Chinese Journal of Tissue Engineering Research ›› 2018, Vol. 22 ›› Issue (15): 2321-2326.doi: 10.3969/j.issn.2095-4344.0730
Previous Articles Next Articles
Efficacy and safety of aspirin for venous thromboembolism after total knee arthroplasty
Zhang Hang, Zhang Zhi-qiang, He Qiang, He Yun-li, Zhang Qian, Feng Zhe, Li Yan, He Sen
- Department of Orthopedics, Beichen Hospital, Tianjin 300400, China
-
Online:2018-05-28Published:2018-05-28 -
Contact:He Sen, Master, Associate chief physician, Department of Orthopedics, Beichen Hospital, Tianjin 300400, China -
About author:Zhang Hang, Master, Physician, Department of Orthopedics, Beichen Hospital, Tianjin 300400, China
CLC Number:
Cite this article
Zhang Hang, Zhang Zhi-qiang, He Qiang, He Yun-li, Zhang Qian, Feng Zhe, Li Yan, He Sen. Efficacy and safety of aspirin for venous thromboembolism after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2018, 22(15): 2321-2326.
share this article
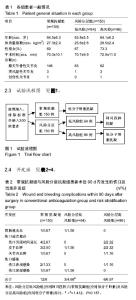
2.1 参与者数量分析 收集初次行单侧全膝关节置换患者378例,根据纳入、排除标准共纳入300例患者,按入院顺序用随机数字表法分为常规抗凝治疗组150例和风险分层组150例,根据VTE风险分层标准将风险风层组分为低风险组64例,高风险组86例,按意向性处理,均进入结果分析。 2.2 两组患者基线资料分析 常规抗凝组平均年龄(64.5±6.3)岁,风险分层低风险组平均年龄(63.8±5.5)岁,风险分层高风险组平均年龄(64.1±6.2)岁,组间相比差异无显著性意义。常规抗凝组平均体质量指数为(27.3±2.9) kg/m2,风险分层低风险组平均体质量指数为(25.6±2.6) kg/m2,风险分层高风险组平均体质量指数为(28.5±2.4) kg/m2,低风险组与高风险组相比,差异有显著性意义(t=10.489,P=0.000)。 两组性别女比率及手术时间相比差异无显著性意义(P > 0.05)。见表1。"
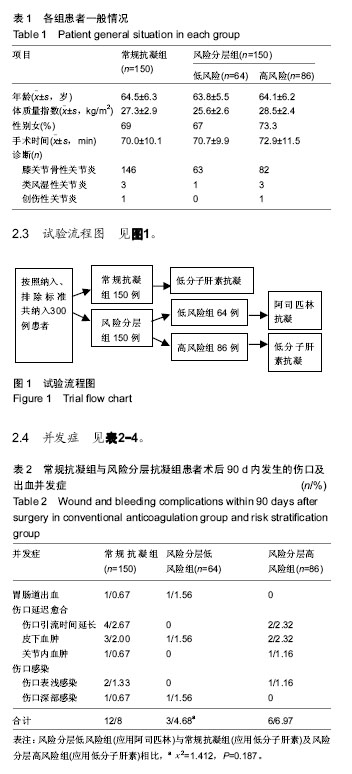
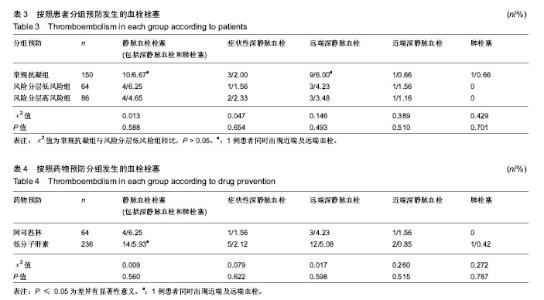
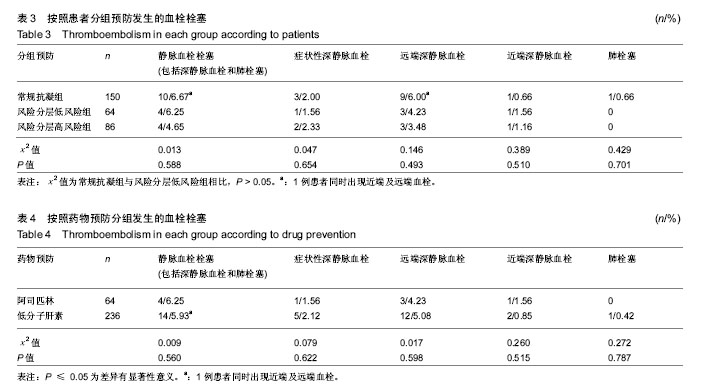
随访术后90 d内共有39例(13%)出现并发症。其中症状性下肢深静脉血栓并发症的总发生率为2%(6/300),伤口并发症的发生率为6.3%(19/300)。 常规抗凝组和风险分层组各有3例(2%,3/150)发生症状性下肢深静脉血栓。 接受低分子量肝素与阿司匹林作为药物血栓预防的患者具有相似的静脉血栓栓塞发生率(5.93%∶6.25%)。 常规抗凝组患者发生VTE(包括深静脉血栓和肺栓塞)10例,其中3例症状性下肢深静脉血栓(2%,3/150),1例近端深静脉血栓(0.66%,1/150),8例远端及肌间深静脉血栓(5.33%,8/150);1例肺栓塞(0.66%,1/150)。 风险分层低风险组患者发生VTE(包括深静脉血栓和肺栓塞)4例,其中1例症状性下肢深静脉血栓(1.56%,1/64),1例近端深静脉血栓(1.56%,1/64),3例远端及肌间深静脉血栓(4.23%,3/64);没有发生肺栓塞。 风险分层高风险组患者发生VTE(包括深静脉血栓和肺栓塞)4例,其中2例症状性下肢深静脉血栓(2.33%,2/86),1例近端深静脉血栓(1.16%,1/86),3例远端及肌间深静脉血栓(3.48%,3/86);没有发生肺栓塞。 常规抗凝组与风险分层低风险组两组总体下肢深静脉血栓发生率、远端深静脉血栓发生率和肌间深静脉血栓发生率差异无显著性意义(P > 0.05)。 常规抗凝组共计1例死亡,膝关节置换后突发心肌梗死。1例疑似肺栓塞病例,经查肺血管CTA为阴性,转入ICU后好转出院。 常规抗凝组伤口并发症11例(发生率7.33%),而风险分层组8例(发生率5.33%),差异无显著性意义(χ2=506,P=0.318)。风险分层低风险组患者伤口延迟愈合、表浅伤口感染和深部伤口感染发生率分别为1.56%(1/64),0%(0/64),1.56%(1/64),风险分层高风险组分别为5.81%(5/86),1.16%(1/86),0%(0/86),而常规抗凝组分别为5.33%(8 /150),1.33%(2/150)和0.67%(1/150)。 按照药物分组接受阿司匹林治疗的患者伤口延迟愈合、表浅伤口感染和深部伤口感染发生率分别为1.56%(1例),0%,1.56%(1例),接受低分子量肝素治疗的患者分别为5.51%(13例),1.27%(3例)和0.42%(1例)。 3例伤口表浅感染患者经过手术室清创、伤口换药痊愈,2例伤口深部感染患者均通过一期骨水泥假体植入,二期行膝关节假体翻修术。 "
| [1] 杨庆铭,王鸿利.骨科大手术后静脉血栓栓塞症预防的临床趋势[J].中华骨科杂志, 2015,35(11):1121-1128.[2] Dorr LD, Gendelman V, Maheshwari AV, et al. Multimodal thromboprophylaxis for total hip and knee arthroplasty based on risk assessment. J Bone Joint Surg Am. 2007;89(12):2648-2657.[3] 彭慧明,翁习生,翟吉良,等.初次全膝关节成形术后常规抗凝患者症状性静脉血栓症发生率的调查研究[J].中华骨与关节外科, 2014, 7(2):101-104. [4] Suen K, Westh RN, Churilov L, et al. Low-molecular-weight heparin and the relative risk of surgical site bleeding complications: results of a systematic review and meta-analysis of randomized controlled trials of venous thromboprophylaxis in patients after total joint arthroplasty. J Arthroplasty. 2017;32(9): 2911-2919.e6.[5] Patel VP, Walsh M, Sehgal B, et al. Factors associated with prolonged wound drainage after primary total hip and knee arthroplasty. J Bone Joint Surg Am. 2007;89(1):33-38. [6] Huang RC, Parvizi J, Hozack WJ, et al. Aspirin is as effective as and safer than warfarin for patients at higher risk of venous thromboembolism undergoing total joint arthroplasty. J Arthroplasty. 2016;31(9 Suppl):83-86. [7] Drescher FS, Sirovich BE, Lee A, et al. Aspirin versus anticoagulation for prevention of venous thromboembolism major lower extremity orthopedic surgery: a systematic review and meta-analysis. J Hosp Med. 2014;9(9):579-585.[8] Lieberman JR, Pensak MJ. Prevention of venous thromboembolic disease after total hip and knee arthroplasty. J Bone Joint Surg Am. 2013;95(19):1801-1811.[9] Chu JN, Maselli J, Auerbach AD, et al. The risk of venous thromboembolism with aspirin compared to anticoagulants after hip and knee arthroplasty. Thromb Res. 2017;155:65-71.[10] Deirmengian GK, Heller S, Smith EB, et al. Aspirin can be used as prophylaxis for prevention of venous thromboembolism after revision hip and knee arthroplasty. J Arthroplasty. 2016;31(10): 2237-2240.[11] Raphael IJ, Tischler EH, Huang R, et al. Aspirin: an alternative for pulmonary embolism prophylaxis after arthroplasty. Clin Orthop Relat Res. 2014;472(2):482-488.[12] Jameson SS, Charman SC, Gregg PJ, et al. The effect of aspirin and low-molecular-weight heparin on venous thromboembolism after hip replacement: a non-randomised comparison from information in the National Joint Registry. J Bone Joint Surg Br. 2011;93(11):1465-1470.[13] Cafri G, Paxton EW, Chen Y, et al. Comparative effectiveness and safety of drug prophylaxis for prevention of venous thromboembolism after total knee arthroplasty. J Arthroplasty. 2017;32(11):3524-3528.e1.[14] Bala A, Huddleston JI 3rd, Goodman SB, et al. Venous thromboembolism prophylaxis after TKA: aspirin, warfarin, enoxaparin, or factor Xa inhibitors. Clin Orthop Relat Res. 2017; 475(9):2205-2213.[15] Nielen JT, Dagnelie PC, Emans PJ, et al. Safety and efficacy of new oral anticoagulants and low-molecular-weight heparins compared with aspirin in patients undergoing total knee and hip replacements. Pharmacoepidemiol Drug Saf. 2016;25(11): 1245-1252.[16] Odeh K, Doran J, Yu S, et al. Risk-stratified venous thromboembolism prophylaxis after total joint arthroplasty: aspirin and sequential pneumatic compression devices vs aggressive chemoprophylaxis. J Arthroplasty. 2016;31(9 Suppl):78-82.[17] 中华医学会骨科学分会.骨关节炎诊治指南(2007年版)[J].中华关节外科杂志:电子版,2007,1(4):280-283.[18] González Della Valle A, Serota A, Go G, et al. Venous thromboembolism is rare with a multimodal prophylaxis protocol after total hip arthroplasty. Clin Orthop Relat Res. 2006;444: 146-153.[19] Dorr LD, Gendelman V, Maheshwari AV, et al. Multimodal thromboprophylaxis for total hip and knee arthroplasty based on risk assessment. J Bone Joint Surg Am. 2007;89(12):2648-2657.[20] Parvizi J, Smith EB, Pulido L, et al. The rise in the incidence of pulmonary embolus after joint arthroplasty: is modern imaging to blame. Clin Orthop Relat Res. 2007;463:107-113.[21] Parvizi J, Huang R, Rezapoor M, et al. Individualized risk model for venous thromboembolism after total joint arthroplasty. J Arthroplasty. 2016;31(9 Suppl):180-186.[22] Ogonda L, Hill J, Doran E, et al. Aspirin for thromboprophylaxis after primary lower limb arthroplasty: early thromboembolic events and 90 day mortality in 11,459 patients. Bone Joint J.2016; 98-B (3):341-348.[23] 钱文伟,翁习生,常晓,等.人工髋关节置换后深静脉血栓形成影响因素的回顾分析[J].中国组织工程研究,2012,16(4):622-625.[24] Sharrock NE, Gonzalez Della Valle A, Go G, et al. Potent anticoagulants are associated with a higher all-cause mortality rate after hip and knee arthroplasty. Clin Orthop Relat Res. 2008; 466(3):714-721.[25] Huang R, Buckley PS, Scott B, et al. Administration of aspirin as a prophylaxis agent against venous thromboembolism results in lower incidence of periprosthetic joint infection. J Arthroplasty. 2015;30(9 Suppl):39-41. [26] Markel DC, York S, Liston MJ Jr, et al. Venous thromboembolism: management by American Association of Hip and Knee Surgeons. J Arthroplasty. 2010;25(1):3-9.e1-2.[27] Devereaux PJ, Mrkobrada M, Sessler DI, et al. Aspirin in patients undergoing noncardiac surgery. N Engl J Med. 2014;370(16): 1494-1503.[28] Ozbudak O, Ero?ullari I, O?ü? C, et al. Doppler ultrasonography versus venography in the detection of deep vein thrombosis in patients with pulmonary embolism. J Thromb Thrombolysis. 2006;21(2):159-162.[29] Colwell CW Jr, Froimson MI, Mont MA, et al. Thrombosis prevention after total hip arthroplasty: a prospective, randomized trial comparing a mobile compression device with low-molecular- weight heparin. J Bone Joint Surg Am. 2010;92(3):527-535.[30] Jiang Y, Du H, Liu J, et al. Aspirin combined with mechanical measures to prevent venous thromboembolism after total knee arthroplasty: a randomized controlled trial. Chin Med J (Engl). 2014;127(12):2201-2205.[31] Parvizi J, Huang R, Restrepo C, et al. Low-dose aspirin is effective chemoprophylaxis against clinically important venous thromboembolism following total joint arthroplasty: a preliminary analysis. J Bone Joint Surg Am. 2017;99(2):91-98.[32] Khatod M, Inacio MC, Bini SA, et al. Pulmonary embolism prophylaxis in more than 30,000 total knee arthroplasty patients: is there a best choice. J Arthroplasty. 2012;27(2):167-172. |
| [1] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [2] | Zhang Tongtong, Wang Zhonghua, Wen Jie, Song Yuxin, Liu Lin. Application of three-dimensional printing model in surgical resection and reconstruction of cervical tumor [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1335-1339. |
| [3] | Zhang Yu, Tian Shaoqi, Zeng Guobo, Hu Chuan. Risk factors for myocardial infarction following primary total joint arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1340-1345. |
| [4] | Li Dadi, Zhu Liang, Zheng Li, Zhao Fengchao. Correlation of total knee arthroplasty efficacy with satisfaction and personality characteristics [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1346-1350. |
| [5] | Wei Wei, Li Jian, Huang Linhai, Lan Mindong, Lu Xianwei, Huang Shaodong. Factors affecting fall fear in the first movement of elderly patients after total knee or hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1351-1355. |
| [6] | Wang Jinjun, Deng Zengfa, Liu Kang, He Zhiyong, Yu Xinping, Liang Jianji, Li Chen, Guo Zhouyang. Hemostatic effect and safety of intravenous drip of tranexamic acid combined with topical application of cocktail containing tranexamic acid in total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1356-1361. |
| [7] | Xiao Guoqing, Liu Xuanze, Yan Yuhao, Zhong Xihong. Influencing factors of knee flexion limitation after total knee arthroplasty with posterior stabilized prostheses [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1362-1367. |
| [8] | Huang Zexiao, Yang Mei, Lin Shiwei, He Heyu. Correlation between the level of serum n-3 polyunsaturated fatty acids and quadriceps weakness in the early stage after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1375-1380. |
| [9] | Zhang Chong, Liu Zhiang, Yao Shuaihui, Gao Junsheng, Jiang Yan, Zhang Lu. Safety and effectiveness of topical application of tranexamic acid to reduce drainage of elderly femoral neck fractures after total hip arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1381-1386. |
| [10] | Yuan Jiawei, Zhang Haitao, Jie Ke, Cao Houran, Zeng Yirong. Underlying targets and mechanism of Taohong Siwu Decoction in prosthetic joint infection on network pharmacology [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1428-1433. |
| [11] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [12] | Zeng Yanhua, Hao Yanlei. In vitro culture and purification of Schwann cells: a systematic review [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1135-1141. |
| [13] | Zhong Hehe, Sun Pengpeng, Sang Peng, Wu Shuhong, Liu Yi. Evaluation of knee stability after simulated reconstruction of the core ligament of the posterolateral complex [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 821-825. |
| [14] | Zhao Zhongyi, Li Yongzhen, Chen Feng, Ji Aiyu. Comparison of total knee arthroplasty and unicompartmental knee arthroplasty in treatment of traumatic osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 854-859. |
| [15] | Liu Shaohua, Zhou Guanming, Chen Xicong, Xiao Keming, Cai Jian, Liu Xiaofang. Influence of anterior cruciate ligament defect on the mid-term outcome of fixed-bearing unicompartmental knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 860-865. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||