Chinese Journal of Tissue Engineering Research ›› 2022, Vol. 26 ›› Issue (29): 4666-4671.doi: 10.12307/2022.882
Previous Articles Next Articles
Aerobic and resistance exercises can alleviate liver inflammation in type 2 diabetic rats
Fu Yu1, Shang Huayu1, Li Shunchang2
- 1School of Sport Medicine and Health, 2Sports Medicine and Health Institute, Chengdu Sport University, Chengdu 610041, Sichuan Province, China
-
Received:2021-11-25Accepted:2021-12-23Online:2022-10-18Published:2022-03-28 -
Contact:Li Shunchang, MD, Professor, Sports Medicine and Health Institute, Chengdu Sport University, Chengdu 610041, Sichuan Province, China -
About author:Fu Yu, Master, Lecturer, School of Sport Medicine and Health, Chengdu Sport University, Chengdu 610041, Sichuan Province, China -
Supported by:the 2019 Innovation Project of Sports Medicine and Health Institute of Chengdu Sport University / Zheng Huaixian Orthopedic Research Institute, No. CX19D06 (to FY)
CLC Number:
Cite this article
Fu Yu, Shang Huayu, Li Shunchang. Aerobic and resistance exercises can alleviate liver inflammation in type 2 diabetic rats[J]. Chinese Journal of Tissue Engineering Research, 2022, 26(29): 4666-4671.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
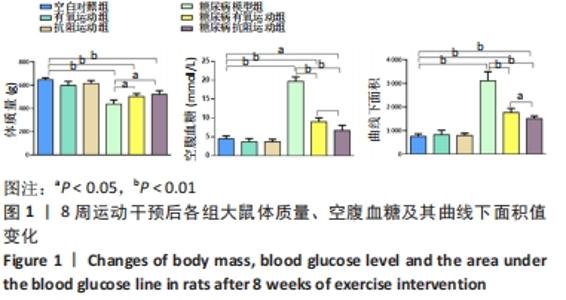
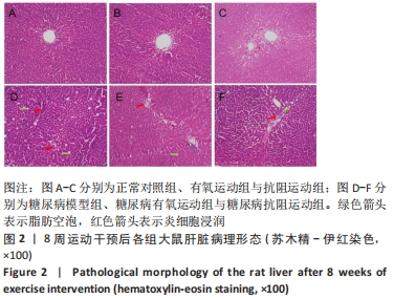
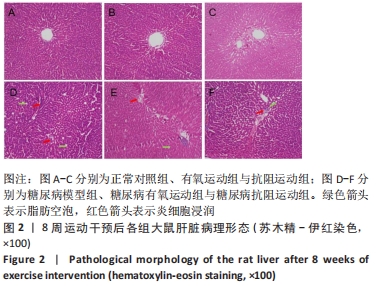
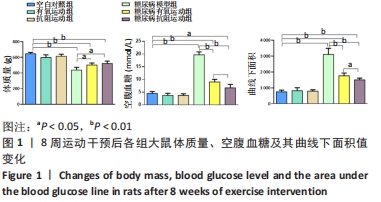
2.1 实验动物数量分析 实验纳入60只SD大鼠,由于糖尿病造模及后期干预,最终纳入48只SD大鼠,共计6组。 2.2 各组大鼠体质量、血糖情况 与空白对照组相比,糖尿病组大鼠体质量均显著下降(P < 0.01);与糖尿病模型组相比,糖尿病有氧运动与抗阻运动组大鼠体质量显著增加(P < 0.05),但两组间无显著性意义(P > 0.05);与空白对照组相比,糖尿病模型组与糖尿病有氧运动组大鼠血糖水平及其曲线下面积值显著升高(P < 0.01),糖尿病抗阻运动组血糖水平显著升高(P < 0.05);与糖尿病模型组相比,糖尿病有氧运动与抗阻运动组血糖水平均显著下降(P < 0.01),糖尿病抗阻运动组低于糖尿病有氧运动组(P < 0.05);糖尿病有氧运动与抗阻运动组大鼠血糖曲线下面积值均显著减小(P < 0.01);糖尿病抗阻运动组相比于糖尿病有氧运动组下降更明显(P < 0.05),见图1。"
| [1] GOEDEKE L, PERRY RJ, SHULMAN GI. Emerging Pharmacological Targets for the Treatment of Nonalcoholic Fatty Liver Disease, Insulin Resistance, and Type 2 Diabetes. Ann Rev Pharmacol. 2019;59(1):65-87. [2] KLISIC A, ISAKOVIC A, KOCIC G, et al. Relationship between Oxidative Stress, Inflammation and Dyslipidemia with Fatty Liver Index in Patients with Type 2 Diabetes Mellitus. Exp Clin Endocrinol Diabetes. 2018;126(6):371-378. [3] FRANCESCONI C, NIEBAUER J, HABER P, et al. Lebensstil: körperliche Aktivität und Training in der Prävention und Therapie des Typ 2 Diabetes mellitus (Update 2019) [Lifestyle: physical activity and training as prevetion and therapy of type 2 diabetes mellitus (Update 2019)]. Wien Klin Wochenschr. 2019;131(Suppl 1):61-66. [4] ELIAS D, PRIGOZIN H, POLAK N, et al. Autoimmune diabetes induced by the beta-cell toxin STZ. Immunity to the 60-kDa heat shock protein and to insulin. Diabetes. 1994;43(8):992-998. [5] BEDFORD TG, TIPTON CM, WILSON NC, et al. Maximum oxygen consumption of rats and its changes with various experimental procedures. J Appl Physiol Respir Environ Exerc Physiol. 1979;47(6): 1278-1283. [6] HORNBERGER TA JR, FARRAR RP. Physiological hypertrophy of the FHL muscle following 8 weeks of progressive resistance exercise in the rat. Can J Appl Physiol. 2004;29(1):16-31. [7] AL-AWAR A, KUPAI K, VESZELKA M, et al. Experimental Diabetes Mellitus in Different Animal Models. J Diabetes Res. 2016;2016:9051426. [8] GHEIBI S, KASHFI K, GHASEMI A. A practical guide for induction of type-2 diabetes in rat: Incorporating a high-fat diet and streptozotocin. Biomed Pharmacother. 2017;95:605-613. [9] MEHTA BK, SINGH KK, BANERJEE S. Effect of exercise on type 2 diabetes-associated cognitive impairment in rats. Int J Neurosci. 2019; 129(3):252-263. [10] 尚画雨,夏志,张丹,等.8周游泳运动对2型糖尿病大鼠周围神经病变的影响[J].中国病理生理杂志,2014,30(4):719-724. [11] CHO NH, SHAW JE, KARURANGA S, et al. IDF Diabetes Atlas: Global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res Clin Pract. 2018;138:271-281. [12] GHASEMI A, JEDDI S. Anti-obesity and anti-diabetic effects of nitrate and nitrite. Nitric Oxide. 2017;70:9-24. [13] CZECH MP. Insulin action and resistance in obesity and type 2 diabetes. Nat Med. 2017;23(7):804-814. [14] BARAZZONI R, GORTAN CAPPELLARI G, et al. Insulin resistance in obesity: an overview of fundamental alterations. Eat Weight Disord. 2018;23(2):149-157. [15] KIRWAN JP, SACKS J, NIEUWOUDT S. The essential role of exercise in the management of type 2 diabetes. Cleve Clin J Med. 2017;84(7 Suppl 1): S15-S21. [16] YANG D, YANG Y, LI Y, et al. Physical Exercise as Therapy for Type 2 Diabetes Mellitus: From Mechanism to Orientation. Ann Nutr Metab. 2019;74(4):313-321. [17] AMANAT S, GHAHRI S, DIANATINASAB A, et al. Exercise and Type 2 Diabetes. Adv Exp Med Biol. 2020;1228:91-105. [18] DONGHUI T, SHUANG B, XULONG L, et al. Improvement of microvascular endothelial dysfunction induced by exercise and diet is associated with microRNA-126 in obese adolescents. Microvasc Res. 2019;123:86-91. [19] RÖHLING M, HERDER C, RODEN M, et al. Effects of Long-Term Exercise Interventions on Glycaemic Control in Type 1 and Type 2 Diabetes: a Systematic Review. Exp Clin Endocrinol Diabetes. 2016;124(8):487-494. [20] CHIANG SL, HEITKEMPER MM, HUNG YJ, et al. Effects of a 12-week moderate-intensity exercise training on blood glucose response in patients with type 2 diabetes: A prospective longitudinal study. Medicine (Baltimore). 2019;98(36):e16860. [21] LI S, LIANG M, PAN Y, et al. Exercise modulates heat shock protein 27 activity in diabetic cardiomyopathy. Life Sci. 2020;243:117251. [22] MANNUCCI E, BONIFAZI A, MONAMI M. Comparison between different types of exercise training in patients with type 2 diabetes mellitus: A systematic review and network metanalysis of randomized controlled trials. Nutr Metab Cardiovasc Dis. 2021;31(7):1985-1992. [23] REDDY R, WITTENBERG A, CASTLE JR, et al. Effect of Aerobic and Resistance Exercise on Glycemic Control in Adults With Type 1 Diabetes. Can J Diabetes. 2019;43(6):406-414.e1. [24] LI S, LIANG M, GAO D, et al. Changes in Titin and Collagen Modulate Effects of Aerobic and Resistance Exercise on Diabetic Cardiac Function. J Cardiovasc Transl Res. 2019;12(5):404-414. [25] NERY C, MORAES SRA, NOVAES KA, et al. Effectiveness of resistance exercise compared to aerobic exercise without insulin therapy in patients with type 2 diabetes mellitus: a meta-analysis.Braz J Phys Ther. 2017;21(6):400-415. [26] KARSTOFT K, PEDERSEN BK. Exercise and type 2 diabetes: focus on metabolism and inflammation. Immunol Cell Biol. 2016;94(2):146-150. [27] JAFARIPOUR S, SEDIGHI S, JOKAR MH, et al. Inflammation, diet, and type 2 diabetes: a mini-review. J Immunoassay Immunochem. 2020; 41(4):768-777. [28] PEDERSEN BK. Anti-inflammatory effects of exercise: role in diabetes and cardiovascular disease. Eur J Clin Invest. 2017;47(8):600-611. [29] MEIJNIKMAN AS, GERDES VE, NIEUWDORP M, et al. Evaluating Causality of Gut Microbiota in Obesity and Diabetes in Humans. Endocr Rev. 2018;39(2):133-153. [30] ZHOU W, CHEN C, CHEN Z, et al. NLRP3: A Novel Mediator in Cardiovascular Disease. J Immunol Res. 2018;2018:5702103. [31] AN N, GAO Y, SI Z, et al. Regulatory Mechanisms of the NLRP3 Inflammasome, a Novel Immune-Inflammatory Marker in Cardiovascular Diseases. Front Immunol. 2019;10:1592. [32] HONG P, GU RN, LI FX, et al. NLRP3 inflammasome as a potential treatment in ischemic stroke concomitant with diabetes. J Neuroinflammation. 2019;16(1):121. [33] KAYAGAKI N, STOWE IB, LEE BL, et al. Caspase-11 cleaves gasdermin D for non-canonical inflammasome signalling. Nature. 2015;526(7575): 666-671. [34] LI W, CHANG Y, LIANG S, et al. NLRP3 inflammasome activation contributes to Listeria monocytogenes-induced animal pregnancy failure. BMC Vet Res. 2016;12:36. [35] SHARMA D, KANNEGANTI TD. The cell biology of inflammasomes: Mechanisms of inflammasome activation and regulation. Cell Biol. 2016;213(6):617-629. [36] MALIK A, KANNEGANTI TD. Inflammasome activation and assembly at a glance. J Cell Sci. 2017;130(23):3955-3963. [37] DING S, XU S, MA Y, et al. Modulatory Mechanisms of the NLRP3 Inflammasomes in Diabetes. Biomolecules. 2019;9(12):850. [38] ZHANG W, XU X, KAO R, et al. Cardiac fibroblasts contribute to myocardial dysfunction in mice with sepsis: the role of NLRP3 inflammasome activation. PLoS One. 2014;9(9):e107639. [39] XIE Y, HUANG Y, LING X, et al. Chemerin/CMKLR1 Axis Promotes Inflammation and Pyroptosis by Activating NLRP3 Inflammasome in Diabetic Cardiomyopathy Rat. Front Physiol. 2020;11:381. [40] LUO B, HUANG F, LIU Y, et al. NLRP3 Inflammasome as a Molecular Marker in Diabetic Cardiomyopathy. Front Physiol. 2017;8:519. [41] LI X, LI Z, LI B, et al. Klotho improves diabetic cardiomyopathy by suppressing the NLRP3 inflammasome pathway. Life Sci. 2019;234: 116773. [42] VANDANMAGSAR B, YOUM YH, RAVUSSIN A, et al. The NLRP3 inflammasome instigates obesity-induced inflammation and insulin resistance. Nat Med. 2011;17(2):179-188. [43] WANG Q, HU J, LIU Y, et al. Aerobic Exercise Improves Synaptic-Related Proteins of Diabetic Rats by Inhibiting FOXO1/NF-κB/NLRP3 Inflammatory Signaling Pathway and Ameliorating PI3K/Akt Insulin Signaling Pathway. J Mol Neurosci. 2019;69(1):28-38. [44] LI J, LIU Y, LIU B, et al. Mechanisms of Aerobic Exercise Upregulating the Expression of Hippocampal Synaptic Plasticity-Associated Proteins in Diabetic Rats. Neural Plast. 2019;2019:7920540. [45] MARDARE C, KRÜGER K, LIEBISCH G, et al. Endurance and Resistance Training Affect High Fat Diet-Induced Increase of Ceramides, Inflammasome Expression, and Systemic Inflammation in Mice. J Diabetes Res. 2016;2016:4536470. [46] YANG W, LIU L, WEI Y, et al. Exercise suppresses NLRP3 inflammasome activation in mice with diet-induced NASH: a plausible role of adropin. Lab Invest. 2021;101(3):369-380. [47] HONG J, PARK E, LEE J, et al. Exercise training mitigates ER stress and UCP2 deficiency-associated coronary vascular dysfunction in atherosclerosis. Sci Rep. 2021;11(1):15449. [48] ZHUGE DL, JAVAID HMA, SAHAR NE, et al. Fibroblast growth factor 2 exacerbates inflammation in adipocytes through NLRP3 inflammasome activation. Arch Pharm Res. 2020;43(12):1311-1324. [49] KHAKROO ABKENAR I, RAHMANI-NIA F, LOMBARDI G. The effects of acute and chronic aerobic activity on the signaling pathway of the inflammasome NLRP3 complex in young men. Medicina. 2019;55(4): 105. |
| [1] | LIU Danni, SUN Guanghua, ZHOU Guijuan, LIU Hongya, ZHOU Jun, TAN Jinqu, HUANG Xiarong, PENG Ting, FENG Wei-bin, LUO Fu. Effect of electroacupuncture on apoptosis of neurons in cerebral cortex of rats with cerebral ischemia-reperfusion injury at "Shuigou" and "Baihui" points [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(在线): 1-6. |
| [2] | Chen Xianghe, Liu Bo, Yang Kang, Lu Pengcheng, Yu Huilin. Treadmill exercise improves the myocardial fibrosis of spontaneous type 2 diabetic mice: an exploration on the functional pathway [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1210-1215. |
| [3] | Xiang Xinjian, Liu Fang, Wu Liangliang, Jia Daping, Tao Yue, Zhao Zhengnan, Zhao Yu. High-dose vitamin C promotes the survival of autologous fat transplantation in rats [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(8): 1242-1246. |
| [4] | He Junjun, Huang Zeling, Hong Zhenqiang. Interventional effect of Yanghe Decoction on synovial inflammation in a rabbit model of early knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 694-699. |
| [5] | Shui Xiaoping, Li Chunying, Li Shunchang, Sun Junzhi, Su Quansheng . Effects of aerobic and resistance exercises on brain-derived neurotrophic factor, nuclear factor-kappa B and inflammatory cytokines in skeletal muscle of type II diabetic rats [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 669-675. |
| [6] | Liu Yiyi, Qiu Junqiang, Yi Longyan, Zhou Cailiang. Effect of resistance training on interleukin-6 and C-reactive protein in middle-age and elderly people: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(5): 804-812. |
| [7] | Yang Wei, Han Qingmin. Exploring peripheral blood biomarkers and therapeutic drugs for osteoarthritis based on bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(29): 4672-4679. |
| [8] | Yang Yi, Wang Kun, Liu Hengxu, Zhang Tingran, Lu Wenyun, Chen Peijie, Luo Jiong. Aerobic exercise improves the cognitive function of elderly patients with mild cognitive impairment [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(29): 4716-4722. |
| [9] | Wu Haineng, Geng Kang, Wang Jing, Xiong Aibing. Platelet-rich fibrin combined with curcumin nanoparticle hydrogel promotes wound healing in diabetic mice [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(27): 4300-4307. |
| [10] | Yang Jinxin, Wang Kun, Zhao Jing, Chen Peijie, Zhang Tingran, Lu Wenyun, Luo Jiong. Effects of aerobic exercise intervention on synaptic plasticity in Alzheimer’s disease patients [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4216-4223. |
| [11] | Liu Ya, Liu Xia, Deng Penghui, Ji Wei, Li Jianping. Exercise effects on myocardial type I, III collagen and angiotensin II/transforming growth factor beta1/Smad2 pathway in diabetic myocardial fibrosis rats [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4173-4179. |
| [12] | Xiang Mingzhi, Yuan Zilin, Wang Gang, Cheng Jie, Diao Bo, Liu Yueping. CD1d-mediated inhibition of the nucleotide-binding oligomerization domain-like receptor protein 3 inflammatory factor expression via signal regulatory protein-alpha [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(24): 3826-3832. |
| [13] | Wu Siyi, Wu Qiong. Effect of adipose-derived stem cell transplantation on the immune microenvironment of adipose tissue in aged mice [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(24): 3773-3778. |
| [14] | Jiang Jie, Zhao Baixiao, Chen Libin, Wen Li, Zhang Shanshan, Ma Jie, Zhao Hua. Effect of moxibustion pretreatment on autophagy and NLRP3 inflammasome expression in cerebral ischemia-reperfusion model rats [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(23): 3615-3619. |
| [15] | Su Jianqing, Sun Bo, Ding Yunrong, Liu Guangming, Ji Wei, Jiang Enyu, Yang Jiayu. Preparing a rabbit model of synovitis in knee osteoarthritis based on the “injury-repair-reinjury” method [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(23): 3738-3743. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||