Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (16): 2461-2466.doi: 10.12307/2022.241
Comparison of biomechanical properties of calcium phosphate/polymethyl methacrylate composite bone cement and polymethyl methacrylate bone cement
Li Shengkai1, 2, Li Tao2, Wei Chao2, Shi Ming2
- 1The First Clinical Medical College of Binzhou Medical College, Binzhou 256600, Shandong Province, China; 2Zibo Central Hospital, Zibo 255000, Shandong Province, China
-
Received:2020-11-30Revised:2020-12-04Accepted:2021-01-09Online:2022-06-08Published:2021-10-29 -
Contact:Li Tao, MD, Doctoral supervisor, Professor, Zibo Central Hospital, Zibo 255000, Shandong Province, China -
About author:Li Shengkai, Master candidate, The First Clinical Medical College of Binzhou Medical College, Binzhou 256600, Shandong Province, China; Zibo Central Hospital, Zibo 255000, Shandong Province, China
CLC Number:
Cite this article
Li Shengkai, Li Tao, Wei Chao, Shi Ming. Comparison of biomechanical properties of calcium phosphate/polymethyl methacrylate composite bone cement and polymethyl methacrylate bone cement[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(16): 2461-2466.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
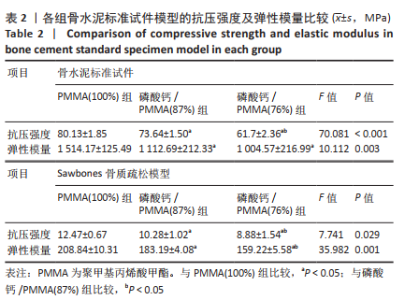
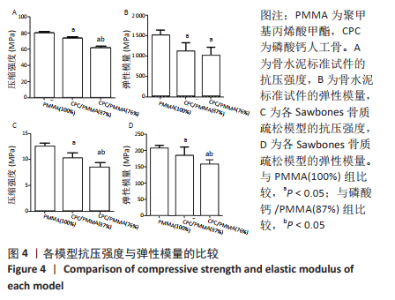
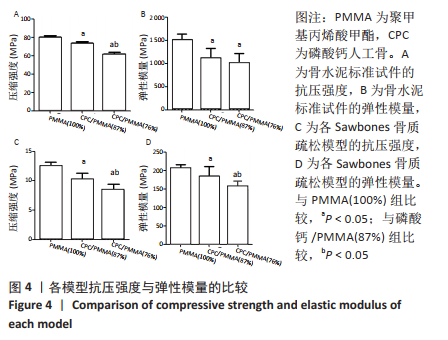
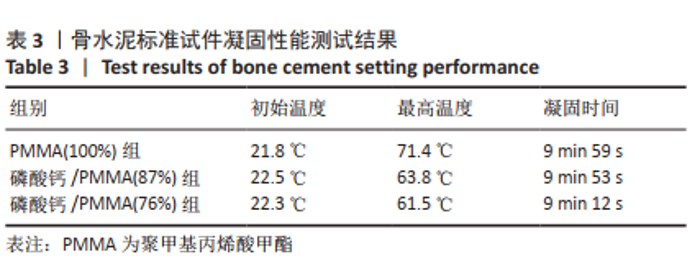
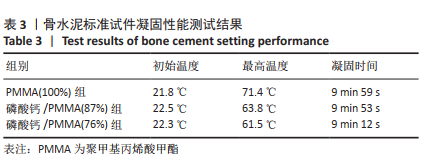
2.1 各组模型的抗压强度及弹性模量检测结果 在构建的骨水泥标准试件模型中,PMMA骨水泥及添加磷酸钙后复合骨水泥的抗压强度及弹性模量见表2,图4A、B。 磷酸钙/PMMA(87%)组、磷酸钙/PMMA(76%)组的最大抗压缩强度均低于PMMA(100%)组(P < 0.05),且磷酸钙/PMMA(76%)组的最大抗压缩强度低于磷酸钙/PMMA(87%)组(P < 0.05);磷酸钙/PMMA(87%)组、 磷酸钙/PMMA(76%)组的弹性模量均低于PMMA(100%)组(P < 0.05),磷酸钙/PMMA(87%)组与磷酸钙/PMMA(76%)组的弹性模量比较差异无显著性意义(P > 0.05)。在构建的骨质疏松模型中,PMMA骨水泥及添加磷酸钙后复合骨水泥的抗压强度及弹性模量见表2。如图4C、D所示,磷酸钙/PMMA(87%)组、磷酸钙/PMMA(76%)组的最大抗压缩强度均低于PMMA(100%)组(P < 0.05),磷酸钙/PMMA(87%)组的弹性模量高于磷酸钙/PMMA(76%)组(P < 0.05)。"
| [1] HE Z, ZHAI Q, HU M, et al. Bone cements for percutaneous vertebroplasty and balloon kyphoplasty: Current status and future developments. J Orthop Translat. 2014;3(1):1-11. [2] RIEK AE, TOWLER DA. The pharmacological management of osteoporosis. Mo Med. 2011;108(2):118-123. [3] KALLMES DF, JENSEN ME. Percutaneous vertebroplasty. Radiology. 2003;229(1):27-36. [4] WANG H, SRIBASTAV SS, YE F, et al. Comparison of Percutaneous Vertebroplasty and Balloon Kyphoplasty for the Treatment of Single Level Vertebral Compression Fractures: A Meta-analysis of the Literature. Pain Physician. 2015;18(3):209-222. [5] HEINI PF, WÄLCHLI B, BERLEMANN U. Percutaneous transpedicular vertebroplasty with PMMA: operative technique and early results. A prospective study for the treatment of osteoporotic compression fractures. Eur Spine J. 2000;9(5):445-450. [6] LIN D, HAO J, LI L, et al. Effect of Bone Cement Volume Fraction on Adjacent Vertebral Fractures After Unilateral Percutaneous Kyphoplasty. Clin Spine Surg. 2017;30(3):E270-E275. [7] FRIEDMAN CD, COSTANTINO PD, TAKAGI S, et al. BoneSource hydroxyapatite cement: a novel biomaterial for craniofacial skeletal tissue engineering and reconstruction. J Biomed Mater Res. 1998;43(4): 428-432. [8] MILLER PD. Management of severe osteoporosis. Expert Opin Pharmacother. 2016;17(4):473-488. [9] KHANNA AJ, LEE S, VILLARRAGA M, et al. Biomechanical evaluation of kyphoplasty with calcium phosphate cement in a 2-functional spinal unit vertebral compression fracture model. Spine J. 2008;8(5):770-777. [10] KIM SB, KIM YJ, YOON TL, et al. The characteristics of a hydroxyapatite-chitosan-PMMA bone cement. Biomaterials. 2004;25(26):5715-5723. [11] ORYAN A, ALIDADI S, BIGHAM-SADEGH A, et al. Healing potentials of polymethylmethacrylate bone cement combined with platelet gel in the critical-sized radial bone defect of rats. PLoS One. 2018;13(4): e0194751. [12] PAHLEVANZADEH F, BAKHSHESHI-RAD HR, ISMAIL AF, et al. Development of PMMA-Mon-CNT bone cement with superiormechanical properties and favorable biological properties for use in bone-defect treatment. Mater Lett. 2019;240:9-12. [13] BUCHTOVÁ N, D’ORLANDO A, JUDEINSTEIN P, et al. Water dynamics in silanized hydroxypropyl methylcellulose based hydrogels designed for tissue engineering. Carbohydr Polym. 2018;202:404-408. [14] BAUDÍN C, BENET T, PENA P. Effect of graphene on setting and mechanical behaviour of tricalcium phosphate bioactive cements. J Mech Behav Biomed Mater. 2019;89:33-47. [15] SMITH BT, LU A, WATSON E, SANTORO M, et al. Incorporation of fast dissolving glucose porogens and poly(lactic-co-glycolic acid) microparticles within calcium phosphate cements for bone tissue regeneration. Acta Biomater. 2018;78:341-350. [16] APARICIO JL, RUEDA C, MANCHÓN Á, et al. Effect of physicochemical properties of a cement based on silicocarnotite/calcium silicate on in vitro cell adhesion and in vivo cement degradation. Biomed Mater. 2016;11(4):045005. [17] CHEN Z, LIU H, LIU X, et al. Injectable calcium sulfate/mineralized collagen-based bone repair materials with regulable self-setting properties. J Biomed Mater Res A. 2011;99(4):554-563. [18] BAE H, SHEN M, MAURER P, et al. Clinical experience using Cortoss for treating vertebral compression fractures with vertebroplasty and kyphoplasty: twenty four-month follow-up. Spine (Phila Pa 1976). 2010;35(20):E1030-1036. [19] YANG J, ZHANG KR, FAN JP, et al.Preparation of calcium phosphate cement and polymethyl methacrylate for biological composite bone cements. Med Sci Monit. 2015;21:1162-1172. [20] HOLUB O, LÓPEZ A, BORSE V, et al. Biomechanics of low-modulus and standard acrylic bone cements in simulated vertebroplasty: A human ex vivo study. J Biomech. 2015;48(12):3258-3266. [21] ROBO C, HULSART-BILLSTRÖM G, NILSSON M, et al. In vivo response to a low-modulus PMMA bone cement in an ovine model. Acta Biomater. 2018;72:362-370. [22] RHO JY, KUHN-SPEARING L, ZIOUPOS P. Mechanical properties and the hierarchical structure of bone. Med Eng Phys. 1998;20(2):92-102. [23] PHAKATKAR AH, SHIRDAR MR, QI ML, et al. Novel PMMA bone cement nanocomposites containing magnesium phosphate nanosheets and hydroxyapatite nanofibers. Mater Sci Eng C Mater Biol Appl. 2020; 109:110497. [24] BOGER A, BOHNER M, HEINI P, et al. Properties of an injectable low modulus PMMA bone cement for osteoporotic bone. J Biomed Mater Res B Appl Biomater. 2008;86(2):474-482. [25] BOGER A, BISIG A, BOHNER M, et al. Variation of the mechanical properties of PMMA to suit osteoporotic cancellous bone. J Biomater Sci Polym Ed. 2008;19(9):1125-1142. [26] GUTIÉRREZ-MEJÍA A, HERRERA-KAO W, DUARTE-ARANDA S, et al. Synthesis and characterization of core-shell nanoparticles and their influence on the mechanical behavior of acrylic bone cements. Mater Sci Eng C Mater Biol Appl. 2013;33(3):1737-1743. [27] LÓPEZ A, HOESS A, THERSLEFF T, et al. Low-modulus PMMA bone cement modified with castor oil. Biomed Mater Eng. 2011;21(5-6): 323-332. [28] CUCURUZ AT, ANDRONESCU E, FICAI A, et al. Synthesis and characterization of new composite materials based on poly(methacrylic acid) and hydroxyapatite with applications in dentistry. Int J Pharm. 2016;510(2):516-523. [29] BAI H, WALSH F, GLUDOVATZ B, et al. Bioinspired Hydroxyapatite/Poly(methyl methacrylate) Composite with a Nacre-Mimetic Architecture by a Bidirectional Freezing Method. Adv Mater. 2016; 28(1):50-56. [30] BAI M, YIN H, ZHAO J, et al. Application of PMMA bone cement composited with bone-mineralized collagen in percutaneous kyphoplasty. Regen Biomater. 2017;4(4):251-255. [31] CHEN LH, TAI CL, LEE DM, et al. Pullout strength of pedicle screws with cement augmentation in severe osteoporosis: a comparative study between cannulated screws with cement injection and solid screws with cement pre-filling. BMC Musculoskelet Disord. 2011;12:33. [32] GOLDSTEIN SA. The mechanical properties of trabecular bone: dependence on anatomic location and function. J Biomech. 1987; 20(11-12):1055-1061. [33] MORGAN EF, KEAVENY TM. Dependence of yield strain of human trabecular bone on anatomic site. J Biomech. 2001;34(5):569-577. [34] GÓMEZ S, VLAD MD, LÓPEZ J, et al. Characterization and three-dimensional reconstruction of synthetic bone model foams. Mater Sci Eng C Mater Biol Appl. 2013;33(6):3329-3335. [35] Sawbones®EuropeAB[http://www.sawbones.com/products/bio/testblocks/rigidfoam.aspx] [36] International Organization for Standardization standard 5833 (ISO 5833). https://www.iso.org/home.html [37] MONTAÑO CJ, CAMPOS TPR, LEMOS BRS, et al. Effects of hydroxyapatite on PMMA-HAp cement for biomedical applications. Biomed Mater Eng. 2020;31(3):191-201. [38] BOGER A, WHEELER KD, SCHENK B, et al. Clinical investigations of polymethylmethacrylate cement viscosity during vertebroplasty and related in vitro measurements. Eur Spine J. 2009;18(9):1272-1278. [39] LU Q, LIU C, WANG D, et al. Biomechanical evaluation of calcium phosphate-based nanocomposite versus polymethylmethacrylate cement for percutaneous kyphoplasty. Spine J. 2019;19(11):1871-1884. [40] GHAFFARI S, SOLATI-HASHJIN M, ZABIHI-NEYSHABOURI E, et al. Novel calcium phosphate coated calcium silicate-based cement: in vitro evaluation. Biomed Mater. 2020;15(3):035008. [41] AGHYARIAN S, HU X, HADDAS R, et al. Biomechanical behavior of novel composite PMMA-CaP bone cements in an anatomically accurate cadaveric vertebroplasty model. J Orthop Res. 2017;35(9):2067-2074. [42] DENG XG, XIONG XM, CUI W, et al. Preliminary application of CPC/PMMA composite bone cement in kyphoplasty for the elderly. Zhongguo Gu Shang. 2020;33(9):831-836. [43] JI X, XU F, DONG G, et al. Loading necrostatin-1 composite bone cement inhibits necroptosis of bone tissue in rabbit. Regen Biomater. 2019; 6(2):113-119. [44] KIM HW, KIM HE, SALIH V. Stimulation of osteoblast responses to biomimetic nanocomposites of gelatin-hydroxyapatite for tissue engineering scaffolds. Biomaterials. 2005;26(25):5221-5230. [45] TAN F, NACIRI M, DOWLING D, et al. In vitro and in vivo bioactivity of CoBlast hydroxyapatite coating and the effect of impaction on its osteoconductivity. Biotechnol Adv. 2012;30(1):352-362. [46] CAMPANA V, MILANO G, PAGANO E, et al. Bone substitutes in orthopaedic surgery: from basic science to clinical practice. J Mater Sci Mater Med. 2014;25(10):2445-2461. [47] DALBY MJ, DI SILVIO L, HARPER EJ, et al. Increasing hydroxyapatite incorporation into poly(methylmethacrylate) cement increases osteoblast adhesion and response. Biomaterials. 2002;23(2):569-576. |
| [1] | Wang Jianping, Zhang Xiaohui, Yu Jinwei, Wei Shaoliang, Zhang Xinmin, Xu Xingxin, Qu Haijun. Application of knee joint motion analysis in machanism based on three-dimensional image registration and coordinate transformation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-5. |
| [2] | Zhang Yufang, Lü Meng, Mei Zhao. Construction and verification of a full spine biomechanical model of adolescent scoliosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1351-1356. |
| [3] | Bai Zixing, Cao Xuhan, Sun Chengyi, Yang Yanjun, Chen Si, Wen Jianmin, Lin Xinxiao, Sun Weidong. Construction and biomechanical analysis of ankle joint finite element model in gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1362-1366. |
| [4] | Liu Feng, Feng Yi. Finite element analysis of different Kirschner wire tension bands on transverse patella fractures during gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1367-1371. |
| [5] | Jiang Huanchang, Zhang Zhaofei, Liang De, Jiang Xiaobing, Yang Xiaodong, Liu Zhixiang. Comparison of advantages between unilateral multidirectional curved and straight vertebroplasty in the treatment of thoracolumbar osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1407-1411. |
| [6] | Yu Chengxiang, Liu Lehong, Li Wenbo, Chen Jinshi, Ran Chunlei, Wang Zhongping. Correlation between spine-pelvic sagittal parameters and prognosis of vertebroplasty in the treatment of thoracolumbar osteoporotic vertebral compression fractures [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1412-1417. |
| [7] | Liu Yuhang, Zhou Jianqiang, Xu Xuebin, Qu Xingyue, Li Ziyu, Li Kun, Wang Xing, Li Zhijun, Li Xiaohe, Zhang Shaojie. Establishment and validation of finite element model of lower cervical spine in 6-year-old children [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 870-874. |
| [8] | Duan Chao, Shang Xiaoqiang, Duan Xianglin, Yang Ping, Tao Shengxiang. Stability of patellar claw versus loop plate combined with patellar claw for the treatment of comminuted fractures of the lower pole of the patella [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 934-937. |
| [9] | Wen Mingtao, Liang Xuezhen, Li Jiacheng, Xu Bo, Li Gang. Mechanical stability of Sanders II type calcaneal fractures fixed by two internal fixation methods [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 838-842. |
| [10] | Huang Hao, Hong Song, Wa Qingde. Finite element analysis of the effect of femoral component rotation on patellofemoral joint contact pressure in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 848-852. |
| [11] | Zheng Yongze, Zheng Liqin, He Xingpeng, Chen Xinmin, Li Musheng, Li Pengfei, Lin Ziling. Extended finite element modeling analysis of femoral neck fracture based on ABAQUS software [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 853-857. |
| [12] | Wang Zhiqiang, Lin Lu, Chen Xiaolin, Ke Zhenyong. Percutaneous vertebral augmentation for osteoporotic vertebral compression fractures: navigation, fracture reduction system, bone cement leakage, and material modification [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 631-636. |
| [13] | Ou Liang, Kong Dezhong, Xu Daoqing, Ni Jing, Fu Xingqian, Huang Weichen. Comparative clinical efficacy of polymethyl methacrylate and self-solidifying calcium phosphate cement in vertebroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 649-656. |
| [14] | Shen Song, Xu Bin. Diffuse distribution of bone cement in percutaneous vertebroplasty reduces the incidence of refracture of adjacent vertebral bodies [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 499-503. |
| [15] | Hou Wanxing, Li Hongwei, Zheng Xin, Zhu Xianren. Correlation between preoperative magnetic resonance imaging findings and bone cement leakage after percutaneous vertebral augmentation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 504-509. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||