Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (32): 5144-5149.doi: 10.12307/2023.592
Previous Articles Next Articles
Effects of naringin on healing of tooth extraction wound in osteoporotic rats
Huang Haozhe1, 2, 3, Zheng Min1, 2, 3, Li Na1, 2, 3, Sun Libo4, Lan Yuyan1, 2, 3, Liu Min1, 2, 3
- 1Department of Prosthodontics, The Affiliated Stomatological Hospital of Southwest Medical University, Luzhou 646000, Sichuan Province, China; 2Luzhou Key Laboratory of Oral & Maxillofacial Reconstruction and Regeneration, Luzhou 646000, Sichuan Province, China; 3Institute of Stomatology, Southwest Medical University, Luzhou 646000, Sichuan Province, China; 4Department of Stomatology, Luzhou People’s Hospital, Luzhou 646000, Sichuan Province, China
-
Received:2022-07-22Accepted:2022-09-15Online:2023-11-18Published:2023-03-23 -
Contact:Lan Yuyan, Master, Lecturer, Department of Prosthodontics, The Affiliated Stomatological Hospital of Southwest Medical University, Luzhou 646000, Sichuan Province, China; Luzhou Key Laboratory of Oral & Maxillofacial Reconstruction and Regeneration, Luzhou 646000, Sichuan Province, China; Institute of Stomatology, Southwest Medical University, Luzhou 646000, Sichuan Province, China -
About author:Huang Haozhe, Master candidate, Department of Prosthodontics, The Affiliated Stomatological Hospital of Southwest Medical University, Luzhou 646000, Sichuan Province, China; Luzhou Key Laboratory of Oral & Maxillofacial Reconstruction and Regeneration, Luzhou 646000, Sichuan Province, China; Institute of Stomatology, Southwest Medical University, Luzhou 646000, Sichuan Province, China -
Supported by:Science and Technology Bureau of Luzhou City, No. 2017-S-42(1/2) (to SLB); Innovation and Entrepreneurship Training Program for College Students of Sichuan Province, No. Q18011 (to LYY [advisor]); Sichuan College Students Innovation and Entrepreneurship Training Program, No. S202210632150 (to LYY [advisor])
CLC Number:
Cite this article
Huang Haozhe, Zheng Min, Li Na, Sun Libo, Lan Yuyan, Liu Min. Effects of naringin on healing of tooth extraction wound in osteoporotic rats[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(32): 5144-5149.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
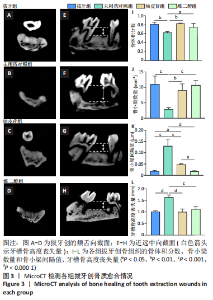
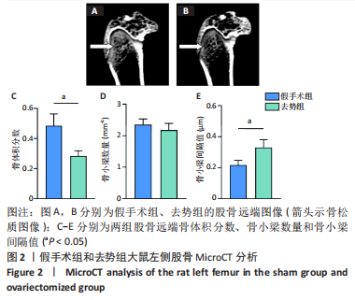
2.3 MicroCT检测拔牙创骨质愈合情况 与未用药对照组大鼠相比,柚皮苷组大鼠拔牙创骨小梁形态均较正常,排列紧密,骨髓腔小。柚皮苷组大鼠拔牙创骨体积分数和骨小梁数量分别为(82.82±1.25)%和(9.104±2.044) mm-1,明显高于未用药对照组[(62.64±2.34)%和(2.944±0.460) mm-1](P < 0.01),而骨小梁间隔和牙槽骨高度丧失量显著降低,分别由(0.130±0.030) μm和(1.637±0.098) mm降低至(0.050±0.003) μm和(1.006±0.098) mm(P < 0.001)。柚皮苷组大鼠拔牙创与雌二醇组相比,仅骨小梁间隔有显著差异(P < 0.01),其余指标差异无显著性意义(P > 0.05),见图3。"

| [1] PAVONE V, TESTA G, GIARDINA SMC, et al. Pharmacological Therapy of Osteoporosis: A Systematic Current Review of Literature. Front Pharmacol. 2017;8:803. [2] JOHNELL O, KANIS JA. An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int. 2006;17(12):1726-1733. [3] KOTH VS, SALUM FG, DE FIGUEIREDO MAZ, et al. Repercussions of osteoporosis on the maxillofacial complex: a critical overview. J Bone Miner Metab. 2021;39(2):117-125. [4] ARIOKA M, ZHANG X, LI Z, et al. Osteoporotic Changes in the Periodontium Impair Alveolar Bone Healing. J Dent Res. 2019;98(4):450-458. [5] CHEN CH, WANG L, SERDAR TULU U, et al. An osteopenic/osteoporotic phenotype delays alveolar bone repair. Bone. 2018;112:212-219. [6] 杨红梅. 1987-2019年中国老年人牙周病流行趋势的系统评价及meta分析 [D].重庆:重庆医科大学,2019. [7] 国家卫生健康委员会官网.国家卫生健康委发布首个中国骨质疏松症流行病学调查结果[J].人口文摘,2018(11):55-56. [8] NICOLIELO LFP, VAN DESSEL J, JACOBS R, et al. Relationship between trabecular bone architecture and early dental implant failure in the posterior region of the mandible. Clin Oral Implants Res. 2020;31(2):153-161. [9] DO TA, LE HS, SHEN YW, et al. Risk Factors related to Late Failure of Dental Implant-A Systematic Review of Recent Studies. Int J Environ Res Public Health. 2020;17(11):3931. [10] 李微, 张博, 张雨薇,等.雌激素调节骨代谢作用的研究进展 [J].中国骨质疏松杂志,2017,23(2):262-266. [11] WAJANAVISIT W, SUPPACHOKMONGKORN S, WORATANARAT P, et al. The Association of Bone Mineral Density and G2014A Polymorphism in the Estrogen Receptor Alpha Gene in Osteoporotic Hip Fracture in Thai Population. J Med Assoc Thai. 2015;98 Suppl 8:S82-87. [12] LAVRADOR P, GASPAR VM, MANO JF. Bioinspired bone therapies using naringin: applications and advances. Drug Discov Today. 2018;23(6):1293-1304. [13] SHAO Y, YOU D, LOU Y, et al. Controlled Release of Naringin in GelMA-Incorporated Rutile Nanorod Films to Regulate Osteogenic Differentiation of Mesenchymal Stem Cells. ACS Omega. 2019; 4(21): 19350-19357. [14] 刘小坡,冯云波,曹国龙,等. 柚皮苷对老年大鼠骨质疏松性骨折愈合的影响[J].中国临床药理学杂志,2020,36(9):1117-1120. [15] 王庚启,王黎明,谢林,等.柚皮苷对去势大鼠骨质疏松性骨折愈合的影响[J].上海中医药大学学报,2016,30(4):73-79. [16] CHEN LL, LEI LH, DING PH, et al. Osteogenic effect of Drynariae rhizoma extracts and Naringin on MC3T3-E1 cells and an induced rat alveolar bone resorption model. Arch Oral Biol. 2011;56(12):1655-1662. [17] YASUDA H. Discovery of the RANKL/RANK/OPG system. J Bone Miner Metab. 2021;39(1):2-11. [18] ZENG H, ZHAO X, WANG L, et al. Effects of Drynaria Total Flavonoid on the Microstructure of the Mandible in Ovariectomized Rats. Med Sci Monit. 2020;26: e926171. [19] YU KE, ALDER KD, MORRIS MT, et al. Re-appraising the potential of naringin for natural, novel orthopedic biotherapies. Ther Adv Musculoskelet Dis. 2020;12: 1759720X20966135. [20] 李明,吕厚辰,尹鹏滨,等.两种卵巢切除术式建立大鼠骨质疏松模型的优势比较[J].解放军医学院学报,2015,36(4):383-387. [21] 何小苏.柚皮苷对绝经后骨质疏松症的成骨作用研究[D].大理:大理大学, 2019. [22] 刘攀杰,李永贤,马延怀,等.改良式背部正中单切口入路卵巢切除术构建大鼠骨质疏松模型的研究[J].山西医科大学学报,2020,51(8):813-818. [23] 侯佳伟. 从七次全国人口普查看我国人口发展新特点及新趋势 [J].学术论坛, 2021,44(5):1-14. [24] PASSARELLI PC, PAGNONI S, PICCIRILLO GB, et al. Reasons for Tooth Extractions and Related Risk Factors in Adult Patients: A Cohort Study. Int J Environ Res Public Health. 2020;17(7):2575. [25] VAN DE RIJT LJM, STOOP CC, WEIJENBERG RAF, et al. The Influence of Oral Health Factors on the Quality of Life in Older People: A Systematic Review. Gerontologist. 2020;60(5):e378-e394. [26] LEE JH, HAN SS, LEE C, et al. Microarchitectural changes in the mandibles of ovariectomized rats: a systematic review and meta-analysis. BMC Oral Health. 2019;19(1):128. [27] YUAN X, PEI X, ZHAO Y, et al. A Wnt-Responsive PDL Population Effectuates Extraction Socket Healing. J Dent Res. 2018;97(7):803-809. [28] LIU Y, LI Z, ARIOKA M, et al. WNT3A accelerates delayed alveolar bone repair in ovariectomized mice. Osteoporos Int. 2019;30(9):1873-1885. [29] CHATTERJEE M, FAOT F, CORREA C, et al. Is the Jaw Bone Micro-Structure Altered in Response to Osteoporosis and Bisphosphonate Treatment? A Micro-CT Analysis. Int J Mol Sci. 2021;22(12):6559. [30] PATULLO IM, TAKAYAMA L, PATULLO RF, et al. Influence of ovariectomy and masticatory hypofunction on mandibular bone remodeling. Oral Dis. 2009;15(8):580-586. [31] MA Z, LI S, SUN Y. Effect of enhanced masticatory force on OPG, RANKL and MGF in alveolar bone of ovariectomized rats. J Appl Oral Sci. 2020;28:e20190409. [32] SUN Y, WAN B, WANG R, et al. Mechanical Stimulation on Mesenchymal Stem Cells and Surrounding Microenvironments in Bone Regeneration: Regulations and Applications. Front Cell Dev Biol. 2022;10:808303. [33] SUN Z, HERRING SW, TEE BC, et al. Alveolar ridge reduction after tooth extraction in adolescents: an animal study. Arch Oral Biol. 2013;58(7):813-825. [34] WHITE SC, RUDOLPH DJ. Alterations of the trabecular pattern of the jaws in patients with osteoporosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(5):628-635. [35] SÓ BB, SILVEIRA FM, LLANTADA GS, et al. Effects of osteoporosis on alveolar bone repair after tooth extraction: A systematic review of preclinical studies. Arch Oral Biol. 2021;125:105054. [36] 王宁涛,李萌宇,华洪飞, 等.去卵巢骨质疏松大鼠拔牙创模型研究[J].口腔医学,2017,37(6):481-484. [37] AN J, YANG H, ZHANG Q, et al. Natural products for treatment of osteoporosis: The effects and mechanisms on promoting osteoblast-mediated bone formation. Life Sci. 2016;147:46-58. [38] SHANGGUAN WJ, ZHANG YH, LI ZC, et al. Naringin inhibits vascular endothelial cell apoptosis via endoplasmic reticulum stress‑ and mitochondrial‑mediated pathways and promotes intraosseous angiogenesis in ovariectomized rats. Int J Mol Med. 2017;40(6):1741-1749. [39] LI P, WU H, WANG Y, et al. Toxicological evaluation of naringin: Acute, subchronic, and chronic toxicity in Beagle dogs. Regul Toxicol Pharmacol. 2020;111:104580. [40] ZHU Z, XIE W, LI Y, et al. Effect of Naringin Treatment on Postmenopausal Osteoporosis in Ovariectomized Rats: A Meta-Analysis and Systematic Review. Evid Based Complement Alternat Med. 2021;2021:6016874. [41] RAMESH P, JAGADEESAN R, SEKARAN S, et al. Flavonoids: Classification, Function, and Molecular Mechanisms Involved in Bone Remodelling. Front Endocrinol (Lausanne). 2021;12:779638. [42] LI N, JIANG Y, WOOLEY PH, et al. Naringin promotes osteoblast differentiation and effectively reverses ovariectomy-associated osteoporosis. J Orthop Sci. 2013; 18(3):478-485. [43] GE X, ZHOU G. Protective effects of naringin on glucocorticoid-induced osteoporosis through regulating the PI3K/Akt/mTOR signaling pathway. Am J Transl Res. 2021;13(6):6330-6341. [44] VARGAS-SANCHEZ PK, FERNANDES RR, FURLANETO FAC, et al. Osteoporosis Affects Functional Activity and Gene Expression of Osteoblastic Cells Derived from Rat Alveolar Bone. Braz Dent J. 2020;31(6):617-622. [45] NIU Q, HE J, WU M, et al. Transplantation of bone marrow mesenchymal stem cells and fibrin glue into extraction socket in maxilla promoted bone regeneration in osteoporosis rat. Life Sci. 2022;290:119480. [46] GENG Q, GAO H, YANG R, et al. Pyrroloquinoline Quinone Prevents Estrogen Deficiency-Induced Osteoporosis by Inhibiting Oxidative Stress and Osteocyte Senescence. Int J Biol Sci. 2019;15(1):58-68. [47] TAKEGAHARA N, KIM H, CHOI Y. RANKL biology. Bone. 2022;159:116353. [48] UDAGAWA N, KOIDE M, NAKAMURA M, et al. Osteoclast differentiation by RANKL and OPG signaling pathways. J Bone Miner Metab. 2021;39(1):19-26. [49] YASUDA H. Anti-RANKL antibody was approved for the treatment of osteoporosis in Japan. Nihon Rinsho Meneki Gakkai Kaishi. 2013;36(4):209-216. [50] TSUKASAKI M, ASANO T, MURO R, et al. OPG Production Matters Where It Happened. Cell Rep. 2020;32(10):108124. [51] WU GJ, CHEN KY, YANG JD, et al. Naringin Improves Osteoblast Mineralization and Bone Healing and Strength through Regulating Estrogen Receptor Alpha-Dependent Alkaline Phosphatase Gene Expression. J Agric Food Chem. 2021;69(44):13020-13033. |
| [1] | He Xi, Wan Yu, Tang Yuting, Yang Anning, Wu Kai, Jiao Yun, Bai Zhigang, Jiang Yideng, Shen Jiangyong. Erastin inhibits proliferation of hypertrophic scar fibroblasts [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-. |
| [2] | Zhong Yizheng, Huang Peizhen, Cai Qunbin, Zheng Liqin, He Xingpeng, Dong Hang. Microstructural indexes that determine the trabecular bone maximum stress of micro-finite element models [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1313-1318. |
| [3] | Cao Sheng, Kong Lingwei, Xu Kun, Sun Zhijie. Correlation of cervical sagittal force line parameters with degenerative segment and Pfirrmann classification in patients with cervical intervertebral disc degeneration [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1319-1324. |
| [4] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [5] | Ke Yuqi, Chen Changjian, Wu Hao, Zheng Lianjie. Comparison of 12-month follow-up results of primary total hip arthroplasty between modified direct anterior approach and direct anterior approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1377-1382. |
| [6] | Zhang Lichuang, Gao Huali, Wang Jingchao, Lin Huijun, Wu Chonggui, Ma Yinghui, Huang Yunfei, Fang Xue, Zhai Weitao. Effect of tendon manipulation with equal emphasis on muscles and bones on accelerating the functional rehabilitation of quadriceps femoris after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1383-1389. |
| [7] | Du Xueting, Zhang Xiaodong, Chen Yanjun, Wang Mei, Chen Wubiao, Huang Wenhua. Application of compressed sensing technology in two-dimensional magnetic resonance imaging of the ankle joint [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1396-1402. |
| [8] | You Zhengqiu, Zhang Zhongzu, Wang Qunbo. Early symptomatic intervertebral disc pseudocysts after discectomy detected on MRI [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1403-1409. |
| [9] | Li Chao, Zhang Peipei, Xu Mengting, Li Linlin, Ding Jiangtao, Liu Xihua, Bi Hongyan. Respiratory training improves morphological changes of the multifidus muscle in patients with chronic nonspecific lower back pain assessed by musculoskeletal ultrasound [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1417-1421. |
| [10] | He Yinhao, Li Xiaosheng, Chen Hongwen, Chen Tiezhu. 3D printed porous tantalum metal in the treatment of developmental dysplasia of the hip: current status and application prospect [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1455-1461. |
| [11] | Jiang Xiaocheng, Shi Lu, Wang Yinbin, Li Qiujiang, Xi Chuangzhen, Ma Zefeng, Cai Lijun. Systematical evaluation of bone fusion rate after interbody fusion in patients with osteoporosis and lumbar degenerative disease treated with teriparatide [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1427-1433. |
| [12] | Sun Jiajia, Zhu Haidi, Lu Yun, Zhang Kai. Comparison of bone metabolism markers between type 2 diabetes mellitus and non-type 2 diabetes mellitus patients with hip fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1156-1160. |
| [13] | Tang Liang, Li Xiheng, Niu Ruijuan, Li Xinyue, Zou Xinying, Mao Tianjiao, Li Jiang. Naringin regulates the function of RAW264.7 macrophages to affect the osteogenic differentiation of MC-3T3-E1 cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1205-1210. |
| [14] | Li Mengfei, Zhang Hong, Zhao Shaojian, Yin Guanghao, Wang Qibao. Expression of forkhead box protein 3 in refractory periapical periodontitis in rats with Enterococcus faecalis infection [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1187-1192. |
| [15] | Lian Shilin, Zhang Yan, Jiang Qiang, Zhang Hanshuo, Li Tusheng, Ding Yu. Interventional effects of whole blood and platelet-rich plasma with different preparation methods on nucleus pulposus cells [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1199-1204. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||