Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (21): 3321-3328.doi: 10.3969/j.issn.2095-4344.2652
Previous Articles Next Articles
Morphological analysis of optimal selection of lumbar pedicle screws in adolescents aged 12-15 years
Xu Yangyang1, Zhang Kai2, Li Zhijun3, Zhang Yunfeng4, Su Baoke1, Wang Xing3, Wang Lidong5, Wang Yidan1, He Yujie3, Li Kun3, Wang Haiyan3, Li Xiaohe3
- 1Graduate School of Inner Mongolia Medical University; 2Department of Orthopedics, Ulanqab Second Hospital; 3Department of Anatomy, School of Basic Medicine, Inner Mongolia Medical University; 4Department of Radiology, the Second Affiliated Hospital of Inner Mongolia Medical University; 5Deoartment of Radiology, Inner Mongolia International Mongolian Hospital
-
Received:2019-10-21Revised:2019-10-25Accepted:2019-11-29Online:2020-07-28Published:2020-04-16 -
Contact:Wang Haiyan, Master, Associate professor, Master’s supervisor, Department of Anatomy, School of Basic Medicine, Inner Mongolia Medical University, Hohhot 010110, Inner Mongolia Autonomous Region, China Li Xiaohe, MD, Professor, Master’s supervisor, Department of Anatomy, School of Basic Medicine, Inner Mongolia Medical University, Hohhot 010110, Inner Mongolia Autonomous Region, China -
About author:Xu Yangyang, Master candidate, Graduate School of Inner Mongolia Medical University, Hohhot 010110, Inner Mongolia Autonomous Region, China Zhang Kai, Doctoral candidate, Attending physician, Department of Orthopedics, Ulanqab Second Hospital, Ulanqab 012000, Inner Mongolia Autonomous Region, China Xu Yangyang and Zhang Kai contributed equally to this work. -
Supported by:the National Natural Science Foundation of China, No. 81460330, 81560348, and 81860383; the Youth Science and Technology Talent Project of Inner Mongolia Education Department, No. njyt-15-b05; Science and Technology Program of Inner Mongolia Autonomous Region, No. 2016; the Science and Technology Innovation Guide Project of Inner Mongolia Autonomous Region, No. 2017; the Natural Science Foundation of Inner Mongolia Autonomous Region, No. 2016ms08131; the Returned Scholar Foundation of Human Resources and Social Security Department of Inner Mongolia Autonomous Region, No. TKD2017KJBW012; the Science and Technology Million Program of Inner Mongolia Medical University, No. YKD2017KJBW012
CLC Number:
Cite this article
Xu Yangyang, Zhang Kai, Li Zhijun, Zhang Yunfeng, Su Baoke, Wang Xing, Wang Lidong, Wang Yidan, He Yujie, Li Kun, Wang Haiyan, Li Xiaohe. Morphological analysis of optimal selection of lumbar pedicle screws in adolescents aged 12-15 years[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(21): 3321-3328.
share this article

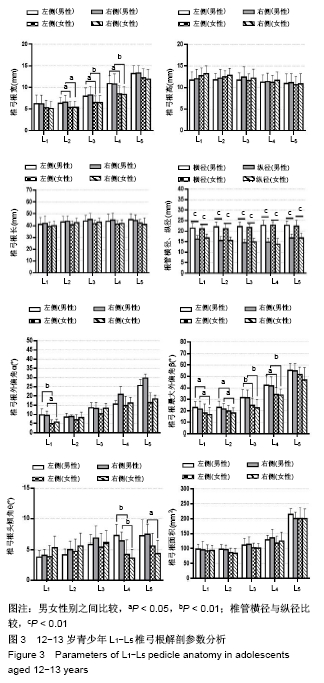
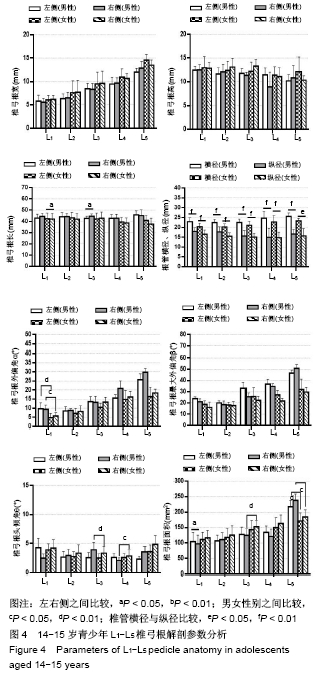
2.1.1 椎弓根宽 12-13岁,L1-L5逐渐增大,L1-L5最小值分别为(5.11±1.64),(5.38±1.38),(6.48±1.62),(8.41±1.81)及(11.9±2.19) mm,男性大于女性,左右侧差异无显著性意义,L2-L4男女之间差异有显著性意义,L1-L5节段差异有显著性意义。 14-15岁,椎弓根宽变化趋势同12-13岁,L1-L5逐渐增大,L1-L5最小值分别为(5.59±0.82),(6.33±0.89),(6.32± 1.35),(9.45±1.47)及(12.03±0.83)mm,男性小于女性,左右侧差异无显著性意义,L1-L5节段差异有显著性意义。 2.1.2 椎弓根高 12-13岁,L1-L5逐渐减小,L1-L5最小值分别为(12.70±1.82),(11.78±1.49),(11.71±1.70),(11.19± 1.59)及(10.66±1.88) mm,L4,L5节段差异有显著性意义。 14-15岁,此次研究中变化趋势不确定,L1-L5最小值分别为(12.42±0.90),(11.65±1.32),(11.38±0.62),(11.11± 1.90) 及(10.17±1.39) mm;左右侧与性别间均差异无显著性意义,L4,L5节段差异有显著性意义。 2.1.3 模拟椎弓根长 12-13岁,L1-L5变化范围不大,均为40-45 mm,左右侧与性别间差异均有显著性意义,L1节段差异有显著性意义。 14-15岁,L1-L4变化范围不大,均为40-45 mm;L5在45-50 mm之间,L1,L3左右之间差异有显著性意义,L1节段差异有显著性意义。 2.1.4 椎管横径与椎管纵径 2组规律相同,椎管橫径L1-L5逐渐增大;椎管纵径L1-L4先轻微减小,L4-L5增大。椎管橫径均大于椎管纵径,椎管呈现椭圆-倒三角的形态变化,椎管橫径、椎管纵径之间差异均有显著性意义,男女之间差异无显著性意义。 2.1.5 椎弓根外偏角(α) 12-13岁,L1-L2变化不大,L2-L5逐渐增大,男(8.23±3.27)°至(30.41±6.33)°,女(6.40±2.32)°至(26.98±5.51)°,男性大于女性,L3-L4男女之间差异有显著性意义,L4,L5节段差异有显著性意义。 14-15岁,L1-L5逐渐增大,男(9.32±2.63)°至(29.75± 2.45)°,女(4.84±2.32)°至(18.37±2.11)°,男性大于女性,L1男女之间差异有显著性意义,L1-L5节段差异有显著性意义。 2.1.6 椎弓根最大外偏角(β) 12-13岁,L1-L5逐渐增大,男(21.58±7.02)°至(54.81±6.39)°,女(16.70±6.53)°至(51.79±6.44)°,男性大于女性。 14-15岁,L1-L5逐渐增大,男(20.76±2.63)°至(50.73± 3.66)°,女(16.04±4.65)°至(31.95±4.07)°;β值随年龄增长而减小,左右侧与性别间均差异无显著性意义,不同年龄间差异有显著性意义,2组L1-L5节段差异有显著性意义。 2.1.7 椎弓根头倾角(θ) 腰椎不同于胸椎,腰椎椎弓根宽且θ较小,胸椎头倾角明显,螺钉置入时要指向下终板方向,但腰椎指向上终板。12-13岁,L1-L5有一个3°-8°的角度指向上终板,男(3.80±2.84)°至(7.39±3.51)°,女(3.87±2.60)°至(5.62±3.30)°;L4-L5男女之间差异有显著性意义。 14-15岁,L1-L5有一个0°-5°的角度指向上终板,男(2.47±0.26)°-(3.56±0.97)°,女(3.89±1.06)°-(4.86±1.49)°;θ值随年龄增长而减小,L3-L4男女之间差异有显著性意义,2组L1节段差异有显著性意义。 2.1.8 椎弓根面积 12-13岁,L1-L5逐渐增大,L4-L5有一个明显的变化趋势,L1-L5为(92.45±20.22) mm2至(214.62± 18.66)mm2。 14-15岁,L1-L5逐渐增大,L4-L5有一个明显的变化趋势,L1-L5为(96.37±28.73) mm2至(237.52±21.29) mm2,L1左右间差异有显著性意义,L3,L5男女之间差异有显著性意义,2组L1-L5节段差异有显著性意义。 2.2 与国内外文献比较 2.2.1 椎弓根宽 此次研究中12-15岁青少年腰椎L1-L5,椎弓根宽逐渐增加(5.11-12.03 mm),与DZIER?ANOWSKI等[5]、MOHAMED等[6]、MOHANTY等[7]、LOTFINIA等[8]、SANI等[9]得出的规律相同,男性大于女性,均大于此次研究测量值。MUGHIR等[10]对马来西亚17岁以下青少年研究得出,椎弓根宽男性明显大于女性,上腰椎建议使用3.5 mm直径的螺钉,下腰椎使用5.0-6.5mm直径的螺钉;18岁以上L1-L5椎弓根宽,男7.3-16.2 mm,女5.8-13.9 mm。成年日本人L1-L5的椎弓根宽,男7.4-11.1 mm,女6.9-10.6 mm[11]。在成年印度人中L1-L5椎弓根宽,男7.1-16.2 mm,女5.9- 12.8 mm[12]。Kim等[13]报道成年朝鲜族人L1-L5椎弓根宽,男7.0-18.9 mm,女6.6-17.6 mm。 2.2.2 椎弓根高 12-13岁L1-L5逐渐减小(12.70- 10.17 mm);而14-15岁,L1-L4减小,L4-L5增大,L4最小。DZIER?ANOWSKI等[5]对27-75岁白人CT资料研究得出,椎弓根高值L1-L4减小,L4-L5增大,L4节段最小,与此次实验结果相似。戚力升等[14]通过对100例成人腰椎CT资料研究得出L1-L5逐渐减小(15.1-10.4 mm),变化趋势与此次研究相似,但测量值大于此次研究结果。WANG等[15]对6-11岁儿童影像学资料进行研究,椎弓根宽,L1-L5逐渐增大;椎弓根高,6-8岁L1-L5逐渐增大,9-11岁L1-L4减小,L4-L5增大;椎管橫径与椎管纵径,L1-L5逐渐增大,与此次研究变化趋势一致,但椎弓根尺寸小于此次实验数据。SANI等[10]对南非人群进行研究,椎弓根高L1-L5逐渐下降,与此次实验结果相似。L1-L4节段椎弓根宽小于椎弓根高,所以L1-L4的螺钉尺寸取决于椎弓根宽,L5节段椎弓根高小于椎弓根宽,所以L5的螺钉尺寸取决于椎弓根高。 2.2.3 椎弓根长 此次研究中12-15岁青少年腰椎L1-L5椎弓根长值变化范围较小(40-45 mm)。DZIER?ANOWSKI等[5]对27-75岁白人CT资料研究得出,椎弓根长值为50-52 mm,大于此次研究结果。GRIVAS 等[16]对100例33-87岁希腊成人CT资料进行研究,发现L4处最长(55.31±4.52)mm,比此次研究测量值大,变化趋势与此次研究12-13岁相似。戚力升等[14]通过对100例成人腰椎CT资料研究得出L1-L5逐渐增大(48.6-52.7 mm),变化趋势与此次研究相似,但测量值大于此次研究结果。SANI等[10]对南非人群研究,椎弓根长L1-L5略有下降,与此次研究14-15岁组结果相似。MUGHIR等[11]对马来西亚17岁以下青少年研究得出,椎弓根长从L1-L3逐渐增加,L3-L4逐渐减少,L3最长,L5最短,并且提倡在青少年人群中使用更短的椎弓根螺钉,在所有的腰椎水平上,选择30-35 mm的螺钉长度。KADIOGLU等[17]发现土耳其成人椎弓根轴长在L1最长(42.7 mm),L5最短(40.8 mm),土耳其成人与国内青少年尺寸相似。 2.2.4 椎管橫径和椎管纵径 椎管橫径,L1-L5逐渐增大(21.07-27.80 mm);椎管纵径,L1-L4先轻微减小,L4-L5增大(14.49-16.72 mm)。 2.2.5 外偏角α和最大外偏角β L1-L5均逐渐增大趋势,α角男为8.23°-30.41°,女为6.40°-26.98°;β角男为21.58°-54.81°,女为16.70°-51.79°。张军等[18]通过对300份椎弓根CT资料研究得出相似的结论,外偏角α为13.04°-33.07°。DZIER?ANOWSKI等[5]对27-75岁白人CT资料研究得出,α角为20°-32°,大于此次研究结果。CACCIOLA等[19]通过对意大利325名健康人(平均年龄62岁)L4,L5的CT资料研究得出,90%外偏角>30°,10%外偏角<30°。?APAR等[20]使用CT测量测量α角,L1为10.9°,L2为12°,L3为14.4°,L4为17.7°,L5为29.8°,与此次研究有差别。MOHANTY等[7]、SANI等[10]研究得出外偏角α的变化趋势与此次研究大体一致。AZAR等[21]对50例印度人群的CT研究发现,L1为(10.90±3.13)°,L5为(24.75±3.83)°,与西方人群相似。 2.2.6 头倾角θ L1-L5与上终板有小于8°的θ角,角度较小。DZIER?ANOWSKI等[5]对27-75岁白人CT资料研究得出,θ为10°-12°,大于此次研究结果。SANI等[10]对南非人群研究得出θ角为4.43°-4.88°,L1-L5略有增加,与此次研究结果相似。 2.2.7 椎弓根面积 L1-L5逐渐增大,为92.45- 237.52 mm2。DZIER?ANOWSKI等[5]研究得出,L1-L5逐渐增大,为62-140 mm2,与此次实验差别较大。分析得出中国青少年椎弓根外偏角较大,与冠状面成角,测得椎弓根面积值在冠状面投影的椎弓根轴面面积会变大。 LOTFINIA等[8]对50例伊朗人(男25例,女25例)的研究中发现,椎弓根宽值男性大于女性。ALAM等[22]分析了49例巴基斯坦人的220块腰椎CT图像,发现男性直径较大,女性角度更大。GüLE?等[23]研究了土耳其人群的腰椎结果,发现椎弓根宽、椎弓根高和椎弓根长随性别、年龄和身高而变化;外偏角α随年龄变化,不随性别或身高变化,没有发现α值在不同性别上的差异。美国人群的503具尸体测量结果表明,椎弓根宽、椎弓根高男性均大于女性,男性身高较高、体质量较大则具有较大的腰椎椎弓根[24]。椎弓根的大小随着年龄的增长而增加;在女性则相反[25],此次研究却发现2组结果中女性发育快于男性,尤其是椎弓根宽。选择合适的椎弓根螺钉时应考虑到这些差异,年龄和性别是正确选择合适椎弓根螺钉的特殊变量。 椎弓根尺寸受到遗传和种族的差异[26]。ALBAN等[27]研究发现,椎弓根宽,L1黑人最大(7.73 mm),亚洲人最小 (5.98 mm);L2,黑人、亚洲人最大(7.90 mm和7.32 mm);L3-L5,白种人最大(9.42 mm,11.32 mm,14.73 mm),亚洲人最小(8.79 mm,10.5 mm,14.05 mm)。STOCKTON等[28]报道,α角在L2中,白种人>黄种人>黑人和西班牙人。在L3,黄种人>黑人和西班牙人。亚洲人的腰椎椎弓根明显小于黑人或白人,与TSE等[29]的研究一致。 KIM等[13]和TAN等[30]报道韩国人和华裔新加坡人的椎弓根尺寸小于欧洲人。CHADHA等[31]和ACHARYA等[32]报道白人的椎弓根尺寸明显大于印度人。CHARLES等[33]得出结论,椎弓根的总体尺寸随着年龄增长。MCLAIN等[34]发现,椎弓根的大小受性别或种族影响,椎弓根的大小与个体的身高成比例。这可以解释为什么在目前的研究中,东方人椎弓根的尺寸比西方人群要小。CACCIOLA等[21]指出,椎弓根尺寸小,神经根结构更接近椎弓根,这也可能是腰椎稳定手术中椎弓根螺钉错位的一个重要危险因素。 "

| [1] PUTZIER M, STRUBE P, CECCHINATO R, et al. A new navigational tool for pedicle screw placement in patients with severe scoliosis: a pilot study to prove feasibility, accuracy, and identify operative challenges. Clin Spine Surg. 2017; 30: E430-E439. [2] FARSHAD M, BETZ M, FARSHAD-AMACKER NA, et al. Accuracy of patient-specific templateguided vs. free-hand fluoroscopically controlled pedicle screw placement in the thoracic and lumbar spine: a randomized cadaveric study. Eur Spine J. 2017; 26: 738-749. [3] HU Y, YUAN Z, SPIKER WR, et al. Deviation analysis of C2 translaminar screw placement assisted by a novel rapid prototyping drill template: a cadaveric study. Eur Spine J.2013; 22: 2770-2776. [4] HU QF, XU RM, PAN H, et al. Translaminar screw fixation in the upper thoracic spine: computed tomography-based quantitative laminar analysis and feasibility study of translaminar virtual screw placement. Cell Biochem Biophys. 2015; 73: 191-198. [5] DZIERŻANOWSKI J, SKOTARCZYK M, BACZKOWSKA-WALISZEWSKA Z, et al. Morphometric analysis of the lumbar vertebrae concerning the optimal screw selection for transpedicular stabilization. Adv Med Med Res. 2019; 11(33):83-96. [6] MAALY MA, SAAD A, HOULEL MEE. Morphological measurements of lumbar pedicles in Egyptian population using computerized tomography and cadaver direct caliber measurements. Egypt J Radiol Nucl Med. 2010;41(4): 475-481. [7] MOHANTY SP, KANHANGAD MP, BHAT SN, et al. Morphometry of the lower thoracic and lumbar pedicles and its relevance in pedicle fixation. Musculoskelet Surg. 2018; 102(3): 299-305. [8] LOTFINIA I, HADDADI K, SAYYAHMELLI S. Computed tomographic evaluation of pedicle dimension and lumbar spinal canal. Neurosurg Quart. 2010;20(3): 194-198. [9] SANI HY. The morphometric description of the thoracic and lumbar vertebral pedicles in European, African and mixed population of South Africa. The Faculty of Health Sciences, University of the Witwatersrand, Johannesburg,2018. [10] MUGHIR AMA, YUSOF MI, ABDULLAH S, et al. Morphological comparison between adolescent and adult lumbar pedicles using computerised tomography scanning. Surg Radiol Anat. 2010; 32(6): 587-592. [11] NOJIRI K, MATSUMOTO M, CHIBA K, et al. Morphometric analysis of the thoracic and lumbar spine in Japanese on the use of pedicle screws. Surgical and Radiologic Anatomy, 2005; 27(2): 123-128. [12] MITRA SR, DATIR SP, JADHAV SO. Morphometric study of the lumbar pedicle in the Indian population as related to pedicular screw fixation. Spine. 2002;27(5):453-459. [13] KIM NH, LEE HM, CHUNG IH, et al. Morphometric study of the pedicles of thoracic and lumbar vertebrae in Koreans. Spine. 1994;19(12): 1390-1394. [14] 戚力升,李森,谢明忠,等.腰椎椎弓根形态学研究及相关因素分析[J].西南医科大学学报,2018,41(6):541-545. [15] WANG X, ZHANG SJ, ZHANG YZ, et al. Three-dimensional digitizing and anatomic study of lumbar vertebral canal and pedicle in children. Wideochir Inne Tech Maloinwazyjne. 2018;13(4): 518-524. [16] GRIVAS TB, SAVVIDOU O, BINOS S, et al. Morphometric characteristics of the thoracοlumbar and lumbar vertebrae in the Greek population: a computed tomography-based study on 900 vertebrae-“Hellenic Spine Society (HSS) 2017 Award Winner”. Scoliosis Spinal Disord. 2019;14(1):1-12. [17] KADIOGLU HH, TAKCI E, LEVENT A, et al. Measurements of the lumbar pedicles in the Eastern Anatolian population. Surg Radiol Anat. 2003;25(2): 120-126. [18] 张军. 腰椎经皮椎弓根螺钉进钉点优化的体外研究[D].上海:上海交通大学,2017. [19] CACCIOLA G, ANASTASI G, BERTINO S, et al. Anatomical differences in the bony structure of L5 and L4: A possible classification according to the lateral tilt of the pedicles. J Orthop. 2018;15(1): 205-209. [20] ÇAPAR B, KARAGÜVEN D, BENLI İT, et al. Morphometric analysis of thoracolumbar pedicle dimensions of the adolescent and adult age groups. Turkish Spinal Surg. 2012; 23(4):19-26. [21] AZAR N, AKMAN YE, YALÇINKAYA M, et al. L5 vertebral mor phometric characteristics of Turkish society. Turk Spinal Surg. 2008; 19(7): 373-380. [22] ALAM MM, WAQAS M, SHALLWANI H, et al. Lumbar morphometry: a study of lumbar vertebrae from a Pakistani population using computed tomography scans. Asian Spine J. 2014;8(4):421-426. [23] GÜLEÇ A, KAÇIRA BK, KÜTAHYA H, et al. Morphometric analysis of the lumbar vertebrae in the Turkish population using three-dimensional computed tomography: correlation with sex, age, and height. Folia Morphologica. 2017;76(3): 433-439. [24] CHARLES CY, YUH RT, BAJWA NS, et al. Pedicle morphometry of lumbar vertebrae: male, taller, and heavier specimens have bigger pedicles. Spine. 2015;40(21): 1639-1646. [25] MORALES AVALOS R, LEYVA VILLEGAS J, SÁNCHEZ MEJORADA G, et al. Age-and gender-related variations in morphometric characteristics of thoracic spine pedicle: A Study of 4,800 Pedicles. Clin Anat. 2014;27(3): 441-450. [26] MERLOZ P, TONETTI J, PITTET L, et al. Pedicle screw placement using image guided techniques. Clin Orthop Relat Res. 1998;354: 39-48. [27] ALBANO J, LENTZ J, STOCKTON R, et al. Demographic Analysis of Lumbar Pedicle Diameters in a Diverse Population. Asian Spine J. 2019;13(3): 410. [28] STOCKTON R, ALBANO J, LENTZ J, et al. A comparison of lumbar transverse pedicle angles between ethnic groups: a retrospective review. BMC Musculoskelet Disord. 2019;20(1): 114-121. [29] TSE MSH, CHAN CH, WONG KK, et al. Quantitative anatomy of C7 vertebra in Southern Chinese for insertion of lateral mass screws and pedicle screws. Asian Spine J. 2016;10(4): 705-710. [30] TAN SH, TEO EC, CHUA HC. Quantitative three-dimensional anatomy of cervical, thoracic and lumbar vertebrae of Chinese Singaporeans. Eur Spine J. 2004;13(2): 137-146. [31] CHADHA M, BALAIN B, MAINI L, et al. Pedicle morphology of the lower thoracic, lumbar, and S1 vertebrae: an Indian perspective. Spine. 2003; 28(8): 744-749. [32] ACHARYA S, DORJE T, SRIVASTAVA A. Lower dorsal and lumbar pedicle morphometry in Indian population: a study of four hundred fifty vertebrae. Spine. 2010;35(10): E378-E384. [33] CHARLES CY, BAJWA NS, TOY JO, et al. Pedicle morphometry of upper thoracic vertebrae: an anatomic study of 503 cadaveric specimens. Spine. 2014;39(20): E1201-E1209. [34] MCLAIN RF, FERRARA L, KABINS M. Pedicle morphometry in the upper thoracic spine: limits to safe screw placement in older patients. Spine. 2002; 27(22): 2467-2471. [35] PERDOMO-PANTOJA A, ISHIDA W, ZYGOURAKIS C, et al. Accuracy of Current Techniques for Placement of Pedicle Screws in the Spine: A Comprehensive Systematic Review and Meta-Analysis of 51,161 Screws. World Neurosurg. 2019;23(2):1-15. [36] KOBAYASHI K, ANDO K, ITO K, et al. Intraoperative radiation exposure in spinal scoliosis surgery for pediatric patients using the O-arm® imaging system. Eur J Orthop Surg Traumatol. 2018; 28(4): 579-583. [37] PITTELOUD N, GAMULIN A, BAREA C, et al. Radiation exposure using the O-arm® surgical imaging system. Eur Spine J. 2017; 26(3): 651-657. [38] ZHU W, SUN W, XU L, et al. Minimally invasive scoliosis surgery assisted by O-arm navigation for Lenke Type 5C adolescent idiopathic scoliosis: a comparison with standard open approach spinal instrumentation. J Neurosurg. 2017; 19(4):472-478. [39] SIDDIQUI MI, WALLACE DJ, SALAZAR LM, et al. Robot-assisted pedicle screw placement: learning curve experience. World Neurosurg, 2019;107(6).E1-E6. [40] CHUA M J, SIDDIQUI S, YU C S, et al. The optimal screw length of lumbar pedicle screws during minimally invasive surgery fixation: a computed tomography-guided evaluation of 771 screws. Asian Spine J. 2019;76(2):1-6. [41] LAI DM, SHIH YT, CHEN YH, et al. Effect of pedicle screw diameter on screw fixation efficacy in human osteoporotic thoracic vertebrae. J Biomech. 2018;70(6):196-203. [42] VARGHESE V, KUMAR GS, KRISHNAN V. Effect of various factors on pull out strength of pedicle screw in normal and osteoporotic cancellous bone models. Med Eng Phys. 2017; 40(8):28-38. [43] MATSUKAWA K, YATO Y, IMABAYASHI H, et al. Biomechanical evaluation of fixation strength among different sizes of pedicle screws using the cortical bone trajectory: what is the ideal screw size for optimal fixation? Acta Neurochirurgica. 2016; 158(3): 465-471. [44] HIRANO T, HASEGAWA K, TAKAHASHI H E, et al. Structural Characteristics of the Pedicle and Its Role in Screw Stability. Spine. 1997; 22(21):2504-2510. [45] LI X, WANG X, GAO S, et al. Computed tomography measurement of the bone matrix of vertebral pedicle and its clinical significance. Folia Morphologica. 2019;21(1):1-11. [46] LIU K, ZHANG Q, LI X, et al. Preliminary application of a multi-level 3D printing drill guide template for pedicle screw placement in severe and rigid scoliosis. Eur Spine J. 2017; 26(8): 1684-1689. [47] SOLITRO GF, WHITLOCK K, AMIROUCHE F, et al. Currently Adopted Criteria for Pedicle Screw Diameter Selection. Int J Spine Surg. 2019; 13(4): 132-145. [48] HELGESON MD, KANG DG, HELGESON MD, et al. Tapping insertional torque allows prediction for better pedicle screw fixation and optimal screw size selection.Spine J.2013;13(8): 957-965. [49] STOCKTON R, ALBANO J, LENTZ J, et al. A comparison of lumbar transverse pedicle angles between ethnic groups: a retrospective review. BMC Musculoskelet Disord. 2019; 20(12):114-124. [50] GARFIN SR, EISMONT FJ, BELL GR, et al. Rothman-Simeone and Herkowitz’s the Spine 7th edition. 2017;28(1):360-370. |
| [1] | Liu Yafei, Wang Yalin, Zuo Yanping, Sun Qi, Wei Jing, Zhao Lixia. Structural changes of the temporomandibular joint in adolescents with skeletal Class III malocclusions after maxillary protraction: an X-ray measurement analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1154-1159. |
| [2] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [3] | Hu Jing, Xiang Yang, Ye Chuan, Han Ziji. Three-dimensional printing assisted screw placement and freehand pedicle screw fixation in the treatment of thoracolumbar fractures: 1-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3804-3809. |
| [4] | Zou Shouping, Lu Daoyun, Ye Li. Minimally invasive percutaneous pedicle screw technique for thoracolumbar fractures: biomechanical changes of the spine during 6-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3865-3869. |
| [5] | Wei Yuanbiao, Guo Huizhi, Zhang Shuncong. Finite element analysis of cortical bone trajectory screw fixation on adjacent segments [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2799-2804. |
| [6] | Qu Xingyue, Zhou Jianqiang, Xu Xuebin, Zhang Shaojie, Li Zhijun, Wang Xing. Finite element analysis of screw-bone anti-pullout in four models of anterior lower cervical fixation in children [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2816-2821. |
| [7] | Xue Jingbo, Zhu Bin, Li Zepeng, Wang Cheng, Ouyang Zhihua, Yan Yiguo. Biomechanical characteristics of a sleeve-type guided growth rod in a six-degree-of-freedom joint robot [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2297-2302. |
| [8] |
Zhang Cong, Zhao Yan, Du Xiaoyu, Du Xinrui, Pang Tingjuan, Fu Yining, Zhang Hao, Zhang Buzhou, Li Xiaohe, Wang Lidong.
Biomechanical analysis of the lumbar spine and pelvis in adolescent
idiopathic scoliosis with lumbar major curve |
| [9] | He Yujie, Wang Haiyan, Li Zhijun, Li Xiaohe, Cai Yongqiang, Dai Lina, Xu Yangyang, Wang Yidan, Xu Xuebin. Digital measurements of the anatomical parameters of pedicle-rib unit screw fixation in thoracic vertebrae of preschoolers [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(6): 869-876. |
| [10] |
Liu Lu, Wang Xing, Kang Xiaoyan, Li Guihua, Li Xiaohe, Gao Shang, Cai Yongqiang, Zhang Shaojie, Li Zhijun.
Digital three-dimensional morphology of cervical joint facet in 7-12-year-old children |
| [11] | Luo Peijie, Yuan Kai, Li Daxing, Zhang Shuncong, Guo Huizhi, Tang Yongchao, Zhou Tengpeng, Guo Danqing, Li Yongxian, Mo Guoye. Comparison of the short-segment and long-segment cement-augmented pedicle screw fixation for osteoporotic thoracolumbar fracture: a finite element study [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 342-347. |
| [12] | Sun Jian, Fang Chao, Gao Fei, Wei Laifu, Qian Jun. Clinical efficacy and complications of short versus long segments of internal fixation for the treatment of degenerative scoliosis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 438-445. |
| [13] | Gao Yangyang, Che Xianda, Han Pengfei, Liang Bin, Li Pengcui. Accuracy of robot-assisted and fluoroscopy-guided pedicle screw placement: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(3): 446-452. |
| [14] | Chen Shengguo, Yang Wenqing, Jia Long, Maerhaba•Tuerdihuojia, Wang Shuiquan, Bai Xin, Dong Jianjiang, Kaisaierjiang • Duolaiti, Nuermaimaiti • Bahaxiaer. Morphological traits in the head and face of Kazakh adults in Yili, Xinjiang [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(29): 4702-4708. |
| [15] | Hou Jichun, Cao Yang. Biomechanical characteristics of transforaminal lumbar interbody fusion combined with different pedicle screw fixation methods in single-segment lumbar spine and adjacent segments [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(27): 4297-4304. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||