Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (18): 2906-2911.doi: 10.12307/2024.038
Previous Articles Next Articles
Construction of shoulder joint complex model and finite element research and progress in this field
Zeng Yuyuan1, Yang Zhen2, You Yihang1, Zhang Enshui3, Zhang Tao3
- 1Shandong First Medical University (Shandong Academy of Medical Sciences), Jinan 250000, Shandong Province, China; 2Weifang Medical University, Weifang 261000, Shandong Province, China; 3Jinan Central Hospital, Jinan 250014, Shandong Province, China
-
Received:2023-03-01Accepted:2023-04-14Online:2024-06-28Published:2023-08-26 -
Contact:Zhang Tao, MD, Associate chief physician, Master’s supervisor, Jinan Central Hospital, Jinan 250014, Shandong Province, China Zhang Enshui, MD, Attending physician, Jinan Central Hospital, Jinan 250014, Shandong Province, China -
About author:Zeng Yuyuan, Master candidate, Shandong First Medical University (Shandong Academy of Medical Sciences), Jinan 250000, Shandong Province, China -
Supported by:Clinical Medicine Science and Technology Innovation Program of Jinan Science and Technology Bureau, No. 202019037 (to ZES); Science and Technology Development Program of Jinan Science and Technology Bureau, No. 20120206 (to ZT)
CLC Number:
Cite this article
Zeng Yuyuan, Yang Zhen, You Yihang, Zhang Enshui, Zhang Tao. Construction of shoulder joint complex model and finite element research and progress in this field[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(18): 2906-2911.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
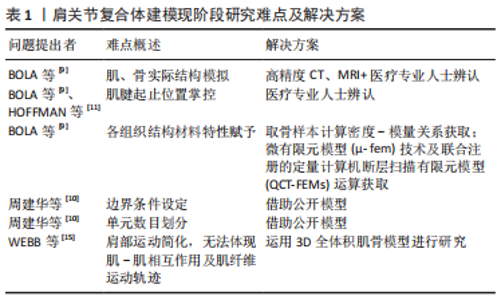
2.1 肩关节复合体的模型验证及相关研究 有限元分析方法在骨科的应用方式多样,从预测骨折发生机制,到评估手术效果、指导手术技术革新,应用于骨科临床多领域的探讨。DAHAN等[4]通过有限元模型分析结合实验模型,预测了肱骨近端解剖颈骨折的发生机制。MENEGAZ等[5]及GAO等[6]则将有限元分析方法运用于对肩锁关节脱位的手术技术探讨,对手术技术的革新提供了一定的技术支持。WANG等[7]通过对比肱骨干骨折术后旋转不良的生物力学环境,发现术中复位不佳致肱骨近端内旋畸形,将使得关节盂和肱骨头前下部应力过于集中,会导致肩关节退行性疾病的发生;复位不佳所致的外旋畸形则会导致肩部相对较低的应力分布,可能会增加肩关节脱位的风险,为骨折的术后康复情况做出了合理预测。ELWALL等[8]则开发并验证了全肩及反肩置换术后的肩关节肌骨模型,为关节假体的设计优化提供了可行性选择。以上这些有限元技术应用,都表明有限元技术可以从疾病发生机制、治疗方案决策、术后康复预期及内植物设计优化等各个方面为临床决策服务。 BOLA等[9]通过对比肩关节有限元建模与实验模型之间的各种工况下的应力、应变情况,并借助统计学方法验证了各数据并不存在明显统计学差异,证实了有限元模型对复杂生物力学研究的可行性及必要性。此外,在其实验过程中,提出有限元建模是否可靠,需解决如下难点:肌肉、骨骼的实际结构,肌肉的起止位置及材料特性。除上述几点外,周建华等[10]在其研究中也指出:边界条件设定、单元数目的划分均会对结果的精准造成一定影响。肌肉、骨骼的实际结构的保证,可以通过高精度CT及MRI获得,并在建模过程中通过医疗专业人士对各组织结构的精确辨认得以实现;但对肌肉的起止位置的把控,往往会出现些许误差。HOFFMAN等[11]通过计算肩袖、三角肌的生理作用线以评估力矩臂与肌腱起止点之间的相关性,其实验过程模拟了外展、内收及旋转的动态运动范围,并与HIK等[12] 的数据进行对比,发现肌肉插入点的错误会导致动作线预测结果的背道而驰。对于材料特性的把控,既往多通过取骨标本的方法作为计算密度-模量关系的“金标准”,而KNOWLES等[13]通过微有限元模型(μ- fem)技术及联合注册的定量计算机断层扫描有限元模型(QCT-FEMs),对肩胛骨骨小梁进行密度-模量关系的运算,发现运算结果与传统力学测试结果相近,微有限元模型(μ- fem)技术能准确确定骨小梁骨的生物力学性能。既拓宽了有限元技术的应用领域,又与传统力学测试对材料特性的研究相辅相成。 早期有限元研究集中于静力学分析,但对于人体复杂运动而言,运动状态分析显得越来越迫切。既往在肩关节领域,为缩小计算量,多将肩部运动时肌肉模型简化为线段的简单收缩,例如SADEQI等[14]所开发的一套开源的肩关节有限元模型,其模型对肩关节各活动角度下盂肱关节的应力与既往数据对比,保证了模型的分析精度,模型发布于github.com/OSEL-DAM/ShoulderFiniteElementModel以供后来者使用。然而这种将肩部肌肉运动的简化,必然使得对于肌肉-肌肉间相互作用及复杂的肌肉纤维运动轨迹等情况难以在运算结果中体现。WEBB等[15]通过对比基于线段的三角肌模型和3D三角肌模式,指出传统的线段模型并不能准确反映肌肉间机械耦合的影响,且难以约束肌肉路径,使得模型运算的力矩臂将随着肩关节旋转而变化,而3D模型则能准确预测各肌肉内纤维间的力矩臂的显著变化。这项研究结果也对之后的肌-骨模型的有限元分析提出了更高的要求。鉴于肩关节建模的复杂性,ELWELL等[8]开发并验证了一套开源的肩关节全体积肌骨模型,发布于Https://simtk.org/projects/das,为后续的肩关节研究提供了可予以借鉴的模型。 肩关节有限元研究目前存在诸多研究难点,作者将既往研究中所指出的难点及目前的解决方案归纳如表1所示。今后的人体有限元研究,将更需要多学科、多领域共同合作才能实现对模型运算结果精准度的把控,同时,基础领域的不断研究深入,也对既往研究结果的可信度提出了新的挑战。"
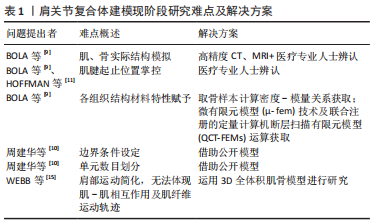
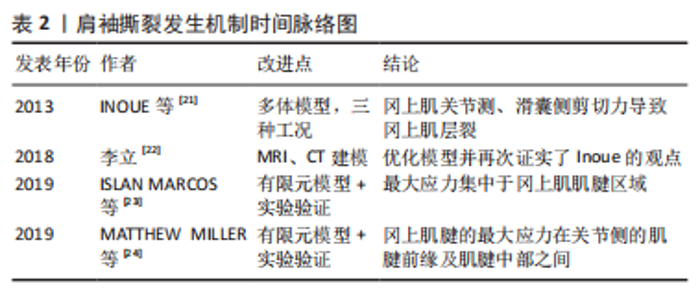
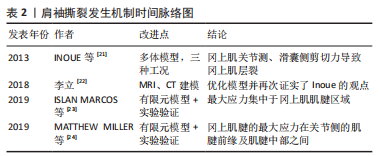
2.2 肩袖撕裂的有限元研究 肩袖是由冈上肌、冈下肌、小圆肌及肩胛下肌4块肌肉组成,并如同袖套状结构包裹、控制盂肱关节活动,门诊主诉为肩痛的患者中,半数以上患有肩袖撕裂[16]。肩袖撕裂发生机制主要分为内源性理论和外源性理论两大类。简言之,内源性理论认为肩袖撕裂是由于肌腱的退行性改变所致;外源性理论则认为肩袖撕裂的产生,是由于肩袖组织的肩峰下撞击或明确外伤史所产生的[17]。而近年来对撞击的深入研究又将撞击分为肩峰下撞击、喙突撞击、后上内部撞击及前上内部撞击4种情况[18]。EL-AMIN等[19]通过统计学研究,发现喙突形态、肌腱脂肪浸润程度、喙肱间隙、肩肱间隙、喙突过度覆盖等与肩袖撕裂的发生均存在相关性。VIEHOFER等[20]通过3D有限元模型发现,较大的临界肩角倾向于导致盂肱关节的不稳定,从而使得在外展过程中需要更强的冈上肌拉力维持稳定,并合理推测大临界肩角是诱发冈上肌撕裂的原因。有限元分析方法主要的研究倾向于对外源性机制的加深探讨。 既往的肩关节有限元研究文献,多存在模型过度简化、模型工况单一的情况。INOUE等[21]通过CT图像,建模了包含有冈上肌、冈下肌及肩胛下肌3块主要肩袖组织及肱骨、肩胛骨的多体模型,并模拟了0°,45°及90°外展角下3种工况,其在研究中发现,随着外展角度的增大,冈上肌腱关节侧、滑囊侧应力及两者间的应力差值均在不断增大,由此合理猜测两层间的剪切应力导致冈上肌腱的层裂。李立[22]在其基础上改进,通过MRI、CT数据分别建模肌腱软组织及骨骼结构,充分保证了建模结构的准确性,并通过空间位置匹配,还原了完整且仿真的肩关节复合体结构,其研究模拟了更多的外展角度,支持了前者的研究结果。 除模型过于简化及工况模拟欠缺外,材料赋值简化、缺少实验验证也是需不断改进的方向。ISLAN MARCOS等[23]为了追求在不修改初始网格的情况下,实现同一关节不同位置的有限元分析,将韧带、肌肉等可变形的解剖结构使用1D梁单元,而对关节骨骼、肌腱等使用3D体单元,建模了一个包含肩袖主要肌肉(冈上肌、冈下肌、肩胛下肌、小圆肌)、韧带、盂唇、软骨及肩胛骨、肱骨等骨骼结构的完整肩关节模型,分别分析:①重力情况无外力;②重力+50 N垂直于盂唇方向压力;③重力+50 N沿重力方向下拉力3种工况下的受力情况,并将所运算结构与实际工况下的人体关节加载状态对比,验证了建模的准确性,从而发现:①对于骨骼而言,最大应力在肌骨交界处;②对于软骨而言,最大应力在盂肱关节软骨的前下部;③对于肌肉肌腱而言,最大应力表现在肌腱区域。MATTHEW MILLER等[24]则建模了含有冈上肌腱的3D有限元模型,并采集尸体标本上观察区域的特定几何结构及特定位置的材料属性进行应变运算及验证,分析了60°,70°及90°外展情况,发现冈上肌腱的最大张力在关节侧的肌腱前缘及肌腱中部之间。这两项研究均对之后的有限元建模研究起到了一定的借鉴作用。各研究对肩袖撕裂发生机制的探讨,归纳如表2。"
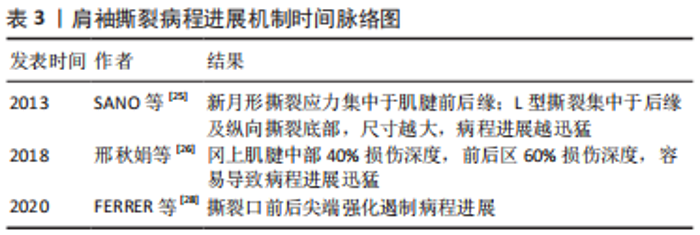
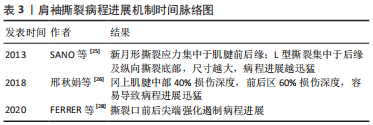
然而,既往的有限元研究多集中于机械应力引发肌腱组织撕裂的假设去探讨肩袖撕裂病因,少有对撕裂发展机制的探讨。为实现对撕裂发展机制探讨,可通过建模过程中刻意构建病理模型而实现。SANO等[25]通过构建新月形及L型肩袖撕裂模型,模拟了外展、外旋的运动过程,发现新月形撕裂的高应力集中在肌腱前、后缘;L型撕裂则集中于肌腱后缘及纵向撕裂的底部;对于撕裂尺寸而言,尺寸越大、则撕裂的病程进展越迅速。邢秋娟等[26]通过CT构建包含有冈上肌、肱骨及肩胛骨的简易模型,发现冈上肌腱的应力主要集中于肌腱的中部,其次为前、后部,并同时发现当冈上肌腱中部损伤深度达40%,前后区损伤深度达60%时,周围肌腱应力会过度集中,从而建议此时应尽快行手术治疗。除了模拟病理模型外,亦可通过对肌腱的多次赋值创造差异而进行研究。MILLER等[27]通过对冈上肌腱赋予不同退变程度的力学参数,得出退变越严重,撕裂的进展则越迅猛。FERRER等[28]则在1 cm冈上肌撕裂病理模型上,分别模拟了前后尖端提升50%胶原纤维模量、前后尖端降低50%胶原纤维模量、内外侧中点附近降低50%胶原纤维模量,并加入空白对照,对这4种情况模拟从而得出:在撕裂前后尖端的强化对撕裂的进一步扩大具有阻遏作用,为后续的肩袖治疗的研究提供了一定理论指导。对肩袖撕裂病程进展机制的探讨,归纳如表3。"
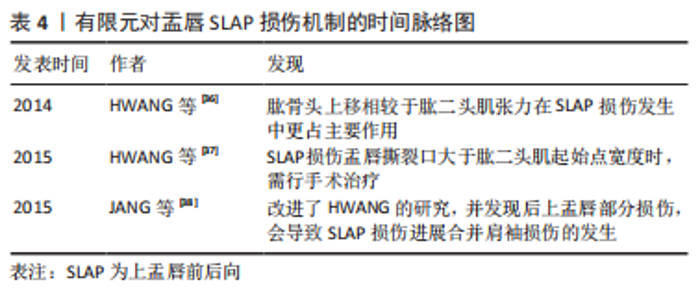
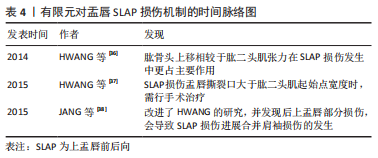
对于肩袖撕裂治疗方案选择,涉及缝合方式、锚钉固定效能等多方面考量。既往研究普遍认为增大肌骨接触面积,可使得应力分布分散,缝合效果更佳[29]。除对缝合方式的探讨外,缝线锚钉的置入角度也会对缝合效果产生影响。包呼日查等[30]通过3D有限元模型,模拟了45°,90°两种锚钉置入角度,并得出90°的置入角度所获得的应力更分散,更不易出现缝合失败的情况。对于植入物锚钉的拔出机制,CHEVALIER 等[31]通过micro CT分别构建微型有限元(micro finite element,μFE)模型及均质化有限元(homogenized classical FE models,hFE)模型并对比进行锚钉拔出实验,并得出结论:均质化有限元模型用于评估骨锚定的可行性,并且认为通过骨水泥等方式加固植入点的周围骨表观密度、多载荷背景下的修补强度、植入物的场景等均会对骨锚定固定强度造成影响。SANO等[32]通过对TwinFix Ti植入锚钉的3D有限元分析,发现当锚钉的平均拉应力载荷< 75.4 N时,锚钉固定效果尚可,如若大于这个数值,将会导致锚钉的固定失效,为之后的相关锚钉固定效果评估给出了可借鉴的数据。同年,SANO等[33]又对TwinFix Ti,HEALICOIL PK 及HEALICOIL RG 3种锚钉进行了肩袖缝合强度测试,得出如下结论:①TwinFix Ti锚钉主要应力集中于骨表面螺纹处,易导致该处出现固定失败;②HEALICOIL RG锚钉具备最佳的初始固定效能。 肩袖撕裂是临床肩痛主诉中最常见的疾病,由于肩关节复杂的运动方式,肩袖撕裂模型具备建模简单、组件较少及运算结果易收敛等优势,早些年的文献对肩袖撕裂的研究报道较多,主要集中于对肩袖撕裂的发生、发展机制的探讨较多,也有对治疗方案决策优化的探讨。借助有限元分析方法,使得目前对肩袖撕裂的治疗已趋于规范,由此可见有限元分析方法在临床工作决策中不可或缺的价值。随着有限元建模及对肩关节生理结构的研究的深入,越来越多的研究已往盂唇损伤及肩关节置换等方向进展。 2.3 肩关节盂唇损伤的有限元研究 肩关节作为活动度最大的人体关节,代价是牺牲了一部分关节稳定性,故肩关节脱位在临床中较为常见。肩关节脱位发生后,通常伴有软组织损伤,盂唇作为盂肱关节的主要被动稳定结构之一,常常在肩关节脱位后发生损伤。KLEMT等[34]借助有限元模型,模拟了在生理关节负荷下盂唇对盂肱关节稳定性贡献的定量分析,并认为盂唇对肩关节的稳定性占11.5%-27.1%[男(19.3±7.8)% ;女(18.1±5.9)%],且盂唇后下方及下方结构对盂肱关节稳定性尤甚。盂唇在盂肱关节中,有增加关节窝的深度及凹度,并抵抗肱骨头平移的作用[35]。近年来,随着运动医学领域的发展,越来越多的研究聚焦在盂唇等软组织结构。 既往研究认为,上盂唇前后向(superior labrum anterior posterior,SLAP)损伤机制可能是:①由于肱骨头受压及肱二头肌腱联合作用;②肱二头肌腱的牵拉及扭曲所致。HWANG等[36]通过构建包含有肱骨、肩胛骨、盂唇、软骨及肱二头肌的有限元盂肱关节模型,模拟了肱二头肌4种张力(0,22,55及88 N)及肱骨头缓慢向上(0-5 mm,以1 mm为分析步)平移对盂唇应变的影响,并认为在盂唇SLAP损伤中,肱骨上移相较于肱二头肌张力更占主导地位。随后,HWANG等[37]又运用了类似模型,模拟了不同大小SLAP撕裂时肱二头长头肌腱张力对撕裂传播的影响,并认为当盂唇应变大于40%时,撕裂进展将不可避免,从而得出当盂唇撕裂口大于肱二头肌腱盂唇起始处宽度时,应积极进行手术治疗的结论。遗憾的是,其研究并未对手臂位置进行探讨。JANG等[38]通过模拟肱骨从0°外展位到外展外旋位的运动过程中,观察肩关节内各结构撞击行为,其建立了健康对照组及SLAP损伤观察组2个模型,发现当存在SLAP损伤时,后上盂唇部分由于失去了对肱骨头的间隔作用(The Spacer Effect),导致肱骨头后上脱位,进而导致肩袖损伤的发生。各研究成果的时间脉络图归纳如表4。"
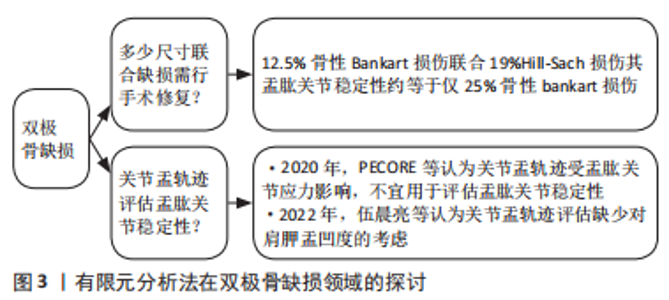
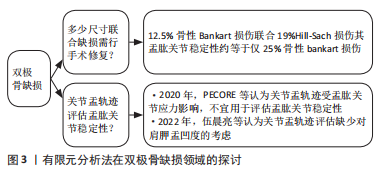
但肩关节脱位发生时,除造成关节盂盂唇、关节盂骨质等结构损伤外,还会因与肱骨头撞击的相互力学作用,导致肱骨头处的骨质损伤,这种双极骨缺损将导致肩关节复位后脱位的再发生。有研究表明,双极骨缺损的发生在复发性肩关节前向不稳患者中甚至可高达68%-90%及77%-100%[39-40]。WALIA等[41]通过构建包含4种宽度缺损(12.5%,25%,37.5%及50%)缺损的关节盂骨性Bankart损伤及4种直径缺损(6%,19%,31%,44%)的肱骨头Hill-Sach损伤模型,采用位移控制的准静态分析方法,得出双极骨缺损的盂肱关节稳定性较仅骨性Bankart损伤的盂肱稳定性显著降低,其在实验运算后得出12.5%骨性Bankart损伤联合19%Hill-Sach损伤其盂肱关节稳定性约等于仅25%骨性bankart损伤,而当关节盂处存在25%骨性Bankart损伤,正是行植骨手术治疗的临界点。对双极骨缺损的手术决策,早在十余年前,便有学者提出肩胛盂轨迹的概念进行术前评估[42]。然而这一概念的准确性,如今仍存在争议。通过构建肩关节有限元模型,PECORE等[43]重现了双极骨缺损病理情况,并对肩胛盂轨迹进行测量,虽然其计算数值与其他研究结果相近,但也发现肩胛盂轨迹的参数会受盂肱关节应力的影响,因此认为肩胛盂轨迹不应作为评估前盂肱关节不稳的普遍参考。随后,伍晨亮等[44]也在其研究中指出,目前的肩胛盂轨迹模型存在诸如肩胛盂轨迹宽度公式系数有待优化、缺少对肩胛盂凹度的考量等缺陷。有限元分析应用于双极骨缺损的探讨如图3所示。"

对于盂唇损伤的治疗,多根据损伤程度大小进行手术决策,然而既往研究多聚焦于非生理情况下的临界值探讨。KLEMT等[45]通过模拟完整肩关节模型在完成30次日常生活活动时,评估肩胛盂骨缺损大小对发生脱位的风险,从而认为当肩胛盂缺损长度大于16%时,在日常生活活动中,脱位风险明显增高,此时即需行植骨手术治疗。这项研究进一步扩大了行植骨手术的肩胛盂缺损临界值。除对手术决策进行指导外,有限元技术也运用于对手术方式的深入探讨。INOUE等[46]通过构建Bankart修复术肩关节有限元模型,分别比较了去除及保留肩胛盂前下软骨的2种Bankart修复术,进而探讨Bankart修复术后出现的肩胛盂骨吸收现象,并得出保留软骨并修复盂肱韧带复合体的手术方式,能够避免应力屏蔽(Stress Shielding)现象的发生,从而使得手术预后更佳。SANO等[47]则通过对比改良Bristow和Latarjet术这两种骨性Bankart植骨修复手术方式,根据植骨块的应力分布,得出两种术式的优劣:①Laterjet手术由于植骨块近端应力较低,容易出现应力屏蔽(Stress Shielding)现象而导致近端骨吸收、移植骨失败;②改良Bristow术则由于应力过于集中于固定螺钉处,使得术后固定螺钉断裂的风险增加。UNSAL等[48]则对比了传统Laterjet及等角Laterjet两种手术方式的应力分布情况,并认为虽然等角Laterjet手术提供了更佳的骨遮挡作用,避免了肩关节脱位的发生,但同时也导致了移植骨块近端应力减小,术后可能由于应力屏蔽作用导致骨吸收,且肩胛盂缺损宽度小于35%时,更不宜选用等角Laterjet技术进行治疗。 借助有限元分析方法,实现了切实有效的盂唇损伤发生机制及治疗方式等诸多方面的探讨、研究,对临床治疗方式决策也起到了指导作用。近年来,随着国内运动医学领域的不断发展,以往难以治疗的诸如肩关节创伤后习惯性脱位等疾病,也慢慢得以攻克。有限元分析从早年的材料赋值等探讨得以奠基,到如今模拟术后固定效能、指导手术决策,成为了临床工作不可或缺的一环。 2.4 肩关节置换的有限元研究 自1950年NEER首次提出半肩关节置换术治疗肩关节病变[49],由于肩关节独特的结构,后续不断发展出全肩关节置换术、反式肩关节置换术等其他术式,肩关节置换术的手术适应证扩大到治疗巨大肩袖损伤、严重炎性关节病等众多领域[50-53]。随着有限元技术的发展,对于临床上常见的手术技巧、手术方式的探讨,也在不断深入。 由于肩关节置换术中肱骨、肩胛骨部分同时存在密质骨、松质骨,且内植物人工关节与人体骨质间材料差异的影响,对肩关节置换术建模的材料赋值、运算收敛提出了不小的挑战。REEVES等[54]通过对比对模型赋予不同的骨小梁刚度关系,并观测评估:①种植体-骨骼接触百分比;②体积-质量的Von Mises应力变化;③吸收/形成骨量与初始骨量的百分比3个指标,认为在肩关节置换术研究中,可对骨骼结构赋予人体其他部位的非均质数据,并不会对运算结果造成大的误差,这一研究结果也支持了既往对骨小梁赋值的其他简化方式[55]。 在假体设计方面,有限元分析技术也贡献了一些研究成果。众所周知,内植物材料特性与周围骨质结构差异会导致肩关节置换术后的不良预后,诸如老年骨质疏松患者,容易因应力屏蔽作用致骨吸收现象的发生。SOLTANMOHAMMADJ等[56]由髋关节置换术中股骨端空心柄的启发,对肩关节置换术中肱骨端空心柄结构进行有限元分析,并认为在保持空心柄强度的前提下,空心柄仅减少了少部分骨吸收骨量,相对于髋关节假体的空心柄使用,肩关节假体使用空心柄结构对患者受益度有限。ARENAS-MIQUELEZ 等[57]利用CT数据建模,分析对比了肱骨端不同颈干角假体数据,认为145°颈干角结合肩盂球4 mm的偏侧化和2 mm的下位偏心处理对术后活动范围改善最为明显。这两项研究均对之后的肩关节假体设计提供了一定的理论支持及指导。 对于手术方式的探讨,半肩关节置换由于对肩胛盂结构要求完整、骨质要求良好等术前要求,较少对其进行有限元分析研究,目前主要集中在对全肩关节置换术及反式全肩关节置换术的研究。BOLA等[58]通过对体外全肩关节置换术后模型进行有限元建模分析,得出全肩关节置换术后,盂肱关节最大主应变集中在肩胛骨前端,最小主应变在肩胛骨后侧,肱骨侧的前后区域应变相近,这一研究对行全肩关节置换术后假体周围骨折的发生部位具备前瞻性预测作用。相比于以恢复正常解剖结构为主的全肩关节置换术,当患者合并有严重肩袖损伤的肩关节骨性关节炎时,反式全肩关节置换术具备更广泛的适应证[59]。但由于假体设计及手术技术等原因,临床上最常见的手术并发症就是肩胛骨切迹。ELWELL等[60]通过尸体肩关节CT模型,模拟了在临床上为避免肩胛骨切迹发生所采用的偏移旋转中心的手术技术,发现虽然偏移旋转中心使得术后肩关节内收活动度增大,达到了避免肩胛骨切迹发生的目的,但同时也使得肩盂基座微动产生,使得内植物寿命将会降低。 肩关节置换术的有限元研究由于受限于多组件材料赋值复杂、难以准确模拟体内各组织间负荷及边界条件等原因,较研究其他肩部组织结构的有限元研究更少,但随着有限元技术的不断发展及对有限元研究方法的不断探索优化,未来的工作必将涉及更多目前尚未解决的问题,诸如关节置换术后关节不稳、脱位,不同手术技术对术后康复的预测等方面。"

| [1] ABOUELKHAIR F, DUPREY S. Assessing shoulder posture ergonomy thanks to a finite element analysis. Comput Methods Biomech Biomed Engin. 2012; 15 Suppl 1:348-349. [2] ZHENG M, ZOU Z, BARTOLO PJ, et al. Finite element models of the human shoulder complex: a review of their clinical implications and modelling techniques. Int J Numer Method Biomed Eng. 2017;33(2):e02777. [3] BOLSTERLEE B, VEEGER DH, CHADWICK EK. Clinical applications of musculoskeletal modelling for the shoulder and upper limb. Med Biol Eng Comput. 2013;51(9):953-963. [4] DAHAN G, TRABELSI N, SAFRAN O, et al. Finite element analyses for predicting anatomical neck fractures in the proximal humerus. Clin Biomech (Bristol, Avon). 2019;68:114-121. [5] MENEGAZ GL, GOMIDE LC, ARAUJO CA. Biomechanical evaluation of acromioclavicular joint reconstructions using a 3-dimensional model based on the finite element method. Clin Biomech (Bristol, Avon). 2019;70:170-176. [6] GAO R, ZHANG W, YANG Y, et al. Evaluation of the coracoid bone tunnel placement on Dog Bone button fixation for acromioclavicular joint dislocation: a cadaver study combined with finite element analysis. BMC Musculoskelet Disord. 2023;24(1):18. [7] WANG C, MA XY, LU LT, et al. A finite element model of the shoulder: application to the changes of biomechanical environment induced by postoperative malrotation of humeral shaft fracture. BMC Musculoskelet Disord. 2022;23(1):525. [8] ELWELL JA, ATHWAL GS, WILLING R. Development and validation of a muscle wrapping model applied to intact and reverse total shoulder arthroplasty shoulders. J Orthop Res. 2018;36(12):3308-3317. [9] BOLA M, SIMOES J, RAMOS A. Finite element model validation based on an experimental model of the intact shoulder joint. Med Eng Phys. 2021;87:1-8. [10] 周建华,王跃.有限元分析在骨科中的应用及研究进展[J].实用医院临床杂志,2018,15(1):205-208. [11] HOFFMANN M, BEGON M, LAFON Y, et al. Influence of glenohumeral joint muscle insertion on moment arms using a finite element model. Comput Methods Biomech Biomed Engin. 2020;23(14):1117-1126. [12] HIK F, ACKLAND DC. The moment arms of the muscles spanning the glenohumeral joint: a systematic review. J Anat. 2019;234(1):1-15. [13] KNOWLES NK, LANGOHR GDG, FAIEGHI M, et al. A comparison of density-modulus relationships used in finite element modeling of the shoulder. Med Eng Phys. 2019;66:40-46. [14] SADEQI S, BAUMANN AP, GOEL VK, et al. A Validated Open-Source Shoulder Finite Element Model and Investigation of the Effect of Analysis Precision. Ann Biomed Eng. 2023;51(1):24-33. [15] WEBB JD, BLEMKER SS, DELP SL. 3D finite element models of shoulder muscles for computing lines of actions and moment arms. Comput Methods Biomech Biomed Enging. 2012;17(8):829-837. [16] KANATLI U, GEMALMAZ HC, OZTURK BY, et al. The role of radiological subacromial distance measurements in the subacromial impingement syndrome. Eur J Orthop Surg Traumatol. 2013;23(3):317-322. [17] 范宁,藏磊,袁硕,等.有限元分析在肩袖撕裂中的应用进展[J].中华创伤骨科杂志,2021,23(8):732-736. [18] GARVING C, JAKOB S, BAUER I, et al. Impingement Syndrome of the Shoulder. Dtsch Arztebl Int. 2017;114(45):765-776. [19] EL-AMIN S F, 3RD, MAFFULLI N, MAI MC, et al. Coracoid Impingement and Morphology Is Associated with Fatty Infiltration and Rotator Cuff Tears. J Clin Med. 2022;11(9):2661. [20] VIEHOFER AF, GERBER C, FAVRE P, et al. A larger critical shoulder angle requires more rotator cuff activity to preserve joint stability. J Orthop Res. 2016;34(6):961-968. [21] INOUE A, CHOSA E, GOTO K, et al. Nonlinear stress analysis of the supraspinatus tendon using three-dimensional finite element analysis. Knee Surg Sports Traumatol Arthrosc. 2013;21(5):1151-1157. [22] 李立.肩关节复合体有限元建模及肱骨外展动作中肩袖生物力学分析[D].上海:上海交通大学,2018. [23] ISLAN MARCOS M, LECHOSA URQUIJO E, BLAYA HARO F, et al. Behavior under Load of A Human Shoulder: Finite Element Simulation and Analysis. J Med Syst. 2019;43(5):132. [24] MATTHEW MILLER R, THUNES J, MUSAHL V, et al. A Validated, Specimen-Specific Finite Element Model of the Supraspinatus Tendon Mechanical Environment. J Biomech Eng. 2019;141(11):111003. [25] SANO H, HATTA T, YAMAMOTO N, et al. Stress distribution within rotator cuff tendons with a crescent-shaped and an L-shaped tear. Am J Sports Med. 2013;41(10):2262-2269. [26] 邢秋娟,赵东峰,戴薇薇,等.冈上肌部分损伤对肌腱应力分布影响的有限元分析[J].实用骨科杂志,2018,24(6):519-522. [27] MILLER RM, THUNES J, MAITI S, et al. Effects of Tendon Degeneration on Predictions of Supraspinatus Tear Propagation. Ann Biomed Eng. 2019;47(1): 154-161. [28] FERRER GA, FORTUNATO RN, MUSAHL V, et al. Effect of localized tendon remodeling on supraspinatus tear propagation. J Biomech. 2020;108:109903. [29] MANTOVANI M, PELLEGRINI A, GAROFALO P, et al. A 3D finite element model for geometrical and mechanical comparison of different supraspinatus repair techniques. J Shoulder Elbow Surg. 2016;25(4):557-563. [30] 包呼日查,齐岩松,陶立元,等.肩袖损伤修补金属锚钉置入角度——有限元分析[J].中华肩肘外科电子杂志,2019,7(1):56-62. [31] CHEVALIER Y. Numerical Methodology to Evaluate the Effects of Bone Density and Cement Augmentation on Fixation Stiffness of Bone-Anchoring Devices. J Biomech Eng. 2015;137(9). doi: 10.1115/1.4030943. [32] SANO H, IMAGAWA K, YAMAMOTO N, et al. Predicting failures of suture anchors used for rotator cuff repair: a CT-based 3-dimensional finite element analysis. Biomed Mater Eng. 2015;25(4):371-380. [33] SANO H, TOKUNAGA M, NOGUCHI M, et al. Comparison of fixation properties between coil-type and screw-type anchors for rotator cuff repair: A virtual pullout testing using 3-dimensional finite element method. J Orthop Sci. 2016;21(4):452-457. [34] KLEMT C, NOLTE D, GRIGORIADIS G, et al. The contribution of the glenoid labrum to glenohumeral stability under physiological joint loading using finite element analysis. Comput Methods Biomech Biomed Engin. 2017;20(15):1613-1622. [35] DRURY NJ, ELLIS BJ, WEISS JA, et al. The impact of glenoid labrum thickness and modulus on labrum and glenohumeral capsule function. J Biomech Eng. 2010;132(12):121003. [36] HWANG E, CARPENTER JE, HUGHES RE, et al. Effects of biceps tension and superior humeral head translation on the glenoid labrum. J Orthop Res. 2014;32(11):1424-1429. [37] HWANG E, HUGHES RE, PALMER ML, et al. Effects of biceps tension on the torn superior glenoid labrum. J Orthop Res. 2015;33(10):1545-1551. [38] JANG SW, YOO YS, LEE HY, et al. Stress Distribution in Superior Labral Complex and Rotator Cuff During In Vivo Shoulder Motion: A Finite Element Analysis. Arthroscopy. 2015;31(11):2073-2081. [39] NAKAGAWA S, IUCHI R, HANAI H, et al. The Development Process of Bipolar Bone Defects From Primary to Recurrent Instability in Shoulders With Traumatic Anterior Instability. Am J Sports Med. 2019;47(3):695-703. [40] GOLIJANIN P, PEEBLES L, ARNER JW, et al. Advanced 3-Dimensional Characterization of Hill-Sachs Lesions in 100 Anterior Shoulder Instability Patients. Arthroscopy. 2021;37(11):3255-3261. [41] WALIA P, MINIACI A, JONES MH, et al. Influence of Combined Hill-Sachs and Bony Bankart Defects on Range of Motion in Anterior Instability of the Shoulder in a Finite Element Model. Arthroscopy. 2015;31(11):2119-2127. [42] YAMAMOTO N, ITOI E, ABE H, et al. Contact between the glenoid and the humeral head in abduction, external rotation, and horizontal extension: a new concept of glenoid track. J Shoulder Elbow Surg. 2007;16(5):649-656. [43] PECORA JOR, NEVES JUNIOR AT, ROESLER CRM, et al. Glenoid track evaluation by a validated finite-element shoulder numerical model. Orthop Traumatol Surg Res. 2020;106(4):735-742. [44] 伍晨亮,赵金忠.肩胛盂轨迹概念在肩关节前向不稳诊疗中的应用与挑战[J].国际骨科学杂志,2022,43:261-266. [45] KLEMT C, TODERITA D, NOLTE D, et al. The critical size of a defect in the glenoid causing anterior instability of the shoulder after a Bankart repair, under physiological joint loading. Bone Joint J. 2019;101-B(1):68-74. [46] INOUE K, SUENAGA N, OIZUMI N, et al. Glenoid bone resorption after Bankart repair: finite element analysis of postoperative stress distribution of the glenoid. J Shoulder Elbow Surg. 2021;30(1):188-193. [47] SANO H, KOMATSUDA T, ABE H, et al. Intra-articular biomechanical environment following modified Bristow and Latarjet procedures in shoulders with large glenoid defects: relationship with postoperative complications. J Shoulder Elbow Surg. 2021;30(10):2260-2269. [48] UNSAL SS, YILDIRIM T, KAYALAR M. Comparison of two coracoid process transfer techniques on stress shielding using three-dimensional finite-element model. J Orthop Surg Res. 2022;17(1):371. [49] NEER CS 2ND, CRAIG EV, FUKUDA H. Cuff-tear arthropathy. J Bone Joint Surg Am. 1983;65(9):1232-1244. [50] RUGG CM, COUGHLAN MJ, LANSDOWN DA. Reverse Total Shoulder Arthroplasty: Biomechanics and Indications. Curr Rev Musculoskelet Med. 2019;12(4):542-553. [51] ERNSTBRUNNER L, ANDRONIC O, GRUBHOFER F, et al. Long-term results of reverse total shoulder arthroplasty for rotator cuff dysfunction: a systematic review of longitudinal outcomes. J Shoulder Elbow Surg. 2019;28(4):774-781. [52] HARITINIAN E G, BELGAID V, LINO T, et al. Reverse versus anatomical shoulder arthroplasty in patients with intact rotator cuff. Int Orthop. 2020; 44(11):2395-2405. [53] AIM F, MARION B, KERROUMI Y, et al. One- or two-stage exchange for periprosthetic shoulder infection: Systematic review and meta-analysis. Orthop Traumatol Surg Res. 2020;106(1):5-15. [54] REEVES JM, ATHWAL GS, JOHNSON JA, et al. The Effect of Inhomogeneous Trabecular Stiffness Relationship Selection on Finite Element Outcomes for Shoulder Arthroplasty. J Biomech Eng. 2019;141(3). doi: 10.1115/1.4042172. [55] REIMERINGER M, NUNO N, DESMARAIS-TREPANIER C, et al. The influence of uncemented femoral stem length and design on its primary stability: a finite element analysis. Comput Methods Biomech Biomed Engin. 2013; 16(11):1221-1231. [56] SOLTANMOHAMMADI P, TAVAKOLI A, LANGOHR GDG, et al. Structural analysis of hollow versus solid-stemmed shoulder implants of proximal humeri with different bone qualities. J Orthop Res. 2022;40(3):674-684. [57] ARENAS-MIQUELEZ A, MURPHY RJ, ROSA A, et al. Impact of humeral and glenoid component variations on range of motion in reverse geometry total shoulder arthroplasty: a standardized computer model study. J Shoulder Elbow Surg. 2021;30(4):763-771. [58] BOLA M, SIMOES JA, RAMOS A. Finite element modelling and experimental validation of a total implanted shoulder joint. Comput Methods Programs Biomed. 2021;207:106158. [59] 柳金浪,段志豪,周游.反式全肩关节置换的研究进展[J].中国矫形外科杂志,2021,29:2063-2066. [60] ELWELL J, CHOI J, WILLING R. Quantifying the competing relationship between adduction range of motion and baseplate micromotion with lateralization of reverse total shoulder arthroplasty. J Biomech. 2017;52:24-30. |
| [1] | Li Zhifei, Yang Yin, Chen Hualong, Liang Qinqiu, Zhong Yuanming, Zhang Yisheng. Finite element analysis of the correlation between tilt angle of titanium cage and postoperative subsidence of titanium cage after anterior subtotal cervical corpectomy, decompression and fusion [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1313-1319. |
| [2] | Chen Mengmeng, Bao Li, Chen Hao, Jia Pu, Feng Fei, Shi Guan, Tang Hai. Biomechanical characteristics of a novel interspinous distraction fusion device BacFuse for the repair of lumbar degenerative disease [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1325-1329. |
| [3] | Liang Cheng, Zhang Linqi, Wang Guan, Li Wen, Duan Ke, Li Zhong, Lu Xiaobo, Zhuo Naiqiang. Finite element and biomechanical analysis of different implants in repair for unilateral unstable pelvic posterior ring injury [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1336-1341. |
| [4] | Yang Junliang, Lu Tan, Xu Biao, Jiang Yaqiong, Wang Fucheng. Three-dimensional finite element analysis of effects of partial anterior cruciate ligament rupture on knee joint stress [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1347-1353. |
| [5] | Min Meipeng, Wu Jin, URBA RAFI, Zhang Wenjie, Gao Jia, Wang Yunhua, He Bin, Fan Lei. Role and significance of artificial intelligence preoperative planning in total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1372-1377. |
| [6] | Shan Jiaxin, Zhang Yilong, Wu Hongtao, Zhang Jiayuan, Li Anan, Liu Wengang, Xu Xuemeng, Zhao Chuanxi. Changes in muscle strength and pain in patients receiving Jianpi Yiqi Huoxue Formula after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1378-1382. |
| [7] | Qi Haodong, Lu Chao, Xu Hanbo, Wang Mengfei, Hao Yangquan. Effect of diabetes mellitus on perioperative blood loss and pain after primary total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1383-1387. |
| [8] | Li Xiaoqiang, Chen Wei, Li Mingyue, Shan Tianchi, Shen Wen. Value of preoperative quantitative ultrasound analysis of quadriceps femoris in predicting chronic post-surgical pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1388-1393. |
| [9] | Weng Rui, Lin Dongxin, Guo Haiwei, Zhang Wensheng, Song Yuke, Lin Hongheng, Li Wenchao, Ye Linqiang. Abnormal types of intervertebral disc structure and related mechanical loading with biomechanical factors [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1436-1442. |
| [10] | Xiaheida·Yilaerjiang, Nijiati·Tuerxun, Reyila·Kuerban, Baibujiafu·Yelisi, Chen Xin. Three-dimensional finite element analysis of the distribution pattern of stress in bone tissues with different characteristics [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(8): 1277-1282. |
| [11] | Wang Qiang, Li Shiyun, Xiong Ying, Li Tiantian. Biomechanical changes of the cervical spine in internal fixation with different anterior cervical interbody fusion systems [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 821-826. |
| [12] | Wei Yuanbiao, Lin Zhan, Chen Yanmei, Yang Tenghui, Zhao Xiao, Chen Yangsheng, Zhou Yanhui, Yang Minchao, Huang Feiqi. Finite element analysis of effects of sagittal cervical manipulation on intervertebral disc and facet joints [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 827-832. |
| [13] | Zhang Rui, Wang Kun, Shen Zicong, Mao Lu, Wu Xiaotao. Effects of endoscopic foraminoplasty and laminoplasty on biomechanical properties of intervertebral disc and isthmus [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 833-839. |
| [14] | Kang Zhijie, Cao Zhenhua, Xu Yangyang, Zhang Yunfeng, Jin Feng, Su Baoke, Wang Lidong, Tong Ling, Liu Qinghua, Fang Yuan, Sha Lirong, Liang Liang, Li Mengmeng, Du Yifei, Lin Lin, Wang Haiyan, Li Xiaohe, Li Zhijun. Finite element model establishment and stress analysis of lumbar-sacral intervertebral disc in ankylosing spondylitis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 840-846. |
| [15] | Zhang Min, Peng Jing, Zhang Qiang, Chen Dewang. Mechanical properties of L3/4 laminar decompression and intervertebral fusion in elderly osteoporosis patients analyzed by finite element method [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 847-851. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||