Chinese Journal of Tissue Engineering Research
Insulin-like growth factor 1 affects the apoptosis of rat condylar chondrocytes
Wei Li1, Jiang Li-ting2, Zhou Qi1, Zhu Ya-ping1, Gao Yi-ming2
- 1Shanghai Institute of Orthopaedics Injury, 2Department of Stomatology, Ruijin Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 200025, China
-
Received:2013-05-13Revised:2013-06-18Online:2013-08-13Published:2013-08-13 -
Contact:Gao Yi-ming, Department of Stomatology, Ruijin Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 200025, China drgaoym@yahoo.com.cn -
About author:Wei Li, Technician, Shanghai Institute of Orthopaedics injury, Ruijin Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai 200025, China weili30@163.com -
Supported by:上海市科委医学引导项目(114119a3500)
CLC Number:
Cite this article
Wei Li, Jiang Li-ting, Zhou Qi, Zhu Ya-ping, Gao Yi-ming. Insulin-like growth factor 1 affects the apoptosis of rat condylar chondrocytes[J]. Chinese Journal of Tissue Engineering Research, doi: 10.3969/j.issn.2095-4344.2013.033.001.
share this article
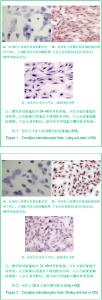
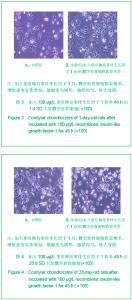
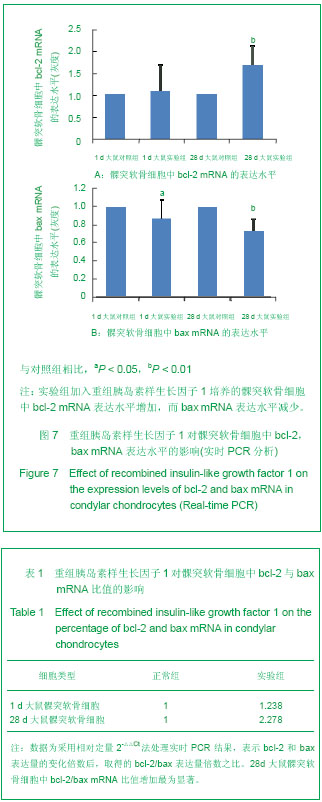
2.1 培养的大鼠髁突软骨细胞的鉴定结果 甲苯胺蓝染色显示,各组细胞染成浅蓝色,核深染,可见一两个核仁,胞质内可见紫红色异染基质出现,说明有葡萄糖胺聚糖合成。 免疫组化染色可见各组细胞胞质呈棕黄色,胞核不着色,Ⅱ型胶原呈强阳性表达,见图1,2,说明培养的细胞具有软骨细胞的特征。 2.2 重组胰岛素样生长因子1对髁突软骨细胞形态的影响 倒置显微镜下显示,加入重组胰岛素样生长因子1后各组髁突软骨细胞数量增多,增殖速度显著增加,细胞变为圆形,胞浆均匀,核大而圆,呈铺路石状,见图3,4。 2.3 重组胰岛素样生长因子1对髁突软骨细胞活性的影响 加入100 μg/L重组胰岛素样生长因子1培养24,48 h后,鼠龄为1,28 d的SD大鼠的髁突软骨细胞活性增加,见图5。"
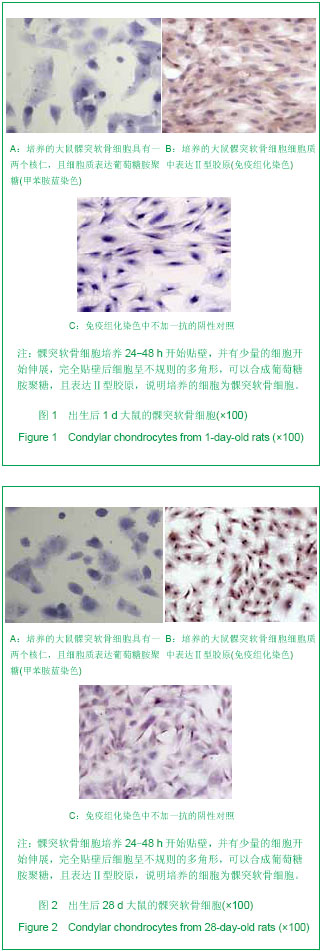

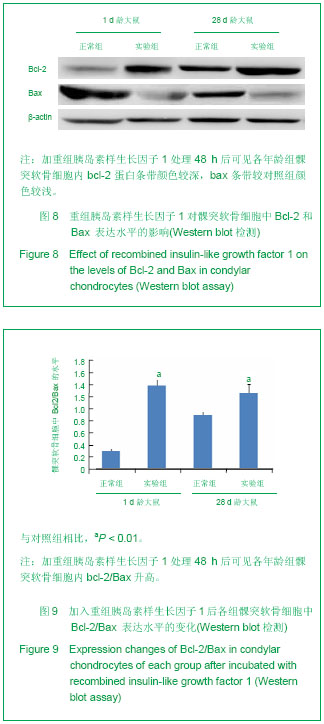
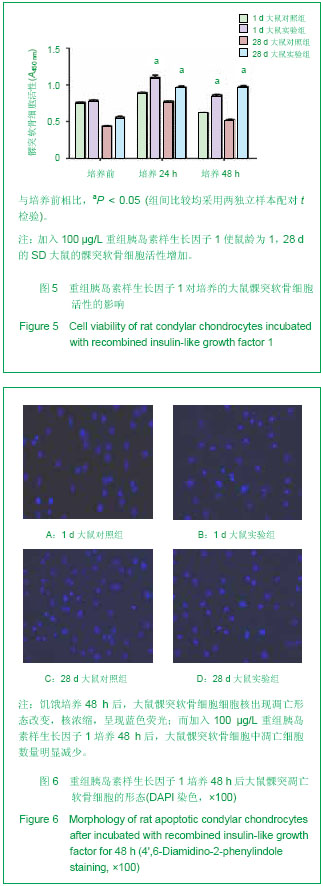
2.4 重组胰岛素样生长因子1对髁突软骨细胞凋亡的影响 DAPI染色结果显示,饥饿培养48 h后,大鼠髁突软骨细胞细胞核出现凋亡形态改变,核浓缩,呈现蓝色荧光;而加入100 μg/L重组胰岛素样生长因子1培养48 h后,大鼠髁突软骨细胞中凋亡细胞数量明显减少,见图6。 2.5 重组胰岛素样生长因子1对髁突软骨细胞中bcl-2,bax mRNA表达水平的影响 实时PCR分析结果显示,与对照组相比,1 d SD大鼠组实验组加入重组胰岛素样生长因子1培养的髁突软骨细胞中抑凋亡基因bcl-2 mRNA表达波动不明显,但在28 d时表达显著增加,而 1 d及28 d SD大鼠组实验组促凋亡基因bax mRNA表达水平减少(P < 0.05),见图7,且在28 d时bcl-2/bax mRNA比值增加最为显著,见表1。"
| [1] Singh M, Detamore MS. Biomechanical properties of the mandibular condylar cartilage and their relevance to the TMJ disc. J Biomech. 2009;42(4):405-417. [2] Kuroda S, Tanimoto K, Izawa T, et al. Biomechanical and biochemical characteristics of the mandibular condylar cartilage. Osteoarthritis Cartilage. 2009;17(11):1408-1415.[3] Giustina A, Mazziotti G, Canalis E. Growth hormone, insulin-like growth factors, and the skeleton. Endocr Rev. 2008;29(5):535-559. [4] Ohlsson C, Mohan S, Sjögren K, et al. The role of liver-derived insulin-like growth factor-I. Endocr Rev. 2009;30(5): 494-535. [5] Maor G, Hochberg Z, Silbermann M. Insulin-like growth factor I accelerates proliferation and differentiation of cartilage progenitor cells in cultures of neonatal mandibular condyles. Acta Endocrinol (Copenh). 1993;128(1):56-64.[6] Visnapuu V, Peltomäki T, Rönning O, et al. Distribution of insulin-like growth factor-I mRNA in the mandibular condyle and rib cartilage of the rat during growth. Arch Oral Biol. 2002; 47(11):791-798.[7] Ohlsson C, Sjögren K, Jansson JO, et al. The relative importance of endocrine versus autocrine/paracrine insulin-like growth factor-I in the regulation of body growth. Pediatr Nephrol. 2000;14(7):541-543.[8] Datta HK, Ng WF, Walker JA, et al. The cell biology of bone metabolism. J Clin Pathol. 2008;61(5):577-587. [9] Shibata S, Fukuoka H, Sato R, et al. An in situ hybridization study of the insulin-like growth factor system in developing condylar cartilage of the fetal mouse mandible. Eur J Histochem. 2012;56(2):e23. [10] Hinton RJ, Serrano M, So S. Differential gene expression in the perichondrium and cartilage of the neonatal mouse temporomandibular joint. Orthod Craniofac Res. 2009;12(3): 168-177. [11] Sriram D, Jones A, Alatli-Burt I, et al. Effects of mechanical stimuli on adaptive remodeling of condylar cartilage. J Dent Res. 2009;88(5):466-470.[12] Fuentes MA, Opperman LA, Bellinger LL, et al. Regulation of cell proliferation in rat mandibular condylar cartilage in explant culture by insulin-like growth factor-1 and fibroblast growth factor-2. Arch Oral Biol. 2002;47(9):643-654.[13] Higgins TF, Johnson BD. Effect of exogenous IGF-1 on chondrocyte apoptosis in a rabbit intraarticular osteotomy model. J Orthop Res. 2010;28(1):125-130. [14] Hajjar D, Santos MF, Kimura ET. Propulsive appliance stimulates the synthesis of insulin-like growth factors I and II in the mandibular condylar cartilage of young rats. Arch Oral Biol. 2003;48(9):635-642.[15] Chen Y, Ke J, Long X, et al. Insulin-like growth factor-1 boosts the developing process of condylar hyperplasia by stimulating chondrocytes proliferation. Osteoarthritis Cartilage. 2012; 20(4): 279-287.[16] Yokota T, Shimokawa H, Shibata S, et al. Insulin-like growth factor I regulates apoptosis in condylar cartilage. J Dent Res. 2008;87(2):159-163.[17] Götz W, Kunert D, Zhang D, et al. Insulin-like growth factor system components in the periodontium during tooth root resorption and early repair processes in the rat. Eur J Oral Sci. 2006;114(4):318-327.[18] Matsuda S, Mishima K, Yoshimura Y, et al. Apoptosis in the development of the temporomandibular joint. Anat Embryol (Berl). 1997;196(5):383-391.[19] Watahiki J, Yamaguchi T, Irie T, et al. Gene expression profiling of mouse condylar cartilage during mastication by means of laser microdissection and cDNA array. J Dent Res. 2004;83(3):245-249.[20] 江莉婷,朱雅萍,魏立,等.大鼠髁突软骨细胞冻存复苏后的生物学特性观察[J].现代口腔医学杂志,2012,26(4):251-257。[21] Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods. 2001;25(4):402-408.[22] Meikle MC. Remodeling the dentofacial skeleton: the biological basis of orthodontics and dentofacial orthopedics. J Dent Res. 2007;86(1):12-24.[23] Sriram D, Jones A, Alatli-Burt I, et al. Effects of mechanical stimuli on adaptive remodeling of condylar cartilage. J Dent Res. 2009;88(5):466-470.[24] Loreto C, Almeida LE, Trevilatto P, et al. Apoptosis in displaced temporomandibular joint disc with and without reduction: an immunohistochemical study. J Oral Pathol Med. 2011;40(1):103-110.[25] Ohshima T, Yonezu H, Nishibori Y, et al. Morphological observation of process of mouse temporomandibular joint formation. Bull Tokyo Dent Coll. 2011;52(4):183-190.[26] Caltabiano R, Leonardi R, Musumeci G, et al. Apoptosis in temporomandibular joint disc with internal derangement involves mitochondrial-dependent pathways. An in vivo study. Acta Odontol Scand. 2013;71(3-4):577-583. [27] Yokota T, Shimokawa H, Shibata S, et al. Insulin-like growth factor I regulates apoptosis in condylar cartilage. J Dent Res. 2008;87(2):159-163.[28] Mackey TJ, Borkowski A, Amin P, et al. bcl-2/bax ratio as a predictive marker for therapeutic response to radiotherapy in patients with prostate cancer. Urology. 1998;52(6):1085-1090.[29] Petros AM, Olejniczak ET, Fesik SW. Structural biology of the Bcl-2 family of proteins. Biochim Biophys Acta. 2004;1644 (2-3): 83-94.[30] Wu MJ, Zhan J, Gu ZY. Time course of expression of bcl-2 and bax in rabbit condylar chondrocytes following forward mandibular positioning. Angle Orthod. 2008;78(3):453-459. [31] Wu M, Gu Z, Xiao J, et al. Differential expression of apoptosis-associated proteins in chondrocytes of the mandibular condyles of rabbits with anterior disk displacement. Cranio. 2008;26(2):144-149.[32] Huang Q, Singh B, Sharawy M. Immunohistochemical analysis of Bcl-2 and Bax oncoproteins in rabbit craniomandibular joint. Arch Oral Biol. 2004;49(2):143-148.[33] Trump BF, Berezesky IK, Chang SH, et al. The pathways of cell death: oncosis, apoptosis, and necrosis. Toxicol Pathol. 1997;25(1):82-88.[34] Elmore S. Apoptosis: a review of programmed cell death. Toxicol Pathol. 2007;35(4):495-516.[35] Loreto C, Almeida LE, Migliore MR, et al. TRAIL, DR5 and caspase 3-dependent apoptosis in vessels of diseased human temporomandibular joint disc. An immunohistochemical study. Eur J Histochem. 2010;54(3):e40.[36] Loreto C, Musumeci G, Leonardi R. Chondrocyte-like apoptosis in temporomandibular joint disc internal derangement as a repair-limiting mechanism. An in vivo study. Histol Histopathol. 2009;24(3):293-298.[37] Ciarmatori S, Kiepe D, Haarmann A, et al. Signaling mechanisms leading to regulation of proliferation and differentiation of the mesenchymal chondrogenic cell line RCJ3.1C5.18 in response to IGF-I. J Mol Endocrinol. 2007; 38(4):493-508.[38] Navarro M, Baserga R. Limited redundancy of survival signals from the type 1 insulin-like growth factor receptor. Endocrinology. 2001;142(3):1073-1081.[39] Qiao M, Shapiro P, Kumar R, et al. Insulin-like growth factor-1 regulates endogenous RUNX2 activity in endothelial cells through a phosphatidylinositol 3-kinase/ERK-dependent and Akt-independent signaling pathway. J Biol Chem. 2004;279 (41): 42709-42718. [40] Prasadam I, Mao X, Wang Y, et al. Inhibition of p38 pathway leads to OA-like changes in a rat animal model. Rheumatology (Oxford). 2012;51(5):813-823. [41] Bobick BE, Kulyk WM. Regulation of cartilage formation and maturation by mitogen-activated protein kinase signaling. Birth Defects Res C Embryo Today. 2008;84(2):131-154. |
| [1] | Geng Qiudong, Ge Haiya, Wang Heming, Li Nan. Role and mechanism of Guilu Erxianjiao in treatment of osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1229-1236. |
| [2] | Li Cai, Zhao Ting, Tan Ge, Zheng Yulin, Zhang Ruonan, Wu Yan, Tang Junming. Platelet-derived growth factor-BB promotes proliferation, differentiation and migration of skeletal muscle myoblast [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1050-1055. |
| [3] | Liu Cong, Liu Su. Molecular mechanism of miR-17-5p regulation of hypoxia inducible factor-1α mediated adipocyte differentiation and angiogenesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1069-1074. |
| [4] | Ma Zetao, Zeng Hui, Wang Deli, Weng Jian, Feng Song. MicroRNA-138-5p regulates chondrocyte proliferation and autophagy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 674-678. |
| [5] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [6] | Wang Yujiao, Liu Dan, Sun Song, Sun Yong. Biphasic calcium phosphate loaded with advanced platelet rich fibrin can promote the activity of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 504-509. |
| [7] | Zhou Jihui, Yao Meng, Wang Yansong, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Influence of novel nanoscaffolds on biological behaviors of neural stem cells and the related gene expression [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 532-536. |
| [8] | Zhou Wu, Wang Binping, Wang Yawen, Cheng Yanan, Huang Xieshan. Transforming growth factor beta combined with bone morphogenetic protein-2 induces the proliferation and differentiation of mouse MC3T3-E1 cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3630-3635. |
| [9] | Zuo Zhenkui, Han Jiarui, Ji Shuling, He Lulu. Pretreatment with ginkgo biloba extract 50 alleviates radiation-induced acute intestinal injury in mice [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3666-3671. |
| [10] | Xu Bin, Yang Xiushu, Liu Xuan, Wang Zhenxing. Changes of intestinal epithelial cells and their apoptotic factors Caspase-3, Bax and Bcl-2 under urinary environment [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3173-3177. |
| [11] | Tong Jie, Liao Ying, Chen Zhengyu, Sun Guanghua . Osteoarthritic chondrocyte autophagy and regulation of mitogen-activated protein kinase signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3246-3251. |
| [12] | Yu Chengshuai, Du Gang, Pang Shenning, Lao Shan. Chemerin, a pro-inflammatory adipokine, regulates chondrocyte proliferation and metabolism by increasing production of nitric oxide [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(2): 258-263. |
| [13] | Yan Xiurui, Tao Jin, Liang Xueyun. Mechanism by which exosomes from human fetal placental mesenchymal stem cells protect lung epithelial cells against oxidative stress injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 2994-2999. |
| [14] | Dai Yaling, Chen Lewen, He Xiaojun, Lin Huawei, Jia Weiwei, Chen Lidian, Tao Jing, Liu Weilin. Construction of miR-146b overexpression lentiviral vector and the effect on the proliferation of hippocampal neural stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3024-3030. |
| [15] | Ailimaierdan·Ainiwaer, Wang Ling, Gu Li, Dilidaer•Taxifulati, Wang Shan, Yin Hongbin. Effect of transforming growth factor-beta3 on the proliferation and osteogenic capability of osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(17): 2664-2669. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||