Chinese Journal of Tissue Engineering Research ›› 2016, Vol. 20 ›› Issue (53): 8043-8050.doi: 10.3969/j.issn.2095-4344.2016.53.019
Previous Articles Next Articles
Common peroneal nerve injury after primary total knee arthroplasty: risk factors and strategies of prevention and treatment
Chen You-rong1, Wan Fu-yin1, Guo Wan-shou2, Wang Wei-guo2, Cheng Li-ming2, Zhang Qi-dong2, Ding Ran2
- 1China-Japan Friendship School of Clinical Medicine, Peking University, Beijing 100029, China; 2Department of Orthopedic Surgery, China-Japan Friendship Hospital, Beijing 100029, China
-
Revised:2016-10-17Online:2016-12-23Published:2016-12-23 -
Contact:Guo Wan-shou, M.D., Chief physician, Professor, Doctoral supervisor, Department of Orthopedic Surgery, China-Japan Friendship Hospital, Beijing 100029, China -
About author:Chen You-rong, Studying for master’s degree, China-Japan Friendship School of Clinical Medicine, Peking University, Beijing 100029, China -
Supported by:the National Natural Science Foundation of China, No. 81273972
Cite this article
Chen You-rong, Wan Fu-yin, Guo Wan-shou, Wang Wei-guo, Cheng Li-ming, Zhang Qi-dong, Ding Ran. Common peroneal nerve injury after primary total knee arthroplasty: risk factors and strategies of prevention and treatment[J]. Chinese Journal of Tissue Engineering Research, 2016, 20(53): 8043-8050.
share this article

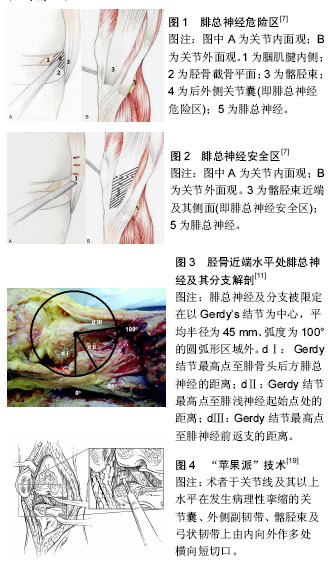
2.1 腓总神经解剖学基础 腓总神经来自L4-S2神经根,作为坐骨神经的重要分支,沿股二头肌肌腱内侧向外下走行,于小腿上段外侧腓骨头颈交界部开始与腓骨骨膜紧密相贴,并进入由腘筋膜、腓骨长肌起始部纤维及腓骨颈三部分组成的骨纤维隧道——腓管,在腓管这一狭窄区域内,腓总神经位置最为表浅,神经外组织缺乏,同时神经束及结缔组织量增加了1倍,容易被外伤或直接压迫所损伤;同时,由于上方骨盆和下方腓骨颈的固定,以及腘窝上下方分支的牵制,腓总神经移动受限易受到牵拉性损伤。在穿行或穿出腓管过程中,腓总神经分为腓浅、腓深及膝返神经等终末支,并分布于小腿前外侧群肌和足背肌以及小腿外侧、足背和趾背的皮肤[4-5]。 2.2 腓总神经损伤后临床表现 英国医学研究会(British Medical Research Council,BMRC)神经外科学会根据外周神经损伤程度,将其由重至轻分为Ⅰ-Ⅴ度[6]。腓总神经损伤严重者可出现完全麻痹症状:如足不能背屈、趾不能伸、足内翻且下垂,呈“马蹄内翻足”畸形,行走时呈”跨阈步态”;同时伴有小腿前外侧及足背区感觉障碍。损伤较轻者可仅出现屈伸膝关节时小腿短暂性疼痛或触痛,而无足趾背伸无力等运动缺失,腓骨水平处腓总神经Tinel试验阳性,此即腓神经功能障碍。与完全腓总神经麻痹相比,后者临床表现不明显,需通过肌电图、神经传导速度、体感诱发电位等电生理学检查方可诊断,因此,腓总神经损伤的实际发生率在一定程度上可能被低估,同时后者也可能是关节置换术后功能恢复不满意和(或)小腿外侧持续性非典型疼痛的原因之一[3]。 2.3 腓总神经损伤危险区 手术过程中,术者及助手对不同程度膝关节畸形时腓神经的局部解剖结构及毗邻不清,是导致腓总神经损伤的主要原因之一,故明确腓总神经及其主要分支在腘窝及胫腓骨近端的解剖结构和手术安全区显得十分重要。Bruzzone等[7]证明,腓总神经走行于由腘肌腱内侧、胫骨截骨平面及髂胫束最后缘纤维所组成的危险三角形区域内(即后外侧关节囊),腓神经距胫骨后外侧骨皮质边缘处约13.5 mm,该距离与胫骨截骨平面前后径及内外径正相关,在胫骨截骨平面松解后外侧关节囊时,最易损伤腓总神经(图1);而腓总神经距髂胫束后缘约35.8 mm,在髂胫束近端及其侧面操作时远离腓总神经,此即为安全区(图2)。Jenkins等[8]则通过研究200例膝关节MRI资料指出,腓总神经位于以胫骨截骨平面前后轴中点为中心、向后外象限旋转29.95°-54.57°的范围内;腓总神经至膝关节后外侧关节囊的平均距离为11.9 mm(4.7-22.13 mm);此方法虽能准确估计腓总神经所在位置,但相较于Bruzzone等[7]的研究,其并不便于临床实际应用。Dearden等[9]指出,腓总神经越过腓骨颈处距离腓骨尖平均约为34.8 mm(21.5-44.3 mm),并认为术中Hoffman板钩在平行胫骨纵轴、紧贴胫骨外侧骨面插入时深度不宜超过20 mm。余正红等[10]则认为松解腓肠肌外侧头及后外侧关节囊时,助手自后向前环抱提拉股骨远端是腓神经损伤的首要高危因素,该操作使腓总神经更贴近股骨,其安全距离及活动度明显下降,并建议松解过程中利用髓内杆向上提拉股骨干,使腓总神经较为游离,即便受到器械刃口冲击,其损伤概率也相对较小而更为安全。为探讨腓总神经与周围组织的三维立体关系、确认一个体表解剖学标志,以利于提高临床可行性,Rubel等[11]解剖31例新鲜膝关节标本并测量Gerdy’s结节至腓总神经及其各分支的距离与相关角度后指出,腓总神经及分支被限定在以Gerdy’s结节为中心,平均半径为45 mm、弧度为100°的圆弧形区域外(图3)。由于Gerdy’s结节位置表浅恒定、易于定位,术前即可标记出手术安全区。但该方法不适用于存在先天畸形、合并上胫腓联合韧带撕裂等可能改变腓总神经在腓骨头处位置以及严重软组织肿胀、过度肥胖影响腓骨头和Gerdy’s结节定位的情况。 2.4 危险因素及预防策略 2.4.1 矫正膝关节严重外翻和屈曲畸形 既往研究指出,膝关节严重外翻(> 12°)和屈曲畸形(> 20°)与腓神经损伤关系密切,在矫正畸形时腓神经及其周围软组织所受牵拉较正常膝关节大幅增加,随即引起的神经延长或外周血供受损是其主要损伤机制[12-13]。有研究表明,人类神经延长4%-11%可出现严重的轴索损伤;兔胫神经延长8%即发生微循环损害;且畸形程度越严重,其损伤可能越大[2]。Montgomery等[14]回顾性分析71例因关节僵直而行全膝关节置换的患者(共81例膝),其中2例膝术后出现腓总神经麻痹,该2例膝关节术前均存在严重屈曲外翻畸形。为此周殿阁等[15]指出,对> 15°的重度固定膝外翻者,采用外侧髌旁入路、关节囊“Z”字形切开法能够直接松解外侧韧带及软组织,有效缓解腓神经压力。同时,针对高度屈曲畸形患者,为避免术中一次牵引过度,术前即可行持续牵引以松解软组织[15],但对于术前长期屈曲挛缩畸形甚至强直状态的膝关节能否采用该方法尚无相关文献提及。然而并非所有出现腓神经损伤的患者均存在外翻及屈曲畸形,胫骨截骨过多(> 1 cm) 、清理胫骨平台后外缘时过度向前脱位、股骨远端截骨时胫骨向后移位挤压均可能是其损伤原因[16-18]。 膝外翻畸形患者行全膝关节置换时,采用“苹果派”技术(“pie crust” technique)进行软组织平衡亦是腓神经损伤的原因之一,该方法通过在发生病理性挛缩的关节囊、外侧副韧带、髂胫束及弓状韧带上由内向外作多处横向短切口,以达到松解外侧软组织的目的[19](图4)。为避免该过程腓总神经直接损伤,Jia等[20]采用磁共振成像方式,测量关节线及胫骨截骨水平处腓神经距离关节囊后外侧角内表面分别为15.0 mm (8.5-22.3 mm)、14.0 mm (8.0-23.2 mm),同时指出该距离与膝关节软组织前后径相关,但与胫骨大小无关;并建议松解外侧软组织时,深度不宜超过8 mm,而膝关节外径偏细的患者需更加小心。Clarke等[19]则更为保守,他建议刀尖深入不宜超过5 mm。 2.4.2 止血带的不恰当使用 止血带通过防止术中出血、创造良好术野、缩短手术时间而被广泛用于全膝关节置换中,然而其使用不当将引起止血带麻痹等并发症;多项研究表明,止血带通过直接切割及间接机械压迫作用损伤神经,并与髓鞘功能紊乱、郎飞氏结移位、压迫所致局部缺血而产生的轴索去极化以及压迫解除后的超极化密切相关。在止血带压力、使用时间及种类等诸多因素中,止血带压力最易控制,同时也最易被误用[21-22]。2005年,美国一项基于网络、针对骨科医生的调查报告指出,尽管60%的学者了解相关学术文献,但其中仅25%的术者在临床中正确使用了下肢止血带压力,学术研究与临床实践间仍存在巨大分歧[23]。Olivecrona等[24]研究表明,基于术前计算下肢动脉闭塞压设定止血带压力的方法(下肢动脉闭塞压=[(收缩压-舒张压)×肢体周长/(3×止血带宽度)]+舒张压;止血带压力=下肢动脉闭塞压+50- 100 mm Hg),相较于传统的基于收缩压设定压力的方法(止血带压力=收缩压+100 mm Hg),可在提供良好术野的同时,明显降低止血带压力,但两者在术后疼痛、麻痹、关节活动度等并发症情况接近。Noordin等[25]则认为降低不必要的止血带压力可降低神经损伤风险,并指出弧形止血带相较于直止血带更适于下肢的圆锥状外形,两者吻合度好,压力分布均匀,其向下方组织传导压力的效率高,所需有效压力较低,特别适用于肥胖及肌肉较发达的患者,故建议在不影响术野的情况下尽量使用较宽的弧形止血带。Horlocker等[13]的回顾性研究发现,腓总神经损伤与止血带使用时间密切相关,使用时间超过120 min是其危险因素,且每增加30 min,神经损伤风险增加2.8倍;并建议在延长使用止血带时,放松10-30 min,以提供再灌注时间。Jacob等[26]也证实了两者间的关系,认为止血带时间每增加30 min,神经损伤风险增加1.28倍,但该研究并未阐述止血带允许使用的总时间,是其不足之处。 2.4.3 双极电凝的不恰当使用 双极电凝的术中止血效果确切而被矫形外科医生所肯定,但术者激进的使用方式,以及在膝关节后方间隙进行操作时,由于后方股骨的遮挡,使腓总神经处于潜在危险当中。Lyons等[27]通过比较双极电凝与标准电凝在初次全膝关节置换术中对膝关节后方进行止血时发现,前者所发生的神经病变明显高于后者。然而与标准电凝组相比,双极电凝止血靶点明确、组织保护性更强的优势,在骨科、神经外科得到广泛应用[28-30],虽然Lyons等未进一步探讨相关原因,但可能与双极电凝具有以上优点而使术者在膝关节后方间隙进行操作时放松了警惕有关;此外,Lyons等[27]的研究还表明体质量指数偏低的女性及类风湿性关节炎患者,在使用双极电凝止血时更容易损伤腓神经。由于双极电凝的神经灼伤危险性随功率的增大而上升,故不能盲目增大电凝的输出功率,以刚好保证手术效果为佳,同时尽可能保持输出功率的稳定;以上学者还提醒,在膝关节后方进行止血操作时务必小心,避免使用双极电凝过于激进。 2.4.4 术前神经病变、内科疾病及肥胖 术前存在椎管狭窄、腰骶神经根病变及腰椎间盘摘除史;或通过电生理检查方式诊断的无症状周围神经病变均被认为与全膝关节置换后腓神经麻痹显著相关,该危险因素可用Upton等[2,31]提出的“双卡综合征”解释;双卡综合征是指事先存在的神经近端受压或病变,导致轴浆流速变慢、离子通道上调或下调,从而使同一神经的远端部位对牵拉或卡压的易感性增高[32-33]。由于类风湿性关节炎可通过类风湿血管炎等机制引起血管周围单核细胞浸润、神经纤维轻度脱髓鞘及周围组织炎性渗出、水肿、增生压迫神经,据统计,约33%出现神经性症状的类风湿性关节炎患者可诊断为周围神经病变[34]。故有研究认为,类风湿性关节炎为全膝关节置换后腓神经损伤的危险因素[27]。然而,Knutson等[35]虽发现类风湿性关节炎与全膝关节置换后腓神经损伤之间的相关性,但类风湿性关节炎常伴随屈曲挛缩及外翻畸形,类风湿性关节炎对腓神经的影响是通过上述危险因素间接起作用的。虽然糖尿病亦可通过微血管病变、氧化应激及高血糖毒性等多种致病机制引起神经细胞损伤,但至目前为止尚未发现糖尿病与全膝关节置换后腓神经损伤之间的相关性[36-37]。Park等[38]则发现高身体质量指数更易发生腓神经损伤,这可解释为肥胖患者术中暴露困难,增加了牵拉神经的机会;同时肥胖患者术后平卧时更倾向于将髋关节外旋,从而使腓骨头水平处腓神经受压可能性增大。故对于肥胖患者,术中暴露困难时切忌粗暴,术后注意保持患肢中立位[39]。 2.4.5 麻醉及术后镇痛方式 Idusuyi等[12]回顾性分析10 361例行全膝关节置换患者后发现,硬膜外麻醉及镇痛是腓神经损伤的重要危险因素,相较于仅使用全麻或腰麻患者,腓神经麻痹风险增加2.8倍,其认为硬膜外置管、局麻药的神经毒性以及局麻药中血管收缩剂引起的局部缺血均可造成脊神经及其神经根损伤;同时,硬膜外镇痛使肢体感觉运动功能恢复延迟,下肢外旋及腓骨颈处受压风险增加,即使外包扎压力过大,患者不易感知,也不利于术者早期判断[40]。Beller等[41]也表明持续硬膜外麻醉与镇痛可通过某种不明机制对腓神经相关神经根产生压迫,故强烈建议设置止血带压力于320 mmHg以内,同时安全放置患肢,以避免“双卡综合征”。Aikawa等[42]对17例行全膝关节置换的患者术后使用坐骨神经阻滞或关节周围局部浸润麻醉方式镇痛,结果表明,66.7%使用坐骨神经阻滞镇痛的患者术后出现腓神经麻痹,而使用关节周围局部浸润麻醉镇痛的患者无一例发生该并发症。鉴于坐骨神经阻滞引起腓总神经麻痹的概率极大,不利于术后早期评估腓神经功能,该镇痛方式目前被某些医院所禁用[43];Hishiyama等[43]认为超声引导下股神经阻滞可在全膝关节置换后提供良好镇痛的同时不影响腓神经功能评估。Sinha等[44]的随机对照研究指出,选择性胫神经阻滞联合股神经阻滞可在提供相同镇痛效果的同时避免坐骨神经阻滞引起的腓总神经运动功能完全阻滞。然而,Jacob等[26]并未发现腓神经损伤与麻醉种类的相关性;Tsukada等[45]则指出,硬膜外镇痛的暂时性腓神经麻痹发生率明显低于关节周围局部浸润麻醉镇痛方式,这可能与局部浸润镇痛过程中腓神经直接针刺伤有关,故主张在关节后方操作时避免过度注射浸润麻醉药物。 2.4.6 血肿形成、局部压迫等致腓神经损伤 由于腓总神经穿行腓管处位置表浅、与 周围组织相对固定的解剖结构特点,故容易被直接压迫所损伤,但该类病因仅占腓神经损伤的一小部分。Guzelkucuk等[46]、Yi等[47]和Girolami等[48]分别报道了1例因弹力袜卷曲并压迫腓骨颈处,1例术中体位摆放不当腓总神经受压,以及1例腓骨颈周围血肿形成导致的腓神经损伤。 Wright等[49]则指出非正确使用序贯加压装置亦是导致全膝关节置换后腓神经压迫受损的原因之一。鉴于体位摆放不当等外在压迫是腓总神经损伤的危险因素,故建议术中小心摆放下肢并保护腓骨颈部位,术后膝关节加压包扎防止过紧、同时术后患者平卧位时在患肢同侧的髋部放置一软枕,以防下肢外旋。Girolami等[48]还认为通过手术方式治疗腓总神经麻痹前采用超声或MRI明确腓神经受压原因是有效解除压迫的重要步骤。由于病因较为明确,故及时解除危险因素后预后通常较好,预防也较为简单有效。 2.5 迟发性腓神经麻痹 Deshmukh等[50]报道了1例初次全膝关节置换后12年,由于广泛胫骨近端溶骨继发骨囊肿形成而导致的腓神经麻痹。在翻修过程中发现,胫骨近端溶骨及组件松动较为明显,继发形成的骨囊肿通过胫骨近端的骨皮质缺损处减压并进入小腿前外侧,进而压迫腓总神经。进一步分析骨囊肿内囊液,其内含有较多聚乙烯碎片;翻修后7年再次随访,手术虽解决了骨囊肿问题,但腓神经麻痹一直未恢复。指出全膝关节置换后骨溶解通常与聚乙烯垫磨损并继发假体松动有关,必须注意这种少见但具有引起潜在毁灭性并发症的骨溶解及膨胀性骨囊肿,一旦发现建议早期行翻修手术并对骨囊肿减压,以避免压迫腓神经引起的不可逆性损伤。 2.6 治疗及预后 为避免腓总神经损伤及由此产生的不良后果,全膝关节置换后小心摆放患肢,待患者神志恢复后及时检查腓总神经功能并行双下肢对比,患肢一旦出现感觉、运动缺失等神经损伤迹象,立即解除所有敷料、屈曲膝关节20°-30°,以减少腓神经压迫及牵拉,据统计,约25%早期诊断的病例经上述处理神经功能可部分恢复[31]。Park等[38]认为除非能找到引起腓神经损伤的明确病因,否则推荐使用包括踝足矫形器、踝关节被动背伸锻炼、电刺激以及超声波、红外线等在内的非手术治疗方式;其研究结果显示67.6%的患者神经功能可完全恢复,同时还发现,腓神经初始损伤严重程度是影响预后的惟一因素,腓神经非完全损伤者完全恢复的可能性明显高于完全损伤者,两者差异有显著性意义。有研究主张,同时应用神经营养药物、外源性神经生长因子及激素类等药物,可加快神经的再生速度、防止神经细胞突触可塑性的改变,促进神经损伤的修复、从而达到减轻或防止神经病理性疼痛的发生[51-52]。然而,鉴于以上保守治疗具有不可预测性,既往研究对5位经非手术治疗4-45个月神经功能仍无改善的患者行手术探查腓神经减压,结果显示所有患者神经功能均得到改善,其中4位患者完全恢复,故其推荐3个月后仍无临床或肌电图改善的患者早期行手术探查腓神经减压;若术后运动功能仍无恢复,则行踝关节融合[2]。Zywiel等[3]对手术治疗则更为积极,建议确诊为非典型腓神经损伤且伴有活动度恢复不理想的患者先理疗4周,若无好转即考虑外科松解,其研究结果表明所有经腓神经松解的患者膝关节活动度平均增加40°,功能得到明显改善。"
| [1] Losina E, Thornhill TS, Rome BN, et al. The dramatic increase in total knee replacement utilization rates in the United States cannot be fully explained by growth in population size and the obesity epidemic. J Bone Joint Surg Am. 2012;94(3):201-207.[2] Nercessian OA, Ugwonali OF, Park S. Peroneal nerve palsy after total knee arthroplasty. J Arthroplasty. 2005; 20(8):1068-1073.[3] Zywiel MG, Mont MA, McGrath MS, et al. Peroneal nerve dysfunction after total knee arthroplasty: characterization and treatment. J Arthroplasty. 2011; 26(3):379-385. [4] Watt T, Hariharan AR, Brzezinski DW, et al. Branching patterns and localization of the common fibular (peroneal) nerve: an anatomical basis for planning safe surgical approaches. Surg Radiol Anat. 2014; 36(8):821-828.[5] 张绍祥,张雅芳.局部解剖学[M].北京:人民卫生出版社, 2015:397,403-404.[6] Bsteh G, Wanschitz JV, Gruber H, et al. Prognosis and prognostic factors in non-traumatic acute-onset compressive mononeuropathies--radial and peroneal mononeuropathies.Eur J Neurol. 2013;20(6):981-985. [7] Bruzzone M, Ranawat A, Castoldi F, et al. The risk of direct peroneal nerve injury using the Ranawat "inside-out" lateral release technique in valgus total knee arthroplasty. J Arthroplasty. 2010;25(1):161-165. [8] Jenkins MJ, Farhat M, Hwang P, et al. The Distance of the Common Peroneal Nerve to the Posterolateral Structures of the Knee. J Arthroplasty. 2016. pii: S0883-5403(16)30139-5. [9] Dearden P, Lowery K, Sherman K, et al. Fibular head transfixion wire and its relationship to common peroneal nerve: cadaveric analysis. Strategies Trauma Limb Reconstr. 2015;10(2):73-78. [10] 余正红,蔡胥,李鉴轶,等.膝关节置换术中腓总神经损伤的原因与预防[J].中国矫形外科杂志,2008,16(11): 807-810.[11] Rubel IF, Schwarzbard I, Leonard A, et al. Anatomic location of the peroneal nerve at the level of the proximal aspect of the tibia: Gerdy's safe zone. J Bone Joint Surg Am. 2004;86-A(8):1625-1628.[12] Idusuyi OB, Morrey BF. Peroneal nerve palsy after total knee arthroplasty. Assessment of predisposing and prognostic factors. J Bone Joint Surg Am. 1996;78(2): 177-184.[13] Horlocker TT, Hebl JR, Gali B, et al. Anesthetic, patient, and surgical risk factors for neurologic complications after prolonged total tourniquet time during total knee arthroplasty. Anesth Analg. 2006;102(3):950-955.[14] Montgomery WH 3rd, Insall JN, Haas SB, et al. Primary total knee arthroplasty in stiff and ankylosed knees. Am J Knee Surg. 1998;11(1):20-23.[15] 周殿阁,张斌,寇伯龙,等.膝外翻全膝关节置换外侧髌旁入路的手术方法探讨[J].中华医学杂志,2007,87(27): 1885-1889 .[16] 顾春松,易洪城,彭雅,等.人工全膝关节置换术后常见并发症及预防对策[J].黔南民族医专学报, 2013,26(4): 261-262,265.[17] 徐中华,王业华,王立新,等.全膝关节置换术后腓总神经麻痹的原因及治疗[J].中国矫形外科杂志,2012,20(15): 1430-1431.[18] 彭慧明,翁习生,林进,等.初次全膝关节置换术后腓总神经麻痹的原因及处理[J].中国骨与关节外科,2010,3(3):198-203.[19] Clarke HD, Schwartz JB, Math KR, et al. Anatomic risk of peroneal nerve injury with the "pie crust" technique for valgus release in total knee arthroplasty. J Arthroplasty. 2004;19(1):40-44.[20] Jia Y, Gou W, Geng L, et al. Anatomic proximity of the peroneal nerve to the posterolateral corner of the knee determined by MR imaging. Knee. 2012;19(6):766-768. [21] Estebe JP, Davies JM, Richebe P. The pneumatic tourniquet: mechanical, ischaemia-reperfusion and systemic effects. Eur J Anaesthesiol. 2011;28(6):404-411. [22] Olivecrona C, Blomfeldt R, Ponzer S, et al. Tourniquet cuff pressure and nerve injury in knee arthroplasty in a bloodless field: a neurophysiological study. Acta Orthop. 2013;84(2):159-164. [23] Tejwani NC, Immerman I, Achan P, et al. Tourniquet cuff pressure: The gulf between science and practice. J Trauma. 2006;61(6):1415-1418.[24] Olivecrona C, Ponzer S, Hamberg P, et al. Lower tourniquet cuff pressure reduces postoperative wound complications after total knee arthroplasty: a randomized controlled study of 164 patients. J Bone Joint Surg Am. 2012;94(24):2216-2221. [25] Noordin S, McEwen JA, Kragh JF Jr, et al. Surgical tourniquets in orthopaedics. J Bone Joint Surg Am. 2009;91(12):2958-2967. [26] Jacob AK, Mantilla CB, Sviggum HP, et al. Perioperative nerve injury after total knee arthroplasty: regional anesthesia risk during a 20-year cohort study. Anesthesiology. 2011;114(2):311-317. [27] Lyons S, Morrison K, Tejiram S, et al. Sensory neuropathy associated with aggressive cauterization using a bipolar radiofrequency device in primary TKA. Orthopedics. 2013;36(2):e147-150.[28] Marulanda GA, Ulrich SD, Seyler TM, et al. Reductions in blood loss with a bipolar sealer in total hip arthroplasty. Expert Rev Med Devices. 2008;5(2): 125-131. [29] Marulanda GA, Krebs VE, Bierbaum BE, et al. Hemostasis using a bipolar sealer in primary unilateral total knee arthroplasty. Am J Orthop (Belle Mead NJ). 2009;38(12):E179-183.[30] Bowers CA, Burns G, Salzman K, et al. Comparison of ferromagnetic induction and bipolar electrosurgery and suction in corticotomies in pig cerebrum. Int J Surg. 2015;16(Pt A):55-59. [31] Schinsky MF, Macaulay W, Parks ML, et al. Nerve injury after primary total knee arthroplasty. J Arthroplasty. 2001;16(8):1048-1054.[32] Kane PM, Daniels AH, Akelman E. Double Crush Syndrome. J Am Acad Orthop Surg. 2015;23(9): 558-562. [33] Schmid AB, Coppieters MW. The double crush syndrome revisited--a Delphi study to reveal current expert views on mechanisms underlying dual nerve disorders. Man Ther. 2011;16(6):557-562. [34] Sim MK, Kim DY, Yoon J, et al. Assessment of peripheral neuropathy in patients with rheumatoid arthritis who complain of neurologic symptoms. Ann Rehabil Med. 2014;38(2):249-255. [35] Knutson K, Leden I, Sturfelt G, et al. Nerve palsy after knee arthroplasty in patients with rheumatoid arthritis. Scand J Rheumatol. 1983;12(3):201-205.[36] Callaghan BC, Cheng HT, Stables CL, et al. Diabetic neuropathy: clinical manifestations and current treatments. Lancet Neurol. 2012;11(6):521-534. [37] Hosseini A, Abdollahi M. Diabetic neuropathy and oxidative stress: therapeutic perspectives. Oxid Med Cell Longev. 2013;2013:168039.[38] Park JH, Restrepo C, Norton R, et al. Common peroneal nerve palsy following total knee arthroplasty: prognostic factors and course of recovery. J Arthroplasty. 2013;28(9):1538-1542.[39] Järvenpää J, Kettunen J, Kröger H, et al. Obesity may impair the early outcome of total knee arthroplasty. Scand J Surg. 2010;99(1):45-49.[40] Leech C. Analgesia for total knee arthroplasty. Br J Hosp Med (Lond). 2010;71(9):538.[41] Beller J, Trockel U, Lukoschek M. Peroneal nerve palsy after total knee arthroplasty under continuous epidural anaesthesia. Orthopade. 2008;37(5):475-480. [42] Aikawa K, Hashimoto T, Itosu Y, et al. Comparison of the Effect of Periarticular Infiltration Analgesia versus Sciatic Nerve Block for Total Knee Arthroplasty. Masui. 2016;65(1):50-55.[43] Hishiyama S, Ishiyama T, Asano N, et al. Femoral nerve block for total knee arthroplasty. Masui. 2014; 63(8):872-876.[44] Sinha SK, Abrams JH, Arumugam S, et al. Femoral nerve block with selective tibial nerve block provides effective analgesia without foot drop after total knee arthroplasty: a prospective, randomized, observer-blinded study. Anesth Analg. 2012;115(1): 202-206. [45] Tsukada S, Wakui M, Hoshino A. Postoperative epidural analgesia compared with intraoperative periarticular injection for pain control following total knee arthroplasty under spinal anesthesia: a randomized controlled trial. J Bone Joint Surg Am. 2014;96(17):1433-1438. [46] Güzelküçük Ü, Skempes D, Kumnerddee W. Common peroneal nerve palsy caused by compression stockings after surgery. Am J Phys Med Rehabil. 2014; 93(7):609-611. [47] Yi HJ, Oh SH, Hong HJ, et al. Common peroneal nerve palsy as a complication of anterior cervical operation: a case report. Surg Neurol. 2004;61(4):379-383; discussion 383.[48] Girolami M, Galletti S, Montanari G, et al. Common peroneal nerve palsy due to hematoma at the fibular neck. J Knee Surg. 2013;26 Suppl 1:S132-135. [49] Wright RC, Yacoubian SV. Sequential compression device may cause peroneal nerve palsy. Orthopedics. 2010;33(6):444. [50] Deshmukh AJ, Kuczynski B, Scuderi GR. Delayed peroneal nerve palsy after total knee arthroplasty--a rare complication of tibial osteolysis. Knee. 2014;21(2): 624-627. [51] Liu YR, Liu Q. Meta-analysis of mNGF therapy for peripheral nerve injury: a systematic review. Chin J Traumatol. 2012;15(2):86-91.[52] 侯红艳,刘诗翔.周围神经损伤康复治疗研究进展[J].临床军医杂志,2012,40(2):482-483. |
| [1] | Liang Xin, Wang Heng, Li Xian-rong. Preoperative application of alprazolam for patients with anxiety and depression and pain after total knee arthroplasty: its safety and effectiveness [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 985-992. |
| [2] | Shi Bin, An Jing, Chen Long-gang, Zhang Nan, Tian Ye . Influencing factors for pain after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 993-997. |
| [3] | Wang Xian-xun. Impact of local compression cryotherapy combined with continuous passive motion on the early functional recovery after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 998-1003. |
| [4] | Lu Yao-jia, Xiong Chuan-zhi, Li Xiao-lei, Hu Han-sheng, Chen Gang, Wang Qiang, Lu Zhi-hua. Comparison of two methods for reducing blood loss during total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1004-1008. |
| [5] | Yuan Wei, Zhao Hui, Ding Zhe-ru, Wu Yu-li, Wu Hai-shan, Qian Qi-rong. Association between psychological resilience and acute mental disorders after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1015-1019. |
| [6] | Chen Qun-qun, Qiao Rong-qin, Duan Rui-qi, Hu Nian-hong, Li Zhao, Shao Min. Acu-Loc®2 volar distal radius bone plate system for repairing type C fracture of distal radius [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1025-1030. |
| [7] | Huang Xiang-wang, Liu Hong-zhe. A new low elastic modulus of beta titanium alloy Ti2448 spinal pedicle screw fixation affects thoracic stability: biomechanical analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1031-1035. |
| [8] | Xie Qiang. Three-dimensional finite element model for biomechanical analysis of stress in knee inversion and external rotation after posterior cruciate ligament rupture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1036-1040. |
| [9] | He Ze-dong, Zhao Jing, Chen Liang-yu, Li Ke, Weng Jie. Multilevel finite element analysis on the biological tribology damage of water on bone tissue [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1041-1045. |
| [10] | Jiang Zi-wei, Huang Feng, Cheng Si-yuan, Zheng Xiao-hui, Sun Shi-dong, Zhao Jing-tao, Cong Hai-chen,Sun Han-qiao, Dong Hang. Design and finite element analysis of digital splint [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1052-1056. |
| [11] | Wang Fei, Liu Zhi-bin, Tao Hui-ren, Zhang Jian-hua, Li Chang-hong, Cao Qiang, Zheng Jun, Liu Yan-xiong, Qu Xiao-peng. Clinical efficacy of preoperative osteotomy designs using paper-cut technology versus photoshop software for ankylosing spondylitis with kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1057-1063. |
| [12] | Li Hui, Ma Jun-yi, Ma Yuan, Zhu Xu . Establishment of a three-dimensional finite element model of ankylosing spondylitis kyphosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1069-1073. |
| [13] | Ling Guan-han, Ou Zhi-xue, Yao Lan, Wen Li-chun, Wang Guo-xiang, Lin Heng-feng. Establishment of simulating three-dimensional model of China-Japan Friendship Hospital Classification for L type osteonecrosis of the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1074-1079. |
| [14] | Fu Wei-min, Wang Ben-jie. Assessing the degree of necrotic femoral head, and association of blood supply with pathlogical changes: study protocol for a diagnostic animal trial [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1086-1091. |
| [15] | Zhang Wen-qiang, Ding Qian, Zhang Na. Associations between alpha angle and herniation pit on oblique axial magnetic resonance imaging in asymptomatic hip joints of adults [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1098-1103. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||