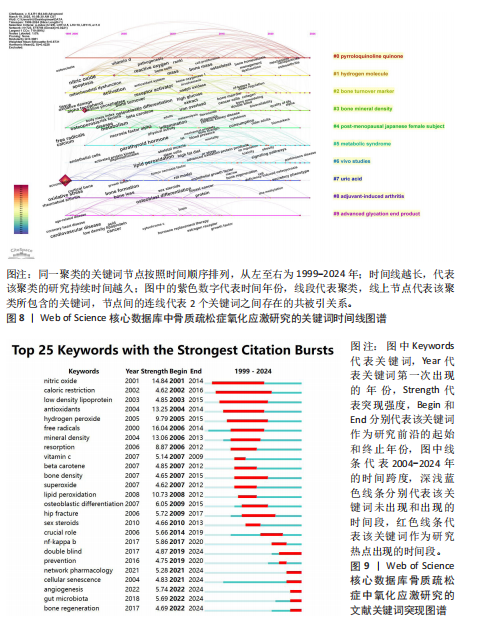
[1] REID IR, BILLINGTON EO. Drug therapy for osteoporosis in older adults. Lancet. 2022; 399(10329):1080-1092.
[2] SHEPSTONE L, LENAGHAN E, COOPER C, et al. Screening in the community to reduce fractures in older women (SCOOP): a randomised controlled trial. Lancet. 2018;391(10122):741-747.
[3] RINONAPOLI G, RUGGIERO C, MECCARIELLO L, et al. Osteoporosis in Men: A Review of an Underestimated Bone Condition. Int J Mol Sci. 2021;22(4):2015.
[4] SU Y, ZHOU B, KWOK T. Fracture risk prediction in old Chinese people-a narrative review. Arch Osteoporos. 2023;19(1):3.
[5] LIU Y, HUANG X, TANG K, et al. Prevalence of osteoporosis and associated factors among Chinese adults: a systematic review and modelling study. J Glob Health. 2025;15:4009.
[6] 章晓云,曾浩,黎征鹏,等.骨质疏松症的发病机制及中医药治疗研究进展[J].中国实验方剂学杂志,2025,31(1):311-320.
[7] ZHANG C, LI H, LI J, et al. Oxidative stress: A common pathological state in a high-risk population for osteoporosis. Biomed Pharmacother. 2023;163:114834.
[8] ZHOU X, TIAN X, CHEN J, et al. Youthful Stem Cell Microenvironments: Rejuvenating Aged Bone Repair Through Mitochondrial Homeostasis Remodeling. Adv Sci (Weinh). 2025; 12(10):e2409644.
[9] KOKOL P, BLAZUN VH, ZAVRSNIK J. Application of bibliometrics in medicine: a historical bibliometrics analysis. Health Info Libr J. 2021;38(2):125-138.
[10] NINKOV A, FRANK JR, MAGGIO LA. Bibliometrics: Methods for studying academic publishing. Perspect Med Educ. 2022;11(3):173-176.
[11] MANOLAGAS SC. From estrogen-centric to aging and oxidative stress: a revised perspective of the pathogenesis of osteoporosis. Endocr Rev. 2010;31(3):266-300.
[12] MAGGIO D, BARABANI M, PIERANDREI M, et al. Marked decrease in plasma antioxidants in aged osteoporotic women: results of a cross-sectional study. J Clin Endocrinol Metab. 2003;88(4):1523-1527.
[13] ALMEIDA M, HAN L, MARTIN-MILLAN M, et al. Skeletal involution by age-associated oxidative stress and its acceleration by loss of sex steroids. J Biol Chem. 2007;282(37):27285-27297.
[14] DOMAZETOVIC V, MARCUCCI G, IANTOMASI T, et al. Oxidative stress in bone remodeling: role of antioxidants. Clin Cases Miner Bone Metab. 2017;14(2):209-216.
[15] BASU S, MICHAELSSON K, OLOFSSON H, et al. Association between oxidative stress and bone mineral densit]. Biochem Biophys Res Commun. 2001;288(1):275-279.
[16] BAI XC, LU D, BAI J, et al. Oxidative stress inhibits osteoblastic differentiation of bone cells by ERK and NF-kappaB. Biochem Biophys Res Commun. 2004;314(1):197-207.
[17] BAEK KH, OH KW, LEE WY, et al. Association of oxidative stress with postmenopausal osteoporosis and the effects of hydrogen peroxide on osteoclast formation in human bone marrow cell cultures. Calcif Tissue Int. 2010;87(3):226-235.
[18] LEE NK, CHOI YG, BAIK JY, et al. A crucial role for reactive oxygen species in RANKL-induced osteoclast differentiation. Blood. 2005;106(3): 852-859.
[19] MODY N, PARHAMI F, SARAFIAN TA, et al. Oxidative stress modulates osteoblastic differentiation of vascular and bone cells. Free Radic Biol Med. 2001;31(4):509-519.
[20] MUTHUSAMI S, RAMACHANDRAN I, MUTHUSAMY B, et al. Ovariectomy induces oxidative stress and impairs bone antioxidant system in adult rats. Clin Chim Acta. 2005;360(1-2):81-86.
[21] DOMAZETOVIC V, MARCUCCI G, IANTOMASI T, et al. Oxidative stress in bone remodeling: role of antioxidants. Clin Cases Miner Bone Metab. 2017;14(2):209-216.
[22] TAO H, LI X, WANG Q, et al. Redox signaling and antioxidant defense in osteoclasts. Free Radic Biol Med. 2024;212:403-414.
[23] GUO Z, WU J, HU Y, et al. Exogenous iron caused osteocyte apoptosis, increased RANKL production, and stimulated bone resorption through oxidative stress in a murine model. Chem Biol Interact. 2024;399:111135.
[24] WEI L, CHAI S, YUE C, et al. Resveratrol protects osteocytes against oxidative stress in ovariectomized rats through AMPK/JNK1-dependent pathway leading to promotion of autophagy and inhibition of apoptosis. Cell Death Discov. 2023;9(1):16.
[25] HE Y, LIU T, PENG X, et al. Molecular mechanism of mitochondrial autophagy mediating impaired energy metabolism leading to osteoporosis. Biochim Biophys Acta Mol Basis Dis. 2025;1871(3): 167685.
[26] ZHOU Y, SU Z, LIU G, et al. The Potential Mechanism of Soy Isoflavones in Treating Osteoporosis: Focusing on Bone Metabolism and Oxidative Stress. Phytother Res. 2025;39(3):1645-1658.
[27] SUN Y, HUANG D, ZHANG Y. The bone-vascular axis: the link between osteoporosis and vascular calcification. Mol Cell Biochem. 2025;480(6): 3413-3427.
[28] KARTHIK V, GUNTUR AR. Energy Metabolism of Osteocytes. Curr Osteoporos Rep. 2021;19(4): 444-451.
[29] SIDDIQUI JA, PARTRIDGE NC. CCL2/Monocyte Chemoattractant Protein 1 and Parathyroid Hormone Action on Bone. Front Endocrinol (Lausanne). 2017;8:49.
[30] HENRY ÓC, O’NEILL L. Metabolic Reprogramming in Stromal and Immune Cells in Rheumatoid Arthritis and Osteoarthritis: Therapeutic Possibilities. Eur J Immunol. 2025;55(4):e202451381.
[31] AKAB SM, ABOZEID HE, ELAZAB SA, et al. Relation between bone mineral density and oxidative stress in Egyptian patients with chronic kidney disease: a cross sectional study. BMC Nephrol. 2025;26(1):197.
[32] HUANG R, WANG H, SHEN Z, et al. Increased Glycemic Variability Evaluated by Continuous Glucose Monitoring is Associated with Osteoporosis in Type 2 Diabetic Patients. Front Endocrinol (Lausanne). 2022;13:861131.
[33] YAN T, NISAR MF, HU X, et al. Pyrroloquinoline Quinone (PQQ): Its impact on human health and potential benefits: PQQ: Human health impacts and benefits. Curr Res Food Sci. 2024;9:100889.
[34] LI J, ZHANG J, XUE Q, et al. Pyrroloquinoline quinone alleviates natural aging-related osteoporosis via a novel MCM3-Keap1-Nrf2 axis-mediated stress response and Fbn1 upregulation. Aging Cell. 2023;22(9):e13912.
[35] PERVEEN I, BUKHARI B, NAJEEB M, et al. Hydrogen Therapy and Its Future Prospects for Ameliorating COVID-19: Clinical Applications, Efficacy, and Modality. Biomedicines. 2023;11(7):1892.
[36] HUANG L. Molecular hydrogen: a therapeutic antioxidant and beyond. Med Gas Res. 2016; 6(4):219-222.
[37] CARNOVALI M, BANFI G, MARIOTTI M. Molecular Hydrogen Prevents Osteoclast Activation in a Glucocorticoid-Induced Osteoporosis Zebrafish Scale Model. Antioxidants (Basel). 2023;12(2): 345.
[38] SAUTCHUK RJ, YU C, MCARTHUR M, et al. Role of the Mitochondrial Permeability Transition in Bone Metabolism and Aging. J Bone Miner Res. 2023;38(4):522-540.
|