Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (6): 835-840.doi: 10.3969/j.issn.2095-4344.2014.06.003
Previous Articles Next Articles
Effects of alpha-zearalanol on the osteogenic differentiation of mouse bone marrow mesenchymal stem cells
Zou Bin1, Zong Shao-hui2, Zeng Gao-feng3, Fang Ye4, Gao Tai-hang4
- 1Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China; 2Department of Spinal Surgery, the First Affiliated Hospital of Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China; 3School of Public Health, Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China; 4Graduate School of Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China
-
Revised:2013-12-14Online:2014-02-05Published:2014-02-05 -
Contact:Zong Shao-hui, Professor, Department of Spinal Surgery, the First Affiliated Hospital of Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China -
About author:Zou Bin, Studying for master’s degree, Guangxi Medical University, Nanning 530021, Guangxi Zhuang Autonomous Region, China
CLC Number:
Cite this article
Zou Bin, Zong Shao-hui, Zeng Gao-feng, Fang Ye, Gao Tai-hang. Effects of alpha-zearalanol on the osteogenic differentiation of mouse bone marrow mesenchymal stem cells[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 835-840.
share this article
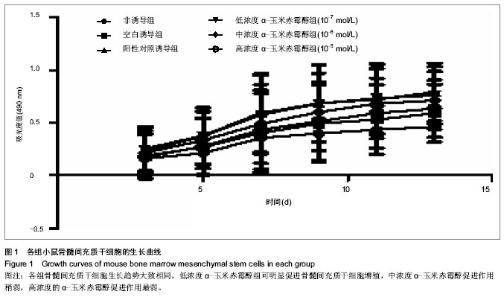
2.1 小鼠骨髓间充质干细胞原代培养和传代培养形态学特征 原代细胞约24 h已部分贴壁,呈透亮圆形,每3 d换液,不断弃除非贴壁细胞,三四天可见集落形成,单核,核仁清晰,短梭形。6-12 d贴壁的细胞伸展,逐渐形成形态较均一的长梭形细胞为主的集落并渐渐融合成片。传代细胞较原代细胞均一性好,呈均一的长梭形。原代及传代培养过程中,小鼠骨髓间充质干细胞均呈单层生长,有接触抑制现象。 2.2 α-玉米赤霉醇干预小鼠骨髓间充质干细胞的形态学变化 非诱导组骨髓间充质干细胞仍保持均一的长梭形形态生长,当长满24板孔底时出现生长抑制,最后逐渐凋亡;各诱导组细胞逐渐变为三角形、多角形、不规则形态,当生长近融合时,这部分细胞可以重叠生长,其中以低浓度α-玉米赤霉醇组最为典型。 2.3 α-玉米赤霉醇对小鼠骨髓间充质干细胞生长曲线的影响 结果显示:各组骨髓间充质干细胞生长趋势大致相同,与空白诱导组相比,各诱导组均可促进骨髓间充质干细胞增殖,与空白诱导组相比,阳性对照诱导组和低浓度α-玉米赤霉醇组均可促进骨髓间充质干细胞增殖,但中浓度的α-玉米赤霉醇促进作用较低浓度的稍弱,高浓度的α-玉米赤霉醇促进作用最弱(图1)。"
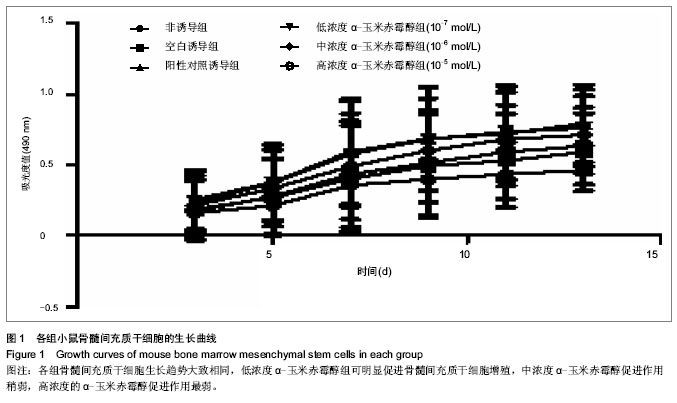
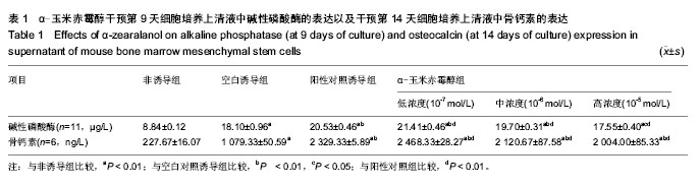
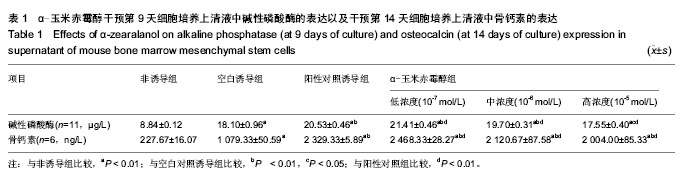
2.4 α-玉米赤霉醇各组对碱性磷酸酶、骨钙素表达的影响 比较各组的碱性磷酸酶表达量,采用单因素方差分析,方差齐性检验P=0.056,P > 0.05,可认为总体方差齐同,与非诱导组相比,各诱导组碱性磷酸酶表达均明显升高,差异有非常显著性意义(P < 0.01);与空白对照诱导组相比,高浓度α-玉米赤霉醇组碱性磷酸酶表达升高(P < 0.05),阳性对照诱导组、中、低浓度α-玉米赤霉醇组明显升高,差异有非常显著性意义(P < 0.01),说明α-玉米赤霉醇组可以促进碱性磷酸酶的分泌。与阳性对照组相比,低浓度α-玉米赤霉醇组碱性磷酸酶表达升高(P < 0.01),中浓度、高浓度α-玉米赤霉醇组下降(P均< 0.01)。说明随着α-玉米赤霉醇浓度升高,碱性磷酸酶表达呈下降趋势(表1)。 比较各组的骨钙素表达量,采用单因素方差分析,方差齐性检验P=0.083,P > 0.05,可认为总体方差齐同。与非诱导组相比,各诱导组骨钙素表达均明显升高,差异有非常显著性意义(P < 0.01);与空白对照诱导组比较,阳性对照诱导组、各浓度α-玉米赤霉醇组骨钙素表达均明显升高(P < 0.01),说明α-玉米赤霉醇组可以促进骨钙素的分泌,差异有显著性意义;与阳性对照组相比,低浓度α-玉米赤霉醇组骨钙素表达升高(P < 0.01),中浓度、高浓度α-玉米赤霉醇组下降(P均< 0.01)。说明随着α-玉米赤霉醇浓度升高,骨钙素表达呈下降趋势,可见α-玉米赤霉醇组促进骨钙素的分泌有最佳浓度,随着浓度的升高,骨钙素分泌反而下降(表1)。"
| [1] Pacifici R.Cytokines, estrogen, and postmenopausal osteoporosis--the second decade.Endocrinology. 1998;139(6): 2659-2661.[2] Baber RJ, O'Hara JL, Boyle FM.Hormone replacement therapy: to use or not to use. Med J Aust. 2003;178(12): 630-633.[3] 宗少晖,韦波,曾高峰,等.α-玉米赤霉醇干预骨质疏松性骨折模型大鼠白细胞介素1、6的表达[J].中国组织工程研究与临床康复, 2011,15(33):6165-6167.[4] 宗少晖,韦波,曾高峰,等.α-玉米赤霉醇对骨质疏松性骨折大鼠骨代谢因子的影响[J].重庆医学, 2011, 40(31):3116-3117.[5] 戴顺龄,段金虹,陆媛,等.α玉米赤霉醇--一个值得重视的新的植物雌激素[J].中国动脉硬化杂志,2005,13(5):670-672.[6] 陈鹭,王雯,蒋东桥.植物雌激素α-玉米赤霉醇的心血管保护作用[J].中国实用医药,2007,2(31):1-2. [7] 赵小元,左萍萍,段金虹,等.α-玉米赤霉醇对实验性高脂血症兔的血脂代谢及血液流变学的影响[J].中国康复理论与实践,2005, 11(11):924-926.[8] 戴顺龄,段金虹,陆媛,等.植物雌激素α-玉米赤霉醇与17β雌二醇、戊酸雌二醇对兔食饵性动脉粥样硬化的作用[J].微循环学杂志, 2006,16(4):15-18,23.[9] 王雯,邱笑违,蒋东桥,等.植物雌激素α-玉米赤霉醇对HUVEC低氧/复氧损伤的保护作用[J].中国病理生理杂志,2006,22(11): 2110-2112.[10] 王雯,朱盈芬,蒋东桥,等.植物雌激素α-玉米赤霉醇对大鼠胸主动脉血管的舒张效应[J].中国临床康复,2006,10(23):87-89.[11] 王雯, 蒋东桥,邱笑违,等.缺氧/复氧损伤人脐静脉内皮细胞黏附分子表达与新型植物雌激素α-玉米赤霉醇的影响[J].中国组织工程研究与临床康复,2007,11(6):1038-1040.[12] 于晓红,王小明,斯琴,等.α-玉米赤霉醇对肿瘤坏死因子α诱导的人内皮细胞活性氧产生及其激活信号通路的影响[J].中华医学杂志,2009,89(4):266-270.[13] 甄攀攀,蒋东桥,洪霓,等.α-玉米赤霉醇改善去卵巢高同型半胱氨酸血症大鼠的血管功能[J].基础医学与临床,2010, 30(10): 1020-1024. [14] 戴顺龄,段金虹,陆媛,等.新的植物雌激素α玉米赤霉醇明显抑制实验性动脉粥样硬化发病进程[J].中国动脉硬化杂志,2003, 11(5): 385-390.[15] 王雯,朱广瑾,祖淑玉.17β-雌二醇及α-玉米赤霉醇对人脐静脉内皮细胞组织因子表达的影响[J].基础医学与临床,2004, 24(01): 56-59.[16] 王雯,朱广瑾.植物雌激素α-玉米赤霉醇对去卵巢大鼠凝血及纤溶功能的影响与补充外源性17β-雌二醇的比较[J].中国临床康复,2005,9(27):195-197.[17] 王雯,杨慧,王红霞, 等.17β-雌二醇及植物雌激素α-玉米赤霉醇致去卵巢大鼠子宫增大作用的比较[J].首都医科大学学报, 2005, 26(1):51-54.[18] 程炜,李少春,崔娜,等.α-玉米赤霉醇对去卵巢大鼠骨代谢生化指标的影响[J].中国民族民间医药,2010,19(20):6,9.[19] 李少春,段斐,程炜,等.植物雌激素α-玉米赤霉醇对去卵巢大鼠骨组织形态学变化的影响[J].时珍国医国药,2011,22(7): 1655- 1656.[20] 李少春,段斐,程炜,等.植物雌激素α-玉米赤霉醇对去卵巢大鼠骨组织雌激素受体α和βmRNA的影响[J].中国老年学杂志,2011, 31(10):1786-1787.[21] 孟洁.α-玉米赤霉醇对体外培养成骨细胞的影响及机制[J].石家庄:河北大学,2010.[22] 高文.α-玉米赤霉醇对体外培养成骨细胞作用的研究[J].石家庄:河北大学,2011.[23] 刘未华,段斐,李少春,等.骨髓间充质干细胞来源成骨细胞培养体系中加入α-玉米赤霉醇干预后的骨保护素表达[J].中国组织工程研究,2012,16(6):977-980.[24] Pittenger MF, Mackay AM, Beck SC,et al. Multilineage potential of adult human mesenchymal stem cells.Science. 1999;284(5411):143-147.[25] Jiang Y, Jahagirdar BN, Reinhardt RL,et al. Pluripotency of mesenchymal stem cells derived from adult marrow.Nature. 2002;418(6893):41-49.[26] Pittenger MF, Mackay AM, Beck SC, et al. Multilineage potential of adult human mesenchymal stem cells. Science. 1999;284(5411): 143-147.[27] Hoemann CD, El-Gabalawy H, McKee MD.In vitro osteogenesis assays: influence of the primary cell source on alkaline phosphatase activity and mineralization.Pathol Biol (Paris). 2009;57(4):318-323. [28] Liu P, Oyajobi BO, Russell RG,et al.Regulation of osteogenic differentiation of human bone marrow stromal cells: interaction between transforming growth factor-beta and 1,25(OH)(2) vitamin D(3) In vitro.Calcif Tissue Int. 1999 Aug;65(2):173-180.[29] Maniatopoulos C, Sodek J, Melcher AH.Bone formation in vitro by stromal cells obtained from bone marrow of young adult rats.Cell Tissue Res. 1988 ;254(2):317-330.[30] Hughes FJ, McCulloch CA.Stimulation of the differentiation of osteogenic rat bone marrow stromal cells by osteoblast cultures.Lab Invest. 1991;64(5):617-622.[31] Croft AP, Przyborski SA. Mesenchymal stem cells from the bone marrow stroma: basic biology and potential for cell therapy. Current Anaesthesia & Critical Care.2004; 15(6): 410-417.[32] 杨丽,张荣华,谢厚杰,等.建立大鼠骨髓间充质干细胞稳定分离培养体系与鉴定[J].中国组织工程研究与临床康复,2009,13(6): 1064-1068.[33] 胡资兵,曾荣,郭伟韬,等.骨髓间充质干细胞诱导分化特征[J].中国组织工程研究与临床康复,2008,12(43):8561-8566.[34] 李晓峰,赵劲民,苏伟,等.大鼠骨髓间充质干细胞的培养与鉴定[J].中国组织工程研究,2011,15(10):1721-1725. [35] Titorencu I, Jinga V, Constantinescu E,et al. Proliferation, differentiation and characterization of osteoblasts from human BM mesenchymal cells.Cytotherapy. 2007;9(7):682-696.[36] 俞猛,于方,付胜良.兔骨髓间充质干细胞体外培养定向诱导分化为软骨细胞[J].中国组织工程研究与临床康复,2011,15(27): 4951-4954.[37] 黄定强,杨大鉴,黎万荣,等.骨髓间充质干细胞定向诱导条件下向脂肪细胞和成骨细胞诱导分化的关系[J].中国临床康复,2006, 10(1):31-33.[38] Woodbury D, Schwarz EJ, Prockop DJ, et al.Adult rat and human bone marrow stromal cells differentiate into neurons.J Neurosci Res. 2000;61(4):364-370.[39] Kopen GC, Prockop DJ, Phinney DG.Marrow stromal cells migrate throughout forebrain and cerebellum, and they differentiate into astrocytes after injection into neonatal mouse brains.Proc Natl Acad Sci U S A. 1999;96(19):10711-10716.[40] Sanchez-Ramos J, Song S, Cardozo-Pelaez F,et al. Adult bone marrow stromal cells differentiate into neural cells in vitro. Exp Neurol. 2000;164(2):247-256.[41] 祁颖,张凤妍,宋革,等. 恒河猴骨髓干细胞诱导分化为胆碱能神经元[J].中国科学C辑:生命科学,2009,39(11):1041-1048.[42] Jaiswal N, Haynesworth SE, Caplan AI,et al.Osteogenic differentiation of purified, culture-expanded human mesenchymal stem cells in vitro.J Cell Biochem. 1997; 64(2):295-312.[43] Cheng SL, Yang JW, Rifas L,et al.Differentiation of human bone marrow osteogenic stromal cells in vitro: induction of the osteoblast phenotype by dexamethasone.Endocrinology. 1994;134(1):277-286.[44] Yin L, Li YB, Wang YS.Dexamethasone-induced adipogenesis in primary marrow stromal cell cultures: mechanism of steroid-induced osteonecrosis.Chin Med J (Engl). 2006;119(7):581-588.[45] Mikami Y, Omoteyama K, Kato S,et al. Inductive effects of dexamethasone on the mineralization and the osteoblastic gene expressions in mature osteoblast-like ROS17/2.8 cells.Biochem Biophys Res Commun. 2007;362(2):368-373.[46] Deng W, Obrocka M, Fischer I,et al. In vitro differentiation of human marrow stromal cells into early progenitors of neural cells by conditions that increase intracellular cyclic AMP.Biochem Biophys Res Commun. 2001;282(1):148-152.[47] Phinney DG.Biochemical heterogeneity of mesenchymal stem cell populations: clues to their therapeutic efficacy.Cell Cycle. 2007;6(23):2884-2889. [48] Chen M, Qu Q, Shen T,et al. Expression of cell surface antigens during the differentiation of osteoblast by human bone marrow-derived mesenchymal stem cells.Zhongguo Yi Xue Ke Xue Yuan Xue Bao. 2007;29(1):62-66.[49] Shimizu K, Ito A, Yoshida T,et al. Bone tissue engineering with human mesenchymal stem cell sheets constructed using magnetite nanoparticles and magnetic force.J Biomed Mater Res B Appl Biomater. 2007;82(2):471-480.[50] Marie PJ, Fromigué O.Osteogenic differentiation of human marrow-derived mesenchymal stem cells.Regen Med. 2006; 1(4):539-548.[51] Duan RP, Wu L, Lin YF,et al.The gene expression patterns of bone-marrow mesenchymal stem cells under different osteogenic induction.Sichuan Da Xue Xue Bao Yi Xue Ban. 2006;37(6):856-859.[52] Mao X, Chu CL, Mao Z,et al. The development and identification of constructing tissue engineered bone by seeding osteoblasts from differentiated rat marrow stromal stem cells onto three-dimensional porous nano-hydroxylapatite bone matrix in vitro.Tissue Cell. 2005; 37(5):349-357.[53] Yamada S, Ozawa Y, Tomoeda M,et al. Regulation of PLAP-1 expression in periodontal ligament cells.J Dent Res. 2006; 85(5): 447-451.[54] Peter SJ, Liang CR, Kim DJ,et al.Osteoblastic phenotype of rat marrow stromal cells cultured in the presence of dexamethasone, beta-glycerolphosphate, and L-ascorbic acid.J Cell Biochem. 1998;71(1):55-62.[55] Hessle L, Johnson KA, Anderson HC,et al.Tissue-nonspecific alkaline phosphatase and plasma cell membrane glycoprotein-1 are central antagonistic regulators of bone mineralization.Proc Natl Acad Sci U S A. 2002;99(14):9445- 9449. [56] Anderson HC, Sipe JB, Hessle L,et al.Impaired calcification around matrix vesicles of growth plate and bone in alkaline phosphatase-deficient mice.Am J Pathol. 2004;164(3):841- 847.[57] Wagner EF, Karsenty G.Genetic control of skeletal development.Curr Opin Genet Dev. 2001;11(5):527-532. [58] Bi LX, Simmons DJ, Mainous E. Expression of BMP-2 by rat bone marrow stromal cells in culture.Calcif Tissue Int. 1999; 64(1):63-68.[59] Kuru L, Griffiths GS, Petrie A,et al.Alkaline phosphatase activity is upregulated in regenerating human periodontal cells.J Periodontal Res. 1999;34(2):123-127.[60] Kim JL, Park SH, Jeong D,et al. Osteogenic activity of silymarin through enhancement of alkaline phosphatase and osteocalcin in osteoblasts and tibia-fractured mice.Exp Biol Med (Maywood). 2012;237(4):417-428. |
| [1] | Wang Jian-ji, Yang Long, Li Jing, Sun Qi, Zuo Wei-min, Ren Qi-feng, Sun Yu, Wu Zhan-yu, Zou Qiang, Ma Min-xian, Ye Chuan. Development and application of special-purpose grafter by femoral head decompression combined with bone marrow mesenchymal stem cells transplantation based on three-dimensional printing technology [J]. Chinese Journal of Tissue Engineering Research, 2016, 20(44): 6636-6642. |
| [2] | Li Shi-hong, Liu Yang. Measurement of bone metabolism markers and changes of bone mineral density in patients with bone and joint disease and fractures in perioperative period [J]. Chinese Journal of Tissue Engineering Research, 2016, 20(35): 5290-5295. |
| [3] | Zhou Chang-yan, Zhou Qing-huan, Bian Jing, Chen Ke, Chen Wen. Bone marrow mesenchymal stem cells combined with calcium phosphate cement to repair articular cartilage defects in rabbits [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(8): 1195-1199. |
| [4] | Xu Xiang, Yin He-ping. Platelet-rich plasma accelerates the proliferation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(14): 2144-2148. |
| [5] | Du Qing-hua, Cao Jun-kai, Dong Xi-xi, E Ling-ling, Wei Li-jun. Osteogenic differentiation of pluripotent stem cells induced by akermanite extracts [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(14): 2236-2242. |
| [6] | Rao Li-jia, Li Qi-meng, Li Jin-ling, Xu Qiong. Expression pattern of ten-eleven translocation family during differentiation of human dental pulp cells [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(14): 2261-2266. |
| [7] | Gao Zhuo-yue, Liu Yong-qi, He Jian-xin, Wu Zhi-wei, Luo Ya-li, Su Yun, Zhang Li-ying, Zhang Qi, Wu You-ming, Zhou Ni-na. Regulatory effects of warming yang and invigorating qi treatment on the inflammatory balance and genetic stability of bone marrow mesenchymal stem cells under tumor microenvironment [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(14): 2267-2272. |
| [8] | Lin Shu-zhong, Liu Jun. Effects of different doses of puerarin on osteoblasts in vitro [J]. Chinese Journal of Tissue Engineering Research, 2015, 19(11): 1658-1662. |
| [9] | Han Xiang-zhen, He Hui-yu, Hu Yang, Ba Jiao-jiao, Wang Huan-huan, Mi Xue, Abulizi•Abudula. Recombinant lentiviral vector transfected sheep bone marrow mesenchymal stem cells and osteogenic gene expression changes [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 821-828. |
| [10] | Huang Jian-feng, Huang Ji-feng, Zhang Wei-cai. Bone marrow mesenchymal stem cells differentiate into neuron-like cells induced by combination of two cytokines [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 829-834. |
| [11] | Yang Yi, Ding Wen-jing, Dong Wan-li. Autophagy-related gene Beclin-1 expression in neuron-like differentiation of human bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 841-846. |
| [12] | Su Xue-lian, Bao Guang-jie, Kang Hong, Liu Lin, Kong Nan-nan. Morphological changes of goat bone marrow mesenchymal stem cells differentiating into fibrochondrocytes [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 860-865. |
| [13] | Nie De-zhi, Wan Ying, Ben Liang, Wang Ying-jun, Liu Xiang-zhu, Wang Li-hui, Li Chao, Zhang Shi-dong. Stem cell tumorigenicity in Balb/c nude mice [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 888-893. |
| [14] | Fan Yan, Wang Jian-jun, Wei Feng, Fan Xiao-hai, Ma Ai-qun. Effect of adipose-derived mesenchymal stem cell transplantation on inflammatory response and ventricular remodeling after myocardial infarction [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 900-905. |
| [15] | Zhao Xiao-jian, Lu Cai-ping, Chu Wei-wei, Zhen Qiang, Tan Guo-liang, Zhang Ya-xiao, Wang Ren-feng, Zhang Bing, Liu Jia-bao. Bone marrow mesenchymal stem cell transplantation suppresses emphysema-induced inflammation and apoptosis [J]. Chinese Journal of Tissue Engineering Research, 2014, 18(6): 906-911. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||