Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (30): 4795-4801.doi: 10.3969/j.issn.2095-4344.2836
Previous Articles Next Articles
Platelet count as a novel potential predictor of periprosthetic joint infection
Cao Houran1, Deng Peng2, Ye Pengcheng2, Jie Ke1, Zeng Jianchun2, Feng Wenjun2, Chen Jinlun2, Qi Xinyu1, Li Jie2, Tan Xueqiu1, Zhang Haitao1, Zeng Yirong2
- 1First Clinical Medical College of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China; 2First Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China
-
Received:2020-01-07Revised:2020-01-16Accepted:2020-03-04Online:2020-10-28Published:2020-09-19 -
Contact:Zeng Yirong, MD, Chief physician, First Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, Guangdong Province, China -
About author:Cao Houran, Master candidate, First Clinical Medical College of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China -
Supported by:the Moral Education Program of Innovation and Strong Academy Project of First Affiliated Hospital of Guangzhou University of Chinese Medicine, No. 2019IIT35
CLC Number:
Cite this article
Cao Houran, Deng Peng, Ye Pengcheng, Jie Ke, Zeng Jianchun, Feng Wenjun, Chen Jinlun, Qi Xinyu, Li Jie, Tan Xueqiu, Zhang Haitao, Zeng Yirong. Platelet count as a novel potential predictor of periprosthetic joint infection[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(30): 4795-4801.
share this article
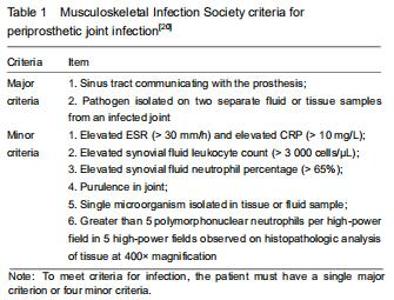
The study was approved by the Institutional Review Board of the First Affiliated Hospital of Guangzhou University of Chinese Medicine (approval No. 2019205). This single-center, retrospective, cohort study enrolled patients who underwent revision arthroplasty because of delayed or chronic infection of joint arthroplasties and aseptic loosening of an implant from March 2013 to December 2018 in the First Affiliated Hospital of Guangzhou University of Chinese Medicine. PJI was diagnosed based on the MSIS criteria noted in Table 1[20]. Patients were excluded if they had hematological disease or underwent a blood transfusion within the last year, used ongoing antiplatelet drugs, had a history of recent trauma or dislocation (within 2 weeks), used lipid emulsion, associated with hepatic disease or other site infections. "
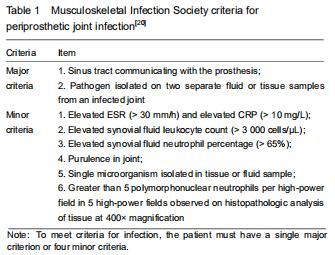
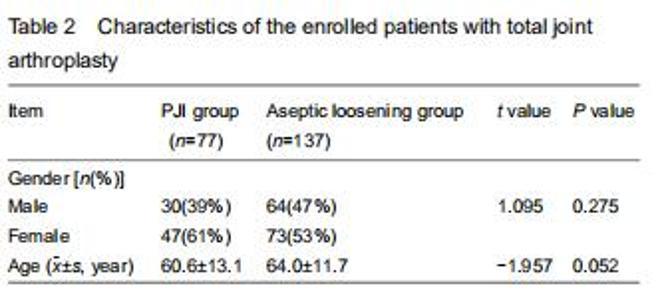
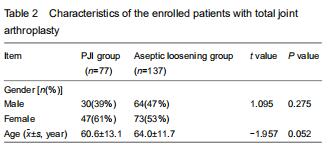
A total of 214 patients were recruited for the final analysis. Based on the MSIS criteria, 77 patients were classified into the PJI group (129 hips and 8 knees), while 137 patients were classified into the aseptic loosening group. The mean age in the PJI group was 60.6±13.1 years (range, 21-80 years); of them, 30 were men and 47 were women. The mean age in the aseptic loosening group was 64.0±11.7 years (range, 30-86 years); of them, 64 were men and 73 were women. No significant intergroup differences were detected in gender or age (P > 0.05). The characteristics of the enrolled patients are shown in Table 2. "
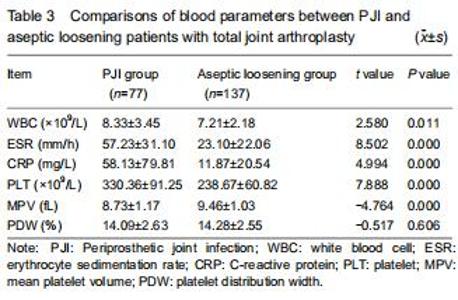
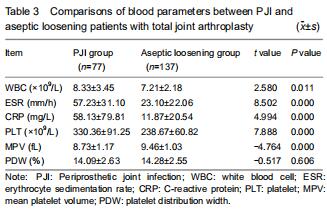
Serum PLT was significantly higher in the PJI group (330.36 ± 91.25 × 109/L) than in the aseptic loosening group (238.67 ± 60.82 × 109/L) (P < 0.001). WBC, ESR, and CRP values were also significantly higher among patients with PJI (P < 0.05). The mean MPV was also significantly higher in the PJI group than in the aseptic loosening group (P < 0.001). No significant intergroup differences were detected in the PDW values (P > 0.05; Table 3). "
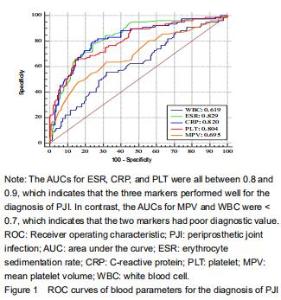
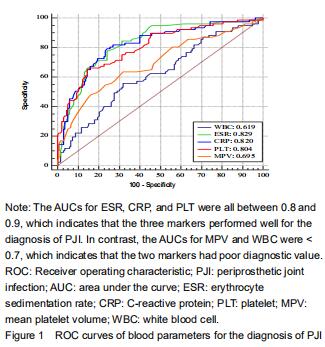
The ROC curves showed that ESR had the highest AUC (0.829), followed by CRP (0.820), and PLT (0.804). The AUCs of these three markers were all between 0.8 and 0.9, indicating good diagnostic value for PJI. In contrast, MPV had an AUC of 0.695, which was the second lowest value but slightly higher than the AUC of WBC (0.619). The AUCs of these two markers were both lower than 0.7, indicating poor diagnostic value (Figure 1). "
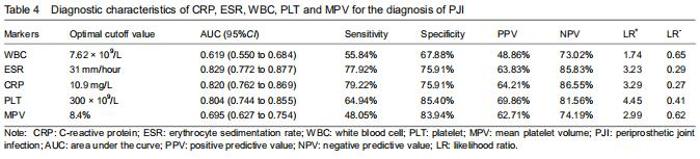
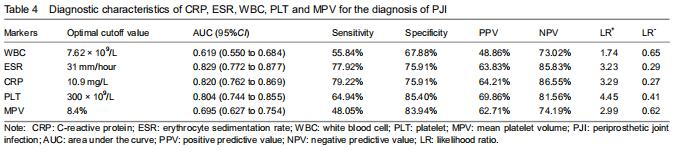
The serum PLT demonstrated a sensitivity of 64.94% and a specificity of 85.40% for diagnosing PJI. Using Youden’s index, the optimal cutoff value for PLT was 300 × 109/L, which resulted in a good PPV and NPV of 69.56% and 81.56%, respectively. Based on the ROC analysis, when WBC was above 7.62 × 109/L, the sensitivity, specificity, PPV, and NPV were 55.84%, 67.88%, 48.86%, and 73.02%, respectively. Using a cutoff value for ESR of 31 mm/h, the sensitivity, specificity, PPV, and NPV were 77.92%, 75.91%, 63.83%, and 85.83%; using a cutoff value for CRP at 10.9 mg/L, the sensitivity, specificity, PPV, and NPV were 79.22%, 75.91%, 64.21%, and 86.55%, respectively. For MPV, the optimal cutoff value was 8.4%, resulting in sensitivity, speci?city, PPV, and NPV of 48.05%, 83.94%, 62.71%, and 74.19%, respectively (Table 4). "
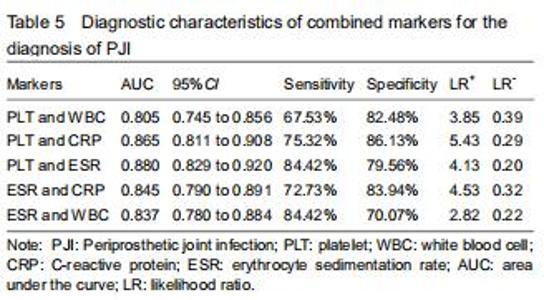
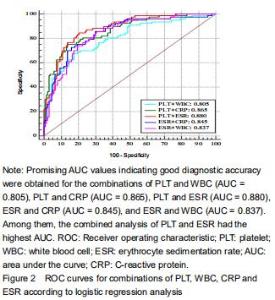
Further analyses of the combined diagnostic value of PLT, WBC, ESR, and CRP were performed to improve their diagnostic accuracies. The combination of serum PLT and WBC/ESR improved the specificity and specificity (Table 5). PLT combined with the CRP improved the specificity but decreased the sensitivity. Promising AUC values indicating good diagnostic accuracy were obtained for the combinations of PLT and WBC (AUC = 0.805), PLT and CRP (AUC = 0.865), PLT and ESR (AUC = 0.880), ESR and CRP (AUC = 0.845), and ESR and WBC (AUC = 0.837) (Figure 2). Among them, the combined analysis of PLT and ESR had the highest AUC. The sensitivity, specificity, and AUC were 84.42%, 79.96%, and 0.880 (95%CI, 0.829-0.920). "
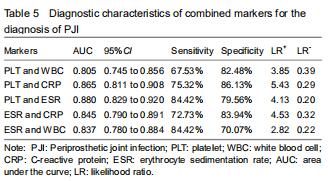
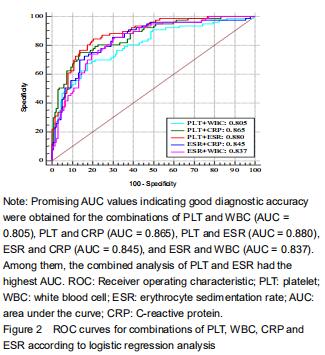
Further analyses of the combined diagnostic value of PLT, WBC, ESR, and CRP were performed to improve their diagnostic accuracies. The combination of serum PLT and WBC/ESR improved the specificity and specificity (Table 5). PLT combined with the CRP improved the specificity but decreased the sensitivity. Promising AUC values indicating good diagnostic accuracy were obtained for the combinations of PLT and WBC (AUC = 0.805), PLT and CRP (AUC = 0.865), PLT and ESR (AUC = 0.880), ESR and CRP (AUC = 0.845), and ESR and WBC (AUC = 0.837) (Figure 2). Among them, the combined analysis of PLT and ESR had the highest AUC. The sensitivity, specificity, and AUC were 84.42%, 79.96%, and 0.880 (95%CI, 0.829-0.920). "
|
[1] KIM K, ZHU M, CAVADINO A, et al. Failed debridement and implant retention does not compromise the success of subsequent staged revision in infected total knee arthroplasty. J Arthroplasty. 2019;34(6):1214-1220.e1.
[2] PETIS SM, PERRY KI, MABRY TM, et al. Two-stage exchange protocol for periprosthetic joint infection following total knee arthroplasty in 245 knees without prior treatment for infection. J Bone Joint Surg Am. 2019; 101(3):239-249.
[3] PREOBRAZHENSKY PM, BOZHKOVA SA, KAZEMIRSKY AV, et al. Functional outcome of two-stage reimplantation in patients with periprosthetic joint infection after primary total knee arthroplasty. Int Orthop. 2019;43(11):2503-2509.
[4] SRIVASTAVA K, BOZIC KJ, SILVERTON C, et al. Reconsidering strategies for managing chronic periprosthetic joint infection in total knee arthroplasty: using decision analytics to find the optimal strategy between one-stage and two-stage total knee revision. J Bone Joint Surg Am. 2019;101(1):14-24.
[5] RENARD G, LAFFOSSE JM, TIBBO M, et al. Periprosthetic joint infection in aseptic total hip arthroplasty revision. Int Orthop. 2020;44(4):735-741.
[6] NIKOLAUS OB, MCLENDON PB, HANSSEN AD, et al. Factors associated with 20-year cumulative risk of infection after aseptic index revision total knee arthroplasty. J Arthroplasty. 2016;31(4):872-877.
[7] PARVIZI J, GEHRKE T; International Consensus Group on Periprosthetic Joint Infection. Definition of periprosthetic joint infection. J Arthroplasty. 2014;29(7):1331.
[8] DI BENEDETTO P, BUTTIRONI MM, CAUSERO A. Biomarkers and infections in orthopedics: our experience and literature review. J Biol Regul Homeost Agents. 2018; 32(6 Suppl. 1):51-56.
[9] SALEH A, GEORGE J, FAOUR M, et al. Serum biomarkers in periprosthetic joint infections. Bone Joint Res. 2018;7(1): 85-93.
[10] KHEIR MM, TAN TL, SHOHAT N, et al. Routine diagnostic tests for periprosthetic joint infection demonstrate a high false-negative rate and are influenced by the infecting organism. J Bone Joint Surg Am. 2018;100(23):2057-2065.
[11] AHMAD SS, HIRSCHMANN MT, BECKER R, et al. A meta-analysis of synovial biomarkers in periprosthetic joint infection: Synovasure™ is less effective than the ELISA-based alpha-defensin test. Knee Surg Sports Traumatol Arthrosc. 2018;26(10):3039-3047.
[12] ZHANG Z, JI Y, WANG Z, et al. The association between platelet indices and deep surgical site infection after open induction internal fixation for traumatic limb fractures. Infect Drug Resist. 2018;11:2533-2538.
[13] DEMIRDAL T, SEN P. The significance of neutrophil-lymphocyte ratio, platelet-lymphocyte ratio and lymphocyte-monocyte ratio in predicting peripheral arterial disease, peripheral neuropathy, osteomyelitis and amputation in diabetic foot infection. Diabetes Res Clin Pract. 2018;144:118-125.
[14] GUCLU M, FARUQ AGAN A. Association of severity of helicobacter pylori infection with peripheral blood neutrophil to lymphocyte ratio and mean platelet volume. Euroasian J Hepatogastroenterol. 2017;7(1):11-16.
[15] CELIK U, CELIK T, TOLUNAY O, et al. Platelet indices in the diagnosis of ventriculoperitoneal shunt infection in children. Turk Neurosurg. 2017;27(4):590-593.
[16] LEE MY, KIM YJ, LEE HJ, et al. Mean platelet volume in mycobacterium tuberculosis infection. Biomed Res Int. 2016;2016:7508763.
[17] KIM JK, JEON JS, KIM JW, et al. Correlation between abnormal platelet count and respiratory viral infection in patients from Cheonan, Korea. J Clin Lab Anal. 2016;30(3): 185-189.
[18] LEE IR, SHIN JI, PARK SJ, et al. Mean platelet volume in young children with urinary tract infection. Sci Rep. 2015;5: 18072.
[19] ZHANG W, GUO Y, KUSS M, et al. Platelet-rich plasma for the treatment of tissue infection: preparation and clinical evaluation. Tissue Eng Part B Rev. 2019;25(3):225-236.
[20] OSMON DR, BERBARI EF, BERENDT AR, et al. Diagnosis and management of prosthetic joint infection: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis. 2013;56(1):e1-e25.
[21] PARVIZI J, TAN TL, GOSWAMI K, et al. The 2018 Definition of periprosthetic hip and knee infection: an evidence-based and validated criteria. J Arthroplasty. 2018;33(5):1309-1314.e2.
[22] YOUDEN WJ. Index for rating diagnostic tests. Cancer. 1950;3(1):32-35.
[23] ADAMS JE, CAPO JT, RIZZO M. International consensus on periprosthetic joint infection. Acta Orthop Belg. 2014; 80(3):293-300.
[24] YOON JR, YANG SH, SHIN YS. Diagnostic accuracy of interleukin-6 and procalcitonin in patients with periprosthetic joint infection: a systematic review and meta-analysis. Int Orthop. 2018;42(6):1213-1226.
[25] XIE K, DAI K, QU X, et al. Serum and synovial fluid interleukin-6 for the diagnosis of periprosthetic joint infection. Sci Rep. 2017;7(1):1496.
[26] RANDAU TM, FRIEDRICH MJ, WIMMER MD, et al. Interleukin-6 in serum and in synovial fluid enhances the differentiation between periprosthetic joint infection and aseptic loosening. PLoS One. 2014;9(2):e89045.
[27] PANNU TS, VILLA JM, RIESGO AM, et al. Serum D-dimer in the diagnosis of periprosthetic knee infection: where are we today? J Knee Surg. 2020;33(2):106-110.
[28] XIONG L, LI S, DAI M. Comparison of D-dimer with CRP and ESR for diagnosis of periprosthetic joint infection. J Orthop Surg Res. 2019;14(1):240.
[29] QIN L, LI F, GONG X, et al. Combined measurement of D-dimer and C-reactive protein levels: highly accurate for diagnosing chronic periprosthetic joint infection. J Arthroplasty. 2020;35(1):229-234.
[30] SHAHI A, KHEIR MM, TARABICHI M, et al. Serum D-dimer test is promising for the diagnosis of periprosthetic joint infection and timing of reimplantation. J Bone Joint Surg Am. 2017;99(17):1419-1427.
[31] LEE YS, LEE YK, HAN SB, et al. Natural progress of D-dimer following total joint arthroplasty: a baseline for the diagnosis of the early postoperative infection. J Orthop Surg Res. 2018;13(1):36.
[32] DEIRMENGIAN C, KARDOS K, KILMARTIN P, et al. Diagnosing periprosthetic joint infection: has the era of the biomarker arrived?. Clin Orthop Relat Res. 2014;472(11): 3254-3262. [33] WYATT MC, BESWICK AD, KUNUTSOR SK, et al. The alpha-defensin immunoassay and leukocyte esterase colorimetric strip test for the diagnosis of periprosthetic infection: a systematic review and meta-analysis. J Bone Joint Surg Am. 2016;98(12):992-1000.
[34] DEIRMENGIAN C, KARDOS K, KILMARTIN P, et al. The alpha-defensin test for periprosthetic joint infection responds to a wide spectrum of organisms. Clin Orthop Relat Res. 2015;473(7):2229-2235.
[35] ZAGRA L, VILLA F, CAPPELLETTI L, et al. Can leucocyte esterase replace frozen sections in the intraoperative diagnosis of prosthetic hip infection? Bone Joint J. 2019; 101-B(4):372-377.
[36] GAUTAM VK, SAINI R, SHARMA S. Effectiveness of leucocyte esterase as a diagnostic test for acute septic arthritis. J Orthop Surg (Hong Kong). 2017;25(1): 2309499016685019.
[37] LI R, SHAO HY, HAO LB, et al. Plasma fibrinogen exhibits better performance than plasma d-dimer in the diagnosis of periprosthetic joint infection: a multicenter retrospective study. J Bone Joint Surg Am. 2019;101(7):613-619.
[38] CARLI AV, ABDELBARY H, AHMADZAI N, et al. Diagnostic accuracy of serum, synovial, and tissue testing for chronic periprosthetic joint infection after hip and knee replacements: a systematic review. J Bone Joint Surg Am. 2019;101(7):635-649.
[39] CHEN CY, ESSIEN MD, JOHNSON AJ, et al. Use of mean platelet volume in the assessment of intrauterine infection in newborns with combined thrombocytopenia and leukopenia at birth. J Matern Fetal Neonatal Med. 2019. doi:10.1080/14767058.2019.1608174.
[40] MURATOGLU M, KAYIPMAZ AE, KAVALCI C, et al. Platelet-to-lymphocyte ratio as a potential indicator of infection-associated emergency visits of renal transplant recipients. Exp Clin Transplant. 2019. doi:10.6002/ect.2018.0249.
[41] GUPTA P, GUDDATTU V, SARAVU K. Characterization of platelet count and platelet indices and their potential role to predict severity in malaria. Pathog Glob Health. 2019; 113(2):86-93.
[42] YUYUN D, ZHIHUA T, HAIJUN W, et al. Predictive value of the red blood cell distribution width-to-platelet ratio for hepatic fibrosis. Scand J Gastroenterol. 2019;54(1):81-86.
[43] RUBIO E, ALEJO-CANCHO I, AYLAGAS C, et al. Diagnostic value of platelet and leukocyte counts in the differential diagnosis of fever in the returning traveler. Am J Trop Med Hyg. 2019;100(2):470-475.
[44] ABDEL-RAZIK A, ELDARS W, RIZK E. Platelet indices and inflammatory markers as diagnostic predictors for ascitic fluid infection. Eur J Gastroenterol Hepatol. 2014;26(12): 1342-1347.
[45] KITAZAWA T, YOSHINO Y, TATSUNO K, et al. Changes in the mean platelet volume levels after bloodstream infection have prognostic value. Intern Med. 2013;52(13):1487-1493.
[46] COULDWELL G, MACHLUS KR. Modulation of megakaryopoiesis and platelet production during inflammation. Thromb Res. 2019;179:114-120. [47] SENINI V, AMARA U, PAUL M, et al. Porphyromonas gingivalis lipopolysaccharide activates platelet Cdc42 and promotes platelet spreading and thrombosis. J Periodontol. 2019;90(11):1336-1345. |
| [1] | Song Shan, Hu Fangyuan, Qiao Jun, Wang Jia, Zhang Shengxiao, Li Xiaofeng. An insight into biomarkers of osteoarthritis synovium based on bioinformatics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 785-790. |
| [2] | Ma Rui, Wang Jialin, Wu Mengjun, Ge Ying, Wang Wei, Wang Kunzheng. Relationship of pathogenic bacteria distribution with drug resistance and treatment cycle for periprosthetic joint infection after total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 380-385. |
| [3] | Wang Qiufei, Gu Ye, Peng Yuqin, Xue Feng, Ju Rong, Zhu Feng, Wang Yijun, Geng Dechun, Xu Yaozeng. Effect of Wnt/beta-catenin signaling pathway on osteoblasts under the action of wear particles [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3894-3901. |
| [4] | Cheng Chongjie, Yan Yan, Zhang Qidong, Guo Wanshou. Diagnostic value and accuracy of D-dimer in periprosthetic joint infection: a systematic review and meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(24): 3921-3928. |
| [5] | Liu Zhiwei, Xie Rui, Sun Kai, Li Kaiming, Wang Xiongwei, Zhan Jiawen, Zhu Liguo. Interpretation of diagnostic criteria for cervicogenic headache: challenges and understandings in diagnosis and differential diagnosis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3746-3751. |
| [6] | Jiang Shengyuan, Li Dan, Jiang Jianhao, Shang-you Yang, Yang Shuye. Biological response of Co2+ to preosteoblasts during aseptic loosening of the prosthesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(21): 3292-3299. |
| [7] | Chen Deng, Zhang Yaxin, Dai Jihang, Chen Duoyun, Sun Yu. Analysis on relative factors affecting pyrexia following total hip replacement [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2846-2850. |
| [8] | Liu Zige, Liu Xinrui, Li Yan, Song Guorui, Zhang Chen, Chen Desheng. In vitro experiment of tetrandrine on the model of osteolysis induced by wear particles around the prosthesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(15): 2358-2363. |
| [9] | Jia Wei, Zhang Mandong, Chen Weiyi, Wang Chenyan, Guo Yuan. Effects of femoral prosthetic materials on artificial knee arthroplasty performance [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(10): 1477-1481. |
| [10] | Zhou Qi, Gao Yi, Wei Kang, Li Jun, Xu Jianda, Jiang Yang, Qu Yuxing. Total knee arthroplasty for rheumatoid arthritis: knee function and biochemical index changes [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(9): 1337-1341. |
| [11] | Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao. Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 796-802. |
| [12] | Zhao Jianfeng, Geng Yu, Chen Qianbo, Yang Jinghui, Li Yan. Changes in insulin resistance and inflammatory factors in cataract patients with glaucoma after phacoemulsification and trabeculectomy: a self-controlled trial [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(11): 1750-1755. |
| [13] | Zhao Hongshun, A Jiancuo, Gao Shunhong, Li Yonggang, Guo Liping. Intraoperative and postoperative blood loss and levels of C-reactive protein and interleukin-6 after local application of tranexamic acid in total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 493-498. |
| [14] | Jian Changchun, Chen Yu, Chen Cheng, Hu Ning, Huang Wei. Anticoagulant effect of low-molecular-weight heparin versus rivaroxaban after arthroplasty assessed by thromboelastography [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 499-504. |
| [15] | Wu Xingyuan, Zhang Guoru, Liu Tang, Zhou Caisheng. Intravenous and intraarticular tranexamic acid can reduce blood loss and inflammatory response during cemented posterior cruciate ligament-retaining unilateral total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(36): 5753-5759. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||