Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (21): 5403-5410.doi: 10.12307/2026.590
Previous Articles Next Articles
Mechanical analysis of a bone cement-augmented cortical bone trajectory screw versus a new variable-diameter all-cortical bone screw
Xie Xuechen1, Julaiti·Maitirouzi1, Li Chunchao1, Zhang Le1, Wang Yixi2, Paerhati·Rexiti2
- 1Institute of Intelligent Manufacturing and Modern Industry, Xinjiang University, Urumqi 830017, Xinjiang Uygur Autonomous Region, China; 2First Affiliated Hospital of Xinjiang Medical University, Urumqi 830054, Xinjiang Uygur Autonomous Region, China
-
Accepted:2025-03-14Online:2026-07-28Published:2026-03-03 -
Contact:Julaiti·Maitirouzi, Associate professor, Institute of Intelligent Manufacturing and Modern Industry, Xinjiang University, Urumqi 830017, Xinjiang Uygur Autonomous Region, China -
About author:Xie Xuechen, Master candidate, Institute of Intelligent Manufacturing and Modern Industry, Xinjiang University, Urumqi 830017, Xinjiang Uygur Autonomous Region, China -
Supported by:Third China Health and Longevity Innovation Competition of Chinese Academy of Medical Sciences, No. 2022-JKCS-19 (to PR); “Tianshan Talents” Medical and Health High-level Talent Training Program Fund Project, No. TSYC202301B026 (to PR)
CLC Number:
Cite this article
Xie Xuechen, Julaiti·Maitirouzi, Li Chunchao, Zhang Le, Wang Yixi, Paerhati·Rexiti. Mechanical analysis of a bone cement-augmented cortical bone trajectory screw versus a new variable-diameter all-cortical bone screw[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(21): 5403-5410.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
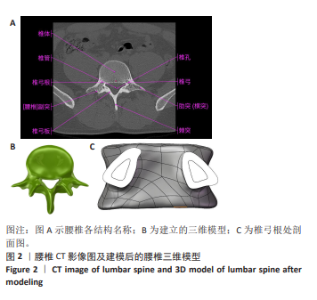
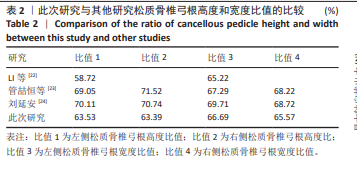
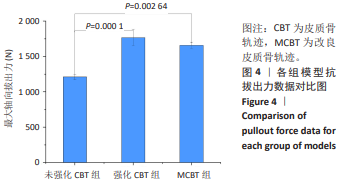
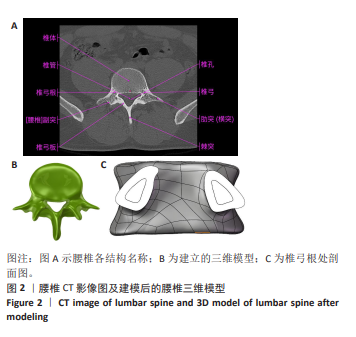
2.1 模型验证 2.1.1 形态学验证 此文选用在骨质疏松椎体中表现更好的CBT技术来进行模型验证。建立CBT所需要的全皮质骨螺纹螺钉,将腰椎三维模型的各部分几何结构与CT扫描显示的腰椎实际形态进行对照,见图2A,同时,将实验模型中的皮质骨与松质骨分布与解剖后腰椎的相应分布进行对比,成功地实现了高度还原性,能够精确模拟腰椎横突、棘突、椎弓根等各个部位,见图2B。骨水泥强化CBT、CBT、MCBT 3种技术进钉路径均经过椎弓根,在固定中起主要作用的是皮质骨,所以皮质骨的占比量直接影响螺钉内固定的性能,所以对椎弓根中皮质骨松质骨的占比参数验证很有必要。目前文献对测定椎弓根的占比参数主要是测定椎弓根峡部的相关数据,此次研究将3组L4腰椎模型导入到SolidWorks 2022中进行测量,测量时椎弓根处剖面图如图2C所示,3组模型的平均测量比值结果如表2所示,经对比与此次研究的测量结果相似,验证了模型的有效性。 2.1.2 拔出力验证 此次有限元分析结果显示,拔出力为(1 210±44.44) N,而参照文献获得的拔出力为(1 254.99±305.40) N[11]、(1 376±254) N[12]。此次研究与所参照文献中呈现的实验数据相近,这有力地证实了此文所构建腰椎模型的有效性。"
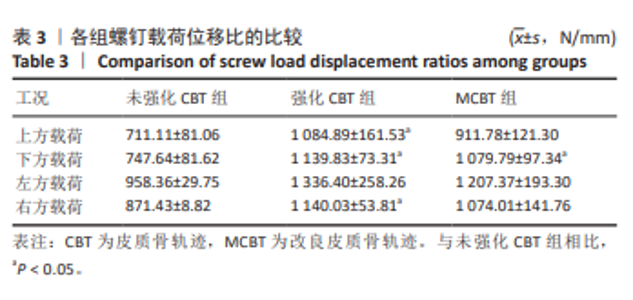
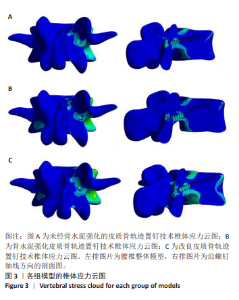
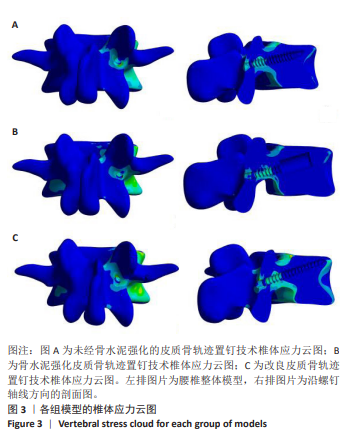
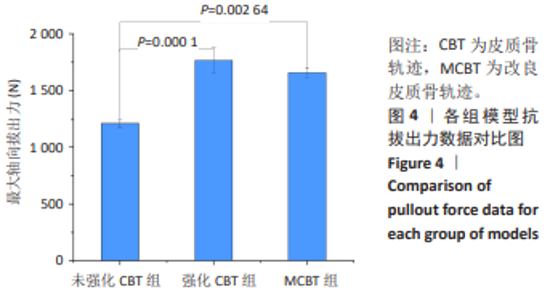
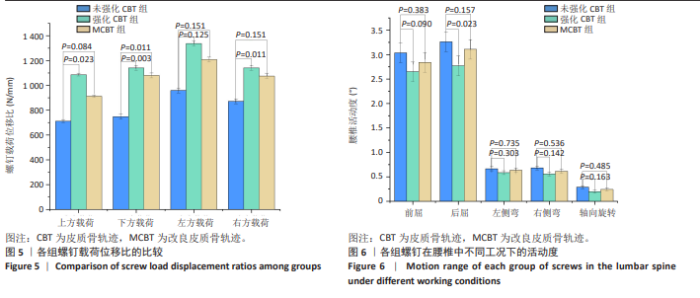
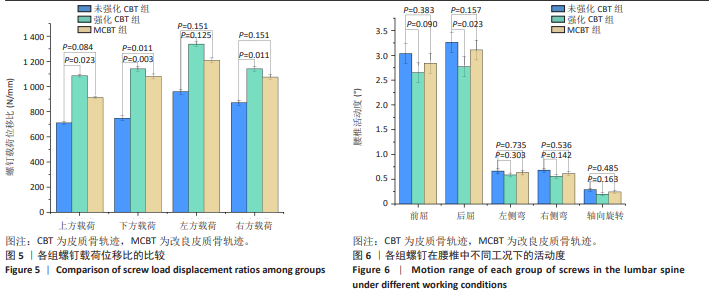
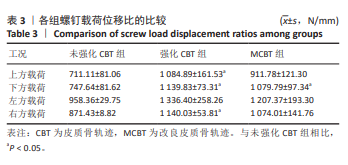
2.3 螺钉稳定性 强化CBT组在上、下、右3种工况下较未强化CBT组均有较大提升,差异有显著性意义(t=-3.592,P=0.023;t=-6.192,P=0.003;t=-8.689 0,P=0.011)。在左方工况,骨水泥强化CBT组的螺钉稳定性比未强化CBT组提升但无显著性差异(t=-2.518 7,P=0.125)。在上、下、左、右工况,对比强化CBT组,MCBT组螺钉稳定性虽有细微下降,但这些变化并无显著性差异(t=-0.402,P=0.708;t=-0.853,P=0.445;t=-0.694,P=0.529;t=-0.756,P=0.516),见表3及图5。另外观察到3组螺钉稳定性中的左侧位移载荷比均明显大于其余3个工况,这与CBT及MCBT技术的置钉技术有关,进钉点更靠近棘突,棘突与椎板交汇处的皮质骨更厚,在施加左侧载荷时,螺钉受到皮质骨影响比其他工况更为明显,所以在螺钉受到向左的力时对力的抵抗能力更强。"
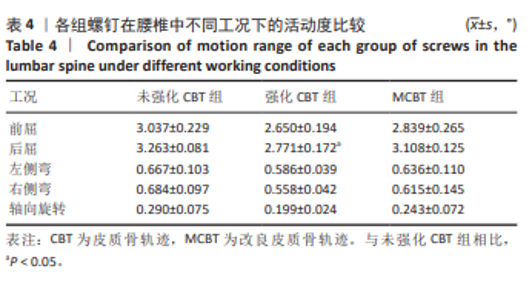
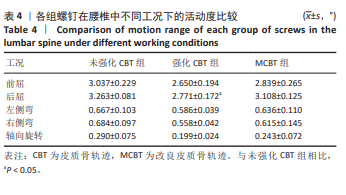
2.4 椎体活动度 在后屈工况下,强化CBT组的腰椎活动度较未强化CBT组显著减少,差异有显著性意义(t=4.492 0,P=0.023 2)。在分析左、右侧弯和轴向旋转工况下,强化CBT组与未强化CBT组之间的比较结果显示,均出现了降低的趋势,但这些变化无显著性差异(t=1.283 8,P=0.303;t=2.053 9,P=0.142;t=1.990 3,P=0.163)。在比较强化CBT组与MCBT组的椎体活动度时,发现在前屈、后屈、左、右侧弯和轴向旋转5种工况下强化CBT组的活动度相较于MCBT组有所减少,但是并无显著性差异(t=-1.000 9,P=0.378 3;t=-2.742 4,P=0.057 0;t=-0.746 8,P=0.519 5;t=-0.647 3,P=0.575 5;t=-1.005 7,P=0.404 1)。在不同工况下,椎体的活动度差异详见表4及图6。"
| [1] 中国老年保健医学研究会老年疼痛疾病分会. 老年骨质疏松性疼痛诊疗与管理中国专家共识(2024版)[J]. 中国疼痛医学杂志, 2024,30(4):241-250. [2] ADLER RA, EL-HAJJ FULEIHAN G, BAUER DC, et al. Managing osteoporosis in patients on long-term bisphosphonate treatment:report of a task force of the American society for bone and mineral reserch. Bone Miner Res. 2016;31(1):16-35. [3] 颜金祥,刘家明,刘子豪,等.不同部位骨质疏松性骨折的患病率调查[J].中华骨与关节外科杂志,2024,17(1):79-83. [4] 万江,刘达,张映波,等.椎体CT值在脊柱外科中的应用研究进展[J].解放军医学杂志,2025,50(7):911-916. [5] AMIROUCHE F, SOLITRO GF, MAGNAN BP. Stability and Spine Pedicle Screws Fixation Strength-A Comparative Study of Bone Density and Insertion Angle. Spine Deform. 2016;4:261-267. [6] HOPPE S, KEEL MJ. Pedicle screw augmentation in osteoporotic spine:indications, limitations and technical aspects. Eur J Trauma Emerg Surg. 2017;43:3-8. [7] MAKHCHOUNE M, COLLARD X, TRIFFAUX M, et al. The utility of the CADISS® system in the dissection of epidural fibrosis in revision lumbar spine surgery (A case series). Ann Med Surg (Lond). 2022;83:104718. [8] LILI Y, WANG S, ZHU Z, et al. Biomechanical Analysis of Cortical Bone Trajectory Screw Versus Bone Cement Screw for Fixation in Porcine Spinal Low Bone Mass Model. Clin Spine Surg. 2023;36(4):145-152. [9] Santoni BG, Hynes RA, McGilvray KC, et al. Cortical bone trajectory for lumbar pedicle screws. Spine J. 2009;9(5):366-373. [10] 王海峰,曾忠友,裴斐,等.后路腰椎椎间融合术中使用皮质骨轨迹椎弓根螺钉或传统椎弓根螺钉治疗骨质疏松性腰椎退行性疾病[J].脊柱外科杂志,2024,22(6):411-416. [11] MATSUKAWA K, YATO Y, IMABAYASHI H, et al. Biomechanical evaluation offixation strength among different sizes of pedicle screws using the cortical bone trajectory:what is the ideal screw size for optimalfixation. Acta Neurochir. 2016;158:465-471. [12] WANG Y, YANG L, LI C, et al. A Biomechanical Study on Cortical Bone Trajectory Screw Fixation Augmented With Cement in Osteoporotic Spines. Global Spine J. 2022;13(8):21925682211070826. [13] GUO S, ZHU K, YAN M, et al. Cortical bone trajectory screws in the treatment of lumbar degenerative disc disease in patients with osteoporosis. World J Clin Cases. 2022;10(36):13179-13188. [14] REXITI P, ABUDUREXITI T, ABUDUWALI N, et al. Measurement of lumbar isthmus parameters for novel starting points for cortical bone trajectory screws using computed radiography. Am J Transl Res. 2018;10(8):2413-2423. [15] CHEN CH, CHEN DC, HUANG HM, et al. Level-based analysis of screw loosening with cortical bone trajectory screws in patients with lumbar degenerative disease. Medicine (Baltimore). 2020;99(40):e22186. [16] PASOTO SG, AUGUSTO KL, ALVARENGA JC, et al. Cortical bone density and thickness alterations by high-resolutimn peripheral quantitative computed tomography: association with vertebral fractures in primary sjögren’s syndrome. Rheumatology (Oxford). 2016;55(12):2200-2211. [17] 任亚楠,张泓,韩剑英,等. 空心侧孔螺钉联合骨水泥强化术对椎体生物力学影响的有限元分析[J]. 天津理工大学学报,2024,40(6): 128-133. [18] 任航宁,居来提·买提肉孜,帕尔哈提·热西提,等.皮质骨轨迹椎弓根系统拔出力下腰椎的有限元分析[J].中国组织工程研究, 2021,25(36):5771-5776. [19] 周志豪,阿拉法特·卡哈尔,王轶希,等.传统椎弓根螺钉与改良皮质骨轨迹置钉技术的生物力学性能有限元分析[J].中国组织工程研究,2022,26(18):2789-2794. [20] 裴卉宁,陈允峰,白仲航,等.弹射救生过程飞行员胸腰椎高负荷损伤分析[J].北京航空航天大学学报报,2025,51(1):102-112. [21] 王轶希,居来提·买提肉孜,王水泉,等.有限元分析腰椎传统椎弓根钉道和改良皮质骨钉道的生物力学性能[J].医用生物力学, 2022,37(3):485-491. [22] LI B, JIANG B, FU Z, et al. Accurate determination of isthmus of lumbar pedicle: a morphometric study using reformatted computed tomographic images. Spine. 2004;29(21):2438-2444. [23] 管喆恒,杨惠林,罗宗平, 等.腰椎椎弓根CT影像学参数的测量与临床意义[J].中国组织工程研究,2018,22(11):1743-1748. [24] 刘延安.腰椎椎弓根延长术中截骨平面影像解剖数据测量与分析[D].苏州:苏州大学,2017. [25] MATSUKAWA K, YATO Y, IMABAYASHI H. Impact of screw diameter and length on pedicle screw fixation strength in osteoporotic vertebrae:A finite element analysis. Asian Spine J. 2021;15(5):566-574. [26] REXITI P, AIKEREMU D, WANG S, et al. Cadaveric study of anatomical measurement of isthmus parameters of lumbar spine to guide cortical bone screw placement. Rev Assoc Med Bras (1992). 2022;68(6):754-758. [27] 木再帕尔·买吐送,肖扬,古丽米热·阿迪力,等.新型全皮质骨螺纹螺钉在腰椎改良皮质骨轨迹螺钉技术中的生物力学性能[J].中国组织工程研究,2025,29(27):5765-5772. [28] 张治豪,居来提·买提肉孜,张连鹏,等.新型变径全皮质骨螺纹螺钉设计以及在腰椎改良皮质骨轨迹的应用[J].医用生物力学, 2024,39(1):91-97. [29] 张连鹏,居来提·买提肉孜,张治豪,等.皮质骨轨迹置钉在腰椎翻修中的力学分析[J].中国组织工程研究,2024,28(24):3783-3788. [30] MATSUKAWA K, YATO Y, IMABAYASHI H. Impact of screw diameter and length on pedicle screw fixation strength in osteoporotic vertebrae: a finite element analysis. Asian Spine J. 2021;15(5):566-574. [31] ZHANG S, LIU Z, LU C, et al. Oblique lateral interbody fusion combined with different internal fixations for the treatment of degenerative lumbar spine disease: a finite element analysis. BMC Musculoskelet Disord. 2022;23(1):206. [32] ZHANG L, LI HM, ZHANG R, et al. Biomechanical changes of adjacent and fixed segments through cortical bone trajectory screw fixation versus traditional trajectory screw fixation in the lumbar spine: a finite element analysis. World Neurosurg. 2021;151:e447-e456. [33] TOBING SDAL, WISNUBAROTO RP. Pull-out strength comparison among conventional pedicle screw,cortical infero-superior, and cortical superoinferior trajectories in yorkshire porcine lumbar spines: a biomechanical study. Int J Spine Surg. 2020;14(4):580-584. [34] ZHANG RJ, SHEN CL. Research status and existing problems of lumbar pedicle double-trajectory screw technique. Zhonghua Yi Xue Za Zhi. 2023;103(9):635-639. |
| [1] | Chen Huiting, Zeng Weiquan, Zhou Jianhong, Wang Jie, Zhuang Congying, Chen Peiyou, Liang Zeqian, Deng Weiming. Tail anchoring technique of vertebroplasty in treatment of osteoporotic vertebral compression fractures with intravertebral cleft: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2145-2152. |
| [2] | Cheng Qisheng, Julaiti·Maitirouzi, Xiao Yang, Zhang Chenwei, Paerhati·Rexiti. Finite element analysis of novel variable-diameter screws in modified cortical bone trajectory of lumbar vertebrae [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2162-2171. |
| [3] | Liu Jiafu, Ren Ruxia, Liao Zhouwei, Zhou Xiali, Wu Yihong, Zhang Shaoqun. Three-dimensional finite element analysis of cervical spine biomechanical characteristics in a rat model of cervical vertigo [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2182-2190. |
| [4] | Liu Wenlong, Dong Lei, Xiao Zhengzheng, Nie Yu. Finite element analysis of tibial prosthesis loosening after fixed-bearing unicompartmental knee arthroplasty for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2191-2198. |
| [5] | Zheng Wangyang, Fei Ji, Yang Di, Zhao Lang, Wang Lingli, Liu Peng, Li Haiyang. Finite element analysis of the force changes of the supraspinatus tendon and glenohumeral joint during the abduction and flexion of the humerus [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2199-2207. |
| [6] | Cai Qirui, Dai Xiaowei, Zheng Xiaobin, Jian Sili, Lu Shaoping, Liu Texi, Liu Guoke, Lin Yuanfang. Mechanical effects of Long’s traction orthopedic method on cervical functional units: quantitative analysis of biomechanical model of head and neck [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2208-2216. |
| [7] | Rao Jingcheng, Li Yuwan, Zheng Hongbing, Xu Zhi, Zhu Aixiang, Shi Ce, Wang Bing, Yang Chun, Kong Xiangru, Zhu Dawei. Biomechanical differences between the new proximal femoral stable intramedullary nail and traditional intramedullary nail#br# [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2217-2225. |
| [8] | Chen Long, Wang Xiaozhen, Xi Jintao, Lu Qilin. Biomechanical performance of short-segment screw fixation combined with expandable polyetheretherketone vertebral body replacement in osteoporotic vertebrae [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2226-2235. |
| [9] | Zhang Zizheng, Luo Wang, Liu Changlu. Application value of finite element analysis on unicompartmental knee arthroplasty for medial knee compartmental osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2313-2322. |
| [10] | Li Qingbin, Lin Jianhui, Huang Wenjie, Wang Mingshuang, Du Jiankai, Lao Yongqiang. Bone cement filling after enlarged curettage of giant cell tumor around the knee joint: a comparison of subchondral bone grafting and non-grafting [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1896-1902. |
| [11] | Zheng Xuying, Hu Hongcheng, Xu Libing, Han Jianmin, Di Ping. Stress magnitude and distribution in two-piece cement-retained zirconia implants under different loading conditions and with varying internal connection shapes [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1979-1987. |
| [12] | Zhong Caihong, Xiao Xiaoge, Li Ming, Lin Jianhong, Hong Jing. Biomechanical mechanism of sports-related patellar tendinitis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1417-1423. |
| [13] | Xu Hao, Ding Lu, Li Xiao. Mechanical effect of mechanical wear of abutment screws on the Morse taper connection implant system: a three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1375-1383. |
| [14] | Shang Depeng, Wei Haiyu, Yang Fan. Finite element analysis for three different types of internal screw fixation in treatment of severe lumbar 1 vertebral body fractures [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 537-545. |
| [15] | Yu Xinlin, Chen Huiyu, Wang Yingying, Guo Weizhong, Feng Bin Lin Chengshou, Lin Wang. Finite element analysis of internal fixation with new retrograde intramedullary nail on lateral femur condyle for distal type A2 femur fractures [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(3): 546-552. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||