Chinese Journal of Tissue Engineering Research ›› 2020, Vol. 24 ›› Issue (30): 4789-4794.doi: 10.3969/j.issn.2095-4344.2842
Previous Articles Next Articles
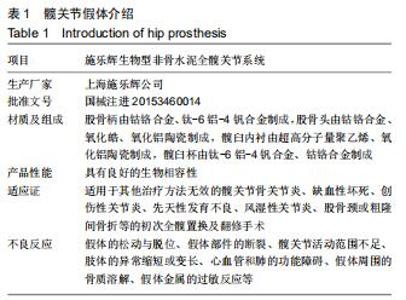
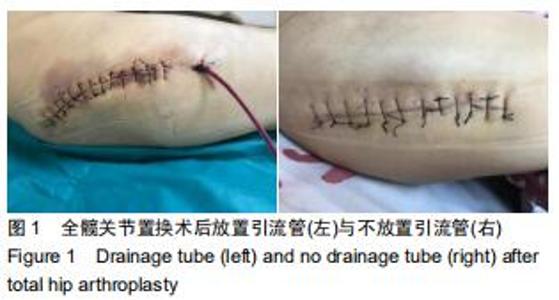
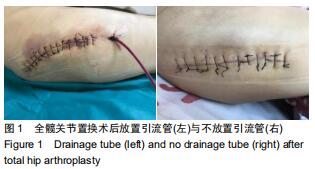
Comparison of placement or non-placement of drainage tube after intravenous drip of tranexamic acid in total hip arthroplasty
Wang Wangren, Shi Junjun, Huang Lingan, Zhang Zhiqiang
- Department of Orthopedics, Second Hospital of Shanxi Medical University, Taiyuan 030000, Shanxi Province, China
-
Received:2020-01-02Revised:2020-01-08Accepted:2020-03-07Online:2020-10-28Published:2020-09-18 -
Contact:Zhang Zhiqiang, Chief physician, Department of Orthopedics, Second Hospital of Shanxi Medical University, Taiyuan 030000, Shanxi Province, China -
About author:Wang Wangren, Master candidate, Physician, Department of Orthopedics, Second Hospital of Shanxi Medical University, Taiyuan 030000, Shanxi Province, China -
Supported by:the Youth Fund of National Natural Science Foundation of China, No. 31300802
CLC Number:
Cite this article
Wang Wangren, Shi Junjun, Huang Lingan, Zhang Zhiqiang. Comparison of placement or non-placement of drainage tube after intravenous drip of tranexamic acid in total hip arthroplasty[J]. Chinese Journal of Tissue Engineering Research, 2020, 24(30): 4789-4794.
share this article
|
[1] 王晖,张亚洲,时莉芳.骨小梁结构髋臼杯和实体结构髋臼杯的三维模型仿真分析[J].中国组织工程研究,2020,24(3):390-394.
[2] ZHANG WC, TANG N, LI XP, et al. The top 100 most cited articles on total hip arthroplasty: a bibliometric analysis.J Orthop Surg Res.2019; 14:412.
[3] BEHEIRY HE, LUBBERDINK A, CLEMENTS N, et al. Tranexamic dministration to older patients undergoing primary total hip arthroplasty conserves hemoglobin and reduces blood loss.Can J Surg. 2018;61(3): 177-184.
[4] GAO F, SUN W, GUO W, et al. Topical Application of Tranexamic acid Plus Diluted Epinephrine Reduces Postoperative Hidden Blood Loss in Total Hip Arthroplaty.J Arthroplaty.2015; 30(12):2196-2200.
[5] MIN JK, ZHANG QH, LI HD, et al. The Efficacy of Bipolar Sealer on Blood Loss in Primary Total Hip Arthroplasty: A Meta-Analysis. Medicine. 2016;95(19):e3435.
[6] ZHANG P, LIANG Y, CHEN P, et al. Combined application versus topical and intravenous application of tranexamic acid following primary total hip arthroplasty :a meta-analysis.BMC Musculoskelet Disord.2017;18(1):90.
[7] GEORGIADIS AG, MUH SJ, SILVERTON CD, et al. A Prospective Double-Blind Placebo Controlled Trial of Topical Tranexamic Acid in Total Knee Arthroplasty.J Arthroplasty.2013;28(8):78-82.
[8] LEE SH, CHO KY, KHURANA S, et al. Less blood loss under concomitant administration of topic tranexamic acid and indirect factor Xa inhibitor following total knee arthroplasty: a prospective randomized controlled trail.Knee Surg Sports Traumatol Arthrosc. 2013;11(24): 2611-2617.
[9] BIERBAUM BE, CALLAGHAN JJ, GALANTE JO, et al. Analysis of blood management in patients having a total hip or knee arthroplasty.J Bone Joint Surg Am.1999;81(1):2-10.
[10] WANG Z, ZHANG HJ. Comparative effectiveness and safety of tranexamic acid plus diluted epinephrine to control blood loss during total hip arthroplasty: a meta-analysis.J Orthop Surg Res. 2018;13(1):242.
[11] RAY S, GUPTA RK, JAIN D. Transfusion-Related Acute Lung Injury due to Iatrogenic IVIG Overdose in Guillain-Barre Syndrome.J Pediatr Neurosci.2019;14(3):140-142.
[12] MADJDPOUR C. Allogeneic red blood cell transfusions: efficacy, risks, alternatives and indications.Br J Anaesth.2005;95(1):33-42.
[13] DUNN CJ, GOA KL. Tranexamic acid: A review of its use in surgery and other indications. Drugs.1999;57(6):1005-1032.
[14] ORTMANN E, BESSER MW, KLEIN AA. Antifibrinolytic agents in current anaesthetic practice. Br J Anaesth.2013;111(4):549-563.
[15] 张少云,肖聪,裴福兴.氨甲环酸在创伤骨科手术中应用的研究进展[J].中国修复重建外科杂志,2019,33(11):1-5.
[16] CHEN X, ZHENG F, ZHENG Z, et al. Oral vs intravenous tranexamic acid in total-knee arthroplasty and total hip arthroplasty: A systematic review and meta-analysis.Medicine.2019;98(20):e15248.
[17] SUN X, DONG Q, ZHANG YG. Intravenous versus topical tranexamic acid in primary total hip replacement: A systemic review and meta-analysis.Medicine.2016;95(50):10-18.
[18] BAI JZ, HANG P, LIANG Y, et al. Efficacy and safety of tranexamic acid usage in patients undergoing posterior lumbar fusion: a meta-analysis. BMC Musculoskelet Disord. 2019; 20: 390. [19] YAO RZ, GAO WQ, WANG BW, et al. Efficacy and Safety of Tranexamic Acid in Reducing Blood Loss of Lower Extremity Osteotomy in Peri-acetabulum and High Tibia: A Systematic Review and Meta-analysis.Orthop Surg.2019;11(4):545-551.
[20] KUO FC, LIN PY, WANG JW, et al.Intravenous tranexamic acid reduces blood transfusions in revision total hip arthroplasty: a meta-analysis. Drug Des Devel Ther.2018;12:3163-3170.
[21] 李金堂,李叔强,王兴,等.Ⅰ期全髋置换治疗严重髋关节骨性关节炎伴股骨近端骨折[J].中国骨伤,2019,32(5):412-417.
[22] MALIK AT, ALEXANDER JH, LI DD, et al. What Are the Costs of Hip Osteoarthritis in the Year Prior to a Total Hip Arthroplasty. J Arthroplasty. 2019;19(19):30869-308871.
[23] GEORGIOS T, MAZIAR M, PETER C, et al. Head size in primary total hip arthroplasty. EFORT Open Rev.2018;3(5):225-231.
[24] UGBEYE ME, LAWAL WO, AYODABO OJ, et al.An Evaluation of Intra‑ and Post‑operative Blood Loss in Total Hip Arthroplasty at the National Orthopaedic Hospital,Lagos.Niger J Surg.2017; 23(1):42-46.
[25] 闵令田,翁文杰,王渭君,等.微创全髋关节置换术疗效的系统评价[J].中国骨与关节损伤杂志,2014, 29(2):117-120.
[26] QIU J, SUN X, ZHANG W, et al. Effect of topical tranexamic acid in total hip arthroplasty patients who receive continuous aspirin for prevention of cardiovascular or cerebrovascular events: A Prospective Randomized Study.Orthop Traumatol Surg Res. 2019;27(19): 30253-30261.
[27] 尹勇,马广文,黄斐,等.氨甲环酸减少全髋关节置换失血量的Meta分析[J].中国组织工程研究, 2014,18(17):134-139.
[28] RAJA A, MANZOOR H, JAN WM, et al. Comparison between closed suction drainage and no drainage following total knee arthroplasty in a tertiary care setting in pakistan.Cureus. 2016;8(10):e842.
[29] ERNE F, WETZEL S, WULKER N, et al. Closed suction drainage after primary total knee arthroplasty:a prospective randomized trial.J Knee Surg.2018;31(8):804-810.
[30] ESLER CN ,BLAKEWAY C, FIDDIAN NF. The use of a closed-suction drain in total knee arthroplasty.J Bone Joint Surg Br. 2003;85(2):215-217.
[31] XU H, XIE J, LEI Y, et al. Closed suction drainage following routine primary total joint arthroplasty is associated with a higher transfusion rate and longer postoperative length of stay: a retrospective cohort study.J Orthop Surg Res.2019;14(1):163.
[32] AGENO W, MANTOVANI LG, HAAS S, et al. Patient Management Strategies and Long-Term Outcomes in Isolated Distal Deep-Vein Thrombosis versus Proximal Deep-Vein Thrombosis: Findings from XALIA. TH Open.2019;3(1):e85-e93.
[33] 刘剑伟,蒋卫平.髋关节置换围手术期深静脉血栓的防治[J].中国组织工程研究,2017,21(31):4927-4932.
[34] SUKEIK M, ALSHRYDA S, POWELL J, et al. The effect of tranexamic acid on wound complications in primary total Hip Arthroplasty: A meta-analysis.Surgeon.2019;10(19):30090-30093.
[35] GULABI D, YUCE Y, ERKAL KH, et al. The combined administration of systemic and topical tranexamic acid for total hip arthroplasty: Is it better than systemic? Acta Orthop Traumatol Turc.2019;53(4): 297-300.
[36] 荆鑫,腾红林,吴海山,等.全关节置换术后关节腔引流问题的探讨[J].中国矫形外科杂志,2002,10(13):1295-1297.
[37] KREMERS K, LEIJTENS B, CAMPS S, et al. Evaluation of early wound leakage as a risk factor for prosthetic joint infection.J Am Assoc Nurse Pract.2019;31(6):337-343.
[38] WILLETT KM, SIMMONS CD, BENTLEY G. The effect of suction drains fol-lowing total hip arthroplasty.J Bone Joint Surg.1988;70: 607-610.
[39] 王浩洋,康鹏德,裴福兴,等.氨甲环酸减少全髋关节置换术围手术期失血的有效性及安全性研究[J].中华骨与关节外科杂志, 2015,8(2):649-654.
[40] 杨伟民,李斯明.加速康复外科理念在髋膝关节置换术围术期的应用研究[J].中华骨与关节外科杂志,2018,11(3):182-185.
[41] DE ANDRADE MA, DE OLIVEIRA CAMPOS TV, SILVA BF, et al. Six month follow-up of patients submitted to total knee arthroplasty with and without placement of suction drainage devices.Rev Bras Ortop. 2015;45(6):549-553. [42] WANG D, XU J, ZENG WN, et al. Closed suction drainage is not associated with faster recovery after total knee arthroplasty: a prospective randomized controlled study of 80 patients. Orthop Surg. 2016;8(2):226-233. |
| [1] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [2] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [3] | Xu Feng, Kang Hui, Wei Tanjun, Xi Jintao. Biomechanical analysis of different fixation methods of pedicle screws for thoracolumbar fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1313-1317. |
| [4] | Jiang Yong, Luo Yi, Ding Yongli, Zhou Yong, Min Li, Tang Fan, Zhang Wenli, Duan Hong, Tu Chongqi. Von Mises stress on the influence of pelvic stability by precise sacral resection and clinical validation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1318-1323. |
| [5] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [6] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [7] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [8] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [9] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [10] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [11] | Peng Zhihao, Feng Zongquan, Zou Yonggen, Niu Guoqing, Wu Feng. Relationship of lower limb force line and the progression of lateral compartment arthritis after unicompartmental knee arthroplasty with mobile bearing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1368-1374. |
| [12] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [13] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [14] | Wang Haiying, Lü Bing, Li Hui, Wang Shunyi. Posterior lumbar interbody fusion for degenerative lumbar spondylolisthesis: prediction of functional prognosis of patients based on spinopelvic parameters [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1393-1397. |
| [15] | Lü Zhen, Bai Jinzhu. A prospective study on the application of staged lumbar motion chain rehabilitation based on McKenzie’s technique after lumbar percutaneous transforaminal endoscopic discectomy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1398-1403. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||