Chinese Journal of Tissue Engineering Research ›› 2019, Vol. 23 ›› Issue (21): 3336-3341.doi: 10.3969/j.issn.2095-4344.1755
Previous Articles Next Articles
Three-dimensional dynamic culture of auricular chondrocytes with microcarriers in vitro
Sun Heng, Ma Shize, Jiang Haiyue, Liu Xia, Teng Li
- Plastic Surgery Hospital, Chinese Academy of Medical Sciences, Beijing 100043, China
-
Revised:2019-03-11Online:2019-07-28Published:2019-07-28 -
Contact:Liu Xia, MD, Associate researcher, Plastic Surgery Hospital, Chinese Academy of Medical Sciences, Beijing 100043, China; Teng Li, MD, Chief physician, Plastic Surgery Hospital, Chinese Academy of Medical Sciences, Beijing 100043, China -
About author:Sun Heng, Doctorate candidate, Plastic Surgery Hospital, Chinese Academy of Medical Sciences, Beijing 100043, China -
Supported by:the Medical and Health Science and Technology Innovation Project of Chinese Academy of Medical Sciences, No. 2017-I2M-1-007 (to JHY); the National Natural Science Foundation of China, No. 81471804 (to LX)
CLC Number:
Cite this article
Sun Heng, Ma Shize, Jiang Haiyue, Liu Xia, Teng Li. Three-dimensional dynamic culture of auricular chondrocytes with microcarriers in vitro[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(21): 3336-3341.
share this article
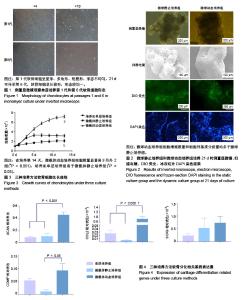
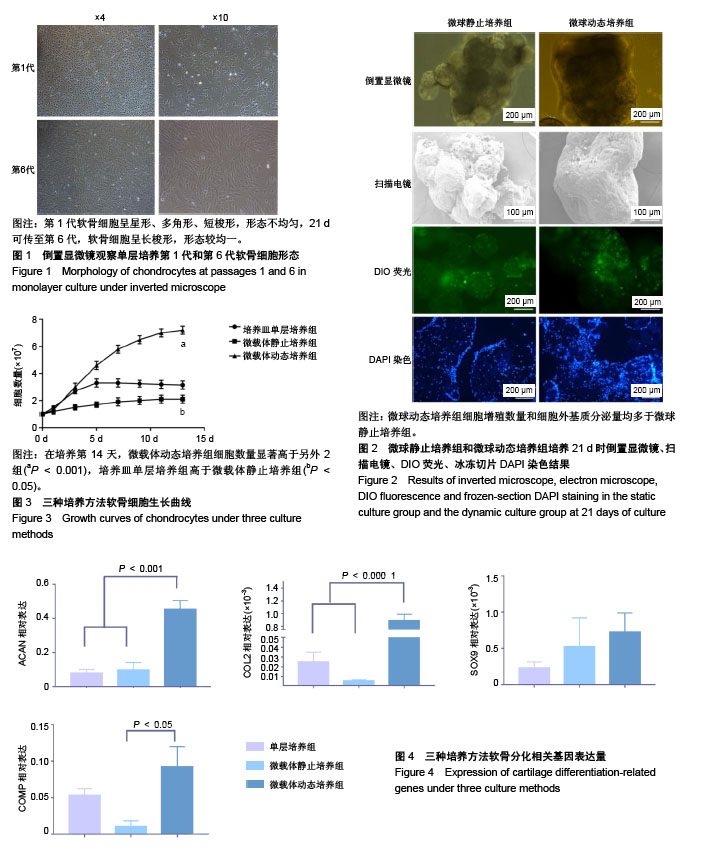
2.1 荧光倒置显微镜、冰冻切片DAPI染色、扫描电镜观察细胞生长情况 倒置显微镜下观察培养皿单层二维培养的细胞,第1代软骨细胞呈星形、多角形、短梭形,形态不均匀,21 d可传至第6代,软骨细胞呈长梭形,形态较均一,见图1。微载体培养时,软骨细胞可快速贴附于微载体表面,微载体静止培养21 d时软骨细胞外基质分泌增加,将微球包裹,聚集成团,而微球动态培养组的细胞外基质分泌量更多,微球之间结合更为牢固,见图2;扫描电镜下观察更为明显,微载体静止组微载体上的细胞量少,微球之间依靠细胞外基质部分相连,微球动态培养组细胞外基质将微球完全包裹,数个微球聚集成紧密的小团块。细胞膜绿色荧光染色和冰冻切片DAPI染色显示:微球中有细胞黏附,表面黏附的细胞更多。微载体动态培养组细胞数量多于微载体静止培养组,而且动态培养组细胞分布更为均匀,见图2。 2.2 增殖能力 如图3所示,培养皿单层培养2-4 d为细胞对数生长期,5 d时细胞量达到高峰;微载体动态培养组软骨细胞对数生长期延长为2-10 d,细胞数量在14 d达到高峰;微载体静止培养组细胞增殖速度缓慢。培养14 d时,培养皿单层培养细胞总量增加约3.3倍,微载体动态培养组细胞总量增加约7.3倍,微载体静止培养组细胞总量增加约2.2倍。在培养第14天,微载体动态培养组细胞数量显著高于另外2组(P < 0.001),培养皿单层培养组高于微载体静止培养组(P < 0.05)。 2.3 软骨细胞表型相关基因表达 各组软骨细胞培养 21 d时,软骨基质特异性基因ACAN和COL2相对表达量在微载体动态培养组表达最高,与其他2组比较差异有显著性意义。SOX9基因相对表达量在3组之间差异无显著性意义。COMP基因相对表达量在微载体动态培养组和微载体静止培养组之间差异有显著性意义,见图4。"
| [1] Macchiarini P, Jungebluth P, Go T, et al. Clinical transplantation of a tissue-engineered airway. Lancet. 2008;372(9655):2023-2030.[2] Huang BJ, Hu JC, Athanasiou KA. Cell-based tissue engineering strategies used in the clinical repair of articular cartilage. Biomaterials. 2016;98:1-22.[3] Stoddart MJ, Grad S, Eglin D, et al. Cells and biomaterials in cartilage tissue engineering. Regen Med. 2009;4(1):81-98.[4] Bichara DA, O'Sullivan NA, Pomerantseva I, et al. The tissue- engineered auricle: past, present, and future. Tissue Eng Part B Rev. 2012;18(1): 51-61.[5] Phull AR, Eo SH, Kim SJ. Oleanolic acid (OA) regulates inflammation and cellular dedifferentiation of chondrocytes via MAPK signaling pathways. Cell Mol Biol (Noisy-le-grand). 2017;63(3):12-17.[6] Beauchamp P, Moritz W, Kelm JM, et al. Development and Characterization of a Scaffold-Free 3D Spheroid Model of Induced Pluripotent Stem Cell-Derived Human Cardiomyocytes. Tissue Eng Part C Methods. 2015;21(8):852-861.[7] Berens EB, Holy JM, Riegel AT, et al. A Cancer Cell Spheroid Assay to Assess Invasion in a 3D Setting. J Vis Exp. 2015;(105):53409.[8] Bonnier F, Keating ME, Wróbel TP, et al. Cell viability assessment using the Alamar blue assay: a comparison of 2D and 3D cell culture models. Toxicol In Vitro. 2015;29(1):124-131.[9] Jiang HL, Kim YK, Cho KH, et al. Roles of spheroid formation of hepatocytes in liver tissue engineering. Int J Stem Cells.2010;3(2): 69-73.[10] Lee SA, No da Y, Kang E, et al. Spheroid-based three-dimensional liver-on-a-chip to investigate hepatocyte-hepatic stellate cell interactions and flow effects. Lab Chip. 2013;13(18):3529-3537.[11] Xie L, Mao M, Zhou L, et al. Signal Factors Secreted by 2D and Spheroid Mesenchymal Stem Cells and by Cocultures of Mesenchymal Stem Cells Derived Microvesicles and Retinal Photoreceptor Neurons. Stem Cells Int. 2017;2017:2730472.[12] 张启英. PLGA微球的制备及其在卵巢癌细胞三维培养中的应用研究[D].南京:东南大学, 2013.[13] 虞泽. nHAP/PLA中空多孔微球的制备及成骨细胞的响应[D]. 大连:大连理工大学,2016.[14] Kudva AK, Luyten FP, Patterson J. Initiating human articular chondrocyte re-differentiation in a 3D system after 2D expansion. J Mater Sci Mater Med. 2017;28(10):156.[15] Mujeeb A, Miller AF, Saiani A, et al. Self-assembled octapeptide scaffolds for in vitro chondrocyte culture. Acta Biomater. 2013;9(1): 4609-4617.[16] van Wezel AL. Growth of cell-strains and primary cells on micro-carriers in homogeneous culture. Nature. 1967;216(5110):64-65.[17] Ushida T, Furukawa K, Toita K, et al. Three-dimensional seeding of chondrocytes encapsulated in collagen gel into PLLA scaffolds. Cell Transplant. 2002;11(5):489-494.[18] Perka C, Schultz O, Spitzer RS, et al. Segmental bone repair by tissue-engineered periosteal cell transplants with bioresorbable fleece and fibrin scaffolds in rabbits. Biomaterials. 2000;21(11): 1145-1153.[19] Werner A, Duvar S, Müthing J, et al. Cultivation of immortalized human hepatocytes HepZ on macroporous CultiSpher G microcarriers. Biotechnol Bioeng. 2000;68(1):59-70.[20] Li P, Liu F, Wu C, et al. Feasibility of human hair follicle-derived mesenchymal stem cells/CultiSpher(®)-G constructs in regenerative medicine. Cell Tissue Res. 2015;362(1):69-86.[21] Phillips BW, Horne R, Lay TS, et al. Attachment and growth of human embryonic stem cells on microcarriers.J Biotechnol.2008;138(1-2):24-32.[22] Ng YC, Berry JM, Butler M. Optimization of physical parameters for cell attachment and growth on macroporous microcarriers. Biotechnol Bioeng.1996;50(6):627-635.[23] Bender MD, Bennett JM, Waddell RL, et al. Multi-channeled biodegradable polymer/CultiSpher composite nerve guides. Biomaterials. 2004;25(7-8):1269-1278.[24] Falk T, Congrove NR, Zhang S, et al. PEDF and VEGF-A output from human retinal pigment epithelial cells grown on novel microcarriers. J Biomed Biotechnol. 2012;2012:278932.[25] Melero-Martin JM, Dowling MA, Smith M, et al. Expansion of chondroprogenitor cells on macroporous microcarriers as an alternative to conventional monolayer systems. Biomaterials. 2006; 27(15): 2970-2979.[26] Yu C, Kornmuller A, Brown C, et al. Decellularized adipose tissue microcarriers as a dynamic culture platform for human adipose- derived stem/stromal cell expansion. Biomaterials. 2017;120:66-80.[27] Storm MP, Orchard CB, Bone HK, et al. Three-dimensional culture systems for the expansion of pluripotent embryonic stem cells. Biotechnol Bioeng. 2010;107(4):683-695.[28] 常彬,肖统光. Cultispher微载体构建组织工程软骨修复关节软骨缺损[J]. 中国组织工程研究, 2017,21(30):4793-4798.[29] Agrawal P, Pramanik K, Biswas A, et al. In vitro cartilage construct generation from silk fibroin- chitosan porous scaffold and umbilical cord blood derived human mesenchymal stem cells in dynamic culture condition. J Biomed Mater Res A. 2018;106(2):397-407.[30] Guo T, Yu L, Lim CG, et al. Effect of Dynamic Culture and Periodic Compression on Human Mesenchymal Stem Cell Proliferation and Chondrogenesis. Ann Biomed Eng. 2016;44(7):2103-2113.[31] Liu Q, Hu X, Zhang X, et al. Effects of mechanical stress on chondrocyte phenotype and chondrocyte extracellular matrix expression. Sci Rep. 2016;6:37268.[32] Carroll SF, Buckley CT, Kelly DJ. Cyclic hydrostatic pressure promotes a stable cartilage phenotype and enhances the functional development of cartilaginous grafts engineered using multipotent stromal cells isolated from bone marrow and infrapatellar fat pad. J Biomech. 2014;47(9):2115-2121.[33] Cao X, Xia H, Li N, et al. A mechanical refractory period of chondrocytes after dynamic hydrostatic pressure. Connect Tissue Res. 2015;56(3): 212-218.[34] Karkhaneh A, Naghizadeh Z, Shokrgozar MA, et al. Effects of hydrostatic pressure on biosynthetic activity during chondrogenic differentiation of MSCs in hybrid scaffolds. Int J Artif Organs. 2014;37(2):142-148.[35] Princz S, Wenzel U, Tritschler H, et al. Automated bioreactor system for cartilage tissue engineering of human primary nasal septal chondrocytes. Biomed Tech (Berl). 2017;62(5):481-486.[36] Khurshid M, Mulet-Sierra A, Adesida A, et al. Osteoarthritic human chondrocytes proliferate in 3D co-culture with mesenchymal stem cells in suspension bioreactors. J Tissue Eng Regen Med. 2018;12(3): e1418-e1432.[37] Bernhard JC, Hulphers E, Rieder B, et al. Perfusion Enhances Hypertrophic Chondrocyte Matrix Deposition, But Not the Bone Formation. Tissue Eng Part A. 2018;24(11-12):1022-1033.[38] Sheehy EJ, Buckley CT, Kelly DJ. Chondrocytes and bone marrow-derived mesenchymal stem cells undergoing chondrogenesis in agarose hydrogels of solid and channelled architectures respond differentially to dynamic culture conditions. J Tissue Eng Regen Med. 2011;5(9):747-758. [39] Lin YC, Hall AC, Simpson AHRW. A novel organ culture model of a joint for the evaluation of static and dynamic load on articular cartilage. Bone Joint Res. 2018;7(3):205-212.[40] Chen CH, Kuo CY, Chen JP. Effect of Cyclic Dynamic Compressive Loading on Chondrocytes and Adipose-Derived Stem Cells Co-Cultured in Highly Elastic Cryogel Scaffolds. Int J Mol Sci. 2018;19(2): E370. |
| [1] | Li Cai, Zhao Ting, Tan Ge, Zheng Yulin, Zhang Ruonan, Wu Yan, Tang Junming. Platelet-derived growth factor-BB promotes proliferation, differentiation and migration of skeletal muscle myoblast [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1050-1055. |
| [2] | Liu Cong, Liu Su. Molecular mechanism of miR-17-5p regulation of hypoxia inducible factor-1α mediated adipocyte differentiation and angiogenesis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1069-1074. |
| [3] | Ma Zetao, Zeng Hui, Wang Deli, Weng Jian, Feng Song. MicroRNA-138-5p regulates chondrocyte proliferation and autophagy [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 674-678. |
| [4] | Xie Chongxin, Zhang Lei. Comparison of knee degeneration after anterior cruciate ligament reconstruction with or without remnant preservation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(5): 735-740. |
| [5] | Wang Yujiao, Liu Dan, Sun Song, Sun Yong. Biphasic calcium phosphate loaded with advanced platelet rich fibrin can promote the activity of rabbit bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 504-509. |
| [6] | Zhou Jihui, Yao Meng, Wang Yansong, Li Xinzhi, Zhou You, Huang Wei, Chen Wenyao. Influence of novel nanoscaffolds on biological behaviors of neural stem cells and the related gene expression [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(4): 532-536. |
| [7] | Chen Yang, Huang Denggao, Gao Yuanhui, Wang Shunlan, Cao Hui, Zheng Linlin, He Haowei, Luo Siqin, Xiao Jingchuan, Zhang Yingai, Zhang Shufang. Low-intensity pulsed ultrasound promotes the proliferation and adhesion of human adipose-derived mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(25): 3949-3955. |
| [8] | Zhou Wu, Wang Binping, Wang Yawen, Cheng Yanan, Huang Xieshan. Transforming growth factor beta combined with bone morphogenetic protein-2 induces the proliferation and differentiation of mouse MC3T3-E1 cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(23): 3630-3635. |
| [9] | Tong Jie, Liao Ying, Chen Zhengyu, Sun Guanghua . Osteoarthritic chondrocyte autophagy and regulation of mitogen-activated protein kinase signaling pathway [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(20): 3246-3251. |
| [10] | Yu Chengshuai, Du Gang, Pang Shenning, Lao Shan. Chemerin, a pro-inflammatory adipokine, regulates chondrocyte proliferation and metabolism by increasing production of nitric oxide [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(2): 258-263. |
| [11] | Dai Yaling, Chen Lewen, He Xiaojun, Lin Huawei, Jia Weiwei, Chen Lidian, Tao Jing, Liu Weilin. Construction of miR-146b overexpression lentiviral vector and the effect on the proliferation of hippocampal neural stem cells [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(19): 3024-3030. |
| [12] | Ailimaierdan·Ainiwaer, Wang Ling, Gu Li, Dilidaer•Taxifulati, Wang Shan, Yin Hongbin. Effect of transforming growth factor-beta3 on the proliferation and osteogenic capability of osteoblasts [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(17): 2664-2669. |
| [13] | Wang Renxian, Cao Jingjing, Wang Honggang, Wan Ben, Liu Weifeng. Effects of dispersants on aggregation, intracellular distribution and cell proliferation of nano-hydroxyapatite [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(16): 2500-2505. |
| [14] | Li Shao, Liang Yongkang, Gao Yi, Peng Qing. Establishment and functional in vitro characteristics of three-dimensional collagen HepaRG microsphere [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(16): 2541-2547. |
| [15] | Wu Yukun, Han Jie, Wen Shuaibo. Mechanism of Runx2 gene in fracture healing [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(14): 2274-2279. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||