Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (20): 3239-3245.doi: 10.3969/j.issn.2095-4344.3140
Previous Articles Next Articles
Applicability and specifications of platelet-rich plasma in musculoskeletal repair
Zuo Xiuqin1, Yin Sasa1, Xie Huimin1, Jia Zishan1, Zhang Lining1, 2
- 1Department of Rehabilitation Medicine, the First Medical Center of Chinese PLA General Hospital, Beijing 100853, China; 2Department of Orthopedics, the Military Prevention and Treatment Center for Training Injury, the Fourth Medical Center of Chinese PLA General Hospital, Beijing 100853, China
-
Received:2020-05-20Revised:2020-05-29Accepted:2020-07-09Online:2021-07-18Published:2021-01-18 -
Contact:Jia Zishan, MD, Chief physician, Department of Rehabilitation Medicine, the First Medical Center of Chinese PLA General Hospital, Beijing 100853, China Zhang Lining, MD, Associate chief physician, Department of Rehabilitation Medicine, the First Medical Center of the Chinese PLA General Hospital, Beijing 100853, China; Department of Orthopedics, the Military Prevention and Treatment Center for Training Injury, the Fourth Medical Center of Chinese PLA General Hospital, Beijing 100853, China -
About author:Zuo Xiuqin, Master, Attending physician, Department of Rehabilitation Medicine, the First Medical Center of Chinese PLA General Hospital, Beijing 100853, China -
Supported by:Plant Nursery Project of Chinese PLA General Hospital, No. 18KMM36 (to ZXQ); Military Medical Program for the Youth, No. QNF19019 (to ZXQ); Military Medical Innovation Program, No. CX19005 (to ZLN)
CLC Number:
Cite this article
Zuo Xiuqin, Yin Sasa, Xie Huimin, Jia Zishan, Zhang Lining. Applicability and specifications of platelet-rich plasma in musculoskeletal repair[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3239-3245.
share this article
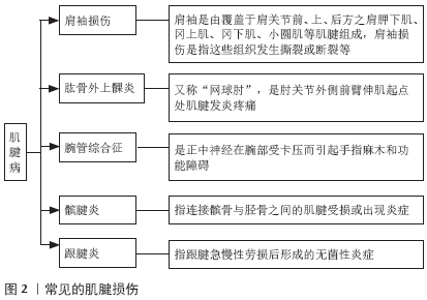
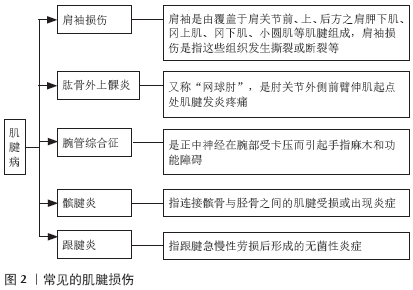
2.1 富血小板血浆的制备及激活 2.1.1 富血小板血浆的制备 目前,富血小板血浆的制备方法主要有手工分离法和全自动法2种。 (1)手工分离法:即密度梯度离心法,即在无菌条件下采集自体抗凝血后进行离心。自体血离心后,各种成分根据密度梯度可分3层:血浆层(上层)、白细胞和血小板层(中间层)、红细胞层(下层),去除血浆层和红细胞层,留取中间层后混合均匀即制得富血小板血浆。手工提取富血小板血浆按制备程序可分为一次离心法、二次离心法和三次离心法。一次离心法血小板的回收率不足,生长因子的浓度相对也比较低;三次离心法操作繁琐且血小板回收率下降,二次离心法富血小板血浆的提取率最高,故临床上应用最为广泛[4]。传统实验室制备富血小板血浆的方法较多,如Anitua法[5]、Petrungaro法[6]、Landesberg法[7]、Aghaloo法等[8],目前尚无统一的制备标准[9]。由于各种方法的离心力、离心次数和离心时间不同,所制备的富血小板血浆中血小板及生长因子的量及活性亦不相同。此外,各实验室的条件不同(如温度、离心设备、离心管材质、抗凝剂种类等),同时由于在离心及多次移液过程中以人工操作为主,每个制备者的操作习惯及衡量标准不一,故即便使用同一种制备方法,所获得的富血小板血浆仍会有误差[10]。 (2)全自动法:即血浆分离置换法,是利用多功能医用血成分自动分离设备采集并浓缩血小板,从而得到富血小板血浆,而其余成分(如红细胞、血浆等)则回输至患者体内。该方法可将白细胞尽可能的从血小板中分离出去,从而使制备血小板的浓度和纯度较高。相对手工操作而言,全自动法制备法能快速提取富血小板血浆,富血小板血浆成分的浓度也会相对较为稳定,且各系统制备的富血小板血浆的差别不大。但由于其设备系统价格相对昂贵,操作技术要求较高,限制了全自动法制备富血小板血浆在临床上的广泛应用[11]。国内有关富血小板血浆的研究及使用大多数仍使用传统的实验室制备方法手工制备。 2.1.2 富血小板血浆的激活 富血小板血浆根据应用形式可分为未激活的富血小板血浆和激活后的富血小板血浆(后者包括富血小板血浆凝胶和富血小板血浆释放物)。未激活的富血小板血浆从血小板中释放生长因子的量较少,激活后的富血小板血浆生长因子的释放量则可明显增加。由于体内有内源性凝血酶原激酶,故富血小板血浆应用于体内时,是否需体外激活仍存在争议。目前有多种激活富血小板血浆的方法,如通过添加凝血酶、钙剂(多为氯化钙)、壳聚糖和巴曲酶等多种方式活化,其中氯化钙和凝血酶是最常见的方式[12]。不同的富血小板血浆活化方式,也会影响生长因子的浓度。 2.2 富血小板血浆的成分及其生物学特性 富血小板血浆中含血小板、白细胞和红细胞等成分。 血小板是血液中具有质膜而无细胞核的有形成分之一,在正常人体血液中其数量较恒定,为(100-300)×109 L-1。高浓度的血小板是富血小板血浆中主要的成分,其主要作用为参与止血、组织修复及炎症反应等生理病理过程。富血小板血浆中的血小板被激活后,通过脱颗粒作用释放出大量生长因子及细胞因子,与修复细胞膜受体偶联后,诱导细胞内基因的表达,合成组织修复和再生过程中所需的蛋白质,促进各种组织的修复与再生[13]。血小板在激活过程中,纤维蛋白原转变成纤维蛋白,其主要作用为通过黏附反应参与凝血过程、收缩创面并为细胞增殖提供三维空间结构,有利于生长因子的分泌和组织修复,从而形成良性修复的正反馈循环[14-15]。研究发现,与未被激活的富血小板血浆相比,激活后的富血小板血浆其生长因子释放量显著增加,且促增殖作用也明显增强[16]。与治疗用外源性生长因子相比,富血小板血浆中的生长因子基本为正常生理比例,其适宜的比例有利于各生长因子之间更好地发挥作用。常见的因子有血管内皮细胞生长因子、转化生长因子β、血小板源性生长因子、成纤维细胞生长因子及胰岛素样生长因子等,其中,某些生长因具有刺激新生血管形成的作用,增加局部微循环,改善受损组织的血供,提供营养物质及氧含量[17-18]。血小板浓度与其相应的生物学效应并不成比例,因为血小板浓度过高或过低均不利于组织愈合,故需将血小板浓度控制在一定的范围,有学者提出最佳浓度为全血血小板生理浓度的3-8倍[19]。此外,不同的组织愈合或不同疾病种类对血小板的需求也存在差异,需根据不同的临床应用制备适宜浓度的血小板。 富血小板血浆根据白细胞含量的不同将其分为富白细胞的富血小板血浆与贫白细胞富血小板血浆[20]。目前富血小板血浆中,白细胞的作用仍然存有一定的争议。白细胞可吞噬病原体,具有抗感染及清除坏死组织的能力,在免疫应答过程中发挥重要作用,如中性粒细胞在炎症因子趋化作用下吞噬细菌,通过产生大量过氧化物和超氧化物杀灭病原体;单核细胞通过释放白细胞介素、细胞毒素及干扰素增强抗感染能力;巨噬细胞可以清除局部坏死组织,促使受损细胞循环再利用,加快组织的修复[21-22]。但也有研究认为,白细胞可能加剧炎性反应,尤其是中性粒细胞产生的促分解因子(如白细胞介素1β、肿瘤坏死因子α、基质金属蛋白酶等)会加速肌腱细胞、软骨细胞的凋亡,故富白细胞的富血小板血浆不适用于慢性退行性关节炎、肌腱病的治疗[23]。而在修复骨与软组织损伤,尤其是存在感染的情况下,建议应用富含白细胞的富血小板血浆[24]。 富血小板血浆中通常含有少量的红细胞。红细胞的主要功能是运送氧气、二氧化碳和一氧化氮,携带的氧气有利于组织修复。但有研究认为高浓度红细胞不利于组织修复,其中亚铁血红素释放的氧自由基,是引起关节软骨退变的主要原因[25]。此外,红细胞运送的一氧化氮可抑制及胰岛素样生长因子1的关节软骨修复从而继发滑膜细胞凋亡[26]。 2.3 临床应用 2.3.1 膝骨关节炎 膝关节骨性关节炎是最常见的慢性退行性疾病之一,严重影响患者的生活质量。研究显示,在中国40岁以上的中老年人膝关节骨性关节炎总患病率高达17%,其中女性约为22.2%,男性约为12.3%[27-28]。HALPERN等[29]对15例早期膝关节骨关节炎患者行富血小板血浆注射治疗,在治疗后6个月及12个月患者疼痛评分显著降低,临床功能评分增加。SIMENTAL-MENDíA等[30]将膝关节骨性关节炎(1至2 级)患者随机分为2组:一组口服6周乙酰氨基酚(500 mg/8 h),另一组行3次膝关节腔内富血小板血浆注射(每2周1次)。治疗后6,12和 24 周富血小板血浆注射患者的疼痛明显降低,生活质量较口服乙酰氨基酚组明显改善。FOROGH等[31]研究显示,与皮质类固醇对比,富血小板血浆单次注射可明显减轻膝关节骨关节炎患者(2至3级)的疼痛,提高患者的生活质量。 MONTA?EZ-HEREDIA等[32]随机对照研究表明,富血小板血浆注射与透明质酸钠注射相比,两者在缓解膝关节骨性关节炎患者疼痛方面没有明显的统计学差异,但富血小板血浆注射治疗能明显改善膝关节骨性关节炎患者的生活质量,尤其是注射后3个月;此外,症状较轻的膝关节骨关节炎患者富血小板血浆注射效果优于透明质酸钠注射。CAMPBELL等[33]通过对3项Meta分析研究发现,与对照组(关节腔内注射玻璃酸钠或安慰剂)相比,富血小板血浆注射对关节炎的影像学征象较少的患者即早期膝骨关节炎的疗效更佳。一项纳入7个随机对照研究,包含722例患者的系统分析显示,富血小板血浆注射对膝关节骨关节炎治疗优于透明质酸钠,但该研究中随访均未超过1年,故富血小板血浆注射对膝关节骨关节炎的长期疗效需进一步研究[34]。G?RMELI等[35]将162例不同分期的膝关节骨关节炎患者随机分为4组,3次富血小板血浆注射组,单次富血小板血浆注射组,单次玻璃酸钠注射组和单次生理盐水注射组(对照组),每组又分2个亚组,即早期骨关节炎组(KL分级1-3级)和晚期骨关节炎组(KL分级为4期)。结果显示,与对照组相比,注射后6个月所有的治疗组均有明显的改善,且3次富血小板血浆注射组效果优于单次富血小板血浆注射组和玻璃酸钠注射组,而单次富血小板血浆注射组和玻璃酸钠注射组之间无明显差异;此外,3次富血小板血浆注射对早期骨关节炎组患者显示出更好的治疗效果,而对晚期骨关节炎患者与其他治疗组比无明显差异。GATO-CALVO等[36]认为,尽管现有证据支持使用富血小板血浆治疗膝关节骨性关节炎,但其临床疗效仍存在争议,尚需进行标准化、高质量、大样本的随机对照研究,且富血小板血浆的长期疗效需进一步证实。 2.3.2 肌腱病 肌腱为束状、平行排列的纤维结构,为乏血供组织,一旦受损,难以愈合。肌腱撕裂或断裂后,往往通过瘢痕组织修复,无法重建良好的力学结构,再次断裂的发生率较高[37]。目前常见的肌腱损伤包括肩袖损伤、肱骨外上髁炎、腕管综合征、髌腱炎、跟腱炎等(图2)。近年来,富血小板血浆已越来越多地应用于肌腱病的治疗。 (1)肩袖损伤:富血小板血浆注射在肩袖损伤保守治疗中的研究相对较少。SENGODAN 等[38]对20例部分肩袖撕裂的患者行超声引导下富血小板血浆注射治疗,治疗后8周及12周患者肩关节疼痛减轻,肩关节功能改善,治疗后8周超声也显示了良好的愈合。SHAMS等[39]将40例肩袖损伤患者随机分为富血小板血浆组和激素治疗组,结果显示两组患者肩袖损伤较治疗前均有不同程度改善,治疗后6周和6个月时,两组间无明显差异,而治疗后3个月时,富血小板血浆注射优于激素治疗组,提示富血小板血浆注射可能成为皮质醇注射的一个替代方法。RHA等[40]的随机对照研究显示,与对照组(2次干针治疗)相比,超声引导下富血小板血浆注射(2次,每次间隔4周)更能减轻肩袖病变或部分撕裂(<1.0 cm)患者的疼痛,改善手臂功能,且能持续到治疗后6个月。一项纳入了 5 个随机对照研究的系统评价显示,对于慢性肩袖损伤行非手术治疗的患者,富血小板血浆注射短期内不能获益;而直接与运动疗法相比,富血小板血浆注射在运动功能、疼痛及关节活动度方面没有明显的优势[41]。 近年来,富血小板血浆越来越多地应用于肩袖损伤后手术的辅助治疗中。一项纳入了8个随机对照研究、包括556例患者的系统评价显示, 富血小板血浆注射可有效改善关节镜下全层肩袖撕裂修复术后的短期疗效,减轻疼痛,改善肩关节功能,降低肩袖再发撕裂的风险,尤其在单排固定中使用富血小板血浆比其他固定技术的临床效果更好[42]。HURLEY等[43]对18项随机对照试验进行了研究,发现关节镜修复术联合应用富血小板血浆能显著降低小-中等和中等-完全撕裂患者的不完全愈合率,提高肌腱愈合速度、减轻疼痛,改善功能。关于富血小板血浆治疗的长期疗效的研究较少。CARR等[44]将60例患者随机分为关节镜下肩峰成形术联合富血小板血浆组及关节镜下肩峰成形术组,经过2年随访结果显示,与单纯手术相比,联合应用富血小板血浆并未显著改善临床结局;此外,在联合应用富血小板血浆组肌腱活检标本中,观察到抗增殖、抗血管新生及促凋亡的组织变化可能对肌腱的愈合产生有害影响,增加撕裂的可能性。 故富血小板血浆可作为一种辅助治疗方法应用于在肩袖损伤的患者中,但其远期疗效需进一步研究。 (2)肱骨外上髁炎:肱骨外上髁炎,又称“网球肘”。MISHRA等[45]的一项纳入230例肱骨外上髁炎患者的多中心随机对照研究显示,治疗后12周,富血小板血浆注射组较对照组(注射布比卡因)在 目测类比(VAS)评分和 PRTEE(病患网球肘评估)评分无明显差异;治疗后24周,富血小板血浆组显著优于对照组。一项纳入了 7 个随机对照研究涉及515例患者的系统评价显示,治疗后6个月,富血小板血浆注射组在减轻疼痛及改善肘功能方面更优于局部激素注射组[46]。另一项纳入9项荟萃分析、包含8 656例患者的系统综述表明,激素注射治疗可在短期内改善肱骨外上髁炎患者的功能和减轻疼痛[47],而富血小板血浆注射治疗是中期最有效的治疗方法。目前,富血小板血浆治疗肱骨外上髁炎,大多数研究效果肯定。 (3)腕管综合征:目前富血小板血浆被用于腕管综合征的研究中。KUO等[48]报道1例皮质类固醇注射无效的双侧腕管综合征患者(病程2个月),在超声引导下将富血小板血浆注入腕管,2周内疼痛、异常感觉及双手感觉迟钝逐渐减轻;治疗3个月后,肌电图显示双侧正中神经远端运动及感觉潜伏期、感觉神经动作电位和复合肌肉动作电位振幅均有明显改善,该研究通过电生理为富血小板血浆的有效性提供了客观证据。WU等[49]研究发现,对于轻到中度腕管综合征患者,富血小板血浆注射治疗更能缓解疼痛及麻木症状,手部功能评分也优于支具固定组,且治疗效果至少维持6个月。一项纳入4个随机对照研究、97例患者的系统回顾显示,与安慰剂、保守治疗及局部注射糖皮质激素相比,富血小板血浆注射治疗至少在短期内能减少患者的疼痛,改善感觉及运动功能,且并发症发生率低,可作为轻至中度患者的治疗方法[50]。但该研究纳入患者人数较少,随访时间短,需进一步研究其临床适应证及长期疗效。 (4)髌腱炎:髌腱炎又称作跳跃者膝 (jumper’s knee),在运动损伤中常见。DRAGOO等[51]通过对保守治疗无效的23例患者行超声引导下富血小板血浆注射或干针治疗,治疗后12周,富血小板血浆治疗组的维多利亚运动学院评分(VISA-P)明显优于干针治疗组,而26周时两组评分无明显差异。这表明富血小板血浆对髌骨肌腱病变的益处可能是症状的早期改善。VETRANO等[52]对46例经超声证实的慢性单侧髌腱病变随机接受2周内2次富血小板血浆注射或3次聚焦体外冲击波治疗(ECSWT)。治疗后2个月,两组无显著性差异,但治疗后6个月和12个月,富血小板血浆组的VISA-P和目测类比评分较聚焦体外冲击波治疗组有显著性改善,且12个月后,改良 Blazina量表评分优于聚焦体外冲击波治疗组,提示注射富血小板血浆治疗髌腱炎较聚焦体外冲击波治疗能取得更好的中期疗效。CHAROUSSET等[53]对28例慢性髌腱炎患者行超声引导下连续3次(间隔1周)富血小板血浆治疗,结果显示其可显著改善患者的症状和功能,MRI提示肌腱结构的完整性也得到改善。一项纳入70个研究、包括2 350例患者的系统综述显示,多次注射富血小板血浆是非手术治疗的慢性髌腱炎患者的合适选择[54]。 (5)跟腱炎:MONTO[55]对30例保守治疗(至少 6 个月)无效的慢性跟腱炎患者行超声引导下单次富血小板血浆治疗,治疗后 3 个月,美国矫形足踝协会(AOFAS)评分明显提高(由34分提高到92 分),治疗后2年平均AOFAS评分维持在88分;且治疗后 6 个月,27 例患者的MRI 和/或超声异常信号缩小,28 例患者临床症状明显改善。BOESEN等[56]通过一项随机双盲前瞻性研究显示离心运动结合高剂量类固醇类注射在短期内改善慢性中段跟腱炎的效果优于离心运动结合富血小板血浆治疗。一项纳入了5个随机对照研究、189例患者的系统回顾显示,富血小板血浆对慢性肌腱病的注射治疗并不优于安慰剂治疗[57]。目前关于富血小板血浆治疗跟腱炎的报道相对较少,需进一步研究。 2.3.3 其他 HEGAB 等[58]将50例颞下颌关节骨关节炎患者随机分为2组,一组行3次1 mL富血小板血浆注射治疗,另一组行3次1 mL低分子透明质酸注射治疗,结果显示富血小板血浆治疗组中患者疼痛减轻及开口度增加程度方面优于透明质酸钠组。一项包含6个随机对照研究的系统回顾显示,与安慰剂组相比,关节内注射富血小板血浆后6个月及12个月,更有效减轻颞下颌关节骨关节炎患者的疼痛;与透明质酸钠相比,富血小板血浆注射后12个月也能看到这种显著的疼痛减轻的差异[59]。由于该研究纳入的所有实验均显示出适度的偏倚风险,故仍需大规模、低偏倚的随机对照研究来证明富血小板血浆注射治疗是否应该成为颞下颌关节骨关节炎患者的常规治疗方法。 很少的研究涉及脊柱融合术[60]、股骨头坏死[61]、骨折愈合等[62],其疗效有待进一步评估。 "
| [1] HARKE H, TANGER D, FÜRST-DENZER S, et al. Effect of a preoperative separation of platelets on the postoperative blood loss subsequent to extracorporeal circulation in open heart surgery (author’s transl). Anaesthesist. 1977;26(2):64-71. [2] OKUDA K, KAWASET, MOMOSEM, et al. Platelet-rich plasma contains high levels of platelet-derived growth factor and transforming growth factor-beta and modulates the proliferation of periodontally related cells in vitro. J Periodontol. 2003;74(6):849-857. [3] WHITMAN DH, BERRY RL, GREEN DM. Platelet gel: an autologous alternative to fibrin glue with applications in oral and maxillofacial surgery. J Oral Maxillofac Surg. 1997;55(11):1294-1299. [4] 王淑君,赵广超,栾建凤,等.不同规格全血制备富血小板血浆的最佳离心条件研究[J].临床输血与检验,2017,19(2):119-122. [5] ANITUA E. Rich in growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants. 1999;14(4):529-535. [6] PETRUNGARO PS. Using platelet-rich plasma to accelerate soft tissue maturation in esthetic periodontal surgery. Compend Contin Educ Dent. 2001;22(9):729-732, 734, 736 passim; quiz 746. [7] LANDESBERG R, ROY M, GLICKMAN RS. Quantification of growth factor levels using a simplified method of platelet-rich plasma gel preparation. J Oral Maxillofac Surg. 2000;58(3):297-300; discussion 300-301. [8] AGHALOO TL, MOY PK, FREYMILLER EG. Investigation of platelet-rich plasma in rabbit cranial defects: A pilot study. J Oral Maxillofac Surg. 2002;60(10):1176-1181. [9] KRAMER MARYJO E, KEANEY TERRENCE C. Systematic review of platelet-rich plasma (PRP) preparation and composition for the treatment of androgenetic alopecia. J CosmetDermatol. 2018;17(5):666-671. [10] OYAMA T, NISHIMOTO S, TSUGAWA T, et al. Efficacy of platelet-rich plasma in alveolar bone grafting. J Oral Maxillofac Surg. 2004;62(5): 555-558. [11] 刘泉体,兰婷,吴佳奇.富血小板血浆制备技术及其抗菌效应的研究进展[J].重庆医学,2019,48(9):1572-1575. [12] 邓勇,葛建华,鲁晓波.富血小板血浆对骨折愈合影响的研究进展[J].西南军医,2012,14(2):345-347. [13] 林敏魁,闫福华.富血小板血浆用于牙周组织再生的研究[J].临床口腔医学杂志,2003,19(11):656-658. [14] DRENGK A, ZAPF A, STURMER EK, et al. Influence of platelet-rich plasma on chondrogenic differentiation and proliferation of chondrocytes and mesenchymal stem cells. Cells Tissues Organs. 2009;189(5):317-326. [15] SOMMAR P, PETTERSSON S, NESS C, et al. Engineering three-dimensional cartilage- and bone-like tissues using human dermal fibroblasts and macroporousgelatinemicrocarriers.J PlastReconstrAesthet Surg. 2010;63(6):1036-1046. [16] LACOSTE E, MM’TINEAU I, GAGNON G. Platelet concentrates:effects of calcitmaandthrombin on endothelial cell proliferationandgrowth factor release. J Periodontol. 2003;74(10):1498-1507. [17] OSTVAR O, SHADVAR S, YAHAGHI E, et al. Effect of platelet-rich plasma on the healing of cutaneous defects exposed to acute to chronic wounds: a clinico-histopathologic study in rabbits.Diagn Pathol. 2015; 10(1):85. [18] WASTERLAIN AS, BRAUN HJ, DRAGOO JL. Contents and formulations of platelet-rich plasma. Ope Tech Orthop. 2012;22(1):33-42. [19] GIUSTI I, RUGHETTI A, D’ASCENZO S, et al. Identifcation of an optimal concentration of platelet gel for promoting angiogenesis in human endothelial cells. Transfusion. 2009;49(4):771-778. [20] EVERTS PA, KNAPE JT, WEIBRICH G, et al. Platelet-rich plasma and platelet gel:a review. Extra Corpor Techol. 2006;38(2):174-187. [21] YUAN T, ZHANG CQ, TANG MJ, et al. Autologous Platelet-rich plasma enhances healing 0f chronic wounds. Wounds. 2009;21(10):280-285. [22] BOSWELL SG, SCHNABEL LV, MOHAMMED HO, et al. Increasing platelet concentrations in leukocyte-reduced platelet-rich plasma decrease collagen gene synthesis in tendons. Am J Sports Med. 2014;42(1): 42-49. [23] YUAN T, ZHANG CQ, WANG JH. Augmenting tendon and ligament repair with platelet-rich plasma (PRP).Muscles ligaments Tendons J. 2013;3(3):139-149. [24] 张长青,袁霆.富血小板血浆在临床应用中的争议与研究进展[J].中华关节外科杂志( 电子版),2016,10(6):588-591. [25] PIAOL, PARK H, JO CH. Theoretical prediction and validation of cell recovery rates in preparing platelet - rich plasma through a centrifugation. PLoSOne. 2017;12(11):eI87509. [26] FRANKLIN SP, GAMER BC, COOK JL. Characteristics of canine platelet-rich plasma prepared with five commercially available systems. Am J Vet Res. 2015;76(9):822. [27] 帖小佳,郑如庚,赵梦,等.中国中老年人膝关节骨关节炎患病率的Meta分析[J].中国组织工程研究,2018,22(4):650-656. [28] 王斌,邢丹,董圣杰,等.中国膝骨关节炎流行病学和疾病负担的系统评价[J].中国循证医学杂志,2018,18(2):134-142. [29] HALPERN B, CHAUDHURY S, RODEO SA, et al. Clinical and MRI outcomes after platelet-rich plasma treatment for knee osteoarthritis . Clin J Sport Med. 2013;23(3):238-239. [30] SIMENTAL-MENDÍA M, VÍLCHEZ-CAVAZOS JF, PEÑA-MARTÍNEZ VM, et al. Leukocyte-poor platelet-rich plasma is more effective than the conventional therapy with acetaminophen for the treatment of early knee osteoarthritis. Arch Orthop Trauma Surg. 2016;136(12): 1723-1732. [31] FOROGH B, MIANEHSAZ E, SHOAEE S, et al. Effect of single injection of platelet-rich plasma in comparison with corticosteroid on knee osteoarthritis: a double-blind randomized clinical trial.J Sports Med Phys Fitness. 2016;56(7-8):901-908. [32] MONTAÑEZ-HEREDIA E, IRÍZAR S, HUERTAS PJ, et al. Intra-Articular Injections of Platelet-Rich Plasma versus Hyaluronic Acid in the Treatment of Osteoarthritic Knee Pain:A Randomized Clinical Trial in the Context of the Spanish National Health Care System. Int J MolSci. 2016;17(7):1064. [33] CAMPBELL KA, SALTZMAN BM, MASCARENHAS R, et al. Does Intra-articular Platelet-Rich Plasma Injection Provide Clinically Superior Outcomes Compared With Other Therapies in the Treatment of Knee Osteoarthritis? A Systematic Review of Overlapping Meta-analyses. Arthroscopy. 2015;31(11):2213-2221. [34] SADABAD HN, BEHZADIFAR M, ARASTEH F, et al. Efficacy of platelet-rich plasma versus hyaluronic acid for treatment of knee osteoarthritis: A systematic review and meta-analysis. Electron Physician. 2016;8(3): 2115-2122. [35] GÖRMELI G, GÖRMELI CA, ATAOGLU B, et al. Multiple PRP injections are more effective than single injections and hyaluronic acid in knees with early osteoarthritis: a randomized, double-blind, placebo-controlled trial. Knee Surg Sports Traumatol Arthrosc. 2017;25(3):958-965. [36] GATO-CALVOL, MAGALHAESJ, RUIZ-ROMERO C, et al. Platelet-rich plasma in osteoarthritis treatment: review of current evidence. TherAdv Chronic Dis. 2019;10:2040622319825567. [37] YUAN T, ZHANG CQ, WANG JH. Augmenting tendon and ligament repair with platelet-rich plasma ( PRP). Muscles Ligaments Tendons J. 2013;3(3):139-149. [38] SENGODAN VC, KURIAN S, RAMASAMY R. Treatment of partial rotator cuff tear with ultrasound-guided platelet-rich plasma. J Clin Imaging Sci. 2017;7:32. [39] SHAMS A, EL-SAYED M, GAMAL O, et al. Subacromial injection of autologous platelet-rich plasma versus corticosteroid for the treatment of symptomatic partial rotator cuff tears. Eur J OrthopSurgTraumatol. 2016;26(8):837-842. [40] RHA DW, PARK GY, KIM YK, et al. Comparison of the therapeutic effects of ultrasound-guided platelet-rich plasma injection and dry needling in rotator cuff disease: a randomized controlled trial. Clin Rehabil. 2013; 27(2):113‐122. [41] HURLEY ET, HANNON CP, PAUZENBERGER L, et al. Nonoperative treatment of rotator cuff disease with platelet-rich plasma:a systematic review of randomized controlled trials. Arthroscopy. 2019;35(5): 1584-1591. [42] WANG C, XU M, GUO W, et al. Clinical efficacy and safety of platelet-rich plasma in arthroscopic full-thickness rotator cuff repair:a meta-analysis. PLoS One. 2019;14(7):e0220392 [43] HURLEY ET, LIM FAT D, MORAN CJ, et al.The Efficacy of Platelet-Rich Plasma and Platelet-Rich Fibrin in Arthroscopic Rotator Cuff Repair: A Meta-analysis of Randomized Controlled Trials.Am J Sports Med. 2019;47(3):753-761. [44] CARR AJ, MURPHY R, DAKIN SG, et al. Platelet-Rich Plasma Injection With Arthroscopic Acromioplasty for Chronic Rotator Cuff Tendinopathy: A Randomized Controlled Trial. Am J Sports Med. 2015; 43(12):2891-2897. [45] MISHRA AK, SKREPNIK NV, EDWARDS SG, et al. Efficacy of platelet-rich plasma for chronic tennis elbow: a double-blind, prospective, multicenter, randomized controlled trial of 230 patients. Am J Sports Med. 2014;42(2):463-471. [46] XU Q, CHEN J, CHENG L.Comparison of platelet rich plasma and corticosteroids in the management of lateral epicondylitis:a meta-analysis of randomized controlled trials. Int J Surg.2019;67:37-46. [47] HOUCK DA, KRAEUTLER MJ, THORNTON LB, et al. Treatment of lateral epicondylitiswith autologous blood, platelet-rich plasma, or corticosteroid Injections: A systematic review of overlapping meta-analyses. Orthop J Sports Med. 2019;7(3):2325967119831052. [48] KUO YC, LEE CC, HSIEH LF. Ultrasound-guided perineural injection with platelet-rich plasma improved the neurophysiological parameters of carpal tunnel syndrome: A case report. J ClinNeurosci. 2017;44: 234-236. [49] WU YT, HO TY, CHOU YC, et al.Six-month efficacy of platelet-rich plasma for carpal tunnel syndrome: A prospective randomized, single-blind controlled trial. Sci Rep. 2017;7(1):94. [50] CATAPANO M, CATAPANO J, BORSCHEL G, et al. Effectiveness of platelet-rich plasma injections for nonsurgical management of carpal tunnel syndrome: asystematic review and meta-analysis of randomized controlled trials. Arch Phys Med Rehabil. 2020;101(5):897‐906. [51] DRAGOO JL, WASTERLAIN AS, BRAUN HJ, et al. Platelet-rich plasma as a treatment for patellar tendinopathy: a double-blind, randomized controlled trial. Am J Sports Med. 2014;42(3):610-618. [52] VETRANO M, CASTORINA A, VULPIANI MC, et al. Platelet-rich plasma versus focused shock waves in the treatment of jumper’s knee in athletes. Am J Sports Med. 2013;41(4):795-803. [53] CHAROUSSET C, ZAOUI A, BELLAICHE L, et al. Are multiple platelet-rich plasma injections useful for treatment of chronic patellar tendinopathy in athletes? a prospective study. Am J Sports Med. 2014;42(4):906-911. [54] ANDRIOLO L, ALTAMURA SA, REALE D, et al. Nonsurgicaltreatments of patellar tendinopathy: multiple injections of platelet-rich plasma are a suitable option: asystematic review and meta-analysis. Am J Sports Med. 2019;47(4):1001-1018. [55] MONTO RR. Platelet rich plasma treatment for chronic Achilles tendinosis. Foot Ankle Int. 2012;33(5):379-385. [56] BOESEN AP, HANSEN R, BOESEN MI, et al. Effect of high-volume injection, platelet-rich plasma, and sham treatment in chronic midportionachillestendinopathy: arandomized double-blinded prospective study. Am J Sports Med. 2017;45(9):2034-2043. [57] LIU CJ, YU KL, BAI JB, et al. Platelet-rich plasma injection for the treatment of chronic Achilles tendinopathy: A meta-analysis. Medicine (Baltimore). 2019;98(16):e15278. [58] HEGAB AF, ALI HE, ELMASRY M, et al. Platelet-Rich Plasma Injection as an Effective Treatment for Temporomandibular Joint Osteoarthritis. J Oral Maxillofac Surg. 2015;73(9):1706-1713. [59] LI F, WU C, SUN H, et al. Effect of Platelet-Rich Plasma Injections on Pain Reduction in Patients with Temporomandibular Joint Osteoarthrosis: A Meta-Analysis of Randomized Controlled Trials.J Oral Facial Pain Headache. 2020;34(2):149-156. [60] SYS J, WEYLER J, VAN DER ZIJDEN T, et al. Platelet-rich plasma in mono-segmental posterior lumbar interbody fusion. Eur Spine J. 2011;20(10): 1650-1657. [61] PAK J, LEE JH, JEON JH, et al. Complete resolution of avascular necrosis of the human femoral head treated with adipose tissue-derived stem cells and platelet-rich plasma. J Int Med Res. 2014;42(6):1353-1362. [62] SAMY AM. The role of platelet rich plasma in management of fracture neck femur: new insights. IntOrthop. 2016;40(5):1019-1024. [63] RUTH S, SARAHH, GIORGIO P, et al. Wound-healing properties of trehalose-stabilized freeze-dried outdated platelets. Transfusion. 2007; 47(4):672-679. |
| [1] | Jiang Hongying, Zhu Liang, Yu Xi, Huang Jing, Xiang Xiaona, Lan Zhengyan, He Hongchen. Effect of platelet-rich plasma on pressure ulcers after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1149-1153. |
| [2] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [3] | Cao Xuhan, Bai Zixing, Sun Chengyi, Yang Yanjun, Sun Weidong. Mechanism of “Ruxiang-Moyao” herbal pair in the treatment of knee osteoarthritis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 746-753. |
| [4] | Li Yonghua, Feng Qiang, Tan Renting, Huang Shifu, Qiu Jinlong, Yin Heng. Molecular mechanism of Eucommia ulmoides active ingredients treating synovitis of knee osteoarthritis: an analysis based on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 765-771. |
| [5] | Yang Wei, Chen Zehua, Yi Zhiyong, Huang Xudong, Han Qingmin, Zhang Ronghua. Effectiveness of intra-articular injection of hyaluronic acid versus placebo in the treatment of early and mid-stage knee osteoarthritis: a Meta-analysis based on randomized, double-blind, controlled, clinical trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3760-3766. |
| [6] | Zhu Shiqiang, Xu Jianfeng, Hei Xiaoyan, Chen Yundong, Tian Xinbao, Zhang Jinchen, Lin Ruizhu. Effect of internal heat-type acupuncture needle therapy on the expression of type I collagen, matrix metalloproteinase-3 and osteopontin in the subchondral bone of rabbit knee osteoarthritis model [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(17): 2636-2642. |
| [7] | Yin Yuhui, Zhan Jiawen, Wang Shangquan, Shao Chenchen, Zhou Liang. Meta-analysis of acupuncture combined with massage in the treatment of knee osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(17): 2719-2726. |
| [8] | Chen Jufang, Tian Yulou, Hao Xin. Role and potential of adipose-derived stem cells in cranio-maxillofacial bone regeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(13): 2087-2096. |
| [9] | Tian Yanping, Li Juan, Liu Xiaobo, Zhang Huiling, Shi Lihong, Jin Rongjiang. Knowledge network mapping of literature regarding platelet-rich plasma in recent 5 years: a visual analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1745-1752. |
| [10] | Liu Peidong, Feng Jiangfeng, Xu Wenjie, Xu Xiaodong, Yang Ziquan . Bioinformatics analysis of gene expression profile and key pathways related to fatty infiltration after rotator cuff injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1773-1778. |
| [11] | Yu Chenghao, Zhang Yi, Qi Chao, Chen Jinli, Gao Jiake, Yu Tengbo. Effect of cytokines and platelet-rich plasma on tendon derived stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(1): 133-140. |
| [12] | Wang Ning, Zhong Weijian. Application and function of autologous blood concentrate in tissue regeneration [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(1): 146-151. |
| [13] | Xiu Yiping, Zhang Liyan, Qian Xueyi, Li Yan, Li Wantong. The clinical application of platelet-rich plasma to repair chronic refractory wounds: a retrospective study and literature retrieval evidence analysis [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(8): 1231-1237. |
| [14] | Qiu Guorong, He Benxiang, Wang Chun. Biological mechanism of platelet-rich plasma for tendinopathy repair: a visual study based on scientific knowledge map [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 787-795. |
| [15] | Jing Xiaowei, Mu Yingxiu. A study on anterior cruciate ligament injury and knee stability with a silicon mesh brace [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(4): 505-510. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||