Chinese Journal of Tissue Engineering Research ›› 2023, Vol. 27 ›› Issue (27): 4421-4428.doi: 10.12307/2023.631
Clinical and imaging features of slipped capital femoral epiphysis
Gao Yue, Fu Ziwei, Wu Yanbo, Pan Shinong, Lu Zhao
- Department of Radiology, Shengjing Hospital of China Medical University, Shenyang 110004, Liaoning Province, China
-
Received:2022-06-02Accepted:2022-08-20Online:2023-09-28Published:2022-11-08 -
Contact:Lu Zhao, Attending physician, Department of Radiology, Shengjing Hospital of China Medical University, Shenyang 110004, Liaoning Province, China -
About author:Gao Yue, PhD, Lecturer, Department of Radiology, Shengjing Hospital of China Medical University, Shenyang 110004, Liaoning Province, China -
Supported by:the Guidance Program of Natural Science Foundation of Liaoning Province, No. 2019-ZD-0794 (to PSN)
CLC Number:
Cite this article
Gao Yue, Fu Ziwei, Wu Yanbo, Pan Shinong, Lu Zhao. Clinical and imaging features of slipped capital femoral epiphysis[J]. Chinese Journal of Tissue Engineering Research, 2023, 27(27): 4421-4428.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
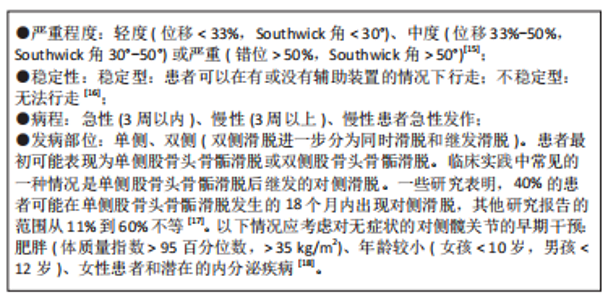
2.1 股骨头骨骺滑脱的流行病学表现 股骨头骨骺滑脱的发病率差异很大[4],这种发病率的差异可能与研究人群的地理位置、种族、季节变化和经济水平等差异有关[5]。股骨头骨骺滑脱的病因尚不明确,可能与患儿的激素水平、体质量指数、放射治疗及创伤相关。股骨头骨骺滑脱对患者造成相当大的经济及身心负担,这主要是因为股骨头骨骺滑脱患者可能继发长期并发症,包括股骨头缺血坏死(Avascular necrosis of femoral head,AVN)、股骨髋臼撞击症(Femoroacetabular impingement,FAI)、软骨溶解和退行性关节炎[6-8]。尽管股骨头骨骺滑脱的病理和临床治疗方案易于理解和掌握,但这种疾病可能困扰患者的余生,因为股骨头骨骺滑脱的长期后遗症或并发症存在不可逆性,可能会导致患者早期残疾并需要髋关节重建手术,严重影响患者工作与生活质量,给家庭和社会带来沉重的经济负担。 2.2 病因及分类 股骨头骨骺滑脱的病因和发病机制是复杂和多因素的,包括性别、机械、内分泌、肥胖和遗传影响等。受影响的患者通常在11-15岁,发病的平均年龄随青春期的提前开始而下降。男孩和女孩患病的比例约为2∶1至3∶1[9]。男孩的发病年龄较高,这主要是因为男孩的青春期晚于女孩的青春期[10]。机械力学因素包括髋臼后倾增加,这改变了髋关节的接触点和应力。股骨近端骨骺的倾斜度也会影响发病率[11]。 内分泌紊乱也使儿童更容易患上股骨头骨骺滑脱。甲状腺激素异常和甲状旁腺功能障碍与股骨头骨骺滑脱具有充分的关联。重组生长激素疗法也被确定为发生股骨头骨骺滑脱的危险因素。股骨头骨骺滑脱发生于10岁之前或16岁之后,是识别患有潜在内分泌病的风险较高儿童的可靠因素。具有潜在内分泌病的单侧股骨头骨骺滑脱患者发生对侧滑脱的风险增加,应进行预防性固定治疗[12]。其他股骨头骨骺滑脱患者中常见的内分泌疾病包括生长激素分泌不足、性腺功能减退、垂体功能减退和肾性骨营养不良[13]。事实上,对于早期(< 10岁)或双侧症状的股骨头骨骺滑脱患者,应进行内分泌检查。肥胖和股骨头骨骺滑脱之间有明显的关联,在较高体质量指数患者中股骨头骨骺滑脱发病率较高。最后,基因的影响也已经被注意到,但没有完全阐明。有研究证实患有股骨头骨骺滑脱儿童的Ⅱ型胶原和聚集素的基因表达下调[14]。作为一个多因素共同影响并作用产生的疾病,研究者们也应该全面认识股骨头骨骺滑脱,对造成股骨头骨骺滑脱的病因进行全面分析判断,避免遗漏潜在的作用因素,消除病因,如垂体源性及肾性股骨头骨骺滑脱,防止股骨头骨骺滑脱治疗后的进展及对策股骨头骨骺滑脱的 发生。 基于不同的临床衡量指标,可以将股骨头骨骺滑脱患者进行以下分类[15-18]:"
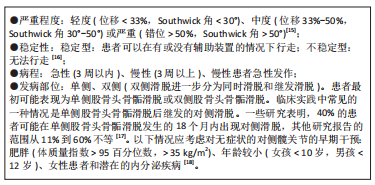
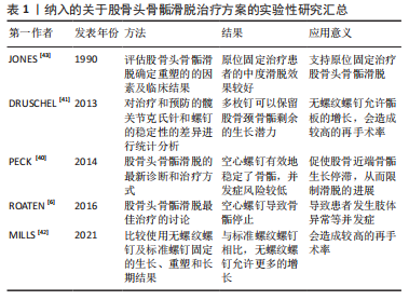
2.3 股骨头骨骺滑脱的并发症 股骨头骨骺滑脱的主要并发症为股骨头缺血性坏死、股骨髋臼撞击症及髋关节软骨溶解与退行性关节炎。这些疾病主要影响股骨头骨骺滑脱患者患侧髋关节的解剖结构与活动功能,造成患者髋部疼痛、跛行甚至无法行走的临床结局。患者的髋关节常需要经历股骨头骨骺滑脱骨骺固定后的二次手术来缓解或根治并发症的持续发展。股骨头骨骺滑脱并发症的出现甚至比股骨头骨骺滑脱本身更具有破坏性、持续性和复杂性。 2.3.1 股骨头缺血性坏死 股骨头缺血性坏死是股骨头骨骺滑脱最严重的并发症,多见于不稳定滑脱,相关研究中股骨头缺血坏死最高发病比例可达58%[19]。股骨头缺血坏死可能在股骨头骨骺滑脱后的几个月内发病,臀部疼痛和无力感随着时间推移而恶化,较多累及的部位是股骨头前上部。随着股骨头坏死骨的塌陷,患者的临床症状加剧,随后髋关节的迅速破坏难以避免。股骨头骨骺滑脱后出现股骨头缺血坏死的原因是,股骨头骨骺的滋养血管在滑脱过程中或滑脱手术复位时出现牵拉扭曲或阻塞,使股骨头骨骺失去血液供应,产生骨坏死的病理改变。不稳定的股骨头骨骺滑脱是股骨头缺血坏死的主要危险因素,滑倒严重程度对股骨头骨骺滑脱的发生没有影响,但不稳定股骨头骨骺滑脱发生股骨头缺血坏死的风险随着滑脱严重程度的增加而增加[20]。但手术治疗股骨头骨骺滑脱造成的股骨头缺血坏死也不可忽视,例如股骨头骨骺的营养血管被插入的钉或螺钉损伤[21]。过分纠正解剖学上的不稳定滑脱会压迫颈部骨痂上的营养血管,导致动静脉络膜坏死[22]。 目前,已有大量的研究证据支持应该避免通过闭合方法对不稳定滑脱进行解剖复位。经分析发现在原位钉扎手术中,不完全还原解剖结构比完全还原解剖具有更好的骨骺保护作用,股骨头缺血坏死发生率从80%下降到33%[23]。预防滑脱后股骨颈畸形的股骨颈截骨手术也可能危及股骨头的动脉供应[6]。不完全骨骺复位时,患者髋关节解剖形态出现异常,塑形能力差者可能会产生股骨髋臼撞击的症状,需要手术矫正髋关节解剖消除股骨颈部与髋臼边缘的撞击症状。完全解剖复位与不完全解剖复位股骨头骨骺都会出现继发并发症的可能。但在股骨头骨骺滑脱后手术复位骨骺时,追求股骨头骨骺解剖复位代价可能十分高昂,一旦危及股骨头骨骺的血液供应,产生的临床预后效果远远低于不完全解剖复位手术效果。股骨头缺血坏死的出现意味着股骨头骨骺滑脱患者髋关节及股骨头结构及功能的丧失,手术行髋关节置换为最终治疗方案。 2.3.2 股骨髋臼撞击症 在股骨头骨骺滑脱患者股骨头颈交界处重塑后,仍在29.4%的患者中观察到股骨髋臼撞击症[24]。股骨髋臼撞击症是一种临床诊断,包括症状、体征和影像学表现,应使用基于临床证据的医生主观检查、体格检查和影像学检查来诊断,必须存在疼痛才能诊断股骨髋臼撞击症。股骨髋臼撞击症是一种不协调的球窝畸形,导致髋关节终末运动时重复接触,产生腹股沟疼痛,并最终造成关节盂唇和软骨退化、髋关节骨关节炎。患者通常会出现腹股沟疼痛、关节僵硬、肌肉无力和运动表现受损,髋关节屈曲和内旋会加剧这种疼痛。一些观点认为,股骨髋臼撞击症不是股骨头骨骺滑脱的并发病,而是股骨头骨骺滑脱稳定或治疗后的预后结局之一。研究表明,在轻度股骨头骨骺滑脱后随访至少20年的病例中79%的髋关节出现股骨髋臼撞击症的临床和影像学征象[25]。一项关于股骨头骨骺滑脱和原发性骨关节炎患者的研究显示,股骨头骨骺滑脱后患者发生股骨髋臼撞击症畸形比原发性骨关节炎患者出现股骨髋臼撞击症畸形年轻11岁[26]。股骨头骨骺滑脱的严重程度与股骨髋臼撞击症的风险相关,股骨髋臼撞击症使100%的严重股骨头骨骺滑脱、50%的中度股骨头骨骺滑脱和33%的轻度股骨头骨骺滑脱复杂化[27]。髋关节原发性或继发性退化过程的主要解剖结构是髋臼盂唇和相邻的边缘软骨。 目前,股骨髋臼撞击症被认为是导致关节软骨损伤的主要机械病理学因素[28]。股骨髋臼撞击症有2种类型,第一种是凸轮型股骨髋臼撞击症,正常的髋关节形态伴有股骨颈畸形,导致前上盂唇和髋臼关节软骨磨损。α角是定义凸轮股骨髋臼撞击症的常用X射线指标,一般大于50°-55°视为异常。第二种是钳型股骨髋臼撞击症,髋关节存在过度覆盖,但股骨颈形态较为正常,畸形股骨颈不能再进入髋臼,冲击髋臼边缘[29]。严重的滑脱既有髋臼边缘的病变,也有股骨颈的病变(混合型股骨髋臼撞击症)[30]。两种类型的股骨髋臼撞击症并非一定引起临床症状。无症状人群中凸轮型股骨髋臼撞击症的患病率最低,有症状人群中的凸轮型股骨髋臼撞击症患病比例最高。男性患者明显多于女性患者,患病比例大约为2∶1,双髋关节受累的男女患病比例约为 3∶1。有症状的股骨髋臼撞击症则取决于个人活动的类型、强度和频率,与无症状人群相比,凸轮撞击在运动员中更为常见[11,31]。股骨髋臼撞击症的治疗包括手术和非手术选择,例如物理治疗师主导的干预措施。近年来,关节镜手术已成为治疗髋关节疼痛的首选治疗方案,但这种类型的手术成本高、风险高,疗效尚不确定。非手术方法是股骨髋臼撞击症的一线选择,手术干预为次要选择。物理治疗师主导的干预措施是一种有效、低风险和节省成本的手术替代方案,可以减少股骨髋臼撞击症患者的临床症状。提升躯干肌肉力量是股骨髋臼撞击症患者的重要治疗目标,当躯干肌肉力量下降时,会增加髋臼后倾和撞击[32]。 2.3.3 髋关节软骨溶解 滑脱稳定可使髋部疼痛迅速缓解。如果手术后患者的临床症状持续不缓解,则可能是髋关节软骨溶解的结果,软骨溶解被定义为进行性关节软骨吸收。软骨溶解的发病率约为7%[33],病因尚不清楚。患有中度股骨头骨骺滑脱和股骨髋臼撞击症的患者可能会承受凸轮畸形的反复微创伤,这种创伤可能发生在锻炼或日常活动中,这种微创伤会产生不可逆的软骨损伤,从而导致髋关节退行性疾病[34]。研究表明,由凸轮型畸形引起的髋关节退化通常在50岁左右发生[35-36]。虽然软骨溶解的病因未知,但发生软骨溶解的危险因素是已知的,与软骨溶解风险相关的因素有刺入关节间隙的植入物(针或螺钉)、严重的股骨头骨骺滑脱、肥胖患者、自身免疫因素、延迟诊断和骺板融合前的转子下截骨术有关[37-39]。股骨头骨骺滑脱患者手术后,出现髋关节软骨溶解时,患者的临床表现不但没有改善,反而恶化,患者主诉髋部疼痛加重,活动受限,一瘸一拐。疼痛会反映在大腿或膝盖上。骨盆X射线片显示有症状髋关节较无症状对侧髋关节间隙缩小50%以上是软骨溶解的诊断证据[39]。在双侧股骨头骨骺滑脱的病例中,关节间隙小于3 mm且有持续症状的患者被认为是软骨溶解的征兆[6]。治疗包括去除关节间隙的植入物,物理治疗和镇痛药等。作为股骨头骨骺滑脱的破坏性并发症,髋关节软骨溶解的预后通常好于股骨头缺血性坏死。 2.4 股骨头骨骺滑脱的治疗 目前,关于股骨头骨骺滑脱的最佳手术治疗方式尚无临床共识。避免滑脱进展和后遗症,维持滑脱稳定是任何形式股骨头骨骺滑脱治疗的主要目的。这可以通过骨科常规使用的植入物(如空心螺钉和销钉)或专门为治疗股骨头骨骺滑脱而设计的植入物(如可伸缩螺钉)来实现。所有的植入物都能有效地稳定滑脱;但它们对股骨颈生长软骨的生长潜力有不同的影响。用空心螺钉在股骨颈干骺端原位固定股骨头骨骺是治疗稳定和不稳定股骨头骨骺滑脱的广泛使用的治疗方法。空心螺钉有效地稳定了骨骺,据研究显示,与其他植入物相比,空心螺钉的并发症风险较低[40]。与此同时,典型的螺钉插入技术促使股骨近端骨骺生长停滞,从而限制滑脱的进展。两三枚光滑的不锈钢钉穿过生长板,从股骨头骨骺软骨下向外推,也是稳定滑脱的安全选择。与典型的空心螺钉固定相比,多枚钉可以保留股骨颈骨骺剩余的生长潜力[41-42],但无螺纹螺钉允许骺板更多的增长会造成较高的再手术率,见表1。"
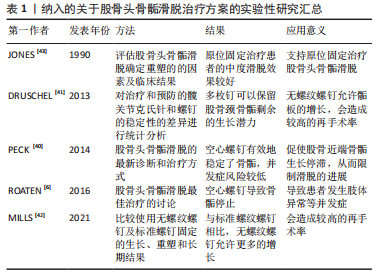
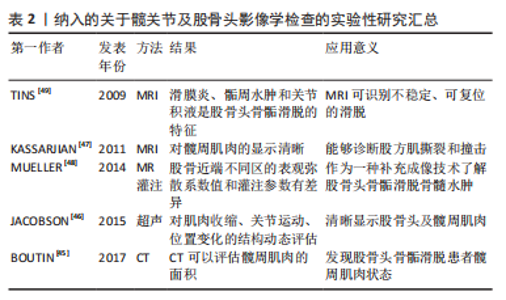
根据其对股骨颈骨骺残留生长的影响,存在2种类型的股骨头骨骺滑脱固定技术:限制骺板生长和保留骺板生长的手术技术。在过去,大多数外科医生的目标是终止骨骺生长,通过插入一个空心螺钉的方式,在股骨颈干骺端压缩股骨头骨骺。研究表明,这可以在6-12个月内导致骨骺停止[6,43]。早期骨骺关闭意味着患者失去了改善股骨头骨骺滑脱相关股骨颈畸形的任何机会,将会导致患者发生短髋、髋内翻和下肢长度不等的肢体异常,影响患者运动能力及生活质量。最近有关股骨颈生长和重塑的研究建议,股骨头骨骺滑脱治疗应该充分利用股骨颈骨骺的剩余生长,以预防股髋臼撞击和肢体长度不等并发症[44]。这在相对年轻的患者中至关重要。因此手术固定植入物的选择需要综合考虑患儿的身体状态及临床收益决定。 2.5 影像学诊断手段在股骨头骨骺滑脱中的价值 X射线成像是初步评估股骨头骨骺滑脱时的主要成像方式。此外,磁共振成像 (Magnetic resonance imaging,MRI)、计算机断层扫描 (Computed tomography,CT)、超声和骨扫描显像技术在评估这种疾病中发挥了作用[45-47]。术前,影像学手段可以在诊断、严重程度评估、手术计划和预后评估方面提供关键帮助。术后,影像学手段可以提供有关短期和长期并发症的信息,包括植入物相关问题、股骨头缺血坏死和股骨髋臼撞击症,并用于计划任何关节保留的手术。根据序列设计(例如,弥散加权序列、MRI灌注成像、特异性软骨高分辨率技术),功能性MRI序列可以揭示股骨头的血液循环障碍和软骨损伤等功能异常及解剖细节[48-50]。影像学追踪股骨头骨骺滑脱的全部病理生理过程有助于患者诊疗计划的制定与实施,使医生对患者病情掌握更加主动,帮助患者恢复更好的临床预后表现,见表2。"
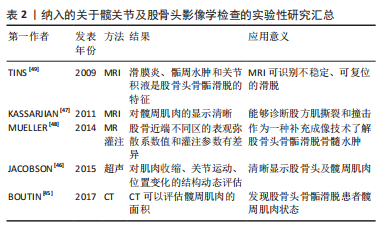
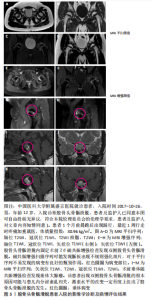
2.5.1 入院的诊断及病情评估 临床上X射线片、CT及MRI常用于股骨头骨骺滑脱患者入院时的诊断与病情评估。X射线片检查多用于最初患者就诊时的初步筛查,可以直观观察到骨骺与干骺端的形态、密度及相对位置,高效地检查出股骨头骨骺滑脱的骨性异常。如果X射线片检查结果正常,但仍怀疑股骨头骨骺滑脱可能,CT及MRI可进一步明确诊断,因为CT及MRI对诊断无临床症状且影像表现较为轻微的股骨头骨骺滑脱具有很高的敏感性及特异性,可用于隐匿及亚临床股骨头骨骺滑脱的诊断。X射线片中测量的α角可以评估股骨头骨骺滑脱的骨骺滑脱严重程度。 由Southwick定义的骨骺-骨干滑移角(侧位X射线片上骨骺线的垂线与股骨干轴之间的角度)在临床上应用广泛,它决定了股骨头骨骺相对于股骨颈的滑脱角度[51-52],从而定义股骨头骨骺滑脱的滑脱严重程度。与X射线片诊断相比,使用MRI检测即将发生的股骨头骨骺滑脱更为敏感,可以更早地做出预防性稳定手术。 与MRI一样,3D重建的薄层CT具有准确估计股骨头骨骺滑脱畸形的范围、形状和方向的优势。因此,如果手术治疗取决于畸形的确切程度和特征,特别是如果计划进行矫正截骨术,则应在术前进行CT检查评估。同时,CT及MRI还可用于股骨头骨骺滑脱患者更为细节及量化的病情评估。CT评价股骨头骨骺滑脱患者髋关节的髋臼覆盖率和髋臼旋转度,可以检测潜在的钳型畸形[53]。与健康对照组相比,在股骨头骨骺滑脱患者中观察到显著的后倾畸形和增加的过度覆盖。有观点认为,后倾的髋臼可能会在股骨近端产生额外的压力,从而可能促进滑脱的发展。术前CT影像还可以用来预测股骨头骨骺滑脱的骨骺稳定性[54],根据预测结果,医疗机构可以对股骨头骨骺滑脱患者进行病情分类并改善患者护理。基于定量磁共振成像 (QMRI) 的技术(例如T1和T2mapping)已被证明在检测患者髋关节软骨成分的早期变化方面足够敏感[55-56]。髋关节MRI检查可以定量评价股骨头骨骺滑脱患者髋周肌肉状态[57]。 1998年,ROBBEN等[58]首次描述了股骨头骨骺滑脱患者患侧髋关节的髋部肌肉萎缩的现象。作者所在研究团队已发表的研究显示,与对照组相比,单侧股骨头骨骺滑脱患者的患侧髋周肌群呈现明显萎缩的状态,且萎缩程度与股骨头骨骺滑脱的严重程度相关[57]。股骨头骨骺滑脱伴有髋部肌肉萎缩时,肌肉力量和髋关节稳定性明显下降,髋关节退行性疾病的风险较高。髋周肌肉的恢复状态可能对股骨头骨骺滑脱患者的步态造成影响。严重的髋部肌肉萎缩是股骨头骨骺滑脱患者髋部退化的危险因素。在股骨头骨骺滑脱发生的早期,稳定骨骺滑脱之后,恢复髋部肌肉的形态和功能至关重要。 图3,4为中国医科大学附属盛京医院放射科收录的股骨头骨骺滑脱患者入院的影像学诊断及病情评估结果。"
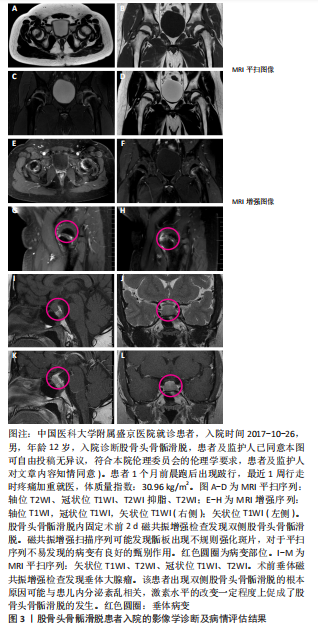

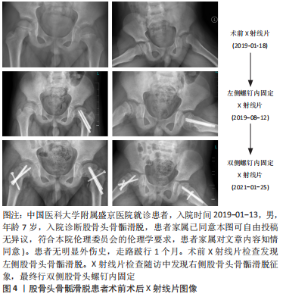
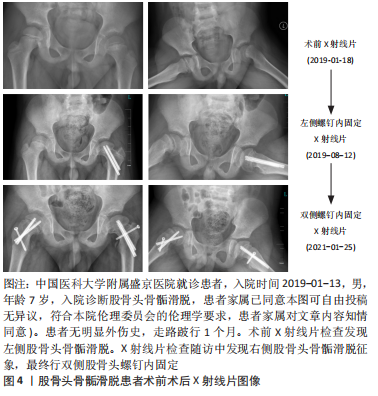
2.5.2 手术效果评价及术后的随访 影像结果可以为临床治疗手段的应用及改进提供可靠且详细的证据。X射线片检查是临床用来追踪患者预后结局及评价手术安全性的最常用手段[59]。通过术后X射线片随访检查发现,伸缩螺钉在稳定股骨头骨骺滑脱方面不劣于传统螺钉,并且它们允许预防性固定的股骨颈持续生长[60]。关节镜下骨软骨成形术可以成功地矫正轻度的股骨头骨骺滑脱非球面头颈连接处,该修正是否在至少5年内保持稳定通过影像学随访确定,结果显示通过MRI图像测量的α角在术后3个月和6年无差异。矫正轻度股骨头骨骺滑脱的原位固定和髋关节镜检查可恢复正常的α角,并在中期随访中显示稳定的形态学矫正[61]。影像学是术后随访及手术效果评估的重要环节,是临床全面评估患者预后的关键佐证。该课题组预试验中1名7岁男性患儿初次就诊时诊断为左侧股骨头骨骺滑脱,行左侧股骨头螺钉内固定,在随后的X射线片及磁共振定期随访中,发现患儿右侧股骨头预滑脱的影像学征象,最终患儿右侧股骨头也进行了螺钉内固定。由此可见,股骨头骨骺滑脱患者影像学随访的重要性,在发现对侧滑脱征象,在滑脱早期为临床提供证据并进行预固定,防止进一步滑脱,为患者争取更好的预后状态(减少股骨髋臼撞击症及股骨头缺血坏死等并发症的出现),见图4,5。"


2.5.3 单侧股骨头骨骺滑脱患者对侧骨骺滑脱的预测 有几个因素与继发对侧髋关节股骨头骨骺滑脱的风险增加有关,包括年龄、代谢紊乱、骨骼成熟度,以及放射学测量角(例如后倾角、α角和骨骺倾斜角)。在以往的一些研究中,年龄较小和后倾角较大是继发对侧 股骨头骨骺滑脱的重要危险因素。单侧股骨头骨骺滑脱患者发生对侧股骨头骨骺滑脱的可能性远远大于普通儿童。在股骨头骨骺滑脱发生早期的影像学表现中,如股骨近端骨质减少,或不规则,如近端生长板增宽,可能差别较为隐匿,临床症状轻微,因此可能被临床忽视。软骨溶解继发关节软骨快速损失、关节间隙缩小及软骨下骨进行性骨质减少可发生在所有严重程度的股骨头骨骺滑脱中。 MRI检查还能够在高危人群骨骺骺板发生实际滑动(预滑脱)之前显示骺板区域的水肿和异常。α角也被一些研究认为是未来对侧髋关节疾病的独立预后因素:α角> 50.5°意味着对侧发生股骨头骨骺滑脱的风险更高,建议作为对侧预防性手术的分界点[62-63]。改良牛津评分被作为骨骼成熟度的代表参数,并且在对侧髋关节继发股骨头骨骺滑脱的患者中,该评分较低。有研究显示,患儿年龄≤11岁、改良牛津评分≤20分和双髋干骺角之差≤21°是对侧继发骨骺滑脱的危险因素。每个危险因素的存在都增加了继发对侧股骨头骨骺滑脱的风险,同时具有3个危险因素将对侧发展成为股骨头骨骺滑脱的风险增加到73%。年龄较小、较低的改良牛津评分以及患侧和健侧的髋部骨骺-骨干角之差较小时,单侧股骨头骨骺滑脱患者后续发生对侧股骨头骨骺滑脱的风险显著增加[17]。除了患儿的流行病学参数及骨骼测量指数,影像学上的角度测量对于评估对侧股骨头骨骺滑脱风险存在较为明显的指向性,掌握干骺端与骨骺成角角度的测量将对诊断健侧股骨头预滑脱的发生提供帮助。"

| [1] SCHROEDER PB, NICHOLES MA. Schmitz MR hip injuries in the adolescent athlete. Clin Sports Med. 2021;40(2):385-398. [2] 贾国强.儿童股骨头骨骺滑脱诊治研究进展[J].国际儿科学杂志, 2019,46(6):449-452. [3] 李浩,张自明.股骨头骨骺滑脱的诊断与治疗相关研究进展[J].中华小儿外科杂志,2018,39(11):872-876. [4] APRATO A, CONTI A, BERTOLO F, et al. Slipped capital femoral epiphysis: current management strategies. Orthop Res Rev. 2019;11:47-54. [5] LEHMANN CL, ARONS RR, LODER RT, et al. The epidemiology of slipped capital femoral epiphysis: an update. J Pediatr Orthop. 2006;26(3): 286-290. [6] ROATEN J, SPENCE DD. Complications related to the treatment of slipped capital femoral epiphysis. Orthop Clin North Am. 2016;47(2): 405-413. [7] HELGESSON L, JOHANSSON PK, AURELL Y, et al. Early osteoarthritis after slipped capital femoral epiphysis. Acta Orthop. 2018;89(2):222-228. [8] ORTEGREN J, PETERSON P, SVENSSON J, et al. Persisting CAM deformity is associated with early cartilage degeneration after Slipped Capital Femoral Epiphysis: 11-year follow-up including dGEMRIC. Osteoarthritis Cartilage. 2018;26(4):557-563. [9] DAVEY S, FISHER T, SCHRADER T. Controversies in the management of unstable slipped capital femoral epiphysis. Orthop Clin North Am. 2022;53(1):51-56. [10] ZILKENS C, JAGER M, BITTERSOHL B, et al. Slipped capital femoral epiphysis. Orthopade. 2010;39(10):1009-1021. [11] PARCELLS BW. Pediatric hip and pelvis. Pediatr Clin North Am. 2020; 67(1):139-152. [12] SHAW KA, SHIVER AL, OAKES T, et al. Slipped capital femoral epiphysis associated with endocrinopathy: a narrative review. JBJS Rev. 2022; 10(2). doi: 10.2106/JBJS.RVW.21.00188. [13] WIRTH T, EBERHARDT O, CERKEZ D, et al. Specific cases of slipped capital femoral epiphysis: endocrinopathies, hormone therapy and other rare causes. Orthopade. 2019;48(8):685-692. [14] SCHARSCHMIDT T, JACQUET R, WEINER D, et al. Gene expression in slipped capital femoral epiphysis. Evaluation with laser capture microdissection and quantitative reverse transcription-polymerase chain reaction. J Bone Joint Surg Am. 2009;91(2):366-377. [15] BOYER DW, MICKELSON MR, PONSETI IV. Slipped capital femoral epiphysis. Long-term follow-up study of one hundred and twenty-one patients. J Bone Joint Surg Am. 1981;63(1):85-95. [16] LODER RT, RICHARDS BS, SHAPIRO PS, et al. Acute slipped capital femoral epiphysis: the importance of physeal stability. J Bone Joint Surg Am. 1993;75(8):1134-1140. [17] SWARUP I, SHAH R, GOHEL S, et al. Predicting subsequent contralateral slipped capital femoral epiphysis: an evidence-based approach. J Child Orthop. 2020;14(2):91-97. [18] SAMELIS PV, PAPAGRIGORAKIS E, KONSTANTINOU AL, et al. Factors affecting outcomes of slipped capital femoral epiphysis. Cureus. 2020; 12(2):e6883. [19] LODER R What is the cause of avascular necrosis in unstable slipped capital femoral epiphysis and what can be done to lower the rate? J Pediatr Orthop. 2013;33:S88-S91. [20] TOKMAKOVA KP, STANTON RP, MASON DE. Factors influencing the development of osteonecrosis in patients treated for slipped capital femoral epiphysis. J Bone Joint Surg Am. 2003;85(5):798-801. [21] RILEY PM, WEINER DS, GILLESPIE R, et al. Hazards of internal fixation in the treatment of slipped capital femoral epiphysis. J Bone Joint Surg Am. 1990;72(10):1500-1509. [22] HERRERA-SOTO JA, DUFFY MF, BIRNBAUM MA, et al. Increased intracapsular pressures after unstable slipped capital femoral epiphysis. J Pediatr Orthop. 2008;28(7):723-728. [23] WALTON RD, MARTIN E, WRIGHT D, et al. The treatment of an unstable slipped capital femoral epiphysis by either intracapsular cuneiform osteotomy or pinning in situ: a comparative study. Bone Joint J. 2015; 97-B(3):412-419. [24] AKIYAMA M, NAKASHIMA Y, KITANO T, et al. Remodelling of femoral head-neck junction in slipped capital femoral epiphysis: a multicentre study. Int Orthop. 2013;37(12):2331-2336. [25] CASTANEDA P, PONCE C, VILLAREAL G, et al. The natural history of osteoarthritis after a slipped capital femoral epiphysis/the pistol grip deformity. J Pediatr Orthop. 2013;33 Suppl 1:S76-S82. [26] ABRAHAM E, GONZALEZ MH, PRATAP S, et al. Clinical implications of anatomical wear characteristics in slipped capital femoral epiphysis and primary osteoarthritis. J Pediatr Orthop. 2007;27(7):788-795. [27] MURGIER J, ESPIE A, BAYLE-INIGUEZ X, et al. Frequency of radiographic signs of slipped capital femoral epiphysiolysis sequelae in hip arthroplasty candidates for coxarthrosis. Orthop Traumatol Surg Res. 2013;99(7):791-797. [28] WIRRIES N, DIENST M. Labral lesions in femoroacetabular impingement syndrome: evidence-based treatment. Orthopade. 2022;51(6):450-457. [29] RAB GT. The geometry of slipped capital femoral epiphysis: implications for movement, impingement, and corrective osteotomy. J Pediatr Orthop. 1999;19(4):419-424. [30] GRIFFIN DR, DICKENSON EJ, O’DONNELL J, et al. The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): an international consensus statement. Br J Sports Med. 2016;50(19):1169-1176. [31] SIEBENROCK KA, FERNER F, NOBLE PC, et al. The cam-type deformity of the proximal femur arises in childhood in response to vigorous sporting activity. Clin Orthop Relat Res. 2011;469(11):3229-3240. [32] KEMP J, GRIMALDI A, HEEREY J, et al. Current trends in sport and exercise hip conditions: intra-articular and extra-articular hip pain, with detailed focus on femoroacetabular impingement (FAI) syndrome. Best Pract Res Clin Rheumatol. 2019;33(1):66-87. [33] LUBICKY JP. Chondrolysis and avascular necrosis: complications of slipped capital femoral epiphysis. J Pediatr Orthop. 1996;5(3):162-167. [34] ULICI A, CARP M, TEVANOV I, et al. Outcome of pinning in patients with slipped capital femoral epiphysis: risk factors associated with avascular necrosis, chondrolysis, and femoral impingement. J Int Med Res. 2018; 46(6):2120-2127. [35] WENSAAS A, SVENNINGSEN S, TERJESEN T Long-term outcome of slipped capital femoral epiphysis: a 38-year follow-up of 66 patients. J Child Orthop. 2011;5(2):75-82. [36] WENSAAS A, GUNDERSON RB, SVENNINGSEN S, et al. Femoroacetabular impingement after slipped upper femoral epiphysis: the radiological diagnosis and clinical outcome at long-term follow-up. J Bone Joint Surg Br. 2012;94(11):1487-1493. [37] JOFE MH, LEHMAN W, EHRLICH MG. Chondrolysis following slipped capital femoral epiphysis. J Pediatr Orthop. 2004;13(1):29-31. [38] TUDISCO C, CATERINI R, FARSETTI P, et al. Chondrolysis of the hip complicating slipped capital femoral epiphysis: long-term follow-up of nine patients. J Pediatr Orthop. 1999;8(2):107-111. [39] ARONSSON DD, LODER RT, BREUR GJ, et al. Slipped capital femoral epiphysis: current concepts. J Am Acad Orthop Surg. 2006;14(12): 666-679. [40] PECK K, HERRERA-SOTO J. Slipped capital femoral epiphysis: what’s new? Orthop Clin North Am. 2014;45(1):77-86. [41] DRUSCHEL C, PLACZEK R, FUNK JF. Growth and deformity after in situ fixation of slipped capital femoral epiphysis. Z Orthop Unfall. 2013; 151(4):371-379. [42] MILLS H, FLOWERS MJ, AGRAWAL Y, et al. Outcomes of distally un-threaded screw fixation of slipped capital femoral epiphysis at skeletal maturity: a matched cohort study. J Pediatr Orthop B. 2021;30(6): 540-548. [43] JONES JR, PATERSON DC, HILLIER TM, et al. Remodelling after pinning for slipped capital femoral epiphysis. J Bone Joint Surg Br. 1990;72(4): 568-573. [44] WÖLFLE-ROOS J, URLAUB S, REICHEL H, et al. Significantly lower femoral neck growth in screw fixation of the asymptomatic contralateral hip in unilateral slipped capital femoral epiphysis. J Pediatr Orthop B. 2016;25(3):197-201. [45] BOUTIN RD, BAMRUNGCHART S, BATENI CP, et al. CT of patients with hip fracture: muscle size and attenuation help predict mortality. AJR Am J Roentgenol. 2017;208(6):W208-W215. [46] JACOBSON JA, KHOURY V, BRANDON CJ. Ultrasound of the groin: techniques, pathology, and pitfalls. AJR Am J Roentgenol. 2015;205(3): 513-523. [47] KASSARJIAN A, TOMAS X, CEREZAL L, et al. MRI of the quadratus femoris muscle: anatomic considerations and pathologic lesions. AJR Am J Roentgenol. 2011;197(1):170-174. [48] MUELLER D, SCHAEFFELER C, BAUM T, et al. Magnetic resonance perfusion and diffusion imaging characteristics of transient bone marrow edema, avascular necrosis and subchondral insufficiency fractures of the proximal femur. Eur J Radiol. 2014;83(10):1862-1869. [49] TINS B, CASSAR-PULLICINO V, MCCALL I. The role of pre-treatment MRI in established cases of slipped capital femoral epiphysis. Eur J Radiol. 2009;70(3):570-578. [50] ZILKENS C, MIESE F, BITTERSOHL B, et al. Delayed gadolinium-enhanced magnetic resonance imaging of cartilage (dGEMRIC), after slipped capital femoral epiphysis. Eur J Radiol. 2011;79(3):400-406. [51] JONES CE, COOPER AP, DOUCETTE J, et al. Southwick angle measurements and SCFE slip severity classifications are affected by frog-lateral positioning. Skeletal Radiol. 2018;47(1):79-84. [52] JARRETT DY, MATHENEY T, KLEINMAN PK. Imaging SCFE: diagnosis, treatment and complications. Pediatr Radiol. 2013;43 Suppl 1:S71-S82. [53] GALLETTA C, APRATO A, GIACHINO M, et al. Hip morphology in slipped capital femoral epiphysis. J Pediatr Orthop. 2021;30(6):535-539. [54] FISCHER-COLBRIE ME, LOUER CR, BOMAR JD, et al. Predicting epiphyseal stability of slipped capital femoral epiphysis with preoperative CT imaging. J Child Orthop. 2020;14(1):68-75. [55] SUBBURAJ K, VALENTINITSCH A, DILLON AB, et al. Regional variations in MR relaxation of hip joint cartilage in subjects with and without femoralacetabular impingement. Magn Reson Imaging. 2013;31(7): 1129-1136. [56] SAMAAN MA, PEDOIA V, ZHANG AL, et al. A novel mr-based method for detection of cartilage delamination in femoroacetabular impingement patients. J Orthop Res. 2018;36(3):971-978. [57] GAO Y, LYU X, LIU Q, et al. Quantitative evaluation of hip muscle atrophy in patients with unilateral slipped capital femoral epiphysis based on magnetic resonance imaging. Acad Radiol. 2020;28(8):1125-1132. [58] ROBBEN SG, MERADJI M, DIEPSTRATEN AF, et al. US of the painful hip in childhood: diagnostic value of cartilage thickening and muscle atrophy in the detection of Perthes disease. Radiology, 1998;208(1):35-42. [59] ZUO B, ZHU JF, WANG XY, et al. Outcome of the modified Dunn procedure in severe slipped capital femoral epiphysis. J Orthop Surg Res. 2020;15(1):506. [60] HANSEN CH, BOMAR JD, BADRINATH R, et al. Telescoping screw fixation compared to traditional in situ screw fixation for slipped capital femoral epiphysis: clinical, radiographic and patient-reported outcomes. J Pediatr Orthop. 2022;31(3):224-231. [61] RAHM S, JUD L, JUNGWIRTH-WEINBERGER A, et al. Mid-term results after in situ pinning and hip arthroscopy for mild slipped capital femoral epiphysis: a minimum five-year follow-up. J Child Orthop. 2020;14(6): 521-528. [62] SWARUP I, GOODBODY C, GOTO R, et al. Risk factors for contralateral slipped capital femoral epiphysis: a meta-analysis of cohort and case-control studies. J Pediatr Orthop. 2020;40(6):e446-e453. [63] BOYLE MJ, LIROLA JF, HOGUE GD, et al. The alpha angle as a predictor of contralateral slipped capital femoral epiphysis. J Child Orthop. 2016;10(3):201-207. |
| [1] | Nong Fuxiang, Jiang Zhixiong, Li Yinghao, Xu Wencong, Shi Zhilan, Luo Hui, Zhang Qinglang, Zhong Shuang, Tang Meiwen. Bone cement augmented proximal femoral nail antirotation for type A3.3 intertrochanteric femoral fracturalysis [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(在线): 1-10. |
| [2] | Zhong Yizheng, Huang Peizhen, Cai Qunbin, Zheng Liqin, He Xingpeng, Dong Hang. Microstructural indexes that determine the trabecular bone maximum stress of micro-finite element models [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1313-1318. |
| [3] | Wu Taoguang, Nie Shaobo, Chen Hua, Zhu Zhengguo, Qi Lin, Tang Peifu. Biomechanical characteristics of a new multi-dimensional cross locking plate in the treatment of subtrochanteric nonunion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1330-1334. |
| [4] | Peng Zhixin, Yan Wengang, Wang Kun, Zhang Zhenjiang. Finite element analysis and structural optimization design of 3D printed forearm braces [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1340-1345. |
| [5] | Liu Guangwei, Feng Minshan, Zhu Liguo, Yin Xunlu, Chen Zhuoxian. Dynamic analysis of structural changes in the lower cervical intervertebral foramen during rotation-traction manipulation by virtual reality technology [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1346-1351. |
| [6] | Wen Xinghua, Ding Huanwen, Cheng Kai, Yan Xiaonan, Peng Yuanhao, Wang Yuning, Liu Kang, Zhang Huiwu. Three-dimensional finite element model analysis of intramedullary nailing fixation design for large femoral defects in Beagle dogs [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1371-1376. |
| [7] | Ke Yuqi, Chen Changjian, Wu Hao, Zheng Lianjie. Comparison of 12-month follow-up results of primary total hip arthroplasty between modified direct anterior approach and direct anterior approach [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1377-1382. |
| [8] | Zhang Lichuang, Gao Huali, Wang Jingchao, Lin Huijun, Wu Chonggui, Ma Yinghui, Huang Yunfei, Fang Xue, Zhai Weitao. Effect of tendon manipulation with equal emphasis on muscles and bones on accelerating the functional rehabilitation of quadriceps femoris after total knee arthroplasty [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1383-1389. |
| [9] | Zheng Hongrui, Zhang Wenjie, Wang Yunhua, He Bin, Shen Yajun, Fan Lei. Femoral neck system combined with platelet-rich plasma in the treatment of femoral neck fracture [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1390-1395. |
| [10] | Du Xueting, Zhang Xiaodong, Chen Yanjun, Wang Mei, Chen Wubiao, Huang Wenhua. Application of compressed sensing technology in two-dimensional magnetic resonance imaging of the ankle joint [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1396-1402. |
| [11] | Zheng Bo, Zhang Xiuli, Zhou Hao, He Zebi, Zhou Jin, Zhou Weiyun, Li Peng. Arthroscopy-assisted locking hollow screw fixation and open reduction plate internal fixation in the treatment of Schatzker II-III tibial plateau fractures: early CT evaluation [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1410-1416. |
| [12] | Cai Zhihao, Xie Zhaoyong. Femoral neck anteversion measurement assessment: how to establish a unified method and standard [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1448-1454. |
| [13] | He Yinhao, Li Xiaosheng, Chen Hongwen, Chen Tiezhu. 3D printed porous tantalum metal in the treatment of developmental dysplasia of the hip: current status and application prospect [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1455-1461. |
| [14] | Hu Xijian, Zhao Bin, Chai Huo, Liu Haifeng. Application of trunk surface morphometry in vertebral column defects [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1462-1468. |
| [15] | Wang Yanjin, Zhou Yingjie, Chai Xubin, Zhuo Hanjie. Meta-analysis of the efficacy and safety of 3D printed porous titanium alloy fusion cage in anterior cervical discectomy and fusion [J]. Chinese Journal of Tissue Engineering Research, 2023, 27(9): 1434-1440. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||