Chinese Journal of Tissue Engineering Research ›› 2013, Vol. 17 ›› Issue (9): 1625-1632.doi: 10.3969/j.issn.2095-4344.2013.09.016
Previous Articles Next Articles
Geometry measurement of the proximal femur in the preoperative plan of hip fractures
Cai Si-qing1, Cai Dong-lu1, Yan Li-sheng1, Pan Yuan-cheng2, Zhuang Hua-feng2, Li Yi-zhong2
- 1 Department of Imaging, the Second Clinical College of Fujian Medical University, Quanzhou 362000, Fujian Province, China
2 Department of Surgery, the Second Clinical College of Fujian Medical University, Quanzhou 362000, Fujian Province, China
-
Received:2012-11-08Revised:2012-11-17Online:2013-02-26Published:2013-02-26 -
Contact:Li Yi-zhong, Master, Professor, Chief physician, Department of Surgery, the Second Clinical College of Fujian Medical University, Quanzhou 362000, Fujian Province, China doctorlyz@sina.com -
About author:Cai Si-qing, Chief physician, Associate professor, Department of Imaging, the Second Clinical College of Fujian Medical University, Quanzhou 362000, Fujian Province, China siqingcai@yahoo.com.cn
CLC Number:
Cite this article
Cai Si-qing, Cai Dong-lu, Yan Li-sheng, Pan Yuan-cheng, Zhuang Hua-feng, Li Yi-zhong. Geometry measurement of the proximal femur in the preoperative plan of hip fractures[J]. Chinese Journal of Tissue Engineering Research, 2013, 17(9): 1625-1632.
share this article
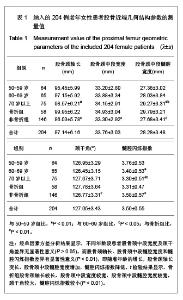
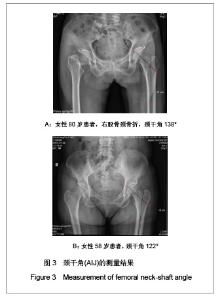
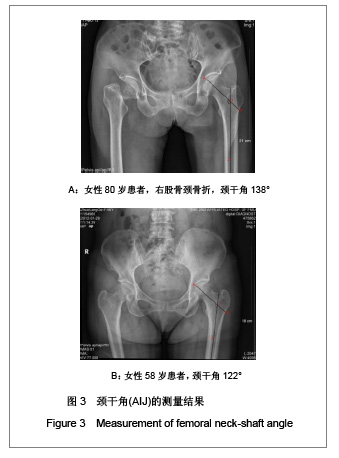
所有患者的股骨近端几何结构参数测量结果见表1。按年龄进行分层分析发现,50-59岁组骨折比例占14%,60-69岁组占18%,70岁及以上组占49%。随着年龄的增大,骨折比率显著增高。50-59岁组与60-69岁组比较,股骨颈轴长、股骨颈中段宽度、股骨颈中段髓腔宽度及颈干角差异均无显著性意义(P > 0.05),但是髓腔闪烁指数60-69岁组明显小于50-59岁(P < 0.01);60-69岁组与70岁以上组比较,股骨颈轴长、股骨颈中段宽度及颈干角差异均无显著性意义(P > 0.05),股骨颈中段髓腔宽度70岁以上组宽于60-69岁组(P < 0.05),髓腔闪烁指数70岁以上组较60-69岁组小(P < 0.05);50-59岁组与70岁以上组比较,股骨颈中段宽度及颈干角差异无显著性意义(P > 0.05),70岁以上组股骨颈轴长明显长于50-59岁组 (P < 0.01),股骨颈中段髓腔宽度70岁以上组宽于50-59岁组(P < 0.01),髓腔闪烁指数70岁以上组明显变小(P < 0.01),见表1。"
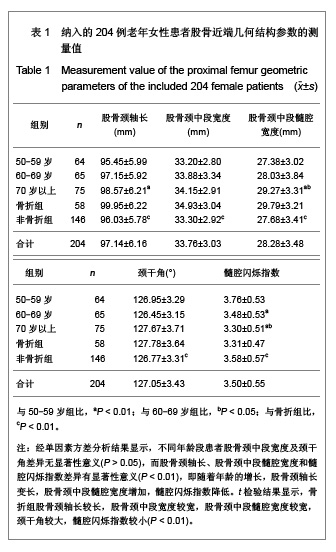
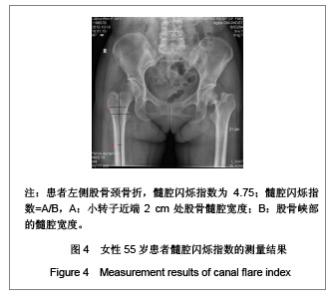
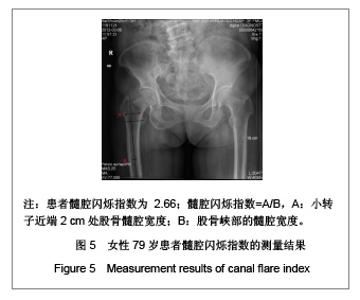
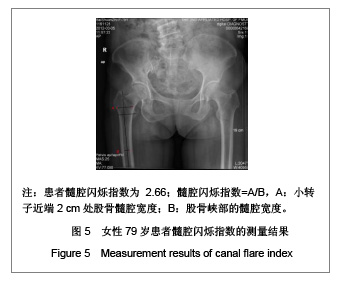
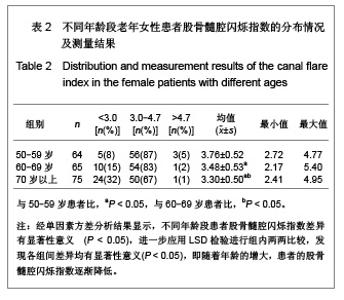
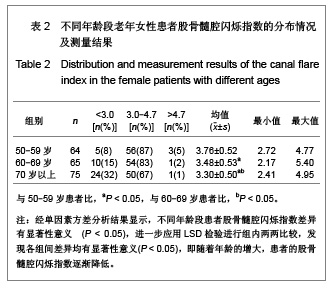
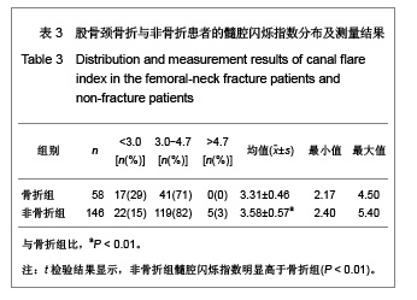
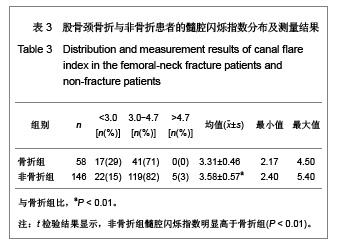
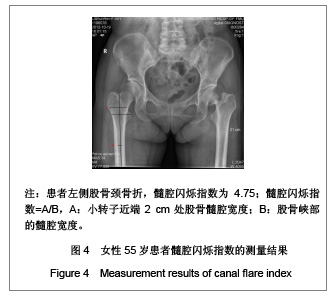
需要说明的是70岁以上组股骨颈轴长明显长于50-59岁组,课题组认为这一结果并不是颈轴长随年龄增长,而是由于70岁以上组中股骨颈骨折患者占49%所引起,因为股骨颈骨折患者的颈轴长明显大于非骨折组。 骨折组与非骨折组比较,股骨近端几何结构参数测量结果差异均有显著性意义(P < 0.01),与非骨折组比较,骨折组股骨颈轴长较长,股骨颈中段宽度较宽,股骨颈中段髓腔宽度较宽,颈干角较大,髓腔闪烁指数较小,见表1。 2.3 研究纳入的老年女性患者股骨髓腔闪烁指数的测量结果 纳入的204例老年女性患者股骨髓腔闪烁指数为2.17-5.40,平均值为3.50±0.55,见图4,5。 各年龄段患者股骨髓腔闪烁指数及分布情况见表2。与50-59岁患者比较,60-69岁及70岁以上患者股骨髓腔闪烁指数明显减小(P < 0.05),且70岁以上患者股骨髓腔闪烁指数小于60-69岁患者(P < 0.05),见表2。同时,骨折组患者髓腔闪烁指数显著低于非骨折组(P < 0.01),见表3。"
| [1] Li YZ, Chen XN, Li YC. Zhongguo Guzhi Shusong Zazhi. 2005; 11(3):342-343. 李毅中,陈献南,李炎川.高龄老人股骨颈骨质疏松性骨折的治疗[J].中国骨质疏松杂志,2005,11(3):342-343.[2] Lin JK, Li YZ, Yu HM, et al. Zhonghua Chuangshang Guke Zazhi. 2011;13(9):885-887. 林金矿,李毅中,俞海明,等.利伐沙班预防老年人髋部骨折术后下肢深静脉血栓形成的研究[J].中华创伤骨科杂志,2011, 13(9): 885-887.[3] Xia WB, He SL, Xu L, et al. Rapidly increasing rates of hip fracture in Beijing, China. J Bone Miner Res. 2011;27: 125-129.[4] Leung F, Blauth M, Bavonratanavech S. Surgery for fragility hip fracture-streamlining the process. Osteoporos Int. 2010; 21(Suppl 4):S519-521.[5] González Della Valle A, Slullitel G, Piccaluga F, et al. The precision and usefulness of preoperative planning for cemented and hybrid primary total hip arthroplasty. J Arthroplasty. 2005;20(1):51-58.[6] Cai SQ, Ren XJ, Yan JX, et al. Chongqing Yike Daxue Xuebao. 2012;37(12):1080-1083. 蔡思清,任晓静,颜建湘,等.年龄对股骨近端几何结构的影响及意义[J].重庆医科大学学报,2012,37(12):1080-1083.[7] Li YZ, Li JL, Lin JK, et al. Zhongguo Guzhi Shusong Zazhi. 2010;16(10):738-741. 李毅中,李建龙,林金矿,等.应用CT扫描观察老年股骨近端皮质骨变化的初步研究[J].中国骨质疏松杂志,2010,16(10):738- 741.[8] Li YZ, Zhuang HF, Lin JK, et al. Comparison of proximal femur geometry among the patients with or without fragile fracture of femoral neck. Osteoporos Int. 2011;22(Suppl 5):S710.[9] Li YZ, Zhuang HF, Lin JK, et al. Zhongguo Guzhi Shusong Zazhi. 2012;18(2):87-89. 李毅中,庄华烽,林金矿,等.年龄对股骨颈骨密度和皮质厚度的影响[J].中国骨质疏松杂志,2012;18(2):87-89.[10] Zhung HF, Li YZ, Lin JK, et al. Zhongguo Guzhi Shusong Zazhi. 2011;17(4):324-327. 庄华烽,李毅中,林金矿,等.脆性股骨颈骨折的股骨近端几何结构分析[J].中国骨质疏松杂志,2011,17(4):324-327.[11] Zhou L, Pei BQ, Lv K, et al. Zhonghua Chuangshang Guke Zazhi. 2007;9(1):58-61. 周力,裴葆青,吕坤,等.股骨颈骨折空心钉内固定手术参数规划与评价系统的研究[J].中华创伤骨科杂志,2007,9(1):58-61.[12] Tang GZ. Zhonghua Chuangshang Guke Zazhi. 2007;9(5): 494-495. 唐国智.空心螺钉固定治疗股骨颈骨折[J].中华创伤骨科杂志, 2007,9(5):494-495.[13] Palm H, Lysén C, Krasheninnikoff M, et al. Intramedullary nailing appears to be superior in pertrochanteric hip fractures with a detached greater trochanter: 311 consecutive patients followed for 1 year. Acta Orthop. 2011;82(2):166-170.[14] Palm H, Jacobsen S, Sonne-Holm S, et al. Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation. J Bone Joint Surg Am. 2007;89(3):470-475.[15] Pajarinen J, Lindahl J, Michelsson O, et al. Pertrochanteric femoral fractures treated with a dynamic hip screw or a proximal femoral nail. A randomised study comparing post-operative rehabilitation. J Bone Joint Surg Br. 2005; 87(1):76-81.[16] Takigami I, Matsumoto K, Ohara A, et al. Treatment of trochanteric fractures with the PFNA (proximal femoral nail antirotation) nail system-report of early results. Bull NYU Hosp Jt Dis. 2008;66(4):276-279.[17] Baumgaertner MR, Curtin SL, Lindskog DM, et al. The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip. J Bone Joint Surg Am. 1995;77(7):1058-1064.[18] Della Valle AG, Padgett DE, Salvati EA. Preoperative planning for primary total hip arthroplasty. J Am Acad Orthop Surg. 2005; 13(7):455-462.[19] Li YZ, Lin JK, Zhang J, et al. Significance of proximal femoral computed tomography scanning in the prediction of femoral prosthesis before total hip arthroplasty. Eur J Orthop Surg Traumatol. 2013;23(1):67-72.[20] Li YZ, Li JL, Lin JK, et al. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2010;14(30):5535-5538. 李毅中,李建龙,林金矿,等.股骨颈内侧径测量法术前选择股骨假体型号[J].中国组织工程研究与临床康复,2010,14(30): 5535- 5538.[21] Li YZ, Li JL, Lin JK, et al. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu.2010;14(9):1586-1590. 李毅中,李建龙,林金矿,等.股骨峡部在非骨水泥型全髋关节置换中的作用[J].中国组织工程研究与临床康复,2010,14(9): 1586-1590.[22] Noble PC. Biomechanical advances in total hip replacement. In: Niwa S, Perrem SM, Hattori T, eds. Biomechanics in orthopedics. Tokyo: Springer. 1992.[23] Rubin PJ, Leyvraz PF, Aubaniac JM, et al. The morphology of the proximal femur. A three-dimensional radiographic analysis. J Bone Joint Surg Br. 1992;74(1):28-32.[24] Noble PC, Alexander JW, Lindahl LJ, et al. The anatomic basis of femoral component design. Clin Orthop Relat Res. 1988;(235):148-165.[25] Wang W, Wang Y, Cui J. Zhongguo Linchuang Jiepouxue Zazhi. 2003;21(2):125-128. 汪伟,王岩,崔健.正常股骨近端CT测量及其临床意义[J].中国临床解剖学杂志,2003,21(2):125-128.[26] Li YZ, Li JL, Lin JK et al. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2012;16(52):9702-9706. 李毅中,李建龙,林金矿,等. 髓腔闪烁指数在全髋关节置换测量中的意义[J].中国组织工程研究与临床康复, 2012,16(52): 9702-9706.[27] Noble PC, Box GG, Kamaric E, et al. The effect of aging on the shape of the proximal femur. Clin Orthop Relat Res. 1995; (316):31-44.[28] LEE CE, Lai YS, Cheng CG. Zhonghua Guanjie Waike Zazhi(Dianziban). 2009;3(4):420-426. 李永恩,赖玉树,郑诚功.近端股骨髓腔几何形状的改变对人工髋关节置换术后存活率的影响[J].中华关节外科杂志(电子版), 2009,3(4):420-426.[29] Kobayashi S, Takaoka K, Saito N, et al. Factors affecting aseptic failure of fixation after primary Charnley total hip arthroplasty. Multivariate survival analysis. J Bone Joint Surg Am. 1997;79(11):1618-1627.[30] Aro HT, Alm JJ, Moritz N, et al. Low BMD affects initial stability and delays stem osseointegration in cementless total hip arthroplasty in women: a 2-year RSA study of 39 patients. Acta Orthop. 2012;83(2):107-114.[31] Joshi AB, Markovic L, Hardinge K, et al. Total hip arthroplasty in ankylosing spondylitis: an analysis of 181 hips. J Arthroplasty. 2002;17(4):427-433.[32] Liu HW, Sun JY, Zhang YK, et al. Zhongguo Linchuang Jiepouxue Zazhi. 2011;29(1):67-71. 刘宏伟,孙俊英,张云坤,等.股骨近段髓腔解剖参数测量与不同类型人工股骨假体的选择[J].中国临床解剖学杂志,2011,29(1): 67-71.[33] Griza S, Ueki MM, Souza DH, et al. Thermally induced strains and total shrinkage of the polymethyl-methacrylate cement in simplified models of total hip arthroplasty. J Mech Behav Biomed Mater. 2012;18C:29-36.[34] van der Veen HC, van Jonbergen HP, Poolman RW, et al. Is there evidence for accelerated polyethylene wear in uncemented compared to cemented acetabular components? A systematic review of the literature. Int Orthop. 2013;37(1):9-14.[35] Lindgren V, Garellick G, Kärrholm J, et al. The type of surgical approach influences the risk of revision in total hip arthroplasty: a study from the Swedish Hip Arthroplasty Register of 90,662 total hipreplacements with 3 different cemented prostheses. Acta Orthop. 2012;83(6):559-565.[36] Hailer NP, Weiss RJ, Stark A, et al. Dual-mobility cups for revision due to instability are associated with a low rate of re-revisions due to dislocation: 228 patients from the Swedish Hip Arthroplasty Register. Acta Orthop. 2012;83(6):566-571.[37] Imamura M, Munro NA, Zhu S, et al. Single mini-incision total hip replacement for the management of arthritic disease of the hip: a systematic review and meta-analysis of randomized controlled trials. J Bone Joint Surg Am. 2012;94(20):1897-1905.[38] Reininga IH, Stevens M, Wagenmakers R, et al. Comparison of gait in patients following a computer-navigated minimally invasive anterior approach and a conventional posterolateral approach for total hip arthroplasty: A randomized controlled trial. J Orthop Res. 2013;31(2):288-294. |
| [1] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [2] | Du Xiupeng, Yang Zhaohui. Effect of degree of initial deformity of impacted femoral neck fractures under 65 years of age on femoral neck shortening [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1410-1416. |
| [3] | Zhou Jihui, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Multiple problems in the selection of implants for patellar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1440-1445. |
| [4] | Tang Hui, Yao Zhihao, Luo Daowen, Peng Shuanglin, Yang Shuanglin, Wang Lang, Xiao Jingang. High fat and high sugar diet combined with streptozotocin to establish a rat model of type 2 diabetic osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1207-1211. |
| [5] | Li Zhongfeng, Chen Minghai, Fan Yinuo, Wei Qiushi, He Wei, Chen Zhenqiu. Mechanism of Yougui Yin for steroid-induced femoral head necrosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1256-1263. |
| [6] | Hou Guangyuan, Zhang Jixue, Zhang Zhijun, Meng Xianghui, Duan Wen, Gao Weilu. Bone cement pedicle screw fixation and fusion in the treatment of degenerative spinal disease with osteoporosis: one-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 878-883. |
| [7] | Li Shibin, Lai Yu, Zhou Yi, Liao Jianzhao, Zhang Xiaoyun, Zhang Xuan. Pathogenesis of hormonal osteonecrosis of the femoral head and the target effect of related signaling pathways [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 935-941. |
| [8] | Xiao Fangjun, Chen Shudong, Luan Jiyao, Hou Yu, He Kun, Lin Dingkun. An insight into the mechanism of Salvia miltiorrhiza intervention on osteoporosis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 772-778. |
| [9] | Liu Bo, Chen Xianghe, Yang Kang, Yu Huilin, Lu Pengcheng. Mechanism of DNA methylation in exercise intervention for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 791-797. |
| [10] | Nie Shaobo, Li Jiantao, Sun Jien, Zhao Zhe, Zhao Yanpeng, Zhang Licheng, Tang Peifu. Mechanical stability of medial support nail in treatment of severe osteoporotic intertrochanteric fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 329-333. |
| [11] | Xiang Feifan, Ye Junwu, Zhang Xihai, Ge Jianhua, Tang Lian, Yang Yunkang. Comparison of three different internal fixation methods in treatment of ipsilateral femoral neck and shaft fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 403-408. |
| [12] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [13] | Feng Guancheng, Fang Jianming, Lü Haoran, Zhang Dongsheng, Wei Jiadong, Yu Bingbing. How does bone cement dispersion affect the early outcome of percutaneous vertebroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3450-3457. |
| [14] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [15] | Cai Qunbin, Yang Lijuan, Li Qiumin, Chen Xinmin, Zheng Liqin, Huang Peizhen, Lin Ziling, Jiang Ziwei . Feasibility of internal fixation removal of intertrochanteric fractures in elderly patients based on fracture mechanics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3313-3318. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||