Chinese Journal of Tissue Engineering Research ›› 2025, Vol. 29 ›› Issue (8): 1643-1649.doi: 10.12307/2025.342
Previous Articles Next Articles
Differences in postural control ability between older adults with mild cognitive impairment and those with normal cognition under different single-task and dual-task conditions
Zhang Yuxin1, Yu Cong1, Zhang Cui2, Ding Jianjun1, Chen Yan3
- 1Shandong Sport University, Jinan 250102, Shandong Province, China; 2Shandong Sports Science Research Center, Jinan 250102, Shandong Province, China; 3College of Sports and Health, Shandong Sport University, Jinan 250102, Shandong Province, China
-
Received:2024-03-25Accepted:2024-04-30Online:2025-03-18Published:2024-07-05 -
Contact:Chen Yan, PhD, Professor, College of Sports and Health, Shandong Sport University, Jinan 250102, Shandong Province, China -
About author:Zhang Yuxin, Master candidate, Shandong Sport University, Jinan 250102, Shandong Province, China -
Supported by:National Natural Science Foundation of China, No. 12102235 (to ZC); Science and Technology Innovation Project of General Administration of Sport of China, No. 23KJCX058 (to CY)
CLC Number:
Cite this article
Zhang Yuxin, Yu Cong, Zhang Cui, Ding Jianjun, Chen Yan. Differences in postural control ability between older adults with mild cognitive impairment and those with normal cognition under different single-task and dual-task conditions[J]. Chinese Journal of Tissue Engineering Research, 2025, 29(8): 1643-1649.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
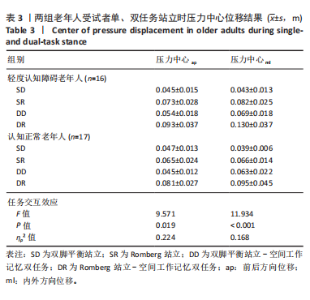
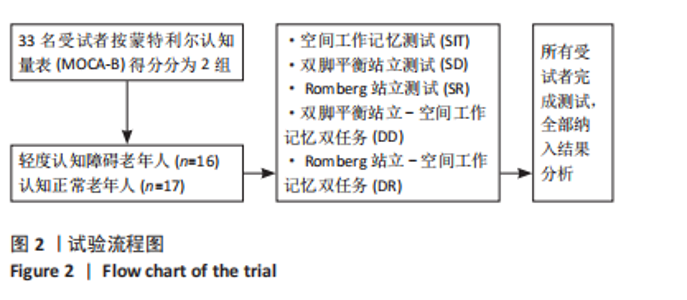
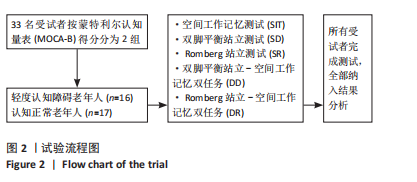
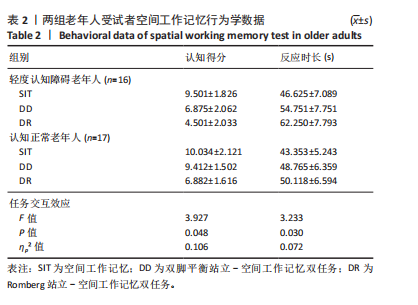
①轻度认知障碍老年人在执行SIT任务时认知得分最大,DD任务居中,DR任务最小,任务间比较差异均有显著性意义(SIT vs. DD,P < 0.001;SIT vs. DR,P < 0.001;DD vs. DR,P=0.002);轻度认知障碍老年人在执行SIT任务时反应时长最短,DD任务居中,DR任务最长,任务间比较差异均有显著性意义(SIT vs. DD,P=0.003;SIT vs. DR,P < 0.001;DD vs. DR,P=0.008)。②认知正常老年人在执行DR任务时认知得分最小,显著小于SIT任务(P < 0.001)和DD任务(P=0.006),SIT任务与DD任务比较差异无显著性意义(P=0.528);认知正常老年人在执行SIT任务时反应时长最短,显著短于DD任务(P=0.019)和DR任务(P=0.015),但DD任务与DR任务比较差异无显著性意义(P=0.788)。③在SIT任务下,两组老年人的认知得分、反应时长比较均差异无显著性意义(认知得分P=0.445,反应时长P=0.439);在DD任务下,轻度认知障碍老年人的认知得分显著小于认知正常老年人(P < 0.001),反应时长显著大于认知正常老年人(P=0.014);在DR任务下,轻度认知障碍老年人的认知得分显著小于认知正常老年人(P < 0.001),反应时长显著大于认知正常老年人(P < 0.001)。 2.5 不同站立任务下足底压力中心位移结果 压力中心位移在组别与任务间具有交互效应(P < 0.05),事后两两比较见表3。"
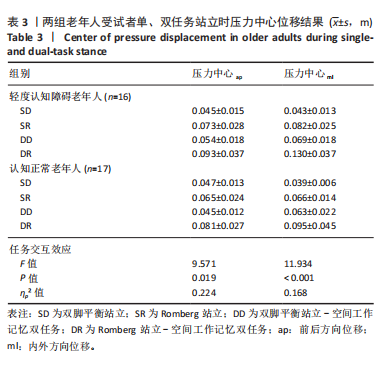
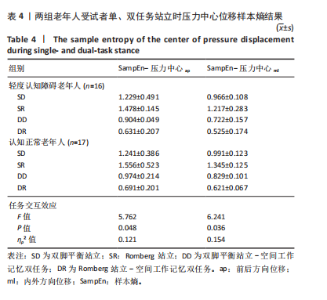
轻度认知障碍老年人在执行DR任务时前后、内外方向压力中心位移最大(DR vs. SD,前后P < 0.001,内外P < 0.001;DR vs. SR,前后P=0.017,内外P < 0.001;DR vs. DD,前后P < 0.001,内外P < 0.001),执行SD时最小(SD vs. SR,前后P < 0.001,内外P < 0.001;SD vs. DD,前后P=0.031,内外P < 0.001)。 在SR、DD、DR任务下,轻度认知障碍老年人前后、内外方向压力中心位移显著大于认知正常老年人(SR前后P=0.034,内外P < 0.001;DD前后P=0.043,内外P=0.001;DR前后P=0.015,内外P=0.026)。 2.6 不同站立任务下足底压力中心位移样本熵结果 压力中心位移样本熵在组别与任务间具有交互效应(P < 0.05),事后两两比较见表4。"
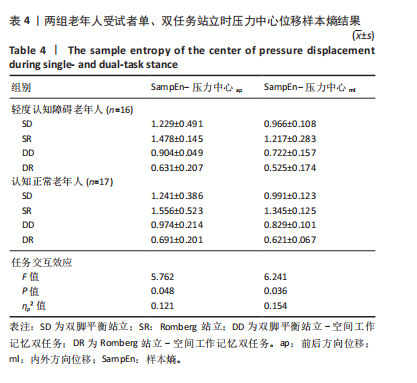

轻度认知障碍老年人在执行DR任务时前后、内外方向的压力中心位移样本熵最小(DR vs. SD,前后P < 0.001,内外P < 0.001;DR vs. SR,前后P < 0.001,内外P < 0.001;DR vs. DD,前后P < 0.001,内外P < 0.001),执行SR任务时最大(SR vs. SD,前后P < 0.001,内外P < 0.001;SR vs. DD,前后P < 0.001,内外P < 0.001)。 在SR、DD、DR任务下,轻度认知障碍老年人前后、内外方向压力中心位移样本熵显著小于认知正常老年人(SR前后P < 0.001,内外P < 0.001;DD前后P=0.001,内外P=0.001;DR前后P=0.003,内外P=0.002)。 2.7 不良事件 两组受试者在完成5种测试任务的过程中,全程受到安全保护,未发生发生跌倒、身体不适、身体或肢体受伤等情况。"

| [1] KNOPMAN DS, PETERSEN RC. Mild cognitive impairment and mild dementia: a clinical perspective. Mayo Clin Proc. 2014;89(10): 1452-1459. [2] 史路平, 姚水洪, 王薇. 中国老年人群轻度认知障碍患病率及发展趋势的Meta分析[J]. 中国全科医学,2022,25(1):109-114. [3] 袁梓健, 郭立燕, 张妍,等. 中国老年人轻度认知障碍现状及其影响因素 [J]. 济宁医学院学报,2022,45(3):183-188. [4] HOSOKI S, SACHDEV PS. Molecular biomarkers for vascular cognitive impairment and dementia: the current status and directions for the future. Neural Regen Res. 2024;19(12):2579-2580. [5] MUIR-HUNTER SW, WITTWER JE. Dual-task testing to predict falls in community-dwelling older adults: a systematic review. Physiotherapy. 2016;102(1):29-40. [6] TROPP H, ODENRICK P. Postural control in single-limb stance. J Orthop Res. 1988;6(6):833-839. [7] STURNIEKS DL, ST GEORGE R, LORD SR. Balance disorders in the elderly. Neurophysiol Clin. 2008;38(6):467-478. [8] SALIHU AT, HILL KD, JABERZADEH S. Effect of cognitive task complexity on dual task postural stability: a systematic review and meta-analysis. Exp Brain Res. 2022;240(3):703-731. [9] WENG WH, YANG YR, YEH NC, et al. Gait performance and prefrontal cortex activation during single and dual task walking in older adults with different cognitive levels. Front Aging Neurosci.2023;15:1177082. [10] WINTER DA, PATLA A E, ISHAC M, et al. Motor mechanisms of balance during quiet standing. J Electromyogr Kinesiol. 2003;13(1):49-56. [11] HOWE TE, ROCHESTER L, NEIL F, et al. Exercise for improving balance in older people. Cochrane Database Syst Rev. 2011;9(11):CD004963. [12] BALDINI A, NOTA A, ASSI V, et al. Intersession reliability of a posturo-stabilometric test, using a force platform. J Electromyogr Kinesiol. 2013; 23(6):1474-1479. [13] RUHE A, FEJER R, WALKER B. The test-retest reliability of centre of pressure measures in bipedal static task conditions--a systematic review of the literature. Gait Posture. 2010;32(4):436-445. [14] QUATMAN-YATES C, BONNETTE S, GUPTA R, et al. Spatial and temporal analysis center of pressure displacement during adolescence: Clinical implications of developmental changes. Hum Mov Sci. 2018;58:148-154. [15] 刘鑫玥, 霍洪峰.认知负荷对人体静态平衡及动态稳定性的影响[J].医用生物力学,2021,36(S1):360. [16] SONG Q, ZHANG X, MAO M, et al. Relationship of proprioception, cutaneous sensitivity, and muscle strength with the balance control among older adults.J Sport Health Sci. 2021;10(5):585-593. [17] 齐刘心, 周勉, 王祥宇,等. 支撑面稳定度在不同视觉输入条件下对轻度认知障碍老年人平衡能力的影响[J].中国组织工程研究, 2024,28(24):3897-902. [18] LIAO FY, WU CC, WEI Y C, et al. Analysis of Center of Pressure Signals by Using Decision Tree and Empirical Mode Decomposition to Predict Falls among Older Adults. J Healthc Eng. 2021;2021:6252445. [19] QUIJOUX F, VIENNE-JUMEAU A, BERTIN-HUGAULT F, et al. Center of pressure displacement characteristics differentiate fall risk in older people: A systematic review with meta-analysis. Ageing Res Rev. 2020; 62:101117. [20] RAMDANI S, TALLON G, BERNARD PL, et al. Recurrence Quantification Analysis of Human Postural Fluctuations in Older Fallers and Non-fallers.Ann Biomed Eng. 2013;41(8):1713-1725. [21] STANIA M, EMICH-WIDERA E, KAZEK B, et al. Modulation of center-of-pressure signal in children on the autism spectrum: A case-control study. Gait Posture. 2023;103:67-72. [22] KEDZIOREK J, BLAZKIEWICZ M. Nonlinear Measures to Evaluate Upright Postural Stability: A Systematic Review. Entropy (Basel). 2020; 22(12):1357. [23] FISCHER OM, MISSEN KJ, TOKUNO CD, et al. Postural threat increases sample entropy of postural control. Front Neurol. 2023;14:1179237. [24] HANSEN C, WEI Q, SHIEH J S, et al. Sample Entropy, Univariate, and Multivariate Multi-Scale Entropy in Comparison with Classical Postural Sway Parameters in Young Healthy Adults. Front Hum Neurosci. 2017; 11:206. [25] GEORGOULIS AD, MORAITI C, RISTANIS S, et al. A novel approach to measure variability in the anterior cruciate ligament deficient knee during walking: the use of the approximate entropy in orthopaedics. J Clin Monit Comput. 2006;20(1):11-18. [26] BROOKS LR. The suppression of visualization by reading. Q J Exp Psychol. 1967;19(4):289-299. [27] SHAO Z, LI L, MAO M, et al. Exploring the effects of peripheral sensibility on visuospatial and postural capacities during goal-directed movements in long-term Tai Chi practitioners. Front Aging Neurosci. 2022;14:881972. [28] PAJALA S, ERA P, KOSKENVUO M, et al. Force platform balance measures as predictors of indoor and outdoor falls in community-dwelling women aged 63-76 years. J Gerontol A Biol Sci Med Sci. 2008; 63(2):171-178. [29] PAPALIA GF, MANGANO G, DIAZ BALZANI LA, et al. Strabismus and postural control: a systematic review. Musculoskelet Surg. 2022;106(4): 345-356. [30] CHOU LW, CHANG KM, WEI YC, et al. Empirical Mode Decomposition-Derived Entropy Features Are Beneficial to Distinguish Elderly People with a Falling History on a Force Plate Signal. Entropy (Basel). 2021;23(4):472. [31] ROERDINK M, HLAVACKOVA P, VUILLERME N. Center-of-pressure regularity as a marker for attentional investment in postural control: a comparison between sitting and standing postures. Hum Mov Sci. 2011;30(2):203-212. [32] MANOR B, COSTA MD, HU K, et al. Physiological complexity and system adaptability: evidence from postural control dynamics of older adults. J Appl Physiol (1985). 2010;109(6):1786-1791. [33] BOHLE H, RIMPEL J, SCHAUENBURG G, et al. Behavioral and Neural Correlates of Cognitive-Motor Interference during Multitasking in Young and Old Adults. Neural Plast. 2019;2019:9478656. [34] MITRA S, VERNON M, BOULTON H. The role of spatial alignment in posture-cognition dual task interaction. Gait Posture. 2022;93:54-58. [35] 范勇, 吕汇. 认知负荷条件下老年人站姿稳定性及其控制策略策略研究[J]. 体育科技文献通报,2019,27(1):6-9. [36] FUHRMAN SI, REDFERN MS, JENNINGS JR, et al. Interference between postural control and spatial vs. non-spatial auditory reaction time tasks in older adults. J Vestib Res. 2015;25(2):47-55. [37] CHENG KC, PRATT J, MAKI BE. Effects of spatial-memory decay and dual-task interference on perturbation-evoked reach-to-grasp reactions in the absence of online visual feedback. Hum Mov Sci. 2013;32(2):328-342. [38] RIZZATO A, BENAZZATO M, COGNOLATO M, et al. Different neuromuscular control mechanisms regulate static and dynamic balance: A center-of-pressure analysis in young adults. Hum Mov Sci. 2023;90:103120. [39] BOISGONTIER M P, BEETS I A, DUYSENS J, et al. Age-related differences in attentional cost associated with postural dual tasks: increased recruitment of generic cognitive resources in older adults. Neurosci Biobehav Rev. 2013;37(8):1824-1837. [40] MONTERO-ODASSO M, MUIR SW, SPEECHLEY M. Dual-task complexity affects gait in people with mild cognitive impairment: the interplay between gait variability, dual tasking, and risk of falls. Arch Phys Med Rehabil. 2012;93(2):293-299. [41] BAHUREKSA L, NAJAFI B, SALEH A, et al. The Impact of Mild Cognitive Impairment on Gait and Balance: A Systematic Review and Meta-Analysis of Studies Using Instrumented Assessment. Gerontology. 2017; 63(1):67-83. [42] MANOR B, LIPSITZ LA. Physiologic complexity and aging: implications for physical function and rehabilitation. Prog Neuropsychopharmacol Biol Psychiatry. 2013;45:287-293. [43] DONKER SF, ROERDINK M, GREVEN AJ, et al. Regularity of center-of-pressure trajectories depends on the amount of attention invested in postural control. Exp Brain Res. 2007;181(1):1-11. [44] COSTA M, PRIPLATA AA, LIPSITZ LA, et al. Noise and poise: Enhancement of postural complexity in the elderly with a stochastic-resonance-based therapy. Europhys Lett. 2007;77:68008. [45] LIPSITZ LA. Dynamics of stability: the physiologic basis of functional health and frailty. J Gerontol A Biol Sci Med Sci. 2002;57(3):B115-125. [46] PENA M, PETRILLO K, BOSSET M, et al. Brain function complexity during dual-tasking is associated with cognitive impairment and age. J Neuroimaging. 2022;32(6):1211-1223. |
| [1] | Zhang Zihua. Simulation and force characterization of the lower limbs in elderly people from sitting to standing [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1407-1416. |
| [2] | Li Huijun, Li Huangyan, Zhang Yeting. Physical activity and cognition in older adults: research hotspot and topic evolution [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(5): 1073-1080. |
| [3] | Wang Jinfu, Yang Guan. Meta-analysis of wearable device interventions to promote physical activity in older adults [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(28): 6146-6160. |
| [4] | Wang Xia, Xue Boshi, Yang Chen, Zhou Zhipeng, Zheng Liangliang. Influence of neuromuscular function on the risk of biomechanical injury in landing manoeuvres in patients undergoing anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(26): 5556-5562. |
| [5] | Hong Jintao, Wang Jingjing, Li Yansong, Wang Chen, Mi Shouling. Sedentary behavior and lower-limb muscle strength in community-dwelling older adults: the mediating and moderating effects of fear of falling and age [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(17): 3566-3571. |
| [6] | Dong Zhiwen, Yu Cong, Chen Yan, Ding Jianjun . Central nervous mechanisms underlying effects of cognitive impairment on dual-task stance: #br# functional near-infrared spectroscopy analysis [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(17): 3579-3587. |
| [7] | Zhao Yanan, Lu Donglei, Tan Sijie, . Exercise intervention for sarcopenic obesity in older adults [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(17): 3657-3667. |
| [8] | Zhang Jiaqi, Liu Yanhong, Liang Huiting, Zhou Jingjing, Wang Yawen, Xu Jingyu, Li Yushuang, Lei Lijian, Hu Xiaoqin. Bioinformatics analysis and functional verification of hsa-miR-3202 in osteoarthritic chondrocytes [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(12): 2458-2465. |
| [9] | Zhang Wenli, Zhao Ziqi, Liang Leichao, Tang Yunqi, Wang Yong. Differences in dynamic stability across different height barriers between obese and average men [J]. Chinese Journal of Tissue Engineering Research, 2025, 29(11): 2319-2326. |
| [10] | Lu Donglei, Feng Zhanpeng, Cao Liquan, Tang Yi, Tan Sijie, Yu Zhongtao. Exercise intervention methods for senile sarcopenia [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(35): 5723-5731. |
| [11] | Dong Hongming, Li Jianping, Liu Chao, Zhang Honghao, Li Guqiang. Relationship between muscle activation characterization and fall risk in older adults during walking up and down stairs [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(34): 5419-5424. |
| [12] | Xue Boshi, Lin Changrui, Zheng Liangliang, Yang Chen, Zhou Zhipeng. Core stability training reduces risk of anterior cruciate ligament injury in landing movements [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(16): 2467-2472. |
| [13] | Liu Xinxin, Geng Zhizhong, Chen Jian. Effects of high-intensity interval training with different intervention durations on cognitive function in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2024, 28(14): 2282-2289. |
| [14] | Pan Weimin, Wang Bing, Han Yabing, Li Ting, Song Jiaqi, Qin Huasheng, Liu Yang. Effects of blood flow restriction training on muscle strength, muscle mass and physical performance in older adults: a Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 805-812. |
| [15] | Peng Tuanhui, Yang Ling, Ding Xiaoge, Meng Pengjun. A systematic review and meta-analysis of the effects of long-term exercise on blood lipids in healthy elderly people [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(14): 2276-2282. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||