Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (17): 2678-2683.doi: 10.3969/j.issn.2095-4344.1719
Previous Articles Next Articles
Bone repair using skeletal muscle stem cells combined with platelet-rich plasma
Yin Nuo, Xue Feng, Xiao Haijun, Ding Liang, Yuan Junjie, Pan Mingmang, Yu Du, Ju Jinyong, Zhu Longzhang
- Shanghai Fengxian District Central Hospital (South Campus, Sixth People’s Hospital Affiliated to Shanghai Jiao Tong University), Shanghai 201499, China
-
Revised:2019-02-17Online:2019-06-18Published:2019-06-18 -
Contact:Zhu Longzhang, Master, Associate chief physician, Shanghai Fengxian District Central Hospital (South Campus, Sixth People’s Hospital Affiliated to Shanghai Jiao Tong University), Shanghai 201499, China -
About author:Yin Nuo, Master, Attending physician, Shanghai Fengxian District Central Hospital (South Campus, Sixth People’s Hospital Affiliated to Shanghai Jiao Tong University), Shanghai 201499, China -
Supported by:Shanghai Key Medical Specialist Construction Project, No. ZK2015B06 (to XF); a grant from Shanghai Fengxian District Science and Technology Commission, Fengweike2010-01 (to YN); and the Seed Fund of Shanghai University of Medicine & Health Sciences, No. HMSF-17-21-025 (to YN)
CLC Number:
Cite this article
Yin Nuo, Xue Feng, Xiao Haijun, Ding Liang, Yuan Junjie, Pan Mingmang, Yu Du, Ju Jinyong, Zhu Longzhang. Bone repair using skeletal muscle stem cells combined with platelet-rich plasma[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(17): 2678-2683.
share this article
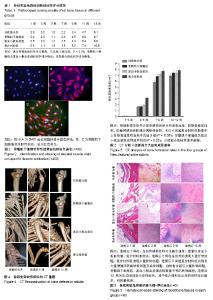
2.1 骨骼肌干细胞形态及鉴定结果 从兔比目鱼肌中分离出来的骨骼肌干细胞初始为散在有较强折光性的圆形细胞;在培养基中培养12 h开始观察到细胞贴壁,其后细胞逐渐开始增殖。经流式细胞仪检测鉴定:兔细胞特异性结蛋白抗原染色呈阳性,荧光显微镜下可见细胞胞浆发出红色荧光,流式细胞仪检测染色阳性率达到98.36%,见图2。 2.2 实验动物数量分析 纳入新西兰大白兔数量28只,分4组,全部纳入结果统计分析,无脱失。 2.3 实验动物一般情况 术后9 d拆线,所有新西兰大白兔手术切口愈合良好,无炎症反应表现。术后活动情况、饮食量、精神状况、二便均无异常。 2.4 影像学检查 术后当天及术后每周进行CT检查,观察骨愈合情况。术后当天CT影像学测量缺损横向直径R0,纵向直径r0,术后第1周分别为R1,r1,术后第2周分别为R2,r2,以此类推。术后4周起复合材料组影像学上骨修复速度明显高于其他3组(P < 0.05)。骨骼肌干细胞组、富血小板血浆组影像学上骨修复速度明显高于自然愈合组(P < 0.05),见图3,4。 2.5 组织学检查结果 术后1,3,5,7,9,11,13周每组各取1只实验兔骨缺损处骨组织进行组织学染色。骨标本苏木精-伊红染色后,采用Lane-Sandhu组织学评分法进行评分比较,见表1。复合材料组成骨能力最强,骨骼肌干细胞组和富血小板血浆组成骨能力无明显差异,自然愈合组成骨能力最弱,见图5。"
| [1] Luo CQ, Fang Y, Tu CQ, et al. Current treatment situation and progress on bone defect of collapsed tibial plateau fractures. Zhongguo Gu Shang. 2016;29(2):187-191.[2] Tall M. Treatment of aseptic tibial shaft non-union without bone defect. Orthop Traumatol Surg Res. 2018;104(1S): S63-S69. [3] Brinker MR, O'Connor DP. Management of Aseptic Tibial and Femoral Diaphyseal Nonunions Without Bony Defects. Orthop Clin North Am. 2016;47(1):67-75.[4] Tang D, Tare RS, Yang LY, et al. Biofabrication of bone tissue: approaches, challenges and translation for bone regeneration. Biomaterials. 2016;83:363-382.[5] Black CR, Goriainov V, Gibbs D, et al. Bone Tissue Engineering. Curr Mol Biol Rep. 2015;1(3):132-140.[6] 单连成,王刚,张长青,等.富血小板血浆对体外培养骨骼肌干细胞增殖及成骨活性的作用[J].中国组织工程研究与临床康复, 2009, 13(20):3833-3837.[7] Qu Z, Balkir L, van Deutekom JC, et al. Development of approaches to improve cell survival in myoblast transfer therapy. J Cell Biol. 1998;142(5): 1257-1267. [8] 单连成,王刚,张长青,等.不同浓度PRP对骨骼肌干细胞成骨分化的影响[J],中国修复重建外科杂志,2009,23(8):991-996.[9] Lane JM, Sandhu HS. Current approaches to experimental bone grafting. Orthop Clin North Am. 1987;18(2):213-225.[10] Pobloth AM, Schell H, Petersen A, et al. Tubular open-porous β-tricalcium phosphate polycaprolactone scaffolds as guiding structure for segmental bone defect regeneration in a novel sheep model. J Tissue Eng Regen Med. 2018;12(4):897-911.[11] Decambron A, Manassero M, Bensidhoum M, et al. A comparative study of tissue-engineered constructs from Acropora and Porites coral in a large animal bone defect model. Bone Joint Res. 2017;6(4):208-215.[12] Parizi AM, Oryan A, Shafiei-Sarvestani Z, et al. Effectiveness of synthetic hydroxyapatite versus Persian Gulf coral in an animal model of long bone defect reconstruction. J Orthop Traumatol. 2013;14(4):259-268.[13] Martinez SA, Probst CW, Hauptman JG, et al. Effects of a fixed compression load on the osteogenic effect of autogenous cancellous bone grafts in dogs. Am J Vet Res. 1992;53(12):2381-2385.[14] Turner TM, Urban RM, Hall DJ, et al. Restoration of large bone defects using a hard-setting, injectable putty containing demineralized bone particles compared to cancellous autograft bone. Orthopedics. 2003;26(5 Suppl):s561-565.[15] Nuss KM, Auer JA, Boos A, et al. An animal model in sheep for biocompatibility testing of biomaterials in cancellous bones. BMC Musculoskelet Disord. 2006;7:67.[16] Pobloth AM, Johnson KA, Schell H, et al. Establishment of a preclinical ovine screening model for the investigation of bone tissue engineering strategies in cancellous and cortical bone defects. BMC Musculoskelet Disord. 2016;17:111.[17] Prat S, Gallardo-Villares S, Vives M, et al. Clinical translation of a mesenchymal stromal cell-based therapy developed in a large animal model and two case studies of the treatment of atrophic pseudoarthrosis. J Tissue Eng Regen Med. 2018; 12(1): e532-e540.[18] Qian W, Gong L, Cui X, et al. Nanotopographic Regulation of Human Mesenchymal Stem Cell Osteogenesis. ACS Appl Mater Interfaces. 2017;9(48):41794-41806.[19] Fan X, Li L, Ye Z, et al. Regulation of osteogenesis of human amniotic mesenchymal stem cells by sodium butyrate. Cell Biol Int. 2018;42(4):457-469.[20] Bilem I, Plawinski L, Chevallier P, et al. The spatial patterning of RGD and BMP-2 mimetic peptides at the subcellular scale modulates human mesenchymal stem cells osteogenesis. J Biomed Mater Res A. 2018;106(4):959-970.[21] Heo JS, Lee SG, Kim HO. Distal-less homeobox 5 is a master regulator of the osteogenesis of human mesenchymal stem cells. Int J Mol Med. 2017;40(5):1486-1494.[22] Tohidnezhad M, Varoga D, Wruck CJ, et al. Platelets display potent antimicrobial activity and release human beta-defensin 2. Platelets. 2012;23(3):217-223.[23] Khojasteh A, Behnia H, Dashti SG, et al. Current trends in mesenchymal stem cell application in bone augmentation: a review of the literature. J Oral Maxillofac Surg. 2012;70(4): 972-982.[24] Li S, Huang KJ, Wu JC, et al. Peripheral blood-derived mesenchymal stem cells: candidate cells responsible for healing critical-sized calvarial bone defects. Stem Cells Transl Med. 2015;4(4):359-368.[25] New SE, Alvarez-Gonzalez C, Vagaska B, et al. A matter of identity - Phenotype and differentiation potential of human somatic stem cells. Stem Cell Res. 2015;15(1):1-13.[26] Morcos MW, Al-Jallad H, Hamdy R. Comprehensive Review of Adipose Stem Cells and Their Implication in Distraction Osteogenesis and Bone Regeneration. Biomed Res Int. 2015; 2015:842975.[27] Arrighi N, Moratal C, Clément N, et al. Characterization of adipocytes derived from fibro/adipogenic progenitors resident in human skeletal muscle. Cell Death Dis. 2015;6:e1733.[28] Liu R, Birke O, Morse A, et al. Myogenic progenitors contribute to open but not closed fracture repair. BMC Musculoskelet Disord. 2011;12:288.[29] Cairns DM, Liu R, Sen M, et al. Interplay of Nkx3.2, Sox9 and Pax3 regulates chondrogenic differentiation of muscle progenitor cells. PLoS One. 2012;7(7):e39642.[30] Mifune Y, Matsumoto T, Takayama K, et al. The effect of platelet-rich plasma on the regenerative therapy of muscle derived stem cells for articular cartilage repair. Osteoarthritis Cartilage. 2013;21(1):175-185.[31] Samuel S, Ahmad RE, Ramasamy TS, et al. Platelet rich concentrate enhances mesenchymal stem cells capacity to repair focal cartilage injury in rabbits. Injury. 2018;49(4): 775-783. |
| [1] | Jiang Tao, Ma Lei, Li Zhiqiang, Shou Xi, Duan Mingjun, Wu Shuo, Ma Chuang, Wei Qin. Platelet-derived growth factor BB induces bone marrow mesenchymal stem cells to differentiate into vascular endothelial cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3937-3942. |
| [2] | Chen Yang, Huang Denggao, Gao Yuanhui, Wang Shunlan, Cao Hui, Zheng Linlin, He Haowei, Luo Siqin, Xiao Jingchuan, Zhang Yingai, Zhang Shufang. Low-intensity pulsed ultrasound promotes the proliferation and adhesion of human adipose-derived mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3949-3955. |
| [3] | Zhang Lishu, Liu Anqi, He Xiaoning, Jin Yan, Li Bei, Jin Fang. Alpl gene affects the therapeutic effect of bone marrow mesenchymal stem cells on ulcerative colitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3970-3975. |
| [4] | Ruan Guangping, Yao Xiang, Liu-Gao Miyang, Cai Xuemin, Li Zian, Pang Rongqing, Wang Jinxiang, Pan Xinghua. Umbilical cord mesenchymal stem cell transplantation for traumatic systemic inflammatory response syndrome in tree shrews [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3994-4000. |
| [5] | Chen Lei, Zheng Rui, Jie Yongsheng, Qi Hui, Sun Lei, Shu Xiong. In vitro evaluation of adipose-derived stromal vascular fraction combined with osteochondral integrated scaffold [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(22): 3487-3492. |
| [6] | Wei Qin, Zhang Xue, Ma Lei, Li Zhiqiang, Shou Xi, Duan Mingjun, Wu Shuo, Jia Qiyu, Ma Chuang. Platelet-derived growth factor-BB induces the differentiation of rat bone marrow mesenchymal stem cells into osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 2953-2957. |
| [7] | Guo Zhibin, Wu Chunfang, Liu Zihong, Zhang Yuying, Chi Bojing, Wang Bao, Ma Chao, Zhang Guobin, Tian Faming. Simvastatin stimulates osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 2963-2968. |
| [8] | Li Congcong, Yao Nan, Huang Dane, Song Min, Peng Sha, Li Anan, Lu Chao, Liu Wengang. Identification and chondrogenic differentiation of human infrapatellar fat pad derived stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 2976-2981. |
| [9] | Gao Yuanhui, Xiang Yang, Cao Hui, Wang Shunlan, Zheng Linlin, He Haowei, Zhang Yingai, Zhang Shufang, Huang Denggao. Comparison of biological characteristics of adipose derived mesenchymal stem cells in Wuzhishan inbreed miniature pigs aged two different months [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 2988-2993. |
| [10] | Cao Yang, Zhang Junping, Peng Li, Ding Yi, Li Guanghui. Isolation and culture of rabbit aortic endothelial cells and biological characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3000-3003. |
| [11] | Dai Min, Wang Shuai, Zhang Nini, Huang Guilin, Yu Limei, Hu Xiaohua, Yi Jie, Yao Li, Zhang Ligang. Biological characteristics of hypoxic preconditioned human amniotic mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3004-3008. |
| [12] | Qin Yanchun, Rong Zhen, Jiang Ruiyuan, Fu Bin, Hong Xiaohua, Mo Chunmei. Chinese medicine compound preparation inhibits proliferation of CD133+ liver cancer stem cells and the expression of stemness transcription factors [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3016-3023. |
| [13] | Dai Yaling, Chen Lewen, He Xiaojun, Lin Huawei, Jia Weiwei, Chen Lidian, Tao Jing, Liu Weilin. Construction of miR-146b overexpression lentiviral vector and the effect on the proliferation of hippocampal neural stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3024-3030. |
| [14] | Chen Jie, Liao Chengcheng, Chen Zhiwei, Wang Yan. Bladder cancer stem cell markers and related signaling pathways: antibody targeted therapy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3090-3096. |
| [15] | Zhang Wei, Cui Shuaishuai, Zhou Zhichao, Hu Xiaohua, Yang Xiaohong. MicroRNA regulates histone deacetylase in the treatment of bone-related diseases [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(17): 2767-2774. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||