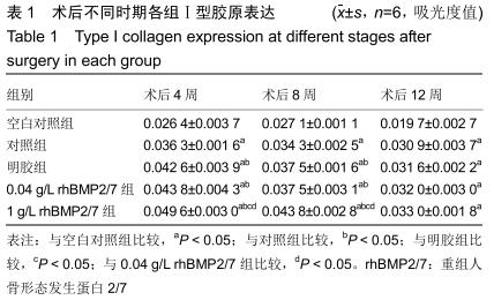
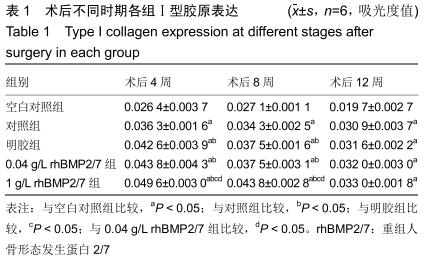
Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (28): 4533-4539.doi: 10.3969/j.issn.2095-4344.2314
Previous Articles Next Articles
Calcium hydrogen phosphate dehydrate combined with gelatin and recombinant human bone morphologic protein 2/7 for repair of bone defects in rabbits
Li Xuewei1, Hu Beibei2, Zhang Dawei1, Quan Lulu1, Liang Yongqiang1
1Department of Orthodontics, College of Stomatology, North China University of Science and Technology, Tangshan 063000, Hebei Province, China; 2Department of Stomatology, Ankang Hospital of Traditional Chinese Medicine, Xi’an 725000, Shaanxi Province, China
-
Received:2019-12-06Revised:2019-12-11Accepted:2020-01-16Online:2020-10-08Published:2020-09-01 -
Contact:Liang Yongqiang, MD, Associate professor, Associate chief physician, Department of Orthodontics, School of Stomatology, North China University of Science and Technology, Tangshan 063000, Hebei Province, China -
About author:Li Xuewei, Master, Physician, Department of Orthodontics, School of Stomatology, North China University of Science and Technology, Tangshan 063000, Hebei Province, China -
Supported by:the National Natural Science Foundation of China, No. 81270965; a Key Program of Education Department of Hebei Province, No. ZD2015016
CLC Number:
Cite this article
Li Xuewei, Hu Beibei, Zhang Dawei, Quan Lulu, Liang Yongqiang. Calcium hydrogen phosphate dehydrate combined with gelatin and recombinant human bone morphologic protein 2/7 for repair of bone defects in rabbits[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(28): 4533-4539.
share this article
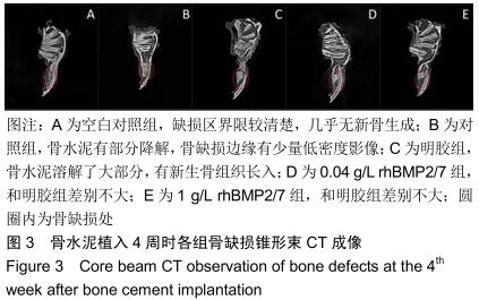
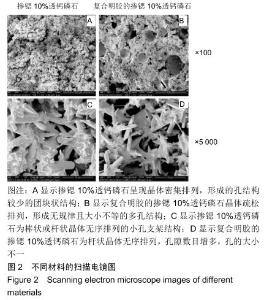
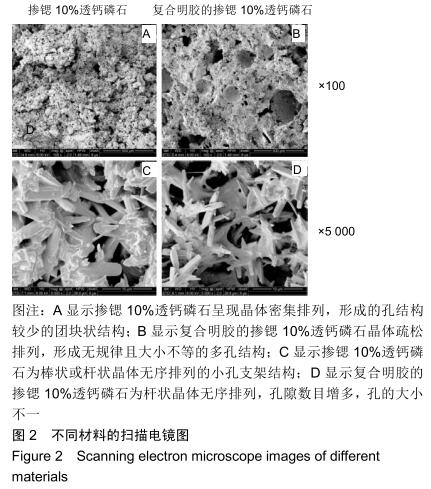
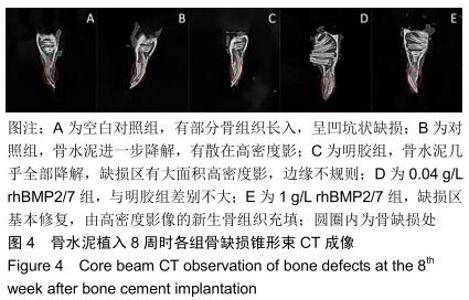
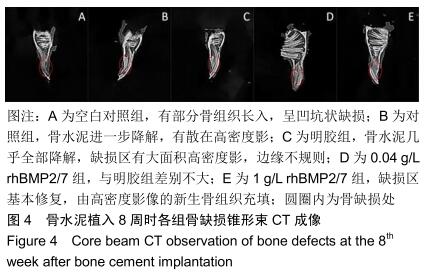
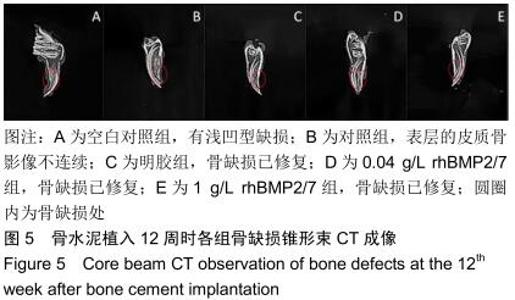
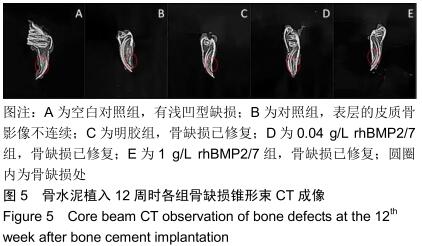
2.2 骨缺损修复大体观察结果 术后4周时,缺损区有一层纤维组织覆盖,探针探查空白组有界限清楚的凹陷状骨缺损;对照组材料与骨缺损界限清楚,有少量骨痂形成;明胶组材料与骨缺损界限模糊,有部分骨痂形成;0.04 g/L rhBMP2/7组材料与骨缺损界限模糊,骨痂形成较多;1 g/L rhBMP2/7组骨缺损区减小,表面有纤维骨痂覆盖。术后8周时,空白组较4周时缺损区缩小,边限模糊;对照组缺损区有部分纤维样的瘢痕组织且缺损区缩小;明胶组缺损区减小,表面有纤维骨痂形成;0.04 g/L rhBMP2/7组缺损区大部分由新生硬组织填充;1 g/L rhBMP2/7组凹陷区基本平整,完成修复。术后12周时,空白组缺损区减小,仍有部分凹陷样结构;其余4组缺损均已完成修复。 2.3 骨缺损修复锥形束CT表现 将兔下颌骨颊面(缺损处)朝上摆放进行锥形束CT扫描锥形束CT是三维成像,但只有冠状面图像是清晰的,故选择冠状面进行观察,选择测量位置时结合矢状面和横断面,选择缺损区中心的冠状面进行观察,因缺损区中心区域是最后修复的,选取中心位置有助于判断骨修复的效果,避免出现假阳性结果。但有时锥形束CT由于各种原因扫描后的结果不够好,只能在尽量靠近缺损区中心的位置选取断层图片。 术后4周时,空白组可见缺损区边界稍清楚的低密度影像;对照组可见比空白组缺损区密度稍高的界限较清晰的影像;明胶组缺损区边界模糊,0.04,1 g/L rhBMP2/7组与明胶组差别不明显,见图3。术后8周时,空白组低密度凹陷区缩小;对照组骨缺损区低密度影像减小,有散在高密度影像;明胶组缺损区有为高密度影像,边缘呈现不规则的低密度影像;0.04 g/L rhBMP2/7组和明胶组差别不明显,缺损区大部分修复,新骨修复边缘不平整;1 g/L rhBMP2/7组基本修复,皮质骨影像不连续,见图4。术后12周时,空白组缺损区仍有部分低密度影像;对照组可见骨皮质不连续影像;其余3组缺损区与正常骨组织影像密度一致,见图5。 "
|
[1] LOMAS R, CHANDRASEKAR A, BOARD TN. Bone allograft in the UK: perceptions and realities.Hip Int. 2013;23(5): 427-433.
[2] STERNHEIM A, DREXLER M, KUZYK PR, et al. Treatment of failed allograft prosthesis composites used for hip arthroplasty in the setting of severe proximal femoral bone defects.J Arthroplasty. 2014;29(5):1058-1062.
[3] HERMANSON O. Advances in tissue engineering.Acta Paediatr. 2009;98(10):1699-1699.
[4] KIM HD, AMIRTHALINGAM S, KIM SL, et al. Biomimetic Materials and Fabrication Approaches for Bone Tissue Engineering.Adv Healthc Mater.2017;6(23):365-377.
[5] TAMIMI F, SHEIKH Z, BARRALET J. Dicalcium phosphate cements: brushite and monetite.Acta Biomater. 2012;8(2): 474-487.
[6] NIDA T, WAI L, GOEBEL W, et al. Fabrication of Poly-l-lactic Acid/Dicalcium Phosphate Dihydrate Composite Scaffolds with High Mechanical, Strength—Implications for Bone Tissue Engineering. J Funct Biomater.2015;6(4):1036-1053.
[7] VAHABZADEN S, ROY M, BOSE S. Effects of silicon on osteoclast cell mediated degradation, in vivo osteogenesis and vasculogenesis of brushite cement.J Mater Chem B. 2015;3(46):8973-8982.
[8] PILMANE M, SALMA-ANCANE K, LOCA D, et al. Strontium and strontium ranelate: Historical review of some of their functions. Mater Sci Eng C Mater Biol Appl. 2017;78:1222-1230.
[9] ALKHRAISAT MH, MOSEKE C, BLANCO L, et al. Strontium modified biocements with zero order release kinetics. Biomaterials.2008;29(35):4691-4697.
[10] PINA S, VIEIRA SI, TORRES PM, et al. In vitro performance assessment of new brushite-forming Zn- and ZnSr-substituted beta-TCP bone cements.J biomed Mater Res B Appl biomater.2010;94(2):414-420.
[11] PINA S, TORRES PM, FERREIRA JM. Injectability of brushite-forming Mg-substituted and Sr-substituted α-TCP bone cements.J Mater Sci Mater Med.2010;21(2):431-438.
[12] LILLEY KJ, GBURECK U, KNOWLES JC, et al. Cement from magnesium substituted hydroxyapatite. J Mater Sci Mater Med.2005;16(5):455-460.
[13] 方俊,董伟,彭宏峰,等.掺锶透钙磷石骨水泥修复骨质疏松家兔牙槽骨缺损的实验研究[J].实用医学杂志,2018,34(5):720-724.
[14] 李淑静.掺锶透钙磷石骨水泥修复骨质疏松骨缺损的实验研究[D].唐山:华北理工大学,2017.
[15] 周秋娟,梁永强,李淑静,等.掺锶透钙磷石骨水泥修复家兔牙槽骨缺损的研究[J].安徽医科大学学报,2017,52(4):589-592.
[16] 闫玉婷.掺锶透钙磷石骨水泥修复牙槽骨缺损的实验研究[D].唐山:华北理工大学,2016.
[17] GARCÍA-GARETA E,COATHUP MJ,BLUNN GW. Osteoinduction of bone grafting materials for bone repair and regeneration.Bone.2015;81:112-121.
[18] ROY A, JHUNJHUNWALA S, BAYER E, et al. Porous calcium phosphate-poly (lactic-co-glycolic) acid composite bone cement: A viable tunable drug delivery system.Mater Sci Eng C Mater Biol Appl. 2016;59:92-101.
[19] KIKUCHI M, MATSUMOTO HN, YAMADA T, et al. Glutaraldehyde cross-linked hydroxyapatite/collagen self-organized nanocomposites.Biomaterials.2004;25(1): 63-69.
[20] SILVA SS, JOÃO FM, REIS RL. Potential applications of natural origin polymer-based systems in soft tissue regeneration. Crit Rev Biotechnol.2010;30(3):200-221.
[21] RAMMELT S, SCHULZE E, BERNHARDT R, et al. Coating of titanium implants with type-I collagen. J Orthop Res. 2004; 22(5):1025-1034.
[22] WANG W, YEUNG KWK. Bone grafts and biomaterials substitutes for bone defect repair: A review.Bioact Mater. 2017; 2(4):224-247.
[23] CHEN M, SONG K, RAO N, et al. Effect of bone marrow mesenchymal stem cells transfected with rAAV2-bFGF on early angiogenesis of calvarial defects in rats.J Huazhong Univ Sci Technolog Med Sci.2010;30(4):519-524.
[24] KERAMARIS NC, CALORI GM, NIKOLAOU VS, et al. Fracture vascularity and bone healing: A systematic review of the role of VEGF.Injury.2008;39(2):S45-S57.
[25] SHUANG Y, YIZHEN L, ZHANG Y, et al. In vitro characterization of an osteoinductive biphasic calcium phosphate in combination with recombinant BMP2. BMC Oral Health. 2016;17(1):35-44.
[26] YONGSUN K, BYUNG-JAE K, WAN K, et al. Evaluation of Mesenchymal Stem Cell Sheets Overexpressing BMP-7 in Canine Critical-Sized Bone Defects.Int J Mol Sci. 2018;19(7): 2073-2086.
[27] 谢程欣,胡庄明,王维,等.重组人骨形态发生蛋白2在四肢骨创伤中的应用:深入探讨理想载体及最佳剂量等问题[J].中国组织工程研究,2019,23(30):4882-4888.
[28] ZHENG Y, WU G, ZHAO J, et al. rhBMP2/7 Heterodimer: An Osteoblastogenesis Inducer of Not Higher Potency but Lower Effective Concentration Compared with rhBMP2 and rhBMP7 Homodimers. Tissue Eng Part A.2010;16(3):879-887.
[29] WANG J, ZHENG Y, ZHAO J, et al. Low-dose rhBMP2/7 heterodimer to reconstruct peri-implant bone defects: A micro-CT evaluation.J Clin Periodontol.2011;39(1):98-105.
[30] 贾婉萍,梁立硕,冯凯悦,等.掺镁透钙磷石对骨质疏松兔骨缺损的成骨效果[J].山西医科大学学报,2017,48(12):1260-1264.
[31] KOTSAR A, NIEMINEN R, ISOTALO T, et al. Biocompatibility of New Drug-eluting Biodegradable Urethral Stent Materials. Urology.2009;75(1):229-234.
[32] ORYAN A, BIGHAM-SADEGH A, ABBASI-TESHNIZI F. Effects of osteogenic medium on healing of the experimental critical bone defect in a rabbit model.Bone.2014;63:53-60.
[33] MCGOVERN JA, GRIFFIN M, HUTMACHER DW. Animal models for bone tissue engineering and modelling disease. Dis Model Mech.2018;11(4):33-84. [34] 鄂玲玲,王东胜,师占平,等.一种新型的兔牙槽骨缺损模型的建立[J].中华老年口腔医学杂志,2011,9(3):137-140.
[35] HOLLINGER JO, KLEINSCHMIDT JC. The critical size defect as an experimental model to test bone repair materials. J Craniofac Sur.1990;1(1):60-80.
[36] SCHMITZ JP, HOLLINGER JO. The critical size defect as an experimental model for craniomandibulofacial nonunions.Clin Orthop Relat Res.1986;205:299-304.
[37] 程谷.运用不同的接种方法构建组织工程化骨修复颌骨缺损的实验研究[D].武汉:武汉大学,2016.
[38] BOHNER M, LOOSLI Y, BAROUD G, et al. Commentary: Deciphering the link between architecture and biological response of a bone graft substitute.Acta Biomater. 2011;7(2): 478-484.
[39] LU JX, FLAUTRE B, ANSELME K, et al. Role of Interconnections in Porous Bioceramics on Bone Recolonization In Vitro and In Vivo.J Mater Sci Mater Med. 1999;10(2):111-120.
[40] 张单单.明胶的戊二醛、转谷氨酰胺酶改性与性能研究[D].北京:北京工商大学,2016.
[41] GOTHARD D, SMITH EL, KANCZLER JM, et al. Tissue engineered bone using select growth factors: A comprehensive review of animal studies and clinical translation studies in man.Eur Cell Mater. 2014;28(28): 166-208.
[42] YUAN S, PAN Q, LIU W, et al. Recombinant BMP 4/7 fusion protein induces differentiation of bone marrow stem cells.J Cell Biochem.2011;112(10):3054-3060.
[43] KANEKO H, ARAKAWA T, MANO H, et al. Direct stimulation of osteoclastic bone resorption by bone morphogenetic protein (BMP)-2 and expression of BMP receptors in mature osteoclasts. Bone.2000; 27(4):479-486.
[44] SANDHU H. Use of recombinant human bone morphogenetic protein-2 to achieve posterolateral lumbar spine fusion in humans: a prospective, randomized clinical pilot trial: 2002 Volvo Award in clinical studies.Spine (Phila Pa 1976). 2002; 27(23):2662-2673.
[45] GUO J, WU G. The signaling and functions of heterodimeric bone morphogenetic proteins.Cytokine Growth Factor Rev. 2012;23(1-2):61-67.
[46] KAITO T, MORIMOTO T, MORI Y, et al. BMP-2/7 heterodimer strongly induces bone regeneration in the absence of increased soft tissue inflammation.Spine J. 2017;18(1): 139-146.
[47] SUN P, WANG J, ZHENG Y, et al. BMP2/7 heterodimer is a stronger inducer of bone regeneration in peri-implant bone defects model than BMP2 or BMP7 homodimer.Dental Mate J.2012; 31(2):239-248.
[48] ISRAEL DI, NOVE J, KERNS KM, et al. Heterodimeric Bone Morphogenetic Proteins Show Enhanced Activity In Vitro and In Vivo.Growth Factors.1996;13(3):291-300.
[49] OXLUND H, MOSEKILDE L, ORTOFT G. Reduced concentration of collagen reducible cross links in human trabecular bone with respect to age and osteoporosis.Bone. 1996;19(5):479-484.
[50] 梁立硕,贾婉萍,方俊,等.不同浓度掺镁透钙磷石骨水泥修复骨质疏松家兔骨缺损及BMP-2表达的实验研究[J].科学技术与工程, 2018,18(8):187-190. |
| [1] | Wu Xun, Meng Juanhong, Zhang Jianyun, Wang Liang. Concentrated growth factors in the repair of a full-thickness condylar cartilage defect in a rabbit [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1166-1171. |
| [2] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [3] | Zhang Bin, Sun Lihua, Zhang Junhua, Liu Yusan, Cui Caiyun. A modified flap immediate implant is beneficial to soft tissue reconstruction in maxillary aesthetic area [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 707-712. |
| [4] | Chen Junyi, Wang Ning, Peng Chengfei, Zhu Lunjing, Duan Jiangtao, Wang Ye, Bei Chaoyong. Decalcified bone matrix and lentivirus-mediated silencing of P75 neurotrophin receptor transfected bone marrow mesenchymal stem cells to construct tissue-engineered bone [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 510-515. |
| [5] | Li Chenjie, Lü Linwei, Song Yang, Liu Jingna, Zhang Chunqiu. Measurement and statistical analysis of trabecular morphological parameters of titanium alloy peri-prosthesis under preload [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 516-520. |
| [6] | Ma Zhijie, Li Jingyu, Cao Fang, Liu Rong, Zhao Dewei. Influencing factors and biological property of novel biomedical materials: porous silicon carbide coated with bioactive tantalum [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 558-563. |
| [7] | Shi Xiaoxiu, Mao Shilong, Liu Yang, Ma Xingshuang, Luo Yanfeng. Comparison of tantalum and titanium (alloy) as orthopedic materials: physical and chemical indexes, antibacterial and osteogenic ability [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 593-599. |
| [8] | Li Xiaozhuang, Duan Hao, Wang Weizhou, Tang Zhihong, Wang Yanghao, He Fei. Application of bone tissue engineering materials in the treatment of bone defect diseases in vivo [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 626-631. |
| [9] | He Jie, Chang Qi. Biological reconstruction of large bone defects after resection of malignant tumor of extremities [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 420-425. |
| [10] | Xing Hao, Zhang Yonghong, Wang Dong. Advantages and disadvantages of repairing large-segment bone defect [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 426-430. |
| [11] | Yang Junhui, Luo Jinli, Yuan Xiaoping. Effects of human growth hormone on proliferation and osteogenic differentiation of human periodontal ligament stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3956-3961. |
| [12] | Gao Kun, Chen Dayu, Zhang Yong, Liu Weidong, Sun Shufen, Lai Wenqiang, Ma Dujun, Wu Yihong, Lin Zhanpeng, Jiang Yinglu, Yu Weiji. Achyranthes bidentata alcohol extract inhibits extracellular matrix degradation of the cartilage by regulating synovial fibroblast exosomes [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3636-3640. |
| [13] | Li Xinping, Cui Qiuju, Zeng Shuguang, Ran Gaoying, Zhang Zhaoqiang, Liu Xianwen, Fang Wei, Xu Shuaimei. Effect of modification of β-tricalcium phosphate/chitosan hydrogel on growth and mineralization of dental pulp stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3493-3499. |
| [14] | Zhou Anqi, Tang Yufei, Wu Bingfeng, Xiang Lin. Designing of periosteum tissue engineering: combination of generality and individuality [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3551-3557. |
| [15] | Chen Song, He Yuanli, Xie Wenjia, Zhong Linna, Wang Jian. Advantages of calcium phosphate nanoparticles for drug delivery in bone tissue engineering research and application [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3565-3570. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||