Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (31): 4977-4983.doi: 10.12307/2023.689
Previous Articles Next Articles
Relationship between anatomical morphology of the tibial plateau and meniscal tears
Zhou Hang, Feng Shuo, Zhang Jincheng, Zhang Leshu, Chen Jiahao, Chen Xiangyang
- Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221006, Jiangsu Province, China
-
Received:2022-08-17Accepted:2022-10-14Online:2023-11-08Published:2023-01-31 -
Contact:Chen Xiangyang, MD, Chief physician, Associate professor, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221006, Jiangsu Province, China -
About author:Zhou Hang, Master candidate, Physician, Department of Orthopedics, Affiliated Hospital of Xuzhou Medical University, Xuzhou 221006, Jiangsu Province, China -
Supported by:Youth Medical Science and Technology Innovation Project of Xuzhou Health Commission, No. XWKYHT20210577 (to FS); Jiangsu Aging Health Research Project, No. LX2021010 (to CXY)
CLC Number:
Cite this article
Zhou Hang, Feng Shuo, Zhang Jincheng, Zhang Leshu, Chen Jiahao, Chen Xiangyang. Relationship between anatomical morphology of the tibial plateau and meniscal tears[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(31): 4977-4983.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
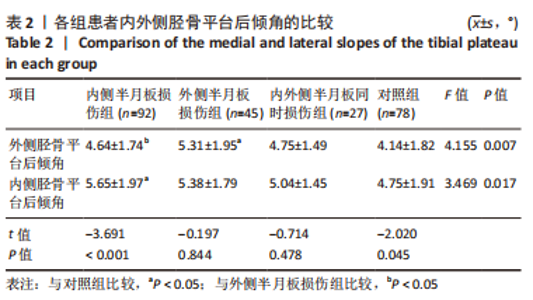
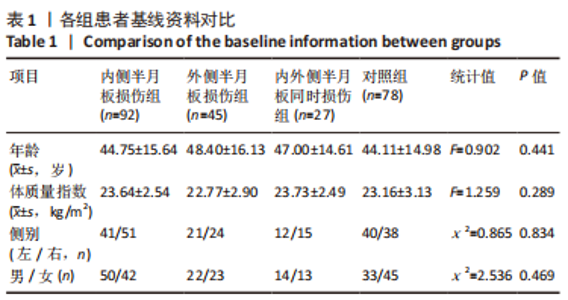
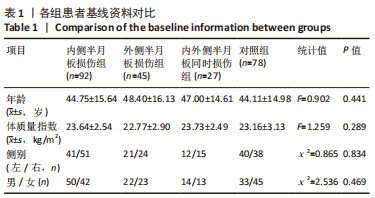
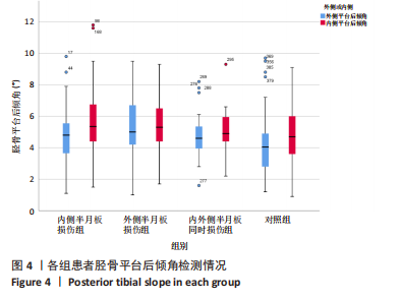
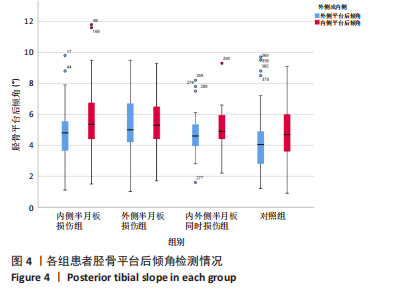
2.5 各组患者胫骨平台形态比较 2位医师测量结果的一致性检验为:外侧胫骨平台后倾角的组内相关系数为0.912,内侧胫骨平台后倾角的组内相关系数为0.865,内侧胫骨平台凹陷深度的组内相关系数为0.909,外侧胫骨平台凸出高度的组内相关系数为0.824,2位医师的测量结果一致性高,结果可靠。 胫骨平台后倾角组内比较:内侧半月板损伤组与对照组的外侧胫骨平台后倾角平均值显著小于内侧平台后倾角(P < 0.001,P=0.045),外侧半月板损伤组的胫骨平台后倾角与内侧胫骨平台后倾角比较差异无显著性意义(P > 0.05),内外侧半月板同时损伤组的胫骨平台后倾角外侧与内侧胫骨平台后倾角比较差异无显著性意义(P > 0.05),见表2,图4。"
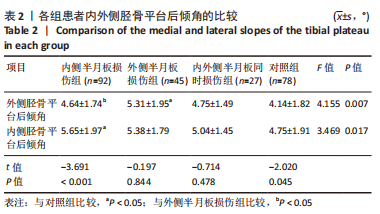
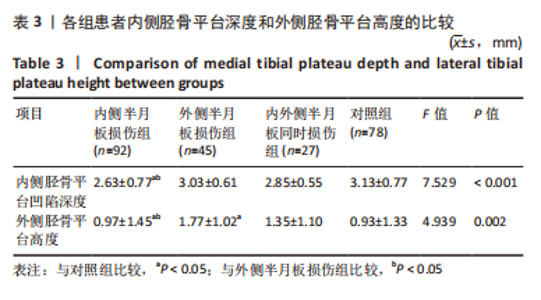
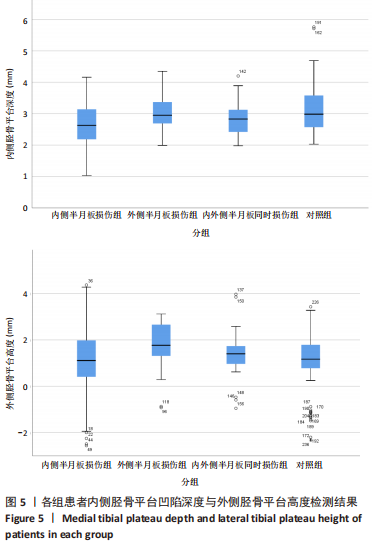
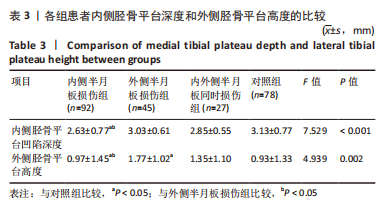
胫骨平台后倾角组间比较:外侧半月板损伤组的外侧平台后倾角明显大于内侧半月板损伤组、对照组(P=0.037,P < 0.001),内外侧半月板同时损伤组的外侧胫骨平台后倾角与其他组比较差异无显著性意义(P > 0.05),内侧半月板损伤组的内侧胫骨平台后倾角大于对照组(P=0.002),外侧半月板损伤组、内外侧半月板同时损伤组的内侧胫骨平台后倾角与其他组比较差异无显著性意义(P > 0.05),见表2,图4。 各组之间内侧胫骨平台凹陷深度对比,内侧半月板损伤组的内侧胫骨平台凹陷深度明显小于外侧半月板损伤组、对照组(P=0.002,P < 0.001)。各组之间外侧胫骨平台高度对比,外侧半月板损伤组的外侧胫骨平台高度明显大于内侧半月板损伤组、对照组(P=0.001,P=0.001)。内外侧半月板同时损伤组的内侧胫骨平台深度和外侧胫骨平台高度与其他各组比较差异均无显著性意义(P > 0.05),见表3,图5。"
| [1] KORTHAUS A, KRAUSE M, PAGENSTERT G, et al. Tibial slope in the posterolateral quadrant with and without ACL injury. Arch Orthop Trauma Surg. 2021. doi: 10.1007/s00402-021-04298-w. [2] LUCZKIEWICZ P, DASZKIEWICZ K, WITKOWSKI W, et al. Influence of meniscus shape in the cross sectional plane on the knee contact mechanics. J Biomech. 2015;48(8):1356-1363. [3] SONG GY, LIU X, ZHANG H, et al. Increased Medial Meniscal Slope Is Associated With Greater Risk of Ramp Lesion in Noncontact Anterior Cruciate Ligament Injury. Am J Sports Med. 2016;44(8):2039-2046. [4] 岳德波,鄂森,王佰亮,等.胫骨后倾与非接触性前交叉韧带断裂的关系及其对关节稳定性的影响[J].中华医学杂志,2013,93(17): 1309-1312. [5] KUMAR PANIGRAHI T, DAS A, MOHANTY T, et al. Study of relationship of posterior tibial slope in anterior cruciate ligament injury. J Orthop. 2020;21:487-490. [6] ALICI T, ESENYEL CZ, ESENYEL M, et al. Relationship between meniscal tears and tibial slope on the tibial plateau. Eurasian J Med. 2011;43(3): 146-151. [7] WU J, HUANG JM, ZHAO B, et al. Risk Factors Comparison for Radial and Horizontal Tears. J Knee Surg. 2016;29(8):679-683. [8] JIANG J, LIU Z, WANG X, et al. Increased Posterior Tibial Slope and Meniscal Slope Could Be Risk Factors for Meniscal Injuries: A Systematic Review. Arthroscopy. 2022;38(7):2331-2341. [9] BERNHOLT D, DEPHILLIPO NN, AMAN ZS, et al. Increased posterior tibial slope results in increased incidence of posterior lateral meniscal root tears in ACL reconstruction patients. Knee Surg Sports Traumatol Arthrosc. 2021;29(11):3883-3891. [10] HASHEMI J, CHANDRASHEKAR N, MANSOURI H, et al. Shallow medial tibial plateau and steep medial and lateral tibial slopes: new risk factors for anterior cruciate ligament injuries. Am J Sports Med. 2010;38(1): 54-62. [11] OKAZAKI Y, FURUMATSU T, KODAMA Y, et al. Steep posterior slope and shallow concave shape of the medial tibial plateau are risk factors for medial meniscus posterior root tears. Knee Surg Sports Traumatol Arthrosc. 2021;29(1):44-50. [12] KHAN N, MCMAHON PANDOBAID H. Bony morphology of the knee and non-traumatic meniscal tears: is there a role for meniscal impingement? Skeletal Radiol. 2014;43(7):955-962. [13] MOON HS, CHOI CH, JUNG M, et al. Medial Meniscal Posterior Horn Tears Are Associated With Increased Posterior Tibial Slope: A Case-Control Study. Am J Sports Med. 2020;48(7):1702-1710. [14] HUDEK R, SCHMUTZ S, REGENFELDER F, et al. Novel measurement technique of the tibial slope on conventional MRI. Clin Orthop Relat Res. 2009;467(8):2066-2072. [15] HASHEMI J, CHANDRASHEKAR N, GILL B, et al. The geometry of the tibial plateau and its influence on the biomechanics of the tibiofemoral joint. J Bone Joint Surg Am. 2008;90(12):2724-2734. [16] BERNHARDSON AS, AMAN ZS, DEPHILLIPO NN, et al. Tibial Slope and Its Effect on Graft Force in Posterior Cruciate Ligament Reconstructions. Am J Sports Med. 2019;47(5):1168-1174. [17] DE BOER JJ, BLANKEVOORT L, KINGMA I, et al. In vitro study of inter-individual variation in posterior slope in the knee joint. Clin Biomech (Bristol, Avon). 2009;24(6):488-492. [18] QI Y, SUN H, FAN Y, et al. Three dimensional finite element analysis of the influence of posterior tibial slope on the anterior cruciate ligament and knee joint forward stability. J Back Musculoskelet Rehabil. 2018;31(4):629-636. [19] JOJIMA H, WHITESIDE LAANDOGATA K. Effect of tibial slope or posterior cruciate ligament release on knee kinematics. Clin Orthop Relat Res. 2004;(426):194-198. [20] JENNY JY, BOÉRI C, BALLONZOLI L, et al. Difficultés et reproductibilité de la mesure radiographique de l’axe épiphysaire proximal du tibia selon la technique de Lévigne. Rev Chir Orthop Reparatrice Appar Mot. 2005;91(7):658-663. [21] Zhang Y, Chen Y, Qiang M,et al. Comparison between three-dimensional CT and conventional radiography in proximal tibia morphology. Medicine (Baltimore). 2018;97(30):e11632. [22] Waiwaiole A, Gurbani A, Motamedi K,et al. Relationship of ACL Injury and Posterior Tibial Slope With Patient Age, Sex, and Race. Orthop J Sports Med. 2016;4(11):2325967116672852. [23] HOHMANN E, TETSWORTH K, GLATT V, et al. Medial and Lateral Posterior Tibial Slope Are Independent Risk Factors for Noncontact ACL Injury in Both Men and Women. Orthop J Sports Med. 2021;9(8): 23259671211015940. [24] 孙英华.年龄相关的胫骨平台后倾角变化规律与交叉韧带损伤关系的临床研究[D].济南:山东大学, 2016. [25] WANG YL, YANG T, ZENG C, et al. Association Between Tibial Plateau Slopes and Anterior Cruciate Ligament Injury: A Meta-analysis. Arthroscopy. 2017;33(6):1248-1259.e4. [26] CHURCH S, KEATING JF. Reconstruction of the anterior cruciate ligament: timing of surgery and the incidence of meniscal tears and degenerative change. J Bone Joint Surg Br. 2005;87(12):1639-1642. [27] KOLBE R, SCHMIDT-HEBBEL A, FORKEL P, et al. Steep lateral tibial slope and lateral-to-medial slope asymmetry are risk factors for concomitant posterolateral meniscus root tears in anterior cruciate ligament injuries. Knee Surg Sports Traumatol Arthrosc. 2019;27(8):2585-2591. [28] THORLUND JB, JUHL CB, INGELSRUD LH, et al. Risk factors, diagnosis and non-surgical treatment for meniscal tears: evidence and recommendations: a statement paper commissioned by the Danish Society of Sports Physical Therapy (DSSF). Br J Sports Med. 2018;52(9): 557-565. [29] FEUCHT MJ, BIGDON S, BODE G, et al. Associated tears of the lateral meniscus in anterior cruciate ligament injuries: risk factors for different tear patterns. J Orthop Surg Res. 2015;10:34. [30] MARKL I, ZANTOP T, ZEMAN F, et al. The effect of tibial slope in acute ACL-insufficient patients on concurrent meniscal tears. Arch Orthop Trauma Surg. 2015;135(8):1141-1149. [31] BALCAREK P, TERWEY A, JUNG K, et al. Influence of tibial slope asymmetry on femoral rotation in patients with lateral patellar instability. Knee Surg Sports Traumatol Arthrosc. 2013;21(9):2155-2163. [32] SONG GY, ZHANG H, ZHANG J, et al. Greater Static Anterior Tibial Subluxation of the Lateral Compartment After an Acute Anterior Cruciate Ligament Injury Is Associated With an Increased Posterior Tibial Slope. Am J Sports Med. 2018;46(7):1617-1623. [33] MINAMI T, MUNETA T, SEKIYA I, et al. Lateral meniscus posterior root tear contributes to anterolateral rotational instability and meniscus extrusion in anterior cruciate ligament-injured patients. Knee Surg Sports Traumatol Arthrosc. 2018;26(4):1174-1181. [34] 张艺, 亓建洪.胫骨平台后倾角与半月板损伤的相关性研究进展[J].中国矫形外科杂志,2020,28(8):721-724. [35] GIFFIN JR, VOGRIN TM, ZANTOP T, et al. Effects of increasing tibial slope on the biomechanics of the knee. Am J Sports Med. 2004;32(2):376-382. [36] CHOI CJ, CHOI YJ, SONG IB, et al. Characteristics of radial tears in the posterior horn of the medial meniscus compared to horizontal tears. Clin Orthop Surg. 2011;3(2):128-132. |
| [1] | Li Xiaomin, Tian Xiangdong, Tan Yetong, Zhu Guangyu, Wang Rongtian, Wang Jian, Xue Zhipeng, Ma Sheng, Hu Yuanyi, Huang Ye, Ding Tiansong. Changes of lower limb force line and knee function after high tibial osteotomy in osteoporotic medial ventricular knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1325-1329. |
| [2] | Zhang Lichuang, Gao Huali, Wang Jingchao, Lin Huijun, Wu Chonggui, Ma Yinghui, Huang Yunfei, Fang Xue, Zhai Weitao. Effect of tendon manipulation with equal emphasis on muscles and bones on accelerating the functional rehabilitation of quadriceps femoris after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1383-1389. |
| [3] | Bi Gengchao, Zhang Yanlong, Li Qiuyue, Hu Longwei, Zhang Yu. Knee joint mechanics and activation characteristics of surrounding muscles during deep jumps at different heights and distances [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(8): 1211-1218. |
| [4] | Xiong Bohan, Yu Yang, Lu Xiaojun, Wang Xu, Yang Tengyun, Zhang Yaozhang, Liao Xinyu, Zhou Xiaoxiang, He Lu, Li Yanlin. Research progress in promoting tendon to bone healing during anterior cruciate ligament reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 779-786. |
| [5] | Liu Guangluan, Guo Zonglei, Ge Jin, Huang Dong, Wang Yehua. Anatomic risk factors for medial meniscus posterior root tears combined with anterior cruciate ligament injuries [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(5): 663-668. |
| [6] | Li Yaping, Liu Hong, Gao Zhen, Chen Xiaolin, Huang Wujie, Jiang Zheng. Three-dimensional motion analysis of lower limb biomechanical performance in Tai Chi practitioners accompanied by knee joint pain [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 520-526. |
| [7] | Wei Bo, Yao Qingqiang, Tang Cheng, Li Xuxiang, Xu Yan, Wang Liming. Advantage of medial pivot prosthesis in total knee arthroplasty via medial subvastus approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 552-557. |
| [8] | Wan Guoli, Shi Chenhui, Wang Weishan, Li Ang, Shi Xunda, Cai Yi. Retrospective analysis of the influencing factors of chronic pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 558-564. |
| [9] | Gu Mingxi, Wang Bo, Tian Fengde, An Ning, Hao Ruihu, Wang Changcheng, Guo Lin. Comparison of early efficacy and safety of simultaneous and staged bilateral total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 565-571. |
| [10] | Zhang Jinbiao, Li Xiaoming, Xing Wanlin, Ma Fei, Yu Qiaoya, Dai Rongqin. Early warning efficacy of thrombus molecular markers after total knee arthroplasty in patients complicated with venous thromboembolism [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 572-577. |
| [11] | Guo Yingqi, Gong Xianxu, Zhang Yan, Xiao Han, Wang Ye, Gu Wenguang. Meniscus extrusion and patellofemoral joint cartilage injury and bone marrow lesions: MRI semi-quantitative score [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 600-605. |
| [12] | Xu Xiangjun, Wang Chao, Song Qunshan, Li Bingyan, Zhang Jichao, Wang Guodong, Dong Yuefu. Optimal angle for prosthesis implantation in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 612-618. |
| [13] | Li Shihao, Li Qi, Li Zhen, Zhang Yuanyuan, Liu Miaomiao, Ouyang Yi, Xu Weiguo. Plantar pressure and gait analysis in patients with anterior cruciate ligament injury and reconstruction [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 626-631. |
| [14] | Yu Jiaan, Liu Xinwei, Lian Hongyu, Liu Kexin, Li Zitao. Medial open-wedge tibial osteotomy versus lateral closed-wedge tibial osteotomy for unicompartmental knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 632-639. |
| [15] | Xu Yangyang, He Peiliang, Meng Qingqi, Li Siming. A meta-analysis of the effects of continuous adductor canal block and continuous femoral nerve block on early activity after knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(4): 640-645. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||