alginate based hydrogels/dressings in wound healing: sustained, dynamic and sequential release [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 638-643. |
| [10] | Chen Jiana, Qiu Yanling, Nie Minhai, Liu Xuqian. Tissue engineering scaffolds in repairing oral and maxillofacial soft tissue defects [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 644-650. |
| [11] | Xie Zhifeng, Liu Qing, Liu Bing, Zhang Tao, Li Kun, Zhang Chunqiu, Sun Yanfang. Biomechanical characteristics of the lumbar disc after fatigue injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 339-343. |
| [12] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [13] | Zeng Xianghong, Liang Bowei. A new strategy for the treatment of osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 431-437. |
| [14] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [15] | Liu Jinyu, Ding Yiwei, Lu Zhengcao, Gao Tianjun, Cui Hongpeng, Li Wen, Du Wei, Ding Yu. Finite element biomechanical study of full endoscopic fenestration decompression for cervical spondylotic myelopathy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3850-3854. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||