Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (12): 1957-1961.doi: 10.3969/j.issn.2095-4344.2518
Previous Articles Next Articles
Research and development of fluoroscopy for the detection of dorsal screw penetration in the fixation of distal radius fracture with volar locking plate
Wang Haonan1, Wen Shuzheng2, Wang Jihong2, Hao Zengtao2, Fan Dongsheng2, Jing Shangfei2, Han Chaoqian2, Wang Yongfei2, Wang Xiaolong2, Yin Chao2, Jiang Dong2
- 1Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China; 2Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China
-
Received:2019-07-27Revised:2019-07-31Accepted:2019-10-15Online:2020-04-28Published:2020-03-03 -
Contact:Wen Shuzheng, Professor, Second Affiliated Hospital of Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China -
About author:Wang Haonan, Inner Mongolia Medical University, Hohhot 010030, Inner Mongolia Autonomous Region, China
CLC Number:
Cite this article
Wang Haonan, Wen Shuzheng, Wang Jihong, Hao Zengtao, Fan Dongsheng, Jing Shangfei, Han Chaoqian, Wang Yongfei, Wang Xiaolong, Yin Chao, Jiang Dong. Research and development of fluoroscopy for the detection of dorsal screw penetration in the fixation of distal radius fracture with volar locking plate[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(12): 1957-1961.
share this article
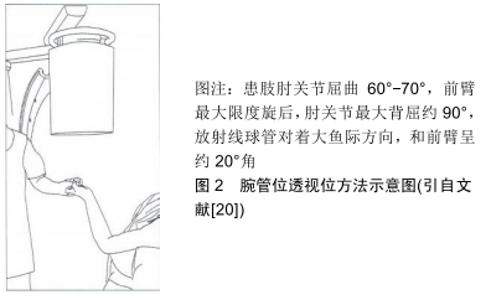
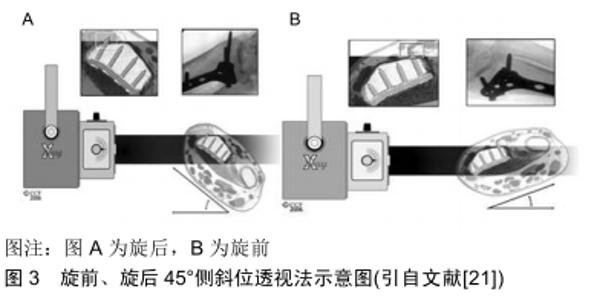
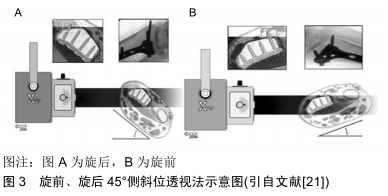
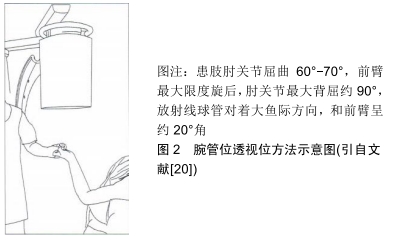
2.1 标准正、侧位方法 正位透视采用后前位;侧位透视采用纯侧位,即第三掌骨的长轴与桡骨远端的长轴共轴平行,此时豌豆骨叠加于舟骨远极。 2.2 腕管位透视法 MARSLAND等[18]描述了一种腕关节在完全背屈下进行透视的方法,并称之为腕管位透视。在其报道的42例患者中,与标准侧位透视图像相比,腕管位透视可以更准确地评估螺钉穿出长度,从而使术中螺钉更换率达到17%(7/42)。事实上术中进行背侧螺钉穿出长度的精确测量是非常困难的[19]。MARSLAND等[18]进行的试验表明,对于穿出长度>2 mm的螺钉,腕管位透视方法能够有效发现其是否穿出背侧骨皮质。 遗憾的是这种透视方法往往需要多次调整患肢位置及术中透视角度才能取得满意的图像,这不仅增加了手术时间,同时也增加了医护人员放射线暴露的机会。因此,作者认为这种方法对于这一类型骨折患者有一定的帮助,但是也为患者及医护人员带来一些健康问题。 2.3 改良腕管位透视法 刘涛等[20]在最近的一项临床试验中应用了改良腕管位透视法来检测桡骨远端骨折时掌侧锁定钢板内固定后背侧螺钉穿出长度,见图2。试验结果表明,标准正、侧位透视发现5例患者螺钉穿出背侧皮质(10.4%,5/48),改良腕管位透视法发现包括上述5例在内的16例患者螺钉穿出背侧皮质(33.3%,16/48),2种透视方法检出率的差异有显著性意义;另外有2例患者螺钉进入下尺桡关节,且仅在改良腕管位透视法中发现。刘涛等[20]认为与标准正、侧位透视方法相比较,改良腕管位透视法能可靠的探测到螺钉的背侧皮质穿出,并能对下尺桡关节提供良好的术中透视,从而尽可能减少背侧穿出螺钉过长导致背侧肌腱的激惹、磨损及断裂等的发生概率[20]。 "
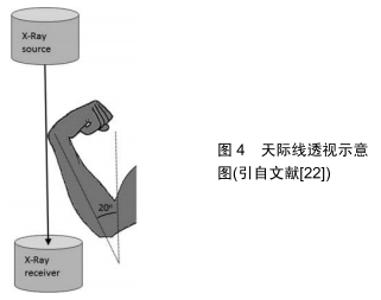
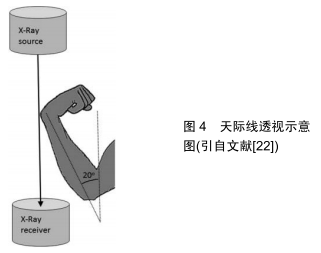
但是这种方法对于螺钉穿出桡骨远端背侧骨皮质<2 mm的螺钉的检出率仍效果不佳,因此作者认为该方法对于将螺钉穿出长度控制在<2 mm方面有一定的作用,但是尚不能非常有效的将螺钉长度完全控制在背侧骨皮质内。 2.5 天际线透视法 PICHLER等[22]最近描述了一种术中检测背侧皮质穿出长度的方法,并称为天际线透视图像。在试验中通过对30个标本的前臂进行三维计算后,进行扫描矢状面CT切片检测到Lister结节的最高峰值。为了量化最高峰值,其在垂直于轴的方向上测量结节尖端和桡骨掌侧表面之间的距离。事实证明,Lister结节的存在和变异会引起术中X射线透视的差异。 RIDDICK等[23]在最近的一项研究中证实检测螺钉是否穿出背侧皮质时,天际线透视比标准侧位更灵敏和准确,见图4。RIDDICK等[23]文献报道中表明,天际线视图在探测到仅1 mm长的背侧皮质螺钉时的灵敏度为83%。因此,如果螺钉较长,则其灵敏度可能更高。同时他们发现,使用天际线透视检测放置在桡骨远端尺侧的螺钉是否穿出骨皮质时,灵敏度高达90%。而标准侧位显示放置到尺侧区域螺钉的穿透性,其敏感性为75%[19]。 "
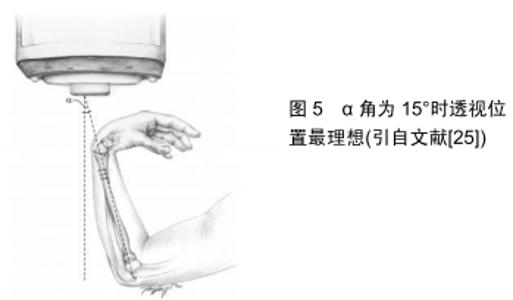
尽管SOONG等[24]的研究结果表明,桡骨远端骨折时掌侧锁定钢板内固定后背侧伸肌腱的激惹、磨损及断裂等是现代掌侧钢板治疗时不常见的并发症。但是如果发生,将会严重影响患者的腕部功能,同时为患者的生活及经济等方面带来一定的困扰。因此,在桡骨远端骨折掌侧钢板内固定过程中,天际线透视应作为检测背侧皮质螺钉穿出的一种方法[22]。 2.6 背侧切线视图法 HAUG等[25]报道了一项关于背侧切线透视方法的实验,见图5。实验中采用6具尸体的前臂,进行掌侧锁定钢板内固定后,使用背侧切线透视方法图像采集,同时在直视下观测背侧螺钉是否穿出并测量穿出螺钉的长度。结果表明,直视下测量的实际背侧螺钉穿出长度与背侧切线透视图像中测量的螺钉长度之间具有统计学意义的相关性。对于穿透背侧骨皮质2 mm的螺钉,两者相关性的统计显著性显示为肘部半径从5°-20°的倾斜角度。在倾斜度为15°时发现了最高的相关性,并且检测到除了1个螺钉以外的所有螺钉都太长。 "
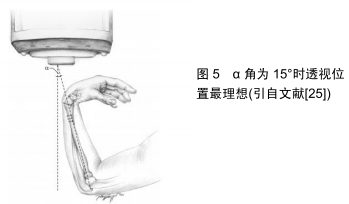
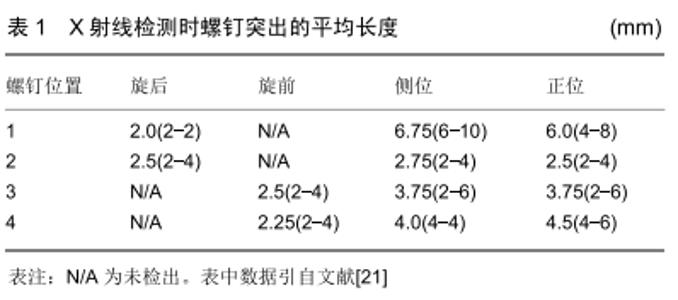
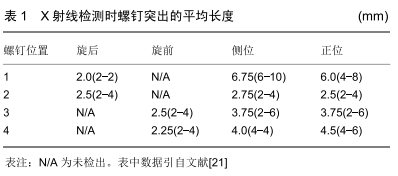
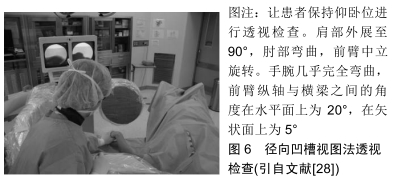
在掌侧锁定钢板内固定过程中,从背侧应用背侧切线透视方法检测桡骨远端螺钉时,可以使螺钉穿出背侧骨皮质的长度最小。HAUG等[25]得出的结论:理想的肘关节弯曲半径倾角为15°,可以获得最好的透视图像,有助于预防腕背侧伸肌腱激惹、磨损及断裂等并发症的发生。但作者发现该研究是基于尸体标本,还需要进一步的临床研究来验证这种放射技术的可行性。而且在临床实践中,准确地确定15°倾角是一个难题。 JOSEPH等[26]近期进行了一项临床试验,对15例桡骨远端骨折患者使用掌侧锁定钢板进行骨折固定,在手术中通过使用背侧切线透视作为最后检查背侧皮质螺钉突出的长度。为了获得背侧视野,手腕过度弯曲,透视装置的光束沿桡骨纵轴方向移动。术中通过该透视方法有4例患者共有4枚螺钉穿出,并在术中进行更换。被发现的4枚螺钉平均突出长度为2.25 mm,且仅在该透视图像上被发现。JOSEPH等[26]认为背侧切线透视方法提供了确定桡骨远端骨折掌侧锁定钢板内固定中确定螺钉穿出背侧皮质的新方法。因此在桡骨远端骨折时进行骨内固定时,利用背侧切线透视是一种有效的辅助手段,可预防螺钉穿出于背侧皮质之外。OZER等[27]在最近的一项报道中也证实了背侧切线视图是一种能够提高透视诊断准确率的简单方法。 作者认为,由于JOSEPH等[26]在临床试验中不能对15例患者的桡骨远端背侧进行直视下观测,所以在这组患者中,螺钉穿出的真实发生率可能更高。同时作者也发现该报道中未指出腕关节屈曲角度,因此在临床实践中可能需要手术医师多次调整腕关节才能获得较为可靠的图像,这同样增加了医护人员放射线暴露的机会。 2.7 径向凹槽视图法 LEE等[28]在最近的文献报道中提出了一种新的术中透视方法,他们将其命名为“径向凹槽视图”,见图6。文献报道中指出,LEE等[28]使用径向凹槽视图法在93例骨折患者中检测到13例(14%)腕背侧螺钉突出到凹槽中。在术中更换较短的螺钉后,未发现螺钉在X射线片上突出。统计学评估得出术中使用径向沟槽视图在桡骨远端骨折的掌侧锁定钢板内固定治疗后检测拇长伸肌腱沟槽中的突出螺钉的灵敏度为92.8%(95%CI:91.3-98.4),因此他们建议术中使用该透视技术,避免桡骨远端骨折时掌侧锁定钢板内固定后螺钉穿出背侧骨皮质,预防腕背侧伸肌腱的激惹、磨损及断裂等并发症的发生。 "
| [1] COURT-BROWN CM, CAESAR B. Epidemiology of adult fractures: A review. Injury. 2006;37(8):691-697. [2] MCKAY SD, MACDERMID JC, ROTH JH, et al. Assessment of complications of distal radius fractures and development of a complication checklist. J Hand Surg. 2001;26(5):916-922. [3] JUPITER JB, FERNANDEZ DL, TOH CL, et al. Operative treatment of volar intra-articular fractures of the distal end of the radius. J Bone Joint Surg. 1997;78(12):1817-1828. [4] BENSON EC, DECARVALHO A, MIKOLA EA, et al. Two potential causes of epl rupture after distal radius volar plate fixation. Clin Orthop Relat Res. 2006;451(451):218-222. [5] WOODEN G. Computer tomography aided 3D analysis of the distal dorsal radius surface and the effects on volar plate osteosynthesis. J Hand Surg Eur Vol. 2009; 34(5):598-602. [6] LICHTMAN DM, BINDRA RR, BOYER MI, et al. Treatment of distal radius fractures. J Am Acad Orthop Surg. 2010;18(3):180-189. [7] LIPORACE FA, ADAMS MR, CAPO JT, et al. Distal radius fractures. J Orthop Trauma. 2009;23(10):739-748. [8] KAMANO M, KOSHIMUNE M, TOYAMA M, et al. Palmar plating system for Colles’ fractures: a preliminary report. J Hand Surg Am. 2005;30:750-755. [9] SIMIC PM, ROBISON J, GARDNER MJ, et al. Treatment of distal radius fractures with a low-profile dorsal plating system: an outcomes assessment. J Hand Surg Am. 2006;31:382-386. [10] PERRY DC, MACHIN DM, CASALETTO JA, et al. Minimising the risk of extensor pollicis longus rupture following volar plate fixation of distal radius fractures: a cadaveric study. Ann R Coll Surg Engl. 2011;93: 57-60. [11] BENSON EC, DECARVALHO A, MIKOLA EA, et al. Two potential causes of EPL rupture after distal radius volar plate fixation. Clin Orthop Relat Res 2006;451:218-222. [12] RAMPOLDI M, MARSICO S. Complications of volar plating of distal radius fractures. Acta Orthop Belg. 2007;73:714-719. [13] BIANCHI S, VAN AAKEN J, GLAUSER T, et al. Screw impingement on the extensor ten dons in distal radius fractures treated by volar plating: sonographic appearance. AJR Am J Roentgenol. 2008;191:199-203. [14] ARORA R, LUTZ M, HENNERBICHLER A, et al. Complications following internal fixation of unstable distal radius fracture with a palmar locking-plate. J Orthop Trauma. 2007;21:316-322. [15] MCKAY SD, MACDERMID JC, ROTH JH, et al. Assessment of complications of distal radius fractures and development of a complication checklist. J Hand Surg Am. 2001;26:916-922. [16] ROZENTAL TD, BLAZAR PE. Functional outcome and complications after volar plating for dorsally displaced, unstable fractures of the distal radius. J Hand Surg Am. 2006;31:359-365. [17] MEYER C, CHANG J, STERN P, et al. Complications of distal radial and scaphoid fracture treatment. J Bone Joint Surg Am. 2013;95(16): 1517-1526. [18] MARSLAND D, HOBBS CM, SAUVÉ PS. Volar locking plate fixation of distal radius fractures: use of an intra-operative 'carpal shoot through' view to identify dorsal compartment and distal radioulnar joint screw penetration. Hand (N Y). 2014;9(4):516-521. [19] THOMAS AD, GREENBERG JA. Use of fluoroscopy in determining screw overshoot in the dorsal distal radius: a cadaveric study. J Hand Surg. 2009;34A:258-261. [20] 刘涛,亢世杰,黄东生,等.腕管位透视法在桡骨远端骨折掌侧接骨板固定术中的应用价值[J].中华骨科杂志, 2017,37(12):721-727. [21] MASCHKE SD, EVANS PJ, SCHUB D, et al. Radiographic evaluation of dorsal screw penetration after volar fixed-angle plating of the distal radius: a cadaveric study. Hand (New York). 2007;2(3):144-150. [22] PICHLER W, WINDISCH G, SCHAFFLER G, et al. Computer tomography aided 3D analysis of the distal dorsal radius surface and the effects on volar plate osteosynthesis. J Hand Surg Eur. 2009; 34: 598-602. [23] RIDDICK AP , HICKEY B , WHITE SP. Accuracy of the skyline view for detecting dorsal cortical penetration during volar distal radius fixation. J Hand Surg (European Volume). 2012;37(5):407-411. [24] SOONG M, VAN LEERDAM R, GUITTON TG, et al. Fracture of the distal radius: Risk factors for complications after locked volar plate fixation. J Hand Surg Am. 2011;36: 3-9. [25] HAUG LC, GLODNY B, DEML C, et al. A new radiological method to detect dorsally penetrating screws when using volar locking plates in distal radial fractures. The dorsal horizon view. Bone Joint J. 2013; 95-B(8):1101-1105. [26] JOSEPH SJ, HARVEY JN. The dorsal horizon view: detecting screw protrusion at the distal radius. J Hand Surg Am. 2011;36(10):1691-1693. [27] OZER K, WOLF JM, WATKINS B, et al. Comparison of 4 fluoroscopic views for dorsal cortex screw penetration after volar plating of the distal radius. J Hand Surg. 2012;37(5):963-967. [28] LEE SK, BAE KW, CHOY WS. Use of the radial groove view intra-operatively to prevent damage to the extensor pollicis longus tendon by protruding screws during volar plating of a distal radial fracture. Bone Joint J. 2013; 95-B(10):1372-1376. [29] CLEMENT H, PICHLER W, NELSON D, et al. Morphometric analysis of lister's tubercle and its consequences on volar plate fixation of distal radius fractures. J Hand Surg Am. 2008;33:1716-1719. [30] WALL LB, BRODT MD, SILVA MJ, et al. The effects of screw length on stability of simulated osteoporotic distal radius fractures fixed with volar locking plates. J Hand Surg Am. 2012;37:446-453. [31] AL-RASHID M, THEIVENDRAN K, CRAIGEN MA. Delayed ruptures of the extensor tendon secondary to the use of volar locking compression plates for distal radial fractures. J Bone Joint Surg [Br].2006;88-B: 1610-1612. [32] PICHLER W, WINDISCH G, SCHAFFLER G, et al. Computer tomography aided 3D analysis of the distal dorsal radius surface and the effects on volar plate osteosynthesis. J Hand Surg Eur Vol.2009;34: 598-602. |
| [1] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [2] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [3] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [4] | Zhang Shangpu, Ju Xiaodong, Song Hengyi, Dong Zhi, Wang Chen, Sun Guodong. Arthroscopic suture bridge technique with suture anchor in the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1417-1422. |
| [5] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [6] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [7] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [8] | Xu Yulin, Shen Shi, Zhuo Naiqiang, Yang Huilin, Yang Chao, Li Yang, Zhao Heng, Zhao Lu. Biomechanical comparison of three different plate fixation methods for acetabular posterior column fractures in standing and sitting positions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 826-830. |
| [9] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [10] | He Li, Tian Wei, Xu Song, Zhao Xiaoyu, Miao Jun, Jia Jian. Factors influencing the efficacy of lumbopelvic internal fixation in the treatment of traumatic spinopelvic dissociation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 884-889. |
| [11] | Yang Weiqiang, Ding Tong, Yang Weike, Jiang Zhengang. Combined variable stress plate internal fixation affects changes of bone histiocyte function and bone mineral density at the fractured end of goat femur [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 890-894. |
| [12] | Zhang Lei, Ma Li, Fu Shijie, Zhou Xin, Yu Lin, Guo Xiaoguang. Arthroscopic treatment of greater tuberosity avulsion fractures with anterior shoulder dislocation using the double-row suture anchor technique [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 895-900. |
| [13] | Yuan Xinping, Shao Yanbo, Wu Chao, Wang Jianling, Tong Liangcheng, Li Ying. Accuracy of target bone segments in personalized differential modeling and simulation of CT scanning parameters at fracture end [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 912-916. |
| [14] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [15] | Kong Lingbao, Lü Xin. Effect of implant selection and approach on support in the operation of posterolateral tibial plateau fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 942-947. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||