Chinese Journal of Tissue Engineering Research ›› 2024, Vol. 28 ›› Issue (9): 1420-1425.doi: 10.12307/2023.922
Previous Articles Next Articles
Interpretation of key points of International Framework for Examination of the Cervical Region for potential of vascular pathologies of the neck prior to Orthopaedic Manual Therapy (OMT) Intervention: International IFOMPT Cervical Framework
Feng Tianxiao1, Bu Hanmei1, Wang Xu1, Zhu Liguo1, Wei Xu2
- 1Second Department of Spine, 2Academic Development Office, Wangjing Hospital of China Academy of Chinese Medical Sciences, Beijing 100102, China
-
Received:2022-12-07Accepted:2023-02-08Online:2024-03-28Published:2023-07-26 -
Contact:Wei Xu, MD, Researcher, Academic Development Office, Wangjing Hospital of China Academy of Chinese Medical Sciences, Beijing 100102, China -
About author:Feng Tianxiao, Doctoral candidate, Second Department of Spine, Wangjing Hospital of China Academy of Chinese Medical Sciences, Beijing 100102, China -
Supported by:Cross Cooperation Project of Beijing Science and Technology New Star Program, No. 20220484228 (to WX); Traditional Chinese Medicine Inheritance and Innovation Team and Talent Support Plan Project of the State Administration of Traditional Chinese Medicine, No. ZYYCXTD-C-202003 (to ZLG)
CLC Number:
Cite this article
Feng Tianxiao, Bu Hanmei, Wang Xu, Zhu Liguo, Wei Xu. Interpretation of key points of International Framework for Examination of the Cervical Region for potential of vascular pathologies of the neck prior to Orthopaedic Manual Therapy (OMT) Intervention: International IFOMPT Cervical Framework[J]. Chinese Journal of Tissue Engineering Research, 2024, 28(9): 1420-1425.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
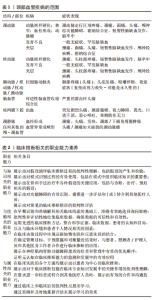

2.1 《IFOMPT 2020》内容概述 《IFOMPT 2020》全文由IFOMPT官方网站发布(www.ifompt.org)。该组织作为世界物理治疗联盟的子组织,一直致力于在世界范围内促进物理治疗师临床和学术标准的卓越和统一。《IFOMPT 2020》是目前国际上影响力较大的由权威物理治疗专业组织发布的聚焦于OMT与颈部血管疾病的国际标准,汇集了来自于系统评价、临床实践指南和专家共识的最佳证据。此标准制定目的在于为物理治疗师和教育者提供必要的信息以指导其在计划开展OMT干预前对颈部潜在的血管疾病进行充分评估。此标准旨在提供相关信息作为参考,而不是规定性内容,旨在增强临床医生的临床推断能力作为患者检查和治疗过程的重要组成部分,促进以患者为中心的临床实践。《IFOMPT 2020》的内容包括:①信息概要图;②标准的目标和范围;③以临床推断为基础的标准;④病史;⑤计划体格检查;⑥体格检查;⑦风险与效益;⑧共同决策、知情同意和医疗法律标准;⑨安全的OMT实践;⑩颈部OMT教学。 2.2 《IFOMPT 2020》要点解读 2.2.1 临床推断 颈部走行着向大脑提供血液供应的重要动脉系统即颈内动脉系和椎-基底动脉系,许多血管源性不良事件的发生与颈部OMT干预密切相关。此外有一系列颈部血管疾病可能以神经肌肉骨骼疼痛和功能障碍为主要症状表现如颈痛和头痛[19-20],见表1,这对物理治疗师临床推断能力提出了更高要求。为有效评估和治疗神经肌肉骨骼患者,《IFOMPT骨科手法治疗教育标准(2016)》从知识、技能、属性三方面列举出高水平临床推断能力的物理治疗师应具备的职业能力素养[1],见表2。"


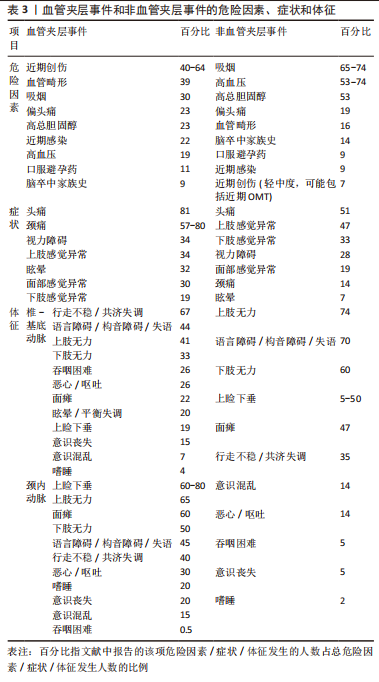
2.2.2 病史 《IFOMPT 2020》一个重要的更新要点在于强调病史采集的重要性。该标准指出良好的患者访谈过程对于评估患者目前症状的性质和严重程度,以及确定是否能使用OMT或需要进一步转诊检查至关重要。物理治疗师病史采集阶段的目标是根据现有信息对严重不良事件发生的可能性和存在的治疗禁忌证进行最佳判断。根据患者病史,物理治疗师应评估患者是否存在颈部血管疾病及发病倾向,识别与颈部血管疾病相关的可疑症状和体征以及诱发神经血管不良事件的危险因素。 《IFOMPT 2020》总结了颈部血管疾病的危险因素、症状和体征以利于物理治疗师的临床推断和最佳决策,见表3。同时,该标准也强调由于颈部血管疾病的病因和临床表现呈现复杂性和多因素特点,这些数据不能用于判断相对风险,而是为提高物理治疗师对临床推断的理解。"

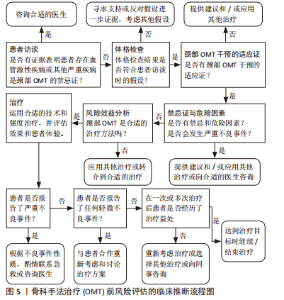
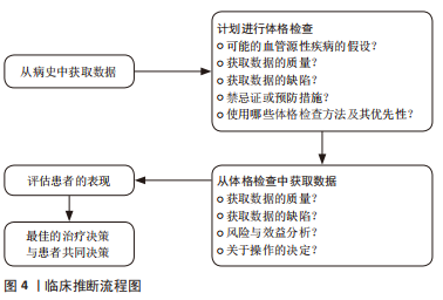
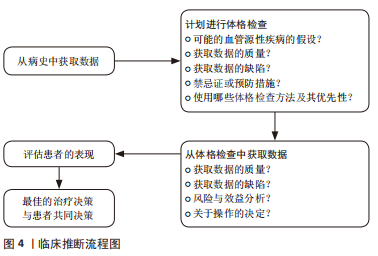
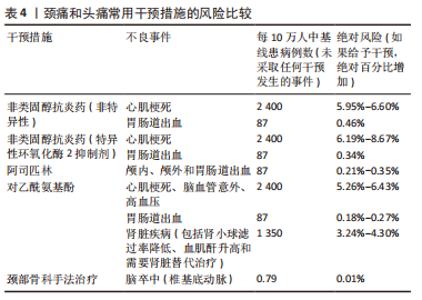
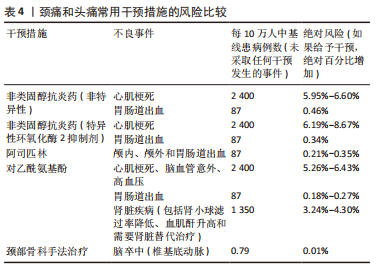
2.2.3 计划体格检查 《IFOMPT 2020》强调计划体格检查的必要性。物理治疗师通过分析病史中的临床数据形成主要的颈部血管疾病假设,并在体格检查中不断检验假设是临床推断的必要环节,是临床决策的基础条件。因此,物理治疗师需要详细地计划进行体格检查。物理治疗师也需要评估是否需要进一步获取患者的临床数据,所获取的信息是否存在缺陷以及临床数据质量是否足够。基于对患者病史数据的评估和分析,物理治疗师在此环节需要考虑:①OMT操作的注意事项;②OMT操作的禁忌证;③考虑到体格检查相关的风险因素,在体格检查中需要进行哪些项目以及需要排除哪些项目;④优先进行哪些体格检查项目;⑤这些体格检查是否适合患者。 2.2.4 体格检查 体格检查的目的旨在继续检验物理治疗师采集病史阶段产生的血管相关疾病假设,以决定是否需要医疗转诊或进行OMT干预。《IFOMPT 2020》和《IFOMPT 2012》相比主要差异在于前者删除了位置觉检查(positional testing)和颅颈韧带检查(craniovertebral ligament testing),更详细地描述血压、神经系统检查和颈动脉检查的重要性。《IFOMPT 2020》推荐的体格检查方法如下:①血压:血压测量可用以评估脑卒中的风险,特别是来源于颈动脉的风险,血压测量也可以评估急性动脉损伤风险如颈动脉和椎动脉;②神经系统检查:检查周围神经和颅神经以评估上运动神经元病变时的表现,将有助于评估神经血管疾病存在的可能性;③颈动脉检查:由于颈动脉的解剖位置相对表浅,物理治疗师可进行颈总动脉和颈内动脉的触诊和听诊。如双侧颈内动脉搏动不对称可能是颈内动脉疾病的重要特征,触诊到搏动性、可扩张的肿块常提示颈动脉瘤可能。听诊存在杂音常提示颈动脉瘤、颈动脉夹层和颈动脉狭窄等疾病可能。 2.2.5 风险与效益 (1)风险:由于OMT相关严重不良事件的发生率较低,现有临床数据难以支撑探究其风险与效益关系。临床诊疗过程中患者的症状和体征不同,已知的危险因素多样,这要求物理治疗师做到个体化评估患者的风险是否会增加并将风险降至最低。《IFOMPT 2020》指出物理治疗师需要考虑的风险主要包括两方面,即现有血管疾病的误诊风险和OMT后发生严重不良事件的风险。研究发现在一般人群中,椎动脉夹层发生率为(0.75-2.90)/10万[21-22],颈内动脉夹层发生率为椎动脉夹层的3-5倍[23-24]。绝大多数OMT导致的严重不良事件是由椎动脉受累所致,现有研究表明与OMT相关的椎动脉夹层发生率为(0.4-5.0)/10万[25],因此在OMT干预前需要进行合理的风险评估流程[26],见图5。同时,该标准总结了颈痛和头痛患者常用干预措施的风险,见表4。"
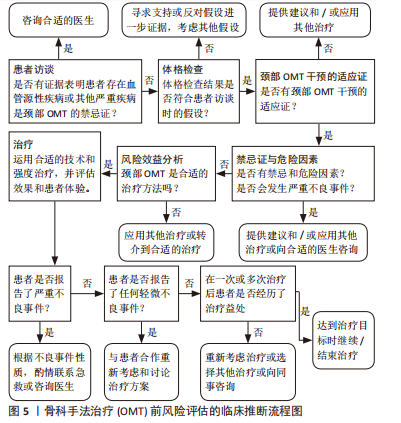
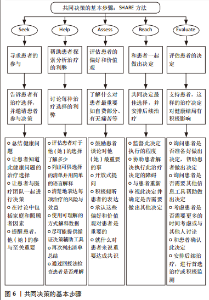
(2) 效益:多项系统评价和Meta分析发现,OMT能够降低颈痛和头痛患者的疼痛,改善功能障碍,提高生活质量。一项Cochrane系统综述显示,与对照组相比颈椎手法可显著改善颈痛患者的疼痛、颈椎功能和生活质量[2]。LOZANO LóPEZ等[3]研究发现,颈椎手法能够降低紧张性头痛患者头痛的频率和(或)强度,减少止痛药物使用,改善患者的生活质量。ZHU等[4]研究发现,中等质量证据表明颈椎手法能够改善神经根型颈椎病患者的颈痛症状。此外,HIDALGO等[5]研究发现,对于亚急性和慢性非特异性颈痛患者,颈椎手法联合运动疗法在改善疼痛、功能状态、患者满意度和生活质量方面优于单独运动疗法。然而颈椎手法联合运动疗法及单纯运动疗法治疗颈痛和头痛患者的有效性仍需高质量的临床证据支撑。 2.2.6 共同决策、知情同意和医疗法律标准 共同决策强调以患者为中心的临床诊疗过程即物理治疗师需要尊重和回应患者的偏好、需求和价值观并确保患者的价值观指导临床决策[27]。通过共同决策,物理治疗师或临床医生向患者传达可用的治疗方法、每种治疗方法的利弊、可能出现的结果以及目前科学研究中的不确定性等内容,患者表达自己的价值观及其认为相对重要的部分,医患共同做出最佳决策。共同决策推动了患者从医疗保健的被动接受者向主动参与者和监督者的转变,可有效改善医疗决策,提升服务质量。《IFOMPT 2020》推荐应用SHARE方法的5个步骤共同决策,分别为:①寻求患者的参与;②帮助患者探索和分析每项治疗的利弊;③评估患者的偏好和价值观;④和患者一起做决定;⑤评估患者的决定。如图6所示。"
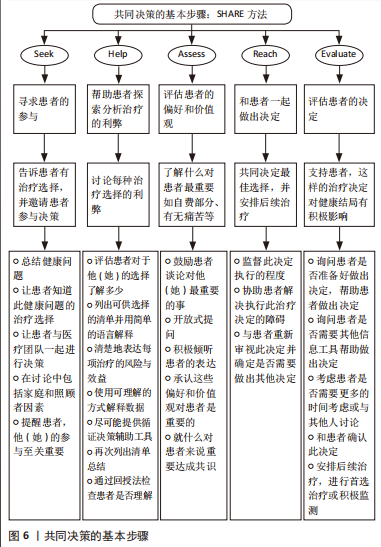

《IFOMPT 2020》建议物理治疗师在共享决策过程结束后获取患者知情同意。知情同意指患者在充分了解治疗或研究程序的性质、目的和影响基础上,自愿同意参与治疗或研究程序的可撤销的协议[28]。知情同意的过程主要包括知情同意的类型、物理治疗师提供信息的要求、获取信息的方式以及知情同意过程记录的要求。知情同意的类型包括明示同意和默示同意。明示同意是患者以书面或口头方式给予明确同意的类型。默示同意则是由物理治疗师根据患者的行为或缺乏某些行为暗示同意。《IFOMPT 2020》强调无论是哪种知情同意类型,患者在治疗期间都可以随时撤回,不应受物理治疗师影响。对于获取知情同意的时间,该标准指出物理治疗师应在治疗前取得知情同意,治疗过程中征取患者知情同意将不利于决策。对于治疗过程中治疗方案的改变,物理治疗师必须进行完整的知情同意程序,并以口头或书面形式明确获得同意。若继续进行相同的治疗方案,建议物理治疗师充分考虑患者的意愿,在多数情况下,患者口头同意继续使用干预措施即可。对于知情同意书的记录,建议物理治疗师对公开信息、知情同意的获取以及双方的讨论内容进行简要说明,建议每次治疗时均如实记录知情同意的获取情况。《IFOMPT 2020》是面向国际范围推广的标准,由于各地法律和卫生条例对知情同意的要求不同,并且考虑到患者病情和干预措施的特异性,该标准未提供标准化的表格和模板。 2.2.7 安全的OMT实践 《IFOMPT 2020》指出物理治疗师在选择和应用颈部OMT时应合理地考虑以下因素以保证颈部OMT的安全实践:①应用低振幅、短杠杆的推力即运用最小力量施加到颈椎的内部结构;②患者的安全和舒适是物理治疗师进行检查和选择治疗技术的基础,应充分尊重患者的偏好和价值观;③在颈椎生理活动范围的极限应谨慎使用检查和治疗技术,尤其是颈椎后伸和旋转,以免对颈部动脉和神经结构造成压迫;④鼓励患者采取仰卧位,一方面物理治疗师通过观察和沟通能够及时接收到反馈,另一方面此体位能够使患者感到舒适;⑤在操作前使患者在预置体位,以评估患者的舒适度和任何不适或意外的反应;⑥治疗频率根据患者病情及个人情况而定,建议联合使用颈椎手法、健康教育、运动疗法等多模式方法治疗颈痛和头痛;⑦应持续监测患者对颈部OMT的反应和不良事件的发生情况;⑧物理治疗师应合理地进行自我评估即是否具备安全有效地完成颈部OMT操作的能力。若临床技能有限,应推荐给在颈部OMT操作方面具有一定资质或已经过专业培训的物理治疗师;⑨在发生严重不良事件时,物理治疗师应迅速采取科学、有效的应急管理措施,必要时联系急救服务或进行心肺复苏。 2.2.8 颈部OMT教学 《IFOMPT 2020》从谁来教、教什么、如何教3个维度提供了建议。首先,颈部OMT的教育者应具备如下资质:①积极参与专业领域内的临床实践;②具有丰富的教学经验,最好包括在成人教育方面的指导或培训;③在临床实践和教学中应用循证医学的概念;④接受过颈椎手法的教学和运动心理方面的培训,经过权威机构或专业组织正式认证;⑤具有充足的神经肌肉骨骼相关疾病的体格检查、鉴别诊断和临床推断能力;⑥定期进行有关颈椎手法的专业学习和培训,并随时掌握最新的研究证据。对于教学内容,《IFOMPT 2020》指出手法教学需要符合最佳临床实践,注重手法安全实践,强调手法操作的振幅、速率、患者的舒适度、操作的敏感性和特异性,学生应在教师的指导下逐步锻炼手法的灵巧性和操作技能。对于如何教学方面,《IFOMPT 2020》指出虽然学生间手法练习是常用教学方式,但要强调安全操作,教师需要在学生练习前和练习过程中需要持续评估和检测风险因素和学生反应,让学生以适当方式锻炼手法的灵巧性,并尊重学生的自主选择,在任何时候均可以寻求教师的帮助。"

| [1] RUSHTON A, BEETON K, JORDAAN R, et al. IFOMPT Educational Standards Document. IFOMPT. 2016.https://www.ifompt.org/Educational+Standards/Standards+Document+2016.html [2] GROSS A, LANGEVIN P, BURNIE SJ, et al. Manipulation and mobilisation for neck pain contrasted against an inactive control or another active treatment. Cochrane Database Syst Rev. 2015;(9):CD004249. [3] LOZANO LÓPEZ C, MESA JIMÉNEZ J, DE LA HOZ AIZPURÚA JL, et al. Efficacy of manual therapy in the treatment of tension-type headache. A systematic review from 2000-2013. Neurologia. 2016;31(6):357-369. [4] ZHU L, WEI X, WANG S. Does cervical spine manipulation reduce pain in people with degenerative cervical radiculopathy? A systematic review of the evidence, and a meta-analysis. Clin Rehabil. 2016;30(2):145-155. [5] HIDALGO B, HALL T, BOSSERT J, et al. The efficacy of manual therapy and exercise for treating non-specific neck pain: A systematic review. J Back Musculoskelet Rehabil. 2017;30(6):1149-1169. [6] WHEDON JM, PETERSEN CL, LI Z, et al. Association between cervical artery dissection and spinal manipulative therapy -a medicare claims analysis. BMC Geriatr. 2022;22(1):917. [7] CHEN Y, MOFATTEH M, NGUYEN TN, et al. Carotid artery dissection and ischemic stroke following cervical chiropractic manipulation: Two case reports. Vasc Endovascular Surg. 2022;56(3):303-307. [8] GARG A, BATHLA G, MOLIAN V, et al. Differential risk factors and outcomes of ischemic stroke due to cervical artery dissection in young adults. Cerebrovasc Dis. 2020;49(5):509-515. [9] CHUNG CLR, CÔTÉ P, STERN P, et al. The association between cervical spine manipulation and carotid artery dissection: a systematic review of the literature. J Manipulative Physiol Ther. 2015;38(9):672-676. [10] RUSHTON A, RIVETT D, CARLESSO L, et al. International framework for examination of the cervical region for potential of Cervical Arterial Dysfunction prior to Orthopaedic Manual Therapy intervention. Man Ther. 2014;19(3):222-228. [11] RUSHTON A, CARLESSO LC, FLYNN T, et al. International Framework for Examination of the Cervical Region for potential of vascular pathologies of the neck prior to Orthopaedic Manual Therapy (OMT) Intervention: International IFOMPT Cervical Framework (2020). IFOMPT. 2020.https://www.ifompt.org/Research+and+Resources/OMPT+Frameworks+Research+and+Clinical+Resources.html [12] HUTTING N, KRANENBURG R, TAYLOR A, et al. Implementation of the International IFOMPT Cervical Framework: A survey among educational programmes. Musculoskelet Sci Pract. 2022;62:102619. [13] DE BEST RF, COPPIETERS MW, VAN TRIJFFEL E, et al. Interexaminer agreement and reliability of an internationally endorsed screening framework for cervical vascular risks following manual therapy and exercise: The Go4Safe Project. Phys Ther. 2021;101(10):pzab166. [14] HAWK C, WHALEN W, FARABAUGH RJ, et al. Best practices for chiropractic management of patients with chronic musculoskeletal pain: A clinical practice guideline. J Altern Complement Med. 2020; 26(10):884-901. [15] WHALEN W, FARABAUGH RJ, HAWK C, et al. Best-practice recommendations for chiropractic management of patients with neck pain. J Manipulative Physiol Ther. 2019;42(9):635-650. [16] KJAER P, KONGSTED A, HARTVIGSEN J, et al. National clinical guidelines for non-surgical treatment of patients with recent onset neck pain or cervical radiculopathy. Eur Spine J. 2017;26(9):2242-2257. [17] BIER J, SCHOLTEN-PEETERS W, STAAL B, et al. KNGF Clinical Practice Guideline for Physical Therapy in patients with neck pain. KNGF. 2016.https://www.kngf.nl/ [18] BONO CM, GHISELLI G, GILBERT TJ, et al. An evidence-based clinical guideline for the diagnosis and treatment of cervical radiculopathy from degenerative disorders. Spine J. 2011;11(1):64-72. [19] MURPHY DR. Current understanding of the relationship between cervical manipulation and stroke: what does it mean for the chiropractic profession? Chiropr Osteopat. 2010;18:22. [20] TAYLOR AJ, KERRY R. A ‘system based’ approach to risk assessment of the cervical spine prior to manual therapy. Int J Osteop Med. 2010; 13(3):85-93. [21] VARATHARAJAN S, FERGUSON B, CHROBAK K, et al. Are non-invasive interventions effective for the management of headaches associated with neck pain? An update of the Bone and Joint Decade Task Force on Neck Pain and Its Associated Disorders by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Eur Spine J. 2016; 25(7):1971-1999. [22] KRANENBURG HA, SCHMITT MA, PUENTEDURA EJ, et al. Adverse events associated with the use of cervical spine manipulation or mobilization and patient characteristics: A systematic review. Musculoskelet Sci Pract. 2017;28:32-38. [23] DEBETTE S, LEYS D. Cervical-artery dissections: predisposing factors, diagnosis, and outcome. Lancet Neurol. 2009;8(7):668-678. [24] DEBETTE S, COMPTER A, LABEYRIE MA, et al. Epidemiology, pathophysiology, diagnosis, and management of intracranial artery dissection. Lancet Neurol. 2015;14(6):640-654. [25] NIELSEN SM, TARP S, CHRISTENSEN R, et al. The risk associated with spinal manipulation: an overview of reviews. Syst Rev. 2017;6(1):64. [26] HUTTING N, KERRY R, COPPIETERS MW, et al. Considerations to improve the safety of cervical spine manual therapy. Musculoskelet Sci Pract. 2018;33:41-45. [27] 李学靖,杨丹,尹依依,等. 《2021 NICE医患共同决策指南》要点解读[J]. 中华现代护理杂志,2022,28(4):421-425. [28] MOULTON B, COLLINS PA, BURNS-COX N, et al. From informed consent to informed request: do we need a new gold standard. J R Soc Med. 2013;106(10):391-394. [29] 陈奕历,劳永华,张少群,等. 颈动脉粥样硬化的流体力学模型:旋转手法下颈动脉粥样硬化斑块的血流动力学变化[J]. 中国组织工程研究,2019,23(15): 2403-2408. [30] 吴宝烽,冯梓誉,雷舒扬,等. 基于流固耦合有限元模型评估颈椎旋转手法下颈动脉粥样硬化斑块的破裂风险[J]. 医用生物力学,2022,37(4):684-691. [31] JOUGHIN A, IBITOYE S, CREES A, et al. Developing a virtual geriatric perioperative medicine clinic: a mixed methods healthcare improvement study. Age Ageing. 2021;50(4):1391-1396. [32] HÄRTER M, MOUMJID N, CORNUZ J, et al. Shared decision making in 2017: International accomplishments in policy, research and implementation. Z Evid Fortbild Qual Gesundhwes. 2017;123-124:1-5. [33] 赵羚谷,王涛,王颖,等. 国内外医患共同决策研究及应用进展之比较[J]. 医学与哲学(A),2018,39(10):6-9+57. [34] 霍路遥,符碧峰,冯天笑,等. 颈椎旋提手法教学机器人用于旋提手法规范化培训的自身对照研究[J]. 中国中医骨伤科杂志,2021,29(5):6-11. [35] 魏戌,王旭,孙凯,等. 中医手法治疗颈椎病的研究现状与展望[J]. 中华中医药杂志,2020,35(10):4781-4784. [36] 张帅攀,朱清广,孔令军,等. 脊柱微调手法治疗颈型颈椎病的临床疗效观察[J]. 中华中医药杂志,2021,36(5):3034-3037. |
| [1] | Wei Yuanbiao, Lin Zhan, Chen Yanmei, Yang Tenghui, Zhao Xiao, Chen Yangsheng, Zhou Yanhui, Yang Minchao, Huang Feiqi. Finite element analysis of effects of sagittal cervical manipulation on intervertebral disc and facet joints [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(6): 827-832. |
| [2] | Han Weiyu, Chen Yuanxing, Huang Youyang, Liu Weiwei, Zhao Yongchao, Zhao Ranzun. Regulation of cardiovascular diseases by histone deacetylation modification [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(35): 5707-5713. |
| [3] | Zhou Jinyan, Zhong Yuanming, Li Zhifei, Xu Wei, Zhang Jiali, Liang Ziyang. Pressure biofeedback training for treating cervical spondylosis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(31): 5052-5057. |
| [4] | Wang Nanfeng, Shen Shengmei, Zhang Peisheng, Teng Wei. Effects of hydrogels loaded with hepatocyte growth factor on myocardial infarction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(30): 4802-4808. |
| [5] | Peng Fengli, Li Chaofu, Shi Bei. Application of the nanovesicle delivery system in cardiovascular diseases [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(30): 4862-4868. |
| [6] | Jiang Honghui, Kong Yuanyuan, Liu Jing, Wang Zhihong. Preparation and applications of decellularized extracellular matrix bioink in cardiovascular fields [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(30): 4904-4911. |
| [7] | Wei Qin, Amanguli·Ruze, Chen Bingxin, Zhao Ling, Zhao Banghao, Jiang Tao, Zhang Chun, Li Zhiqiang, Gao Xiaoming, Duan Mingjun. Relaxin protects myocardial microvascular endothelial cells from hypoxia-reoxygenation injury [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(28): 4519-4524. |
| [8] | Li Rui, Ou Xiaolan, Liu Jun, Tian Heng, Qu Wenrui, Zhu Zhe, Zhang Zhenyu, Liu Qianqian, Guo Wenlai. Introduction to the ANTI∙DF principle for diabetic foot prevention and treatment [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(14): 2291-2296. |
| [9] | Gu Xia, Wang Pingyi, Zhao Wanhua, Lin Yushi, Li Yimei, Li Wenhua. Important role of exosomes-mediated hypoxia-related signaling pathways in the occurrence and progression of diseases [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(19): 3065-3070. |
| [10] | Gu Xia, Zhao Min, Wang Pingyi, Li Yimei, Li Wenhua. Relationship between hypoxia inducible factor 1 alpha and hypoxia signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1284-1289. |
| [11] | Zhao Min, Feng Liuxiang, Chen Yao, Gu Xia, Wang Pingyi, Li Yimei, Li Wenhua. Exosomes as a disease marker under hypoxic conditions [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1104-1108. |
| [12] |
Zheng Haijun, Jin Hui, Cui Hongling, Zhu Yakun, Zeng Hui, Han Fengjie, Qiu Cuiting, Liu Jing.
Safety of drug-coated balloon versus drug-eluting stents in the treatment of type 2 diabetes mellitus complicated by coronary artery small vessel disease in older adult patients [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(28): 4573-4579. |
| [13] | Gao Zhencheng, Liu Xin. The role and application of mesenchymal stem cells-derived exosomes in the treatment of nervous system diseases [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(19): 3048-3054. |
| [14] | Shen Rui, Hu Chuan, Wang Cui, Rao Huili, Ding Tao, Sun Kang, Tian Shaoqi. Early acute complications after total knee arthroplasty in patients with rheumatoid arthritis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(18): 2836-2841. |
| [15] | Zeng Jianyin, Han Shen, Li Yaxiong, Liu Bin, Zhang Yayong, Jiang Lihong. Application of induced pluripotent stem cells in cardiovascular diseases: efficiency and safety [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(9): 1448-1454. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||