Chinese Journal of Tissue Engineering Research ›› 2021, Vol. 25 ›› Issue (14): 2287-2296.doi: 10.3969/j.issn.2095-4344.3132
Gait training for spinal cord injury based on radar plotting: an overview of systematic reviews
Wu Cunshu1, Zhan Xiaoxuan1, Zhao Siyi2, Huang Fan2, Zhang Yue1, Qiu Mingwang1, Xia Jingxian1, Lu Xiaobo3#br#
- 1Acupuncture and Rehabilitation School of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China; 2The Second Clinical School of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China; 3Department of Rehabilitation, Jieyang Hospital of Traditional Chinese Medicine, Jieyang 522000, Guangdong Province, China
-
Received:2020-05-25Revised:2020-05-26Accepted:2020-08-19Online:2021-05-18Published:2020-12-31 -
Contact:Lu Xiaobo, Department of Rehabilitation, Jieyang Hospital of Traditional Chinese Medicine, Jieyang 522000, Guangdong Province, China -
About author:Wu Cunshu, Acupuncture and Rehabilitation School of Guangzhou University of Chinese Medicine, Guangzhou 510006, Guangdong Province, China -
Supported by:the National College Student Innovation and Entrepreneurship Training Project in 2019, No. 201910572001 (to ZSY)
CLC Number:
Cite this article
Wu Cunshu, Zhan Xiaoxuan, Zhao Siyi, Huang Fan, Zhang Yue, Qiu Mingwang, Xia Jingxian, Lu Xiaobo. Gait training for spinal cord injury based on radar plotting: an overview of systematic reviews[J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2287-2296.
share this article
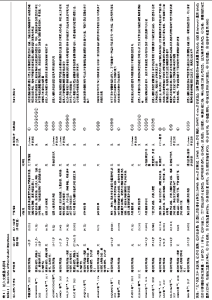
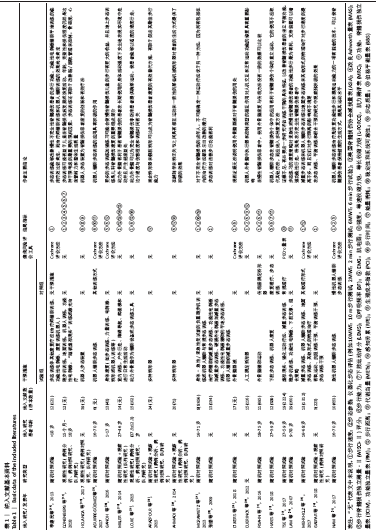
2.2 纳入文献基本特征 文章最终共纳入20篇文献[18-37],均已在国内外期刊上发表。文献发表的年份在2009至2018年,其中纳入文献题名标注为“A Systematic Review”的有14篇[19-20,22,24,27,29-37],为“A System Review and Meta-analysis”的有2篇[21,23],为“Meta分析”的有2篇[18,28],“Review”的有2篇[25-26]。纳入的文献中,有2篇所属国家为中国[18, 28],有4篇所属国家为美国[19,23,29-31],有4篇所属国家为加拿大[22,26,33-34],有2篇所属国家为巴西[20,36],有2篇所属国家为伊朗[24-25],有2篇所属国家为英国[27,32],另外有4篇分别属于墨西哥、加拿大、德国和韩国[21,28,35,37],有16篇文献没有具体的实验组与对照组[18-27,28-30,34-36],但都是以研究步态训练的有效性为前提,使用机器人辅助或其他康复机器辅助训练,有1篇以外骨骼辅助运动作为试验组对比传统膝踝足矫形器的疗效[31],有1篇以下肢步态训练、机器人康复作为试验组对比康复理疗和步态训练的疗效[32],有1篇以虚拟现实、强化运动疗法、BWS训练、BWST训练作为试验组对比常规理疗的疗效[33],有1篇以急性RAGT疗法作为试验组对比慢性RAGT疗法的疗效[37];在对纳入随机对照试验偏倚风险评价中,其中有6篇采用Cochrane系统评价员手册推荐的偏倚风险评估工具[18,21-22,25,29, 37],有1篇使用PEDro量表作为偏倚风险评价工具[33],有7篇没有采用采用量表评价偏倚风险[19-20,23-27]。 结局指标总结:①主要结局指标:有12篇报道了步行速度[18-19,23-24,27-31,35-37],有10篇文献报道了步态参数-仪表化步态评估[19-22,24,26,29-32];②次要结局指标:有5篇报道了步行能力[19,27,30-31,37],有5篇报道了步行距离[22-24, 30,35],有4篇报道了脊髓损伤的步行独立性测量[19,22,32,37],有4篇报道了脊髓损伤独立量表(SCIM)功能评分、功能独立量表(FIM)评分[21,31-32,34],有2篇报道了下肢运动评分[19,32],有2篇报道了肌电图[19,29],有2篇报道了步行时间[24,27],有2篇报道了步行能量消耗情况[25-26]。 纳入研究的基本特征见表1。 "
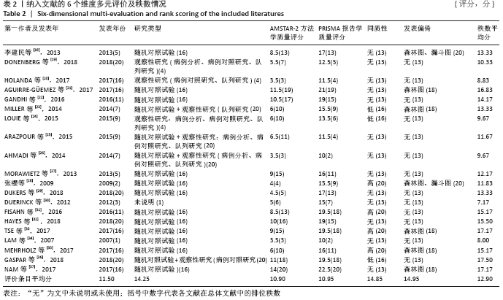
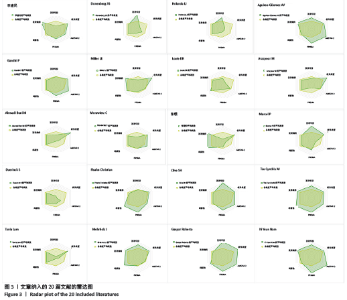
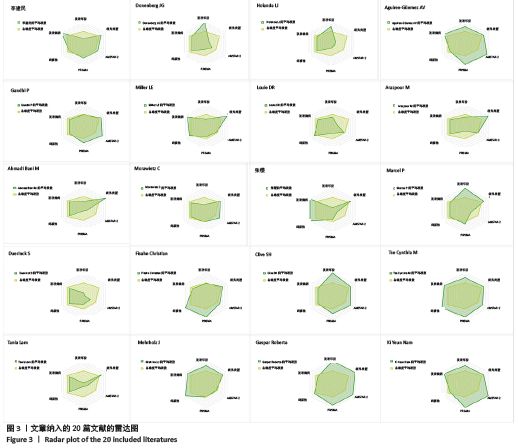
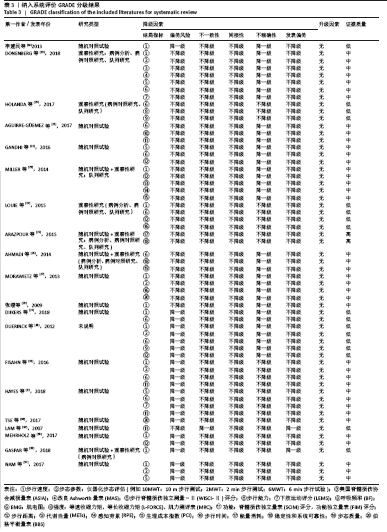
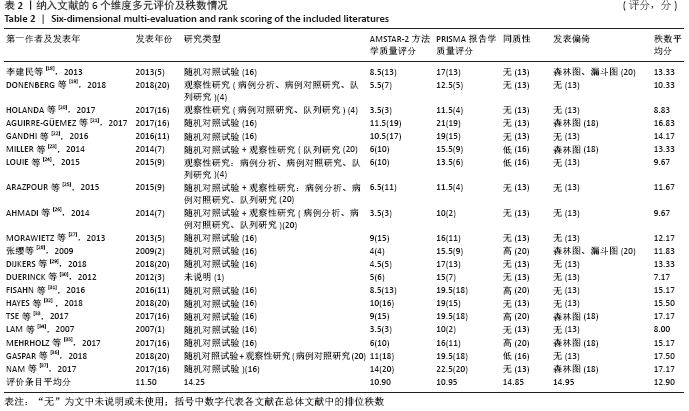
2.3 发表年份比较 每1篇文献所研究的问题对临床的指导意义的强度与研究文献年份、涵盖范围和时间跨度有关。研究越新及时间跨度越大,对临床的指导意义越强。文章纳入20篇系统评价/Meta分析,故将2018年发表文献秩数定为20,在系统评价/Meta分析文献中,出版时间较新最早为2007年,包含1篇[34];最晚为2018年,包含4篇[19,29,32,36];期间2017年5篇[20-21,33,35,37],2016年2篇[22,31],2015年2篇[24-25],2014年2篇[23,26],2013年2篇[18,27],2012年1篇[30],2009年1篇[28]。 2.4 研究类型比较 评价某项治疗的有效性的最高级别临床证据是临床的随机对照试验(随机对照试验)。此次研究发现,多数文献仅纳入随机对照试验,共有12篇[18,21-22,27-29,31-36],另外,有4篇文献纳入了随机对照试验和不同程度的观察性研究(包括病例分析、病例对照研究和队列研究)[23,25-26,36],有3篇仅纳入了不同程度观察性研究(包括病例分析、病例对照研究、队列研究)[19-20,24],有1篇文献未说明研究类型[30]。 2.5 AMSTAR-2评价结果 AMSTAR-2方法学评分量表共16项条目。有20篇文献的分值区间为3.5-14分。其中评价为3.5分的文章为3篇[20,26,34],4分的有1篇[28],4.5分的有1篇[29],5分的有1篇[30],5.5分的有1篇[19],6分的有3篇[23-24,35],6.5分的有1篇[25],8.5分的有一篇[31],9分的有3 篇[18,27,33],10分的有1篇[32],10.5分的有1篇[22],11分的有1篇[36],11.5分的有1篇[21],14分的有1篇[37],总体总分分值偏低。其中评价AMSTAR-2评价结果根据结果效度关键的7个条目,分别为条目2,4,7,9,11,13和15,分为高、中、低、极低4个等级,有18篇文献均为极低,只有2篇为低[21,37]。主要存在的问题:①在第2项(是否声明在系统评价实施前已经确定了系统评价的研究方法?对于与研究方案不一致处是否进行说明?)中,仅4篇研究为 “是”[33,35-37],仅1篇为部分“是”[27],其他均为“否”;②在第4项(系统评价作者是否采用了全面的检索策略?)中,仅4篇研究[27,33,36-37]为“是”,5篇研究为“否”[25-26,29,34-35],其他为部分“是”;③在第9项(系统评价作者是否采用合适工具评估每个纳入研究的偏倚风险?)中,仅5篇研究为“ “是”[18,29,33,35,37],仅3篇研究为部分“是”[21-22,32],其他均为“否”;④在第11项(作Meta分析时,系统评价作者是否采用了合适的统计方法合并研究结果?)中,7篇研究为“是”[21-24,28,36-37],其他均为“否”;⑤在第13项(系统评价作者解释或讨论每个研究结果时是否考虑纳入研究的偏倚风险?)中,仅5篇研究为“是”[21-22,27,31-32,37],其他均为“否”;⑥在第15项(如果系统评价作者进行定量合并,是否对发表偏倚(小样文章偏倚)进行充分的调查,并讨论其对结果可能的影响?)中,仅3篇研究为“是”[18,21,28],其他均为“否”。 2.6 PRISMA评价结果比较 PRISMA满分为27分,20篇文献分值为10-22.5分[18-37]。文献分值偏低的因素有:①有18篇文章均没有提供注册号[18-28,30-32,34-37];②除了2篇研究[29,33],其他纳入文献的摘要信息不充分;③除7篇研究[21-22,28, 30,33-34,37]外,其他文献没有评估可能影响数据综合结果的可能存在的偏倚;④除2篇研究外[28,31],其他纳入文献没有其他分析方法;⑤除了6篇研究[21-22,24,28,33,37],其他均没有报告研究间的偏倚;⑥除7篇研究使用了漏斗图或森林图进行分析[18,21,23,28,33,35,37],其他均未使用漏斗图或者森林图分析结果;⑦除9篇研究外[18,21-22,29,31-33,36-37],其他文献均没有报告研究内部偏倚。 2.7 雷达图多元评价条目 见表2。"
| [1] 曾红,周谋望.脊髓损伤生物标记物的研究进展[J].中国康复医学杂志,2018, 33(10):1226-1230. [2] WYNDAELE M, WYNDAELE JJ. Incidence, prevalence and epidemiolo-gy of spinal cord injury: what learns a worldwide literature survey. Spinal Cord. 2006;44(9):523-529. [3] QIU J. China spinal cord injury network: changes from within. Lancet Neurol. 2009; 8(7):606-607. [4] CHISHOLM AE, QAISER T, WILLIAMS AMM, et al. Acquisition of a precision walking skill and the impact of proprioceptive deficits in people with motor-incomplete spinal cord injury. J Neurophysiol. 2019; 121(3): 1078-1084. [5] ANGELI CA, BOAKYE M, MORTON RA, et al. Recovery of over-ground walking after chronic motor complete spinal cord injury. N Engl J Med. 2018;379(13):1244-1250. [6] 康海琼,周红俊,刘根林,等.脊髓损伤神经学分类国际标准检查表2019版最新修订及解读[J].中国康复理论与实践, 2019,25(8):983-985. [7] 王寒明,王欢,郄淑燕,等.早期综合康复疗法对脊髓损伤患者的康复效果[J].中国临床研究,2019,32(1):89-92. [8] YILDIRIM MA, ÖNEŞ K, GÖKŞENOĞLU G. Early term effects of robotic assisted gait training on ambulation and functional capacity in patients with spinal cord injury. Turk J Med Sci. 2019;49(3):838-843. [9] FIELD-FOTE EC, LINDLEY SD, SHERMAN AL. Locomotor training approaches for individuals with spinal cord injury: a preliminary report of walking-related outcomes. J Neurol Phys Ther. 2005;29(3):127-137. [10] NEVILLE BT, MURRAY D, ROSEN KB, et al. Effects of performance-based training on gait and balance in individuals with incomplete spinal cord injury. Arch Phys Med Rehabil. 2019;100(10):1888-1893. [11] 郭素梅,李建民,吴庆文,等.步态训练机器人对不完全性脊髓损伤患者步态的影响[J].中国康复理论与实践,2013,19(7):676-679. [12] ILHA J, MEIRELES A, DE FREITAS GR, et al. Overground gait training promotes functional recovery and cortical neuroplasticity in an incomplete spinal cord injury model. Life Sci. 2019;232:116627. [13] 董悦颖.meta分析方法学质量与报告质量评价的主要问题[J].中国卫生统计, 2017,34(6):1006-1008. [14] MOHER D, LIBERATI A, TETZLAFF J,等.The PRISMA Group.系统综述和荟萃分析优先报告的条目:PRISMA声明[J].中西医结合学报,2009,7(9):889-896. [15] 张方圆,沈傲梅,曾宪涛,等.系统评价方法学质量评价工具AMSTAR 2解读[J]. 中国循证心血管医学杂志,2018,10(1):14-18. [16] PANESAR SS, RAO C, VECHT JA, et al. Development of the Veritas plot and its application in cardiac surgery: an evidence-synthesis graphic tool for the clinician to assess multiple meta-analyses reporting on a common outcome. Can J Surg. 2009; 52(5):E137-E145. [17] 王晓彤,林海雄,陈贵珍.基于雷达图多元评价针灸治疗中风后抑郁系统评价/Meta分析文献质量[J].中国中医基础医学杂志,2018,24(4):518-522. [18] 李建民,郝正玮,赵雅宁.不同步态训练方法对慢性不完全性脊髓损伤患者步行功能效果的Meta分析[J].中国康复理论与实践,2013,19(2):183-188. [19] DONENBERG JG, FETTERS L, JOHNSON R. The effects of locomotor training in children with spinal cord injury: a systematic review. Dev Neurorehabil. 2019;22(4):272-287. [20] HOLANDA LJ, SILVA PMM, AMORIM TC, et al. Robotic assisted gait as a tool for rehabilitation of individuals with spinal cord injury: a systematic review. J Neuroeng Rehabil. 2017;14(1):126. [21] AGUIRRE-GÜEMEZ AV, PÉREZ-SANPABLO AI, QUINZAÑOS-FRESNEDO J, et al. Walking speed is not the best outcome to evaluate the effect of robotic assisted gait training in people with motor incomplete Spinal Cord Injury: a Systematic Review with meta-analysis. J Spinal Cord Med. 2019;42(2): 142-154. [22] GANDHI P, CHAN K, VERRIER MC, et al. Training to improve walking after pediatric spinal cord injury: a systematic review of parameters and walking outcomes. J Neurotrauma. 2017;34(9):1713-1725. [23] MILLER LE, ZIMMERMANN AK, HERBERT WG. Clinical effectiveness and safety of powered exoskeleton-assisted walking in patients with spinal cord injury: systematic review with meta-analysis. Med Devices (Auckl). 2016;9:455-466. [24] LOUIE DR, ENG JJ, LAM T, et al. Gait speed using powered robotic exoskeletons after spinal cord injury: a systematic review and correlational study. J Neuroeng Rehabil. 2015;12:82. [25] ARAZPOUR M, SAMADIAN M, BAHRAMIZADEH M, et al. The efficiency of orthotic interventions on energy consumption in paraplegic patients: a literature review. Spinal Cord. 2015;53(3):168-175. [26] AHMADI BANI M, ARAZPOUR M, FARAHMAND F, et al. The efficiency of mechanical orthoses in affecting parameters associated with daily living in spinal cord injury patients: a literature review. Disabil Rehabil Assist Technol. 2015;10(3):183-190. [27] MORAWIETZ C, MOFFAT F. Effects of locomotor training after incomplete spinal cord injury: a systematic review. Arch Phys Med Rehabil. 2013;94(11):2297-2308. [28] 张缨,纪树荣,彭晓霞,等.慢性脊髓损伤患者步行训练有效性的Meta分析[J].中国康复医学杂志,2009,24(2):153-157. [29] DIJKERS MP, AKERS KG, DIEFFENBACH S, et al. Systematic reviews of clinical benefits of exoskeleton use for gait and mobility in neurologic disorders: a tertiary study. Arch Phys Med Rehabil. 2019. Doi: 10.1016/j.apmr.2019.01.025. [30] DUERINCK S, SWINNEN E, BEYL P, et al. The added value of an actuated ankle-foot orthosis to restore normal gait function in patients with spinal cord injury: a systematic review. J Rehabil Med. 2012;44(4):299-309. [31] FISAHN C, AACH M, JANSEN O, et al. The effectiveness and safety of exoskeletons as assistive and rehabilitation devices in the treatment of neurologic gait disorders in patients with spinal cord injury: a systematic review. Global Spine J. 2016;6(8):822-841. [32] HAYES SC, JAMES WILCOX CR, FORBES WHITE HS, et al. The effects of robot assisted gait training on temporal-spatial characteristics of people with spinal cord injuries: a systematic review. J Spinal Cord Med. 2018;41(5):529-543. [33] Tse CM, Chisholm AE, Lam T, et al. A systematic review of the effectiveness of task-specific rehabilitation interventions for improving independent sitting and standing function in spinal cord injury. J Spinal Cord Med. 2018;41(3):254-266. [34] LAM T, ENG JJ, WOLFE DL, et al. A systematic review of the efficacy of gait rehabilitation strategies for spinal cord injury. Top Spinal Cord Inj Rehabil. 2007;13(1):32-57. [35] MEHRHOLZ J, HARVEY LA, THOMAS S, et al. Is body-weight-supported treadmill training or robotic-assisted gait training superior to overground gait training and other forms of physiotherapy in people with spinal cord injury? A systematic review. Spinal cord. 2017;55(8):722-729. [36] GASPAR R, PADULA N, FREITAS TB, et al. Physical exercise for individuals with spinal cord injury: systematic review based on the international classification of functioning, disability, and health. J Sport Rehabil. 2019; 28(5):505-516. [37] NAM KY, KIM HJ, KWON BS, et al. Robot-assisted gait training (Lokomat) improves walking function and activity in people with spinal cord injury: a systematic review. J Neuroeng Rehabil. 2017;14(1):24. [38] KARSY M, HAWRYLUK G. Modern medical management of spinal cord injury. Curr Neurol Neurosci Rep. 2019;19(9):65. [39] 张缨,纪树荣,彭晓霞,等.Meta分析慢性脊髓损伤患者步行训练的有效性[C].中国康复研究中心.第三届北京国际康复论坛论文集.中国康复研究中心:《中国康复理论与实践》编辑部,2008: 196-197. [40] 黄俊杰,王坤善,侯铁东.吸气肌训练联合rTMS改善脊髓损伤患者肌肉和步行功能的效果观察[J].中国医学创新,2019, 16(33):19-24. [41] 吴金玲,杜宁,石秀秀,等.截瘫步行器Walkabout与ARGO对脊髓损伤患者平衡及日常生活能力的干预效果[J].临床与病理杂志,2019,39(11):2496-2500. [42] 高正超,牛斌斌,顾梦超,等.高频重复经颅磁刺激治疗不完全性脊髓损伤后运动障碍疗效的Meta分析[J].中国骨伤, 2018,31(1):47-55. [43] DIJKERS MP, AKERS KG, GALEN SS, et al. Letter to the editor regarding “Clinical effectiveness and safety of powered exoskeleton-assisted walking in patients with spinal cord injury:systematic review with meta-analysis”. Med Devices (Auckl). 2016,9:419-421. [44] CAO G. Letter to the Editor: “Is body-weight-supported treadmill training or robotic-assisted gait training superior to overground gait training and other forms of physiotherapy in people with spinal cord injury? A systematic review”. Spinal Cord. 2019;57(5):434. [45] MA DN, ZHANG XQ, YING J, et al. Efficacy and safety of 9 nonoperative regimens for the treatment of spinal cord injury: A network meta-analysis. Medicine (Baltimore). 2017;96(47):e8679. [46] MEHRHOLZ J, HARVEY LA, THOMAS S, et al. Response to Letter to the Editor by Dr Cao regarding paper titled - “Is body-weight-supported treadmill training or robotic-assisted gait training superior to overground gait training and other forms of physiotherapy in people with spinal cord injury? A systematic review”. Spinal Cord. 2019;57(5):435-436. [47] HWANG S, KIM HR, HAN ZA, et al. Improved gait speed after robot-assisted gait training in patients with motor incomplete spinal cord injury: a preliminary study. Ann Rehabil Med. 2017;41(1):34-41. [48] BARBEAU H, BASSO M, BEHRMAN A, et al. Treadmill training after spinal cord injury: good but not better. Neurology. 2016; 67(10):1900-1902. [49] WERNIG A. Treadmill training after spinal cord injury: good but not better. Neurology. 2006;67(10):1901-1902. [50] HARKEMA SJ, SCHMIDT-READ M, LORENZ D, et al. The authors respond: balance and ambulation improvements in individuals with chronic incomplete spinal cord injury using locomotor training-based rehabilitation. Arch Phys Med Rehabil. 2012; 93(5):919-921. [51] DIETZ V. Locomotor recovery after spinal cord injury. Trends Neurosci. 1997;20(8): 346-347. [52] SPIESS M, SCHULD C. Comment on “Restoration of walking function in an individual with chronic complete (AISA) spinal cord injury”. J Rehabil Med. 2011; 43(4):367-368. [53] VAN HEDEL HJ. Weight-supported treadmill versus over-ground training after spinal cord injury: from a physical therapist’s point of view. Phys Ther. 2006;86(10):1444-1447. [54] ROSSIGNOL IS, BARBEAU H. New approaches to locomotor rehabilitation in spinal cord injury. Ann Neurol. 1995;37(5):555-556. [55] CHAVAKULA V, VASUDEVA V, CHI J. Epidural spinal cord stimulation for the restoration of balance and gait following spinal cord injury. J Rehabil Med. 2016;78(6):N19-N20. [56] SUNNERHAGEN KS. Commentary on gait training in patients with spinal cord injury. J Rehabil Med. 2010;42(6):527. [57] SHIN JC, KIM JY, PARK HK, et al. Effect of robotic-assisted gait training in patients with incomplete spinal cord injury. Ann Rehabil Med. 2014;38(6):719-725. [58] SRIVASTAV AK, SHARMA N, KHADAYAT S. Commentary on: “Combined transcranial direct current stimulation and breathing-controlled electrical stimulation for the management of neuropathic pain after spinal cord injury”. J Rehabil Med. 2019; 51(8):622-623. [59] MEHRHOLZ J, HARVEY LA, THOMAS S, et al. Author Correction: is body-weight supported treadmill training or robotic-assisted gait training superior to overground gait trainingand other forms of physiotherapy in people with spinal cord injury? A systematic reviw. Spinal Cord. 2018;56(4):412. [60] CHRISTENSEN C, FICKES L. Commentary on “Interventions for Gait Training in Children With Spinal Cord Impairments: a Scoping Review”. Pediatr Phys Ther. 2017;29(4):349. [61] FUNDERBURG SE, JOSEPHSON HE, PRICE AA, et al. Interventions for gait training in children with spinal cord impairments: a scoping review. Pediatr Phys Ther. 2017; 29(4):342-349. [62] QUEL DE OLIVEIRA C, REFSHAUGE K, MIDDLETON J, et al. Effects of activity-based therapy interventions on mobility, independence, and quality of life for people with spinal cord injuries: a systematic review and meta-analysis. J Neurotrauma. 2017;34(9):1726-1743. [63] Warner FM, Cragg JJ, Jutzeler CR, et al. Progression of neuropathic pain after acute spinal cord injury: a meta-analysis and framework for clinical trials. J Neurotrauma. 2019;36(9):1461-1468. [64] GUYATT DH, OXMAN AD, VIST GE等.GRADE:证据质量和推荐强度分级的共识[J].中国循证医学杂志,2009,9(1):8-11. [65] 盛峰.康复治疗不同程度脊髓损伤的临床疗效分析[J].中国卫生标准管理,2018, 9(21):48-50. [66] 张郑.浅析康复治疗对脊髓损伤患者功能恢复的临床效果[J].中国卫生标准管理,2017,8(3):44-45. [67] 黄友,彭博.中医康复治疗脊髓损伤的临床研究进展[J].湖南中医杂志,2017, 33(8):204-207. [68] 何志良,张继荣.脊髓损伤后步行功能障碍的康复现状[J].中国康复,2016,31(6): 476-479. [69] 林海丹,张韬,陈青.康复机器人辅助步行训练对不完全性脊髓损伤患者步行能力的影响[J].自动化学报,2016,42(12): 1832-1838. [70] CHEUNG EYY, YU KKK, KWAN RLC, et al. Effect of EMG-biofeedback robotic-assisted body weight supported treadmill training on walking ability and cardiopulmonary function on people with subacute spinal cord injuries - a randomized controlled trial. BMC Neurol. 2019;19(1):140. [71] RICHARDSON J, TANG A, GUYATT G, et al. FIT for FUNCTION: study protocol for a randomized controlled trial. Trials. 2018; 19(1):39. [72] FOROUTAN F, GUYATT G, ALBA AC, et al. Meta-analysis: mistake or milestone in medicine? Heart. 2018;104(19):1559-1561. [73] Arazpour M, Gholami M, Bahramizadeh M, et al. Influence of Reciprocating Link When Using an Isocentric Reciprocating Gait Orthosis (IRGO) on Walking in Patients with Spinal Cord Injury: a Pilot Study. Top Spinal Cord Inj Rehabil. 2017;23(3):256-262. |
| [1] | Min Youjiang, Yao Haihua, Sun Jie, Zhou Xuan, Yu Hang, Sun Qianpu, Hong Ensi. Effect of “three-tong acupuncture” on brain function of patients with spinal cord injury based on magnetic resonance technology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(在线): 1-8. |
| [2] | Jiang Hongying, Zhu Liang, Yu Xi, Huang Jing, Xiang Xiaona, Lan Zhengyan, He Hongchen. Effect of platelet-rich plasma on pressure ulcers after spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1149-1153. |
| [3] | Wan Ran, Shi Xu, Liu Jingsong, Wang Yansong. Research progress in the treatment of spinal cord injury with mesenchymal stem cell secretome [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1088-1095. |
| [4] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [5] | Ma Binxiang, He Wanqing, Zhou Guangchao, Guan Yonglin. Triptolide improves motor dysfunction in rats following spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 701-706. |
| [6] | Sun Jianwei, Yang Xinming, Zhang Ying. Effect of montelukast combined with bone marrow mesenchymal stem cell transplantation on spinal cord injury in rat models [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3962-3969. |
| [7] | Yan Peng, Ma Yufei, Cui Jingfu, Hao Shaofei, Liu Jinhui, Guan Chunlei, Wang Xiaoran, Yang Xiaoyu. Mechanism of anodic block electrical stimulation of sacral nerve root to reconstruct bladder function [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3684-3689. |
| [8] | Xu Weilong, Zuo Yuan, Xin Daqi, He Chenyang, Zhao Peng, Shi Ming, Zhou Boyuan, Liu Yating, Zhao Yan. Selection of modeling methods for acute compressive spinal cord injury: a network Meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3767-3772. |
| [9] | Tian Ting, Li Xiaoguang. Problems and challenges in regeneration and repair of spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3039-3048. |
| [10] | Ren Bingkai, Zheng Yibin, Huang Leiwen, Wu Fanhui, Yang Dong . Value of respiratory tract management and fiberoptic bronchoscopy in traumatic cervical spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(18): 2902-2907. |
| [11] | Chen Xingying, Hao Fei, Gao Yudan, Zhao Wen, Duan Hongmei, Yang Chaoyang, Li Xiaoguang. Rehabilitation training combined with neurotrophin 3-chitosan scaffolds enhanced skeletal muscle morphology and functional recovery in rats with spinal cord injury [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(16): 2514-2520. |
| [12] | Qian Nannan, Zhang Qian, Yang Rui, Ao Jun, Zhang Tao. Mesenchymal stem cells in the treatment of spinal cord injury: cell therapy and combination of new drugs and biomaterials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(13): 2114-2120. |
| [13] | Fang Chao, Sun Jian, Wei Laifu, Gao Fei, Qian Jun . Oscillating field stimulation inhibits neuroinflammatory response and promotes functional recovery after spinal cord injury in rats [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(11): 1717-1722. |
| [14] | Zhou Jihui, Yao Meng, Wang Yansong, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Spinal cord injury repaired by using nano tissue-engineered spinal cord [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(10): 1550-1554. |
| [15] | Zhu Ning, Yang Xinming, Ruan Jianwei. Triptolide improves spinal cord injury recovery via upregulation of autophagy and inhibition of apoptosis in Thy-yfp transgenic mice [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(在线): 1-. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||