Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (38): 6184-6188.doi: 10.3969/j.issn.2095-4344.2014.38.020
Previous Articles Next Articles
An adaptation to changes in knee muscle strength is a basic principle for rehabilitation after anterior cruciate ligament reconstruction
Chen Jian
- Center of Physical Fitness, School of Health Science, Wuhan Institute of Physical Education, Wuhan 430079, Hubei Province, China
-
Received:2014-08-22Online:2014-09-10Published:2014-09-10 -
About author:Chen Jian, M.D., Associate professor, Center of Physical Fitness, School of Health Science, Wuhan Institute of Physical Education, Wuhan 430079, Hubei Province, China
CLC Number:
Cite this article
Chen Jian. An adaptation to changes in knee muscle strength is a basic principle for rehabilitation after anterior cruciate ligament reconstruction[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(38): 6184-6188.
share this article
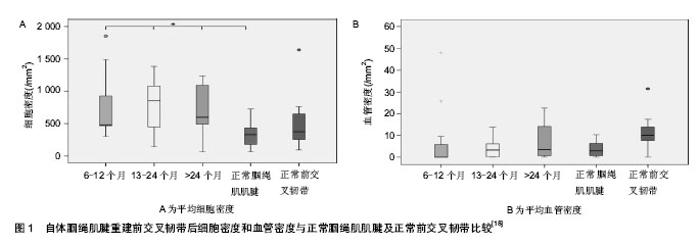
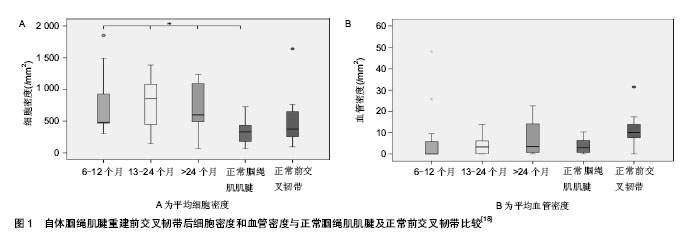
2.1 前交叉韧带重建后肌力变化与评价的研究进展 2.1.1 前交叉韧带重建后肌力的改变 过去认为自体腘绳肌腱重建前交叉韧带后,腘绳肌腱组织能够再生并可恢复良好的功能,因此对腘绳肌的功能影响很小。但最近越来越多的研究表明:切取腘绳肌腱会导致术后的屈膝肌力和胫骨内旋肌力的降低,从而影响膝关节的稳定性和功能活动水平[1-2]。有研究表明,前交叉韧带重建后前3周患侧股四头肌体积即减小25%-33%[3],骨髌腱移植患者腘绳肌体积下降2%-3%,而半腱肌股薄肌移植患者腘绳肌体积下降7%-8%,且股薄肌体积呈持久下降(术后3周、15周和1年分别下降22%,37%,44%)。 Nakamura等[4]进一步研究了单纯切取半腱肌和同时切取半腱肌股薄肌重建前交叉韧带后对患侧屈膝肌力和胫骨内旋肌力的影响,结果表明:在屈膝90°时,半腱肌腱移植组和半腱肌腱加股薄肌腱移植组比较,两组的患侧屈膝肌肌力恢复在产生峰力矩的屈膝角度时较差;双膝屈肌峰力矩比值和屈膝90°时的屈肌力矩,两组间无显著差异。Adachi等[5]研究表明, 两组患者的峰力矩值和总功与正常膝关节无显著差异,但切取的腘绳肌腱越多,主动屈膝角度丧失越大,而且峰力矩角度变得越小,表明切取腘绳肌腱后导致屈膝末端时腘绳肌肌力的减弱(屈膝角度越大,峰力矩越小)。有研究表明:慢性前交叉韧带损伤患者损伤侧下肢股四头肌和腘绳肌峰力矩值显著降低[6],离心腘绳肌/离心股四头肌比率、向心腘绳肌/离心股四头肌比率均显著大于健侧下肢;然而,患侧下肢离心腘绳肌/向心股四头肌比率与健侧相近。这表明前交叉韧带损伤后,股四头肌的离心肌肉活动比其向心肌肉活动受到的影响更大。 keays等[7]对不同移植物重建前交叉韧带术后肌肉力量、关节稳定性、关节活动范围、关节功能水平及关节退变的效果进行了6年随访的研究,结果表明半腱肌重建组术后有较高的同侧再伤发生率,可能原因为肌力下降致本体感觉功能障碍。Tadokoro等[8]报道了用磁共振(magnetic resonance imaging,MRI)评价腘绳肌腱重建前交叉韧带后2年腘绳肌腱再生情况,并测定等速腘绳肌肌力和股四头肌肌力,结果发现,尽管MRI显示75%以上的患者有半腱肌腱再生,但不论腘绳肌腱是否有再生,手术侧下肢的等速腘绳肌肌力和股四头肌肌力均显著低于健侧下肢。Ristanis等[9]应用表面肌电图对比研究了自体腘绳肌重建前交叉韧带术后2年腘绳肌肌电变化后发现,与健侧相比患侧股二头肌和半腱肌电机械延迟(electromechanical delay,EMD)明显增加,屈膝肌的神经肌肉控制能力下降,从而影响运动员在急停急转时膝关节的稳定性。Ristanis等[10]也观察了自体腘绳肌重建前交叉韧带术后2年患者疲劳状态下电机械延迟的表现,结果显示疲劳导致患侧股二头肌和半腱肌电机械延迟增加,但对股二头肌和半腱肌收缩同步性没有影响。Georgoulis 等[11]研究了采用髌腱重建前交叉韧带患者术后伸膝肌电机械延迟,结果较术前没有变化。Muraoka等[12]研究表明肌腱松弛度是影响电机械延迟的重要因素之一。 2.1.2 前交叉韧带缺损后肌力的评价方法 目前,如何量化前交叉韧带重建后膝关节肌力变化成为制定康复程序的重要依据之一。已有的研究表明综合临床和等速肌力测试的结果,可以对前交叉韧带重建后的疗效进行综合评定,通过了解采用不同移植物重建前交叉韧带后的肌力缺陷情况来指导移植物供区的选择,更重要的是可据此调整术后康复计划,以纠正这些肌力不平衡,或将肌力不平衡降到最小程度[13]。Eitzen等[14]研究表明前交叉韧带损伤后等速力量评价应用特殊角度力矩值的曲线比传统应用峰力矩更能反映患者功能水平,因为前交叉韧带损伤后股四头肌力量下降在屈膝小于45°范围内更严重。 Hamstring/Quadriceps比率(H/Q,屈/伸比)的改变能够用于指导前交叉韧带损伤和手术后的康复,为提高前交叉韧带损伤后膝关节的稳定性提供理论依据。恢复或改变前交叉韧带损伤及韧带重建人群的H/Q比率,对运动员恢复高水平的运动能力和预防再损伤具有重要意义[15]。 近些年有学者提出了H/Q功能比率:动态肌力控制比率(dynamic control ratio,DCR)的概念,计算H/Q比率时,应当用膝关节动态运动中各个不同角度对应的离心腘绳肌肌力/向心股四头肌肌力比率来代表伸膝功能,向心腘绳肌肌力/离心股四头肌肌力比率代表屈膝功能,因为在动态运动过程中,当主动肌处于向心性收缩时拮抗肌为离心性收缩。这种H/Q比率符合实际运动中的膝关节功能, 更能反映膝关节屈肌和伸肌的协同收缩模式,前交叉韧带损伤患者术前与术后的肌力控制比率尚无正常值标准[16]。 Svensson等[17]采用MRI连续观察髌腱移植重建前交叉韧带术后髌腱再生情况,结果显示术后6年供区髌腱仍未恢复正常组织。Ristanis等[9]却发现半腱肌股薄肌重建前交叉韧带术后2年MRI显示取腱部位肌腱已完全再生,但腱组织性质可能发生改变而导致肌肉收缩延迟。 从以上研究结果可以看出,自体腘绳肌腱重建前交叉韧带术后患侧膝关节肌力明显下降,但评定指标、测试时间、测试结果均有所差异。如何在术后早期选择特异性的指标及评价手段进行分析还有待进一步研究。 2.2 前交叉韧带重建后肌力康复的研究进展 前交叉韧带重建后康复方案目前尚无统一的标准和方法,存在着许多争议。作者者认为由于重建时使用的材料及方法不同,故术后康复训练的措施也不尽相同。而无论何种方法,其功能练习的核心是如何解决前交叉韧带重建后“移植物和骨髓道良好的长入与尽早恢复关节功能及运动能力”这个矛盾,前交叉韧带重建后移植物腱骨愈合需经过4个阶段:缺血坏死、血管重建、细胞增殖和塑型成熟期。但腱骨愈合过程受移植物类型、骨道状况、患者年龄等诸多因素影响。 Janssen等[18]研究了自体腘绳肌腱重建前交叉韧带术后移植物塑形过程,结果表明:腘绳肌重建前交叉韧带移植物表现出典型的塑形阶段,一直持续2年尚未完成(图1),人类重塑持续时间相比其他动物实验研究更长。故在实施康复训练程序时应遵循个体化、渐进性、全面性三大原则,在基本康复训练原则的基础上根据个体功能水平及时做出相应的调整,充分体现个性化训练。 前交叉韧带重建后多年仍存在患侧肌力缺失10%-20%[3],从而影响患者功能活动和生活质量水平,因而促进肌力恢复是前交叉韧带重建后的重要康复目标之一。但前交叉韧带重建后肌力康复的开始时间、手段与方法、恢复运动的时机等尚无公认的标准程序。 Shelbourne[19]研究了不同髌腱宽度及术前股四头肌力量对自体同侧骨髌腱骨移植重建前交叉韧带术后肌力恢复的影响,结果表明髌腱宽度越小及术前股四头肌力量越弱的患者术后肌力恢复越差,尤其在术后第1年更为明显。 2.2.1 前交叉韧带重建后肌力康复的开始时间 目前,国内外研究均表明前交叉韧带重建术肌力康复始于重建手术之前,术前肌肉等长收缩练习能够使患者术后较快掌握不同肌肉的等长收缩练习方法,以尽早开始肌肉收缩的再训练从而最大程度地防止肌肉萎缩,但当前存在的分歧主要集中在早期训练的“度”的把握上[20]。Sekir等[21]对自体髌腱移植重建前交叉韧带术后等速训练开始时间早晚进行了对比研究,早期开始组自术后第3周开始屈膝40°-100°范围内股四头肌和腘绳肌向心性等速练习,晚期开始组则在术后第9周开始同样程序的等速力量训练,包括6种不同角速度[30,60,90,120,150,180,210,240 (°)/s],每种速度重复8次,组间休息20 s,于术后 1,2,3,4,12个月分别测试等速肌肉力量、IKDC评分,结果表明等速训练可以安全有效地恢复患侧肌力和功能活动水平。 2.2.2 前交叉韧带重建后肌力康复的手段 国外有研究表明:前交叉韧带术后3周即开始进行持续12周的离心性力量训练[3],MRI测量股四头肌和臀大肌横断面结果显示离心训练组股四头肌和臀大肌的肌肉体积增大25%,而标准康复组增大8%,1年后离心训练组较标准康复组股四头肌体积大50%,离心训练组中移植为半腱肌和股薄肌患者股四头肌和臀大肌肌肉体积分别增大27%和22%,而移植"
| [1] Armour T,Forwell L,Litchfield R,et al.Isokinetic evaluation of internal/external tibial rotation strength after the use of hamstring tendons for anterior cruciate ligament reconstruction. Am J Sports Med.2004;32(7):1639. |
| [1] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [2] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [3] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| [4] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [5] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [6] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| [7] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [8] | Ma Ziyue, Ju Xiaochen, Zhang Lei, Sun Rongxin. Tendon-bone healing in anterior cruciate ligament reconstruction with and without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 582-587. |
| [9] | Wang Weigang, Yang Zhidong, Feng Zongquan, Wang Ding. A mid-term clinical follow-up of unicompartmental knee arthroplasty with fixed bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 368-373. |
| [10] | Wang Xiaofei, Teng Xueren, Cong Linyan, Zhou Xu, Ma Zhenhua. Herbert screw internal fixation for treating adult osteochondritis dissecans of the knees [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 397-402. |
| [11] | Cheng Chongjie, Yan Yan, Zhang Qidong, Guo Wanshou. Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3921-3928. |
| [12] | Wang Dasai, Zhang Yang, Cheng Yin, Wang Qiang. Efficacy and safety of staged versus simultaneous unicompartmental knee arthroplasty: a meta-analysis#br# [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3929-3936. |
| [13] | Luo Anyu, Liu Hanlin, Xie Xiaofei, Huang Chen. Effect of antioxidant mixture on structural degeneration of an osteoarthritis rat model [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3625-3629. |
| [14] | Yu Yinghao, Zhao Jijun, Liu Dongcheng, Chen Yuhao, Feng Dehong. Clinical significance of preoperative planning assisted unicompartmental knee arthroplasty with digital imaging system for fixed-bearing prosthesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3324-3331. |
| [15] | Deng Zhibo, Li Zhi, Wu Yahong, Mu Yuan, Mu Yuexi, Yin Liangjun. Local infiltration anesthesia versus femoral nerve block for pain control and safety after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3401-3408. |
| Viewed | ||||||||||||||||||||||||||||||||||||||||||||||||||
|
Full text 277
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||
|
Abstract 352
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||