Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (29): 4620-4627.doi: 10.12307/2023.656
Previous Articles Next Articles
Comparative analysis of artificial intelligence and two-dimensional digital template preoperative planning-assisted total hip arthroplasty to predict prosthesis size
Zhang Hang1, He Qiang1, Liu Qing2, He Yunli1, Wang Tao1, Feng Zhe1, Zhang Qian1, He Sen1
- 1Department of Orthopedic Surgery, 2Department of Radiology, Tianjin Beichen Hospital, Tianjin 300400, China
-
Received:2022-07-21Accepted:2022-09-09Online:2023-10-18Published:2022-12-02 -
Contact:He Sen, Master, Associate chief physician, Department of Orthopedic Surgery, Tianjin Beichen Hospital, Tianjin 300400, China -
About author:Zhang Hang, Master, Attending physician, Department of Orthopedic Surgery, Tianjin Beichen Hospital, Tianjin 300400, China -
Supported by:Tianjin Beichen District Health System Technology Project, No. SHGY-2021012 (to ZH)
CLC Number:
Cite this article
Zhang Hang, He Qiang, Liu Qing, He Yunli, Wang Tao, Feng Zhe, Zhang Qian, He Sen. Comparative analysis of artificial intelligence and two-dimensional digital template preoperative planning-assisted total hip arthroplasty to predict prosthesis size[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(29): 4620-4627.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
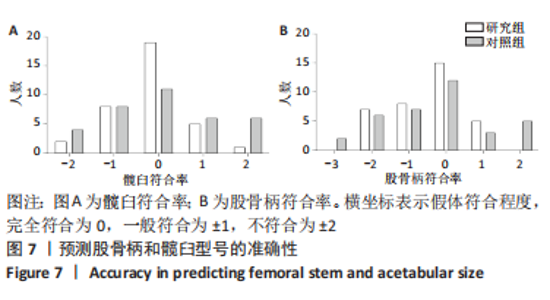
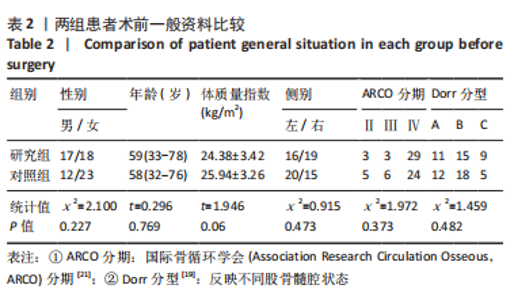
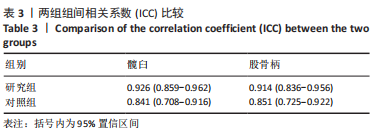
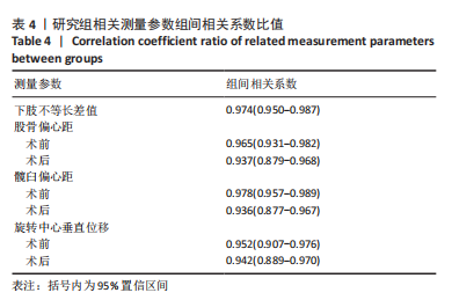
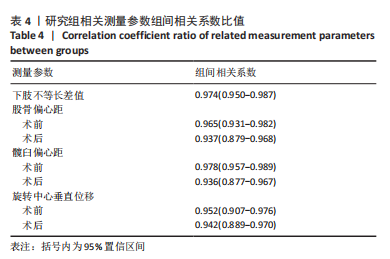
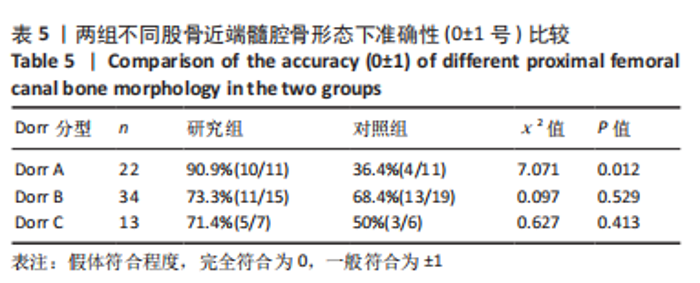
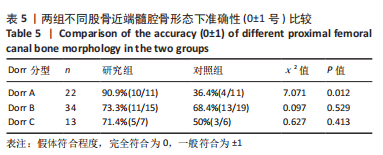
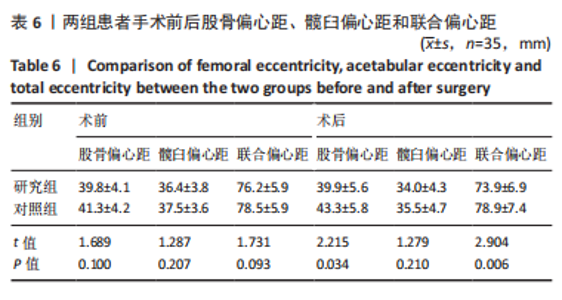
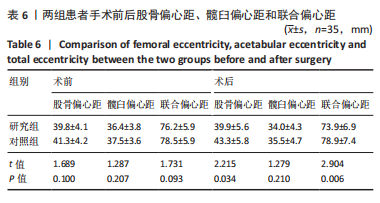
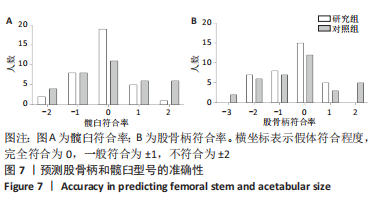
2.4 两组患者术后影像学随访结果 患者术后1 d及术后6个月随访时复查X射线片示假体位置良好,随访过程中未发现假体周围骨折、假体松动、脱位等情况。 2.5 两组患者手术时间和失血量 研究组平均手术时间为(74.66±14.97) min,对照组平均手术时间为(79.29±17.37) min,差异无显著性意义 (t=1.19,P=0.243)。研究组平均失血量为(294.29±50.76) mL,对照组平均失血量为(318.86±74.39) mL,差异无显著性意义(t=1.62,P=0.115)。 2.6 两组患者Harris评分 术后6个月末次随访,研究组Harris评分高于对照组(92.4±2.1,91.2±2.4),差异有显著性意义(t=3.15,P=0.003),两组优良率均为100%。 2.7 预测股骨柄和髋臼型号的准确性 研究组髋臼侧、股骨侧假体型号完全符合率为57.1%(20/35),42.9%(15/35),对照组为31.4%(11/35),34.3%(12/35);研究组髋臼侧、股骨侧假体符合率为94.3%(33/35),82.9%(29/35),对照组为74.3%(26/35),62.9%(22/35);两组间完全符合率和符合率差异均有显著性意义(P < 0.05),见图7。两组组间相关系数比较,研究组髋臼和股骨均高于0.9,表明AI HIP在不同观察者之间基本一致,见表3;研究组所有X射线片测量的组内相关系数均高于0.9,表明观察者之间基本一致,见表4。 "
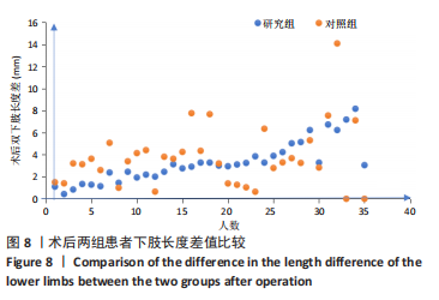
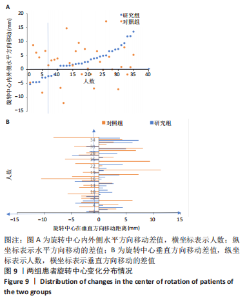
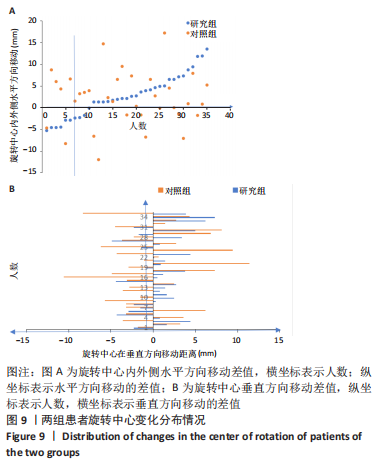
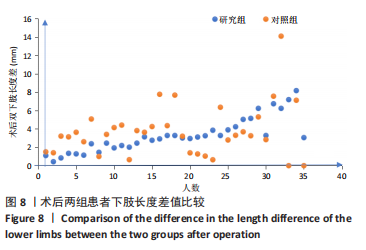
按照联合偏心距差异5 mm标准分类,两组在5 mm以内及在5-10 mm占比差异均无显著性意义(χ2=1.507,0.280,均P > 0.05);而研究组术前和术后联合偏心距差异> 10 mm者为5.71%(2/35),对照组为25.8%(7/35),两组差异无显著性意义(χ2=3.188,P=0.075)。研究组联合偏心距的差值多集中在5 mm以内,而对照组联合偏心距的差值比较分散。 2.10 两组术后双下肢长度及旋转中心比较 两组术后双下肢长度差值比较,其中研究组3.05(2.01,3.89) mm与对照组3.63(2.60,5.30) mm差异无显著性意义(Z=-1.736,P=0.083)。研究组双下肢长度差值在5 mm以内更集中,而对照组则更为分散,见图8。"
| [1] INOUE D, KABATA T, MAEDA T, et al. Value of computed tomography-based three-dimensional surgical preoperative planning software in total hip arthroplasty with developmental dysplasia of the hip. J Orthop Sci. 2015;20(2):340-346. [2] MAINARD D, BARBIER O, KNAFO Y, et al. Accuracy and reproducibility of preoperative three-dimensional planning for total hip arthroplasty using biplanar low-dose radiographs : A pilot study. Orthop Traumatol Surg Res. 2017;103(4):531-536. [3] MALONEY WJ, KEENEY JA. Leg length discrepancy after total hip arthroplasty. J Arthroplasty. 2004;19(4 Suppl 1):108-110. [4] SEAGRAVE KG, TROELSEN A, MALCHAU H, et al. Acetabular cup position and risk of dislocation in primary total hip arthroplasty. Acta Orthop. 2017;88(1):10-17. [5] LINDBERG-LARSEN M, JØRGENSEN CC, SOLGAARD S, et al. Increased risk of intraoperative and early postoperative periprosthetic femoral fracture with uncemented stems. Acta Orthop. 2017;88(4):390-394. [6] PETRETTA R, STRELZOW J, OHLY NE, et al. Acetate templating on digital images is more accurate than computer-based templating for total hip arthroplasty. Clin Orthop Relat Res. 2015;473(12):3752-3759. [7] HOLZER LA, SCHOLLER G, WAGNER S, et al. The accuracy of digital templating in uncemented total hip arthroplasty. Arch Orthop Trauma Surg. 2019;139(2):263-268. [8] DAMMERER D, KEILER A, HERRNEGGER S, et al. Accuracy of digital templating of uncemented total hip arthroplasty at a certified arthroplasty center: a retrospective comparative study. Arch Orthop Trauma Surg. 2021 Mar 16. doi: 10.1007/s00402-021-03836-w. Online ahead of print. [9] SARIALI E, MAUPRIVEZ R, KHIAMI F, et al. Accuracy of the preoperative planning for cementless total hip arthroplasty. A randomised comparison between three-dimensional computerised planning and conventional templating. Orthop Traumatol Surg Res. 2012;98(2):151-158. [10] WAKO Y, NAKAMURA J, MIURA M, et al. Interobserver and Intraobserver Reliability of Three-Dimensional Preoperative Planning Software in Total Hip Arthroplasty. J Arthroplasty. 2018;33(2):601-607. [11] KNAFO Y, HOUFANI F, ZAHARIA B, et al. Value of 3D Preoperative Planning for Primary Total Hip Arthroplasty Based on Biplanar Weightbearing Radiographs. Biomed Res Int. 2019;2019:1932191. [12] BANERJEE S, CHERIAN JJ, ELMALLAH RK, et al. Robot-assisted total hip arthroplasty. Expert Rev Med Devices. 2016;13(1):47-56. [13] BORJALI A, CHEN AF, BEDAIR HS, et al. Comparing the performance of a deep convolutional neural network with orthopedic surgeons on the identification of total hip prosthesis design from plain radiographs. Med Phys. 2021;48(5):2327-2336. [14] HAEBERLE HS, HELM JM, NAVARRO SM, et al. Artificial Intelligence and Machine Learning in Lower Extremity Arthroplasty: A Review. J Arthroplasty. 2019;34(10):2201-2203. [15] 吴东,柴伟,刘星宇,等.人工智能全髋关节置换术髋臼杯放置算法的实验研究[J].中华骨科杂志,2021,41(3):176-185. [16] DING X, ZHANG B, LI W, et al. Value of preoperative three-dimensional planning software (AI-HIP) in primary total hip arthroplasty: a retrospective study. J Int Med Res. 2021;49(11):3000605211058874. [17] HUO J, HUANG G, HAN D, et al. Value of 3D preoperative planning for primary total hip arthroplasty based on artificial intelligence technology. J Orthop Surg Res. 2021;16(1):156. [18] ALNAHHAL A, ASLAM-PERVEZ N, SHEIKH HQ. Templating Hip Arthroplasty. Open Access Maced J Med Sci. 2019;7(4):672-685. [19] DORR LD, FAUGERE MC, MACKEL AM, et al. Structural and cellular assessment of bone quality of proximal femur. Bone. 1993;14(3): 231-242. [20] HARRIS WH. Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end‐result study using a new method of result evaluation. J Bone Joint Surg Am. 1969;51(4):737-755. [21] 孙伟,李子荣.2019国际骨循环研究协会股骨头坏死分期[J].中华骨科杂志,2020,40(13):889-892. [22] SARIALI E, BOUKHELIFA N, CATONNE Y, et al. Comparison of Three-Dimensional Planning-Assisted and Conventional Acetabular Cup Positioning in Total Hip Arthroplasty: A Randomized Controlled Trial. J Bone Joint Surg Am. 2016;98(2):108-116. [23] ISSA K, PIVEC R, BOYD B, et al. Comparing the accuracy of radiographic preoperative digital templating for a second- versus a first-generation THA stem. Orthopedics. 2012;35(12):1028-1034. [24] OGAWA T, TAKAO M, SAKAI T, et al. Factors related to disagreement in implant size between preoperative CT-based planning and the actual implants used intraoperatively for total hip arthroplasty. Int J Comput Assist Radiol Surg. 2018;13(4):551-562. [25] LITTLE NJ, BUSCH CA, GALLAGHER JA, et al. Acetabular polyethylene wear and acetabular inclination and femoral offset. Clin Orthop Relat Res. 2009;467(11):2895-2900. [26] CECH A, KASE M, KOBAYASHI H, et al. Pre-operative planning in THA. Part III: do implant size prediction and offset restoration influence functional outcomes after THA? Arch Orthop Trauma Surg. 2020; 140(4):563-573. [27] MAHMOOD SS, MUKKA SS, CRNALIC S, et al. Association between changes in global femoral offset after total hip arthroplasty and function, quality of life, and abductor muscle strength. A prospective cohort study of 222 patients. Acta Orthop. 2016;87(1):36-41. [28] XU J, PIERREPONT J, MADURAWE C, et al. The effect of varus stem placement on joint offset during total hip arthroplasty: a virtual study. Hip Int. 2022;32(5):620-626. [29] HELLER MO, SCHRÖDER JH, MATZIOLIS G, et al. Musculoskeletal load analysis. A biomechanical explanation for clinical results--and more. Orthopade. 2007;36(3):188,190-194. [30] SCHEERLINCK T, DE WINTER E, SAS A, et al. Hip implants can restore anatomical and medialized rotation centres in most cases : a 3D templating study comparing four implantation strategies. Bone Jt Open. 2021;2(7):476-485. [31] SHEN J, SUN J, MA H, et al. High Hip Center Technique in Total Hip Arthroplasty for Crowe Type II-III Developmental Dysplasia: Results of Midterm Follow-up. Orthop Surg. 2020;12(4):1245-1252. [32] MEERMANS G, DOORN JV, KATS JJ. Restoration of the centre of rotation in primary total hip arthroplasty: the influence of acetabular floor depth and reaming technique. Bone Joint J. 2016;98-B(12):1597-1603. [33] DASTANE M, DORR LD, TARWALA R, et al. Hip offset in total hip arthroplasty: quantitative measurement with navigation. Clin Orthop Relat Res. 2011;469(2):429-436. [34] NOSSA JM, MUÑOZ JM, RIVEROS EA, et al. Leg length discrepancy after total hip arthroplasty: comparison of 3 intraoperative measurement methods. Hip Int. 2018;28(3):254-258. |
| [1] | Ke Yuqi, Chen Changjian, Wu Hao, Zheng Lianjie. Comparison of 12-month follow-up results of primary total hip arthroplasty between modified direct anterior approach and direct anterior approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1377-1382. |
| [2] | Cai Zhihao, Xie Zhaoyong. Femoral neck anteversion measurement assessment: how to establish a unified method and standard [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1448-1454. |
| [3] | You Aijia, Li Wenjie, Zhou Junli, Li Chun. Systematic evaluation of six dressings on wound safety following total hip and knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(3): 486-492. |
| [4] | Li Junran, Zhai Jingxiu, Zhao Hongbo, Wang Lei, Wang Hongrun, Liang Junsheng, Li Ligeng. Assistance of traction table for total hip arthroplasty through the direct anterior approach for treating femoral neck fracture in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(27): 4312-4317. |
| [5] | Ren Yi, Lu Ming, Qin Kunpeng, Zhang Hui, Gao Weilu, Li Yetian, Wang Jun, Yin Li, Yin Zongsheng. OrthoPilot navigation system assisted total hip arthroplasty improves the accuracy and safety of acetabular cup placement [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(27): 4318-4323. |
| [6] | Zhou Hongxing, Zhang Baojian, Yuan Xiangsheng. Recent evaluation of individual biological acetabular cup application in hip revision [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(22): 3521-3525. |
| [7] | Wang Zhangzheng, Mo Liang, Zhou Chi, Liu Yuhao, Yan Hongsong, He Wei. Influence of hip-preservation surgeries on subsequent total hip arthroplasty for osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(22): 3594-3601. |
| [8] | Zhuang Zhikun, Wu Rongkai, Lin Hanghui, Gong Zhibing, Zhang Qianjin, Wei Qiushi, Zhang Qingwen, Wu Zhaoke. Application of stable and enhanced lined hip joint system in total hip arthroplasty in elderly patients with femoral neck fractures complicated with hemiplegia [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1429-1433. |
| [9] | Huang Shibo, Xie Hui, Wang Zongpu, Wang Weidan, Qin Kairong, Zhao Dewei. Application of degradable high-purity magnesium screw in the treatment of developmental dysplasia of the hip [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 493-498. |
| [10] | He Guowen, Hu Baijun, Gao Dawei, Chen Liang. Treatment of Schatzker type V and VI tibial plateau fractures with 3D printing preoperative planning combined with double reverse traction device [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(36): 5764-5769. |
| [11] | Yuan Bo, Li Kainan, Jia Zishan. Comparison of the effects of different modes of balance disorder rehabilitation robots after total hip arthroplasty in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(36): 5826-5830. |
| [12] | Ma Ning, Wang Cong, Liu Ningqiang, Xie Tong, Yang Chaojian, Guo Chongjun, Niu Dongsheng, Liang Yuqi. Stability of 3D-printed titanium trabecular metal socket cups during total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(33): 5278-5282. |
| [13] | Li Kai, Liu Zhendong, Li Xiaolei, Wang Jingcheng. Risk factors for recurrent prosthesis dislocation after total hip arthroplasty through posterolateral approach [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 354-358. |
| [14] | Wang Chong, Zhang Meiying, Zhou Jian, Lao Kecheng. Early gait changes after total hip arthroplasty through direct anterior approach and posterolateral approach [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 359-364. |
| [15] | Chen Yong, Sun Yang. Effect of zoledronic acid on femoral implant subsidence after hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(12): 1812-1815. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||