Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (23): 3716-3721.doi: 10.3969/j.issn.2095-4344.1319
Previous Articles Next Articles
Value of erythrocyte distribution width, fibrinogen and D-dimer in predicting the occurrence and development risk of diabetic foot
Huang Yongqing, Shen Jie, Yuan Sijie, Pan Daoyan
- (Department of Endocrinology and Metabolism, the Third Affiliated Hospital of Southern Medical University, Guangzhou 510630, Guangdong Province, China)
-
Received:2019-02-22Online:2019-08-18Published:2019-08-18 -
Contact:Shen Jie, Professor, Chief physician, Doctoral supervisor, Department of Endocrinology and Metabolism, the Third Affiliated Hospital of Southern Medical University, Guangzhou 510630, Guangdong Province, China -
About author:Huang Yongqing, Master candidate, Attending physician, Department of Endocrinology and Metabolism, the Third Affiliated Hospital of Southern Medical University, Guangzhou 510630, Guangdong Province, China -
Supported by:the Health and Medical Collaborative Innovation Project of Guangzhou, No. 201604020007 (to SJ)
CLC Number:
Cite this article
Huang Yongqing, Shen Jie, Yuan Sijie, Pan Daoyan. Value of erythrocyte distribution width, fibrinogen and D-dimer in predicting the occurrence and development risk of diabetic foot [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(23): 3716-3721.
share this article
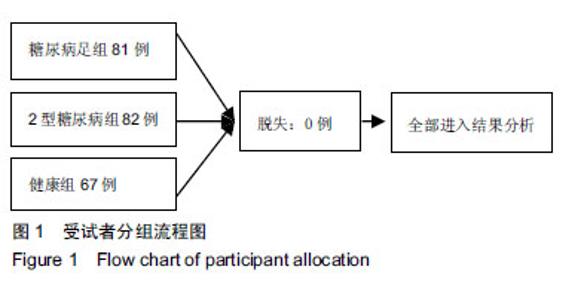
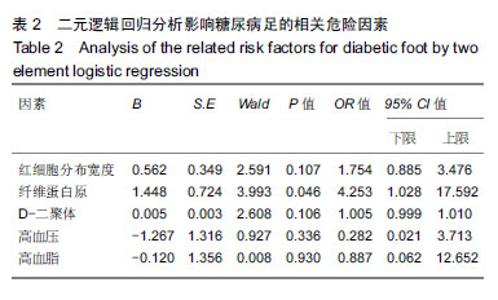
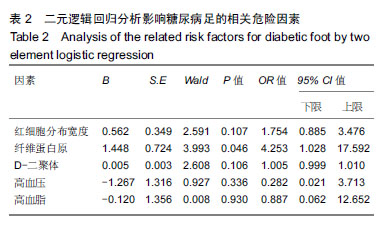
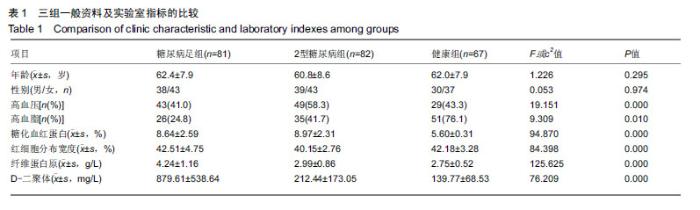
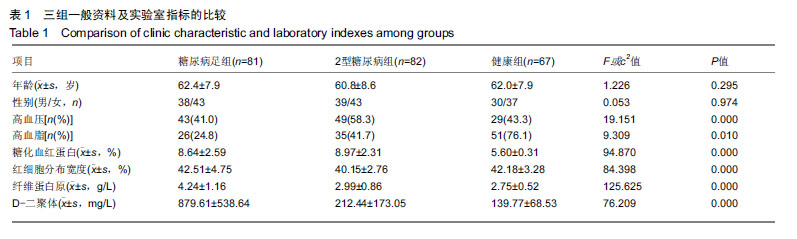
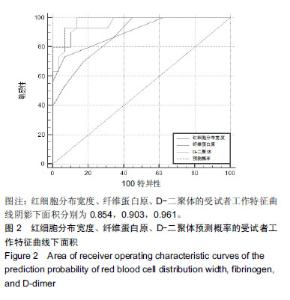
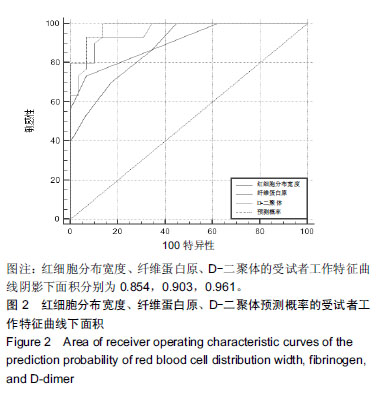
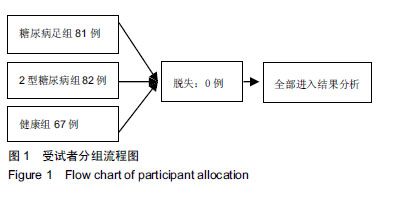
2.1 参与者数量分析 纳入糖尿病足组81例,2型糖尿病组82例,健康组67例,试验过程无脱,全部进入结果分析。 2.2 各组一般资料及实验室指标比较 3组之间年龄、性别差异无显著性意义;糖尿病足组和2型糖尿病组糖化血红蛋白水平差异无显著性意义。K-W检验表明每组的计量资料是正态分布,方差均匀性检验(F 检验)表明各组间方差是均匀的,见表1。 方差分析表明,3组的红细胞分布宽度、纤维蛋白原、D-二聚体、红细胞分布宽度指标存在差异,P值均为0.000。组间比较表明,糖尿病足组的红细胞分布宽度、纤维蛋白原、D-二聚体、糖化血红蛋白均高于2型糖尿病组和健康组(P < 0.001);2型糖尿病组的纤维蛋白原、D-二聚体、糖化血红蛋白比健康组高(P < 0.05),但红细胞分布宽度比健康组低,差异无显著性意义。检验显示3组间血压和血脂差异有显著性意义(P ≤ 0.01)。受试者分组流程图见图1。 "
| [1]Baglioni P,Malik M,Okosieme OE.Acute Charcot foot. BMJ. 2012;344(344):e1397.[2]Löndahl M. Hyperbaric Oxygen Therapy as Adjunctive Treatment of Diabetic Foot Ulcers. MED CLIN N AM.2013; 97(5):957-980.[3]Lipsky BA, Berendt AR, Cornia PB, et al.Executive Summary: 2012 Infectious Diseases Society of America Clinical Practice Guideline for the Diagnosis and Treatment of Diabetic Foot Infections. 2012. Clin Infect Dis. 2012;54(12):1679-84[4]Demetriou M,Papanas N,Panopoulou M,et al.Determinants of Microbial Load in Infected Diabetic Foot Ulcers: A Pilot Study. Int J Endocrinol. 2013;2013:858206.[5]Tabur AS,Eren MA,Çelik Y,et al.The major predictors of amputation and length of stay in diabetic patients with acute foot ulceration. Wien Klin Wochenschr. 2015;127(1-2): 45-50.[6]Isik T,Uyarel H,Tanboga IH,et al.Relation of red cell distribution width with the presence, severity, and complexity of coronary artery disease.Coron Artery Dis.2012;23(1):51-56.[7]Ak?n F,Köse N,Ayça B,et al.Relation Between Red Cell Distribution Width and Severity of Coronary Artery Disease in Patients With Acute Myocardial Infarction.ANGIOLOGY. 2012; 64(8):592-596.[8]Wonnerth A, Krychtiuk KA, Mayer FJ, et al. Red cell distribution width and mortality in carotid atherosclerosis. Eur J Clin Invest. 2016;46(2):198-204.[9]Veeranna V,Zalawadiya SK, Panaich S, et al. Comparative analysis of red cell distribution width and high sensitivity C-reactive protein for coronary heart disease mortality prediction in multi-ethnic population: Findings from the 1999–2004 NHANES. Int J Cardiol. 2013;168(6): 5156-5161.[10]Wells PS,Owen C,Doucette S,et al.Does this patient have deep vein thrombosis?.Jama. 1998;279(14):1094.[11]Wells PS,Anderson DR,Rodger M,et al.Excluding pulmonary embolism at the bedside without diagnostic imaging: management of patients with suspected pulmonary embolism presenting to the emergency department by using a simple clinical model and d-dimer. Ann Intern Med. 2001;135(2): 98-107.[12]Lowe GD.Fibrinogen and cardiovascular disease: historical introduction. Eur Heart J. 1995;16 Suppl A:2-5.[13]Smith EB.Fibrinogen, Fibrin and the Arterial Wall. Eur Heart J. 1995;16 Suppl A:11-4; discussion 14-15. Review.[14]Zubair M, Malik A, Ahmad J. Incidence, risk factors for amputation among patients with diabetic foot ulcer in a North Indian tertiary care hospital.The Foot.2012;22(1):24-30.[15]Karrer S.Diabetisches Fu?syndrom.Der Hautarzt.2011;62(7): 493-503.[16]Gupta AK,Humke S.The prevalence and management of onychomycosis in diabetic patients. Eur J Dermatol. 2000; 10(5):379-84. Review..[17]Geerlings SE, Hoepelman AI.Immune dysfunction in patients with diabetes mellitus (DM). FEMS Immunol Med Microbiol. 1999;26(3-4):259-265.[18]Cole-King A,Harding KG.Psychological factors and delayed healing in chronic wounds. Psychosom Med. 2001;63(2): 216-220.[19]Harrington AM,Ward PC,Kroft SH.Iron deficiency anemia, beta-thalassemia minor, and anemia of chronic disease: a morphologic reappraisal. Am J Clin Pathol. 2008;129(3): 466-471.[20]Romero AJ,Carbia CD,Ceballo MF,et al.[Red cell distribution width (RDW): its use in the characterization of microcytic and hypochromic anemias].Medicina.1999;59(1):17-22.[21]Symeonidis A,Athanassiou G,Psiroyannis A,et al.Impairment of erythrocyte viscoelasticity is correlated with levels of glycosylated haemoglobin in diabetic patients.Clin Lab Haematol. 2001;23(2):103-109.[22]Livshits L,Srulevich A,Raz I,et al.Effect of Short-Term Hyperglycemia on Protein Kinase C Alpha Activation in Human Erythrocytes. Rev Diabet Stud. 2012;9(2-3):94-103.[23]Patel KV, Mohanty JG, Kanapuru B. Association of the Red Cell Distribution Width with Red Blood Cell Deformability.Adv Exp Med Biol.2013;(765):211-216.[24]Rodrã Guez-Carrio J, Alperi-Lã Pez M, Lã Pez P, et al.Red cell distribution width is associated with endothelial progenitor cell depletion and vascular-related mediators in rheumatoid arthritis. Atherosclerosis.2015;240(1):131-136.[25]Solak Y,Yilmaz MI,Saglam M,et al.Red cell distribution width is independently related to endothelial dysfunction in patients with chronic kidney disease.Am J Med Sci. 2014;347(2): 118-124.[26]Demirkol S,Balta S, Celik T, et al. Assessment of the relationship between red cell distribution width and cardiac syndrome X. Kardiol Pol. 2013;71(5):480-484.[27]Nada AM.Red cell distribution width in type 2 diabetic patients.Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2015;(8):525-533.[28]Xiong X,Yang Y,Chen X,et al.Red cell distribution width as a significant indicator of medication and prognosis in type 2 diabetic patients. Sci Rep. 2017;7(1):2709.[29]Li XH,Guan LY, Lin HY, et al. Fibrinogen: A Marker in Predicting Diabetic Foot Ulcer Severity. J Diabetes Res. 2016;2016:2358321.[30]Howard SC, Algra A, Rothwell PM. Effect of age and glycaemic control on the association between fibrinogen and risk of acute coronary events after transient ischaemic attack or stroke. Cerebrovasc Dis. 2008;25(1-2):136-143.[31]Lip GY,Lowe GD.Fibrin D-dimer: a useful clinical marker of thrombogenesis?. Clin Sci (Lond). 1995;89(3):205-214.[32]Yarnell JW,Baker IA,Sweetnam PM,et al.Fibrinogen, viscosity, and white blood cell count are major risk factors for ischemic heart disease. The Caerphilly and Speedwell collaborative heart disease studies. Circulation. 1991;83(3):836-844.[33]Thaulow E,Erikssen J,Sandvik L,et al.Blood platelet count and function are related to total and cardiovascular death in apparently healthy men. Circulation. 1991;84(2):613-617.[34]Papageorgiou N,Tousoulis D,Siasos G,et al.Is fibrinogen a marker of inflammation in coronary artery disease?. Hellenic J Cardiol. 2010;51(1):1-9.[35]Kotbi S,Mjabber A,Chadli A,et al.Correlation between the plasma fibrinogen concentration and coronary heart disease severity in Moroccan patients with type 2 diabetes. Prospective study. Ann Endocrinol (Paris). 2016;77(5): 606-614.[36]Yao HQ,Wang FJ,Kang Z.Effects of endovascular interventions on vWF and Fb levels in type 2 diabetic patients with peripheral artery disease. Ann Vasc Surg. 2016;33: 159-166.[37]Wells PS, Owen C,Doucette S,et al.Does this patient have deep vein thrombosis?.Jama. 1998;279(14):1094.[38]Lippi G,Franchini M,Targher G,et al.Help me, Doctor! My D-dimer is raised. Ann Med. 2008;40(8):594-605.[39]Fu Z, Yao F, Abou-Samra AB,et al.Lipasin, thermoregulated in brown fat, is a novel but atypical member of the angiopoietin- like protein family. Biochem Biophys Res Commun. 2013; 430(3):1126-1131.[40]Hess K.The vulnerable blood. Coagulation and clot structure in diabetes mellitus. Hamostaseologie. 2015;35(1):25-33.[41]Nwose EU,Richards RS,Jelinek HF,et al.D-dimer identifies stages in the progression of diabetes mellitus from family history of diabetes to cardiovascular complications. Pathology. 2007;39(2):252-257. |
| [1] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [2] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [3] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [4] | Liu Lihua, Sun Wei, Wang Yunting, Gao Fuqiang, Cheng Liming, Li Zirong, Wang Jiangning. Type L1 steroid-induced osteonecrosis of the femoral head through femoral head and neck junction decompression by fenestration: a single-center prospective clinical study [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 906-911. |
| [5] | Fan Xinchao, Bao Wenjuan, Zhang Kai, Sun Xilong, Huang Teng, Gao Bo, Zhai Jinshuai, Zhou Yibin, Qiu Changmao, Li Wenyi, Li Xicheng. Diagnostic value of D-dimer, erythrocyte sedimentation rate and C-reactive protein in deep vein thrombosis of lower extremity after hip and knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(33): 5324-5328. |
| [6] | Bai Fuyu, Wang Mengqi, Xue Feng, Li Zhenrui, Yan Qinghao, Zhang Zhiyi, Wang Feng. Characteristics of randomized controlled trials on acupuncture for stress urinary incontinence in women [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(32): 5197-5203. |
| [7] | Su Baotong, Wang Hanyu, Xu Yilang, Xie Yajuan, Cheng Zhian. Construction of a Nomogram prediction model for postoperative delirium after hip fracture in the elderly based on medical records from a hospital [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3844-3849. |
| [8] | Cheng Chongjie, Yan Yan, Zhang Qidong, Guo Wanshou. Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3921-3928. |
| [9] | Liu Chang, Li Datong, Liu Yuan, Kong Lingbo, Guo Rui, Yang Lixue, Hao Dingjun, He Baorong. Poor efficacy after vertebral augmentation surgery of acute symptomatic thoracolumbar osteoporotic compression fracture: relationship with bone cement, bone mineral density, and adjacent fractures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3510-3516. |
| [10] | Gan Lili, Xiong Na, Liu Yanfei. Hydrogel as drug scaffold in skin wound repair: challenges of clinical application possibilities [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3578-3583. |
| [11] | Li Wenhui, Liu Guobin. Knowledge mapping analysis on the international research of diabetic foot: a visual analysis based on CiteSpace [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3178-3184. |
| [12] | Zhang Mingyan, Liu Xiangyang, Chang Lei, Chen Jing, Shen Xiongjie, Liu Bin, Peng Shuai, Zhang Chao, Wu Huanyu, Zhu Feng, Mou Haipin . Relationship between the intraoperative endplate injury and cage retropulsion after lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2856-2862. |
| [13] | Wang Xiaobo, Wang Changan, Han Jianle, Yang Qingyan, Yang Shuaiping, Yang Junwei. Influence of conversion from cyclosporine to tacrolimus on glucose metabolism and cardiovascular risk profiles in stable kidney transplant patients [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2236-2240. |
| [14] | Liu Yongyu, Xu Jingli, Lin Tianye, Wu Feng, Shen Chulong, Xiong Binglang, Zou Qizhao, Lai Qizhong, Zhang Qingwen . Sensitivity and specificity of D-dimer in the diagnosis of chronic periprosthetic infection after hip replacement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1853-1857. |
| [15] | Zhang Tengfei, Wang Kun, Zhu Yanyu, Mei Wei, Wang Qingde. Meta-analysis of risk factors associated with adjacent segment degeneration after lumbar posterior fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(12): 1936-1943. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||