Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (5): 774-779.doi: 10.12307/2022.126
Previous Articles Next Articles
Roles and values of blood flow restriction training in the rehabilitation of knee joint diseases
Wei Xing, Liu Shufang, Mao Ning
- Guangzhou Sport University, Guangzhou 510500, Guangdong Province, China
-
Received:2020-10-04Revised:2020-10-12Accepted:2020-11-13Online:2022-02-18Published:2021-12-02 -
Contact:Liu Shufang, MD, Associate professor, Guangzhou Sport University, Guangzhou 510500, Guangdong Province, China -
About author:Wei Xing, Master candidate, Guangzhou Sport University, Guangzhou 510500, Guangdong Province, China -
Supported by:a grant from Guangdong Provincial Sports Bureau Project, No. GDSS2020N103 (to LSF)
CLC Number:
Cite this article
Wei Xing, Liu Shufang, Mao Ning. Roles and values of blood flow restriction training in the rehabilitation of knee joint diseases[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 774-779.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

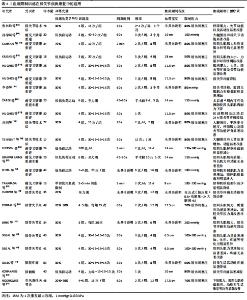
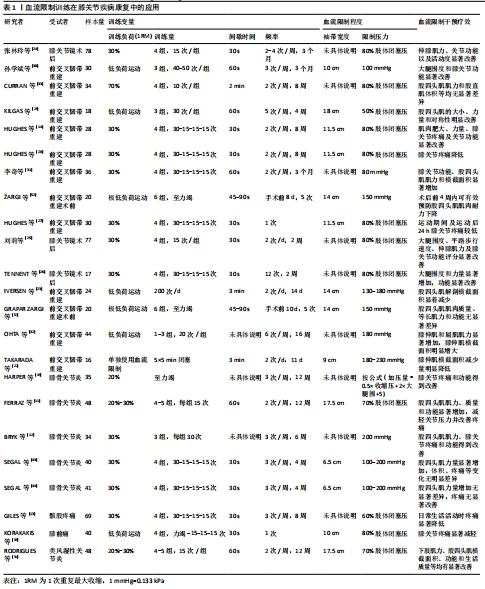
2.1.1 膝关节术后 膝关节前交叉韧带和半月板损伤是一种常见的运动损伤,为了减少活动相关的失能和可能导致再次损伤的膝关节不稳定,对前交叉韧带撕裂患者,支持进行外科手术[18-19]。膝关节术后康复的主要目标是恢复到损伤前的运动水平,目前的康复指南建议,为引起肌肉大小和力量的显著增长,需使用≥70%1RM的质量进行训练[8]。然而,术后患者常因疼痛或肌无力而无法完成高强度训练或在训练进展阶段不能完全耐受高强度训练;另外,术后下肢肌肉萎缩和肌肉无力问题可能导致患者长期康复和预后下降[20-21]。因此,预防肌肉萎缩、促进肌肉力量增长和肌肉肥大、使患者能够尽早恢复到伤前运动水平尤为重要。 BFRT作为一种新兴的康复训练方式在膝关节术后康复中的应用在逐渐增加,其以较低的运动强度便能促进肌肉力量增长和肌肉肥大。研究表明即使是在单独使用血流限制的情况下,与对照组相比,血流限制组使肌肉萎缩减少了近50%[22]。而另一项对前交叉韧带重建术后患者的研究采用类似的研究方案(2次/d,5组5 min闭塞,限制压力值为130-180 mmHg,组间间歇3 min)进行股四头肌等长收缩和直腿抬高训练,干预14 d后发现对照组和干预组的股四头肌解剖横截面积均明显减少,在股四头肌萎缩方面,两组之间没有显著差异[23]。值得注意的是,IVERSEN等[23]认为结果上的差异可能与研究中训练强度低于减少股四头肌萎缩所必需的最小强度(10%1RM)有关,并建议未来的研究应使用肌肉体积而不是解剖横截面积作为股四头肌萎缩预后指标。 此外,大多数研究表明,即使在低至20%-30%1RM的运动强度下也显示出有益的训练效果。张林玲等[24]将78例膝关节微创手术患者分为常规康复训练组和常规康复训练结合血流限制组,两组均进行常规康复训练,血流限制组运动前在大腿近端放置充气式止血带,并充气至80%肢体闭塞压以30%1RM的阻力进行伸膝运动,结果发现血流限制组膝关节功能评分、活动度以及伸膝肌力显著高于常规组。研究表明BFRT有助于提高膝关节微创手术早期肌力、关节功能以及活动度,能降低慢性疼痛、下肢瘀斑/肿胀等并发症的发生率。另外刘莉等[25]和TENNENT等[26]以膝关节镜术后患者为实验对象,进行为期2周的BFRT,阻力为30%1RM,限制压力值为80%肢体闭塞压,训练量为每次4组,分别重复60次和75次,训练频率分别为每天2次和每周6次,结果发现血流限制组大腿围度、伸膝肌力及膝关节功能在两项研究中均有显著改善。研究表明术后治疗方案中增加BFRT干预可改善患者的肌肉力量、肌肉体积及关节功能,且在研究期间未观察到任何不良事件[24-26]。HUGHES等[14]对28例前交叉韧带重建患者进行了为期8周的康复干预,研究发现BFRT(30% 1RM)在改善肌肉力量和大小方面与高强度抗阻训练(70%1RM)相似,并且可以更大程度地减少膝关节疼痛和肿胀,从而改善整体身体功能。HUGHES等[27]比较了前交叉韧带重建患者和非受伤人群对BFRT和高强度抗阻训练的急性知觉和血压反应,对前交叉韧带重建患者研究发现,BFRT组的主观感觉疲劳程度与高强度抗阻训练组相似,肌肉疼痛高于高强度训练组,运动期间及运动后24 h膝关节疼痛均低于高强度训练组,两组运动前后血压无异常。因此,作者认为BFRT对训练期间患者的依从性产生积极影响,并对膝关节疼痛产生有利影响。同一作者的另一项关于BFRT舒适性和疼痛性的研究也有类似的发现[28]。HUGHES等[14,27-28]的前后3项研究证明了BFRT比高负荷抗阻训练更适合前交叉韧带重建患者,同时也能有效改善患者的肌力和功能。 在一项基于家庭的BFRT中,KILGAS等[29]对9例平均前交叉韧带术后5年的患者进行为期4周训练后,发现试验组有效提高了股四头肌大小和力量,且减少了患腿/健腿的不对称性。此外,孙学斌等[30]、李奇等[31]和OHTA等[32]对前交叉韧带重建术后患者进行血流限制结合低负荷训练的研究也发现了BFRT改善肌肉大小和力量的积极作用。然而,CURRAN等[33]研究了血流限制(80% 肢体闭塞压)结合高强度抗阻训练(70%1RM)对前交叉韧带重建患者股四头肌功能恢复的影响,对34例患者进行为期8周(每周2次,每次4组,重复40次,组间间歇2 min)的康复介入后,发现血流限制与高强度抗阻训练结合使用对前交叉韧带重建术后股四头肌肌力、激活或萎缩恢复没有显著改善。研究表明前交叉韧带重建术后改善股四头肌肌肉功能,BFRT与高强度抗阻训练的结合使用可能不是必要的。 综上所述,在膝关节术后康复中以较低的运动强度(20%-30% 1RM)进行为期2-12周[11,25-26,34]、每周两三次、每次三四组、重复10-50次/力竭的血流限制(50%-80%肢体闭塞压)抗阻训练,便能促进肌肉力量增长和肌肉肥大,并且血流限制单独使用可以有效防止由于无负荷状态导致的失用性肌萎缩,有利于加速膝关节术后康复进程。 2.1.2 髌股关节痛和膝前痛 髌股疼痛是一种常见的慢性肌肉骨骼疾病,表现为髌股关节负荷活动(如下蹲、上下楼梯和跑步)时髌骨周围或后面的疼痛[35],与髌股疼痛相关的疼痛和症状限制了对日常和工作活动的参与,并降低了身体活动水平[36-37]。膝前痛是一种非特异性诊断,常见于前交叉韧带重建和/或半月板手术后,股四头肌强化被认为可以减少膝前痛[38]。GILES等[13]将79例髌股疼痛患者分为标准股四头肌强化组(70%1RM)和血流限制组(30%1RM),进行为期8周的康复干预,结果发现,与标准组相比,血流限制组在减少日常活动的疼痛方面更有效,可以使股四头肌力量得到更大的改善。此外,另一项关于膝前痛患者的研究发现低负荷BFRT可有效减轻功能活动中的疼痛[39]。因此,对于因疼痛而不能耐受标准化股四头肌强化训练(70%1RM)的髌股疼痛和膝前痛患者而言,BFRT可能是一种有用的替代方案。 2.1.3 膝关节骨关节炎 膝关节骨关节炎是一种慢性退行性病变,其特征是慢性疼痛、身体功能障碍和生活质量下降[40-41]。美国风湿病学院和关节炎基金会建议,对膝关节炎患者而言,增加力量不仅可以减轻症状,还有助于降低关节恶化风险[42]。 目前,在对膝骨关节炎人群进行BFRT干预的研究中,受试者主要为女性。且仅有一项研究对限制压力进行个体化设置[11],其他要么是根据前人研究设置加压值[12,43-44],要么是根据公式设置加压值[45]。HARPER等[45]为了观察BFRT在老年膝骨关节炎患者中的安全性和可行性,将35例患有膝关节炎的老年人(≥60岁)分为BFRT组和中等强度抗阻训练组,血流限制组以20%1RM的负荷进行为期12周、每周3次运动至力竭的康复训练,其中加压值按照公式(加压量=0.5×收缩压+2×大腿围+5)设置,研究报道了14例膝关节疼痛的报告(血流限制组3例,中等强度抗阻训练组11例),两组的训练出勤率达80%以上,结果发现对于老年骨关节炎患者而言,BFRT是一种安全可行的替代方案,可以改善老年骨关节炎患者的疼痛和功能。FERRAZ等[11]以48例女性膝关节骨关节炎患者为研究对象,进行为期12周、每周2次的低强度(20%-30%1RM)血流限制(70%肢体闭塞压)训练,结果发现血流限制组和高强度抗阻训练组均能够增加骨关节炎患者的肌肉力量、质量和功能,而且BFRT还能够在减少关节压力的同时改善疼痛。另一项对34例女性骨关节炎患者的研究[为期6周,每周3次的低强度(30%1RM)血流限制 (200 mmHg)训练]也有类似的发现[12]。SEGAL等[43]对有膝关节炎风险的40例女性进行为期4周、每周3次的低强度康复训练,血流限制组在训练基础上加上100-200 mmHg的限制压力,结果发现与对照组相比,BFRT可有效增加膝骨关节炎风险女性的腿部蹬伸和膝伸肌力量。然而,另一项对有膝关节炎风险男性的研究使用相同的BFRT方案,结果发现与对照组相比,BFRT并不能显著增加有膝骨关节炎风险男性的腿部蹬伸和膝伸肌力量[44]。这种结果上的差异可能是因为性别差异引起的实际血流限制程度不一致,统一设定的限制压力可能不会对所有人的血流造成相同程度的限制,即男性的大腿围通常比女性大,对男性患者而言,统一设置的加压值100-200 mmHg可能不足以诱导肌肉生长。 综上所述,血流限制能够改善膝骨关节炎患者的肌肉力量、肌肉体积,以及减少运动或日常生活中的疼痛和不适感。有学者指出大腿围是血流限制压力的一个重要预测因子[46],较大的肢体需要更高的压力才能达到与较小肢体相同的压力水平[47]。因此,在实际应用中,应考虑肢体围度对血流限制程度的影响,建议使用肢体闭塞压的百分比设定加压值以便安全有效地限制血流。 2.1.4 类风湿性关节炎 类风湿性关节炎是一种慢性、全身性自身免疫性疾病,其典型症状为关节疼痛、肿胀、畸形[48],肌力丧失是类风湿性关节炎患者的常见特征[49]。RODRIGUES等[34]将48例类风湿性关节炎患者分为高强度训练组(70%1RM)、血流限制组(30%1RM)和对照组,进行为期12周、每周2次的血流限制(70%肢体闭塞压)训练后,发现BFRT能有效改善类风湿性关节炎患者的下肢肌力、股四头肌横截面积、功能和健康相关的生活质量。研究表明,对于类风湿性关节炎患者而言,低强度抗阻BFRT是一种可行的治疗方法。 2.2 BFRT在膝关节疾病康复中的应用方案 目前的研究表明,在膝关节疾病康复中,BFRT具有与高强度抗阻训练相似的效益,且膝关节疼痛较少;与单纯的低强度抗阻训练相比,BFRT在肌肉肥大和力量方面表现出更有效的提高。BFRT的低负荷性使其受到越来越多的关注,但在实际应用中,血流限制训练仍受训练变量和血流限制程度以及个体特征的影响,主要包括训练类型、训练负荷、训练量、间歇时间、训练频率、袖带宽度、肢体围度及限制压力等。 2.2.1 训练类型 在膝关节疾病康复中,血流限制多与低负荷抗阻训练结合使用,采用单关节和/或多关节力量训练,这些研究大都证实了其对肌肉大小和力量的益处[11-12,14,24-26,29-32,34,43]。此外,血流限制的单独使用(5×5 min闭塞,限制压力值为180-230 mmHg,组间间歇3 min)可以减轻前交叉韧带重建患者术后失用性肌肉萎缩[22]。综合来看,在康复早期,对于无法承受低负荷抗阻训练的患者而言,单独使用血流限制可以减轻失用性肌肉萎缩。在康复进展阶段,血流限制可结合低负荷的单关节和/或多关节抗阻训练以促进肌肉肥大和力量增长。 2.2.2 训练负荷 现有BFRT研究常采用的负荷质量为20%-30%1RM,血流限制结合低负荷抗阻训练可以有效增加肌肉质量和力量,减轻关节压力并改善关节疼痛[11]。一项对膝关节骨关节炎患者的研究表明,为期6周的血流限制结合低负荷抗阻训练(30%1RM,每周训练3次,每次3组,每组重复30次),可以有效改善股四头肌肌力、功能并减轻疼痛[12]。另有在同等训练负荷下结合血流限制的研究也显示出同等疗效[11,14]。然而,CURRAN等[33]的研究表明,前交叉韧带重建患者进行为期8周、每周2次的血流限制(限制压力值为80%肢体闭塞压)结合高强度抗阻训练(4组,重复40次,70%1RM,组间间歇2 min),股四头肌肌力和股直肌体积变化均无显著差异。由此可见,在膝关节疾病康复中,血流限制抗阻训练的负荷质量设置为20%-30%1RM可能有利于增强肌肉的大小和力量。 2.2.3 训练量 以往关于血流限制结合阻力训练的研究中有常用的重复次数方案,共4组练习,第1组重复30次,后3组分别重复15次共75次[50-51]。有些研究依据75次重复方案来实施阻力训练[13-14,26-28,31,43-44],有些进行3-5组练习,重复次数10-50次不等[11-12,24-25,29- 30,32-34,42],或运动至力竭[45,52-53]。 2.2.4 间歇时间 大部分血流限制结合低负荷抗阻训练都采用30-60 s,有些研究组间间歇两三分钟[22-23,33]。为保证足够的静脉阻塞,研究建议休息期间保持闭塞刺激[51]。 2.2.5 训练频率 大多保持每周两三次,持续时间2-12周不等。根据以往研究可知,每周两三次的训练频率足以促进肥大效应[51],BFRT的训练频率从6次/周到2次/d不等[22-23,25,32]。刘莉等[25]采用30%1RM、4组共60次的方案进行每天2次的BFRT后,发现大腿围度、平路步行速度、伸膝肌力及膝关节功能评分显著改善,且未发现任何不良事件。另一项对前交叉韧带重建患者急性知觉反应的研究(1 d)发现,相比于高负荷组,血流限制组运动期间及运动后24 h膝关节疼痛较轻[27]。 2.2.6 袖带宽度和肢体围度 现有研究的袖带宽度为6.5-18 cm,而有些研究未具体说明所使用袖带尺寸[12-13,24-26,31-32,45]。有学者报道,宽的血流限制袖带限制动脉血流的压力比窄的血流限制袖带低,高幅度(160-240 mmHg)的闭塞压力可能会导致部分人完全缺血,这取决于肢体围度[46]。因此,未来的研究应考虑所用袖带的宽度以及肢体围度,加压部位围度越大,所需的加压压力也越大。 2.2.7 限制压力 限制压力是影响BFRT效果的一个重要因素,现有研究中,设定压力值的方式不尽相同,12项研究以肢体闭塞压的百分比(50%-80%)来确定压力值[11,13-14,24-29,33-34,39];10项研究是根据前人经验设定压力值,主要在80-230 mmHg范围内[12,22-23,30-32,43-44,52-53];也有研究按公式(加压量=0.5×收缩 压+2×大腿围+5)设定限制压力值[45]。 2.3 BFRT在应用中的注意事项 目前,血流限制的最佳方案仍是未知的。SCOTT等[51]的指南为BFRT的应用提供了一个框架,建议袖带宽度为下肢(6-13.5 cm)宽袖带(较宽的袖带在更低的压力下完成闭塞);血流限制压力为40%-80%的肢体闭塞压(较大的肢体需要更高的压力);训练强度为20%-40% 1RM/最大自主收缩力量;单关节和多关节运动均有益;训练量为50-80次(分组完成),推荐标准的30-15-15-15方案共75次重复;组间休息30-45 s(为保证足够的静脉阻塞,建议休息期间保持闭塞刺激),训练频率为每周两三次。在使用血流限制进行训练时,还应该考虑所用袖带的宽度以及肢体围度,即宽袖带限制动脉血流的压力值比窄袖带低、较大的肢体需要更高的压力才能达到与较小肢体相同的限制性水平。另外,限制压力应针对每个肢体设定,以规范个性化BFRT运动处方。 2.4 BFRT在常见膝关节疾病康复中应用的安全性 与BFRT相关的不良事件很少发生,OHTA等[32]报道,在训练期间,2例患者因下肢不适或隐痛而脱落。KILGAS等[29]报道,运动训练后平均肌肉酸痛<1.0 cm。IVERSEN等[23]报告的横纹肌溶解症少于 1/10 000例(0.008%)。另有一些学者报道进行BFRT后,两组患者在训练期间均未出现下肢瘀斑、肿胀及局部压痛等并发症,彩超检查也未发现深静脉学血栓形成[24-26]。大部分研究报告无不良事件或没有报告血流限制的不良事件,目前有限的数据表明这种训练方式是安全的,不良反应很少见。专家建议,所有患者在临床应用前均应进行血流限制禁忌证筛查[50]。总体而言,在应用前对血流限制禁忌证进行筛查、并且强调个性化的血流限制运动处方以及在适当的医务监督下,BFRT的风险不会比其他抗阻训练大。"

| [1] MARCON M, CIRITSIS B, LAUX C, et al. Quantitative and qualitative MR-imaging assessment of vastus medialis muscle volume loss in asymptomatic patients after anterior cruciate ligament reconstruction. J Magn Reson Imaging. 2015;42(2): 515-525. [2] MARCON M, CIRITSIS B, LAUX C, et al. Cross-sectional area measurements versus volumetric assessment of the quadriceps femoris muscle in patients with anterior cruciate ligament reconstructions. Eur Radiol. 2015;25(2): 290-298. [3] DE JONG SN, VAN CASPEL DR, VAN HAEFF MJ, et al. Functional assessment and muscle strength before and after reconstruction of chronic anterior cruciate ligament lesions. Arthroscopy. 2007;23(1):21-28,28.e21-23. [4] PETTERSON SC, BARRANCE P, BUCHANAN T, et al. Mechanisms underlying quadriceps weakness in knee osteoarthritis. Med Sci Sports Exerc. 2008;40(3): 422-427. [5] PALMIERI-SMITH RM, THOMAS AC, KARVONEN-GUTIERREZ C, et al. Isometric quadriceps strength in women with mild, moderate, and severe knee osteoarthritis. Am J Phys Med Rehabil. 2010;89(7):541-548. [6] THOMAS AC, VILLWOCK M, WOJTYS EM, et al. Lower extremity muscle strength after anterior cruciate ligament injury and reconstruction. J Athl Train. 2013; 48(5):610-620. [7] PAPALIA R, ZAMPOGNA B, TORRE G, et al. Sarcopenia and its relationship with osteoarthritis: risk factor or direct consequence? Musculoskelet Surg. 2014; 98(1):9-14. [8] GARBER CE, BLISSMER B, DESCHENES MR, et al. American College of Sports Medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med Sci Sports Exerc. 2011;43(7):1334-1359. [9] SATO Y. The history and future of KAATSU Training. Int J Kaatsu Train Res. 2005; 1(1):1-5. [10] TEGTBUR U, HAUFE S, BUSSE MW. [Application and effects of blood flow restriction training]. Unfallchirurg. 2020;123(3):170-175. [11] FERRAZ RB, GUALANO B, RODRIGUES R, et al. Benefits of Resistance Training with Blood Flow Restriction in Knee Osteoarthritis. Med Sci Sports Exerc. 2018;50(5): 897-905. [12] BRYK FF, DOS REIS AC, FINGERHUT D, et al. Exercises with partial vascular occlusion in patients with knee osteoarthritis: a randomized clinical trial. Knee Surg Sports Traumatol Arthrosc. 2016;24(5):1580-1586. [13] GILES L, WEBSTER KE, MCCLELLAND J, et al. Quadriceps strengthening with and without blood flow restriction in the treatment of patellofemoral pain: a double-blind randomised trial. Br J Sports Med. 2017;51(23):1688-1694. [14] HUGHES L, ROSENBLATT B, HADDAD F, et al. Comparing the Effectiveness of Blood Flow Restriction and Traditional Heavy Load Resistance Training in the Post-Surgery Rehabilitation of Anterior Cruciate Ligament Reconstruction Patients: A UK National Health Service Randomised Controlled Trial. Sports Med. 2019;49(11):1787-1805. [15] HWANG PS, WILLOUGHBY DS. Mechanisms Behind Blood Flow-Restricted Training and its Effect Toward Muscle Growth. J Strength Cond Res. 2019;33 Suppl 1: S167-s179. [16] PEARSON SJ, HUSSAIN SR. A review on the mechanisms of blood-flow restriction resistance training-induced muscle hypertrophy. Sports Med. 2015;45(2):187-200. [17] HUGHES L, PATON B, ROSENBLATT B, et al. Blood flow restriction training in clinical musculoskeletal rehabilitation: a systematic review and meta-analysis. Br J Sports Med. 2017;51(13): 1003-1011. [18] MUSAHL V, KARLSSON J. Anterior Cruciate Ligament Tear. N Engl J Med. 2019; 380(24):2341-2348. [19] WEINREB JH, YOSHIDA R, COTE MP, et al. A Review of Databases Used in Orthopaedic Surgery Research and an Analysis of Database Use in Arthroscopy: The Journal of Arthroscopic and Related Surgery. Arthroscopy. 2017;33(1):225-231. [20] WILLIAMS GN, BUCHANAN TS, BARRANCE PJ, et al. Quadriceps weakness, atrophy, and activation failure in predicted noncopers after anterior cruciate ligament injury. Am J Sports Med. 2005;33(3):402-407. [21] GOETSCHIUS J, HART JM. Knee-Extension Torque Variability and Subjective Knee Function in Patients with a History of Anterior Cruciate Ligament Reconstruction. J Athl Train. 2016;51(1):22-27. [22] TAKARADA Y, TAKAZAWA H, ISHII N. Applications of vascular occlusion diminish disuse atrophy of knee extensor muscles. Med Sci Sports Exerc. 2000;32(12): 2035-2039. [23] IVERSEN E, RØSTAD V, LARMO A. Intermittent blood flow restriction does not reduce atrophy following anterior cruciate ligament reconstruction. J Sport Health Sci. 2016;5(1):115-118. [24] 张林玲, 王玉明, 赵燕燕, 等. 血流限制训练在膝关节微创手术早期康复中的应用[J]. 护理实践与研究,2020,17(16):87-89. [25] 刘莉, 李静, 赵冬梅, 等. 血流限制训练在膝关节镜术后患者康复训练中的应用[J]. 护理学杂志,2017,32(24): 82-84. [26] TENNENT DJ, HYLDEN CM, JOHNSON AE, et al. Blood Flow Restriction Training After Knee Arthroscopy: A Randomized Controlled Pilot Study. Clin J Sport Med. 2017;27(3):245-252. [27] HUGHES L, PATON B, HADDAD F, et al. Comparison of the acute perceptual and blood pressure response to heavy load and light load blood flow restriction resistance exercise in anterior cruciate ligament reconstruction patients and non-injured populations. Phys Ther Sport. 2018;33:54-61. [28] HUGHES L, PATTERSON S. D, HADDAD F, et al. Examination of the comfort and pain experienced with blood flow restriction training during post-surgery rehabilitation of anterior cruciate ligament reconstruction patients: A UK National Health Service trial. Phys Ther Sport. 2019;39:90-98. [29] KILGAS MA, LYTLE LLM, DRUM SN, et al. Exercise with Blood Flow Restriction to Improve Quadriceps Function Long After ACL Reconstruction. Int J Sports Med. 2019;40(10):650-656. [30] 孙学斌, 岐飞,曹力. 不同康复治疗方法对关节镜下前交叉韧带重建术后患者的短期疗效观察[J]. 新疆医学,2020,50(5):441-445. [31] 李奇, 李蕊, 罗昌禄, 等. 血流限制性运动对前交叉韧带重建术后膝关节功能的影响[J]. 广东医学,2019,40(10):1405-1408. [32] OHTA H, KUROSAWA H, IKEDA H, et al. Low-load resistance muscular training with moderate restriction of blood flow after anterior cruciate ligament reconstruction. Acta Orthop Scand. 2003;74(1):62-68. [33] CURRAN MT, BEDI A, MENDIAS CL, et al. Blood Flow Restriction Training Applied With High-Intensity Exercise Does Not Improve Quadriceps Muscle Function After Anterior Cruciate Ligament Reconstruction: A Randomized Controlled Trial. Am J Sports Med. 2020;48(4):825-837. [34] RODRIGUES R, FERRAZ RB, KURIMORI CO, et al. Low-Load Resistance Training With Blood-Flow Restriction in Relation to Muscle Function, Mass, and Functionality in Women With Rheumatoid Arthritis. Arthritis Care Res (Hoboken). 2020;72(6):787-797. [35] COLLINS NJ, BARTON CJ, VAN MIDDELKOOP M, et al. 2018 Consensus statement on exercise therapy and physical interventions (orthoses, taping and manual therapy) to treat patellofemoral pain: recommendations from the 5th International Patellofemoral Pain Research Retreat, Gold Coast, Australia, 2017. Br J Sports Med. 2018;52(18):1170-1178. [36] RATHLEFF MS, RATHLEFF CR, OLESEN JL, et al. Is Knee Pain During Adolescence a Self-limiting Condition? Prognosis of Patellofemoral Pain and Other Types of Knee Pain. Am J Sports Med. 2016;44(5):1165-1171. [37] HALL R, BARBER FOSS K, HEWETT TE, et al. Sport specialization’s association with an increased risk of developing anterior knee pain in adolescent female athletes. J Sport Rehabil. 2015;24(1):31-35. [38] CULVENOR AG, COOK JL, COLLINS NJ, et al. Is patellofemoral joint osteoarthritis an under-recognised outcome of anterior cruciate ligament reconstruction? A narrative literature review. Br J Sports Med. 2013;47(2):66-70. [39] KORAKAKIS V, WHITELEY R, GIAKAS G. Low load resistance training with blood flow restriction decreases anterior knee pain more than resistance training alone. A pilot randomised controlled trial. Phys Ther Sport. 2018;34:121-128. [40] FRANSEN M, MCCONNELL S, HARMER AR, et al. Exercise for osteoarthritis of the knee: a Cochrane systematic review. Br J Sports Med. 2015;49(24): 1554-1557. [41] CROSS M, SMITH E, HOY D, et al. The global burden of hip and knee osteoarthritis: estimates from the global burden of disease 2010 study. Ann Rheum Dis. 2014; 73(7):1323-1330. [42] KOLASINSKI SL, NEOGI T, HOCHBERG MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care Res (Hoboken). 2020;72(2):149-162. [43] SEGAL NA, WILLIAMS GN, DAVIS MC, et al. Efficacy of blood flow-restricted, low-load resistance training in women with risk factors for symptomatic knee osteoarthritis. PM R. 2015;7(4):376-384. [44] SEGAL N, DAVIS MD, MIKESKY AE. Efficacy of Blood Flow-Restricted Low-Load Resistance Training For Quadriceps Strengthening in Men at Risk of Symptomatic Knee Osteoarthritis. Geriatr Orthop Surg Rehabil. 2015;6(3):160-167. [45] HARPER SA, ROBERTS LM, LAYNE AS, et al. Blood-Flow Restriction Resistance Exercise for Older Adults with Knee Osteoarthritis: A Pilot Randomized Clinical Trial. J Clin Med. 2019;8(2):265. [46] LOENNEKE JP, FAHS CA, ROSSOW LM, et al. Effects of cuff width on arterial occlusion: implications for blood flow restricted exercise. Eur J Appl Physiol. 2012;112(8):2903-2912. [47] HEITKAMP HC. Training with blood flow restriction. Mechanisms, gain in strength and safety. J Sports Med Phys Fitness. 2015;55(5):446-456. [48] SINGH JA, SAAG KG, BRIDGES SL JR, et al. 2015 American College of Rheumatology Guideline for the Treatment of Rheumatoid Arthritis. Arthritis Care Res (Hoboken). 2016;68(1): 1-25. [49] SUL B, LEE KB, JOO YB, et al. Twelve Weeks of Strengthening Exercise for Patients with Rheumatoid Arthritis: A Prospective Intervention Study. J Clin Med. 2020; 9(9):2792. [50] DEPHILLIPO NN, KENNEDY MI, AMAN ZS, et al. The Role of Blood Flow Restriction Therapy Following Knee Surgery: Expert Opinion. Arthroscopy. 2018;34(8):2506-2510. [51] SCOTT BR, LOENNEKE JP, SLATTERY KM, et al. Exercise with blood flow restriction: an updated evidence-based approach for enhanced muscular development. Sports Med. 2015;45(3):313-325. [52] ŽARGI T, DROBNIČ M, STRAŽAR K, et al. Short-Term Preconditioning With Blood Flow Restricted Exercise Preserves Quadriceps Muscle Endurance in Patients After Anterior Cruciate Ligament Reconstruction. Front Physiol. 2018;9:1150. [53] GRAPAR ZARGI T, DROBNIC M, JKODER J, et al. The effects of preconditioning with ischemic exercise on quadriceps femoris muscle atrophy following anterior cruciate ligament reconstruction: a quasi-randomized controlled trial. Eur J Phys Rehabil Med. 2016;52(3):310-320. |
| [1] | Wang Jianping, Zhang Xiaohui, Yu Jinwei, Wei Shaoliang, Zhang Xinmin, Xu Xingxin, Qu Haijun. Application of knee joint motion analysis in machanism based on three-dimensional image registration and coordinate transformation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-5. |
| [2] | Gu Zhengqiu, Xu Fei, Wei Jia, Zou Yongdi, Wang Xiaolu, Li Yongming. Exploratory study on talk test as a measure of intensity in blood flow restriction training [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1154-1159. |
| [3] | Wu Bingshuang, Wang Zhi, Tang Yi, Tang Xiaoyu, Li Qi. Anterior cruciate ligament reconstruction: from enthesis to tendon-to-bone healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1293-1298. |
| [4] | Shao Yangyang, Zhang Junxia, Jiang Meijiao, Liu Zelong, Gao Kun, Yu Shuhan. Kinematics characteristics of lower limb joints of young men running wearing knee pads [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 832-837. |
| [5] | Zhou Jianguo, Liu Shiwei, Yuan Changhong, Bi Shengrong, Yang Guoping, Hu Weiquan, Liu Hui, Qian Rui. Total knee arthroplasty with posterior cruciate ligament retaining prosthesis in the treatment of knee osteoarthritis with knee valgus deformity [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 892-897. |
| [6] | Gao Cangjian, Yang Zhen, Liu Shuyun, Li Hao, Fu Liwei, Zhao Tianyuan, Chen Wei, Liao Zhiyao, Li Pinxue, Sui Xiang, Guo Quanyi. Electrospinning for rotator cuff repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 637-642. |
| [7] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Changes in kinematic parameters after unicompartmental knee arthroplasty and high tibial osteotomy [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 390-396. |
| [8] | Wu Yafei, Zhu Liang, Ren Qiujian, Li Daen, Li Dadi, Gao Xuren, Guo Kaijin. Relationship between glenoid version angle and degenerative rotator cuff full-thickness tear: matched case control trial [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 435-439. |
| [9] | Tu Youwei, Liu Yunpeng, Wang Xingliang, Peng Chao, Yang Jiaji . Effect of the match between the medial femoral condyle and tibial plateau on the tear of the posterior root of the medial meniscus evaluated by MRI [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(12): 1872-1876. |
| [10] | Wang Jianping, Zhang Xiaohui, Yu Jinwei, Wei Shaoliang, Zhang Xinmin, Xu Xingxin, Qu Haijun. Application of knee joint motion analysis in machanism based on three-dimensional image registration and coordinate transformation [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(12): 1922-1926. |
| [11] | Zhao Tianyu, Jin Song, Zhang Di, Liu Xiaoxiao, Ma Jiang, Wang Ju. Baduanjin training for patellar tendinopathy in a randomized controlled trial: improving pain, muscle flexibility and lower limb balance stability [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(11): 1662-1668. |
| [12] | Xu Renjie, Zhong Qiao, Liu Yubo, Yu Xiao, Yan Yongqing, Saijilafu, Yang Huilin, Chen Guangxiang. Quantitative analysis of transcriptome and proteome of knee joint synovial cells with osteopontin knockdown [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(11): 1680-1685. |
| [13] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [14] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [15] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||