Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (23): 3699-3703.doi: 10.12307/2024.417
Previous Articles Next Articles
The causal relationship between blood lipids and muscle atrophy based on Mendelian randomization analysis of two samples
Peng Zhihua, Pan Junxi, Feng Qinghui, Tian Tianzhao, Zhang Sheng, Li An, Cai Yingfeng
- The Affiliated TCM Hospital of Guangzhou Medical University, Guangzhou 510000, Guangdong Province, China
-
Received:2023-05-21Accepted:2023-07-15Online:2024-08-18Published:2023-09-13 -
Contact:Cai Yingfeng, Chief physician, The Affiliated TCM Hospital of Guangzhou Medical University -
About author:Peng Zhihua, Associate chief physician, The Affiliated TCM Hospital of Guangzhou Medical University, Guangzhou 510000, Guangdong Province, China -
Supported by:Chinese Medicine Research Project of Guangdong Provincial Administration of Traditional Chinese Medicine, No. 20222182 (to PZH)
CLC Number:
Cite this article
Peng Zhihua, Pan Junxi, Feng Qinghui, Tian Tianzhao, Zhang Sheng, Li An, Cai Yingfeng. The causal relationship between blood lipids and muscle atrophy based on Mendelian randomization analysis of two samples[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3699-3703.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
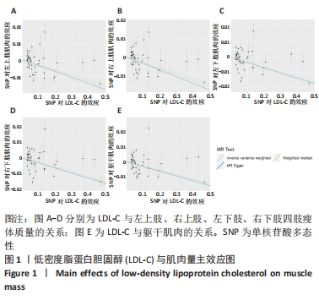
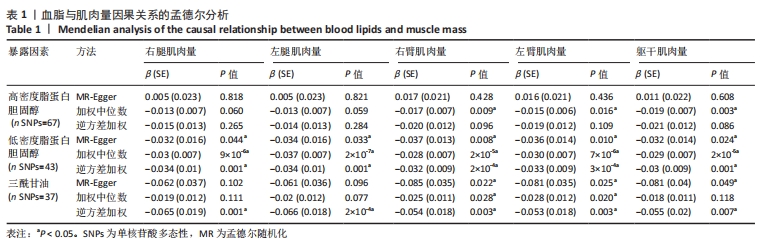
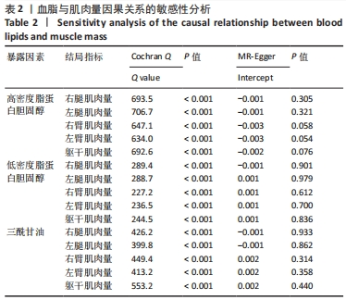
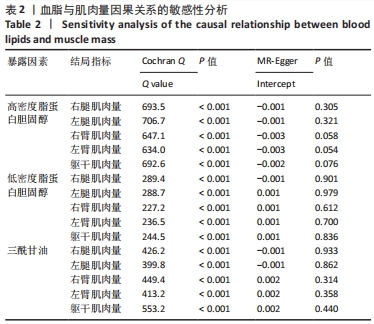
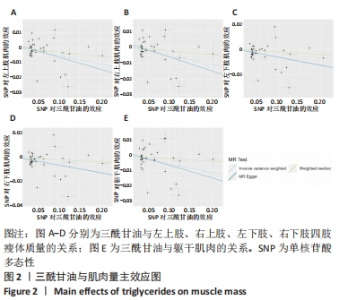
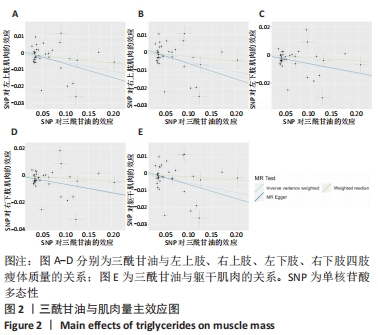
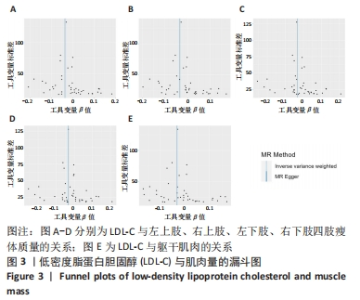
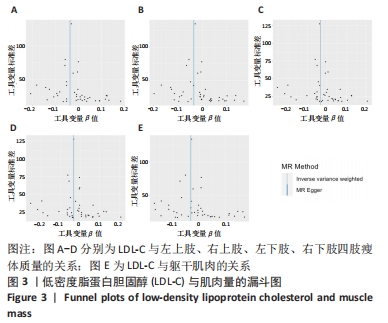
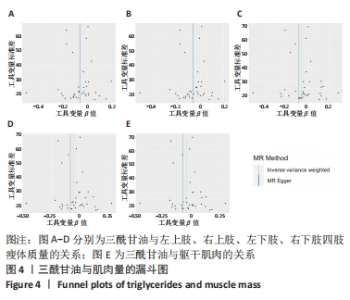
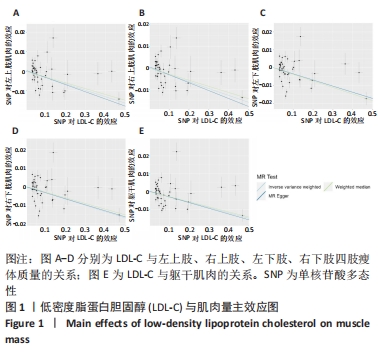
2.3 脂质代谢与躯干肌肉量的因果关系 此外,结果还发现躯干肌肉量与LDL-C和三酰甘油均存在负相关关系(β值均小于0且P < 0.01),见表1,但未发现其与HDL-C的相关性。异质性检验显示所选工具变量之间存在显著异质性(P < 0.01),见表2。考虑到这一点,以上所有MR分析中均使用具有随机效应的逆方差加权方法。每个MR方法的单个SNP效应和组合效应均在散点图中进行可视化(图1,2)。MR-Egger 分析未检测到工具变量中存在定向多效性(P > 0.05),证明因果关系稳健。此外,漏斗图是各个SNP所代表的点为对称分布,表明工具变量不存在多效性(图3,4)。MR-Egger 分析未检测到工具变量中存在定向多效性 (P > 0.05),证明因果关系稳健。结果表明LDL-C和三酰甘油对四肢肌肉和躯干肌肉具有负相关因果关系。"
| [1] JANSSEN I, SHEPARD DS, KATZMARZYK PT, et al. The healthcare costs of sarcopenia in the United States. J Am Geriatr Soc. 2004;52(1):80-85. [2] GANAPATHY A, NIEVES JW. Nutrition and Sarcopenia-What Do We Know? Nutrients. 2020;12(6):1755. [3] 郑振泉,荣杰生.肌肉减少症:与年龄相关的肌量流失和功能下降[J]. 中国组织工程研究,2022,26(5): 792-797. [4] 杜娟,杨玲,黄乙欢,等.肌肉减少症治疗研究进展[J]. 中国老年学杂志,2022, 42(2): 506-511. [5] KANIS JA, ADACHI JD, COOPER C, et al. Standardising the descriptive epidemiology of osteoporosis: recommendations from the Epidemiology and Quality of Life Working Group of IOF. Osteoporos Int. 2013;24(11):2763-2764. [6] WALSH MC, HUNTER GR, LIVINGSTONE MB. Sarcopenia in premenopausal and postmenopausal women with osteopenia, osteoporosis and normal bone mineral density. Osteoporos Int. 2006;17(1):61-67. [7] 杨玲,杜娟,刘荣雁,等.肌肉减少症病因学研究现状与展望[J]. 中国骨质疏松杂志,2020,26(11):1689-1693. [8] HIRSCHFELD HP, KINSELLA R, DUQUE G. Osteosarcopenia: where bone, muscle, and fat collide. Osteoporos Int. 2017;28(10):2781-2790. [9] VELLA CA, NELSON MC, UNKART JT, et al. Skeletal muscle area and density are associated with lipid and lipoprotein cholesterol levels: The Multi-Ethnic Study of Atherosclerosis. J Clin Lipidol. 2020;14(1):143-153. [10] DU Y, OH C, NO J. Associations between Sarcopenia and Metabolic Risk Factors: A Systematic Review and Meta-Analysis. J Obes Metab Syndr. 2018;27(3):175-185. [11] BOEF AG, DEKKERS OM, LE CESSIE S. Mendelian randomization studies: a review of the approaches used and the quality of reporting. Int J Epidemiol. 2015;44(2): 496-511. [12] LAWLOR DA, HARBORD RM, STERNE JA, et al. Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med. 2008;27(8):1133-1163. [13] ZHENG J, BAIRD D, BORGES MC, et al. Recent Developments in Mendelian Randomization Studies. Curr Epidemiol Rep. 2017;4(4):330-345. [14] 王玉琢, 沈洪兵. 孟德尔随机化研究应用于因果推断的影响因素及其结果解读面临的挑战[J]. 中华流行病学杂志,2020,41(8):1231-1236. [15] HOWE LJ, NIVARD MG, MORRIS TT, et al. Within-sibship genome-wide association analyses decrease bias in estimates of direct genetic effects. Nat Genet. 2022; 54(5):581-592. [16] SUDLOW C, GALLACHER J, ALLEN N, et al. UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med. 2015;12(3):e1001779. [17] BUCKINX F, LANDI F, CESARI M, et al. Pitfalls in the measurement of muscle mass: a need for a reference standard. J Cachexia Sarcopenia Muscle. 2018;9(2):269-278. [18] ZILLIKENS MC, DEMISSIE S, HSU YH, et al. Large meta-analysis of genome-wide association studies identifies five loci for lean body mass. Nat Commun. 2017; 8(1):80. [19] LIU HM, ZHANG Q, SHEN WD, et al. Sarcopenia-related traits and coronary artery disease: a bi-directional Mendelian randomization study. Aging (Albany NY). 2020; 12(4):3340-3353. [20] EVANS DM, DAVEY SMITH G. Mendelian Randomization: New Applications in the Coming Age of Hypothesis-Free Causality. Annu Rev Genomics Hum Genet. 2015; 16:327-350. [21] DIDELEZ V, SHEEHAN N. Mendelian randomization as an instrumental variable approach to causal inference. Stat Methods Med Res. 2007;16(4):309-330. [22] BOWDEN J, DEL GRECO MF, MINELLI C, et al. Assessing the suitability of summary data for two-sample Mendelian randomization analyses using MR-Egger regression: the role of the I2 statistic. Int J Epidemiol. 2016;45(6):1961-1974. [23] BOWDEN J, DAVEY SMITH G, HAYCOCK PC, et al. Consistent Estimation in Mendelian Randomization with Some Invalid Instruments Using a Weighted Median Estimator. Genet Epidemiol. 2016;40(4):304-314. [24] BURGESS S, DUDBRIDGE F, THOMPSON SG. Combining information on multiple instrumental variables in Mendelian randomization: comparison of allele score and summarized data methods. Stat Med. 2016;35(11):1880-1906. [25] HEMANI G, ZHENG J, ELSWORTH B, et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife. 2018;7:e34408. [26] DWIPA L, HIDAYAT S, PERMADI SE, et al. Association of Appendicular Skeletal Muscle Mass and Central Obesity Parameters with Lipid Profiles in Older Women. J Med Sci. 2021;9(B):921-924. [27] BAEK SJ, NAM GE, HAN KD, et al. Sarcopenia and sarcopenic obesity and their association with dyslipidemia in Korean elderly men: the 2008-2010 Korea National Health and Nutrition Examination Survey. J Endocrinol Invest. 2014; 37(3):247-260. [28] LENT-SCHOCHET D, JIALAL I. Biochemistry, Lipoprotein Metabolism StatPearls [Internet]. StatPearls Publishing. 2022. [29] YING Z, TRAMPER N, ZHOU E, et al. Role of thermogenic adipose tissue in lipid metabolism and atherosclerotic cardiovascular disease: lessons from studies in mice and humans. Cardiovasc Res. 2023;119(4):905-918. [30] WONDMKUN YT. Obesity, Insulin Resistance, and Type 2 Diabetes: Associations and Therapeutic Implications. Diabetes Metab Syndr Obes. 2020;13:3611-3616. [31] JI Y, LI M, CHANG M, et al. Inflammation: Roles in Skeletal Muscle Atrophy. Antioxidants (Basel). 2022;11(9):1686. [32] HAMRICK MW. The skeletal muscle secretome: an emerging player in muscle-bone crosstalk. Bonekey Rep. 2012;1:60. [33] LI CW, YU K, SHYH-CHANG N, et al. Pathogenesis of sarcopenia and the relationship with fat mass: descriptive review. J Cachexia Sarcopenia Muscle. 2022;13(2):781-794. [34] SHAH VO, SCARIANO J, WATERS D, et al. Mitochondrial DNA deletion and sarcopenia. Genet Med. 2009;11(3):147-152. [35] AGUIRRE GA, DE ITA JR, DE LA GARZA RG, et al. Insulin-like growth factor-1 deficiency and metabolic syndrome. J Transl Med. 2016;14:3. [36] LI Z, XU K, GUO Y, et al. A high-fat diet reverses metabolic disorders and premature aging by modulating insulin and IGF1 signaling in SIRT6 knockout mice. Aging Cell. 2020;19(3):e13104. |
| [1] | Guo Sutong, Feng Dehong, Guo Yu, Wang Ling, Ding Yujian, Liu Yi, Qian Zhengying, Li Mingyang. Construction and finite element analysis of normal and osteoporotic hip models [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1342-1346. |
| [2] | Zhang Xiaoyun, Liu Hua, Chai Yuan, Chen Feng, Zeng Hao, Gao Zhengang, Huang Yourong. Effect of Yishen Gushu Formula on bone metabolic markers and clinical efficacyn in patients with osteoporosis of kidney deficiency and blood stasis type [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1155-1160. |
| [3] | Wang Ji, Zhang Min, Li Wenbo, Yang Zhongya, Zhang Long. Effect of aerobic exercise on glycolipid metabolism, skeletal muscle inflammation and autophagy in type 2 diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1200-1205. |
| [4] | Dai Yuexing, Zheng Liqin, Wu Minhui, Li Zhihong, Li Shaobin, Zheng Desheng, Lin Ziling. Effect of vessel number on computational fluid dynamics in vascular networks [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1206-1210. |
| [5] | Zhang Min, Peng Jing, Zhang Qiang, Chen Dewang. Mechanical properties of L3/4 laminar decompression and intervertebral fusion in elderly osteoporosis patients analyzed by finite element method [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 847-851. |
| [6] | Xue Xiaofeng, Wei Yongkang, Qiao Xiaohong, Du Yuyong, Niu Jianjun, Ren Lixin, Yang Huifeng, Zhang Zhimin, Guo Yuan, Chen Weiyi. Finite element analysis of osteoporosis in proximal femur after cannulated screw fixation for femoral neck fracture [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 862-867. |
| [7] | Kaiyisaier•Abudukelimu, Maimaitimin•Abulimiti, Li Lei, Yang Xiaokai, Zhang Yukun, Liu Shuai. Effect of lumbar CT values in the diagnosis of osteoporosis in women patients with lumbar degenerative diseases [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 945-949. |
| [8] | Wang Liping, Lian Tianxing, Hu Yongrong, Yang Hongsheng, Zeng Zhimou, Liu Hao, Qu Bo. HU value of chest CT vertebral body in the opportunistic screening of type 2 diabetes mellitus osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 950-954. |
| [9] | Yu Zhaoyu, Tan Lixin, Sun Kai, Lu Yao, Li Yong. Meta-analysis of cement-augmented pedicle screw for thoracolumbar degenerative diseases with osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(5): 813-820. |
| [10] | Wei Yuanxun, Chen Feng, Lin Zonghan, Zhang Chi, Pan Chengzhen, Wei Zongbo. The mechanism of Notch signaling pathway in osteoporosis and its prevention and treatment with traditional Chinese medicine [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 587-593. |
| [11] | Abuduwupuer·Haibier, Alimujiang·Yusufu, Maihemuti·Yakufu, Maimaitimin·Abulimiti, Tuerhongjiang·Abudurexiti. Meta-analysis of efficacy and safety of terlipatide and bisphosphate in the treatment of postmenopausal osteoporosis fractures [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(4): 639-645. |
| [12] | Xie Ting, Liu Tingting, Zeng Xuehui, Li Yamin, Zhou Panghu, Yi Nianhua. Fucoxanthin alleviates glucocorticoid-induced osteoblast apoptosis by activating nuclear factor erythroid-2-related factor 2 [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3609-3614. |
| [13] | Lin Chubin, He Xingpeng, Qiu Yuhui, Wu Wenjin, Chang Yu, Ye Tao, Li Pengfei, Yang Jian. Biomechanical analysis of the bones in a rat model of osteoporosis based on the combination of disease and syndrome [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3636-3641. |
| [14] | Yao Ting, Guan Rongwei, Gao Yuan. Overexpression of SMAD4 interferes with the expression of iron metabolism related proteins in osteoporotic rats [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3648-3653. |
| [15] | Wu Ruiqi, Zhou Yi, Xia Tian, Zhang Chi, Yang Qipei, Zhang Xuan, Zhang Yazhong, Cui Wei. Mendelian randomization study on the association between rheumatoid arthritis and osteoporosis and bone mineral density [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(23): 3715-3721. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||