Chinese Journal of Tissue Engineering Research ›› 2026, Vol. 30 ›› Issue (27): 7044-7052.doi: 10.12307/2026.299
Efficacy and biomechanical analysis of L-shaped plate treatment for osteoporotic Schatzker type II tibial plateau fractures
Shi Gaolong, Hu Zhenghui, Ling Zhuoyan, Xie Zonggang
- Department of Orthopedics, The Second Affiliated Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China
-
Received:2025-09-29Accepted:2025-12-16Online:2026-09-28Published:2026-04-17 -
Contact:Xie Zonggang, MD, Chief physician, Department of Orthopedics, The Second Affiliated Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China -
About author:Shi Gaolong, MS, Attending physician, Department of Orthopedics, The Second Affiliated Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China Hu Zhenghui, MS, Physician, Department of Orthopedics, The Second Affiliated Hospital of Soochow University, Suzhou 215000, Jiangsu Province, China Shi Gaolong and Hu Zhenghui contributed equally to this article. -
Supported by:National Natural Science Foundation of China, No. 81974334 (to XZG)
CLC Number:
Cite this article
Shi Gaolong, Hu Zhenghui, Ling Zhuoyan, Xie Zonggang. Efficacy and biomechanical analysis of L-shaped plate treatment for osteoporotic Schatzker type II tibial plateau fractures[J]. Chinese Journal of Tissue Engineering Research, 2026, 30(27): 7044-7052.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks

2.1 回顾性分析结果 2.1.1 参与者数量分析 研究期内共筛选236例骨质疏松性Schatzker Ⅱ型累及后外侧胫骨平台骨折患者,依据既定纳入/排除标准排除197例,其中不符合骨质疏松标准(T值> -2.5)42例、未完成骨密度检测58例、骨折类型不符(非Schatzker Ⅱ型或未累及后外侧胫骨平台)36例、随访不足12个月或资料不完整52例、合并其他严重骨折/全身性疾病6例、术前存在严重膝关节畸形3例,最终纳入39例患者进入统计分析,分为L型钢板组(单纯外侧L型钢板固定,n=24)及联合组(外侧L型钢板联合后方T型钢板固定,n=15)。所有纳入者均完成12个月以上随访,无脱落/失访。 2.1.2 基线资料比较 L型钢板组和联合组患者在基线特征上无显著性差异(P > 0.05)。但L型钢板组手术时间和术中出血量显著少于联合组(P < 0.000 1)。两组术前骨密度(腰椎L1-L4或股骨颈)及胫骨平台塌陷值、受伤至手术时间相比均无显著性差异 (P > 0.05)。详见表4。"
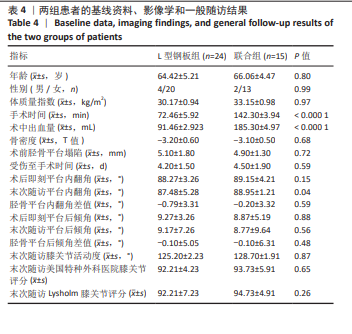

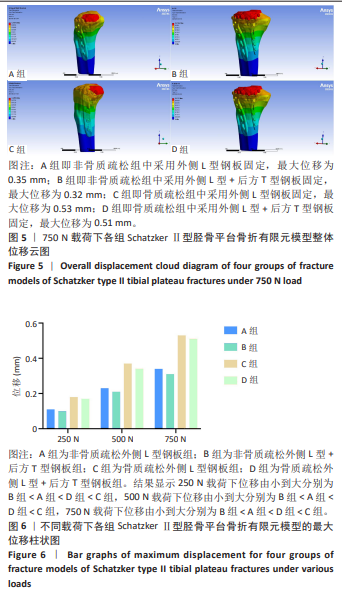
2.1.3 影像学指标比较 平台内翻角:术后即刻两组比较无显著性差异(P=0.15);末次随访L型钢板组平台内翻角小于联合组(P=0.04)。组内对比显示,L型钢板组术后即刻与末次随访无显著变化(P=0.154),联合组亦无显著变化(P=0.230)。L型钢板组术后即刻和末次随访内翻角差值为(-0.79±3.31) °,联合组为(-0.20±3.32) °,两组差值相比无显著性差异(P=0.59)。 平台后倾角:术后即刻两组比较无显著性差异(P=0.88);末次随访两组仍无显著性差异(P=1.56)。组内对比显示,L型钢板组术后即刻与末次随访无显著变化(P=0.278),联合组亦无显著变化(P=0.12)。L型钢板组术后即刻和末次随访后倾角差值为(-0.10±5.05)°,联合组为(-0.10±6.31)°,两组差值相比无显著性差异(P=0.48)。 2.1.4 功能结局比较 末次随访时,两组患者的膝关节活动度、美国特种外科医院评分、Lysholm膝关节评分相比均无显著性差异(P=0.87,0.65,0.26),说明两组功能评分均无显著差异。 2.1.5 术后并发症 两组患者术后均未发生重大并发症。具体而言,两组患者均未出现感染病例,1例L型钢板组患者使用抗生素6 d,后期无感染迹象。两组患者均无深静脉血栓发生,无内固定失败或移位塌陷超过2 mm以上病例。 2.2 有限元分析结果 2.2.1 不同载荷条件下整体的位移云图 图5显示了4组整体模型的位移趋势分布。非骨质疏松骨中,750 N下B组(外侧L型+后方T型钢板组)0.32 mm低于A组(L型钢板组)0.35 mm;骨质疏松骨中,750 N下D组(外侧L型+后方T型钢板组)0.51 mm低于C组(L型钢板组)0.53 mm。整体表现在750 N载荷条件下位移大小分别为B组 < A组 < D组 < C组, 250 N和500 N载荷位移趋势相似。详见图6及表5。 2.2.2 不同载荷条件下胫骨的von Mises应力云图 图7显示了4组胫骨模型的von Mises应力趋势分布。非骨质疏松骨中,750 N 下B组(外侧L型+后方T型钢板组)101 MPa低于A组(L型钢板组)223 MPa;骨质疏松骨中,750 N下D组(外侧L型+后方T型钢板组)101 MPa低于C组(L型钢板组)189 MPa。整体表现在750 N载荷条件下胫骨的最大von Mises应力大小为D组=B组 < C组 < A组。详见图8及表5。"
| [1] BOONEN S, DEJAEGER E, VANDERSCHUEREN D, et al. Osteoporosis and osteoporotic fracture occurrence and prevention in the elderly: a geriatric perspective. Best Pract Res Clin Endocrinol Metab. 2008;22(5):765-785. [2] SAUHTA R, MAKKAR D. Proximal Tibia Fractures in Osteoporosis. Indian J Orthop. 2025;59(3):326-345. [3] SUN H, ZHAI QL, XU YF, et al. Combined approaches for fixation of Schatzker type II tibial plateau fractures involving the posterolateral column: a prospective observational cohort study. Arch Orthop Trauma Surg. 2015; 135(2):209-221. [4] BAGHERIFARD A, MIRKAMALI SF, RASHIDI H, et al. Functional outcomes and quality of life after surgically treated tibial plateau fractures. BMC Psychol. 2023;11(1):146. [5] ZHU Z, WANG H, KANG R, et al. Impact of systematic postoperative rehabilitation training on prognosis in patients with osteoporosis and tibial plateau fractures: a retrospective study. Curr Probl Surg. 2025;64:101729. [6] ROHRA N, SURI HS, GANGRADE K, et al. Functional and radiological outcome of Schatzker type V and VI tibial plateau fracture treatment with dual plates with minimum 3 years follow-up: a prospective study. J Clin Diagn Res. 2016;10(5):RC05-10. [7] LEE MH, HSU CJ, LIN KC, et al. Comparison of outcome of unilateral locking plate and dual plating in the treatment of bicondylar tibial plateau fractures. J Orthop Surg Res. 2014;9:62. [8] YAO Y, LV H, ZAN J, et al. A comparison of lateral fixation versus dual plating for simple bicondylar fractures. Knee. 2015;22(3):225-229. [9] CITAK C, KAYALI C, OZAN F, et al. Lateral locked plating or dual plating: a comparison of two methods in simple bicondylar tibial plateau fractures. Clin Orthop Surg. 2019;11(2):151-158. [10] HUANG X, ZHI Z, YU B, et al. Stress and stability of plate-screw fixation and screw fixation in the treatment of Schatzker type IV medial tibial plateau fracture: a comparative finite element study. J Orthop Surg Res. 2015;10:182. [11] ABDUL WAHAB AH, WUI NB, ABDUL KADIR MR, et al. Biomechanical evaluation of three different configurations of external fixators for treating distal third tibia fracture: finite element analysis in axial, bending and torsion load. Comput Biol Med. 2020;127:104062. [12] DEHOUST J, MÜNCH M, SEIDE K, et al. Biomechanical aspects of the posteromedial split in bicondylar tibial plateau fractures: a finite-element investigation. Eur J Trauma Emerg Surg. 2020;46(6):1257-1266. [13] JIANG J, XU D, JI Z, et al. Application of a combined cancellous lag screw enhances the stability of locking plate fixation of osteoporotic lateral tibial plateau fracture by providing interfragmentary compression force. J Orthop Surg Res. 2024;19(1):139. [14] ZHAO G, LUO J, MA J, et al. Decreased stress shielding with poly-ether-ether-ketone tibial implant for total knee arthroplasty: a preliminary study using finite element analysis. Heliyon. 2024;10(5):e27204. [15] WANG Y, LUO C, ZHU Y, et al. Updated Three-Column Concept in surgical treatment for tibial plateau fractures – A prospective cohort study of 287 patients. Injury. 2016;47(7):1488-1496. [16] HU Z, REN W, ZHANG W, et al. Potential problem and solution of lateral plate postposition for the posterolateral tibial plateau fracture. J Orthop Surg Res. 2023;18(1):984. [17] 胡正辉, 张文, 衡红全, 等. 后外侧胫骨平台骨折应用万向螺钉的有限元分析[J]. 中国组织工程研究,2025,29(27):5735-5742. [18] LIU S, QI W, ZHANG Y, et al. Effect of bone material properties on effective region in screw-bone model: an experimental and finite element study. Biomed Eng Online. 2014;13:83. [19] HASHEMI A, SHIRAZI-ADL A. Finite element analysis of tibial implants: effect of fixation design and friction model. Comput Methods Biomech Biomed Engin. 2000;3(3):183-201. [20] ELSOE R, LARSEN P, NIELSEN NP, et al. Population-based epidemiology of tibial plateau fractures. Orthopedics. 2015;38(9):e780-786. [21] BORMANN M, NEIDLEIN C, GASSNER C, et al. Changing patterns in the epidemiology of tibial plateau fractures: a 10-year review at a level-I trauma center. Eur J Trauma Emerg Surg. 2023;49(1):401-409. [22] HE QF, SUN H, SHU LY, et al. Tibial plateau fractures in elderly people: an institutional retrospective study. J Orthop Surg Res. 2018;13(1):276. [23] ANEJA A, TEASDALL RJ, GRAVES ML. Biomechanics of osteoporotic fracture care: advances in locking plate and intramedullary nail technology. J Orthop Trauma. 2021;35(Suppl 5):S1-S5. [24] JIANG W, LIU X, KONG XR, et al. Treatment of a collapse fracture of the anterolateral tibial plateau with a lateral locking plate and the Jail screw technique. BMC Surg. 2025;25(1):22. [25] WISANUYOTIN T, PAHOLPAK P, SIRICHATIVAPEE W, et al. Effect of bone cement augmentation with different configurations of the dual locking plate for femoral allograft fixation: finite element analysis and biomechanical study. J Orthop Surg Res. 2023;18(1):405. [26] WISANUYOTIN T, SIRICHATIVAPEE W, PAHOLPAK P, et al. Optimal configuration of a dual locking plate for femoral allograft or recycled autograft bone fixation: a finite element and biomechanical analysis. Clin Biomech (Bristol). 2020;80:105156. [27] BLAŽEVIĆ D, KODVANJ J, ADAMOVIĆ P, et al. Comparison between external locking plate fixation and conventional external fixation for extraarticular proximal tibial fractures: a finite element analysis. J Orthop Surg Res. 2022;17(1):16. [28] REN W, ZHANG W, JIANG S, et al. The study of biomechanics and clinical anatomy on a novel plate designed for posterolateral tibial plateau fractures via anterolateral approach. Front Bioeng Biotechnol. 2022;10:818610. [29] JIANG J, XU D, JI Z, et al. Interfragmentary compression force and fixation stability of lateral tibial plateau fractures in normal and osteoporotic bones. J Orthop Res. 2024;42(8):1738-1747. [30] SOLIMAN MM, CHOWDHURY MEH, ISLAM MT, et al. A review of biomaterials and associated performance metrics analysis in pre-clinical finite element model and in implementation stages for total hip implant system. Polymers (Basel). 2022;14(20):4308. [31] LOISEL F, BOURGEOIS M, RONDOT T, et al. Treatment goals for distal radius fractures in 2018: recommendations and practical advice. Eur J Orthop Surg Traumatol. 2018;28(8):1465-1468. |
| [1] | Zhang Zizheng, Luo Wang, Liu Changlu. Application value of finite element analysis on unicompartmental knee arthroplasty for medial knee compartmental osteoarthritis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2313-2322. |
| [2] | Chen Huiting, Zeng Weiquan, Zhou Jianhong, Wang Jie, Zhuang Congying, Chen Peiyou, Liang Zeqian, Deng Weiming. Tail anchoring technique of vertebroplasty in treatment of osteoporotic vertebral compression fractures with intravertebral cleft: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2145-2152. |
| [3] | Zeng Xuan, Weng Rui, Ye Shicheng, Tang Jiadong, Mo Ling, Li Wenchao. Two lumbar rotary manipulation techniques in treating lumbar disc herniation: a finite element analysis of biomechanical differences [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2153-2161. |
| [4] | Cheng Qisheng, Julaiti·Maitirouzi, Xiao Yang, Zhang Chenwei, Paerhati·Rexiti. Finite element analysis of novel variable-diameter screws in modified cortical bone trajectory of lumbar vertebrae [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2162-2171. |
| [5] | Liu Jiafu, Ren Ruxia, Liao Zhouwei, Zhou Xiali, Wu Yihong, Zhang Shaoqun. Three-dimensional finite element analysis of cervical spine biomechanical characteristics in a rat model of cervical vertigo [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2182-2190. |
| [6] | Liu Wenlong, Dong Lei, Xiao Zhengzheng, Nie Yu. Finite element analysis of tibial prosthesis loosening after fixed-bearing unicompartmental knee arthroplasty for osteoporosis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2191-2198. |
| [7] | Zheng Wangyang, Fei Ji, Yang Di, Zhao Lang, Wang Lingli, Liu Peng, Li Haiyang. Finite element analysis of the force changes of the supraspinatus tendon and glenohumeral joint during the abduction and flexion of the humerus [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2199-2207. |
| [8] | Cai Qirui, Dai Xiaowei, Zheng Xiaobin, Jian Sili, Lu Shaoping, Liu Texi, Liu Guoke, Lin Yuanfang. Mechanical effects of Long’s traction orthopedic method on cervical functional units: quantitative analysis of biomechanical model of head and neck [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2208-2216. |
| [9] | Rao Jingcheng, Li Yuwan, Zheng Hongbing, Xu Zhi, Zhu Aixiang, Shi Ce, Wang Bing, Yang Chun, Kong Xiangru, Zhu Dawei. Biomechanical differences between the new proximal femoral stable intramedullary nail and traditional intramedullary nail#br# [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2217-2225. |
| [10] | Chen Long, Wang Xiaozhen, Xi Jintao, Lu Qilin. Biomechanical performance of short-segment screw fixation combined with expandable polyetheretherketone vertebral body replacement in osteoporotic vertebrae [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(9): 2226-2235. |
| [11] | Zheng Xuying, Hu Hongcheng, Xu Libing, Han Jianmin, Di Ping. Stress magnitude and distribution in two-piece cement-retained zirconia implants under different loading conditions and with varying internal connection shapes [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(8): 1979-1987. |
| [12] | Hu Xiongke, Liu Shaohua, Tan Qian, Liu Kun, Zhu Guanghui. Shikonin intervention with bone marrow mesenchymal stem cells improves microstructure of femur in aged mice [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(7): 1609-1615. |
| [13] | Wen Guangwei, Zhen Yinghao, Zheng Taikeng, Zhou Shuyi, Mo Guoye, Zhou Tengpeng, Li Haishan, Lai Yiyi. Effects and mechanisms of isoginkgetin on osteoclastogenesis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1348-1358. |
| [14] | Xu Hao, Ding Lu, Li Xiao. Mechanical effect of mechanical wear of abutment screws on the Morse taper connection implant system: a three-dimensional finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1375-1383. |
| [15] | Wu Zhilin, , He Qin, Wang Pingxi, Shi Xian, Yuan Song, Zhang Jun, Wang Hao . DYRK2: a novel therapeutic target for rheumatoid arthritis combined with osteoporosis based on East Asian and European populations [J]. Chinese Journal of Tissue Engineering Research, 2026, 30(6): 1569-1579. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||