Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (3): 449-455.doi: 10.3969/j.issn.2095-4344.2937
Previous Articles Next Articles
Hot issues in clinical application of dynamic contrast-enhanced magnetic resonance imaging in orthopedics
Yu Langbo, Qing Mingsong, Zhao Chuntao, Peng Jiachen
- Zunyi Medical University-Orthopedic Research Center of University of Rochester, Department of Orthopedics, Affiliated Hospital of Zunyi Medical University, Zunyi 563000, Guizhou Province, China
-
Received:2020-03-19Revised:2020-03-24Accepted:2020-05-09Online:2021-01-28Published:2020-11-19 -
Contact:Peng Jiachen, MD, Professor, Chief physician, Zunyi Medical University-Orthopedic Research Center of University of Rochester, Department of Orthopedics, Affiliated Hospital of Zunyi Medical University, Zunyi 563000, Guizhou Province, China -
About author:Yu Langbo, Master candidate, Physician, Zunyi Medical University-Orthopedic Research Center of University of Rochester, Department of Orthopedics, Affiliated Hospital of Zunyi Medical University, Zunyi 563000, Guizhou Province, China
CLC Number:
Cite this article
Yu Langbo, Qing Mingsong, Zhao Chuntao, Peng Jiachen. Hot issues in clinical application of dynamic contrast-enhanced magnetic resonance imaging in orthopedics[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 449-455.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
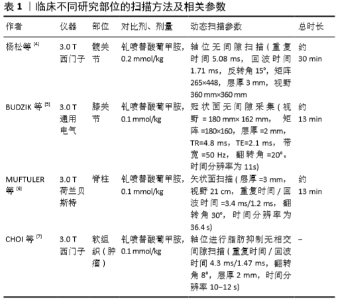
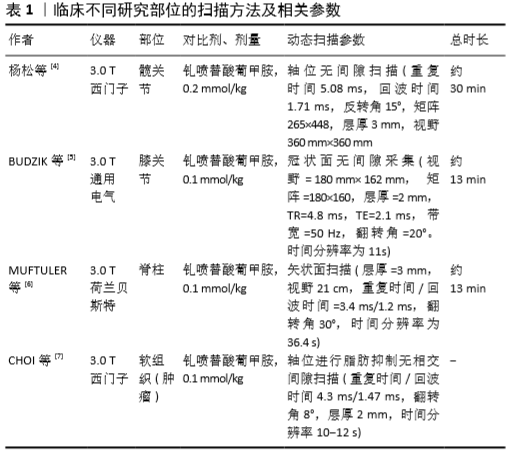
2.1 动态对比增强MRI扫描方法现状及要求 目前,在肌肉骨骼系统中对于获取动态对比增强MRI图像的最佳扫描方法和分析这种图像的理想方法普遍缺乏共识,这主要是因为不同部位的扫描条件存在差异,因此在不同的组织或器官进行检查时所采用的方法也存在差异。文章例举了临床不同研究的扫描方法及相关参数,具体详见表1。目前动态对比增强MRI在骨科的应用中主要两种序列方法:磁共振血管造影,其专注于感兴趣区域的血液动力学,具有较低的解剖分辨率;快速梯度回波采集序列,使用此序列可以具有较高解剖分辨率和较低时间分辨率[2]。此外,就动态对比增强MRI的硬件要求而言,1.5 T或3 T扫描仪的磁强度均可应用于临床。但首要条件是这些磁体需要基于先进梯度或平面回波成像的并行成像序列、合适的相控阵线圈和电源注入器,且并行成像可通过使用相控阵线圈(具有多个元件的表面线圈)对k空间进行部分采集来减少扫描时间,并且无需提高性能即可执行数据重建[3]。"
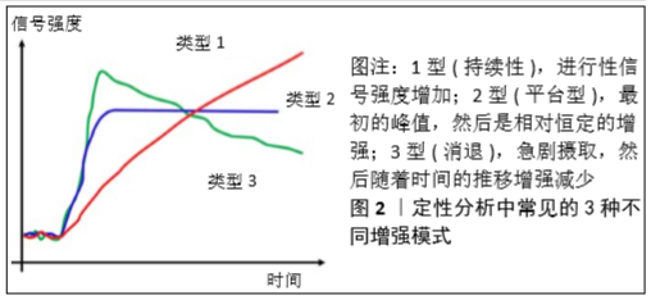
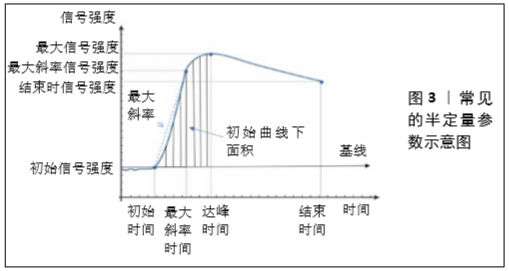
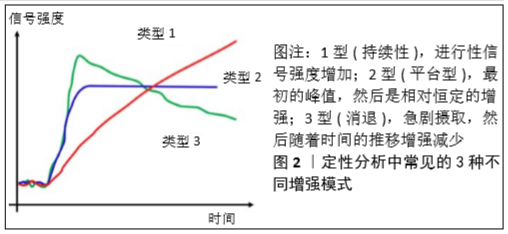
2.2 动态对比增强MRI的分析方法 动态对比增强MRI的灌注参数主要有3种分析方法:定性、半定量和定量分析[8]。定性方法是时间强度曲线的形态学分析,其依赖于目测评估感兴趣区域内是否存在早期动脉增强(而不是后期增强),这是临床上最常用、最直观的分析方法,简单来说就是观察时间强度曲线的形态区别[9],见图2。而半定量的方法是通过从时间强度曲线中计算几个参数,常用的半定量参数有初始曲线下面积、达峰时间、最大信号强度、最大斜率等,见图3。最后,定量分析主要通过药代动力学模型进行,获得可以反映血流灌注和血管通透性的常用参数:容量转移常数、速率常数、血管外、细胞外间隙容积分数、血浆体积等[10]。最早的药代动力学分析模型是由血浆和血管外细胞外空间组成的间隔模型。在该模型中,假设对比剂以可逆过程扩散到血管外细胞外空间中,该可逆过程的特征在于容量转移常数和速率常数,容量转移常数是对比剂流入血浆和血管外细胞外空间的速率,受血浆血流量和组织的渗透性的控制,这些指标可发现肌肉骨骼肿瘤的血管分布,这对确定肿瘤的生存能力和评估新辅助治疗后的治疗效果非常重要。此外,科研人员又提出了许多药代动力学模型,如Larsson(LM)、Brix(BM)、Tofts and Kermode(TK)、extended TK(ETK)等[10-11],并且这些模型随着技术的进步不断的在演变和发展。"

2.3 动态对比增强MRI在骨科临床中的应用进展 2.3.1 在骨骼肌肉肿瘤系统中的应用 几十年来,常规的平扫+增强MRI检查一直用来帮助鉴别骨骼肌肉肿瘤或病变的良恶性,然而这种模式在许多类型的组织中都可以看到强化,如良、恶性实体也均表现为强化,因此在临床工作中可能会产生误诊或漏诊。目前,动态对比增强MRI已被认为是一种帮助鉴别良恶性病变的方法[12],因为动态增强的时间模式包含重要信息,包括灌注参数、组织血管通透性和间质间隙的体积,且容量转移常数反映的是组织内毛细血管通透性及血浆流量共同作用的结果,容量转移常数值越高则表示组织的血浆流量和组织血管渗透性越高,对于肿瘤而言其容量转移常数值越高表明其代谢越快,其恶性程度也可能越高[13],因此动态对比增强MRI被认为可以显示恶性骨骼肌肉肿瘤的特征性。一项研究通过动态对比增强MRI来鉴别脊索瘤和骨巨细胞瘤,发现骨巨细胞瘤容量转移常数和速率常数值明显高于脊索瘤[14]。他们假设骨巨细胞瘤显微镜下观察到的高微血管密度、不规则管腔、薄壁管腔和一些管壁中内皮细胞的缺失可能表明肿瘤有渗漏的血管,提示与容量转移常数和速率常数值的升高有关。DE CONINCK等[15]在研究动态对比增强MRI和常规MRI在内生软骨瘤和软骨肉瘤中的价值中显示,动态对比增强MRI对软骨肉瘤的诊断敏感性为100%,特异性为63.3%,且预测软骨肉瘤的准确率为93%,两者联合应用可以获得最高的准确性。此外,当动态对比增强MRI清楚地显示没有早期增强的迹象,而轻度延迟增强则可能对应于良性病变。通过这样的原理可区别恶性肿瘤与脂肪瘤伴脂肪坏死、朗格汉斯细胞增生症与恶性病变(例如尤因肉瘤)等[16]。而在高级软组织肉瘤中,动态对比增强MRI被证明可以提高MRI成像在确定患者治疗反应中的准确性[17],在这些患者中肿瘤的生长是形成瘢痕和肉芽组织而不是坏死[18]。CHOI等[7]的研究表明,动态对比增强MRI相关参数显示肿瘤的大小、边缘、神经血管受累情况、瘤体周围水肿和不均一性之间的关系,可以明显区分良、恶性病变。 动态对比增强MRI不仅可提高骨骼肌肉肿瘤的诊断率,还可作为术后疗效的评估工具,其有助于评估骨和软组织恶性肿瘤在术前和新辅助化疗或放疗后的治疗效果及存活残留恶性肿瘤的程度[19]。AMIT等[20]对比了临床指标和动态对比增强MRI在评估骨肉瘤新辅助化疗后组织学反应方面的作用,证明斜率降低>60%是良好组织学反应的指标,且可以更准确地判断组织的失活程度。它的意义在于指导、决定是否需要改变化疗方案及时间,选择最佳手术时机,甚至确定手术切除的范围。除此之外,在良性病变中的探索,POTTECHER等[21]发现骨样骨瘤疼痛的严重程度与其血管化的丰富程度有关。而对于定量参数与半定量参数的区别,LEPLAT等[22]的研究认为动态对比增强MRI对良恶性分化的敏感性较高,特异性较差,与半定量参数相似。综上,动态对比增强MRI所呈现的独特优势将有助于临床医师对良恶性肿瘤鉴别诊断、疾病变化评估及治疗的掌控。 2.3.2 在创伤骨科中的应用 动态对比增强MRI可作为临床上研究股骨颈骨折后股骨头血运灌注水平的一种工具。动态对比增强MRI相关参数可显示有关局部动脉和静脉灌注不足的客观信息,这些信息可能有利于更准确地评估股骨头的存活能力,使手术预后的结果预测更加准确,帮助骨科医师前瞻性地为患者选择特定的治疗方案。DYKE JONATHAN等[23]的研究认为患侧股骨头的动脉流入和静脉流出区域灌注降低是显著的,并且可以量化,这也与JONG-EUN等[24]的动物实验结果相一致。KAMANO等[25]对29例股骨颈骨折患者伤后24 h内行动态对比增强MRI检查,股骨头灌注完全增强者预后良好。KONISHIIKE[26]对22个股骨颈骨折进行了类似的评估,并报告在那些股骨头灌注没有增强的患者中,随后发生股骨头坏死的风险很高,其动态对比增强MRI风险预测的准确率为89%;当灌注减少70%时,他们可以检测到股骨头部分的骨坏死。还有研究表明,股骨头外侧柱早期灌注水平良好提示血运开始重建,预后较好;另一方面,缺乏灌注的外侧柱坏死预示着不良的预后。病变股骨头的再血管化部分比正常髋部有更高的强化,可能与血管扩张、通透性增加有关,这些血运重建区也与正常髋部相比表现出延迟增强[27]。最新的一项研究表明,动态对比增强MRI是一种简单、无创、易推广方法,并可以比较准确地判断股骨颈骨折后股骨头血运情况,若与术中股骨头钻孔术联合评估可以获得更准确的结果[28]。 股骨颈骨折复位内固定常伴随着较高的并发症(骨不愈合、股骨头坏死和晚期塌陷)发生,因此再次手术的概率也增加[29]。虽然创伤性骨折和与之相关的股骨头微细血液供应受损被认为是这些并发症的主要病因之一,然而LAZARO等[30]的研究认为虽然股骨颈骨折后损害了股骨头血流供应血管,影响流入和流出系统,导致股骨头细胞死亡和节段性损伤,但是假如能够早期评估股骨头血流微循环的灌注,再加上紧急的切开解剖复位和稳定的固定,尽管在动态对比增强MRI成像上发现了很高的小节段骨坏死,仍可有很好的临床疗效。此外他们还报道,当血管受损和残余灌注减少超过67%将导致股骨头坏死[30]。所以,如何利用动态对比增强MRI检测股骨头血运微循环及灌注变化,值得更加深入的研究,希望能够更加准确地为骨科医师治疗股骨颈骨折指导方向。 骨不连发生占所有骨折的5%-15%,这取决于骨折的部位、软组织损伤程度和感染的严重性[31],以前的重点集中于临床分类不愈合严重程度评分上,以使其治疗标准化。而目前动态对比增强MRI在评价骨灌注和骨不连手术成功方面的重要性越来越明显。一项初步的研究证明,动态对比增强MRI在评估骨折不愈合方面是可行的[32],主要原理是通过评估骨不连裂隙内的血管灌注情况进行分析。FISCHER等[33]利用动态对比增强MRI检测骨折术后骨不连的区域灌注,与骨折术后成功恢复的病例相比,结果显示在随访6,12,26周时成功恢复的病例检测区域显示明显更高的灌注。 骨不连的重要影响因素是感染。WESTGEEST等[34]的研究发现,在791个长骨开放性骨折中17%的病例发生了骨不连,发现深部感染是最关键的因素。对于感染的病例,手术必须分多次应用,并延迟进行骨折内固定手术,此外对于感染确诊的金标准是病理活检,但这需要术中切除标本后才能诊断。CHRISTIAN等[35]一项早期研究表明,动态对比增强MRI的高灌注有助于发现感染。随后他们的研究发现,动态对比增强MRI预测骨不连的敏感性为75%,特异性为87%,且较高的体质量指数和较低NUSS评分与治疗失败相关。然而,目前动态对比增强MRI只能为诊断提供辅助信息,术前感染评估中还应该结合超声联合诊断。最后,骨不连的患者应早期进行动态对比增强MRI分析,如果骨不连区域灌注低,缺乏骨质巩固和持续性疼痛的迹象,应考虑早期手术。希望这种早期评估与干预可以缩短整个治疗期,使患者更快地重返工作和社会生活。 此外,NG等[36]报道在舟状骨骨不连或延迟愈合的情况下,动态对比增强MRI在评估近端骨块中的血运方面提供了更高的准确性。然而,DONATI等[37]、LARRIBE等[38]的研究表明,动态对比增强MRI没有提供任何额外的信息来帮助评估舟状骨的生存能力。据DONATI等报道,动态对比增强MRI对近端骨坏死的评估能力实际上比常规MRI差,这可能与他们之间设备及扫描方法不同有关,不同的硬件设施可能会影响最终的效果。 2.3.3 在关节外科中的应用进展 炎症在骨性关节炎发病机制中的作用正引起人们的广泛关注,其机制可能和软骨下骨髓血管化密切相关。有研究表明,动态对比增强MRI可以识别动物骨关节炎软骨下骨髓血管化的改变[39],这些改变出现在软骨损伤可见之前,并且与骨关节炎的严重程度相关,因此在非侵入性条件下获得对人类骨关节炎软骨下骨髓血管化客观评估的机会,可能有助于更好地理解骨关节炎的病理生理学。在评估早期关节炎患者时,通常不会为了常规的临床目的而评估骨灌注,然而,软骨下骨灌注在软骨丢失的发展过程中是一个潜在的重要参数。正如所上述所说,LEE等[40]在动物模型中通过动态对比增强MRI评估发现,软骨下灌注的减少与关节软骨损伤的后续发展呈正相关。BUDZIK等[5]对19例晚期膝关节骨性关节炎患者进行了膝关节检查,用动态对比增强MRI评估股骨胫骨内侧和外侧室的软骨下骨髓血管化,并在MRI图像上对骨关节炎病变进行分级,最后结论是动态对比增强MRI评估的软骨下骨髓血管化改变与人类骨关节炎的严重程度相关,与上述实验结论一致。此外,NUSMAN等[41]的前瞻性临床随访研究表明,对动态对比增强MRI最大强化的评估能够预测静止期幼年特发性关节炎出现临床症状,从而可指导临床医师对于其静止期的治疗与评估。 滑膜炎是滑膜的炎症,可以在不同的疾病过程中发生,包括骨关节炎和炎性关节炎(如类风湿性关节炎)[42]。动态对比增强MRI在骨关节炎和炎性关节炎中可观察到滑膜炎的存在,这可能是关节炎发病的潜在重要因素,因为滑膜炎可能会导致关节疼痛加重,潜在的加重骨关节炎病变,并可能导致膝关节置换的风险。一些研究已经评估了动态对比增强MRI在滑膜炎中的效用,并得出结论:动态对比增强MRI的发现可用于提示骨关节炎和炎性关节炎中存在组织学滑膜炎[43-44]。RIIS等[43]对比了膝关节骨关节炎患者的动态对比增强MRI和常规MRI成像结果,显示动态对比增强MRI可检测出此类患者的疼痛程度与滑膜炎严重程度相关。此外,VORDENBAUMEN等[45]的另一项研究表明在类风湿性关节炎患者中,动态对比增强MRI参数与滑膜炎相关,特别是最大增强程度。动态对比增强MRI还被证明可以评估髌下脂肪垫的炎症程度,这与膝关节骨性关节炎患者疼痛的严重程度有关[46]。 2.3.4 在脊柱外科中的应用进展 因为动态对比增强MRI在评估组织微循环功能方面所展现的独特优势,部分研究在腰椎灌注定量分析中有了新的发现,如在早期的研究中显示与上腰椎相比,下腰椎骨密度较高,而血液灌注较低[47]。而MA等[48]的研究也证实了之前的结论,其认为椎骨水平与骨密度的相关性不如与灌注参数的相关性显著。此外,MUFTULER等[6]利用动态对比增强MRI成像研究了椎间盘退变与终板灌注的关系,最后的结论是:退变椎间盘软骨终板的灌注信号增强可能表明椎体软骨下骨受损。终板灌注信号增强特征有助于了解椎间盘退变的病理生理学,并更有效地计划治疗,这也与之前的研究结果相一致[49],显示了脊柱水平和椎间盘退变的相关性。此研究还首次报道,在软骨终板中下盘往往表现出增强的差异;下腰椎间盘上增加的机械压力可能是一个因素,损害了这些终板的完整性。 脊柱占所有肿瘤骨转移的70%,是癌症转移的第三常见部位,仅次于肺和肝脏。所有癌症患者中有5%-10%发生脊柱转移,通常导致较高的发病率和死亡率[50]。非侵入性动态对比增强MRI可提供血管微环境和血流动力学的变化,也因此展开了探讨。有研究表明,动态对比增强MRI定量参数在鉴别与常规MRI形态学表现相似的肿瘤时更有价值,如骨髓瘤和脊柱转移瘤。KUMAR等[51]对30例脊柱转移瘤患者在放疗前后测量了瘤体容量转移常数、速率常数和血浆体积等参数,比较治疗前后参数值的百分比变化,最后证明脊柱骨转移瘤放疗后灌注参数的变化是肿瘤局部复发的预测因素,尤其是血浆体积值。有研究发现,骨髓瘤的容量转移常数和速率常数值明显高于脊柱转移瘤,并且作者认为高密度细胞限制了对比剂在血管外细胞外间隙的分布,使其迅速回到血管进行清除[52]。此外,在19个接受放疗后脊柱转移瘤的动态对比增强MRI检测中,STACY等[53]报道了血浆体积的变化能强烈预测治疗效果,所有成功治疗的病例均显示血浆体积降低,且治疗失败的病变均显示血浆体积显着增加。SPRATT等[54]报道灌注参数变化(容量转移常数,血浆体积)的组合在预测预后方面的准确度比传统检查高1倍,动态对比增强MRI灌注参数不仅可以用于评估治疗效果,而且还可以预测将来局部肿瘤的复发。 2.3.5 其他 动态对比增强MRI还可用于检查畸形的血管,并将血管畸形分为高流量畸形和低流量畸形,因为动态成像可以更明确地评估流入和流出血管的血流动力学特征[55]。此外,动态对比增强MRI可以显示肌肉骨骼异常与邻近血管结构的关系,以及与骨骼肌肉相关的血管疾病,如血管卡压综合征、未确诊的假性动脉瘤和活动性出血等。 腘动脉卡压综合征是指腘动脉受到邻近肌肉和(或)肌腱的压迫而产生的综合征,常继发于肥大但解剖正常的邻近肌肉,且常见于较年轻的患者,表现为间歇性跛行。由于发病年龄较小,且缺乏心血管危险因素,该病的诊断往往延误。动态对比增强MRI能充分显示腘动脉及周围的结构,这在临床上很重要,因为如果不寻找外源性压迫的原因,腘动脉卡压综合征通常在血管介入治疗后复发;利用动态序列可以在不同的位置评估腘动脉灌注,以确定各个部位的血管闭塞情况,有利于制定最佳治疗方案[56]。当临床医师在四肢遇到不确定性“肿块”的假性动脉瘤时,动态对比增强MRI动态序列能够可视化“动脉充盈”到假性动脉瘤中,由此将假性动脉瘤与骨骼肌肉肿瘤区分开来[57]。此外,动态对比增强MRI动态图像还可以更好地描绘活动性出血的程度和出血来源,以及与周围结构的关系[58],这为临床医师提供了重要的信息。"

| [1] BRUNO F, ARRIGONI F, PALUMBO P, et al. New advances in MRI diagnosis of degenerative osteoarthropathy of the peripheral joints.Radiol Med.2019;124(11):1121-1127. [2] FAYAD LM, MUGERA C, SOLDATOS T, et al.T echnical innovation in dynamic contrast-enhanced magnetic resonance imaging of musculoskeletal tumors:an MR angiographic sequence using a sparse k-space sampling strategy.Skeletal Radiol.2013;42(7):993-1000. [3] PRUESSMANN KP, WEIGER M, SCHEIDEGGER MB, et al. SENSE: sensitivity encoding for fast MRI.Magn Reson Med.1999;42(5):952-62. [4] 杨松,郭爽,马彦明,等.动态对比增强磁共振成像对正常成人股骨头不同区域的血供评价[J].实用放射学杂志,2019,35(11): 1805-1808,1816. [5] Budzik JF, Ding J, Norberciak L, et al. Perfusion of subchondral bone marrow in knee osteoarthritis:A dynamic contrast-enhanced magnetic resonance imaging preliminary study.Eur J Radiol.2017;88:129-134. [6] MUFTULER LT, JARMAN JP, YU HJ, et al. Association between intervertebral disc degeneration and endplate perfusion studied by DCE-MRI.Eur Spine J.2015;24(4):679-685. [7] CHOI YJ, LEE IS, SONG YS, et al. Diagnostic performance of diffusion-weighted (DWI) and dynamic contrast-enhanced (DCE) MRI for the differentiation of benign from malignant soft-tissue tumors.J Magn Reson Imaging.2019;50(3):798-809. [8] HAFEZI-NEJAD N, DEMEHRI S, GUERMAZI A, et al. Osteoarthritis year in review 2017:updates on imaging advancements.Osteoarthritis Cartilage.2018;26(3):341-349. [9] GIGANTI F, MOORE CM. Magnetic resonance imaging in active surveillance-a modern approach.Transl Androl Urol.2018;7(1):116-131. [10] KHALIFA F, SOLIMAN A, EL-BAZ A, et al. Models and methods for analyzing DCE-MRI:a review.Med Phys.2014;41(12):124301. [11] HANSEN MIKKEL B, ANNA T, SØREN H, et al. Robust estimation of hemo-dynamic parameters in traditional DCE-MRI models.PLoS One. 2019;14(1):e0209891 [12] ZHANG Y, TAN Y, DONG C, et al. Chen H.Evaluating the scope of intramedullary invasion of malignant bone tumor by DCE-MRI quantitative parameters in an animal study.J Bone Oncol. 2019;19: 100269 [13] FUKUDA T, WENGLER K, DE CARVALHO R, et al. MRI biomarkers in osseous tumors.J Magn Reson Imaging.2019;50(3):702-718. [14] NING L, SU M, XING X, et al. Morphological and dynamic contrast enhanced MR imaging features for the differentiation of chordoma and giant cell tumors in the Axial Skeleton.Journal of Magnetic Resonance Imaging Jmri.2016;45(4):1068-1075. [15] DE CONINCK T, JANS L, SYS G, et al. Dynamic contrast-enhanced MR imaging for differentiation between enchondroma and chondrosarcoma.Eur Radiol.2013;23(11):3140-3152. [16] LEONARD L, MEYER HJ, SUROV A. Imaging characteristics of malignant and benign lesions of skeletal muscle.Radiologe. 2017;57(12): 1059-1070. [17] THEODOROS S, SHIVANI A, ELIZABETH M, et al. Multiparametric Assessment of Treatment Response in High-Grade Soft-Tissue Sarcomas with Anatomic and Functional MR Imaging Sequences.Radiology.2016;278(3):831-840. [18] Sujlana P, Skrok J, Fayad LM. Review of dynamic contrast-enhanced MRI:Technical aspects and applications in the musculoskeletal system.J Magn Reson Imaging. 2018;47(4):875-890. [19] GRANDE FD, SUBHAWONG T, WEBER K, et al. Detection of Soft-Tissue Sarcoma Recurrence: Added Value of Functional MR Imaging Techniques at 3.0 T.Radiology.2014;271(2):130844. [20] AMIT P, PATRO DK, BASU D, et al. Role of dynamic MRI and clinical assessment in predicting histologic response to neoadjuvant chemotherapy in bone sarcomas.Am J Clin Oncol. 2014;37(4): 384-390. [21] POTTECHER P, SIBILEAU E, AHO S, et al. Dynamic contrast-enhanced MR imaging in osteoid osteoma:relationships with clinical and CT characteristics.Skeletal Radiol. 2017;46(7):935-948. [22] LEPLAT C, HOSSU G, CHEN B, et al. Contrast-Enhanced 3-T Perfusion MRI With Quantitative Analysis for the Characterization of Musculoskeletal Tumors:Is It Worth the Trouble.AJR Am J Roentgenol. 2018;211(5):1092-1098. [23] DYKE JONATHAN P, LAZARO LIONEL E, HETTRICH CAROLYN M, et al. Regional analysis of femoral head perfusion following displaced fractures of the femoral neck.J Magn Reson Imaging. 2015;41(2): 550-554. [24] JUNG-EUN C, JOON YW, IN-ONE K, et al. Effect of arterial deprivation on growing femoral epiphysis: quantitative magnetic resonance imaging using a piglet model.Korean J Radiol. 2015;16:617-625. [25] KAMANO M, NARITA S, HONDA Y, et al. Contrast enhanced magnetic resonance imaging for femoral neck fracture.Clin Orthop Relat Res. 1998;(350):179-186. [26] KONISHIIKE T. Acute fracture of the neck of the femur.An assessment of perfusion of the head by dynamic MRI.J Bone Joint Surg Br.1999; 81(4):596-599. [27] LAMER S, DORGERET S, KHAIROUNI A, et al. Femoral head vascularisation in Legg-Calvé-Perthes disease:comparison of dynamic gadolinium-enhanced subtraction MRI with bone scintigraphy.Pediatr Radiol.2002;32(8):580-585 [28] 章猛奇.股骨颈骨折后股骨头血运检测方法的比较分析(附15例病例研究)[D].遵义:遵义医科大学, 2019. [29] JOHNSON JOEY P, JUSTIN K, GOODMAN AVI D, et al. Treatment of femoral neck fractures in patients 45-64 years of age.Injury.2019; 50(3):708-712. [30] LAZARO LE, DYKE JP, THACHER RR, et al. Focal osteonecrosis in the femoral head following stable anatomic fixation of displaced femoral neck fractures.Arch Orthop Trauma Surg. 2017;137(11):1529-1538. [31] CANINTIKA AF, DILOGO IH. Teriparatide for treating delayed union and nonunion: A systematic review.J Clin Orthop Trauma.2020;11(Suppl 1): S107-S112. [32] SCHOIERER O, BLOESS K, BENDER D, et al. Dynamic contrast-enhanced magnetic resonance imaging can assess vascularity within fracture non-unions and predicts good outcome.Eur Radiol. 2014;24(2): 449-459. [33] FISCHER C, NISSEN M, SCHMIDMAIER G, et al. Dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI) for the prediction of non-union consolidation.Injury. 2017;48(2):357-363. [34] WESTGEEST J, WEBER D, DULAI SK, et al. Factors Associated With Development of Nonunion or Delayed Healing After an Open Long Bone Fracture:A Prospective Cohort Study of 736 Subjects.J Orthop Trauma.2016;30(3):149-155. [35] CHRISTIAN F, EVA-MARIA P, MICHAEL T, et al. Dynamic Contrast-Enhanced Sonography and Dynamic Contrast-Enhanced Magnetic Resonance Imaging for Preoperative Diagnosis of Infected Nonunions.J Ultrasound Med.2016;35(5):933-942. [36] NG AWH, GRIFFITH JF, TALJANOVIC MS, et al. Is dynamic contrast-enhanced MRI useful for assessing proximal fragment vascularity in scaphoid fracture delayed and non-union.Skeletal Radiol. 2013; 42(7):983-992. [37] DONATI OF, ZANETTI M, NAGY L, et al. Is dynamic gadolinium enhancement needed in MR imaging for preoperative assessment of scaphoidal viability in patients with scaphoid nonunion.Radiology. 2011;260:808-816. [38] LARRIBE M, GAY A, FREIRE V, et al. Usefullness of dynamic contrastenhanced MRI in evaluation of the viability of acute scaphoid fracture.Skeletal Radiol.2014;43:1697-1703. [39] KORCHI AM, CENGARLE-SAMAK A, OKUNO Y, et al. Inflammation and Hypervascularization in a Large Animal Model of Knee Osteoarthritis:Imaging with Pathohistologic Correlation.J Vasc Interv Radiol.2019;30(7):1116-1127. [40] LEE JH, DYKE JP, BALLON D, et al. Subchondral fluid dynamics in a model of osteoarthritis:use of dynamic contrast-enhanced magnetic resonance imaging.Osteoarthritis Cartilage. 2009;17(10):1350-1355. [41] NUSMAN CM, HEMKE R, LAVINI C, et al. Dynamic contrast-enhanced magnetic resonance imaging can play a role in predicting flare in juvenile idiopathic arthritis.Eur J Radiol. 2017;88:77-81. [42] MAGDALENA K, AGNIESZKA O, ZBIGNIEW Ż, et al. Role of Microparticles in the Pathogenesis of Inflammatory Joint Diseases.Int J Mol Sci.2019;20(21):5453. [43] RIIS RGC, GUDBERGSEN H, HENRIKSEN M, et al. Synovitis assessed on static and dynamic contrast-enhanced magnetic resonance imaging and its association with pain in knee osteoarthritis:A cross-sectional study.Eur J Radiol.2016,85(6):1099-1108. [44] RIIS RGC, GUDBERGSEN H, SIMONSEN O, et al. The association between histological,macroscopic and magnetic resonance imaging assessed synovitis in end-stage knee osteoarthritis:a cross-sectional study.Osteoarthritis Cartilage.2017;25(2):272-280. [45] VORDENBÄUMEN S, SCHLEICH C, LÖGTERS T, et al. Dynamic contrast-enhanced magnetic resonance imaging of metacarpophalangeal joints reflects histological signs of synovitis in rheumatoid arthritis. 2014;16(5):452. [46] DE VRIES BA, VAN DER HEIJDEN RA, POOT DHJ, et al. Quantitative dynamic contrast-enhanced MRI blood perfusion in Hoffa’s fatpad signal abnormalities in patients with and without osteoarthritis.Osteoarthritis Cartilage.2020;28:S279. [47] SAVVOPOULOU V, MARIS TG, VLAHOS L, et al. Differences in perfusion parameters between upper and lower lumbar vertebral segments with dynamic contrast-enhanced MRI (DCE MRI).Eur Radiol. 2008;18(9):1876-1883. [48] MA HT, LV H, GRIFFITH JF, et al. Perfusion and bone mineral density as function of vertebral level at lumbar spine.Conf Proc IEEE Eng Med Biol Soc.2012;3488-3491. [49] DOLAN P, LUO J, POLLINTINE P, et al. Intervertebral disc decompression following endplate damage:implications for disc degeneration depend on spinal level and age.Spine (Phila Pa 1976).2013;38(17):1473-1481. [50] CHAO ST, KOYFMAN SA, WOODY N, et al. Recursive partitioning analysis index is predictive for overall survival in patients undergoing spine stereotactic body radiation therapy for spinal metastases.Int J Radiat Oncol Biol Phys.2012;82(5):1738-1743. [51] KUMAR KA, PECK KK, KARIMI S, et al. A Pilot Study Evaluating the Use of Dynamic Contrast-Enhanced Perfusion MRI to Predict Local Recurrence After Radiosurgery on Spinal Metastases.Technol Cancer Res Treat.2017;16(6):857-865. [52] FAYAD LM, JACOBS MA, WANG X, et al. Musculoskeletal tumors: how to use anatomic, functional, and metabolic MR techniques.Radiology.2012;265(2):340-356. [53] STACY C, SASAN K, PECK KYUNG K, et al. Measurement of blood perfusion in spinal metastases with dynamic contrast-enhanced magnetic resonance imaging:evaluation of tumor response to radiation therapy.Spine(Phila Pa 1976).2013;38(22):E1418-1424. [54] SPRATT DE, AREVALO-PEREZ J, LEEMAN JE, et al. Early magnetic resonance imaging biomarkers to predict local control after high dose stereotactic body radiotherapy for patients with sarcoma spine metastases.Spine J.2016;16(3):291-298. [55] OHGIYA Y, HASHIMOTO T, GOKAN T, et al. Dynamic MRI for distinguishing high-flow from low-flow peripheral vascular malformations. AJR Am J Roentgenol.2005;185(5):1131-1137. [56] OZKAN U, OĞUZKURT L, TERCAN F, et al. MRI and DSA findings in popliteal artery entrapment syndromeDiagn Interv Radiol. 2008; 14(2):106-110. [57] MURAKAMI AM, CHANG A, FOO LF. Traumatic Lateral Plantar Artery Pseudoaneurysm and the Use of Time-Resolved MR Angiography.HSS J.2010;6(2):214-218. [58] KOELEMAY MJ, LIJMER JG, STOKER J, et al. Magnetic resonance angiography for the evaluation of lower extremity arterial disease:a meta-analysis.JAMA.2001;285(10):1338-1345. [59] LIAO GJ, HENZE BANCROFT LC, STRIGEL RM, et al. Background parenchymal enhancement on breast MRI:A comprehensive review.J Magn Reson Imaging.2020;51(1):43-61. [60] SCHLEMMER HP. Multiparametric MRI of the prostate :Important radiological findings for urologists.Radiologe.2017;57(8):621-630. [61] CORVINO A, SANDOMENICO F, SETOLA SV, et al. Morphological and dynamic evaluation of complex cystic focal liver lesions by contrast-enhanced ultrasound:current state of the art.J Ultrasound. 2019;22(3):251-259. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Lu Dezhi, Mei Zhao, Li Xianglei, Wang Caiping, Sun Xin, Wang Xiaowen, Wang Jinwu. Digital design and effect evaluation of three-dimensional printing scoliosis orthosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1329-1334. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [7] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [8] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [9] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [10] | Yao Rubin, Wang Shiyong, Yang Kaishun. Minimally invasive transforaminal lumbar interbody fusion for treatment of single-segment lumbar spinal stenosis improves lumbar-pelvic balance [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1387-1392. |
| [11] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [12] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| [13] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [14] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [15] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||