Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (26): 4231-4236.doi: 10.3969/j.issn.2095-4344.2731
Previous Articles Next Articles
Recombinant human parathyroid hormone (1-34): pro-osteogenic action and application in oral field
Dong Xiling, Zhang Xiaoming, Liu Tongbin
Department of Prosthodontics, Binzhou Medical University Hospital, Binzhou 256600, Shandong Province, China
-
Received:2019-11-16Revised:2019-11-20Accepted:2020-01-02Online:2020-09-18Published:2020-09-03 -
Contact:Zhang Xiaoming, Master, Chief physician, Master’s supervisor, Department of Prosthodontics, Binzhou Medical University Hospital, Binzhou 256600, Shandong Province, China -
About author:Dong Xiling, Master candidate, Department of Prosthodontics, Binzhou Medical University Hospital, Binzhou 256600, Shandong Province, China -
Supported by:the Medical and Health Technological Development Plan of Shandong Province, No. 2016WS0121; the Science and Technology Program of Binzhou Medical University, No. BY2017KJ05
CLC Number:
Cite this article
Dong Xiling, Zhang Xiaoming, Liu Tongbin.
Recombinant human parathyroid hormone (1-34): pro-osteogenic action and application in oral field [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4231-4236.
share this article
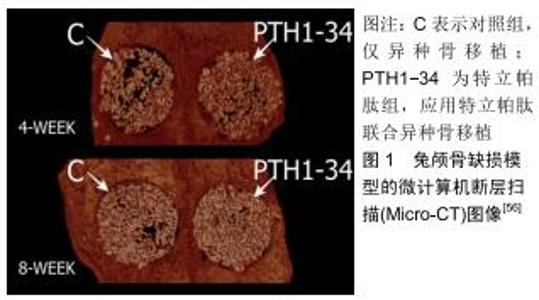
近年来,组织工程骨修复骨缺损成为专家学者们研究讨论的热点。VALDERRAMA等[55]以狗为实验动物,将特立帕肽与合成的聚乙二醇基水凝胶共价结合,并将其植入外科手术造成的缺损周围,其结果显示在仿生合成基质中递送甲状旁腺激素对牙科植入物周围的骨再生有积极作用。OZER等[56]在兔颅骨缺损模型的动物实验中应用异种移植物载体与特立帕肽局部给药相结合进行治疗,结果显示特立帕肽组的总骨量在第4周和第8周均显著高于对照组,见图1,2。间歇性全身施用特立帕肽对骨愈合具有积极作用,然而特立帕肽在动物模型中的局部少量连续用药显示了对骨愈合的积极作用,但是需要使用不同的动物模型以确定其有效性及最佳的剂量方案。尽管对特立帕肽的局部给药进行了一些研究,但将特立帕肽递送至缺损区域的载体系统尚未得到全面评估。在未来的研究中使用其他载体系统来递送特立帕肽,将有助于确定最适合特立帕肽局部给药的载体系统。 "
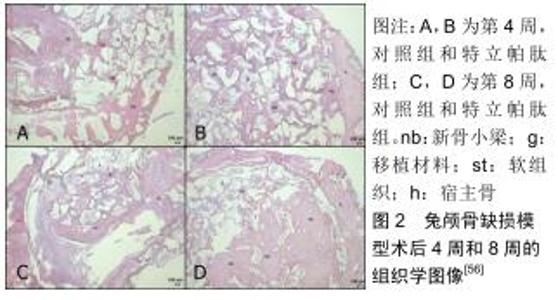
近年来,组织工程骨修复骨缺损成为专家学者们研究讨论的热点。VALDERRAMA等[55]以狗为实验动物,将特立帕肽与合成的聚乙二醇基水凝胶共价结合,并将其植入外科手术造成的缺损周围,其结果显示在仿生合成基质中递送甲状旁腺激素对牙科植入物周围的骨再生有积极作用。OZER等[56]在兔颅骨缺损模型的动物实验中应用异种移植物载体与特立帕肽局部给药相结合进行治疗,结果显示特立帕肽组的总骨量在第4周和第8周均显著高于对照组,见图1,2。间歇性全身施用特立帕肽对骨愈合具有积极作用,然而特立帕肽在动物模型中的局部少量连续用药显示了对骨愈合的积极作用,但是需要使用不同的动物模型以确定其有效性及最佳的剂量方案。尽管对特立帕肽的局部给药进行了一些研究,但将特立帕肽递送至缺损区域的载体系统尚未得到全面评估。在未来的研究中使用其他载体系统来递送特立帕肽,将有助于确定最适合特立帕肽局部给药的载体系统。 "
|
[1] 冯钰,刘福祥.骨质疏松症对颌骨的影响及其治疗的研究进展[J].国际口腔医学杂志,2008,35(S1):11-13.
[2] KANIS JA, COOPER C, RIZZOLI R, et al. Executive summary of the European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Calcif Tissue Int. 2019; 104(3):235-238.
[3] POLYZOS SA, MAKRAS P, EFSTATHIADOU Z, et al. Investigational parathyroid hormone receptor analogs for the treatment of osteoporosis. Expert Opin Investig Drugs. 2015; 24(2):145-157.
[4] BARON R, HESSE E. Update on bone anabolics in osteoporosis treatment: rationale, current status, and perspectives. J Clin Endocrinol Metab. 2012;97(2):311-325.
[5] BOGADO CE, MASSARI FE, ZANCHETTA JR. Parathyroid hormone (1-84) and teriparatide in the treatment of postmenopausal osteoporosis. Womens Health (Lond). 2006; 2(3):447-457.
[6] KEUTMANN HT, SAUER MM, HENDY GN, et al. Complete amino acid sequence of human parathyroid hormone. Biochemistry. 1978;17(26):5723-5729.
[7] LANGDAHL BL, ANDERSEN JD. Treatment of Osteoporosis: Unmet Needs and Emerging Solutions. J Bone Metab. 2018;25(3): 133-140.
[8] 王敏娇,司家文,沈国芳.促进骨形成的甲状旁腺激素:作用及机制[J].中国组织工程研究,2015,19(15):2405-2409.
[9] 陈茜,曹国颖.新型骨质疏松症治疗药abaloparatide的作用机制与临床评价[J].临床药物治疗杂志,2018,16(7):37-40.
[10] BELLIDO T, ALI AA, PLOTKIN LI, et al. Proteasomal degradation of Runx2 shortens parathyroid hormone-induced anti-apoptotic signaling in osteoblasts. A putative explanation for why intermittent administration is needed for bone anabolism. J Biol Chem. 2003;278(50):50259-50272.
[11] QIN L, LI X, KO JK, et al. Parathyroid hormone uses multiple mechanisms to arrest the cell cycle progression of osteoblastic cells from G1 to S phase. J Biol Chem. 2005;280(4):3104-3111.
[12] JILKA RL. Molecular and cellular mechanisms of the anabolic effect of intermittent PTH. Bone. 2007;40(6):1434-1446.
[13] WINKLER DG, SUTHERLAND MK, GEOGHEGAN JC, et al. Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J. 2003;22(23):6267-6276.
[14] KHOSLA S, WESTENDORF JJ, OURSLER MJ. Building bone to reverse osteoporosis and repair fractures. J Clin Invest. 2008; 118(2):421-428.
[15] BIKLE DD, SAKATA T, LEARY C, et al. Insulin-like growth factor I is required for the anabolic actions of parathyroid hormone on mouse bone. J Bone Miner Res. 2002;17(9):1570-1578.
[16] FOX J. Developments in parathyroid hormone and related peptides as bone-formation agents. Curr Opin Pharmacol. 2002;2(3):338-344.
[17] NEER RM, ARNAUD CD, ZANCHETTA JR, et al. Effect of parathyroid hormone (1-34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N Engl J Med. 2001;344(19):1434-1441.
[18] YOO JI, HA YC, RYU HJ, et al. Teriparatide Treatment in Elderly Patients With Sacral Insufficiency Fracture. J Clin Endocrinol Metab. 2017;102(2):560-565.
[19] KITAGUCHI K, KASHII M, EBINA K, et al. Effects of Weekly Teriparatide Administration for Vertebral Stability and Bony Union in Patients with Acute Osteoporotic Vertebral Fractures. Asian Spine J. 2019;13(5):763-771.
[20] CHEN Q, GUO M, MA X, et al. Adherence to Teriparatide Treatment and Risk of Fracture: A Systematic Review and Meta-Analysis. Horm Metab Res. 2019;51(12):785-791.
[21] 徐陆晨,李运峰.骨质疏松性骨折药物治疗的研究进展[J].中国骨质疏松杂志,2017,23(7):947-953.
[22] ANDREWS EB, GILSENAN A, MIDKIFF K, et al. Challenges in studying very rare cancer outcomes and infrequent exposures: example of teriparatide and osteosarcoma. Ann Epidemiol. 2016;26(11):751-753.
[23] DRAKE MT, SRINIVASAN B, MÖDDER UI, et al. Effects of intermittent parathyroid hormone treatment on osteoprogenitor cells in postmenopausal women. Bone. 2011;49(3):349-355.
[24] GREY A. Teriparatide for bone loss in the jaw. N Engl J Med. 2010;363(25):2458-2459.
[25] PAZIANAS M. Anabolic effects of PTH and the 'anabolic window'. Trends Endocrinol Metab. 2015;26(3):111-113.
[26] NAKAMURA T, SUGIMOTO T, NAKANO T, et al. Randomized Teriparatide [human parathyroid hormone (PTH) 1-34] Once-Weekly Efficacy Research (TOWER) trial for examining the reduction in new vertebral fractures in subjects with primary osteoporosis and high fracture risk. J Clin Endocrinol Metab. 2012;97(9):3097-3106.
[27] USUI T, FUNAGOSHI M, SETO K, et al. Persistence of and switches from teriparatide treatment among women and men with osteoporosis in the real world: a claims database analysis. Arch Osteoporos. 2018;13(1):54.
[28] KUMAGAI Y, OSE A, TANAKA K, et al. Safety Profiles, Pharmacokinetics, and Changes in Bone Turnover Markers After Twice-Weekly Subcutaneous Administration of Teriparatide in Healthy Japanese Postmenopausal Women: A Single-Blind Randomized Study. Clin Pharmacol Drug Dev. 2020;9(1):87-96.
[29] COSMAN F, LANE NE, BOLOGNESE MA, et al. Effect of transdermal teriparatide administration on bone mineral density in postmenopausal women. J Clin Endocrinol Metab. 2010;95(1): 151-158.
[30] HÄMMERLE SP, MINDEHOLM L, LAUNONEN A, et al. The single dose pharmacokinetic profile of a novel oral human parathyroid hormone formulation in healthy postmenopausal women. Bone. 2012;50(4):965-973.
[31] PEARSON RG, MASUD T, BLACKSHAW E, et al. Nasal Administration and Plasma Pharmacokinetics of Parathyroid Hormone Peptide PTH 1-34 for the Treatment of Osteoporosis. Pharmaceutics. 2019;11(6): E265.
[32] GUAÑABENS N, MORO-ÁLVAREZ MJ, CASADO E, et al. The next step after anti-osteoporotic drug discontinuation: an up-to-date review of sequential treatment. Endocrine. 2019;64(3): 441-455.
[33] VOHRA F, AL-RIFAIY MQ, ALMAS K, et al. Efficacy of systemic bisphosphonate delivery on osseointegration of implants under osteoporotic conditions: lessons from animal studies. Arch Oral Biol. 2014;59(9):912-920.
[34] BEPPU K, KIDO H, WATAZU A, et al. Peri-implant bone density in senile osteoporosis-changes from implant placement to osseointegration. Clin Implant Dent Relat Res. 2013;15(2): 217-226.
[35] DARCEY J, HORNER K, WALSH T, et al. Tooth loss and osteoporosis: to assess the association between osteoporosis status and tooth number. Br Dent J. 2013;214(4):E10.
[36] ANIL S, PREETHANATH RS, ALMOHARIB HS, et al. Impact of osteoporosis and its treatment on oral health. Am J Med Sci. 2013;346(5):396-401.
[37] SHIROTA T, TASHIRO M, OHNO K, et al. Effect of intermittent parathyroid hormone (1-34) treatment on the bone response after placement of titanium implants into the tibia of ovariectomized rats. J Oral Maxillofac Surg. 2003;61(4):471-480.
[38] ALMAGRO MI, ROMAN-BLAS JA, BELLIDO M, et al. PTH [1-34] enhances bone response around titanium implants in a rabbit model of osteoporosis. Clin Oral Implants Res. 2013;24(9): 1027-1034.
[39] JIANG L, ZHANG W, WEI L, et al. Early effects of parathyroid hormone on vascularized bone regeneration and implant osseointegration in aged rats. Biomaterials. 2018;179:15-28.
[40] KUCHLER U, LUVIZUTO ER, TANGL S, et al. Short-term teriparatide delivery and osseointegration: a clinical feasibility study. J Dent Res. 2011;90(8):1001-1006.
[41] KRAUS D, JÄGER A, ABUDUWALI N, et al. Intermittent PTH(1-34) signals through protein kinase A to regulate osteoprotegerin production in human periodontal ligament cells in vitro. Clin Oral Investig. 2012;16(2):611-618. [42] AUSENDA F, RASPERINI G, ACUNZO R, et al. New Perspectives in the Use of Biomaterials for Periodontal Regeneration. Materials (Basel). 2019;12(13): E2197.
[43] VASCONCELOS DF, MARQUES MR, BENATTI BB, et al. Intermittent parathyroid hormone administration improves periodontal healing in rats. J Periodontol. 2014;85(5):721-728.
[44] SILVA MA, VASCONCELOS DF, MARQUES MR, et al. Parathyroid hormone intermittent administration promotes delay on rat incisor eruption. Arch Oral Biol. 2016;69:102-108.
[45] DE OLIVEIRA PUTTINI I, GOMES-FERREIRA PHDS, DE OLIVEIRA D, et al. Teriparatide improves alveolar bone modelling after tooth extraction in orchiectomized rats. Arch Oral Biol. 2019; 102:147-154.
[46] BASHUTSKI JD, EBER RM, KINNEY JS, et al. Teriparatide and osseous regeneration in the oral cavity. N Engl J Med. 2010; 363(25):2396-2405.
[47] LI F, LI G, HU H, et al. Effect of parathyroid hormone on experimental tooth movement in rats. Am J Orthod Dentofacial Orthop. 2013;144(4):523-532.
[48] LOSSDÖRFER S, YILDIZ F, GÖTZ W, et al. Anabolic effect of intermittent PTH(1-34) on the local microenvironment during the late phase of periodontal repair in a rat model of tooth root resorption. Clin Oral Investig. 2010;14(1):89-98.
[49] ZANDI M, DEHGHAN A, GHEYSARI F, et al. Evaluation of teriparatide effect on healing of autografted mandibular defects in rats. J Craniomaxillofac Surg. 2019;47(1):120-126.
[50] ZANDI M, DEHGHAN A, AMINI P, et al. Evaluation of the effect of teriparatide therapy on mandibular fracture healing in rats with medication-related osteonecrosis of the jaw. Clin Oral Investig. 2019;23(11):3987-3993.
[51] KAKEHASHI H, ANDO T, MINAMIZATO T, et al. Administration of teriparatide improves the symptoms of advanced bisphosphonate-related osteonecrosis of the jaw: preliminary findings. Int J Oral Maxillofac Surg. 2015;44(12):1558-1564.
[52] KIM JY, PARK JH, JUNG HD, et al. Treatment of Medication-Related Osteonecrosis of the Jaw Around the Dental Implant With a Once-Weekly Teriparatide: A Case Report and Literature Review. J Oral Implantol. 2019;45(5):403-407.
[53] JUNG J, YOO HY, KIM GT, et al. Short-Term Teriparatide and Recombinant Human Bone Morphogenetic Protein-2 for Regenerative Approach to Medication-Related Osteonecrosis of the Jaw: A Preliminary Study. J Bone Miner Res. 2017;32(12): 2445-2452.
[54] CHA YH, HONG N, RHEE Y, et al. Teriparatide therapy for severe, refractory osteoradionecrosis of the jaw. Osteoporos Int. 2018; 29(4):987-992.
[55] VALDERRAMA P, JUNG RE, THOMA DS, et al. Evaluation of parathyroid hormone bound to a synthetic matrix for guided bone regeneration around dental implants: a histomorphometric study in dogs. J Periodontol. 2010;81(5):737-747. [56]ÖZER T, BAŞLARLI Ö, AKTAŞ A, et al. Locally administrated single-dose teriparatide affects critical-size rabbit calvarial defects: A histological, histomorphometric and micro-CT study. Acta Orthop Traumatol Turc. 2019;53(6):478-484. |
| [1] | Tang Hui, Yao Zhihao, Luo Daowen, Peng Shuanglin, Yang Shuanglin, Wang Lang, Xiao Jingang. High fat and high sugar diet combined with streptozotocin to establish a rat model of type 2 diabetic osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1207-1211. |
| [2] | Li Zhongfeng, Chen Minghai, Fan Yinuo, Wei Qiushi, He Wei, Chen Zhenqiu. Mechanism of Yougui Yin for steroid-induced femoral head necrosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1256-1263. |
| [3] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [4] | Li Shibin, Lai Yu, Zhou Yi, Liao Jianzhao, Zhang Xiaoyun, Zhang Xuan. Pathogenesis of hormonal osteonecrosis of the femoral head and the target effect of related signaling pathways [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 935-941. |
| [5] | Xiao Fangjun, Chen Shudong, Luan Jiyao, Hou Yu, He Kun, Lin Dingkun. An insight into the mechanism of Salvia miltiorrhiza intervention on osteoporosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 772-778. |
| [6] | Liu Bo, Chen Xianghe, Yang Kang, Yu Huilin, Lu Pengcheng. Mechanism of DNA methylation in exercise intervention for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 791-797. |
| [7] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [8] | Nie Shaobo, Li Jiantao, Sun Jien, Zhao Zhe, Zhao Yanpeng, Zhang Licheng, Tang Peifu. Mechanical stability of medial support nail in treatment of severe osteoporotic intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 329-333. |
| [9] | Yang Junhui, Luo Jinli, Yuan Xiaoping. Effects of human growth hormone on proliferation and osteogenic differentiation of human periodontal ligament stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3956-3961. |
| [10] | Zhu Yun, Chen Yu, Qiu Hao, Liu Dun, Jin Guorong, Chen Shimou, Weng Zheng. Finite element analysis for treatment of osteoporotic femoral fracture with far cortical locking screw [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3832-3837. |
| [11] | Yang Caihui, Liu Qicheng, Dong Ming, Wang Lina, Zuo Meina, Lu Ying, Niu Weidong. Serine/threonine protein kinases can promote bone destruction in mouse models of chronic periapical periodontitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3654-3659. |
| [12] | Feng Guancheng, Fang Jianming, Lü Haoran, Zhang Dongsheng, Wei Jiadong, Yu Bingbing. How does bone cement dispersion affect the early outcome of percutaneous vertebroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3450-3457. |
| [13] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [14] | Cai Qunbin, Yang Lijuan, Li Qiumin, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei . Feasibility of internal fixation removal of intertrochanteric fractures in elderly patients based on fracture mechanics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3313-3318. |
| [15] | Liu Yulin, Li Guotai. Combined effects of hyperbaric oxygen, vibration training and astaxanthin on bone mineral density, glucose metabolism and oxidative stress in diabetic osteoporosis rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3117-3124. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||