Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (3): 443-448.doi: 10.3969/j.issn.2095-4344.2938
Previous Articles Next Articles
Comparison of the advantages and disadvantages of multiple implants in treatment of traumatic dislocation of sternoclavicular joint
Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao
- Department of Orthopedics, Renhe Hospital Affiliated to Three Gorges University, the Second Clinical Hospital of Three Gorges University, Yichang 443001, Hubei Province, China
-
Received:2020-03-10Revised:2020-03-16Accepted:2020-04-15Online:2021-01-28Published:2020-11-18 -
Contact:Zhou Jihui, Department of Orthopedics, Renhe Hospital Affiliated to Three Gorges University, the Second Clinical Hospital of Three Gorges University, Yichang 443001, Hubei Province, China -
About author:Zhou Jihui, MD, Chief physician, Department of Orthopedics, Renhe Hospital Affiliated to Three Gorges University, the Second Clinical Hospital of Three Gorges University, Yichang 443001, Hubei Province, China
CLC Number:
Cite this article
Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Comparison of the advantages and disadvantages of multiple implants in treatment of traumatic dislocation of sternoclavicular joint[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 443-448.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
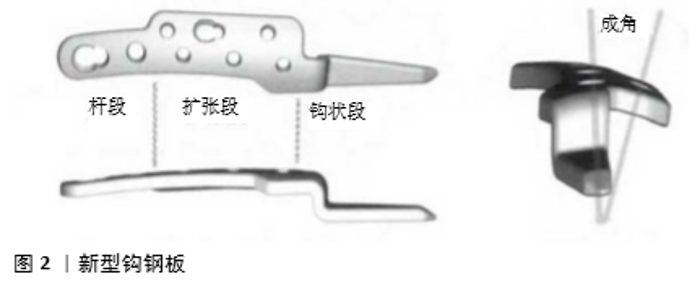
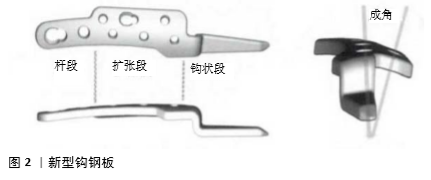
2.1 创伤性胸锁关节脱位的基本特点 胸锁关节脱位发生率较低,占锁骨内侧损伤的12.5%,在德国约为47.0/10万人,多由较大的暴力导致,发生率与从事职业的风险性密切相关,在运动中造成胸锁关节损伤的报道很少,以交通事故伤、快速奔跑中的跌倒或碰撞伤多见,常伴有复合性损伤,其中以胸部和颅脑损伤、肩部或上臂损伤为主。胸锁关节脱位的发病率与年龄密切相关,男性发病高峰在20-50岁,女性发病高峰在70岁以后[2-5]。轻度损伤表现为局部不稳、活动时疼痛、关节易复位,重度损伤时关节弹性固定于脱位状态,疼痛明显,难于复位,伴有纵隔结构损伤者可出现吞咽困难、呼吸困难、颈静脉怒张、上肢脉搏减弱乃至消失及感觉运动障碍等[6]。 根据锁骨内侧头的移位方向可分为前脱位及后脱位,近年来偶有上方脱位的病例报告[7]。根据脱位的程度可分为完全脱位和半脱位。有学者根据胸锁关节脱位时韧带的损伤程度对其进行分级:Ⅰ级,扭伤,韧带结构完整或部分撕裂,关节结构正常;Ⅱ级,胸锁韧带完全撕裂,肋锁韧带部分撕裂,关节失去稳定性,出现半脱位;Ⅲ级,所有韧带及关节囊完全撕裂,关节完全失去稳定性[8]。根据受伤后就诊时间可分为急性脱位、慢性脱位及复发性脱位。近年来有学者将Stanmore分型应用于胸锁关节脱位中,创伤性的胸锁关节脱位属于其中的Ⅰ型。 X射线片难以从多维度对胸锁关节结构进行评估,并非检查的最佳手段,可用作初步检查及排除其他损伤的手段。CT检查可从多个层面、多个维度对胸锁关节全面分析,是目前诊断胸锁关节脱位的首选方法。MRI可对韧带、关节囊损伤程度作出判断,同时也可显示纵隔内结构,作出全面细致的判断。有学者回顾了4年应用数字断层扫描(DT)检查胸锁关节脱位的患者,132例中只有18例(17.6%)需要进一步的CT和/或MRI检查,其余均作出了正确诊断,认为数字断层扫描对于诊断胸锁关节脱位是准确、经济的,应作为常规的影像学检查方法[9]。经验丰富的超声医生可对骨性结构形态和位置作出准确判断,同时可探查韧带及关节囊、关节盘的损伤情况,对胸锁关节脱位作出快速诊断[10]。 急性期进行手法复位,给予保守治疗得到大多数学者的认可,虽然非手术治疗不能确切的恢复关节周围的稳定结构,关节可能出现后期的不稳定,但多数对功能影响很小,无需进一步处理[11]。也有学者认为闭合复位无法修复韧带及关节囊的损伤,长期观察关节稳定性不佳,复发率达50%,主张尽早进行手术干预,重建关节稳定性[12]。对于胸锁关节后脱位的患者应警惕纵隔结构损伤的可能,一旦出现这种情况需要与血管外科、心胸外科、手外科共同评估患者的病情,麻醉师应对风险作出详细的预案[13],根据血管损伤程度可选择介入手术或开放手术[14-15]。血管损伤的处理应优先于神经损伤,神经损伤的位置和严重程度决定了是否进行观察及进行神经移植、神经移位等手术[16-17]。 胸锁关节脱位早期的正确诊断及治疗十分关键,是决定其预后的重要因素。进行正确的处置后大部分病例恢复了良好的肩部功能,而漏诊患者往往错过最佳治疗时机治疗较棘手,可能出现不同程度的功能障碍[18-19]。 2.2 手术治疗及内置物的选择 对于胸锁关节前方及后方脱位,如果闭合复位失败或复位后难以维持稳定,以及造成纵隔结构损伤的病例均需要手术治疗[20]。关于胸锁关节的手术方式较多,尚未形成统一的金标准,手术技术的进步主要体现在内置物的改进,既要求固定确切又要尽量符合胸锁关节生物力学性能。 克氏针张力带固定被较早应用于治疗胸锁关节脱位,钻孔后将“8”字钢丝穿过骨性隧道并环绕钢针形成张力带,以期重建及加强增强胸锁关节的稳定性。该手术创伤小、手术时间短、易掌握,但其稳定性难以满足生物力学要求,早期仍需制动处理。若克氏针发生断裂、移位可造成内固定失效或其他脏器损伤 [21],此项技术已不再单独使用,多作为辅助固定的手段。对于少年患者来说胸锁关节脱位往往合并骨骺损伤,此时应用克氏针治疗可暂时性稳定胸锁关节,防止锁骨近端的后移位,这种稳定技术是一种简单、安全、可行的治疗方法[22]。 应用肩锁关节钩钢板治疗胸锁关节脱位是可选的术式之一,其尾钩钩住胸骨柄的后方,通过杠杆力可将锁骨复位并通过螺钉固定,术中应注意避免胸骨后结构的损伤。QU 等[23]回顾性分析了2015年1月至2017年5月收治的10例胸锁关节前脱位患者的临床资料,其中男7例,女3例,平均年龄43.6岁,患者中无固定失效、无伤口感染、无钢板或螺钉断裂,所有患者的肩关节功能恢复较好,根据ASES评分系统术后肢体功能平均为94.8,作者建议利用缝线进行韧带的修复及重建以加强固定效果,认为此方法安全、有效,但也存在不足:如贴附性不佳,钩结构仍有损伤纵隔的风险,合并锁骨近端骨折时难以有效固定,术后需要随访观察钢板位置,同时缺乏长期随访的资料,插入尾钩时怎样避免造成纵隔结构的损伤,尾钩是否会对胸骨产生磨损、破坏甚至导致固定失效,钢板取出的适当时机等还需要进一步的深入探讨。针对肩锁关节钩钢板的不足之处,一种新型的钩钢板被设计并应用于治疗胸锁关节脱位[24],其外形根据胸锁关节的三维形态设计,钢板与锁骨更加贴附,尾钩自胸骨柄上方向下插入胸骨柄后方,更易显露并在直视下操作,更加安全可靠。ZHANG等[25]采用新型胸锁关节钩钢板治疗32例成人不稳定型胸锁关节脱位或骨折,其中胸锁关节前脱位12例,后脱位5例,术后X射线片和CT显示胸锁关节解剖位置正常,内固定位置良好,术后3-6个月所有患者均获得一期愈合,锁骨内侧解剖结构恢复良好,9例出现胸锁关节周围肿胀,无疼痛,术后6-12个月内取出内固定无后遗症。胸锁关节附近皮肤较薄,钢板尾钩对皮肤的刺激也是患者术后不适的主要原因,术中要求通过适当的塑形减少此类不适的发生。ZHANG等在应用胸骨钩钢板治疗时在尾钩附近加用螺钉及垫片阻挡,能够减少尾钩滑脱失效的风险。林旺等[26]设计了一款新型钩钢板(图2),钢板尾钩从侧方插入胸骨柄髓腔内进行固定,不必进行塑形处理,安放简单,避免了尾钩造成纵隔结构损伤的可能,对前脱位后脱位均可进行有效固定,生物力学测试显示这种钩板能够有效固定胸锁关节脱位,但还未进行临床测试,其疗效还需进一步检验。 "
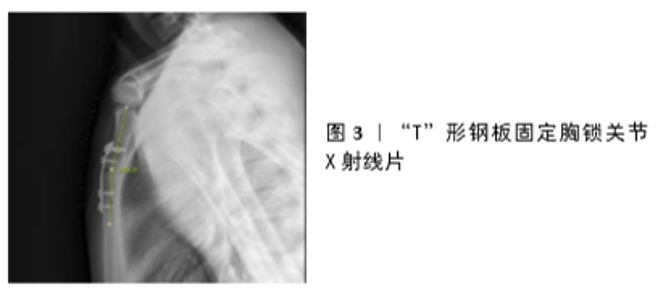
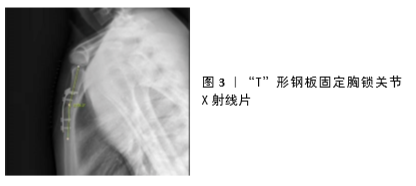
钢板技术是治疗胸锁关节脱位的主要技术之一。近年来有较多相关报道显示,钢板需要跨过关节进行固定,但这并不符合胸锁关节的生物力学特性,由于胸骨柄骨质薄弱,螺钉把持维持稳定的强度有限,如何实现对胸骨柄一侧强有力把持并保护胸骨后的重要结构是取得成功的关键。“T”形钢板可斜形放置于胸锁关节前方,横行部分与胸骨柄通过螺钉固定,纵行部分与锁骨固定使胸锁关节恢复正常形态(图3) [27],虽有报道单独使用锁定钢板获得了满意效果[28],但其单独固定的牢固性并不可靠,尤其对于骨质疏松者多需同时进行韧带结构的修复及重建。YANG等[29]根据胸锁关节形态设计了新型锁定钢板,符合胸骨柄解剖形态进行多孔设计,与斜“T”形钢板对比具有固定可靠、操作简单、创伤小、生物力学性能优越、功能锻炼早等优点,其临床效果还需进一步检验。孙远林等[30]设计了新型钢板用于胸锁关节脱位的临床治疗,依据国人锁关节解剖学特点设计,不需塑形,贴附良好,钢板横行部分的上方弯曲包绕胸骨切迹形成三维固定模式,使固定更加确切。GERICH等[31]应用前方支撑钢板技术对5例胸锁关节后脱位患者进行治疗,利用胸骨柄与钢板的杠杆力提拉锁骨复位,螺钉钢板与骨性结构形成支撑整体,达到固定目的。术后及钢板取出后进行CT扫描,发现关节结构正常,作者认为支撑钢板技术是治疗胸锁关节后脱位的有效方法。"
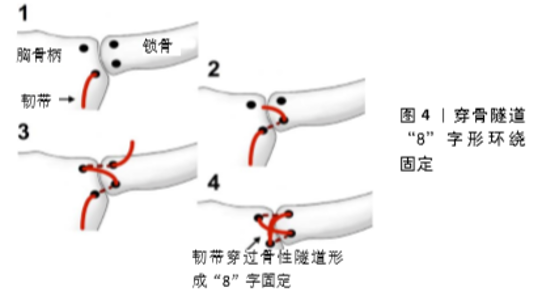
韧带的修复及重建技术更加符合胸锁关节的生物力学要求,使关节结构更加稳定并尽力恢复其原有的生理功能,逐渐成为主流的手术技术。韧带修复及重建材料包括强力缝线、自体肌腱、异体肌腱、锚钉、袢钢板等。WU等[32]对12例保守治疗无效的外伤性胸锁关节前脱位患者采用“W”型编织异体肌腱治疗,通过编织技术使肌腱的强度达到稳定要求,肌腱穿过锁骨与胸骨柄之间的隧道并拉紧,复位重建韧带结构,保留生理性微动,取得满意效果,但异体肌腱的排斥反应还需要长期的观察。PEEBLES等[33]取患者自体半腱肌腱编织后进行胸锁关节韧带重建,同时修复损伤的关节囊,对陈旧性损伤导致锁骨内侧增生退化者进行关节修整。WANG等[34]将编织后的自体股薄肌腱穿过胸骨及锁骨隧道呈“8”字形环绕固定(图4),这种重建技术是安全和可靠的。WIDODO 等[35]采用自体胸锁乳突肌腱移植重建胸锁关节韧带及关节囊的稳定性。TERRA 等[36]报道了1例取同侧掌长肌腱重建胸锁关节稳定性的成功病例,取腱会对患者造成二次损伤且有一定的并发症,需要在术前进行详细有效的沟通。FiberWire?缝合线由多股、长链超高分子量聚乙烯(UHMWPE)芯线和聚酯和长链超高分子量聚乙烯编织护套构成,具有满意的强度、柔软感和耐磨性,纤维线的强度和可靠性使其为韧带重建和加强提供了良好保障。ADAMCIK等[37]用Fiberwire对胸锁关节行“8”字固定,5例患者无发症发生,关节稳定性良好。Ethibond Exel M46 5号缝线及6?mm聚酰胺不可吸收型缝合线主要用于骨块之间的缝合固定,强度可满足韧带重建的需要,在锁骨及胸骨柄建立隧道后使用上述2种缝线重建胸锁关节稳定性均有成功的案例[38-39],但缝线生物力学性能仍受到质疑,对骨质疏松患者骨质的切割作用也是需要考虑的问题。MARTETSCHL?GER等[40]从生物力学角度比较了缝线与肌腱重建胸锁关节稳定性的效果,肌腱更接近韧带的力学特性,缝线的刚度明显大于肌腱,作者更推荐使用肌腱与缝线联合应用,认为此方法力学性能最佳;作者同时比较了前后方向直行和斜行建立骨隧道对于力学强度的影响,发现相同材料通过直行通道的力学性能更佳。袢钢板技术被广泛应用于韧带重建与加强中并取得了良好的效果,如喙锁韧带、距腓韧带重建等,因为其操作简单、无需广泛显露、固定确切、生物力学稳定、无需二次手术取出等优点受到骨科医生的认可。UNTERKOFLER等[41]应用纵弧形切口显露锁骨近端及第一肋骨,双Tight Rope重建肋锁韧带,从而恢复胸锁关节的稳定性,对线缆进行缝线加固绷紧处理,增加了固定强度,作者报告了1例成功的案例,6个月后患者完全恢复正常功能。锚钉技术同样是骨科医生修复韧带损伤的常有手段。陈鹏等[42]应用双锚钉分别锚定胸骨及锁骨近端,线缆呈“8”字收紧固定,术中同时修复关节囊,作者认为此项技术微创、易掌握、固定可靠、无需二次手术。应用袢钢板及锚钉治疗胸锁关节损伤并无足够的生物力学及大样本临床文献支持,其效果还需要进一步探讨。 定制的胸锁关节假体置换可重建已毁损的胸锁关节结构,ROBERTSON等[43]应用此项技术治疗了1例锁骨内侧切除的患者,术中植入定制假体解决了患者术前疼痛、肩部活动受限、不能正常生活及工作的困扰,作者认为定制假体置换治疗胸锁关节毁损伤是令人振奋的新方向,应该进行更多的研究。 2.3 内置物的优劣分析 锁骨的独特“S”形结构使其内侧仅有约50%的面积与胸骨柄相关节,二者之间存在纤维软骨盘,软骨盘损伤被认为是疼痛产生的原因。这种鞍形关节的稳定性主要靠关节囊及周围的韧带结构,包括包括肋锁(菱形)韧带的前束和后束、锁骨间韧带和胸锁关节后韧带和前韧带,而后关节囊是诸多稳定因素中的关键,单独切断其他韧带并未造成或增加关节的移位,前后关节囊的破坏均明显增加前脱位程度,后关节囊的破坏使前脱位更加显著,后关节囊的破坏对可明显增加后脱位的程度,而前关节囊的破坏对后脱位几乎无影响。胸锁关节属微动关节,在周围肌肉的牵拉下与肩锁关节协同,锁骨内侧头相对于胸骨柄进行旋转及平移,使锁骨进行前后、上下及旋转活动,使复杂的肩部运动得以顺利的完成。进行手术治疗时应符合胸锁关节的生物力学特点,既要求强度足够满足稳定的需要又要考虑关节微动的需要及对内置物产生的应力影响。 在诸多的内置物中,克氏针张力带的强度较差,随着关节的微动易造成克氏针的松动及游走;钢丝易发生断裂,胸骨柄的骨质比较薄弱,钢丝易造成切割效应;克氏针在骨科手术中通常作为临时固定工具,对于骨骺未闭的少年患者,克氏针则是更为合适的固定方式,保护骨骺的同时对锁骨近端进行暂时有效控制,最大限度地保持发育及功能的平衡,因此克氏针是少年患者的首选内置物。对于少年患者而言,医生应全面考虑患者日后发育及功能问题,应尽早进行手术干预,应用克氏针进行稳定治疗,使损伤对发育影响降至最低,尽量恢复功能[44]。 跨关节钢板固定很少应用,不符合微动关节的生物力学要求,胸锁关节附近的骨折相对薄弱,胸骨柄形态不规则,后方是纵隔结构,螺钉从前方难以实现双皮质固定,单独的锁定钢板并不是肩锁关节脱位内置物的理想选择,新型的钢板虽然更加贴附并增加了胸骨柄的固定强度,但仍未完全克服生物力学上的劣势。 钩钢板属于弹性固定的内置物,缺点在于尾钩结构造成骨质的磨损和刺激,可以推断尾钩结构对胸骨柄也会造成磨损和刺激,因发病率低,其并发症的报道并不多见。改良钩钢板在胸骨切迹处进行把持或插入胸骨柄髓腔内,避免了损伤胸骨后结构的可能性,也减轻了对胸骨的磨损程度,但这些设计同时减弱了依赖于胸骨柄产生的杠杆力,尾钩在髓腔内微动造成的刺激同样存在隐患,钩钢板对于胸锁关节脱位也不是理想的内置物。 韧带的重建及加强技术在锁骨远端骨折及肩锁关节脱位中越来越受到认可,胸锁关节的生物力学与肩锁关节相似,韧带的重建及加强技术逐渐占据主导地位。内置物材料方面既要满足强度需要又要具有一定的弹性。自体肌腱在诸多材料中无疑是性能最佳的,经过编织处理及隧道技术后可以实现完美的重建,但取腱部位损伤及操作技术要求较高使其应用受到限制;异体肌腱可避免损伤,但其免疫排斥的隐患尚不能完全去除;人工肌腱价格较高,疗效还需进一步验证。强力缝线、锚钉的线缆强度有余而弹性稍差,对关节的弹性固定要求不能完美应对,容易对隧道周围骨质造成切割,可认为是性价比较高的内置物。袢钢板的生物力学性能、术后舒适程度方面均令人满意,因胸锁关节形态特殊,袢钢板无法在水平方向实现固定,重建肋锁韧带需要相对充分的显露,其他内置物配合可使固定效果更加理想。 对于胸锁关节脱位应用内置物治疗的长期随访及比较分析是必要的,因为发病率较低,这项工作需要联合研究及长期的工作积累[45]。对于锁骨骨折及关节脱位而言韧带的重建越来越受到重视,提高了生物力学稳定性[46],KENDAL等[47]通过荟萃分析认为手术治疗胸锁关节脱位总的并发症发生率为16%,肌腱移植重建韧带的不稳定性和并发症发生率最低。 在手法复位中也有应用内置物的案例。IWAI等[48]应用复位钳技术对受伤后72 h左右的柔道运动员实现了闭合复位,指出向上拉动锁骨近端并旋转锁骨可以很容易地完成复位。HADI等[49]应用螺钉钢板形成提拉手柄实现复位,取5孔钢板,自其中间孔向锁骨拧入自攻皮质螺钉(约50 mm)到后皮质,钢板与螺钉形成“T”形手柄,将锁骨向前拉达到复位目的。胸锁关节损伤导致结构缺损难以重建时,定制的人工关节是必备的内置物。 "
| [1] VITALI M, DROSSINOS A, PIRONTI P, et al.The management of Salter-Harris type II fracture with associated posterior sternoclavicular joint displacement using a locking compression plate: A 14-year-old adolescent’s case report.Medicine (Baltimore).2019;98(51):e18433. [2] BAKIR MS, UNTERKOFLER J, HARALAMBIEV L, et al.Medial injuries of the clavicle: more prevalent than expected?A big data analysis of incidence,age,and gender distribution based on nationwide routine data.Eur J Trauma Emerg Surg.2020.doi: 10.1007/s00068-019-01293-0.[Epub ahead of print]. [3] BAKIR MS, UNTERKOFLER J, HÖNNING A, et al.Shoulder girdle injuries involving the medial clavicle differ from lateral clavicle injuries with a focus on concomitant injuries and management strategies:A retrospective study based on nationwide routine data.PLoS One. 2019; 14(10):e0224370. [4] HELLWINKEL JE, MCCARTY EC, KHODAEE M. Sports-related sternoclavicular joint injuries.Phys Sportsmed.2019;47(3):253-261. [5] GUN B, DEAN R, GO B, et al.Non-modifiable Risk Factors Associated with Sternoclavicular Joint Dislocations in the U.S. Military.Mil Med. 2018;183(5-6):188-193. [6] MORELL DJ, THYAGARAJAN DS. Sternoclavicular joint dislocation and its management: A review of the literature.World J Orthop. 2016; 7(4):244-250. [7] MENEZ C, KIELWASSER H, FAIVRE G, et al.Superior sternoclavicular dislocation: A case report.Int J Surg Case Rep.2017;40:102-104. [8] KIEL J, KAISER K. Sternoclavicular Joint Injury.StatPearls [Internet].Treasure Island (FL):StatPearls Publishing,2020. [9] TYTHERLEIGH-STRONG G, MULLIGAN A, BABU S, et al.Digital tomography is an effective investigation for sternoclavicular joint pathology. Eur J Orthop Surg Traumatol. 2019;29(6):1217-1221. [10] BENGTZEN RR, PETERING RC. Point-of-Care Ultrasound Diagnosis of Posterior Sternoclavicular Joint Dislocation.J Emerg Med. 2017; 52(4):513-515. [11] BICOS J, NICHOLSON GP. Treatment and results of sternoclavicular joint injuries.Clin Sports Med.2003;22:359-370. [12] TYTHERLEIGH-STRONG G, PECHEVA M, TITCHENER A. Treatment of First-Time Traumatic Anterior Dislocation of the Sternoclavicular Joint With Surgical Repair of the Anterior Capsule Augmented With Internal Bracing.Orthop J Sports Med.2018;6(7):2325967118783717. [13] WEINBERG R, CHAZEN JL, LICHTMAN AD. Anesthetic Management of Posterior Sternoclavicular Joint Dislocations:A Report of 2 Cases.A A Pract.2020;14(5):152-154. [14] COLOMBIER S, GIROD G, NICLAUSS L, et al. Total Endovascular Repair of Post-Trauma Ascending Aortic Pseudoaneurysm and Secondary Superior Vena Cava Syndrome.Ann Vasc Surg.2019;61:468e.13-468.e17. [15] DI MENTO L, STALETTI L, CAVANNA M, et al. Posterior sternoclavicular joint dislocation with brachiocephalic vein injury:a case report.Injury. 2015;46 Suppl 7:8-10. [16] CHOO AM, SCHOTTEL PC, BURGESS AR. Scapulothoracic Dissociation: Evaluation and Management.J Am Acad Orthop Surg.2017;25(5): 339-347. [17] KIM YH, KIM JJ, CHOI SY, et al.Successful repair of thoracic outlet syndrome in a growing young patient due to posterior sternoclavicular joint dislocation.J Thorac Dis.2017;9(10):912-915. [18] KUSNEZOV N, DUNN JC, DELONG JM, et al.Sternoclavicular Reconstruction in the Young Active Patient: Risk Factor Analysis and Clinical Outcomes at Short-Term Follow-up.J Orthop Trauma. 2016;30(4):111-117. [19] BOESMUELLER S, WECH M, TIEFENBOECK TM, et al.Incidence, characteristics, and long-term follow-up of sternoclavicular injuries:An epidemiologic analysis of 92 cases.J Trauma Acute Care Surg.2016;80(2):289-95. [20] SERNANDEZ H, RIEHL J. Sternoclavicular Joint Dislocation: A Systematic Review and Meta-analysis.J Orthop Trauma.2019;33(7):251-255. [21] 高翔,陈玉宏,李建鹏,等.胸锁关节脱位诊治现状[J].中国矫形外科杂志,2019,27(13):1190-1193. [22] ISHII N, MATSUMURA N, IWAMOTO T, et al. Temporary Sternoclavicular Stabilization Using an Innovative Blocking Technique with Kirschner Wires for the Treatment of Posterior Sternoclavicular Joint Injury in Adolescent Patients: A Report of Two Cases.JBJS Case Connect.2018;8(3):76. [23] QU YZ, XIA T, LIU GH, et al.Treatment of Anterior Sternoclavicular Joint Dislocation with Acromioclavicular Joint Hook Plate.Orthop Surg.2019;11(1):91-96. [24] ZHANG C, LIN L, LIANG J, et al. Efficacy analysis of a novel sternoclavicular hook plate for treatment of unstable sternoclavicular joint dislocation or fracture.J Orthop Surg (Hong Kong).2017;25(1): 2309499016684488. [25] ZHANG CY, LIN L, LIANG JB, et al. A new type sternoclavicular hook plate for unstable sternoclavicular joint dislocation and fracture.Zhongguo Gu Shang.2016;29(11):1040-1044. [26] 林旺,王盈盈,林伟民,等.新型胸锁关节钩状板的研发与生物力学测定[J].中国组织工程研究,2020,24(9):1395-1399. [27] HWANG WJ, LEE Y, YOON YS, et al. Surgical Treatment of Sternoclavicular Joint Dislocation Using a T-plate.Korean J Thorac Cardiovasc Surg. 2016;49(3):221-223. [28] AO R, ZHU Y, ZHOU J, et al. Locking plate for treating traumatic sternoclavicular joint dislocation: a case series. BMC Musculoskelet Disord.2018;19(1):7. [29] YANG K,YANG Y, GE J, et al.Development and biomechanical study of anatomical locking plate of sternoclavicular joint.Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi.2018;32(1):7-13. [30] 孙远林,阳运康,葛建华,等.新型胸锁关节解剖锁定钢板的研制与临床应用[J].中国修复重建外科杂志,2018,32(3):316-321. [31] GERICH T, HOFFMANN A, BACKES F, et al.Anterior buttress plate is successful for treating posterior sterno-clavicular dislocation. Knee Surg Sports Traumatol Arthrosc.2019;27(1):251-258. [32] WU G, CHEN S, LIN S, et al.Treatment of traumatic anterior dislocation of sternoclavicular joint with allogeneic tendon of “W” type knit.Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi.2019;33(8):976-980. [33] PEEBLES LA, AMAN ZS, PREUSS FR, et al.Chronic Instability and Pain of the Sternoclavicular Joint: Treatment With Semitendinosus Allograft to Restore Joint Stability.Arthrosc Tech.2019;8(6):e629-e635. [34] WANG D, CAMP CL, WERNER BC, et al.Figure-of-8 Reconstruction Technique for Chronic Posterior Sternoclavicular Joint Dislocation.Arthrosc Tech.2017;6(5):e1749-e1753. [35] WIDODO W, FAHRUDHIN M, KAMAL AF. Joint reconstruction using sternocleidomastoid tendon autograft as a treatment for traumatic posterior dislocation of sternoclavicular joint:A case report.Trauma Case Rep.2018;18:8-16. [36] TERRA BB, RODRIGUES LM, PÁDUA DV, et al. Sternoclavicular dislocation:case report and surgical technique.Rev Bras Ortop. 2015; 50(4):472-477. [37] ADAMCIK S, AHLER M, GIOUTSOS K, et al.Repair of sternoclavicular joint dislocations with FiberWire®.Arch Orthop Trauma Surg. 2017; 137(3):341-345. [38] LABRONICI PJ, SOUZA FC, PIRES RE, et al. Posterior dislocation of the sternoclavicular joint: report of two cases.Rev Bras Ortop. 2016; 51(5):601-605. [39] AYDıN E, DÜLGEROĞLU TC, ATEŞ A, et al.Repair of Unstable Posterior Sternoclavicular Dislocation Using Nonabsorbable Tape Suture and Tension Band Technique:A Case Report with Good Results.Case Rep Orthop.2015;2015:750898. [40] MARTETSCHLÄGER F, REIFENSCHNEIDER F, FISCHER N, et al. Sternoclavicular Joint Reconstruction Fracture Risk Is Reduced With Straight Drill Tunnels and Optimized With Tendon Graft Suture Augmentation. Orthop J Sports Med.2019;7(4):2325967119838265. [41] UNTERKOFLER J, MERSCHIN D, LANGENBACH A, et al.Injuries of the Sternoclavicular Joint - An Innovative Approach in the Management of a Rare Injury:Tight Rope Fixation of the Costo-Clavicular Ligament.Chirurgia (Bucur).2017;112(5):611-618. [42] 陈 鹏,计飞,陈一舟,等.带线锚钉技术治疗创伤性胸锁关节脱位的临床应用[J].浙江创伤外科,2019,24(2):311-312. [43] ROBERTSON FM, MOHAMMED AA, FROSTICK SP. Sternoclavicular joint replacement case report.J Orthop Surg (Hong Kong).2018;26(1):2309499018761176. [44] STANČÁK A, NĚMEC J, HAVLAS V. Rare Dorsal Traumatic Sternoclavicular Joint Dislocation in a 14-Year-Old Patient - a Case Report. Acta Chir Orthop Traumatol Cech.2017;84(3):215-218. [45] BAKIR MS, MERSCHIN D, UNTERKOFLER J, et al.Injuries of the Medial Clavicle: A Cohort Analysis in a Level-I-Trauma-Center. Concomitant Injuries. Management. Classification.Chirurgia (Bucur). 2017;112(5): 594. [46] GROH GI, MIGHELL MA, BASAMANIA CJ, et al.All Things Clavicle:From Acromioclavicular to Sternoclavicular and All Points in Between.Instr Course Lect.2016;65:181-196. [47] KENDAL JK, THOMAS K, LO IKY, et al.Clinical Outcomes and Complications Following Surgical Management of Traumatic Posterior Sternoclavicular Joint Dislocations:A Systematic Review.JBJS Rev.2018;6(11):2. [48] IWAI T, TANAKA K, OKUBO M. Closed reduction of a posterior sternoclavicular joint dislocation:A case report.Trauma Case Rep. 2018; 17:1-4. [49] HADI S, LIMB D. A safer method for urgent reduction of posterior sternoclavicular dislocation.Ann R Coll Surg Engl.2017;99(4):337. |
| [1] | Pu Rui, Chen Ziyang, Yuan Lingyan. Characteristics and effects of exosomes from different cell sources in cardioprotection [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-. |
| [2] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [3] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [4] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [5] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [6] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [7] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [8] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [9] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [10] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [11] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [12] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [13] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [14] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| [15] | Chen Xinmin, Li Wenbiao, Xiong Kaikai, Xiong Xiaoyan, Zheng Liqin, Li Musheng, Zheng Yongze, Lin Ziling. Type A3.3 femoral intertrochanteric fracture with augmented proximal femoral nail anti-rotation in the elderly: finite element analysis of the optimal amount of bone cement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1404-1409. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||