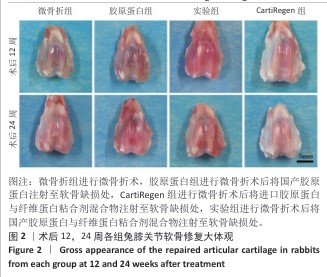
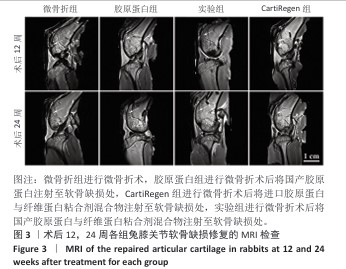
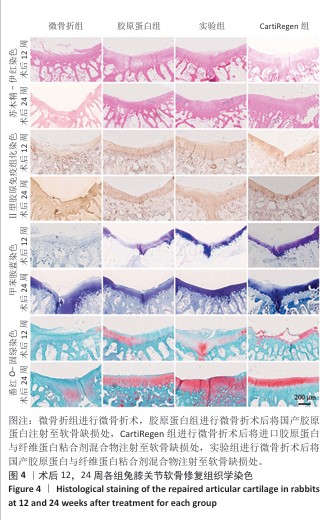
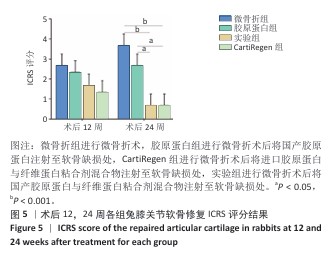
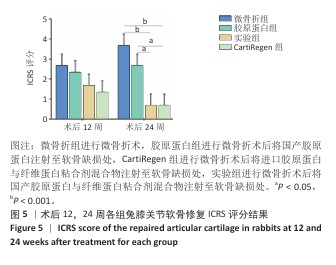
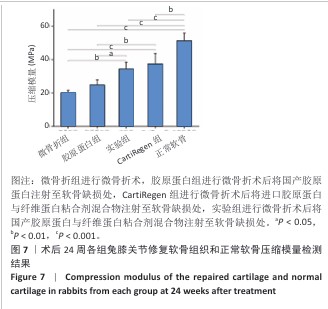
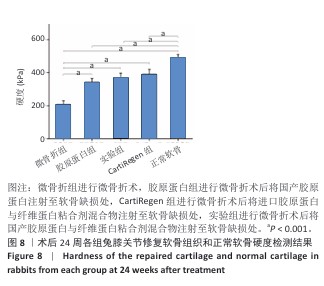
[1] 王新军,沈明球,刘俊昌,等.膝关节骨性关节炎的病因研究现状[J].新疆中医药,2011,29(3):77-80.
[2] 李民仆,胡佳琦,温春蕾,等.膝关节骨性关节炎射频治疗研究进展[J].中国疼痛医学杂志,2020,26(1):61-65.
[3] 宗亿洲,戴易,李哲,等.坏死性凋亡与铁死亡在膝骨关节炎中的研究进展[J].海南医学院学报,2023,29(21):1675-1680.
[4] MARTEL-PELLETIER J, BARR AJ, CICUTTINI FM, et al. Osteoarthritis. Nat Rev Dis Primers. 2016;2:16072.
[5] 赵忠琪,王晓坤,彭慧敏,等.提高关节软骨脱细胞支架孔隙率及细胞渗透性方法的研究进展[J].中国生物医学工程学报,2018,37(1): 112-118.
[6] 史冬泉,李嘉威.软骨修复临床转化的挑战与机遇[J].医学研究生学报, 2019,32(9):897-903.
[7] MEDVEDEVA EV, GREBENIK EA, GORNOSTAEVA SN, et al. Repair of Damaged Articular Cartilage: Current Approaches and Future Directions. Int J Mol Sci. 2018;19(8):2366.
[8] 敖英芳,代文立.关节软骨损伤修复研究展望[J].临床外科杂志,2021, 29(4):301-304.
[9] KANG SW, BADA LP, KANG CS, et al. Articular cartilage regeneration with microfracture and hyaluronic acid. Biotechnol Lett. 2008;30(3):435-439.
[10] ARMIENTO AR, ALINI M, STODDART MJ. Articular fibrocartilage-Why does hyaline cartilage fail to repair? Adv Drug Deliv Rev. 2019;146:289-305.
[11] BERTHO P, PAUVERT A, POUDEROUX T, et al. Treatment of large deep osteochondritis lesions of the knee by autologous matrix-induced chondrogenesis (AMIC): Preliminary results in 13 patients. Orthop Traumatol Surg Res. 2018;104(5):695-700.
[12] 代岭辉.膝关节软骨损伤修复重建指南(2021)[J].中国运动医学杂志, 2022,41(4):249-259.
[13] MITHOEFER K, MCADAMS T, WILLIAMS RJ, et al. Clinical efficacy of the microfracture technique for articular cartilage repair in the knee: an evidence-based systematic analysis. Am J Sports Med. 2009;37(10): 2053-2063.
[14] 李美明,马永胜,林啟泰,等.同种异体骨软骨移植的适应证和禁忌证[J].实用骨科杂志,2024,30(8):673-678.
[15] 兰伟伟,陈维毅,黄棣.骨软骨组织工程研究进展[J].生物医学工程学杂志,2019,36(3):504-510.
[16] 周建林,方洪松,彭昊,等.自体、异体骨软骨移植及组织工程材料修复的关节软骨损伤[J].中国组织工程研究,2015,19(34):5530-5535.
[17] 齐义营,施培华,欧阳宏伟.自体软骨细胞移植治疗关节软骨缺损的进展[J].中华骨科杂志,2008,28(1):71-73.
[18] 徐磊,叶朝阳,周燕,等.体外传代培养兔关节软骨细胞的去分化现象[J].中国组织工程研究,2013,17(20):3626-3634.
[19] 关炼雄,段莉,黄江鸿,等.软骨细胞去分化研究进展[J].国际骨科学杂志,2014,35(4):250-253.
[20] KARLSEN TA, SHAHDADFAR A, BRINCHMANN JE. Human primary articular chondrocytes, chondroblasts-like cells, and dedifferentiated chondrocytes: differences in gene, microRNA, and protein expression and phenotype. Tissue Eng Part C Methods. 2011;17(2):219-227.
[21] KNUTSEN G, DROGSET JO, ENGEBRETSEN L, et al. A randomized trial comparing autologous chondrocyte implantation with microfracture. Findings at five years. J Bone Joint Surg Am. 2007;89(10):2105-2112.
[22] 金璐頔,徐晶晶,张勇,等.软骨细胞体外增殖去分化的拉曼光谱分析[J].物理化学学报,2017,33(12):2446-2453.
[23] 刘振龙,侯振宸,胡晓青,等.关节镜下组织工程支架修复软骨损伤[J].北京大学学报(医学版),2025,57(2):384-387.
[24] 许航,何其泽,黄为,等.组织工程关节软骨的研究进展[J].中国骨与关节损伤杂志,2022,37(5):558-560.
[25] 敖英芳.关节软骨损伤修复重建学[M].北京:北京大学医学出版社, 2020.
[26] 陈微,孙倩雯,韩艳琪,等.丝素蛋白水凝胶在骨关节炎中的应用研究[J].药物流行病学杂志,2023,32(5):582-589.
[27] LI Y, CHEN M, ZHOU W, et al. Cell-free 3D wet-electrospun PCL/silk fibroin/Sr2+ scaffold promotes successful total meniscus regeneration in a rabbit model. Acta Biomater. 2020;113:196-209.
[28] LI Q, XU S, FENG Q, et al. 3D printed silk-gelatin hydrogel scaffold with different porous structure and cell seeding strategy for cartilage regeneration. Bioact Mater. 2021;6(10):3396-3410.
[29] 王武,樊晓磊,谢杰,等.羟基磷灰石-聚乙烯醇/胶原-壳聚糖-明胶复合水凝胶修复兔骨软骨缺损[J]. 中国组织工程研究,2024,28(5): 682-689.
[30] 张本妥,杨昕.人工生物材料在关节软骨损伤修复中的应用[J].中国组织工程研究,2024,28(10):1599-1605.
[31] SALONIUS E, MELLER A, PAATELA T, et al. Cartilage Repair Capacity within a Single Full-Thickness Chondral Defect in a Porcine Autologous Matrix-Induced Chondrogenesis Model Is Affected by the Location within the Defect. Cartilage. 2021;13(2_suppl):744S-754S.
[32] INTINI C, JOYCE M, UBERTI M, et al. A biomimetic reinforced type I/II collagen and hyaluronic acid scaffold in combination with a chondral biomaterial fixation technique for large articular cartilage defect repair: A pilot pre-clinical study. Int J Biol Macromol. 2025;318(Pt 4):145302.
[33] 王征,于会,于尧,等.自体脂肪干细胞、壳聚糖/胶原蛋白支架材料及GDF-5复合物移植修复兔软骨缺损[J].中国组织工程研究,2018, 22(25):3969-3974.
[34] MAINIL-VARLET P, AIGNER T, BRITTBERG M, et al. Histological assessment of cartilage repair: a report by the Histology Endpoint Committee of the International Cartilage Repair Society (ICRS). J Bone Joint Surg Am. 2003; 85-A Suppl 2:45-57.
[35] MANKIN HJ, DORFMAN H, LIPPIELLO L, et al. Biochemical and metabolic abnormalities in articular cartilage from osteo-arthritic human hips. II. Correlation of morphology with biochemical and metabolic data. J Bone Joint Surg Am. 1971;53(3):523-537.
[36] MCCARTHY HS, ROBERTS S. A histological comparison of the repair tissue formed when using either Chondrogide (®) or periosteum during autologous chondrocyte implantation. Osteoarthritis Cartilage. 2013;21(12):2048-2057.
[37] CAREY JL, REMMERS AE, FLANIGAN DC. Use of MACI (autologous cultured chondrocytes on porcine collagen membrane) in the United States: preliminary experience. Orthop J Sports Med. 2020;8(8): 2325967120941816.
[38] MAYBIN JA, CRITCHLEY HO. Menstrual physiology: implications for endometrial pathology and beyond. Hum Reprod Update. 2015;21(6): 748-761.
[39] KIM MK, CHOI SW, KIM SR, et al. Autologous chondrocyte implantation in the knee using fibrin. Knee Surg Sports Traumatol Arthrosc. 2010; 18(4):528-534.
[40] DI CAVE E, VERSARI P, SCIARRETTA F, et al. Biphasic bioresorbable scaffold (TruFit Plug®) for the treatment of osteochondral lesions of talus: 6- to 8-year follow-up. Foot (Edinb). 2017;33:48-52.
[41] PARK IS, JIN RL, OH HJ, et al. Sizable scaffold-free tissue-engineered articular cartilage construct for cartilage defect repair. Artif Organs. 2019;43(3):278-287.
[42] 刘恒宇,阮耀宽,姜振德,等.中晚期踝关节炎治疗方案选择原则及治疗方法的研究进展[J].吉林大学学报(医学版),2025,51(1):266-274.
[43] KIM SJ, SHETTY AA, KURIAN NM, et al. Articular cartilage repair using autologous collagen-induced chondrogenesis (ACIC): a pragmatic and cost-effective enhancement of a traditional technique. Knee Surg Sports Traumatol Arthrosc. 2020;28(8):2598-2603.
[44] ANDERS S, VOLZ M, FRICK H, et al. A randomized, controlled trial comparing autologous matrix-induced chondrogenesis (AMIC®) to microfracture: analysis of 1- and 2-year follow-up data of 2 centers. Open Orthop J. 2013; 7:133-143.
[45] VOLZ M, SCHAUMBURGER J, GELLIßEN J, et al. A randomized controlled trial demonstrating sustained benefit of autologous matrix-induced chondrogenesis (AMIC®) over microfracture: 10-year follow-up. Eur J Orthop Surg Traumatol. 2024;34(5):2429-2437.
[46] 李威.关节镜微骨折术联合使用胶原蛋白软骨再生载体对膝关节软骨缺损患者治疗的临床疗效分析[D].石家庄:河北医科大学,2021.
[47] 罗洁,王凤山.医用软组织粘合剂的研究进展及临床应用现状[J].药物生物技术,2014,21(3):274-278.
[48] 郭偲,刘宏,周萌萌.医用纤维蛋白粘合剂的研究进展[J].中国药房, 2016,27(17):2439-2442.
[49] 曾俐,孙材江.自制纤维蛋白粘合剂对同种异体关节软骨移植的作用[J].中华骨科杂志,1993,13(6):442-445,C2.
[50] 杨万波.关节软骨组织工程学研究进展[J].中国矫形外科杂志,2003(Z2): 96-98.
[51] 杨贵勇,卢世璧.生物组织粘合剂对软骨修复材料和修复过程的影响[J].中国临床康复,2002,6(10):1416-1417.
[52] JEONG IH, SHETTY AA, KIM SJ, et al. Autologous collagen-induced chondrogenesis using fibrin and atelocollagen mixture. Cells Tissues Organs. 2013;198(4):278-288.
[53] 组织工程医疗产品 第10部分:修复或再生关节软骨的植入物体内评价指南:YY/T 0606.10-2008[S]. 2008.
[54] 用于关节软骨组织修复或再生的植入性医疗器械体内评价:T/CSBM 0029-2022[S].2022.
[55] DIAS IR, VIEGAS CA, CARVALHO PP. Large Animal Models for Osteochondral Regeneration. Adv Exp Med Biol. 2018;1059:441-501.
[56] MORAN CJ, RAMESH A, BRAMA PA, et al. The benefits and limitations of animal models for translational research in cartilage repair. J Exp Orthop. 2016;3(1):1.
[57] 国家药监局器审中心.I型胶原软骨修复产品注册审查指导原则:国家药监局器审中心关于发布I型胶原软骨修复产品等10项医疗器械注册审查指导原则的通告2025年第6号[Z].
[58] COOK JL, HUNG CT, KUROKI K, et al. Animal models of cartilage repair. Bone Joint Res. 2014;3(4):89-94.
[59] TESSARO I, NGUYEN VT, DI GIANCAMILLO A, et al. Animal models for cartilage repair. J Biol Regul Homeost Agents. 2018; 32(6 Suppl. 1):
105-116.
|