Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (28): 4461-4467.doi: 10.3969/j.issn.2095-4344.1266
Previous Articles Next Articles
Correlation factors for allogeneic blood transfusion after total knee arthroplasty
Xin Chaofei, Xu Jianzhong, Zhao Shixin, Tian Jinxiang, Chang Yingjian, Shi Jianming
- Sixth Department of Orthopedics, the First Affiliated Hospital of Zhengzhou University, Zhengzhou 450000, Henan Province, China
-
Online:2019-10-08Published:2019-10-08 -
Contact:Xu Jianzhong, MD, Professor, Chief physician, Master’s supervisor, Sixth Department of Orthopedics, the First Affiliated Hospital of Zhengzhou University, Zhengzhou 450000, Henan Province, China -
About author:Xin Chaofei, Master candidate, Sixth Department of Orthopedics, the First Affiliated Hospital of Zhengzhou University, Zhengzhou 450000, Henan Province, China
CLC Number:
Cite this article
Xin Chaofei, Xu Jianzhong, Zhao Shixin, Tian Jinxiang, Chang Yingjian, Shi Jianming. Correlation factors for allogeneic blood transfusion after total knee arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(28): 4461-4467.
share this article
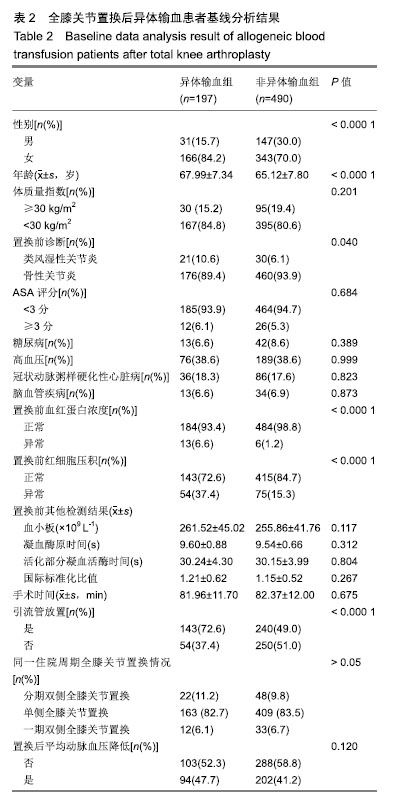
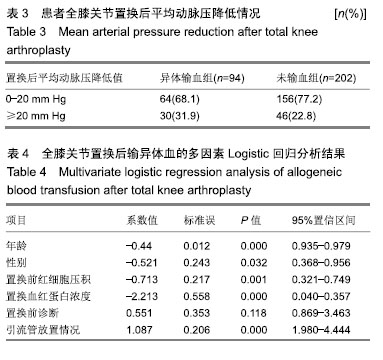
2.3 围术期输血率与输血量 全膝关节置换后总体异体输血率为28.7%(197/687),异体输血量为1-6 U,平均异体输血量为3.2 U。 2.4 影响置换后输血的因素的分析 2组患者年龄、性别、置换前血红蛋白浓度、置换前红细胞压积、引流管放置情况差异有显著性意义(P < 0.05),见表2;在置换后平均动脉压降低与患者输血率之间关系的进一步研究中发现,当平均动脉压降低≥20 mm Hg(1 mmHg=0.133 kPa)时,患者输血率明显增加,见表3;对统计过程中发现差异明显的因素进一步应用Logistic回归分析后,得出年龄、性别、置换前血红蛋白浓度、置换前红细胞压积、引流管放置情况这5项参数为影响全膝关节置换后患者输血的独立危险因素,见表4。"
| [1]Lin C, Qi Y, Jie L, et al. Is combined topical with intravenous tranexamic acid superior than topical, intravenous tranexamic acid alone and control groups for blood loss controlling after total knee arthroplasty: A meta-analysis. Medicine (Baltimore). 2016;95(51):e5344. [2]Ma J, Sun J, Guo W, et al. The effect of platelet-rich plasma on reducing blood loss after total knee arthroplasty: A systematic review and meta-analysis. Medicine (Baltimore). 2017;96(26):e7262.[3]Tian P, Liu WB, Li ZJ, et al. The efficacy and safety of tranexamic acid in revision total knee arthroplasty: a meta-analysis. BMC Musculoskelet Disord. 2017;18(1):273. [4]Balasubramanian N, Natarajan GB, Prakasam S. Prospective Study to compare Intra-articular versus Intravenous Tranexemic Acid in reducing Post-operative Blood Loss in staged bilateral Total Knee Arthroplasty. Malays Orthop J. 2016;10(3):7-11.[5]Kim YT, Kang MW, Lee JK, et al. Combined use of topical intraarticular tranexamic acid and rivaroxaban in total knee arthroplasty safely reduces blood loss, transfusion rates, and wound complications without increasing the risk of thrombosis. BMC Musculoskelet Disord. 2018;19(1):227. [6]Maniar RN, Kumar G, Singhi T, et al. Most effective regimen of tranexamic acid in knee arthroplasty: a prospective randomized controlled study in 240 patients. Clin Orthop Relat Res. 2012;470(9):2605-2612. [7]Pan JK, Hong KH, Xie H, et al. The efficacy and safety of autologous blood transfusion drainage in patients undergoing total knee arthroplasty: a meta-analysis of 16 randomized controlled trials. BMC Musculoskelet Disord. 2016;17(1):452.[8]Fu Y, Shi Z, Han B, et al. Comparing efficacy and safety of 2 methods of tranexamic acid administration in reducing blood loss following total knee arthroplasty: A meta-analysis. Medicine (Baltimore). 2016;95(50):e5583.[9]Ayd?n BK, Durgut F, Erkoçak ÖF, et al. Other benefits of intra-articular injection of tranexamic acid in primary total knee arthroplasty apart from reducing blood transfusion rates. Eklem Hastalik Cerrahisi. 2017;28(1):25-29. [10]Liu D, Dan M, Martinez Martos S, et al. Blood Management Strategies in Total Knee Arthroplasty. Knee Surg Relat Res. 2016;28(3):179-187.[11]Hogan CA, Golightly LK, Phong S, et al. Perioperative blood loss in total hip and knee arthroplasty: Outcomes associated with intravenous tranexamic acid use in an academic medical center. SAGE Open Med. 2016;4:2050312116637024. [12]Mao Z, Yue B, Wang Y, et al. A comparative, retrospective study of peri-articular and intra-articular injection of tranexamic acid for the management of postoperative blood loss after total knee arthroplasty. BMC Musculoskelet Disord. 2016;17(1):438.[13]任国清,刘红云,滕学仁,等.人工全膝关节置换后是否放置引流管:随机对照试验[J].中国组织工程研究,2016,20(22):3219-3226.[14]李玉翠,范文强,陈海英,等.2012年早期类风湿关节炎分类标准的国内多中心临床验证[J].中华风湿病学杂志, 2017,21(12): 807-811.[15]严建锋,李强,杨宗华.老年关节置换患者体质量指数及血脂水平与围置换期血液管理的相关性[J].中国组织工程研究, 2017, 21(35):5609-5615.[16]彭慧明,翁习生,翟吉良,等.全膝关节置换术围手术期异体输血率及其影响因素[J].协和医学杂志,2014,5(2):135-141.[17]龚科,张琦,董纪元.双侧全膝关节置换术后输血的危险因素分析[J].解放军医学院学报,2016,37(1):43-46,55.[18]Brito SA, Rankin EA, Mcnear M. Acute Blood Loss Anemia in the Octogenarian Total Knee Arthroplasty, Estimated Blood Loss and Transfusions Rates. J Natl Med Assoc. 2016;108(1): 86-89. [19]Mufarrih SH, Qureshi NQ, Ali A, et al. Total knee Arthroplasty: risk factors for allogeneic blood transfusions in the South Asian population. BMC Musculoskelet Disord. 2017;18(1): 359. [20]Yoshihara H, Yoneoka D. Predictors of allogeneic blood transfusion in total hip and knee arthroplasty in the United States, 2000-2009. J Arthroplasty. 2014;29(9):1736-1740. [21]Muñoz M, Ariza D, Campos A, et al. The cost of post-operative shed blood salvage after total knee arthroplasty: an analysis of 1,093 consecutive procedures. Blood Transfus. 2013;11(2):260-271. [22]Cao G, Huang Z, Huang Q, et al. Incidence and Risk Factors for Blood Transfusion in Simultaneous Bilateral Total Joint Arthroplasty: A Multicenter Retrospective Study. J Arthroplasty. 2018;33(7):2087-2091.[23]Hart A, Khalil JA, Carli A, et al. Blood transfusion in primary total hip and knee arthroplasty. Incidence, risk factors, and thirty-day complication rates. J Bone Joint Surg Am. 2014; 96(23):1945-1951.[24]Tió M, Basora M, Rios J, et al. Severe and morbid obesity and transfusional risk in total knee arthroplasty: An observational study. Knee. 2018;25(5):923-931. [25]Li Z, Liu D, Long G, et al. Association of tourniquet utilization with blood loss, rehabilitation, and complications in Chinese obese patients undergoing total knee arthroplasty: A retrospective study. Medicine (Baltimore). 2017;96(49):e9030. [26]Paterson JM, Williams JI, Kreder HJ, et al. Provider volumes and early outcomes of primary total joint replacement in Ontario. Can J Surg. 2010;53(3):175-183.[27]McInnes IB, Schett G. The pathogenesis of rheumatoid arthritis. N Engl J Med. 2011;365(23):2205-2219. [28][28] Koskinen E, Remes V, Paavolainen P, et al. Results of total knee replacement with a cruciate-retaining model for severe valgus deformity--a study of 48 patients followed for an average of 9 years. Knee. 2011;18(3):145-150. [29]Prasad N, Padmanabhan V, Mullaji A. Blood loss in total knee arthroplasty: an analysis of risk factors. Int Orthop. 2007; 31(1):39-44. [30]Boutsiadis A, Reynolds RJ, Saffarini M, et al. Factors that influence blood loss and need for transfusion following total knee arthroplasty. Ann Transl Med. 2017;5(21):418.[31]Sepah YJ, Umer M, Ahmad T, et al. Use of tranexamic acid is a cost effective method in preventing blood loss during and after total knee replacement. J Orthop Surg Res. 2011;6:22. [32]Gao F, Ma J, Sun W, et al. Topical fibrin sealant versus intravenous tranexamic acid for reducing blood loss following total knee arthroplasty: A systematic review and meta-analysis. Int J Surg. 2016;32:31-37. [33]Kosins AM, Scholz T, Cetinkaya M, et al. Evidence-based value of subcutaneous surgical wound drainage: the largest systematic review and meta-analysis. Plast Reconstr Surg. 2013;132(2):443-450.[34]Wang D, Xu J, Zeng WN, et al. Closed Suction Drainage Is Not Associated with Faster Recovery after Total Knee Arthroplasty: A Prospective Randomized Controlled Study of 80 Patients. Orthop Surg. 2016;8(2):226-233. [35]Zhang QD, Guo WS, Zhang Q, et al. Comparison between closed suction drainage and nondrainage in total knee arthroplasty: a meta-analysis. J Arthroplasty. 2011;26(8): 1265-1272. [36]Demirkale I, Tecimel O, Sesen H, et al. Nondrainage decreases blood transfusion need and infection rate in bilateral total knee arthroplasty. J Arthroplasty. 2014;29(5): 993-997. [37]Li C, Nijat A, Askar M. No clear advantage to use of wound drains after unilateral total knee arthroplasty: a prospective randomized, controlled trial. J Arthroplasty. 2011;26(4): 519-522.[38]任国清,刘红云,滕学仁,等.人工全膝关节置换后是否放置引流管:随机对照试验[J].中国组织工程研究,2016,20(22):3219-3226.[39]Roy N, Smith M, Anwar M, et al. Delayed release of drain in total knee replacement reduces blood loss. A prospective randomised study. Acta Orthop Belg. 2006;72(1):34-38.[40]Mutsuzaki H, Watanabe A, Komatsuzaki T, et al. Investigation of perioperative safety and clinical results of one-stage bilateral total knee arthroplasty in selected low-risk patients. J Orthop Surg Res. 2018;13(1):14. [41]Lane GJ, Hozack WJ, Shah S, et al. Simultaneous bilateral versus unilateral total knee arthroplasty. Outcomes analysis. Clin Orthop Relat Res. 1997;(345):106-112.[42]Courtney PM, Melnic CM, Alosh H, et al. Is bilateral total knee arthroplasty staged at a one-week interval safe? A matched case control study. J Arthroplasty. 2014;29(10):1946-1949. [43]Parvizi J, Chaudhry S, Rasouli MR, et al. Who needs autologous blood donation in joint replacement? J Knee Surg. 2011;24(1):25-31.[44]Kamath AF, Austin DC, Derman PB, et al. Saline-coupled bipolar sealing in simultaneous bilateral total knee arthroplasty. Clin Orthop Surg. 2014;6(3):298-304.[45]Kim C, Park SS, Dhotar HS, et al. Topical tranexamic acid reduces transfusion rates in simultaneous bilateral total knee arthroplasty: a retrospective case series. Can J Surg. 2017; 60(5):311-315.[46]Jenny JY, Trojani C, Prudhon JL, et al. Simultaneous bilateral total knee arthroplasty. A multicenter feasibility study. Orthop Traumatol Surg Res. 2013;99(2):191-195. [47]Sheffy N, Bentov I, Mills B, et al. Perioperative hypotension and discharge outcomes in non-critically injured trauma patients, a single centre retrospective cohort study. Injury. 2017;48(9):1956-1963.[48]Yu Z, Yao L, Yang Q. Tranexamic acid plus diluted-epinephrine versus tranexamic acid alone for blood loss in total joint arthroplasty: A meta-analysis. Medicine (Baltimore). 2017;96(24):e7095. |
| [1] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [2] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [3] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [4] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [5] | Zhang Chao, Lü Xin. Heterotopic ossification after acetabular fracture fixation: risk factors, prevention and treatment progress [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1434-1439. |
| [6] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [7] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [8] | Liu Xiangxiang, Huang Yunmei, Chen Wenlie, Lin Ruhui, Lu Xiaodong, Li Zuanfang, Xu Yaye, Huang Meiya, Li Xihai. Ultrastructural changes of the white zone cells of the meniscus in a rat model of early osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1237-1242. |
| [9] | Yuan Jun, Yang Jiafu. Hemostatic effect of topical tranexamic acid infiltration in cementless total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 873-877. |
| [10] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [11] | Cao Xuhan, Bai Zixing, Sun Chengyi, Yang Yanjun, Sun Weidong. Mechanism of “Ruxiang-Moyao” herbal pair in the treatment of knee osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 746-753. |
| [12] | Li Yonghua, Feng Qiang, Tan Renting, Huang Shifu, Qiu Jinlong, Yin Heng. Molecular mechanism of Eucommia ulmoides active ingredients treating synovitis of knee osteoarthritis: an analysis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 765-771. |
| [13] | Song Shan, Hu Fangyuan, Qiao Jun, Wang Jia, Zhang Shengxiao, Li Xiaofeng. An insight into biomarkers of osteoarthritis synovium based on bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 785-790. |
| [14] | Deng Zhenhan, Huang Yong, Xiao Lulu, Chen Yulin, Zhu Weimin, Lu Wei, Wang Daping. Role and application of bone morphogenetic proteins in articular cartilage regeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 798-806. |
| [15] | Liu Xin, Yan Feihua, Hong Kunhao. Delaying cartilage degeneration by regulating the expression of aquaporins in rats with knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 668-673. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||