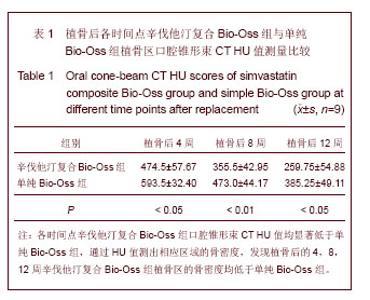
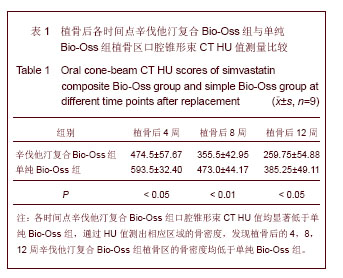
Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (48): 8374-8380.doi: 10.3969/j.issn.2095-4344.2013.48.013
Previous Articles Next Articles
Simvastatin compounded with Bio-Oss repairs rabbit mandibular defects
Wang Yang, Jiao Xin, Liang Heng-yan, Ge Zhen-lin
- Department of Orthodontics, Lanzhou University Stomatology Hospital (School of Stomatology), Lanzhou 730000, Gansu Province, China
-
Online:2013-11-26Published:2013-11-26 -
Contact:Ge Zhen-lin, Professor, Master’s supervisor, Department of Orthodontics, Lanzhou University Stomatology Hospital (School of Stomatology), Lanzhou 730000, Gansu Province, China gezhl@lzu.edu.cn -
About author:Wang Yang★, Master, Department of Orthodontics, Lanzhou University Stomatology Hospital (School of Stomatology), Lanzhou 730000, Gansu Province, China wangyang711@gmail.com -
Supported by:Natural Science Foundation of Gansu Province, No.1208RJZA209*
CLC Number:
Cite this article
Wang Yang, Jiao Xin, Liang Heng-yan, Ge Zhen-lin. Simvastatin compounded with Bio-Oss repairs rabbit mandibular defects[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(48): 8374-8380.
share this article
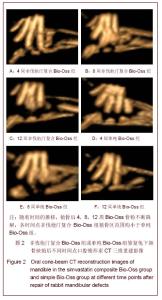
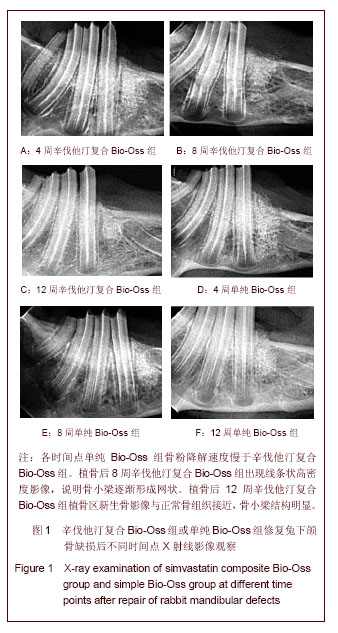
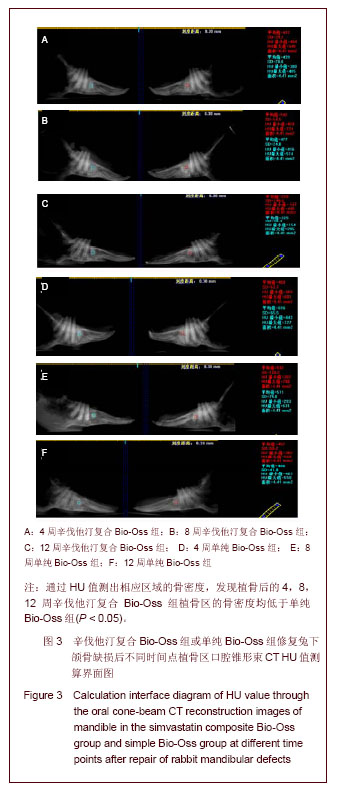
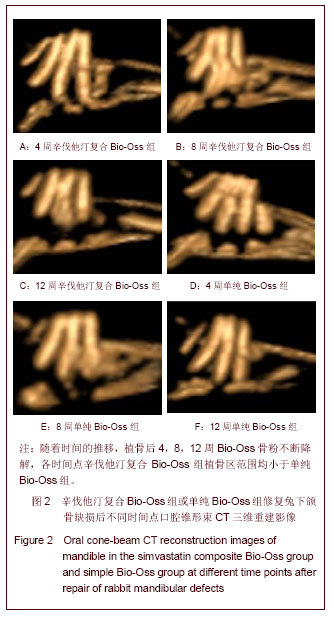
植骨后4周X射线影像可见植骨区Bio-Oss骨粉呈现出的高密度阻射影像。单纯Bio-Oss组与正常骨组织交界较明显,轮廓接近骨缺损范围,见图 1D;辛伐他汀复合Bio-Oss组高密度影像范围缩小较多,边界圆顿,见图 1A。说明骨粉降解速度慢于辛伐他汀复合Bio-Oss组。植骨后8周X射线影像可见高密度阻射范围持续缩小,骨粉进一步降解。单纯Bio-Oss组植骨区仍有较多高密度阻射影像,见图1B,未降解骨粉密度及范围均大于辛伐他汀复合Bio-Oss组。辛伐他汀复合Bio-Oss组出现线条状高密度影像,见图1E,说明骨小梁逐渐形成网状。植骨后12周X射线影像可见单纯Bio-Oss组残余骨粉较多,见图 1F,辛伐他汀复合Bio-Oss组植骨区新生骨影像与正常骨组织接近,骨小梁结构明显,见图1C。 2.4 口腔锥形束CT 三维重建影像结果 口腔锥形束CT三维重建影像可见:随着时间的推移,植骨后4,8,12周Bio-Oss骨粉不断降解,各时间点辛伐他汀复合Bio-Oss组植骨区范围均小于单纯Bio-Oss组,见图2。"
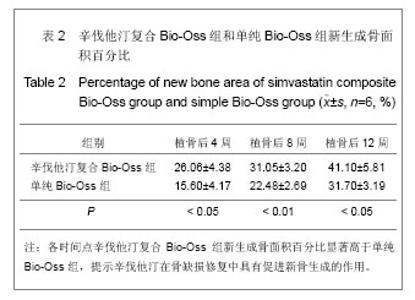
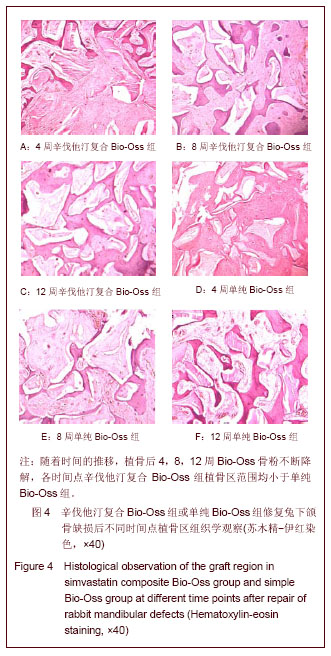
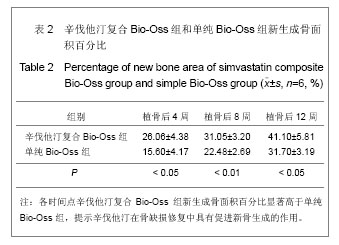
植骨后4周时,辛伐他汀复合Bio-Oss组可见骨粉颗粒少量降解,部分骨粉颗粒周围形成一层新骨,未连续成网状,成骨细胞排列有序,见图4A;单纯Bio-Oss组部分骨粉颗粒周围形成较薄一层新骨,成骨量低于辛伐他汀复合Bio-Oss组,见图4D。植骨后8周时,辛伐他汀复合Bio-Oss组可见骨粉持续降解,新骨形成较多,骨粉颗粒周围形成较厚的新骨,骨小梁逐渐连续呈网状,见图4B;单纯Bio-Oss组骨粉降解速率不及辛伐他汀复合Bio-Oss组,有大量新骨形成,但骨小梁厚度与形成网状骨小梁均低于辛伐他汀复合Bio-Oss组,见图 4E。植骨后12周时,辛伐他汀复合Bio-Oss组骨粉大部分降解,残存片状骨粉碎片,可见大片成熟骨组织形成,骨板排列规则,骨髓腔形成,血供丰富,见图4C;单纯Bio-Oss组新骨数量增加,有骨小梁形成且大部分呈网状,但总体新生骨量及质量不如辛伐他汀复合Bio-Oss组,见图4F。 测量新骨形成面积占视野总面积的百分比,见表2。提示辛伐他汀在骨缺损修复中具有促进新骨生成的作用。"
| [1] Mundy G, Garrett R, Harris S, et al. Stimulation of bone formation in vitro and in rodents by statins. Science.1999; 286(5446):1946-1949. [2] Maeda T, Matsunuma A, Kurahashi I, et al. Induction of osteoblast differentiation indices by statins in MC3T3-E1 cells. J Cell Biochem 2004;92:458-471. [3] 刘志强,周磊,邹剑曾,等.辛伐他汀对大鼠胫骨骨缺损修复作用的实验研究[J].临床口腔医学杂志,2010,26(4):214-217. [4] Valentini P, Abensur D, Wenz B,et al.Sinus grafting withporous bone mineral (Bio-Oss) forimplant placement: a 5-year study on15 patients. Int J Periodontics Restorative Dent.2000;20: 245-253. [5] Maciel-Oliveira N, Bradaschia-Correa V, Arana-Chavez VE. Early alveolar bone regeneration in rats after topical administration of simvastatin. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112(2):170-179. [6] 荣小芳,吴琳,杨晓东,等.兔下颌骨临界骨缺损人工材料植入实验动物模型的建立[J].中国医科大学学报,2008,37(1):62-64. [7] Rho JY, Hobatho MC, Ashman RB.Relations of mechanical properties to density and CT numbers in human bone. Med EngPhys.1995;17(5):347-355. [8] Jensen S S, Aaboe M, Pinholt EM, et al. Tissue reaction and material characteristics of four bone substitutes. The International journal of oral & maxillofacial implants. 1996; 11(1): 55. [9] Piattelli M, Favero GA, Scarano A, et al. Bone reactions to anorganic bovine bone (Bio-Oss) used in sinus augmentation procedures: a histologic long-term report of 20 cases in humans. The International journal of oral & maxillofacial implants. 1999;14(6): 835. [10] Weibrich G, Trettin R, Gnoth S H, et al. Determining the size of the specific surface of bone substitutes with gas adsorption. Mund-, Kiefer-und Gesichtschirurgie: MKG, 2000; 4(3): 148. [11] Berglundh T, Lindhe J. Healing around implants placed in bone defects treated with Bio-Oss: an experimental study in the dog. Clin Oral Implants Res.1997;8:117-124. [12] 邱立新,林野,王兴,等. Bio-Oss骨代用品同引导骨再生膜联合应用效果的观察[J].中华口腔医学杂志,2002,37(6):412-414. [13] 方利华,平金良,孟祥勇,等.下颌骨缺损即刻修复的动物实验研究[J].上海口腔医学, 2008, 17(4): 405-410. [14] 李春明,杨春艳,王鑫,等. bFGF基因修饰的骨髓基质细胞复合多孔矿化Bio-Oss胶原修复下颌骨缺损的实验研究[J].实用口腔医学杂志, 2008, 24(4): 470-474. [15] Zitzmann NU, Naef R, Schärer P. Resorbable versus nonresorbable membranes in combination with Bio-Oss for guided bone regeneration. Int J Oral Maxillofac Implants. 1997;12(6):844-852. [16] Araújo MG, Carmagnola D, Berglundh T, et al. Orthodontic movement in bone defects augmented with Bio-Oss®. J Clin Periodontol. 2001;28(1):73-80. [17] Duda M, Pajak J. The issue of bioresorption of the Bio-Oss xenogeneic bone substitute in bone defects[C]// AnnalesUniversitatisMariae Curie-Sklodowska.Sectio D: Medicina. 2004, 59(1): 269. [18] Gielkens P F M, Schortinghuis J, De Jong J R, et al. Vivosorb®, Bio-Gide®, and Gore‐Tex® as barrier membranes in rat mandibular defects: an evaluation by microradiography and micro-CT. Clin Oral Implants Res. 2008 May;19(5):516-521. [19] Fayed MM, Pazera P, Katsaros C.Optimal sites for orthodonticmini-implant placement assessed by cone beam computed tomography. Angle Orthodontist. 2010;80(5): 939-951. [20] Katsumata A, Nojiri M, Fujishita M, et al.Condylar head remodeling following mandibular setback osteotomy for prognathism:a comparative study of different imaging modalities.Oral Surg Oral Med Oral Pathol Oral Radiol Endod.2006;101:505-514. [21] Nair R, DeguchiSr T, Li X, et al.Quantitative analysis of the maxilla and the mandible in hyper-and hypodivergent skeletal class II pattern. Orthodontics & Craniofacial Res.2009;12(1): 9-13. [22] Rho JY, Hobatho MC, Ashman RB.Relations of mechanical properties to density and CT numbers in human bone. Med Eng Phys.1995;17(5):347-355. [23] 赵刚,尹蒙熔,李德超,等.纳米羟基磷灰石修复牙槽骨缺损后正畸牙齿移动的可行性研究[J].黑龙江医药科学, 2010,33(003): 10-11. [24] 方利华,平金良,孟祥勇,等.下颌骨缺损即刻修复的动物实验研究[J].上海口腔医学, 2008, 17(4): 405-410. [25] 蒋冰坤,吕松桧.不同比例Bio-oss与自体骨联合修复兔颌骨缺损的实验研究[J].黑龙江医药科学, 2008,31(4): 5-6. [26] Nyan M, Sato D, Kihara H, et al. Effects of the combination with alpha -tricalcium phosphate and simvastatinonboneregeneration. Clin Oral Implants Res. 2009;20(3):280-287. [27] Ozec I, Kilic E, Gumus C,et al. Effect of local simvastatin application on mandibular defects. J Craniofac Surg. 2007; 18:546–550. [28] 许莹莹.载辛伐他汀磷酸钙骨水泥/聚乳酸—聚羟基乙酸新型材料对剩余牙槽嵴骨修复影响的实验研究[D].吉林大学,2010. [29] Gutierrez GE, Lalka D, Garrett IR,et al.. Transdermal application of lovastatin to rats causes profound increases in bone formation and plasma concentrations. Osteoporos Int. 2006;17(7):1033-42. [30] Maritz FJ, Conradie MM, Hulley PA, et al. Effect of statins on bone mineral density and bone histomorphometry in rodents. Arterioscler ThrombVascBiol.2001;21(10):1636-1641. [31] Ma B, Clarke SA, Brooks RA, et al.The effect of simvastatin on bone formation and ceramic resorption in a peri-implant defect model.ActaBiomater. Acta Biomater. 2008;4(1): 149-155. [32] Calixto JC, Lima CE, Frederico L, et al. The influence of local administration of simvastatin in calvarial bone healing in rats. J Craniomaxillofac Surg. 2011;39(3):215-220. [33] Anbinder AL, Junqueira JC, Mancini MN,et al. Influence of simvastatin on bone regeneration of tibial defects and blood cholesterol level in rats. Braz Dent J. 2006;17(4):267-273.. [34] Yin H,LiJ,YuX,et al.Effects of Simvastatin on Osseointegration in a Canine Total Hip ArthroplastyModel:An Experimental Study. J Arthroplasty. 2011;26(8):1534-1539. |
| [1] | Liu Zhendong, Qin Sihe. Four-dimensional space events of fracture healing [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(6): 903-910. |
| [2] | Huang Hui, Dai Yao, Li Yongsheng, Chen Wei, Tang Fang, Huang Yuting, Zhou Zheng, Liu Hairong. Application and research of non-coding RNA in bone tissue engineering with cells and scaffold [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(4): 596-605. |
| [3] | Zhang Shuang, Xu Xiaomei, Zeng Yang, Yuan Xiaoping, Lin Fuwei. Rev-erbα’s effect on osteoblastogenesis of mouse bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(31): 4921-4926. |
| [4] | Chen Jia, Yang Yiqiang, Hu Chen, Chen Qi, Zhao Tian, Yong Min, Ma Dongyang, Ren Liling. Fabrication of prevascularized osteogenic differentiated cell sheet based on human bone marrow mesenchymal stem cells and human umbilical vein endothelial cells [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(31): 4934-4940. |
| [5] | Li Xuewei, Hu Beibei, Zhang Dawei, Quan Lulu, Liang Yongqiang. Calcium hydrogen phosphate dehydrate combined with gelatin and recombinant human bone morphologic protein 2/7 for repair of bone defects in rabbits [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(28): 4533-4539. |
| [6] | Xie Lei, Zhang Yan, Jiang Ziwei, Shen Zhen, Feng Junming, Hao Chengyi, Cai Yangting. Guided bone regeneration combined with kidney-tonifying therapy for repairing femoral bone defect in rats [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4106-4111. |
| [7] |
Zhang Xuan, Li Yunpeng, Zhang Xuejian, Yin Chuanrong, Deng Yue.
Guided bone regeneration using preformed titanium mesh combined with bioabsorbable membranes in aesthetic area [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(26): 4112-4117. |
| [8] |
Feng Yuan, Han Zhiqi, Zhou Nuo.
Endothelial progenitor cells promote vasculogenesis and osteogenesis in the repair of bone defects [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(25): 4046-4053. |
| [9] | Zhang Helong, Wang Huiyan, Li Zhuo, Gao Jianguo, Zhai Qian. In vitro anti-tuberculosis effect of chitosan-gelatin/poly(lactic acid co-glycolic acid) combined with drug-loaded hydrogel [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(22): 3480-3485. |
| [10] | Zhang Xue, Zhang Yang, Cui Fuzhai. Bioactivity of the peptide P17-bone morphogenetic protein-2/nano-hydroxyapatite-mineralized collagen composite [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(22): 3547-3552. |
| [11] | Jin Liangyu, Li Weiming. Nell-1 in bone tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(20): 3217-3225. |
| [12] | Wei Xing, Song Lei . Macrophages can regulate bone homeostasis and erythropoiesis: problems and prospects [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(18): 2926-2931. |
| [13] | Li Junyan, Fang Hang, Feng Xiaofeng, Cai Daozhang. Expression and role of retinoblastoma RB1-inducible coiled-coil 1 in the subchondral bone of osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(17): 2642-2647. |
| [14] |
Wang Ning, Cui Tingting, Li Yongqi, Zhao Binbin, Zhong Weijian, Ma Guowu.
Autologous cortical bone block for repair of implant-site jaw bone defects
|
| [15] | Sun Xirao, Wang Chengyue, Zhao Yuan, Zhang Zhenbao. In vitro corrosion and in vivo biosafety of pure magnesium film [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(16): 2578-2584. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||