Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (36): 5784-5789.doi: 10.12307/2023.738
Previous Articles Next Articles
Balance and gait characteristics of static standing and walking after anterior cruciate ligament reconstruction
Ma Shengnan1, Ke Jingyue1, Dong Hongming1, Shen Shuang2, Ding Hao3, Li Jianping1, Li Guqiang2
- 1School of Rehabilitation, 2Rehabilitation Engineering Research Institute, 3Second Clinical Medical College, Binzhou Medical University, Yantai 264003, Shandong Province, China
-
Received:2022-10-14Accepted:2022-11-25Online:2023-12-28Published:2023-03-24 -
Contact:Li Guqiang, Master, Associate professor, Rehabilitation Engineering Research Institute, Binzhou Medical University, Yantai 264003, Shandong Province, China -
About author:Ma Shengnan, Master candidate, School of Rehabilitation, Binzhou Medical University, Yantai 264003, Shandong Province, China -
Supported by:Shandong Natural Science Foundation (General Program), No. ZR2022MA047 (to SS); 2021 Undergraduate Teaching Reform Research Project of Shandong Province, No. M2021213 (to LGQ)
CLC Number:
Cite this article
Ma Shengnan, Ke Jingyue, Dong Hongming, Shen Shuang, Ding Hao, Li Jianping, Li Guqiang. Balance and gait characteristics of static standing and walking after anterior cruciate ligament reconstruction[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(36): 5784-5789.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
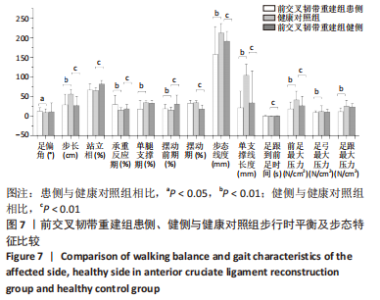
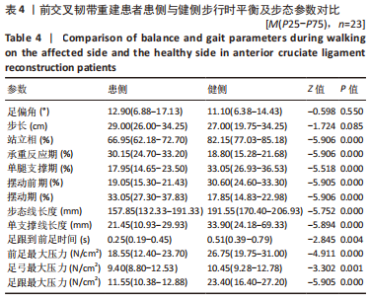
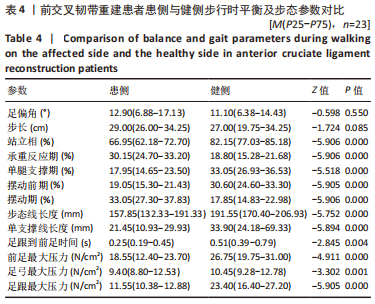
2.7 ACLR组患侧、健侧与健康对照组在步行时的平衡及步态特征分析 步行时,ACLR组患侧与健康对照组相比,步态线长度和单支撑线长度明显减小,差异有显著性意义(P < 0.05);患侧足偏角、承重反应期及摆动前期明显增加,步长、单腿支撑期显著减小,差异均有显著性意义(P < 0.05);同时患侧前足最大压力、足弓最大压力及足跟最大压力均明显降低,差异有显著性意义(P < 0.05);患侧站立相、摆动期及足跟到前足时间无显著变化(P > 0.05)。 步行时,ACLR组健侧与健康对照组相比,健侧的步态线长度和单支撑线长度均小于健康人,差异有显著性意义(P < 0.05);健侧站立相、承重反应期、摆动前期及足跟到前足时间均延长,步长及摆动期缩短,差异有显著性意义(P < 0.05);ACLR患者健侧前足最大压力低于健康人(P < 0.05),但足弓和足跟最大压力无明显差异(P > 0.05);健侧的足偏角和单腿支撑期与健康对照组相比差异无显著性意义(P > 0.05)。见图7。"

| [1] 吴铭杰, 李亮, 张晓强, 等. 关节镜下双袢钛板悬吊重建膝关节前交叉韧带的稳定性[J]. 中国组织工程研究,2023,27(18):2878-2883. [2] 高奉, 李方祥, 李国平. 前交叉韧带的机械感受器与本体感觉[J]. 中国运动医学杂志,2012,31(6):541-547. [3] 陈家, 魏世隽, 王洪. 关节镜下韧带重建术治疗前交叉韧带损伤的研究进展[J]. 中国矫形外科杂志,2018,26(16):1489-1494. [4] FREEMAN MA, WYKE B. Articular contributions to limb muscle reflexes. The effects of partial neurectomy of the knee-joint on postural reflexes. Br J Surg. 1966; 53(1): 61-68. [5] KENNEDY JC, ALEXANDER IJ, HAYES KC. Nerve supply of the human knee and its functional importance. Am J Sports Med. 1982;10(6):329-335. [6] 张磊, 李义凯. 膝关节前交叉韧带本体感觉的研究进展[J]. 中国康复医学杂志,2017,32(2):245-247. [7] 王宇彤, 白伦浩, 温昱, 等. 前交叉韧带断裂后不同状态韧带残端内机械感受器的变化[J]. 中国综合临床,2018,34(1):34-37+97. [8] MUSAHL V, KARLSSON J. Anterior Cruciate Ligament Tear. N Engl J Med. 2019; 380(24):2341-2348. [9] MONTALVO AM, SCHNEIDER DK, WEBSTER KE, et al. Anterior Cruciate Ligament Injury Risk in Sport: A Systematic Review and Meta-Analysis of Injury Incidence by Sex and Sport Classification. J Athl Train. 2019;54(5):472-482. [10] MONTALVO AM, SCHNEIDER DK, YUT L, et al. “What’s my risk of sustaining an ACL injury while playing sports?” A systematic review with meta-analysis. Br J Sports Med. 2019;53(16):1003-1012. [11] 周志鹏, 曲峰, 刘鹏, 等. 不同方向单腿跳跃落地及运动疲劳对非接触性前交叉韧带损伤风险的影响[J]. 中国体育科技,2017,53(1):111-117. [12] GAO B, ZHENG NN. Alterations in three-dimensional joint kinematics of anterior cruciate ligament-deficient and -reconstructed knees during walking. Clin Biomech (Bristol, Avon). 2010;25(3):222-229. [13] RICHMOND JC. Anterior Cruciate Ligament Reconstruction. Sports Med Arthrosc Rev. 2018;26(4):165-167. [14] HERZOG MM, MARSHALL SW, LUND JL, et al. Trends in Incidence of ACL Reconstruction and Concomitant Procedures Among Commercially Insured Individuals in the United States, 2002-2014. Sports Health. 2018;10(6):523-531. [15] ROSSI R, COTTINO U, BRUZZONE M, et al. Total knee arthroplasty in the varus knee: tips and tricks. Int Orthop. 2019;43(1):151-158. [16] LEE HM, CHENG CK, LIAU JJ. Correlation between proprioception, muscle strength, knee laxity, and dynamic standing balance in patients with chronic anterior cruciate ligament deficiency. Knee.2009;16(5):387-391. [17] MELNYK M, FAIST M, GOTHNER M, et al. Changes in stretch reflex excitability are related to “giving way” symptoms in patients with anterior cruciate ligament rupture. J Neurophysiol. 2007;97(1):474-480. [18] 李玉周, 王婧怡, 胡英琪. 前交叉韧带重建术后短期足底压力分布及平衡特征研究[J]. 体育科学,2020,40(5):52-59. [19] 马钊, 周谋望, 谷莉, 等. 前交叉韧带重建术后患者平衡功能的研究[J]. 中国康复医学杂志,2010,25(7):625-627+631. [20] GOKALP O, AKKAYA S, AKKAYA N, et al. Preoperative and postoperative serial assessments of postural balance and fall risk in patients with arthroscopic anterior cruciate ligament reconstruction. J Back Musculoskelet Rehabil. 2016;29(2):343-350. [21] WILLIAMS GN, SNYDER-MACKLER L, BARRANCE PJ, et al. Quadriceps femoris muscle morphology and function after ACL injury: a differential response in copers versus non-copers. J Biomech. 2005;38(4):685-693. [22] PALMIERI-SMITH RM, MCLEAN SG, ASHTON-MILLER JA, et al. Association of quadriceps and hamstrings cocontraction patterns with knee joint loading. J Athl Train. 2009;44(3):256-263. [23] GRANACHER U, GOLLHOFER A, HORTOBÁGYI T, et al. The importance of trunk muscle strength for balance, functional performance, and fall prevention in seniors: a systematic review. Sports Med. 2013;43(7):627-641. [24] FERNANDES TL, FELIX EC, BESSA F, et al. Evaluation of static and dynamic balance in athletes with anterior cruciate ligament injury - A controlled study. Clinics (Sao Paulo). 2016;71(8):425-429. [25] KAPRELI E, ATHANASOPOULOS S, GLIATIS J, et al. Anterior cruciate ligament deficiency causes brain plasticity: a functional MRI study. Am J Sports Med. 2009; 37(12):2419-2426. [26] THOMAS AC, WOJTYS EM, BRANDON C, et al. Muscle atrophy contributes to quadriceps weakness after anterior cruciate ligament reconstruction. J Sci Med Sport. 2016;19(1):7-11. [27] TOURVILLE TW, VOIGT TB, CHOQUETTE RH, et al. Skeletal muscle cellular contractile dysfunction after anterior cruciate ligament reconstruction contributes to quadriceps weakness at 6-month follow-up. J Orthop Res. 2022;40(3):727-737. [28] ALFAYYADH A, NEAL K, WILLIAMS JR, et al. Limb and sex-related differences in knee muscle co-contraction exist 3 months after anterior cruciate ligament reconstruction. J Electromyogr Kinesiol. 2022;66:102693. [29] HOWELLS BE, CLARK RA, ARDERN CL, et al. The assessment of postural control and the influence of a secondary task in people with anterior cruciate ligament reconstructed knees using a Nintendo Wii Balance Board. Br J Sports Med. 2013; 47(14):914-919. [30] YU PA, FAN CH, KUO LT, et al. Differences in gait and muscle strength of patients with acute and chronic anterior cruciate ligament injury. Clin Biomech (Bristol, Avon). 2020;80:105161. [31] POZZI F, DI STASI S, ZENI JA JR, et al. Single-limb drop landing biomechanics in active individuals with and without a history of anterior cruciate ligament reconstruction: A total support analysis. Clin Biomech (Bristol, Avon). 2017;43: 28-33. [32] THOMA LM, GRINDEM H, LOGERSTEDT D, et al. Coper Classification Early After Anterior Cruciate Ligament Rupture Changes With Progressive Neuromuscular and Strength Training and Is Associated With 2-Year Success: The Delaware-Oslo ACL Cohort Study. Am J Sports Med. 2019;47(4):807-814. [33] SHIMIZU T, SAMAAN MA, TANAKA MS, et al. Abnormal Biomechanics at 6 Months Are Associated With Cartilage Degeneration at 3 Years After Anterior Cruciate Ligament Reconstruction. Arthroscopy. 2019;35(2):511-520. [34] WEBSTER KE, HEWETT TE. Anterior Cruciate Ligament Injury and Knee Osteoarthritis: An Umbrella Systematic Review and Meta-analysis. Clin J Sport Med. 2022;32(2):145-152. [35] CHEN T, WANG S, LI Y, et al. Radiographic Osteoarthritis Prevalence Over Ten Years After Anterior Cruciate Ligament Reconstruction. Int J Sports Med. 2019; 40(11):683-695. [36] MANICKAM A, GARDINER MD. Gait assessment in general practice. Aust J Gen Pract. 2021;50(11):801-806. [37] 马启寿,廖燕锬,李中元,等. FES辅助跑步机训练提高脑卒中下肢偏瘫患者步行能力的研究[J]. 按摩与康复医学,2022,13(14):22-25,28. [38] 董元丽,高华,杨瑞贞, 等. 脑血管储备功能与老年人步态及平衡功能的相关性[J]. 中华老年心脑血管病杂志,2021,23(11):1125-1128. [39] 章雨威,张秋霞,袁金凤. 不同速度下功能性踝关节不稳者与常人步态参数的比较研究. 中国康复医学杂志,2015,30(11):1151-1154. [40] LYLE MA, JENSEN JC, HUNNICUTT JL, et al. Identification of strength and spatiotemporal gait parameters associated with knee loading during gait in persons after anterior cruciate ligament reconstruction. J Athl Train. 2021. doi: 10.4085/1062-6050-0186.21. |
| [1] | Zhong Jiamin, Huang Zhaoxin, Li Longxue, Qu Tongtong, Liu Zhuang, Fu Yifeng, Xiao Xiaofei. Effects of visual factors on balance function in young adults [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1245-1249. |
| [2] | Li Shihao, Li Qi, Li Zhen, Zhang Yuanyuan, Liu Miaomiao, Ouyang Yi, Xu Weiguo. Plantar pressure and gait analysis in patients with anterior cruciate ligament injury and reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 626-631. |
| [3] | Chen Peng, Wang Ling, Dong Shiyu, Ding Yue, Jia Shaohui, Kou Xianjuan, Zheng Cheng. Effects of whole-body vibration training on anterior cruciate ligament reconstruction: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(36): 5875-5883. |
| [4] | Luo Wei, Zhong Tao, Huang Zhirui, Gao Yan, Huang Zhen. Static balance and limits of stability in patients with chronic nonspecific low back pain [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(27): 4362-4366. |
| [5] | Xu Zhi, Li Yuwan, Jin Ying, Liu Yi. Effect of partial posterior root tear of medial meniscus on biomechanics of the knee joint during gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2824-2830. |
| [6] | Wu Mingjie, Li Liang, Zhang Xiaoqiang, Luo Zhiping, Wu Jiachang, Sang Hongxun. Stability of anterior cruciate ligament reconstructed by double-loop titanium plate suspension under arthroscopy [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(18): 2878-2883. |
| [7] | Zhang Jichao, Dong Yuefu, Mou Zhifang, Zhang Zhen, Li Bingyan, Xu Xiangjun, Li Jiayi, Ren Meng, Dong Wanpeng. Finite element analysis of biomechanical changes in the osteoarthritis knee joint in different gait flexion angles [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1357-1361. |
| [8] | Bai Zixing, Cao Xuhan, Sun Chengyi, Yang Yanjun, Chen Si, Wen Jianmin, Lin Xinxiao, Sun Weidong. Construction and biomechanical analysis of ankle joint finite element model in gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1362-1366. |
| [9] | Liu Feng, Feng Yi. Finite element analysis of different Kirschner wire tension bands on transverse patella fractures during gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1367-1371. |
| [10] | Wang Yaoting, Lu Yan, Yao Jiaqin, Yang Chunhua, Xu Wenjing, Wang Hongyu. Differential analysis of plantar pressure parameters of lower limbs in stroke patients with different cerebral hemispheric injuries [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(35): 5646-5651. |
| [11] | Li Zhishuai, Zhang Hongqian, Liu Jianquan, Zhang Hankun, Li Li. Visualization analysis of current research hotspots on rehabilitation treatment after anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(26): 4234-4241. |
| [12] | Xiong Binglang, Lin Tianye, Yang Peng, Xu Jingli, Zou Qizhao, Lai Qizhong, Zhang Qingwen. Visualization of global status and trends in anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(29): 4656-4663. |
| [13] | Wang Xinting, Xu Dandi, Zhang Junxia, Su Hailong Wang Qi. Stability of load-bearing cross barrier of different arch structures [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3838-3843. |
| [14] | Han Lei, Liu Haiying, Zhang Hao. Numerical analysis of the mechanical behaviors of cartilage in various levels of osteoarthritis in a gait cycle [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2810-2815. |
| [15] | Sun Kai, Chen Lei, Mai Yao, Hu Hua, Chen Liang, Zhong Jun, Hu Yong, Qiu Bo. Clinical application of enhanced recovery after surgery in the perioperative period of anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1647-1651. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||