Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (18): 2846-2851.doi: 10.12307/2024.034
Previous Articles Next Articles
Comparison of gait and hip ambulation ability after total hip arthroplasty through different approaches
Pan Yunchun1, Wei Hongjun2, Ren Guoqing3, Zhang Qiliang3
- 1Department of Orthopedics, Pingdu People’s Hospital, Qingdao 266700, Shandong Province, China; 2Qingdao Municipal Hospital (East Ward), Qingdao 266071, Shandong Province, China; 3Department of Joint and Sports Medicine, Qingdao Municipal Hospital, Qingdao 266071, Shandong Province, China
-
Received:2023-02-14Accepted:2023-04-04Online:2024-06-28Published:2023-08-24 -
Contact:Zhang Qiliang, Associate chief physician, Department of Joint and Sports Medicine, Qingdao Municipal Hospital, Qingdao 266071, Shandong Province, China -
About author:Pan Yunchun, Associate chief physician, Department of Orthopedics, Pingdu People’s Hospital, Qingdao 266700, Shandong Province, China -
Supported by:Qingdao Medical Science and Technology Guidance Program in 2019, No. 2019-WJZD020 (to ZQL)
CLC Number:
Cite this article
Pan Yunchun, Wei Hongjun, Ren Guoqing, Zhang Qiliang. Comparison of gait and hip ambulation ability after total hip arthroplasty through different approaches[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2846-2851.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

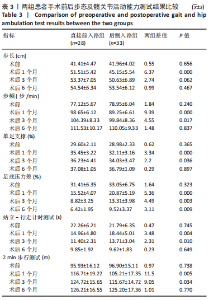
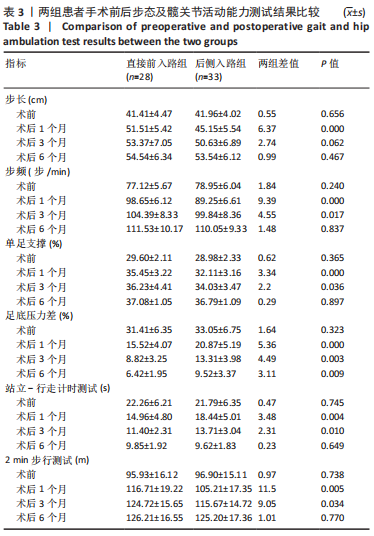
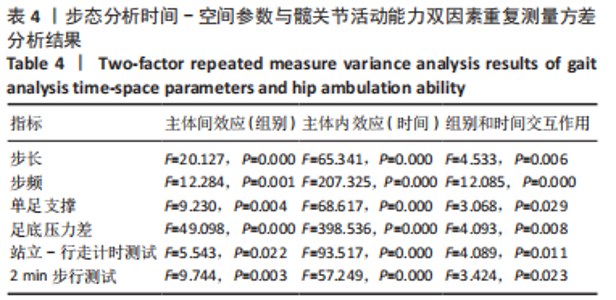
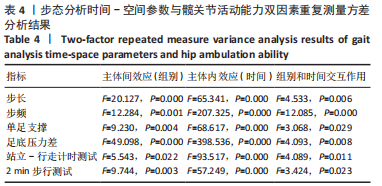
双因素重复测量方差分析:主体间效应检验结果证实,两组患者的步态分析时间-空间参数测试结果比较差异有显著性意义(P < 0.01),直接前入路组优于后侧入路组;主体内效应检验结果显示,两组患者不同时间的步态分析时间-空间参数测试结果比较差异存有显著性意义(P < 0.01),随着时间的延长,两组患者的步态分析时间-空间参数逐步改善;组别和时间之间存在交互效应(P < 0.05),提示步态随着时间变化的趋势会因为分组的不同而不同,需要对不同时点分组的简单效应进行分析。 不同时间点步态分析时间-空间参数的简单效应检验结果显示,两组患者术前的步态分析时间-空间参数测试结果比较差异无显著性意义(P > 0.05);直接前入路组患者术后1个月的步长、步频、单足支撑时间、足底压力差测试结果均优于后侧入路组(P < 0.05),术后3个月的步频、单足支撑时间、足底压力差测试结果优于后侧入路组(P < 0.05),术后6个月的足底压力差测试结果优于后侧入路组(P < 0.01)。 2.5 两组患者髋关节运动功能测试结果 两组患者不同时间点的站立-行走计时测试及2 min步行测试情况见表3。站立-行走计时测试及2 min步行测试的双因素重复测量方差分析结果见表4。 双因素重复测量方差分析:主体间效应检验结果证实,两组患者的站立-行走计时测试及2 min步行测试结果比较差异有显著性意义(P < 0.01),直接前入路组优于后侧入路组;主体内效应检验结果证实,两组患者不同时间点的站立-行走计时测试及2 min步行测试结果比较差异有显著性意义(P < 0.01),随着时间的延长,两组患者的站立-行走计时测试及2 min步行测试逐步改善;组别和时间之间存在交互效应(P < 0.05),提示站立-行走计时测试及2 min步行测试结果随着时间变化的趋势会因为分组的不同而不同,需要对不同时点分组的简单效应进行分析。 不同时间点站立-行走计时测试及2 min步行测试的简单效应检验结果显示,两组患者术前的站立-行走计时测试及2 min步行测试结果比较差异无显著性意义(P > 0.05);直接前入路组患者术后1,3个月的站立-行走计时测试及2 min步行测试结果优于后侧入路组(P < 0.05),术后6个月两组患者的站立-行走计时测试及2 min步行测试结果比较差异无显著性意义(P > 0.05)。 2.6 不良反应 两组测试过程中未发生任何不良事件。随访过程中,两组患者均未发生与植入物相关的不良反应。"

| [1] MCCRORY JL, WHITE SC, LIFESO RM. Vertical ground reaction forces: objective measures of gait following hip arthroplasty. Gait Posture. 2001;14(2):104-109. [2] MANTOVANI G, LAMONTAGNE M, VARIN D, et al. Comparison of total hip arthroplasty surgical approaches by principal component analysis. J Biomech. 2012;45(12):2109-2115. [3] LALEVÉE M, MARTINEZ L, REY B, et al. Gait analysis after total hip arthroplasty by direct minimally invasive anterolateral approach: A controlled study. Orthop Traumatol Surg Res. 2022;103521. doi: 10.1016/j.otsr.2022.103521. [4] HOSKINS W, BINGHAM R, LORIMER M, et al. Early Rate of Revision of Total Hip Arthroplasty Related to Surgical Approach: An Analysis of 122,345 Primary Total Hip Arthroplasties. J Bone Joint Surg Am. 2020;102(21):1874-1882. [5] YAN L, GE L, DONG S, et al. Evaluation of Comparative Efficacy and Safety of Surgical Approaches for Total Hip Arthroplasty: A Systematic Review and Network Meta-analysis. JAMA Netw Open. 2023;6(1):e2253942. [6] PINCUS D, JENKINSON R, PATERSON M, et al. Association Between Surgical Approach and Major Surgical Complications in Patients Undergoing Total Hip Arthroplasty. JAMA. 2020;323(11):1070-1076. [7] HUANG XT, LIU DG, JIA B, et al. Comparisons between Direct Anterior Approach and Lateral Approach for Primary Total Hip Arthroplasty in Postoperative Orthopaedic Complications: A Systematic Review and Meta-Analysis. Orthop Surg. 2021;13(6):1707-1720. [8] STADELMANN VA, RÜDIGER HA, NAUER S, et al. Impact of capsular preservation on patient-reported outcomes and complication rates in total hip arthroplasty using the direct anterior approach. Bone Joint J. 2022;104-B(7):826-832. [9] RIVERA F, COMBA LC, BARDELLI A. Direct anterior approach hip arthroplasty: How to reduce complications - A 10-years single center experience and literature review. World J Orthop. 2022;13(4):388-399. [10] WANG Z, HOU JZ, WU CH, et al. A systematic review and meta-analysis of direct anterior approach versus posterior approach in total hip arthroplasty. J Orthop Surg Res. 2018;13(1):229-240. [11] JIA F, GUO B, XU F, et al. A comparison of clinical, radiographic and surgical outcomes of total hip arthroplasty between direct anterior and posterior approaches: a systematic review and meta-analysis. Hip Int. 2019;29(6):584-596. [12] MOERENHOUT K, DEROME P, LAFLAMME GY, et al. Direct anterior versus posterior approach for total hip arthroplasty: a multicentre, prospective, randomized clinical trial. Can J Surg. 2020;63(5):E412-E417. [13] MAFFIULETTI NA, IMPELLIZZERI FM, WIDLER K, et al. Spatiotemporal parameters of gait after total hip replacement: anterior versus posterior approach. Orthop Clin North Am. 2009;40(3):407-415. [14] BON G, KACEM EB, LEPRETRE PM, et al. Does the direct anterior approach allow earlier recovery of walking following total hip arthroplasty? A randomized prospective trial using accelerometry. Orthop Traumatol Surg Res. 2019;105(3): 445-452. [15] LIN DY, SAMSON AJ, CEHIC MG, et al. Short-term difference only in reported outcomes (PROMs) after anterior or posterior approach to total hip arthroplasty: a 4-year prospective multi-centre observational study. J Orthop Surg Res. 2023; 18(1):119. [16] PINCUS D, JENKINSON R, PATERSON M, et al. Association Between Surgical Approach and Major Surgical Complications in Patients Undergoing Total Hip Arthroplasty. JAMA. 2020;323(11):1070-1076. [17] PENG L, ZENG Y, WU Y, et al. Clinical, functional and radiographic outcomes of primary total hip arthroplasty between direct anterior approach and posterior approach: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2020;21:338. [18] AWAD ME, FARLEY BJ, MOSTAFA G, et al. Direct anterior approach has short-term functional benefit and higher resource requirements compared with the posterior approach in primary total hip arthroplasty : a meta-analysis of functional outcomes and cost. Bone Joint J. 2021;103-B(6):1078-1087. [19] JUNGWIRTH-WEINBERGER A, DO HT, KRELL EC, et al. Blood management in direct anterior versus posterior primary total hip arthroplasty using tranexamic acid: a matched cohort study. Arch Orthop Trauma Surg. 2023;143(1):91-95. [20] CHA Y, YOO JI, KIM JT, et al. Disadvantage during Perioperative Period of Total Hip Arthroplasty Using the Direct Anterior Approach: a Network Meta-Analysis. J Korean Med Sci. 2020;35(18):e111. [21] FAGOTTI L, FALOTICO GG, MARANHO DA, et al. Posterior versus anterior approach to total hip arthroplasty: a systematic review and meta‑analysis of randomized controlled trials. Acta Ortop Bras. 2021;29(6):297-303. [22] NILSDOTTER A, BREMANDER A. Measures of hip function and symptoms: Harris Hip Score (HHS), Hip Disability and Osteoarthritis Outcome Score (HOOS), Oxford Hip Score (OHS), Lequesne Index of Severity for Osteoarthritis of the Hip (LISOH), and American Academy of Orthopedic Surgeons (AAOS) Hip and Knee Questionnaire. Arthritis Care Res (Hoboken). 2011;63( Suppl 11):S200-S207. [23] NAMBIAR M, CHENG TE, ONGGO JR, et al. No Difference in Functional, Radiographic, and Survivorship Outcomes Between Direct Anterior or Posterior Approach THA: 5-Year Results of a Randomized Trial. Clin Orthop Relat Res. 2021; 479(12): 2621-2629. [24] AWAD ME, FARLEY BJ, MOSTAFA G, et al. The risk of hospital readmission, revision, and intra- and postoperative complications between direct anterior versus posterior approaches in primary total hip arthroplasty: a stratified meta-analysis and a probability based cost projection. Hip Int. 2022;11207000211066454.doi: 10.1177/11207000211066454. [25] BOEKESTEIJN R, SMOLDERS J, BUSCH V, et al. Objective monitoring of functional recovery after total knee and hip arthroplasty using sensor-derived gait measures. PeerJ. 2022;10:e14054. [26] KAUFMANN M, NÜESCH C, CLAUSS M, et al. Functional assessment of total hip arthroplasty using inertial measurement units: Improvement in gait kinematics and association with patient-reported outcome measures. J Orthop Res. 2023; 41(4):759-770. [27] RITTER MA, HARTY LD, KEATING ME, et al. A clinical comparison of the anterolateral and posterolateral approaches to the hip. Clin Orthop Relat Res. 2001;4(385):95-99. [28] FOUCHER KC, FREELS S. Preoperative factors associated with postoperative gait kinematics and kinetics after total hip arthroplasty. Osteoarthritis Cartilage. 2015; 23(10):1685-1694. [29] NELMS NJ, BIRCH CE, HALSEY DH, et al. Assessment of Early Gait Recovery After Anterior Approach Compared to Posterior Approach Total Hip Arthroplasty: A Smartphone Accelerometer-Based Study. J Arthroplasty. 2020;35(2):465-470. [30] ZHAO HY, KANG PD, XIA YY, et al. Comparison of Early Functional Recovery After Total Hip Arthroplasty Using a Direct Anterior or Posterolateral Approach: A Randomized Controlled Trial. J Arthroplasty. 2017;32(11):3421-3428. [31] BERGIN PF, DOPPELT JD, KEPHART CJ, et al. Comparison of minimally invasive direct anterior versus posterior total hip arthroplasty based on inflammation and muscle damage markers. J Bone Joint Surg Am. 2011;93(15):1392-1398. [32] ZHANG B, LIU S, LIU Z, et al. Clinical and radiologic outcomes in patients undergoing primary total hip arthroplasty with Collum Femoris Preserving stems: a comparison between the direct anterior approach and the posterior approach. BMC Musculoskelet Disord. 2022;23(1):77. [33] RATHOD PA, ORISHIMO KF, KREMENIC IJ, et al. Similar improvement in gait parameters following direct anterior & posterior approach total hip arthroplasty. J Arthroplasty. 2014;29(6):1261-1264. [34] HÄKKINEN A, BORG H, KAUTIAINEN H, et al. Muscle strength and range of movement deficits 1 year after hip resurfacing surgery using posterior approach. Disabil Rehabil. 2010;32(6):483-491. [35] OUNPUU S. The biomechanics of walking and running. Clin Sports Med. 1994; 13(4):843-863. [36] BORG H, KIVIRANTA I, ANTTILA E, et al. External rotation strength deficit after hip resurfacing surgery. Disabil Rehabil. 2009;31(11):865-870. [37] ZAMPOGNA B, PAPALIA GF, PARISI FR, et al. Early return to activity of daily living after total hip arthroplasty: a systematic review and meta-analysis. Hip Int. 2022; 11207000221146116. [38] YUKSEL E, UNVER B, KALKAN S, et al. Reliability and minimal detectable change of the 2-minute walk test and Timed Up and Go test in patients with total hip arthroplasty. Hip Int. 2021;31(1):43-49. [39] JUNG H, MIKI Y, TANAKA R, et al. The Effects of a Multicomponent Lower Extremity Training Technique on Physical Function in Healthy Older Adults: A Randomized Controlled Trial. Gerontol Geriatr Med. 2020;6:2333721420935702. [40] JUNG H, YAMASAKI M. Association of lower extremity range of motion and muscle strength with physical performance of community-dwelling older women. J Physiol Anthropol. 2016;35(1):30. [41] BARRETT WP, TURNER SE, LEOPOLD JP. Prospective randomized study of direct anterior vs postero-lateral approach for total hip arthroplasty. J Arthroplasty. 2013;28(9):1634-1638. [42] RODRIGUEZ JA, DESHMUKH AJ, RATHOD PA, et al. Does the direct anterior approach in THA offer faster rehabilitation and comparable safety to the posterior approach? Clin Orthop Relat Res. 2014;472(2):455-463. [43] SHEN J, JI R, YAO S, et al. Direct Anterior Approach Provides Superior Prosthesis Adaptability in the Early Postoperative Period of Total Hip Arthroplasty. Orthop Surg. 2023;15(3):679-686. |
| [1] | Li Yongjie, Fu Shenyu, Xia Yuan, Zhang Dakuan, Liu Hongju. Correlation of knee extensor muscle strength and spatiotemporal gait parameters with peak knee flexion/adduction moment in female patients with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1354-1358. |
| [2] | Min Meipeng, Wu Jin, URBA RAFI, Zhang Wenjie, Gao Jia, Wang Yunhua, He Bin, Fan Lei. Role and significance of artificial intelligence preoperative planning in total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1372-1377. |
| [3] | Zhang Zeyi, Yang Yimin, Li Wenyan, Zhang Meizhen. Effect of foot progression angle on lower extremity kinetics of knee osteoarthritis patients of different ages: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 968-975. |
| [4] | Chang Wanpeng, Zhang Zhongwen, Yang Yulin, Zi Yang, Yang Mengqi, Du Bingyu, Wang Nan, Yu Shaohong. Efficacy of rehabilitation exoskeleton robots on post-stroke lower limb motor dysfunction: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(2): 321-328. |
| [5] | Zhu Chenchen, Yin Yuan, Zhou Yingji, Ma Tingting, Su Liyao, Zhang Ming. Effects of body mass index on plantar pressure [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2808-2813. |
| [6] | Zhang Liying, Ding Yuwu, Yu Xiaoming, Liao Wangsheng, Wang Jiening. Body weight support Tai Chi footwork improves balance function after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2840-2845. |
| [7] | Chen Modi, Sun Qibo, Xu Tianyu, Tai Guoliang, Zhao Yuxiang, Pan Zhaohui. Biomechanics of reconstruction of total calcaneus defect using fibular flap based on finite element method [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(12): 1805-1809. |
| [8] | Zhang Kai, Guo Zhuotao, Ma Qiaoqiao, Zha Guochun, Guo Kaijin. Accuracy and influencing factor of artificial intelligence planning system in patients undergoing total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(12): 1863-1868. |
| [9] | Gu Xu, Zheng Xin, Shi Sifeng, Lu Renxiang, Cao Jie, Li Hongwei. Stability of early gait after unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(12): 1875-1879. |
| [10] | Ke Yuqi, Chen Changjian, Wu Hao, Zheng Lianjie. Comparison of 12-month follow-up results of primary total hip arthroplasty between modified direct anterior approach and direct anterior approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1377-1382. |
| [11] | Yu Wenqiang, Ren Fuchao, Shi Guohong, Xu Yuanjing, Liu Tongyou, Xie Youzhuan, Wang Jinwu, . Methods and application of gait analysis of lower limbs after stroke [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1257-1263. |
| [12] | Li Shihao, Li Qi, Li Zhen, Zhang Yuanyuan, Liu Miaomiao, Ouyang Yi, Xu Weiguo. Plantar pressure and gait analysis in patients with anterior cruciate ligament injury and reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 626-631. |
| [13] | Liang Xiao, Zhao Panchao, Li Jiahui, Ji Zhongqiu, Jiang Guiping. Gait and biomechanical characteristics of lower limbs in multi-task walking of 4-6-year-old children [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 505-512. |
| [14] | Yan Ruizhong, Li Jiahui, Lin Shuzhong, Wu Xiaogang, Guo Zhijian, Liu Wenqi, Liu Qiang. Effect of pelvic tilt on the stress at the acetabular side in standing position after total hip arthroplasty: finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(36): 5795-5800. |
| [15] | Guo Zhuotao, Zhang Kai, Zha Guochun, Guo Kaijin. A matched controlled trial of lumbar fusion effect on mid-term outcomes after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(36): 5801-5805. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||