Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (21): 5621-5628.doi: 10.12307/2026.698
Meta-analysis of application effect of 3D-printed artificial vertebral bodies in anterior cervical corpectomy and fusion
Wu Ronghai1, 2, Zheng Zhouhang1, 2, Chen Huan1, 2, You Dongchun1, 2, Guo Weifeng1, 2, Liu Xingming1, 2, Zhang Yu1, 2
- 1Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China; 2Guangdong Second Traditional Chinese Medicine Hospital (Guangdong Research Institute of Traditional Chinese Medicine Manuracturing Technology), Guangzhou 510095, Guangdong Province, China
-
Accepted:2025-07-21Online:2026-07-28Published:2026-03-06 -
Contact:Zhang Yu, MD, Chief physician, Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China; Guangdong Second Traditional Chinese Medicine Hospital (Guangdong Research Institute of Traditional Chinese Medicine Manuracturing Technology), Guangzhou 510095, Guangdong Province, China -
About author:Wu Ronghai, MS, Physician, Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China; Guangdong Second Traditional Chinese Medicine Hospital (Guangdong Research Institute of Traditional Chinese Medicine Manuracturing Technology), Guangzhou 510095, Guangdong Province, China -
Supported by:Guangdong Province Basic and Applied Basic Research Fund Provincial-Enterprise Joint Fund, No. 2022A1515220093 (to ZY)
CLC Number:
Cite this article
Wu Ronghai, Zheng Zhouhang, Chen Huan, You Dongchun, Guo Weifeng, Liu Xingming, Zhang Yu . Meta-analysis of application effect of 3D-printed artificial vertebral bodies in anterior cervical corpectomy and fusion[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5621-5628.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
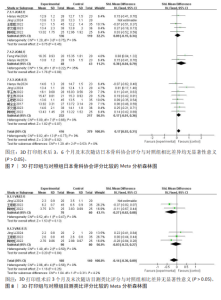
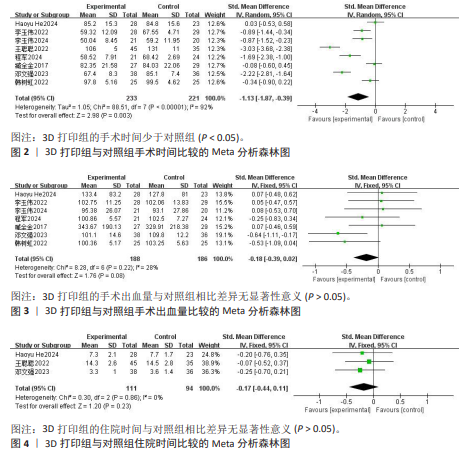
2.3 Meta分析结果 2.3.1 手术时间 8项研究报告了两组患者的手术时间[9,11-17],各研究间异质性较大(I2=92%,P < 0.000 01),经敏感性分析未能消除异质性,选择随机效应模型进行Meta分析,结果显示3D打印组手术时间显著低于对照组,差异有显著性意义[SMD=-1.13,95%CI(-1.87,-0.39),P=0.003],见图2。 2.3.2 手术出血量 7项研究报告了两组患者的手术出血量[9,11-12,14-17],各研究间异质性较小(I2=28%,P= 0.22),选择固定效应模型进行Meta分析,结果显示3D打印组手术出血量与对照组相近,差异无显著性意义[SMD=-0.18,95%CI(-0.39,0.02),P= 0.08],见图3。 2.3.3 住院时间 3项研究报告了两组患者的住院时间[9,13,16],各研究间具有同质性(I2=0%,P=0.86),选择固定效应模型进行Meta分析,结果显示3D打印组住院时间与对照组相近,差异无显著性意义[SMD=-0.17,95%CI(-0.44,0.11),P=0.23],见图4。"
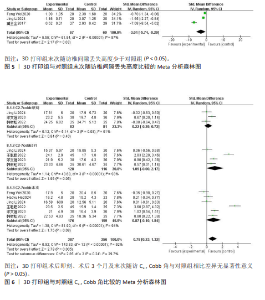
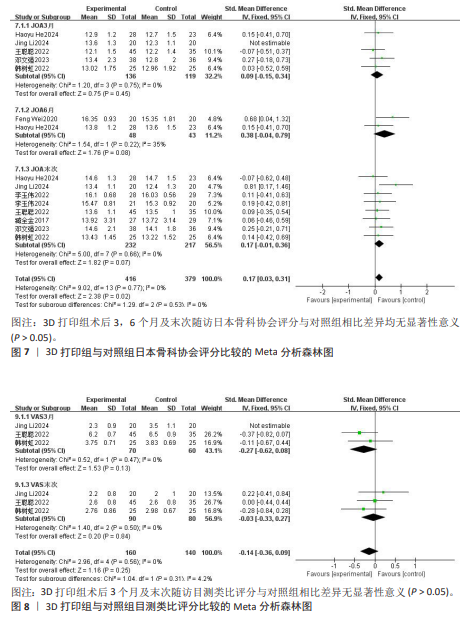
2.3.4 末次随访椎间隙丢失高度 3项研究报告了两组患者末次随访椎间隙丢失高度[8,10,15],各研究间异质性较大(I2=97%,P < 0.000 01),经敏感性分析未能消除异质性,选择随机效应模型进行Meta分析,结果显示3D打印组末次随访椎间隙丢失高度显著低于对照组,差异有显著性意义[SMD=-3.01,95%CI(-5.74,-0.29),P=0.03],见图5。 2.3.5 C2-7 Cobb角 6项研究报告了两组患者的C2-7 Cobb角[8-10,13,16-17],根据随访时间进行亚组分析,评价两组患者在术后即刻、术后3个月、末次随访C2-7 Cobb角情况。其中3项研究报告了两组术后即刻C2-7 Cobb角[10,16-17],各研究间异质性较大(I2= 61%,P=0.08),经敏感性分析未能消除异质性,选择随机效应模型进行Meta分析,结果显示术后即刻3D打印组C2-7 Cobb角与对照组相近,差异无显著性意义[SMD=0.22,95%CI(-0.29,0.72),P=0.40]。4项研究报告了两组术后3个月的C2-7 Cobb 角[10,13,16-17],各研究间异质性较大(I2=93%,P < 0.000 01),经敏感性分析未能消除异质性,选择随机效应模型进行Meta分析,结果显示术后3个月3D打印组C2-7 Cobb角与对照组相近,差异无显著性意义[SMD=1.09,95%CI(0.00,2.17),P=0.05]。6项研究报告了两组术后末次随访C2-7 Cobb角[8-10,13,16-17],各研究间异质性较大(I2=94%,P < 0.000 01),经敏感性分析未能消除异质性,选择随机效应模型进行Meta分析,结果显示末次随访3D打印组C2-7 Cobb角与对照组相近,差异无显著性意义[SMD=0.87,95%CI(-0.10,1.84),P=0.08],见图6。 2.3.6 日本骨科协会评分 9项研究报告了两组的日本骨科协会评分[8-13,15-17],根据随访时间进行亚组分析,评价两组患者在术后3,6个月及末次随访日本骨科协会评分情况。其中5项研究报告了两组术后3个月的日本骨科协会评分[9-10,13,16-17],各研究间具有同质性(I2=0%,P=0.75),选择固定效应模型进行Meta分析,结果显示术后3个月3D打印组日本骨科协会评分与对照组相近,差异无显著性意义[SMD=0.09,95%CI(-0.15,0.34),P= 0.45]。2项研究报告了两组术后6个月的日本骨科协会评分[8-9],各研究间异质性较小(I2=35%,P=0.22),选择固定效应模型进行Meta分析,结果显示术后6个月3D打印组日本骨科协会评分与对照组相近,差异无显著性意义[SMD=0.38,95%CI(-0.04,0.79),P=0.08]。8项研究报告了两组术后末次随访的日本骨科协会评 分[9-13,15-17],各研究间具有同质性(I2= 0%,P=0.66),选择固定效应模型进行Meta分析,结果显示末次随访3D打印组日本骨科协会评分与对照组相近,差异无显著性意义[SMD=0.17,95%CI(-0.01,0.36),P=0.07],见图7。 2.3.7 目测类比评分 3项研究报告了两组患者的目测类比评分[10,13,17],根据随访时间进行亚组分析,评价两组患者在术后3个月及末次随访时的目测类比评分情况。其中3项研究报告了两组术后3个月目测类比评分[10,13,17],各研究间具有同质性(I2=0%,P=0.47),选择固定效应模型进行Meta分析,结果显示术后3个月3D打印组目测类比评分与对照组相近,差异无显著性意义[SMD=-0.27,95%CI(-0.62,0.08),P=0.13]。3项研究报告了两组术后末次随访目测类比评分[10,13,17],各研究间具有同质性(I2=0%,P=0.50),选择固定效应模型进行Meta分析,结果显示末次随访3D打印组目测类比评分与对照组相近,差异无显著性意义[SMD=-0.03,95%CI(-0.33,0.27),P=0.84],见图8。"
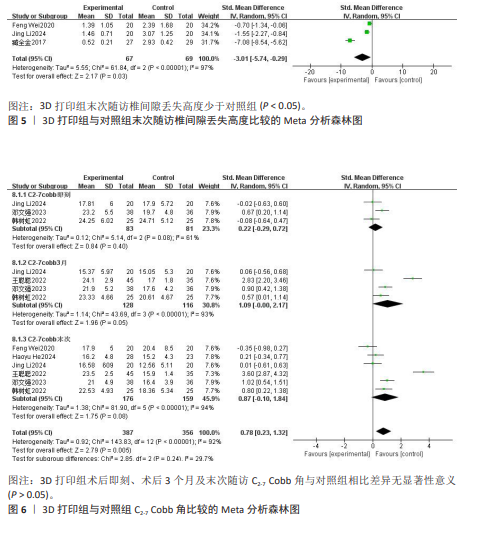
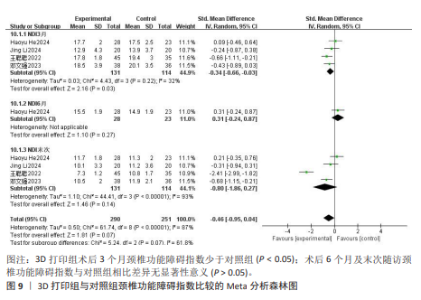
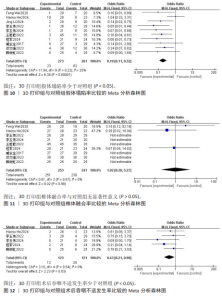
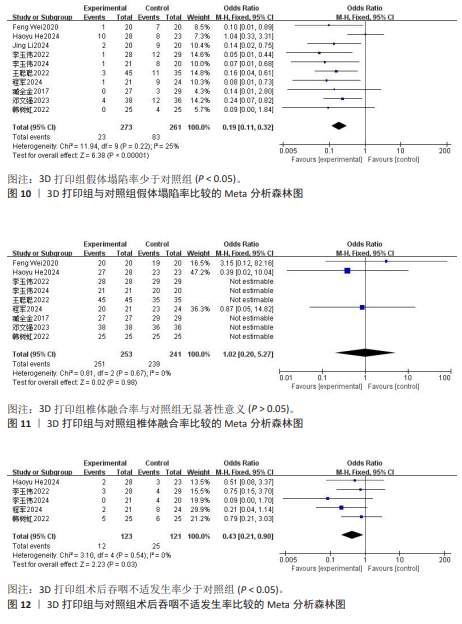
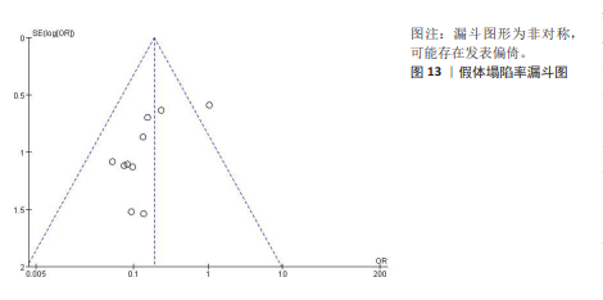
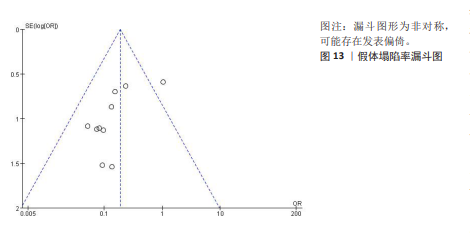
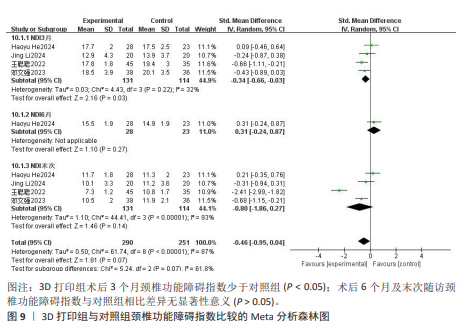
2.3.8 颈椎功能障碍指数 4项研究报告了两组患者的颈椎功能障碍指数[9-10,13,16],根据随访时间进行亚组分析,评价两组患者在术后3,6个月及末次随访颈椎功能障碍指数情况。其中4项研究报告了两组术后3个月的颈椎功能障碍指数[9-10,13,16], 各研究间异质性较小(I2=32%,P= 0.22),选择固定效应模型进行Meta分析,结果显示术后3个月3D打印组颈椎功能障碍指数显著低于对照组,差异有显著性意义[SMD=-0.34,95%CI(-0.66,-0.03),P=0.03]。1项研究报告了两组术后6个月的日本骨科协会评分[9],两组日本骨科协会评分相比差异无显著性意义(P=0.27)。4项研究报告了两组术后末次随访的颈椎功能障碍指数[9-10,13,16],各研究间异质性较大(I2=93%,P < 0.000 01),经敏感性分析未能消除异质性,选择随机效应模型进行Meta分析,结果显示末次随访3D打印组颈椎功能障碍指数与对照组相近,差异无显著性意义[SMD=-0.80,95%CI(-1.86,0.27),P=0.14],见图9。 2.3.9 假体塌陷率 10项研究报告了两组患者的假体塌陷率[8-17],各研究间异质性较小(I2=25%,P=0.22),选择固定效应模型进行Meta分析,结果显示3D打印组假体塌陷率显著低于对照组,差异有显著性意义[OR=0.19,95%CI(0.11,0.32),P < 0.000 01], 见图10。 2.3.10 椎体融合率 9项研究报告了两组患者的椎体融合率[9-17],各研究间具有同质性(I2=0%,P=0.67),选择固定效应模型进行Meta分析,结果显示3D打印组椎体融合率与对照组相近,差异无显著性意义[OR=1.02,95%CI(0.20,5.27),P=0.98],见图11。 2.3.11 术后吞咽不适发生率 5项研究报告了两组患者术后吞咽不适发生率[9,11-12,14,17],各研究间具有同质性(I2=0%,P=0.54),选择固定效应模型进行Meta分析,结果显示3D打印组术后吞咽不适发生率显著低于对照组,差异有显著性意义[OR=0.43,95%CI(0.21,0.90),P=0.03],见图12。"
| [1] LI JC, CHU Y, YI BD, et al. Nano-hydroxyapatite/Polyamide 66 cage in anterior cervical corpectomy and fusion: a comprehensive systematic review and meta-analysis. Eur Rev Med Pharmacol Sci. 2023;27(20):9648-9659. [2] CROFT AJ, WIEDEL AJ, STEINLE AM, et al. Clinical Effectiveness of Anterior Cervical Discectomy and Fusion Using Tritanium C Anterior Cervical Cage vs. PEEK Cage. Spine Surg Relat Res. 2024;8(4):399-408. [3] 马燕燕,桑裴铭,陈斌辉,等.脊髓型颈椎病颈前路椎体次全切钛网植骨融合内固定术后食管肿胀变化的影像学研究[J].中国骨与关节损伤杂志,2021,36(5): 479-481. [4] 郭川,刘庆鹏.颈椎解剖与钛质网笼生物力学研究进展[J].医用生物学,2021, 36(5):829-834. [5] ZHANG HQ, WANG YX, WU JH, et al. Debridement and interbody graft using titanium mesh cage,posterior monosegmental instrumentation,and fusion in the surgical treatment of monosegmental lumbar or lumbosacral pyogenic vertebral osteomyelitis via a posterioronly approach.World Neurosurg. 2020;135:e116-e125. [6] ZHOU E, HUANG H, ZHAO Y, et al. The effects of titanium mesh cage size on the biomechanical responses of cervical spine after anterior cervical corpectomy and fusion: a finite element study. Clin Biomech (Bristol, Avon). 2022;91:105547. [7] KABRA DA, GARG DB. Current applications of 3-dimensional printing in spine surgery. J Orthop. 2023;41:28-32. [8] WEI F, XU N, LI Z, et al. A prospective randomized cohort study on 3D-printed artificial vertebral body in single-level anterior cervical corpectomy for cervical spondylotic myelopathy. Ann Transl Med. 2020;8(17):1070. [9] HE H, FAN L, LÜ G, et al. Myth or fact: 3D-printed off-the-shelf prosthesis is superior to titanium mesh cage in anterior cervical corpectomy and fusion? BMC Musculoskelet Disord. 2024;25(1):96. [10] LI J, ZHANG J, WANG B, et al. Comparison of Titanium Mesh Cage, Nano-Hydroxyapatite/Polyamide Cage, and Three-Dimensional-Printed Vertebral Body for Anterior Cervical Corpectomy and Fusion. Spine (Phila Pa 1976). 2025;50(2):88-95. [11] 李玉伟,王海蛟,崔巍,等.3D打印微孔钛合金人工椎体治疗颈椎后纵韧带骨化症的临床疗效观察[J].陆军军医大学学报,2022,44(15):1542-1548. [12] 李玉伟,李修智,谷世锋,等.自稳定零切迹3D打印人工椎体在颈椎后纵韧带骨化症治疗中的应用观察[J].中华医学杂志,2024,104(7):526-532. [13] 王聪聪,潘伟,王新宏,等.3D打印人工椎体在单节段颈前路椎体次全切除减压融合术中的短期疗效[J].中华骨与关节外科杂志,2022,15(10):785-790. [14] 程军,陈建,谢鲤钟,等.3D打印钛合金骨小梁人工椎体治疗颈椎后纵韧带骨化症[J].中国修复重建外科杂志,2024, 38(5):535-541. [15] 臧全金,卢腾,梁辉,等.3D打印解剖型钛笼与传统钛笼在ACCF术中应用的比较研究[J].中国骨与关节损伤杂志,2017, 32(7):673-676. [16] 邓文强.3D打印人工椎体与钛网重建颈椎序列的对比研究[D].南昌:南昌大学, 2023. [17] 韩树虹,王建华,孙贺,等.3D打印人工椎体与钛笼在颈椎前路椎体次全切除减压植骨融合术中应用的效果比较[J].中国脊柱脊髓杂志,2022,32(5):426-433. [18] 陈恒,薛丛洋,陈双,等.颈椎病的中医认识和经方治疗策略[J].中国中药杂志, 2025,50(9):2596-2604. [19] 崔学军, 姚敏. 颈椎病中西医结合诊疗专家共识[J]. 世界中医药,2023,18(7):918. [20] MCCORMICK JR, SAMA AJ, SCHILLER NC, et al. Cervical spondylotic myelopathy: a guide to diagnosis and management. J Am Board Fam Med. 2020;33(2):303-313. [21] CHEN L, ZHANG Z, LI J, et al. Meta-Analysis of Treatment for Adjacent Two-Segment Cervical Spondylotic Myelopathy: A Comparison Between Anterior Cervical Corpectomy and Fusion and Anterior Cervical Discectomy and Fusion. Global Spine J. 2025;15(3):1839-1848. [22] 曹国龙,陈卓,施集,等.颈椎前路椎体次全切除植骨融合术后钛网沉降的危险因素[J].中国脊柱脊髓杂志,2023, 33(7):602-609. [23] HAJNAL B, POKORNI AJ, TURBUCZ M, et al. Clinical applications of 3D printing in spine surgery: a systematic review. Eur Spine J. 2025;34(2):454-471. [24] 韩俊,黄勇.颈椎ACCF术后出现钛笼下沉的危险因素Logistic 回归分析[J].颈腰痛杂志,2019,40(4):442-444. [25] DIJKMAN MD, VAN BILSEN MWT, FEHLINGS MG, et al. Longterm functional outcome of surgical treatment for degenerative cervical myelopathy. J Neurosurg Spine. 2021;36(5):830-840. [26] 张存鑫,王德春,吕超亮.3D打印技术在脊柱外科应用现状与未来[J].中国矫形外科杂志,2025,33(5):448-453. [27] 江东育,崔跃,吴岳,等.3D打印技术应用于颈椎OPLL前入路术前规划中的临床研究[J].交通医学,2022,36(6):606-609. [28] LI Z, WEI F, LIU Z, et al. Risk factors for Instrumentation failure after total En Bloc Spondylectomy of thoracic and lumbar spine tumors using Titanium Mesh Cage for Anterior Reconstruction. World Neurosurg. 2020;135:e106-106115. [29] MENG M, WANG J, HUANG H, et al.3D printing metal implants in orthopedic surgery: Methods,applications and future prospects. J Orthop Translat. 2023;42:94-112 [30] WANG X, SUN S, JIANG Y, et al. Early clinical efficacy of 3D-printed artificial vertebral body in spinal reconstruction after total en bloc spondylectomy for spinal tumors. BMC Musculoskelet Disord. 2024;25(1):926. [31] CHOY WJ, PARR WCH, PHAN K, et al. 3-dimensional printing for anterior cervical surgery: a review. J Spine Surg. 2018;4(4): 757-769. [32] ZHANG J, WANG S, TANG X, et al. Clinical and radiological comparison of the zero profile anchored cage and traditional cage plate fixation in single level anterior cervical discectomy and fusion. Eur J Med Res. 2022;27(1):189. [33] 勒格石夫,刘知浩,郭灿,等.零切迹椎间融合器与传统钢板联合融合器固定治疗连续三节段颈椎病的疗效比较研究[J].中国修复重建外科杂志,2025,39(2): 193-200. [34] 李玉伟,李修智,严晓云,等.自稳定零切迹3D打印人工椎体治疗脊髓型颈椎病[J].中国修复重建外科杂志,2024,38(5): 529-534. [35] 庄皓翔, 费琦, 杨雍.3D 打印技术在颈椎手术中的应用进展[J].颈腰痛杂志,2022, 43(5):760-762. [36] 蔡兴博, 董艳, 王斌, 等. 金属基 3D 打印支架的构建与功能化研究进展[J]. 生物骨科材料与临床研究 ,2022,19(6):82-87. [37] FOGEL G, MARTIN N, WILLIAMS GM, et al. Choice of Spinal Interbody Fusion Cage Material and Design Influences Subsidence and Osseointegration Performance.World Neurosurg. 2022;162:e626-e634. [38] 贾迎奥,高士涛,王飞.3D打印钛笼裁剪模型在颈前路椎体次全切减压植骨融合中的应用[J].中国组织工程研究,2026, 30(3):604-611. [39] MARTELLI N, SERRANO C, VAN DEN BRINK H, et al.Advantages and disadvantages of 3-dimensional printing in surgery:a systematic review. Surgery. 2016;159(6): 1485-1500. |
| [1] | Wang Qisa, Lu Yuzheng, Han Xiufeng, Zhao Wenling, Shi Haitao, Xu Zhe. Cytocompatibility of 3D printed methyl acrylated hyaluronic acid/decellularized skin hydrogel scaffolds [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1912-1920. |
| [2] | Zhou Hongli, Wang Xiaolong, Guo Rui, Yao Xuanxuan, Guo Ru, Zhou Xiongtao, He Xiangyi. Fabrication and characterization of nanohydroxyapatite/sodium alginate/polycaprolactone/alendronate scaffold [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1962-1970. |
| [3] | Li Guan, Wang Haopeng, Wang Jinbao, Song Xinhao, Qin Guochu, Shao Yang. Feasibility of optimizing radiation dose for three-dimensional printing of the maxillofacial bone based on low-dose CT technology [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1384-1389. |
| [4] | Chen Qiang, Wu Wenjuan, Jiang Shuhua, Huang Da. Physical exercise improves physical function in burn patients: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(5): 1269-1281. |
| [5] | Jiang Yang, Peng Hao, Song Yanping, Yao Na, Song Yueyu, Yin Xingxiao, Li Yanqi, Chen Qigang. Isometric exercise reduces resting blood pressure: a meta-analysis of moderating factors and dose effects [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 975-986. |
| [6] | Sun Jiahe, Shi Jipeng, Zhu Tianrui, Quan Helong, Xu Hongqi. Effect of exercise intervention in elderly individuals with sarcopenia and its comorbidities: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(4): 997-1007. |
| [7] | Jia Yingao, Gao Shitao, Wang Fei. Application of 3D printed titanium cage cutting model in anterior cervical vertebrae subtotal decompression and bone graft fusion [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 604-611. |
| [8] | Wang Jiangjing, Zhao Na, Hu Xiaona, Zhao Na . Safety of 3D printed titanium alloy bone trabecular cup prosthesis combined with modified Kidney Tonifying and Blood Activating Decoction for elderly hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 612-619. |
| [9] | Tang Ya, Li Long, Huang Du, Huang Zhaolu. Systematic review of the effect of 3D-printed exoskeleton on hand function rehabilitation in stroke patients [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(29): 7648-7653. |
| [10] | Fan Mengmeng, Ding Jiali, Wan Yujie, Huang Hailiang. A systematic review and network meta-analysis of neuromodulation techniques for promoting upper limb motor function after stroke [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(28): 7494-7504. |
| [11] | Xia Caigui, Li Wei, Su Yuying, Shi Yu, Yang Zhonghe. Effects of antioxidant pretreatment on skeletal muscle damage and oxidative stress following acute high-intensity exercise: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(24): 6345-6353. |
| [12] | Fang Enhui, Guan Hui, Ma Lihong. Non-invasive brain stimulation for core symptoms in children with autism spectrum disorder: a network meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(24): 6373-6381. |
| [13] | Li Yanfeng, Zhang Yilin, Kong Hao, Zheng Hang, Liu Jiajun, Yin Mingyue, Qiu Bopeng, Huang Kongyun, Liu Hengxian, Zhong Yuming, Chen Jun, Xu Kai. Effect of blood flow restriction training on the magnitude and temporal characteristics of post-activation performance enhancement: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(23): 6150-6146. |
| [14] | Tang Hao, Zhong Qian, Wu Honghan, Wu Hengpeng, Wu Xingkai, Wa Qingde. 3D-printed biodegradable polyester-based scaffolds in bone regeneration therapy [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(20): 5304-5311. |
| [15] | Wang Zitong, Wu Zijian, Yang Aofei, Mao Tian, Fang Nan, Wang Zhigang. Biomaterials regulate microenvironment imbalance for treating spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(20): 5321-5330. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||